Chapter 29 Development BIO 211 Lecture Instructor Dr

Chapter 29: Development BIO 211 Lecture Instructor: Dr. Gollwitzer 1

• Today in class we will: – Define and describe development – Trace the general processes from ovulation through fertilization and formation of a zygote – List the stages of development – List the 3 stages of gestation and briefly describe the major events associated with each • Distinguish between embryo and fetus • Discuss the two major roles of the placenta • Discuss the basic structural and functional changes in the uterus during gestation – Briefly describe the events that occur during labor and delivery – Describe lactation and milk let-down reflex 2

Development • Begins with fertilization (conception) = – When male and female gametes (sperm and egg) unite to form single-cell zygote – Occurs in uterine tube 12 -24 hr after ovulation • Is the gradual modification from fertilization to maturity of: – Anatomical structures – Physiological characteristics 3
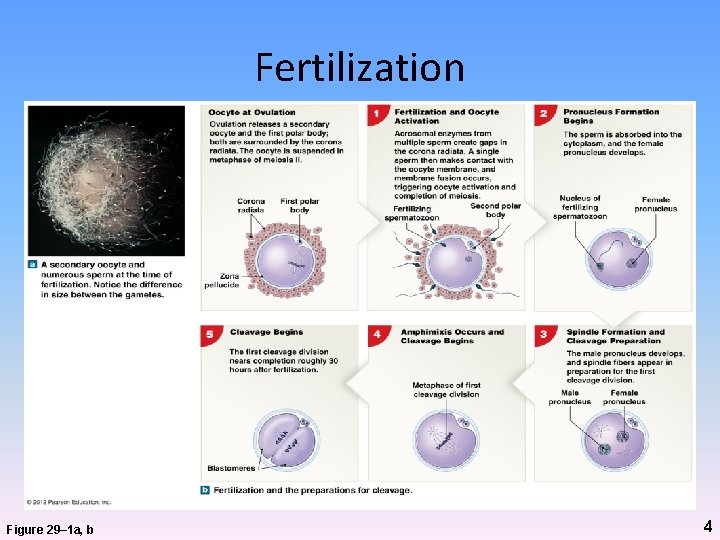
Fertilization Figure 29– 1 a, b 4

Amphimixis • • Fusion of female and male pronuclei Moment of conception Cell becomes zygote (46 chromosomes) Fertilization complete 5

Stages of Development • Prenatal – before birth – Embryological development • Occurs during first 2 mo after fertilization • Organs established – Fetal development • Begins at 9 th wk and continues to birth • Organs develop • Postnatal – after birth – Neonate = newborn 6

Gestation • Time spent in prenatal development • Consists of 3 trimesters, each 3 months long – First trimester – Second trimester – Third trimester 7

First Trimester • Cell cleavage (division) and blastocyst formation • Blastocyst implantation = burrowing into uterine wall • Placentation = formation of placenta – Temporary structure in uterine wall – Permits diffusion between fetal and maternal circulatory systems • Embryogenesis – all organ systems begin to be established; but nonfunctional – Embryo = organism in the developmental stage beginning at fertilization and ending at the start of the third developmental month (weeks 1 – 8) 8

