Chapter 26 The Urinary System General n Kidney

















- Slides: 46

Chapter 26 The Urinary System

General n Kidney functions ¡ ¡ ¡ Blood ionic composition - Na+, Cl-, sulfate (SO 42 -), phosphate (PO 42 -) Blood p. H – physical removal of H+ Blood volume – fluid volume regulation Blood pressure - renin Blood osmolarity – ions and fluid levels Hormone production n n ¡ ¡ Calcitrol Erythropoietin Blood glucose levels - gluconeogenesis Waste removal n n Ammonia and urea from deamination Bilirubin from hgb Creatinine Uric acid

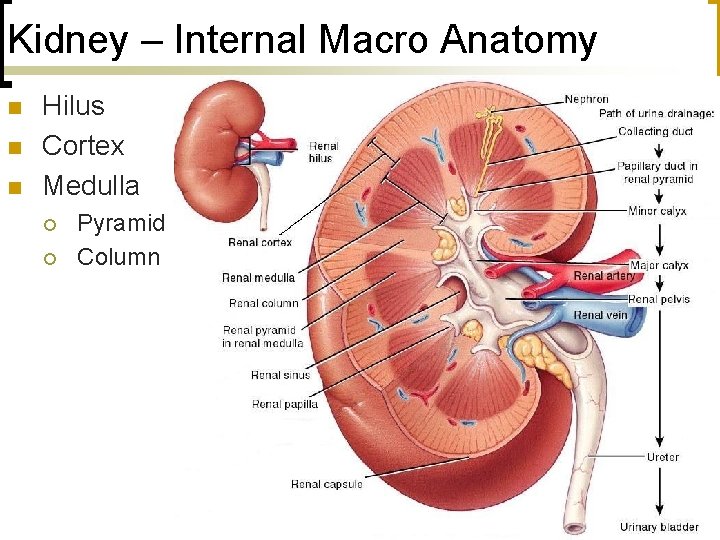
Kidney – Internal Macro Anatomy n n n Hilus Cortex Medulla ¡ ¡ Pyramid Column

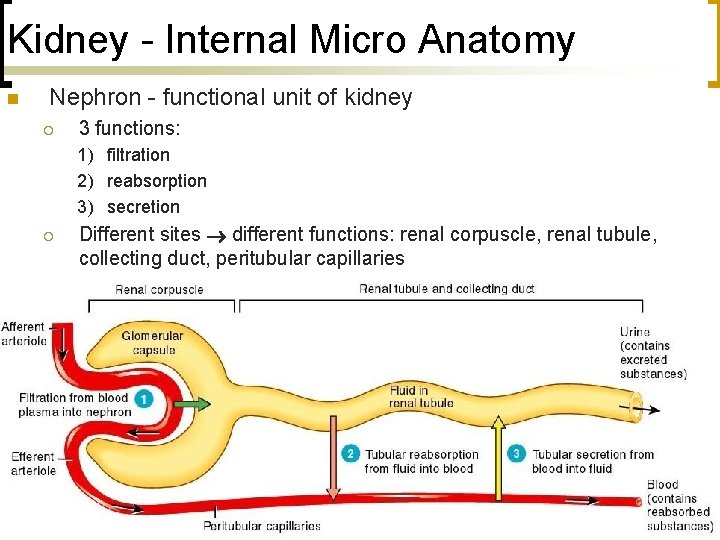
Kidney - Internal Micro Anatomy n Nephron - functional unit of kidney ¡ 3 functions: 1) filtration 2) reabsorption 3) secretion ¡ Different sites different functions: renal corpuscle, renal tubule, collecting duct, peritubular capillaries

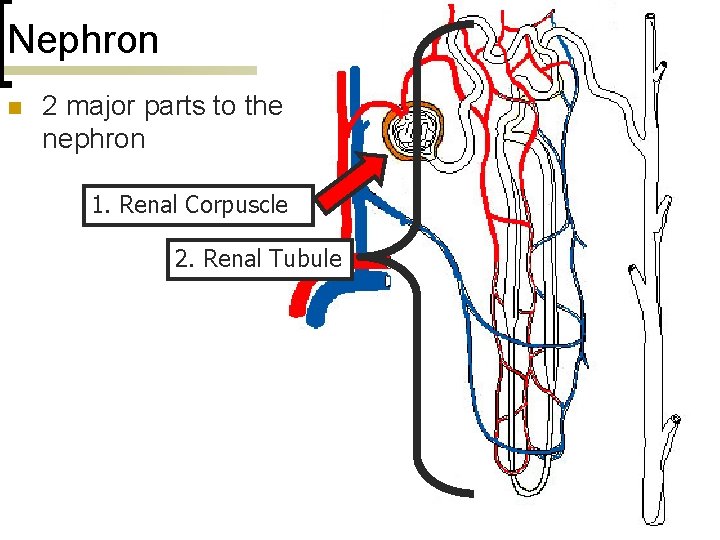
Nephron n 2 major parts to the nephron 1. Renal Corpuscle 2. Renal Tubule

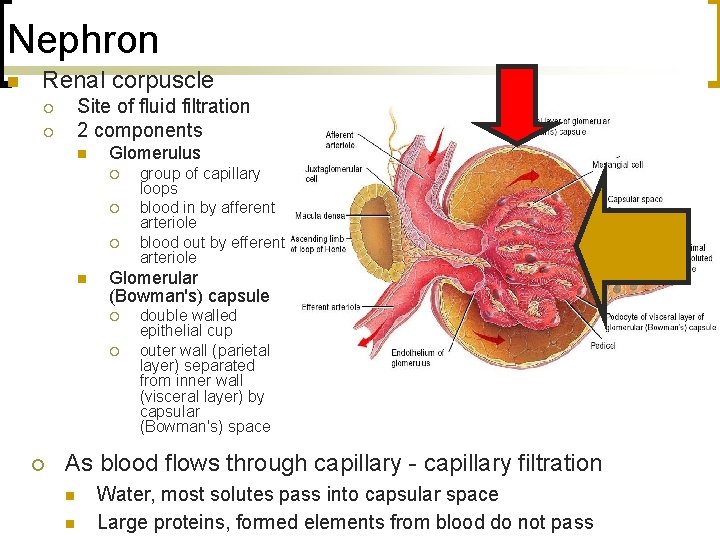
Nephron n Renal corpuscle Site of fluid filtration 2 components ¡ ¡ n Glomerulus ¡ ¡ ¡ n Glomerular (Bowman's) capsule ¡ ¡ ¡ group of capillary loops blood in by afferent arteriole blood out by efferent arteriole double walled epithelial cup outer wall (parietal layer) separated from inner wall (visceral layer) by capsular (Bowman's) space As blood flows through capillary - capillary filtration n n Water, most solutes pass into capsular space Large proteins, formed elements from blood do not pass

