Chapter 24 Microbial Diseases of the Respiratory System

Chapter 24 Microbial Diseases of the Respiratory System © 2013 Pearson Education, Inc. Copyright © 2013 Pearson Education, Inc. Lectures prepared by Christine L. Case Lectures prepared by Christine L.
© 2013 Pearson Education, Inc.
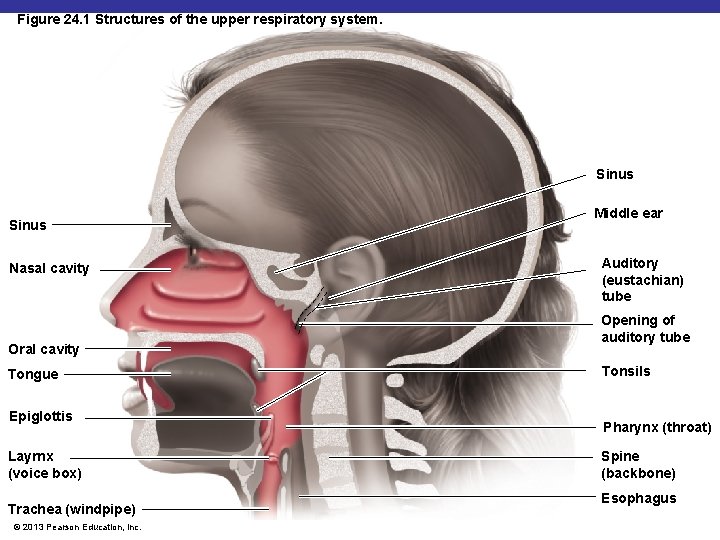
Figure 24. 1 Structures of the upper respiratory system. Sinus Nasal cavity Oral cavity Tongue Epiglottis Layrnx (voice box) Trachea (windpipe) © 2013 Pearson Education, Inc. Middle ear Auditory (eustachian) tube Opening of auditory tube Tonsils Pharynx (throat) Spine (backbone) Esophagus
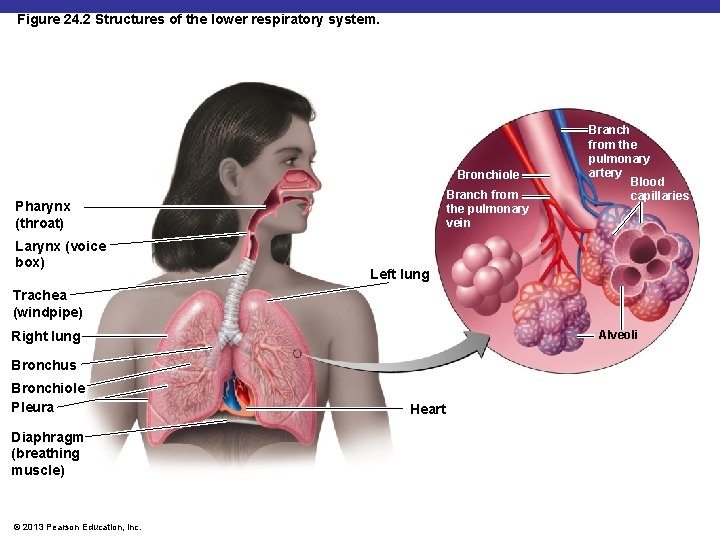
Figure 24. 2 Structures of the lower respiratory system. Bronchiole Branch from the pulmonary vein Pharynx (throat) Larynx (voice box) Branch from the pulmonary artery Blood capillaries Left lung Trachea (windpipe) Right lung Alveoli Bronchus Bronchiole Pleura Diaphragm (breathing muscle) © 2013 Pearson Education, Inc. Heart

Normal Microbiota of the Respiratory System § Suppress pathogens by competitive inhibition in upper respiratory system § Lower respiratory system is sterile © 2013 Pearson Education, Inc.

Upper Respiratory System Diseases § § § Pharyngitis Laryngitis Tonsillitis Sinusitis Epiglottitis: H. influenzae type b © 2013 Pearson Education, Inc.