First Trimester • Most dangerous period in prenatal life • Only 40% of conceptions produce embryos that survive past first trimester 9
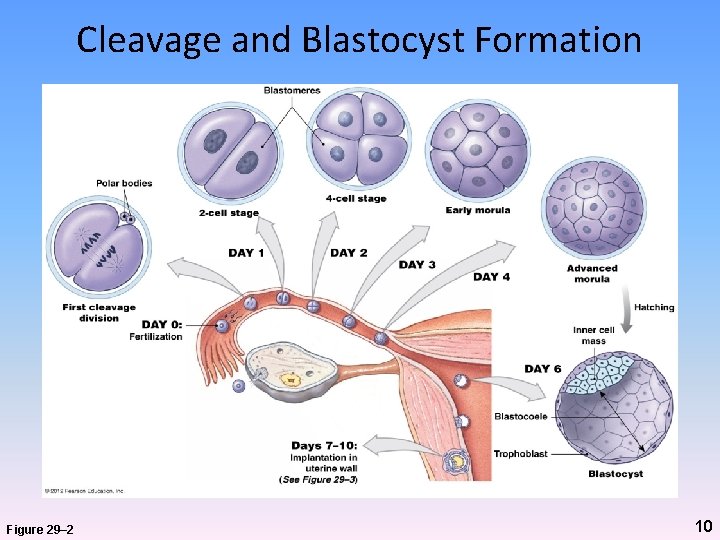
Cleavage and Blastocyst Formation Figure 29– 2 10
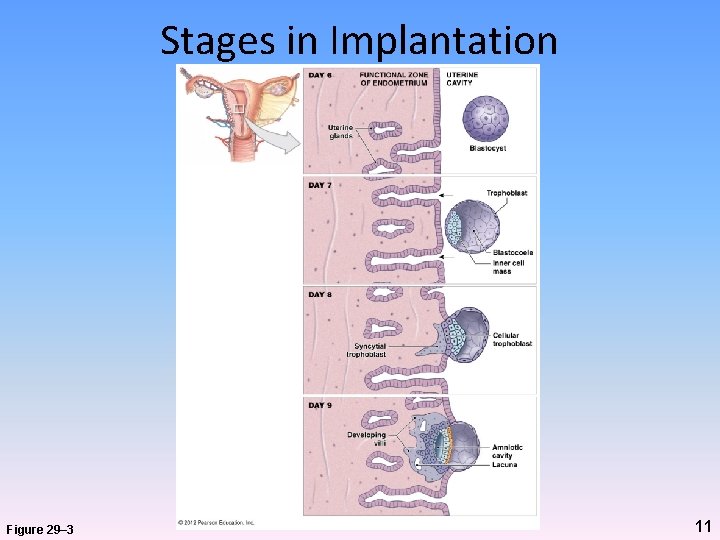
Stages in Implantation Figure 29– 3 11