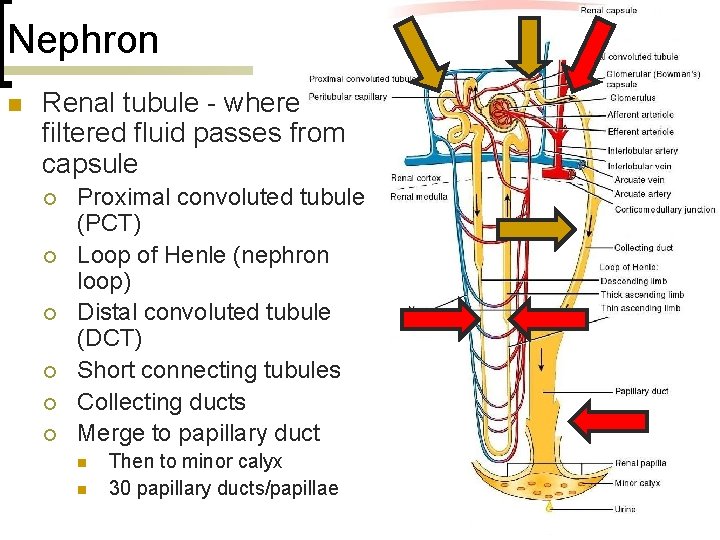
Nephron n Renal tubule - where filtered fluid passes from capsule ¡ ¡ ¡ Proximal convoluted tubule (PCT) Loop of Henle (nephron loop) Distal convoluted tubule (DCT) Short connecting tubules Collecting ducts Merge to papillary duct n n Then to minor calyx 30 papillary ducts/papillae

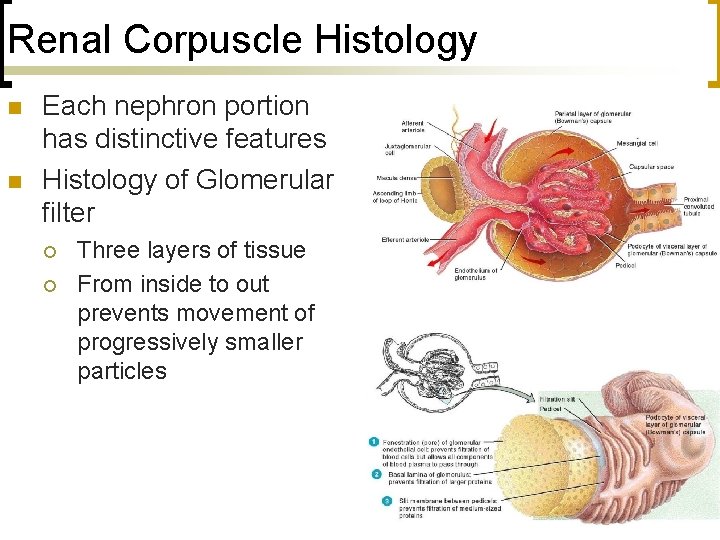
Renal Corpuscle Histology n n Each nephron portion has distinctive features Histology of Glomerular filter ¡ ¡ Three layers of tissue From inside to out prevents movement of progressively smaller particles

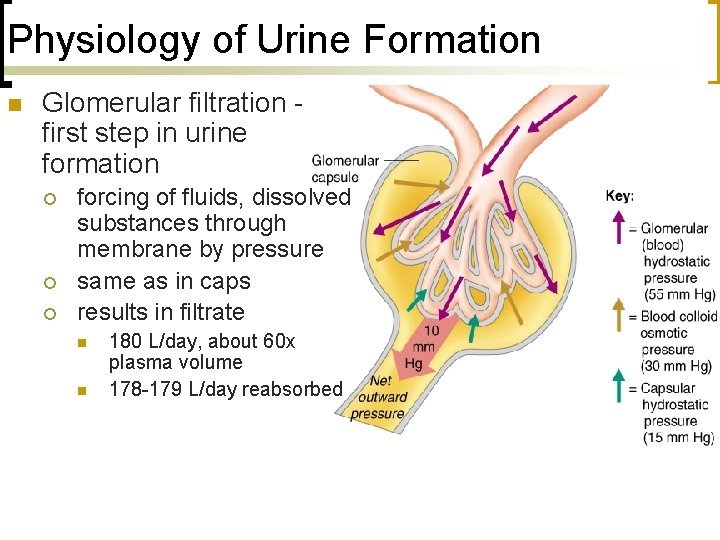
Physiology of Urine Formation n Glomerular filtration first step in urine formation ¡ ¡ ¡ forcing of fluids, dissolved substances through membrane by pressure same as in caps results in filtrate n n 180 L/day, about 60 x plasma volume 178 -179 L/day reabsorbed