Streptococcal Pharyngitis § § § § Also called strep throat Streptococcus pyogenes Resistant to phagocytosis Streptokinases lyse clots Streptolysins are cytotoxic Diagnosis by enzyme immunoassay (EIA) tests Scarlet fever § Erythrogenic toxin produced by lysogenized S. pyogenes © 2013 Pearson Education, Inc.
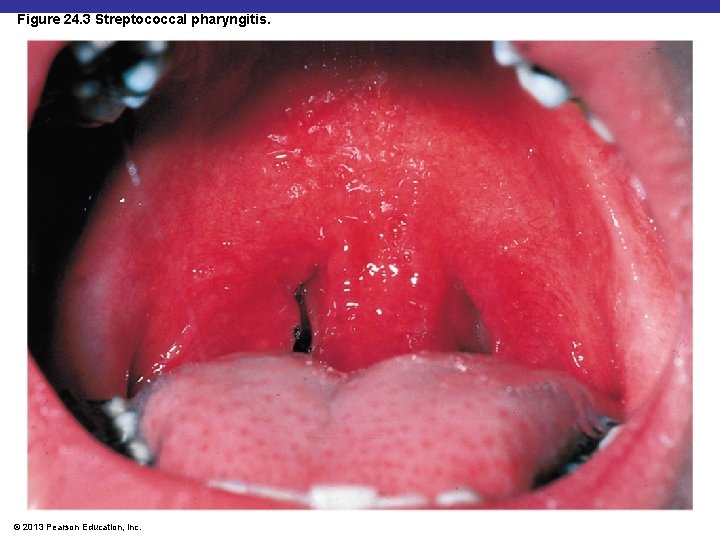
Figure 24. 3 Streptococcal pharyngitis. © 2013 Pearson Education, Inc.
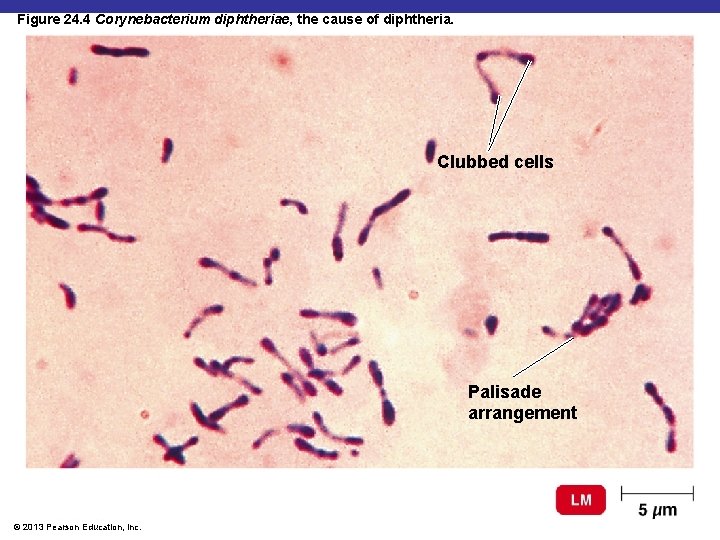
Figure 24. 4 Corynebacterium diphtheriae, the cause of diphtheria. Clubbed cells Palisade arrangement © 2013 Pearson Education, Inc.
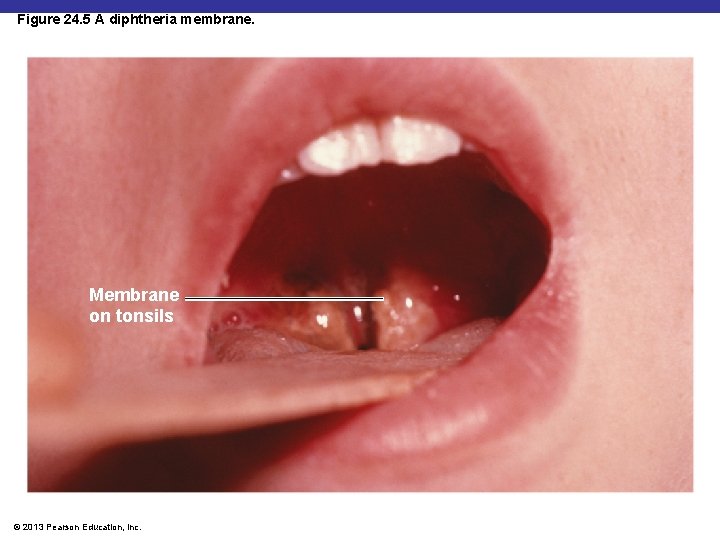
Figure 24. 5 A diphtheria membrane. Membrane on tonsils © 2013 Pearson Education, Inc.

Diphtheria § Corynebacterium diphtheriae: gram-positive rod § Diphtheria toxin produced by lysogenized C. diphtheriae § Prevented by DTa. P vaccine § Diphtheria toxoid § Cutaneous diphtheria § Infected skin wound leads to slow-healing ulcer © 2013 Pearson Education, Inc.

Otitis Media § § § S. pneumoniae (35%) H. influenzae (20– 30%) M. catarrhalis (10– 15%) S. pyogenes (8– 10%) S. aureus (1– 2%) Incidence of S. pneumoniae reduced by vaccine © 2013 Pearson Education, Inc.
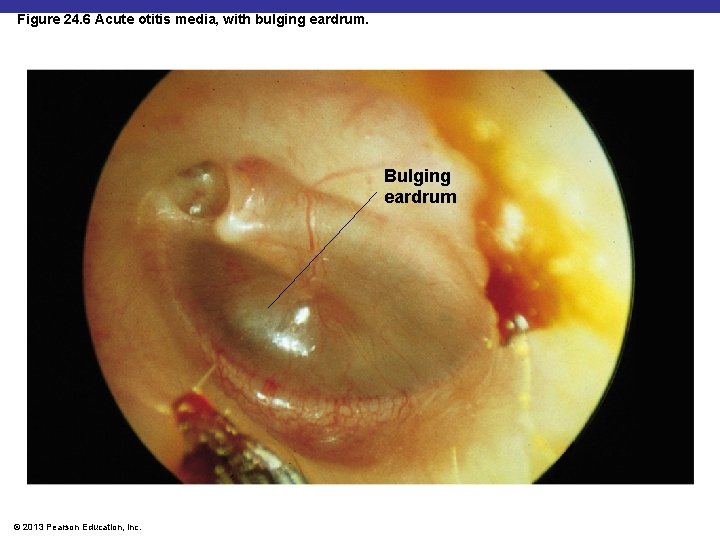
Figure 24. 6 Acute otitis media, with bulging eardrum. Bulging eardrum © 2013 Pearson Education, Inc.