Placenta • Complex organ that permits exchange between maternal and embryonic circulatory systems • Supports fetus in second and third trimesters • Stops functioning and is ejected from uterus after birth 12
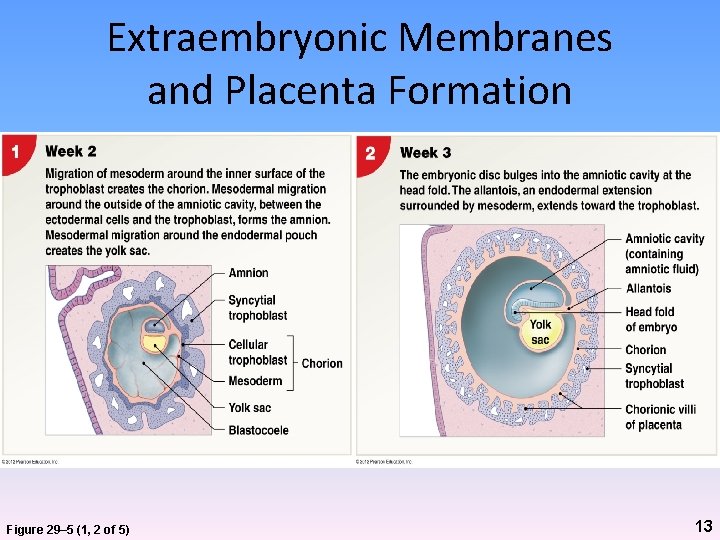
Extraembryonic Membranes and Placenta Formation Figure 29– 5 (1, 2 of 5) 13
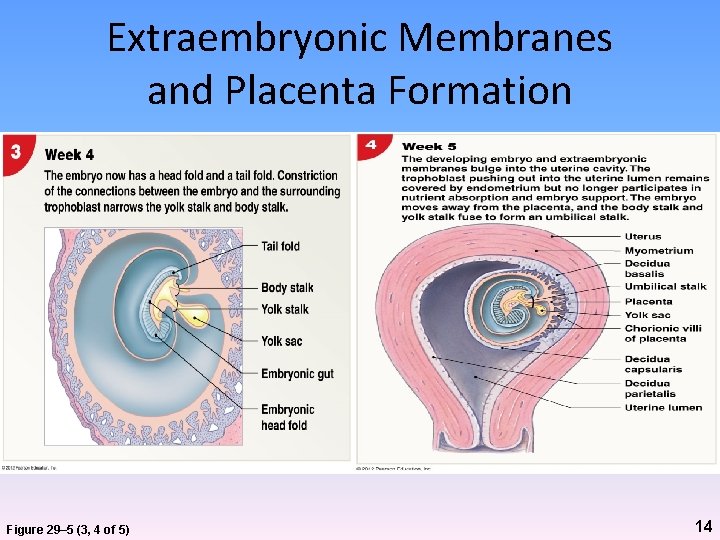
Extraembryonic Membranes and Placenta Formation Figure 29– 5 (3, 4 of 5) 14
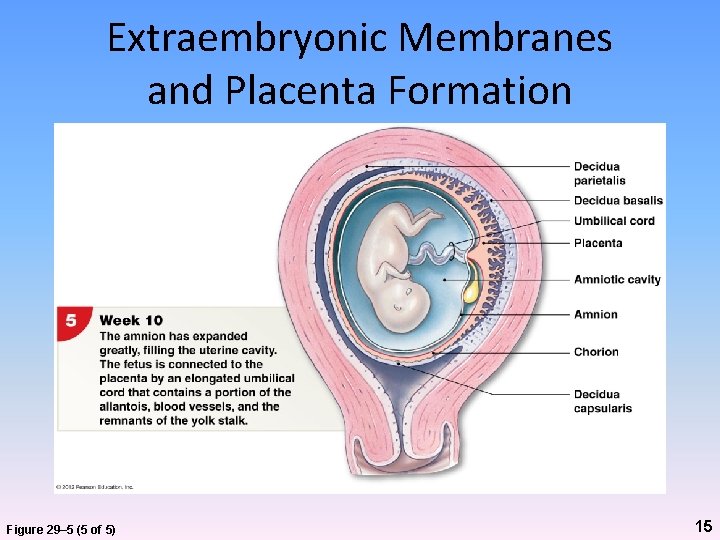
Extraembryonic Membranes and Placenta Formation Figure 29– 5 (5 of 5) 15
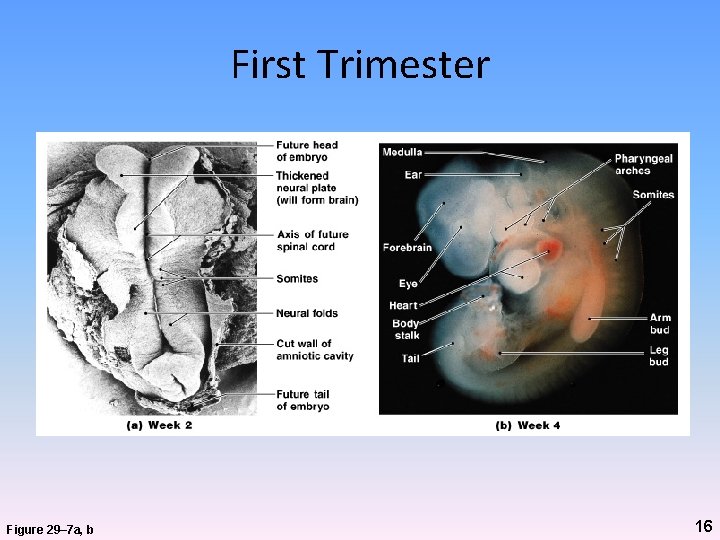
First Trimester Figure 29– 7 a, b 16
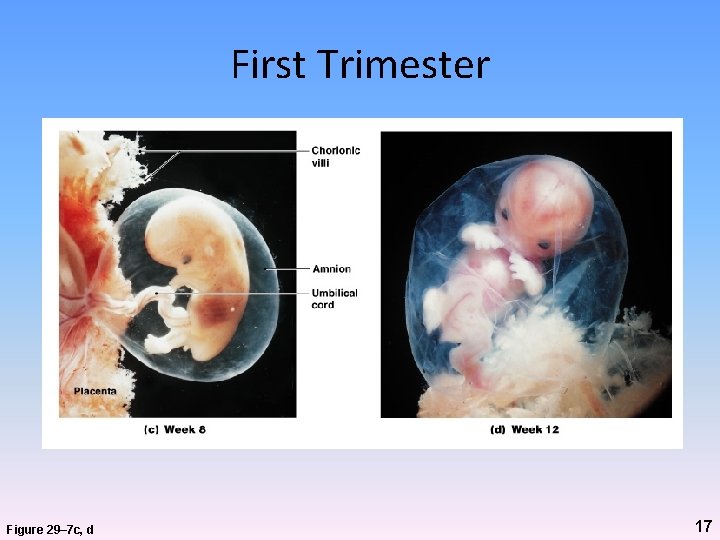
First Trimester Figure 29– 7 c, d 17