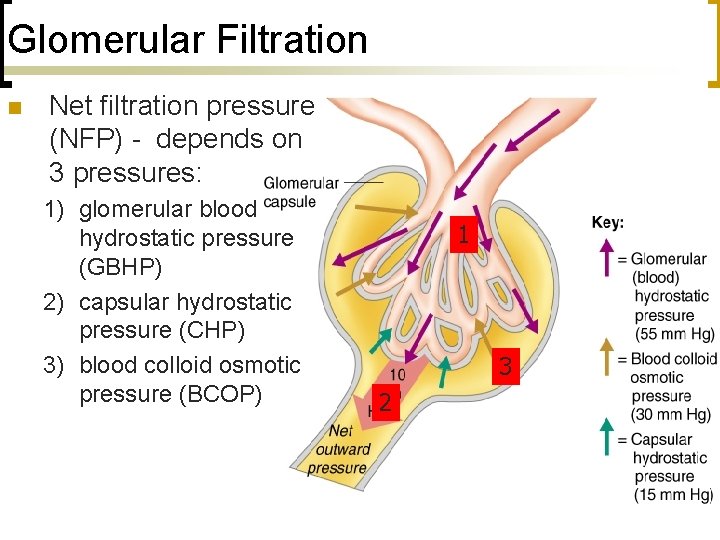
Glomerular Filtration n Net filtration pressure (NFP) - depends on 3 pressures: 1) glomerular blood hydrostatic pressure (GBHP) 2) capsular hydrostatic pressure (CHP) 3) blood colloid osmotic pressure (BCOP) 1 3 2

Glomerular Filtration n 3 structural features of renal corpuscles enhance filtering capacity: 1) Glomerular caps very long - surface area for filtration 2) Filter (endothelium-capsular membrane) is porous, thin Ø Ø glomerular caps 50 x more permeable than regular cap basement membrane, filtration slits only permit passage of small molecules 3) Cap BP high - efferent arteriole < diameter afferent art - filtration pressure

Glomerular Filtration Rate (GFR) n GFR ¡ ¡ n Amount of filtrate that forms in all renal corpuscles in both kidneys/min Adults GFR 125 ml/min (180 L/day) Regulation of GFR ¡ ¡ ¡ When more blood flows into glomerulus GFR Glomerular blood flow (GBF) depends on systemic blood pressure, diameter of afferent/efferent arterioles If BP falls to where glomerular capillary pressure is 42 mm. Hg, no filtration, anuria

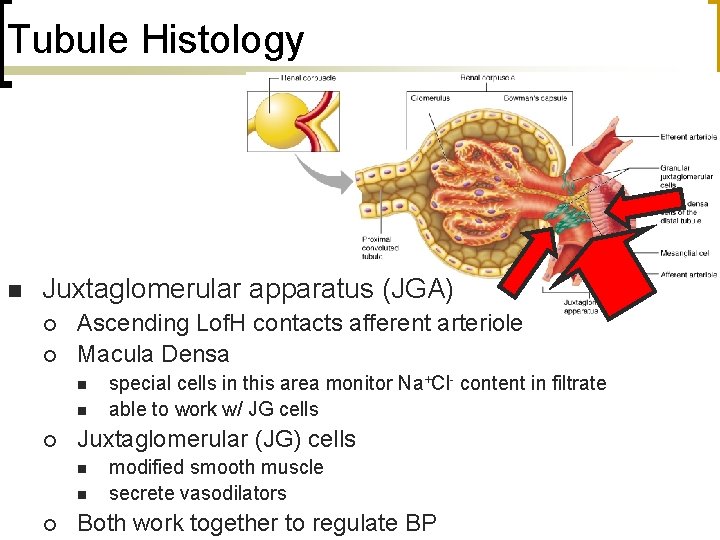
Tubule Histology n Juxtaglomerular apparatus (JGA) ¡ ¡ Ascending Lof. H contacts afferent arteriole Macula Densa n n ¡ Juxtaglomerular (JG) cells n n ¡ special cells in this area monitor Na+Cl- content in filtrate able to work w/ JG cells modified smooth muscle secrete vasodilators Both work together to regulate BP

Glomerular Filtration Rate (GFR) n 3 principal regulators of GFR: 1) Renal autoregulation of GFR n n n ability of kidneys to maintain a constant BP and GFR despite changes in systemic AP high bp causes afferent arteriole to constrict – keeps GBF constant negative feedback from JGA – high delivery of filtered Na+ and Cl- to macula densa causes constriction of afferent arteriole (decrease release of vasodilators)

Glomerular Filtration Rate (GFR) n 3 principal regulators of GFR (cont. ): 2) Hormonal regulation of GFR 1. Angiotensin II ¡ ¡ catalyzed from angiotensinogen by renin released from JGA cells 4 important functions n vasoconstriction (of afferent arteriole) n aldosterone n thirst n ADH n Na+ reabsorption 2. ANP ¡ ¡ ¡ secreted by cells in atria of heart in response to stretch GFR by “relaxing” glomerular cap, promotes excretion of H 2 O, Na+ suppresses ADH, aldosterone, renin

Glomerular Filtration Rate (GFR) n 3 principal regulators of GFR (cont. ): 3) Neural regulation n n vessels of kidney supplied by vasoconstrictor fibers from SNS, with strong stim afferent constricts more than efferent strong SNS stim causes JGA cells to secrete renin and adrenal medulla to secrete Epi

Tubular Reabsorption n Movement of water, solutes back into tubule ¡ Filter 180 L/day of fluid and solutes n n n ¡ n n filtering is non-specific much of this (Na+, K+, Glucose, etc. ) needed by body must get them back into blood about 99% of filtrate reabsorbed in tubule Epithelial cells in PCT surface area (microvilli) for reabsorption – most (65%) reabsorption occurs in PCT DCT and collecting ducts fine tune reabsorption