The Common Cold § Rhinoviruses (30– 50%) § Coronaviruses (10– 15%) © 2013 Pearson Education, Inc.

Diseases in Focus: Diseases of the Upper Respiratory System § A patient presents with fever and a red, sore throat. Later, a grayish membrane appears in the throat. Gram-positive rods are cultured from the membrane. § Can you identify infections that could cause these symptoms? © 2013 Pearson Education, Inc.
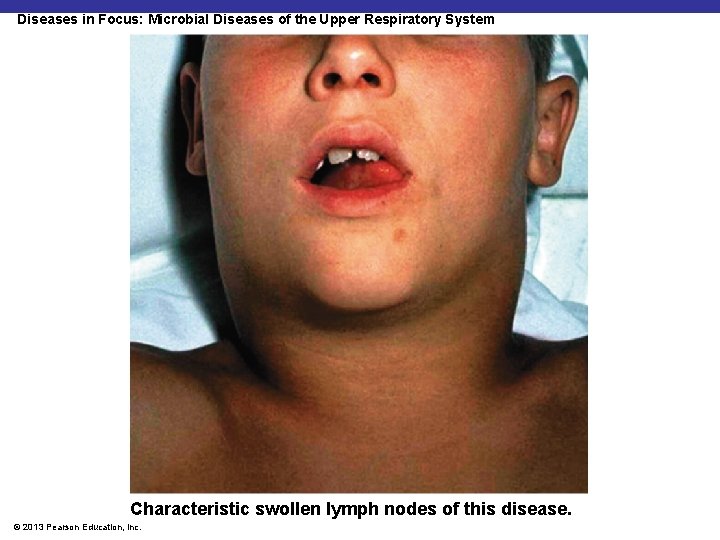
Diseases in Focus: Microbial Diseases of the Upper Respiratory System Characteristic swollen lymph nodes of this disease. © 2013 Pearson Education, Inc.

Lower Respiratory System Diseases § Bacteria, viruses, and fungi cause § Bronchitis § Bronchiolitis § Pneumonia © 2013 Pearson Education, Inc.

Pertussis (Whooping Cough) § Bordetella pertussis § Gram-negative coccobacillus § § Capsule Tracheal cytotoxin of cell wall damages ciliated cells Pertussis toxin Prevented by DTa. P vaccine (acellular Pertussis cell fragments) © 2013 Pearson Education, Inc.
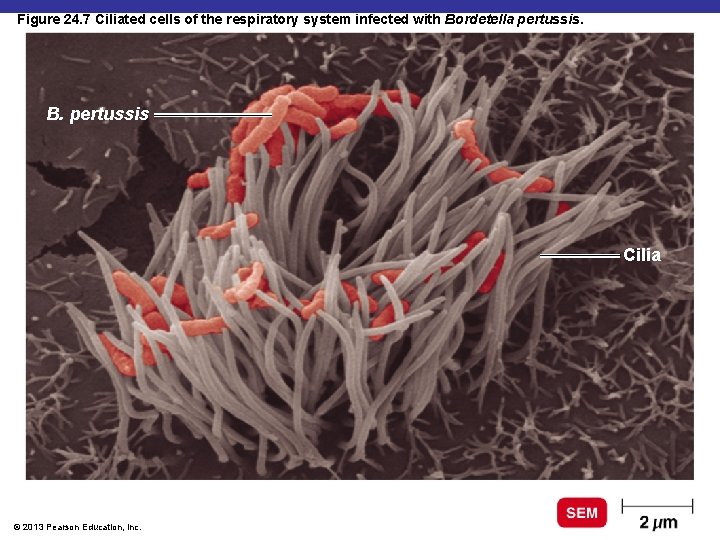
Figure 24. 7 Ciliated cells of the respiratory system infected with Bordetella pertussis. B. pertussis Cilia © 2013 Pearson Education, Inc.