First Trimester: h. CG • h. CG = human chorionic gonadotropin • Produced by placenta • Appears in maternal bloodstream soon after implantation • Used as pregnancy test/kit • Maintains CL for 3 -4 months – So CL P (until placenta takes over P production) 18

Second Trimester • Fetal stage = development of all organ systems (organogenesis) • Rapid growth of fetus – Fetus = organism in the developmental stage lasting from the start of the third developmental month to delivery (week 9 through delivery) • Body proportions change • Progesterone levels increase 19

Third Trimester • Organ systems fully functional • Fetal growth rate slows • Largest weight gain 20
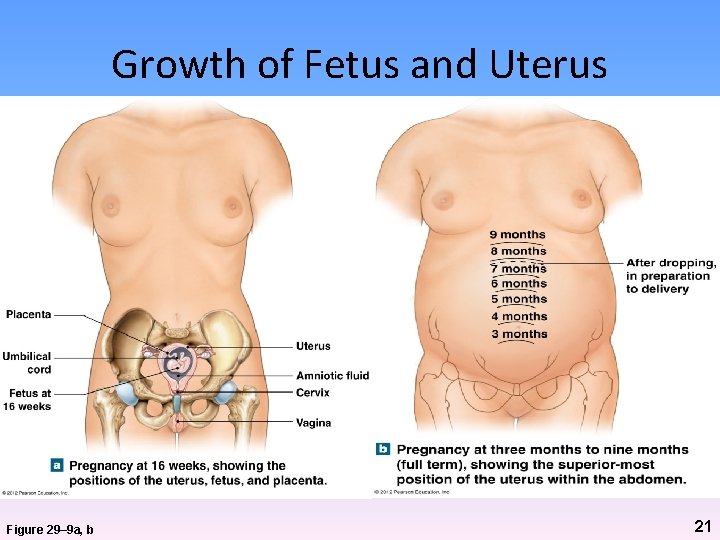
Growth of Fetus and Uterus Figure 29– 9 a, b 21
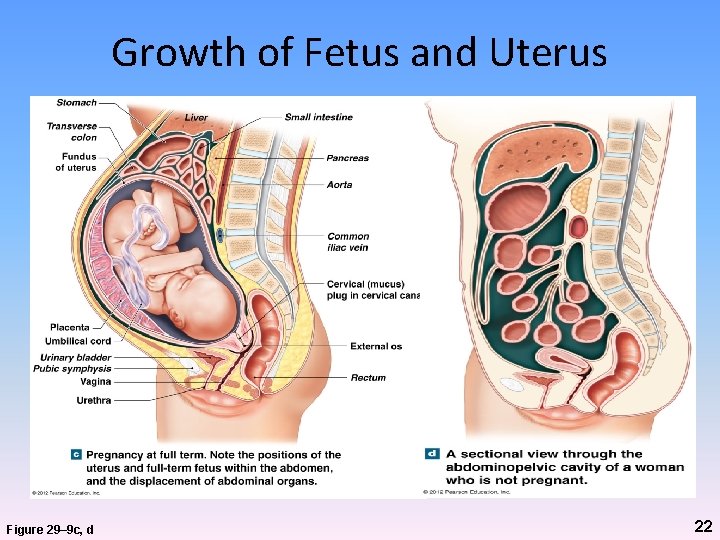
Growth of Fetus and Uterus Figure 29– 9 c, d 22
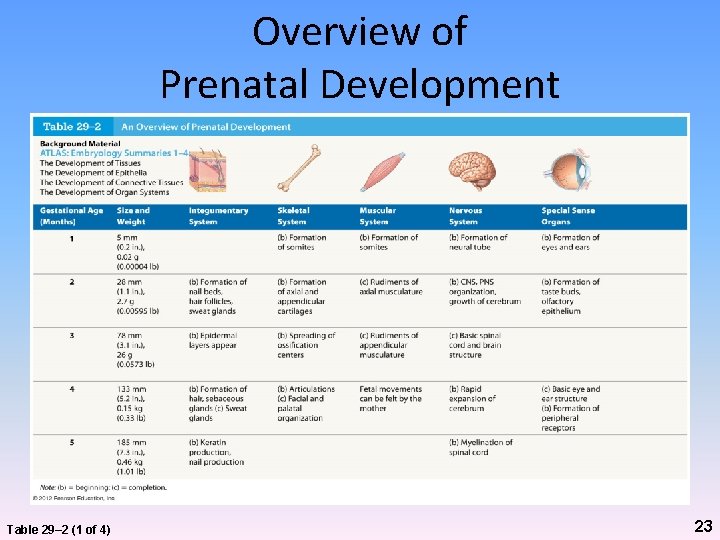
Overview of Prenatal Development Table 29– 2 (1 of 4) 23
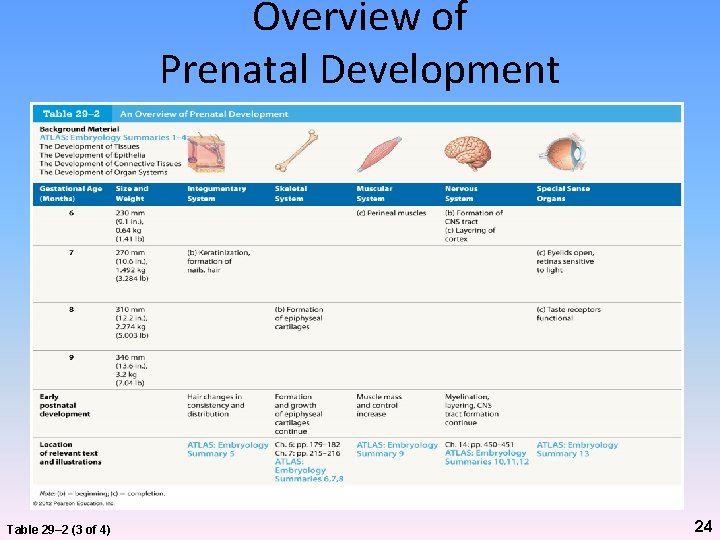
Overview of Prenatal Development Table 29– 2 (3 of 4) 24
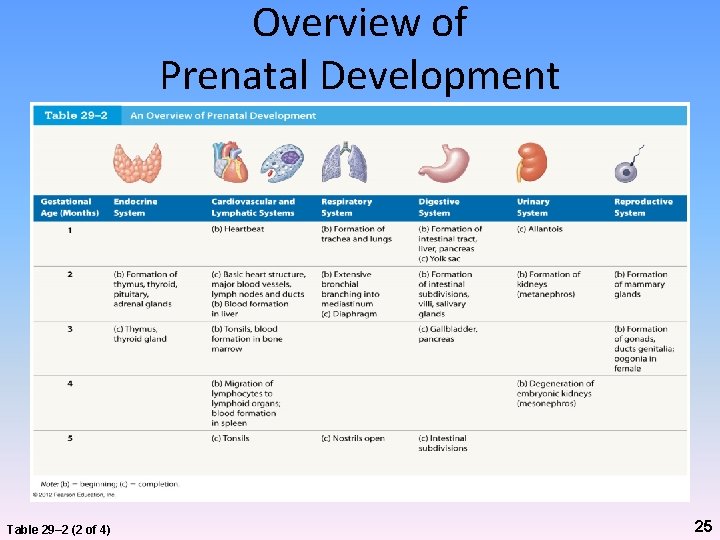
Overview of Prenatal Development Table 29– 2 (2 of 4) 25
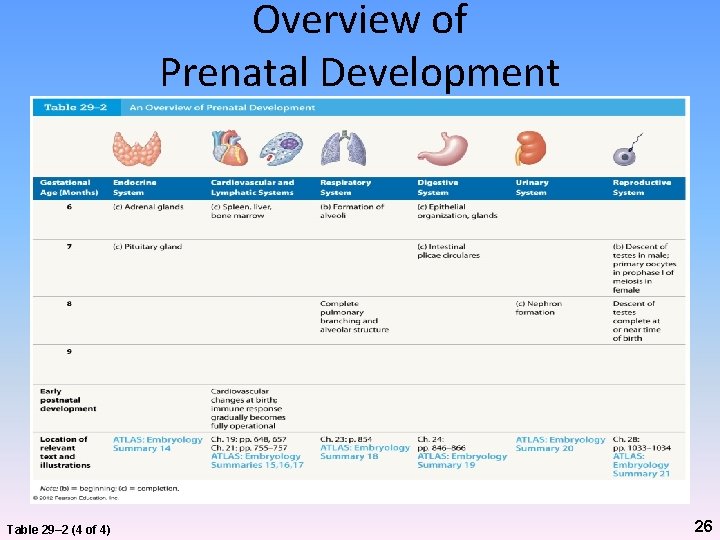
Overview of Prenatal Development Table 29– 2 (4 of 4) 26