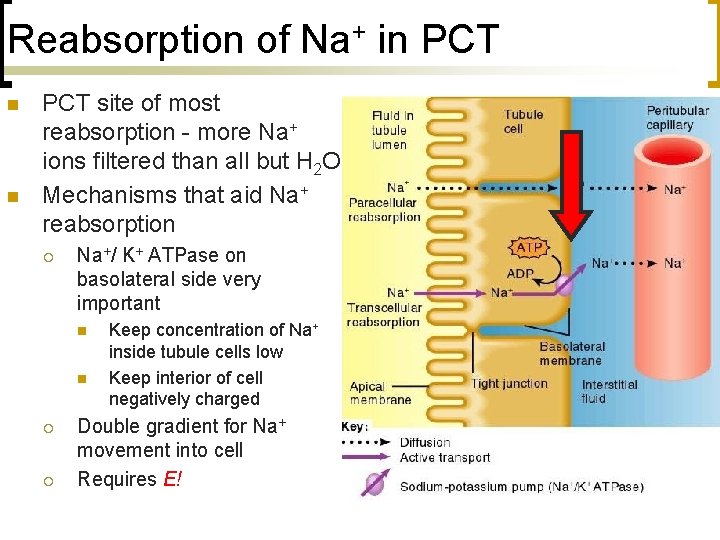
Reabsorption of Na+ in PCT n n PCT site of most reabsorption - more Na+ ions filtered than all but H 2 O Mechanisms that aid Na+ reabsorption ¡ Na+/ K+ ATPase on basolateral side very important n n ¡ ¡ Keep concentration of Na+ inside tubule cells low Keep interior of cell negatively charged Double gradient for Na+ movement into cell Requires E!

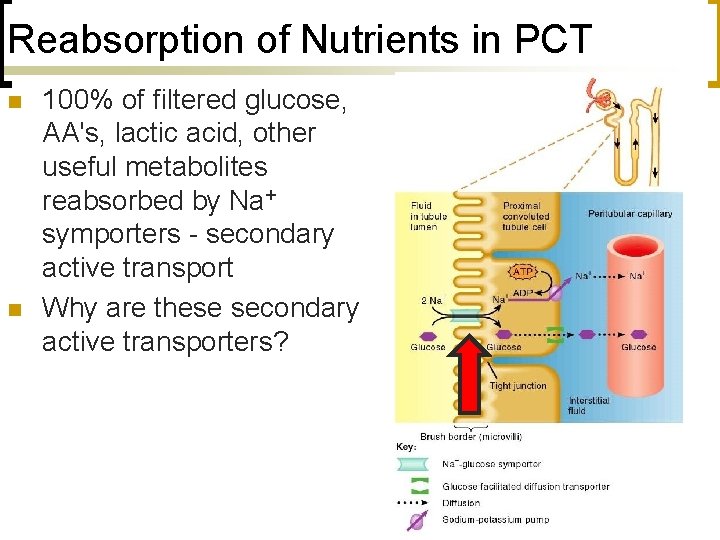
Reabsorption of Nutrients in PCT n n 100% of filtered glucose, AA's, lactic acid, other useful metabolites reabsorbed by Na+ symporters - secondary active transport Why are these secondary active transporters?

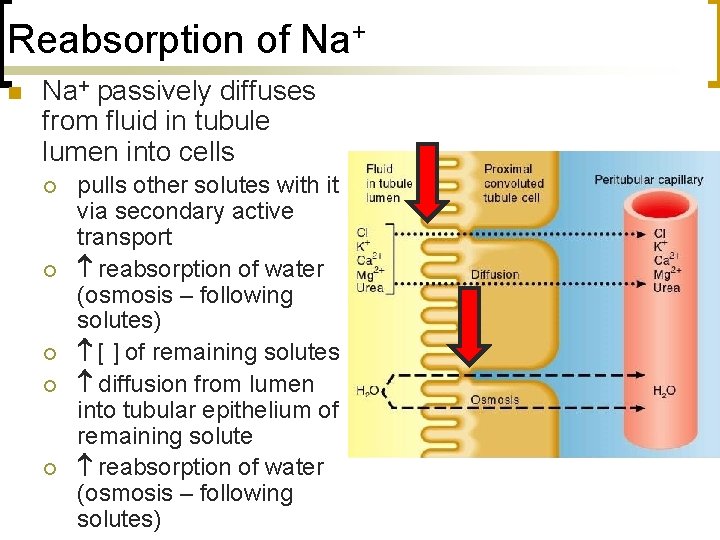
Reabsorption of Na+ n Na+ passively diffuses from fluid in tubule lumen into cells ¡ ¡ ¡ pulls other solutes with it via secondary active transport reabsorption of water (osmosis – following solutes) [ ] of remaining solutes diffusion from lumen into tubular epithelium of remaining solute reabsorption of water (osmosis – following solutes)

Reabsorption of Nutrients n Transport maximum (Tm) ¡ each type of symporter has upper limit on how fast it can work n n ¡ n work is transport of solutes upper limit is max concentration that can still be transported out of tubule, reabsorbed anything above max is lost in the urine Renal threshold ¡ ¡ ¡ plasma concentration at which a substance begins to spill into urine because Tm has been surpassed renal tubule concentration too high, all cannot be reabsorbed by transporters glucose and diabetics

Reabsorption in the PCT n By the end of the PCT the following reabsorption has occurred: ¡ ¡ 100% of filtered nutrients 80 -90% of filtered HCO 365% of Na+ and water, 50% of Cl- and K+

Reabsorption in Loop of Henle n n Cells in thin descending limb only permeable to water No solute movement out of thin descending limb

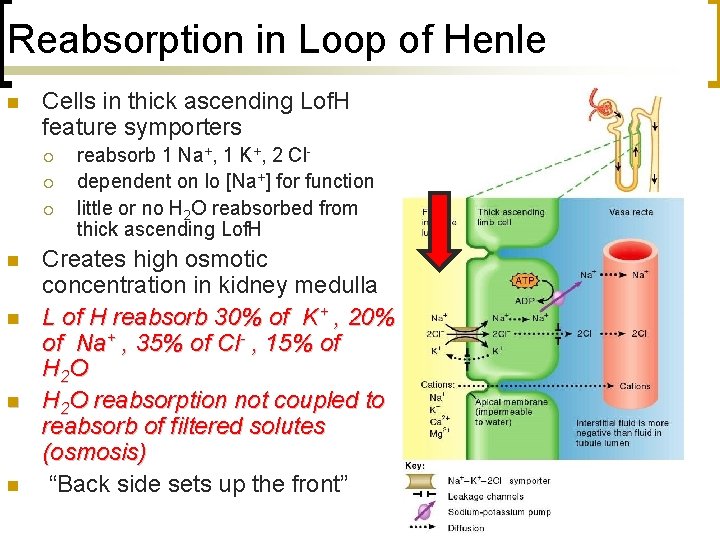
Reabsorption in Loop of Henle n Cells in thick ascending Lof. H feature symporters ¡ ¡ ¡ n n reabsorb 1 Na+, 1 K+, 2 Cldependent on lo [Na+] for function little or no H 2 O reabsorbed from thick ascending Lof. H Creates high osmotic concentration in kidney medulla L of H reabsorb 30% of K+ , 20% of Na+ , 35% of Cl- , 15% of H 2 O reabsorption not coupled to reabsorb of filtered solutes (osmosis) “Back side sets up the front”