Pertussis (Whooping Cough) § Stage 1: catarrhal stage, like common cold § Stage 2: paroxysmal stage—violent coughing sieges § Stage 3: convalescence stage © 2013 Pearson Education, Inc.
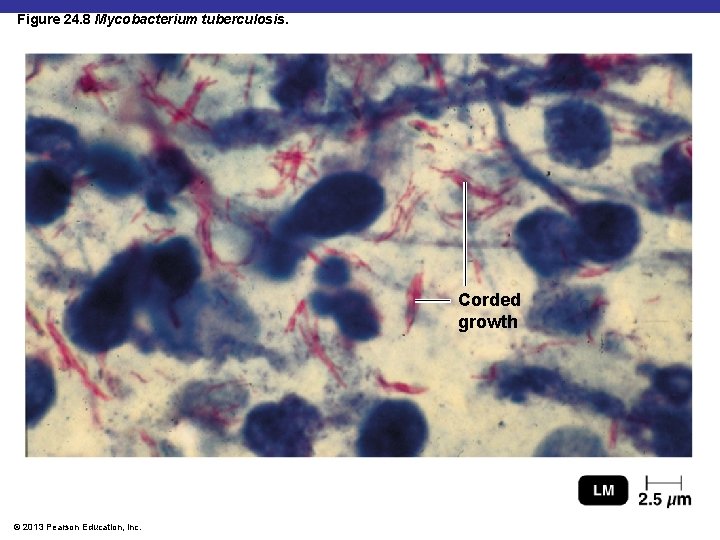
Figure 24. 8 Mycobacterium tuberculosis. Corded growth © 2013 Pearson Education, Inc.