Third Trimester Hormones • P (placental) – Until 3 rd trimester, “calms” myometrium so no contractions • E (placental) – Increases myometrial contractions – Sensitizes uterus to oxytocin (maternal and fetal) prostaglandins (PGs) initiate labor 27

Third Trimester Hormones • Human placental lactogen (h. PL) – Helps prepare mammary glands for milk production – Effects on other tissues comparable to GH • Prolactin (placental) – Helps convert mammary glands to active status • Relaxin (CL and placental) – Increased flexibility of pubic symphysis pelvis expands – Dilation of uterine cervix so fetus can enter vagina 28
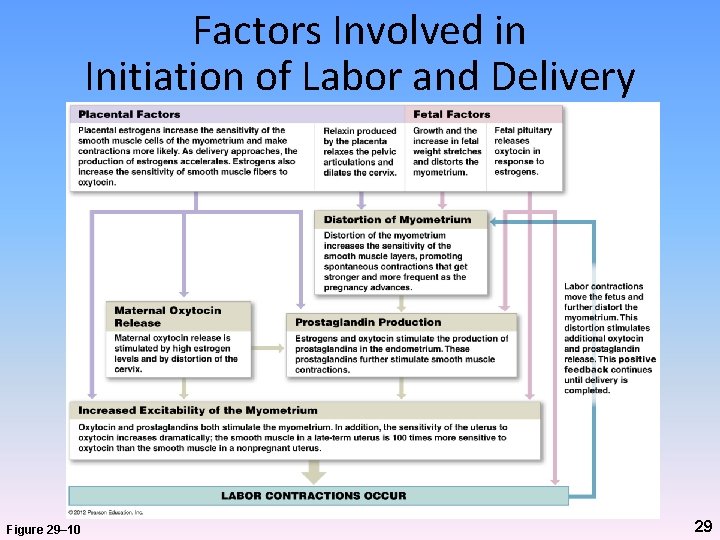
Factors Involved in Initiation of Labor and Delivery Figure 29– 10 29

Labor • False – Occasional spasms in uterine musculature – Contractions not regular or persistent • True – Results from biochemical and mechanical factors – Continues due to positive feedback • Premature – When labor begins before fetal development complete; survival related to BW 30

Labor and Delivery • Goal: parturition = forcible expulsion of fetus • Stages of labor – Dilation – Explusion – Placental 31