Reabsorption in DCT, Collecting Duct n n Filtrate reaching DCT has 80% filtered solutes, H 2 O reabsorbed DCT ¡ ¡ ¡ Na+/ Cl- symporter Ca++ reabsorbed here due to PTH reabsorbs another 10 -15% of filtrate

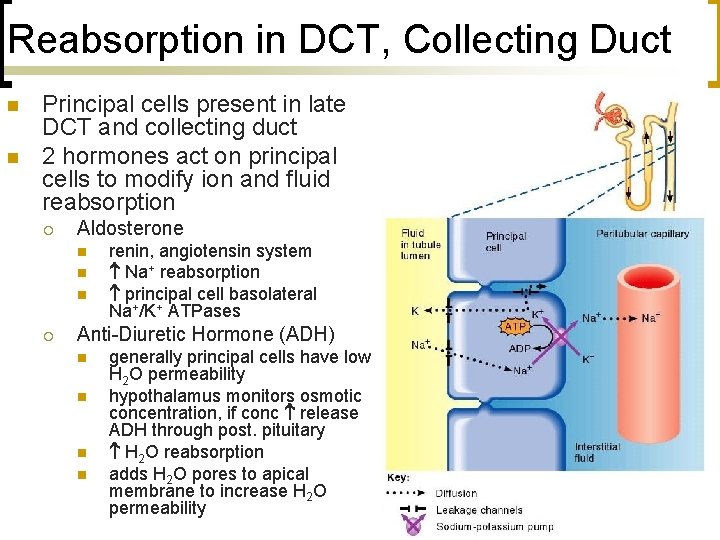
Reabsorption in DCT, Collecting Duct n n Principal cells present in late DCT and collecting duct 2 hormones act on principal cells to modify ion and fluid reabsorption ¡ Aldosterone n n n ¡ renin, angiotensin system Na+ reabsorption principal cell basolateral Na+/K+ ATPases Anti-Diuretic Hormone (ADH) n n generally principal cells have low H 2 O permeability hypothalamus monitors osmotic concentration, if conc release ADH through post. pituitary H 2 O reabsorption adds H 2 O pores to apical membrane to increase H 2 O permeability

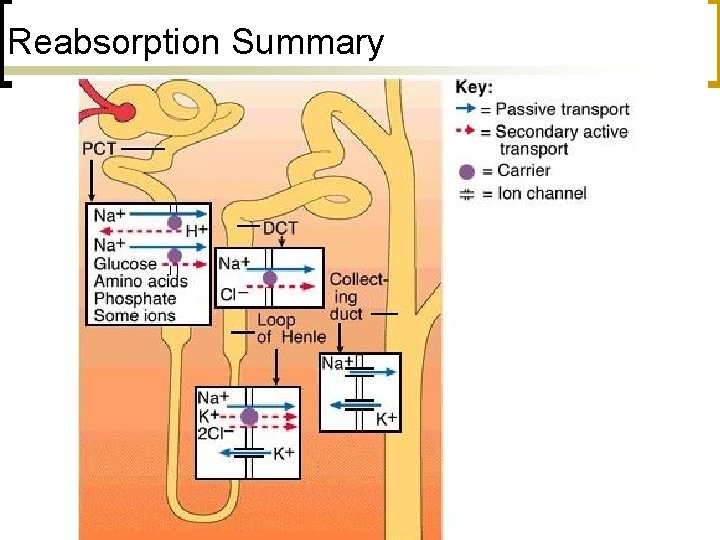
Reabsorption Summary

Tubular Secretion n n Removes substances from blood, add to filtrate - includes K+, ammonium (NH 4+), creatinine, penicillin Two primary functions ¡ ¡ Helps rid body of substances, generally waste products Regulate blood p. H by secretion of H+

Secretion of K+ n Principal cells in collecting ducts secrete variable amount of K+ due to leaky channels in apical membrane+ (opposite of Na+ reabsorption) ¡ ¡ Na+/K+ ATPases in basolateral membrane Controlled by: n n n Aldosterone - aldo, K+ secretion K+ concentration in plasma - levels, secretion Na+ levels in DCT - high levels Na+, Na+ reabsorption, K+ secretion

Secretion of H+ n Cells of renal tubule can blood p. H 3 ways ¡ ¡ ¡ Secrete H+ into filtrate Reabsorb filtered HCO 3 Produce more HCO 3 -

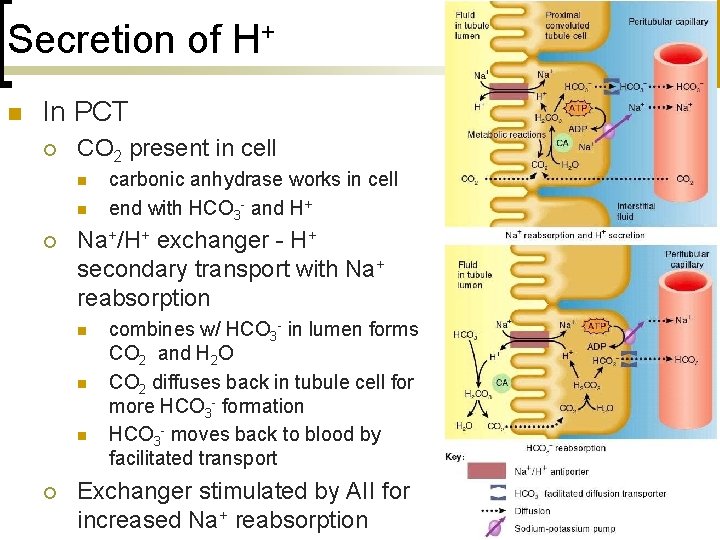
Secretion of H+ n In PCT ¡ CO 2 present in cell n n ¡ Na+/H+ exchanger - H+ secondary transport with Na+ reabsorption n ¡ carbonic anhydrase works in cell end with HCO 3 - and H+ combines w/ HCO 3 - in lumen forms CO 2 and H 2 O CO 2 diffuses back in tubule cell for more HCO 3 - formation HCO 3 - moves back to blood by facilitated transport Exchanger stimulated by AII for increased Na+ reabsorption