Tuberculosis § Mycobacterium tuberculosis § Acid-fast rod; transmitted human-to-human § M. bovis: <1% of U. S. cases; not transmitted from human to human § M. avium-intracellulare complex infects people with late-stage HIV infection © 2013 Pearson Education, Inc.
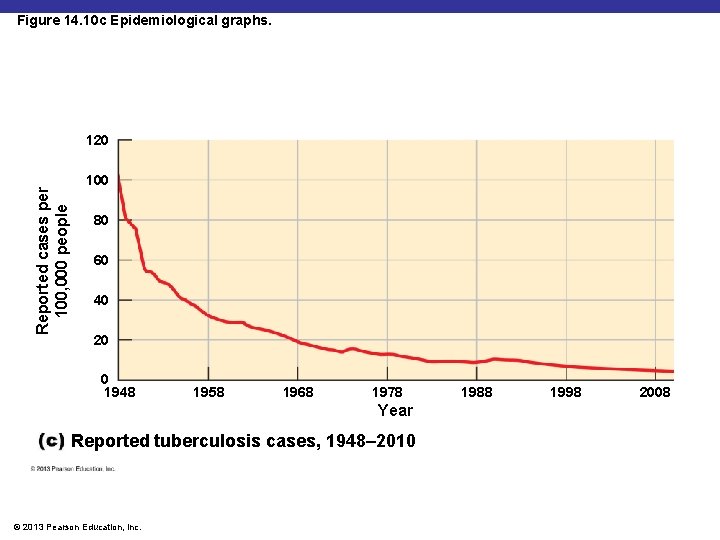
Figure 14. 10 c Epidemiological graphs. Reported cases per 100, 000 people 120 100 80 60 40 20 0 1948 1958 1968 1978 Year Reported tuberculosis cases, 1948– 2010 © 2013 Pearson Education, Inc. 1988 1998 2008
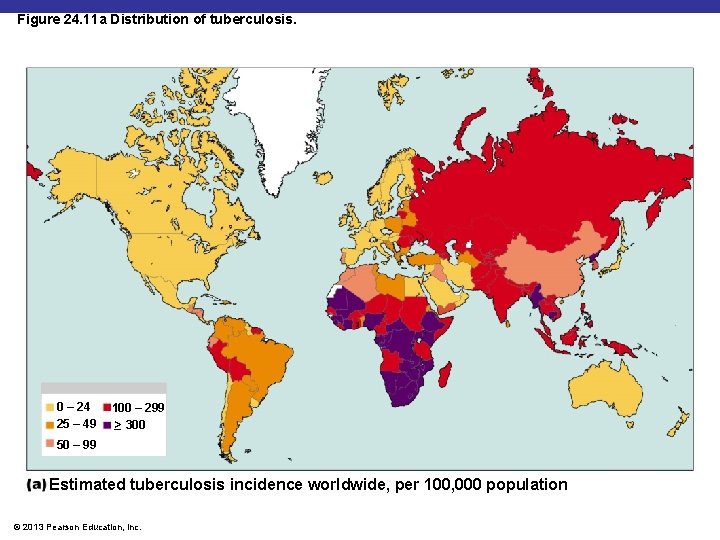
Figure 24. 11 a Distribution of tuberculosis. 0 – 24 25 – 49 100 – 299 _> 300 50 – 99 Estimated tuberculosis incidence worldwide, per 100, 000 population © 2013 Pearson Education, Inc.
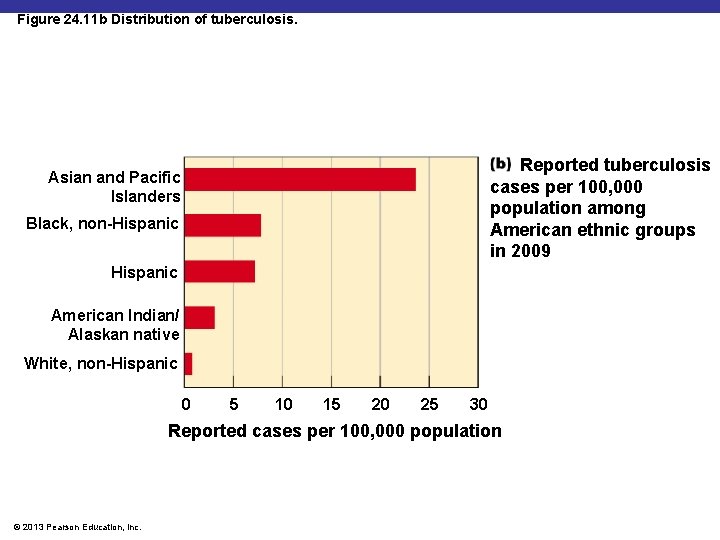
Figure 24. 11 b Distribution of tuberculosis. Reported tuberculosis cases per 100, 000 population among American ethnic groups in 2009 Asian and Pacific Islanders Black, non-Hispanic American Indian/ Alaskan native White, non-Hispanic 0 5 10 15 20 25 30 Reported cases per 100, 000 population © 2013 Pearson Education, Inc.
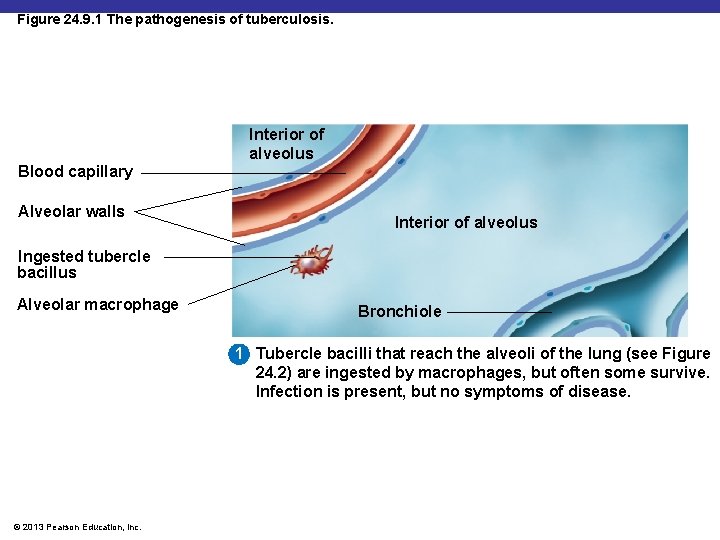
Figure 24. 9. 1 The pathogenesis of tuberculosis. Blood capillary Alveolar walls Interior of alveolus Ingested tubercle bacillus Alveolar macrophage Bronchiole 1 Tubercle bacilli that reach the alveoli of the lung (see Figure 24. 2) are ingested by macrophages, but often some survive. Infection is present, but no symptoms of disease. © 2013 Pearson Education, Inc.
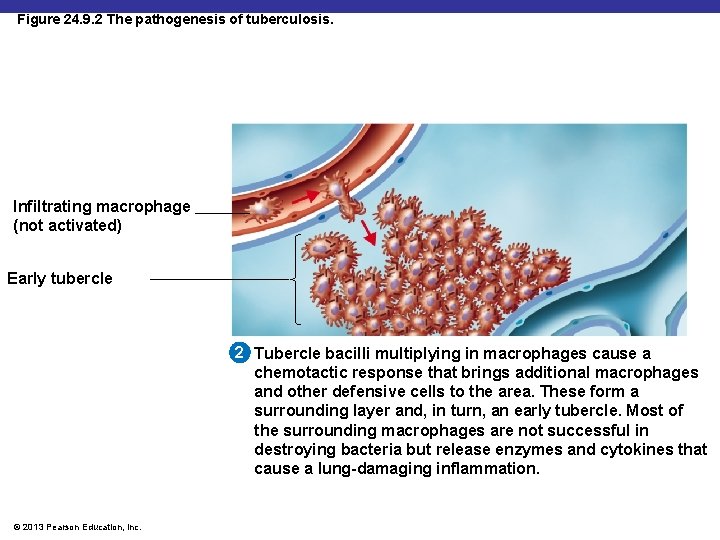
Figure 24. 9. 2 The pathogenesis of tuberculosis. Infiltrating macrophage (not activated) Early tubercle 2 Tubercle bacilli multiplying in macrophages cause a chemotactic response that brings additional macrophages and other defensive cells to the area. These form a surrounding layer and, in turn, an early tubercle. Most of the surrounding macrophages are not successful in destroying bacteria but release enzymes and cytokines that cause a lung-damaging inflammation. © 2013 Pearson Education, Inc.
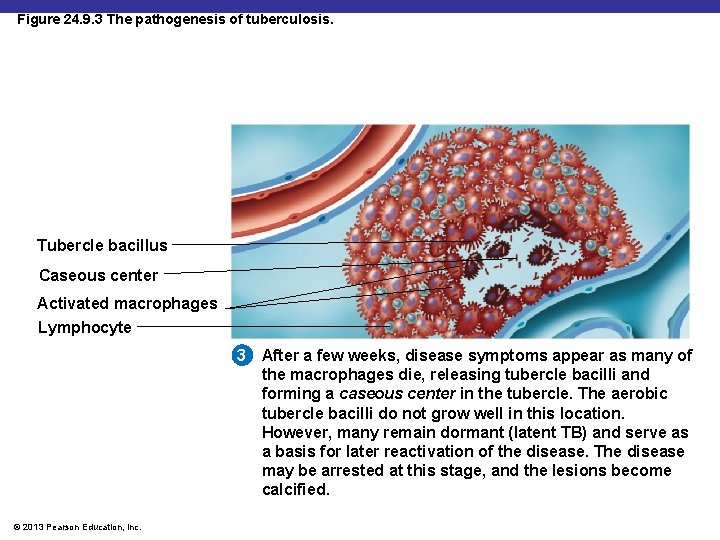
Figure 24. 9. 3 The pathogenesis of tuberculosis. Tubercle bacillus Caseous center Activated macrophages Lymphocyte 3 After a few weeks, disease symptoms appear as many of the macrophages die, releasing tubercle bacilli and forming a caseous center in the tubercle. The aerobic tubercle bacilli do not grow well in this location. However, many remain dormant (latent TB) and serve as a basis for later reactivation of the disease. The disease may be arrested at this stage, and the lesions become calcified. © 2013 Pearson Education, Inc.
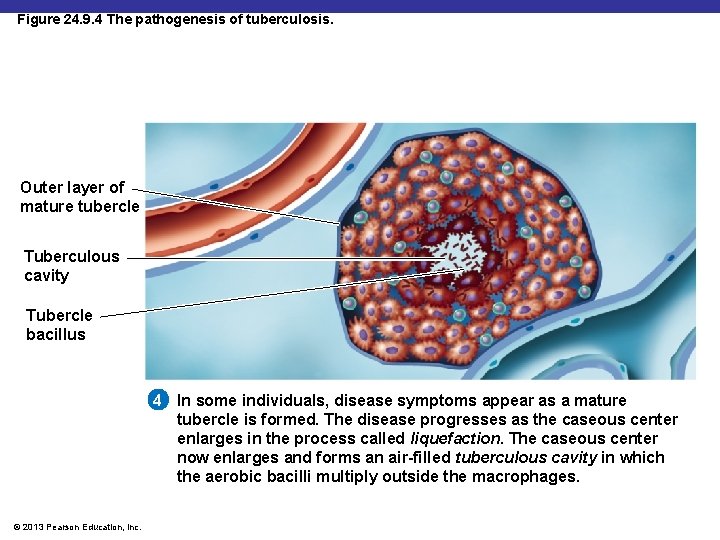
Figure 24. 9. 4 The pathogenesis of tuberculosis. Outer layer of mature tubercle Tuberculous cavity Tubercle bacillus 4 In some individuals, disease symptoms appear as a mature tubercle is formed. The disease progresses as the caseous center enlarges in the process called liquefaction. The caseous center now enlarges and forms an air-filled tuberculous cavity in which the aerobic bacilli multiply outside the macrophages. © 2013 Pearson Education, Inc.
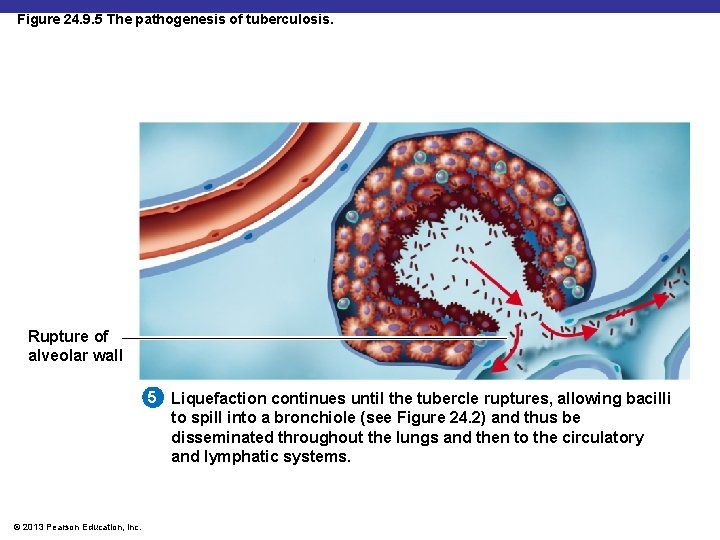
Figure 24. 9. 5 The pathogenesis of tuberculosis. Rupture of alveolar wall 5 Liquefaction continues until the tubercle ruptures, allowing bacilli to spill into a bronchiole (see Figure 24. 2) and thus be disseminated throughout the lungs and then to the circulatory and lymphatic systems. © 2013 Pearson Education, Inc.