Labor and Delivery • Dilation stage – Begins with onset of true labor – Cervix dilates – Fetus moves toward cervical canal – Frequency of contractions increases – Amniochorionic membrane ruptures (“water breaks”) 32
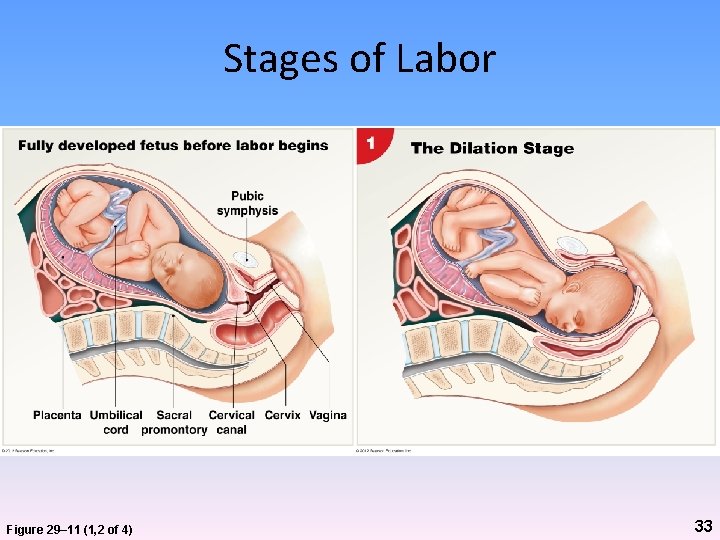
Stages of Labor Figure 29– 11 (1, 2 of 4) 33

Labor and Delivery • Expulsion stage – Cervix completely dilated – Maximum intensity of contractions – Continues until fetus emerges from vagina = delivery/birth 34

Labor and Delivery • Placental stage – Uterine contractions tear connection between endometrium and placenta – Placenta (afterbirth) ejected – Accompanied by loss of blood, usually tolerated without difficulty 35
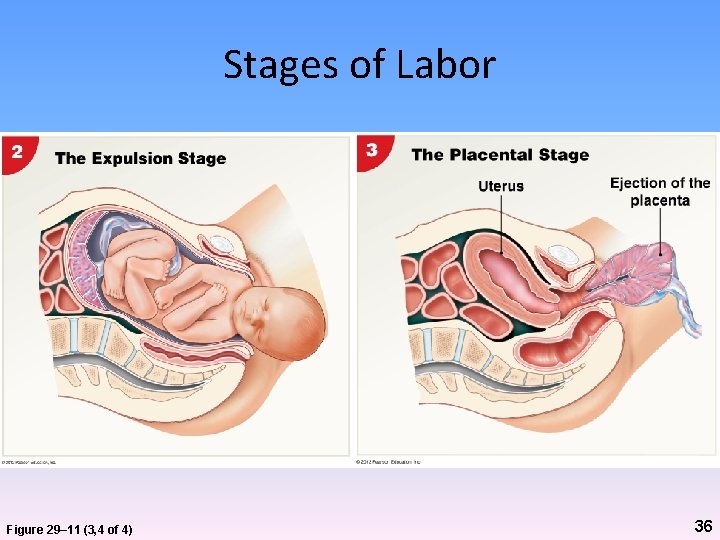
Stages of Labor Figure 29– 11 (3, 4 of 4) 36
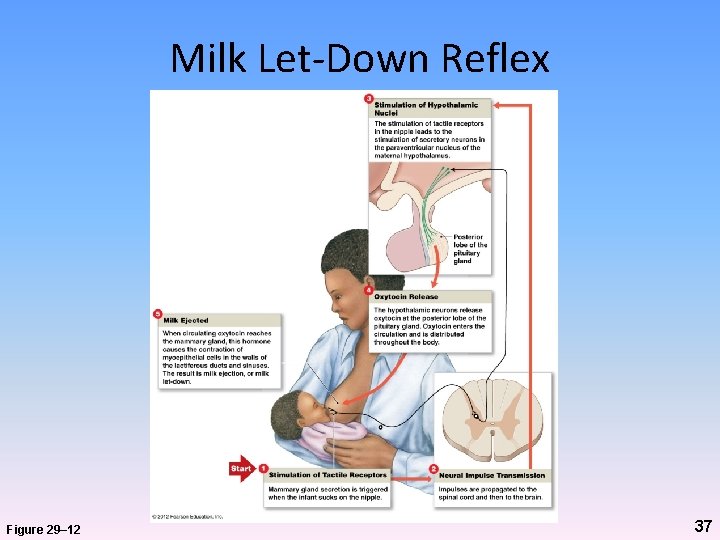
Milk Let-Down Reflex Figure 29– 12 37
- Slides: 37