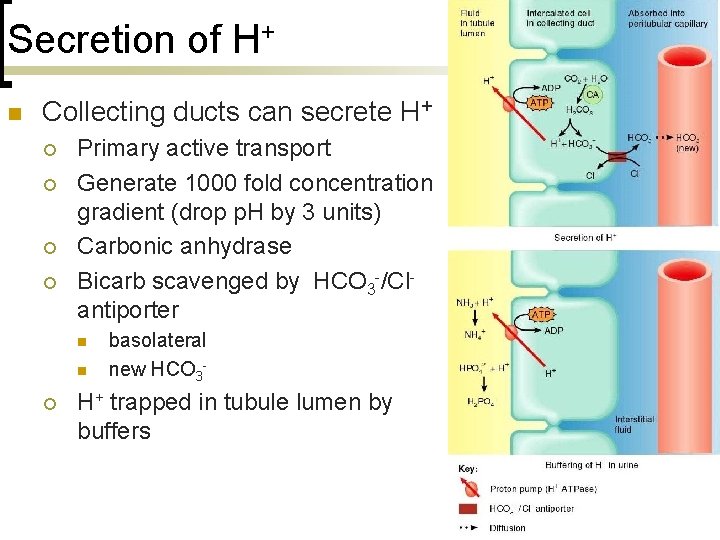
Secretion of H+ n Collecting ducts can secrete H+ ¡ ¡ Primary active transport Generate 1000 fold concentration gradient (drop p. H by 3 units) Carbonic anhydrase Bicarb scavenged by HCO 3 -/Clantiporter n n ¡ basolateral new HCO 3 - H+ trapped in tubule lumen by buffers

Secretion of NH 3 and NH 4+ n n n Ammonia (NH 3) poisonous waste picked up from deamination, generally converted to urea, much less toxic Can be used as a buffer for H+ to form NH 4+ (ammonium) PCT cells can deaminate and secrete NH 4+ in a Na+/NH 4+ antiporter when blood p. H lo

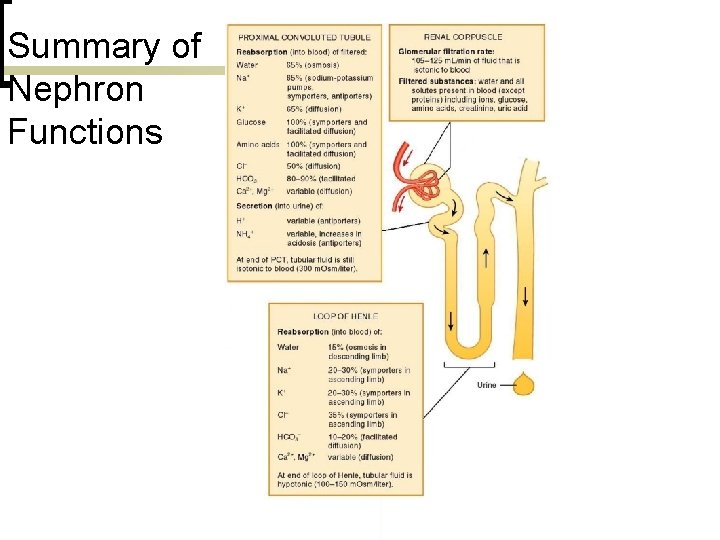
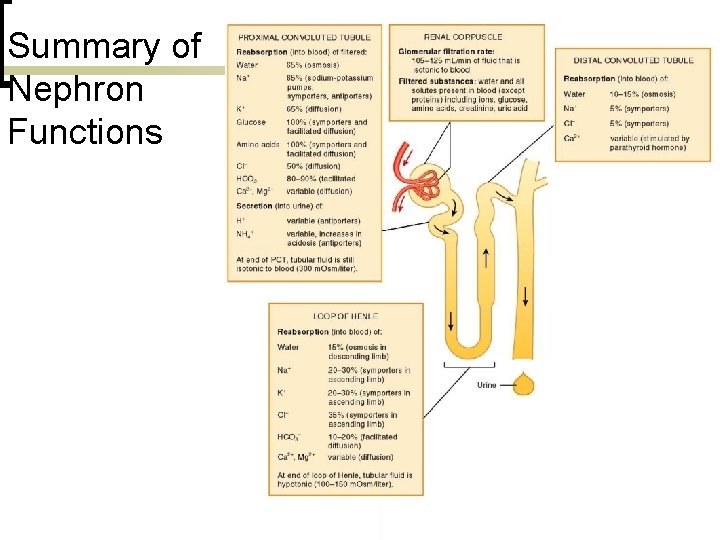
Summary of Nephron Functions