Treatment of Tuberculosis § Treatment: prolonged treatment with multiple antibiotics § Vaccines: BCG vaccine, live culture of avirulent M. bovis; not widely used in United States © 2013 Pearson Education, Inc.
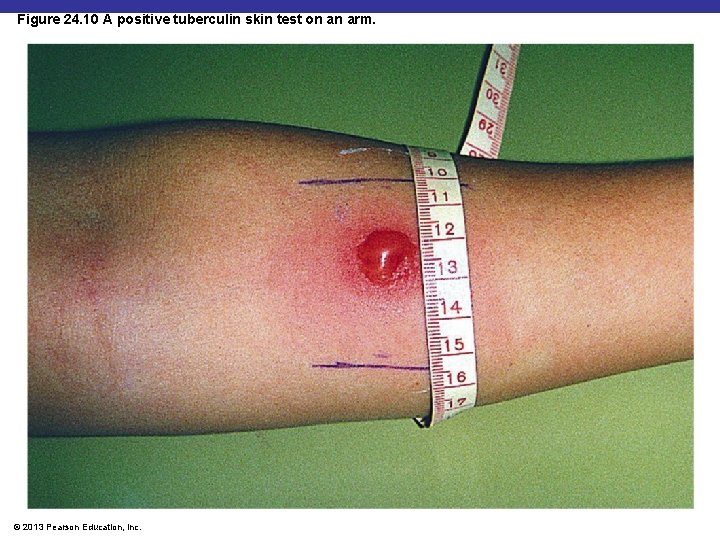
Figure 24. 10 A positive tuberculin skin test on an arm. © 2013 Pearson Education, Inc.