Summary of Nephron Functions

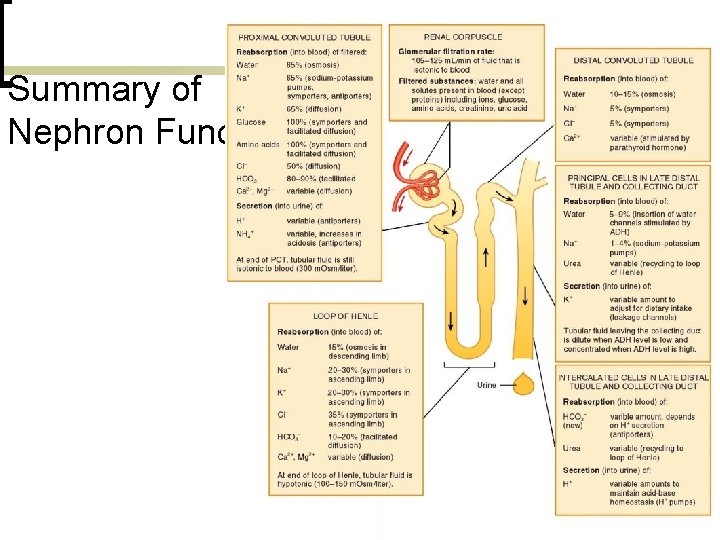
Summary of Nephron Functions

Summary of Nephron Functions

Summary of Nephron Functions

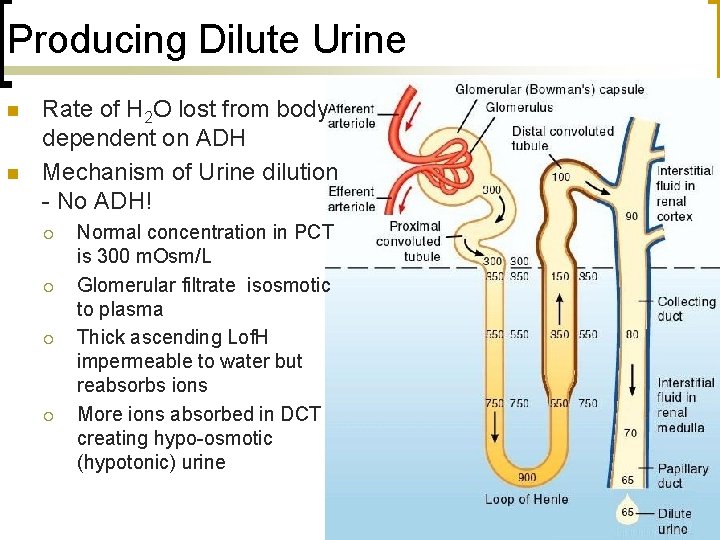
Producing Dilute Urine n n Rate of H 2 O lost from body dependent on ADH Mechanism of Urine dilution - No ADH! ¡ ¡ Normal concentration in PCT is 300 m. Osm/L Glomerular filtrate isosmotic to plasma Thick ascending Lof. H impermeable to water but reabsorbs ions More ions absorbed in DCT creating hypo-osmotic (hypotonic) urine

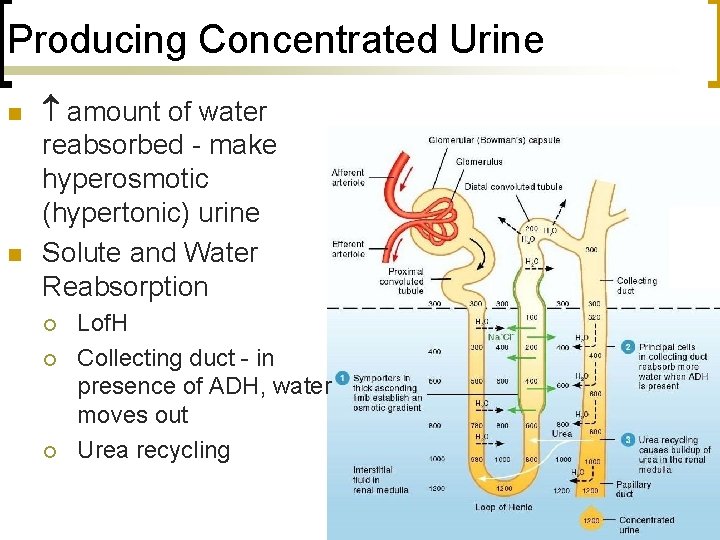
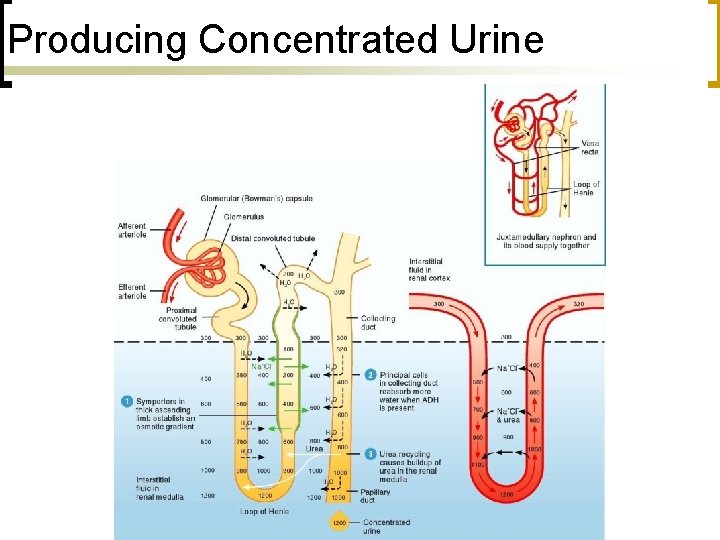
Producing Concentrated Urine n n amount of water reabsorbed - make hyperosmotic (hypertonic) urine Solute and Water Reabsorption ¡ ¡ ¡ Lof. H Collecting duct - in presence of ADH, water moves out Urea recycling