Diagnosis of Tuberculosis § Tuberculin skin test screening § Positive reaction means current or previous infection § Followed by X-ray or CT exam, acid-fast staining of sputum, culturing of bacteria © 2013 Pearson Education, Inc.
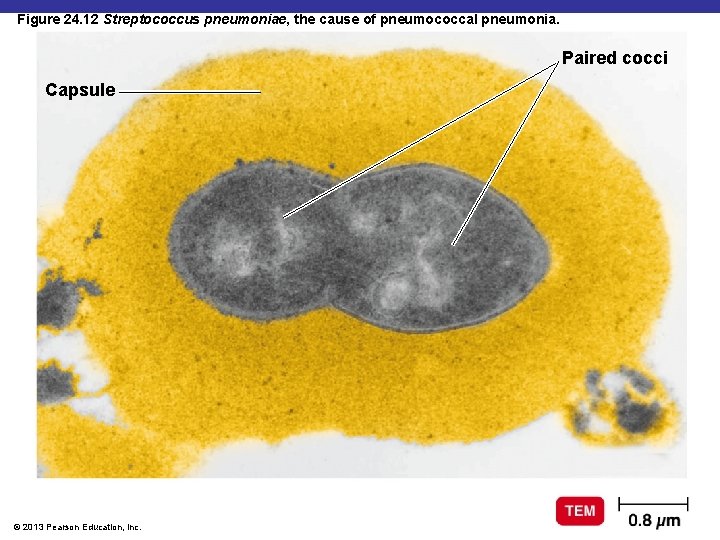
Figure 24. 12 Streptococcus pneumoniae, the cause of pneumococcal pneumonia. Paired cocci Capsule © 2013 Pearson Education, Inc.

Pneumococcal Pneumonia § Streptococcus pneumoniae: encapsulated diplococci § Symptoms: infected alveoli of lung fill with fluids; interferes with oxygen uptake § Diagnosis: optochin-inhibition test or bile solubility test; serological typing of bacteria § Treatment: macrolides, fluoroquinolones § Prevention: pneumococcal vaccine © 2013 Pearson Education, Inc.

Haemophilus influenzae Pneumonia § Gram-negative coccobacillus § Predisposing factors: alcoholism, poor nutrition, cancer, or diabetes § Symptoms: resemble those of pneumococcal pneumonia § Diagnosis: isolation; special media for nutritional requirements § Treatment: cephalosporins © 2013 Pearson Education, Inc.