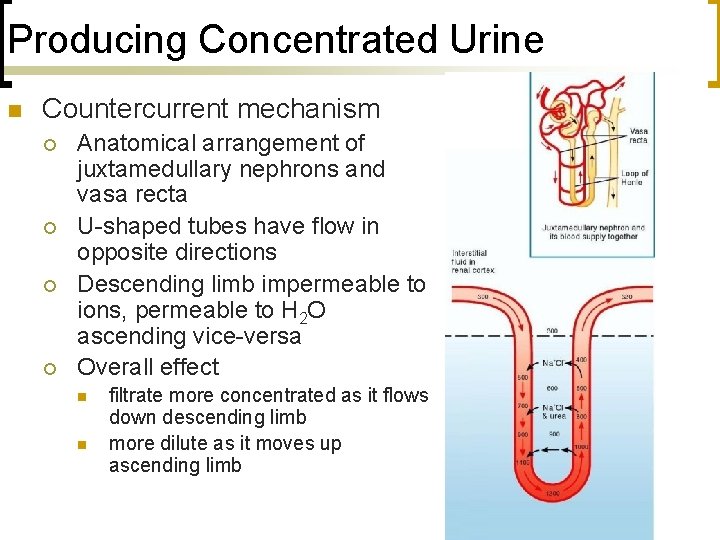
Producing Concentrated Urine n Countercurrent mechanism ¡ ¡ Anatomical arrangement of juxtamedullary nephrons and vasa recta U-shaped tubes have flow in opposite directions Descending limb impermeable to ions, permeable to H 2 O ascending vice-versa Overall effect n n filtrate more concentrated as it flows down descending limb more dilute as it moves up ascending limb

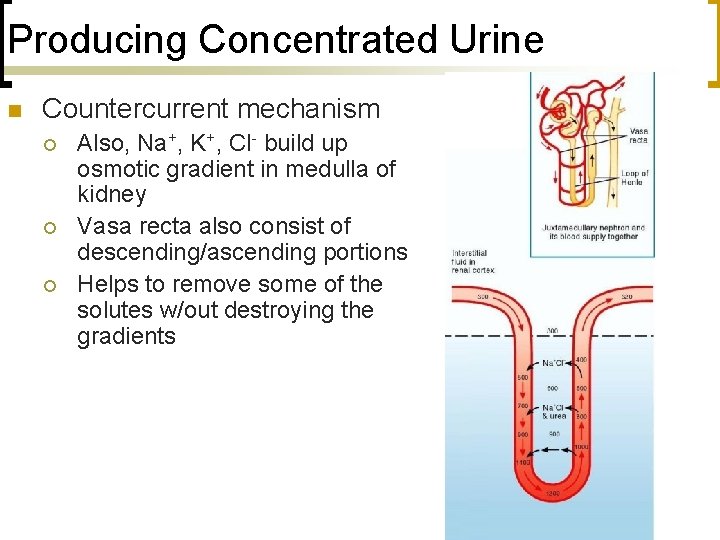
Producing Concentrated Urine n Countercurrent mechanism ¡ ¡ ¡ Also, Na+, K+, Cl- build up osmotic gradient in medulla of kidney Vasa recta also consist of descending/ascending portions Helps to remove some of the solutes w/out destroying the gradients

Producing Concentrated Urine

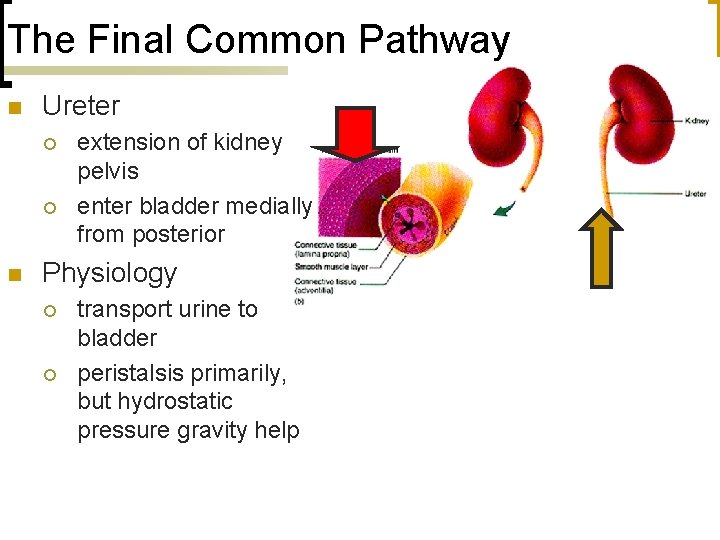
The Final Common Pathway n Ureter ¡ ¡ n extension of kidney pelvis enter bladder medially from posterior Physiology ¡ ¡ transport urine to bladder peristalsis primarily, but hydrostatic pressure gravity help

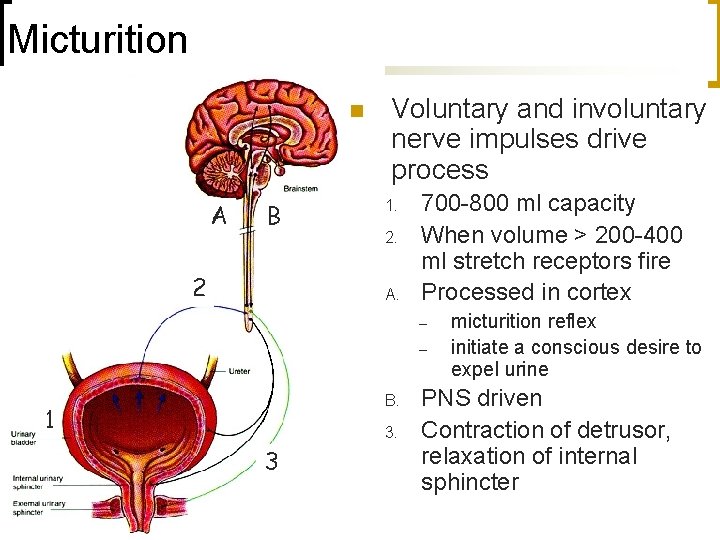
Micturition n A B 2 Voluntary and involuntary nerve impulses drive process 1. 2. A. 700 -800 ml capacity When volume > 200 -400 ml stretch receptors fire Processed in cortex – – B. 1 3. 3 micturition reflex initiate a conscious desire to expel urine PNS driven Contraction of detrusor, relaxation of internal sphincter

The Final Common Pathway n Urethra ¡ n Physiology - terminal portion of urinary tract, in males also serves as duct through which semen is discharged from the body Urine ¡ Volume n n ¡ 1000 -2000 ml/day influenced by blood pressure, blood osmotic pressure, diet, temperature, diuretics, mental state, general health Chemical Composition - 95% water, 5% solutes