Mycoplasmal Pneumonia § Primary atypical pneumonia; walking pneumonia § Mycoplasma pneumoniae § Pleomorphic, wall-less bacteria § Common in children and young adults © 2013 Pearson Education, Inc.
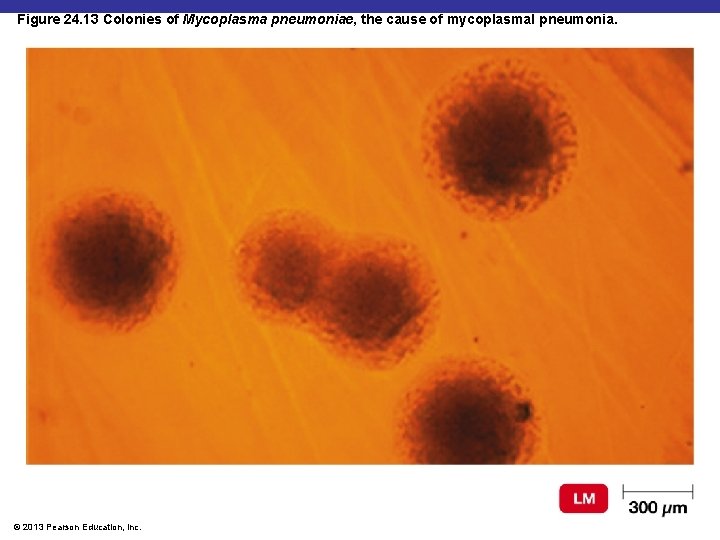
Figure 24. 13 Colonies of Mycoplasma pneumoniae, the cause of mycoplasmal pneumonia. © 2013 Pearson Education, Inc.
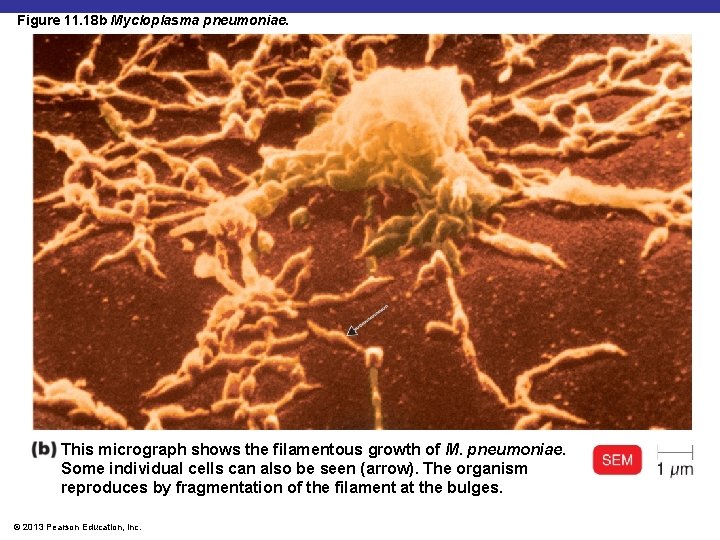
Figure 11. 18 b Mycloplasma pneumoniae. This micrograph shows the filamentous growth of M. pneumoniae. Some individual cells can also be seen (arrow). The organism reproduces by fragmentation of the filament at the bulges. © 2013 Pearson Education, Inc.

Mycoplasmal Pneumonia § Symptoms: mild but persistent respiratory symptoms; low fever, cough, headache § Diagnosis: PCR and serological testing § Treatment: tetracyclines © 2013 Pearson Education, Inc.

Legionellosis § Legionella pneumophila § Gram-negative rod § Found in water § Transmitted by inhaling aerosols; not transmitted from human to human © 2013 Pearson Education, Inc.

Legionellosis § Symptoms: potentially fatal pneumonia that tends to affect older men who drink or smoke heavily § Diagnosis: culture on selective media, DNA probe § Treatment: erythromycin © 2013 Pearson Education, Inc.

Psittacosis (Ornithosis) § Chlamydophila psittaci § Gram-negative intracellular bacterium § Transmitted to humans by elementary bodies from bird droppings § Reorganizes into reticulate body after being phagocytized © 2013 Pearson Education, Inc.

Psittacosis (Ornithosis) § Symptoms: symptoms, if any, are fever, headache, chills § Diagnosis: growth of bacteria in eggs or cell culture § Treatment: tetracyclines © 2013 Pearson Education, Inc.
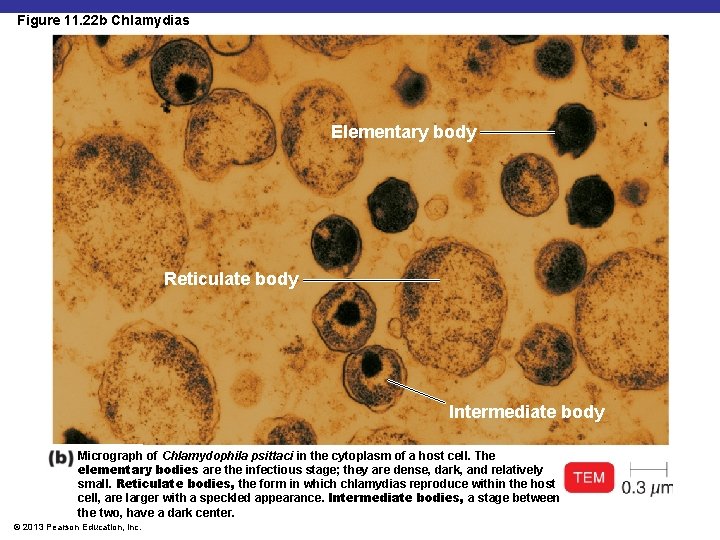
Figure 11. 22 b Chlamydias Elementary body Reticulate body Intermediate body Micrograph of Chlamydophila psittaci in the cytoplasm of a host cell. The elementary bodies are the infectious stage; they are dense, dark, and relatively small. Reticulate bodies, the form in which chlamydias reproduce within the host cell, are larger with a speckled appearance. Intermediate bodies, a stage between the two, have a dark center. © 2013 Pearson Education, Inc.

Chlamydial Pneumonia § Chlamydophila pneumoniae § Transmitted from human to human § Symptoms: mild respiratory illness common in young people; resembles mycoplasmal pneumonia § Diagnosis: serological tests § Treatment: tetracyclines © 2013 Pearson Education, Inc.

Q Fever § § Causative agent: Coxiella burnetii Reservoir: large mammals Tick vector Can be transmitted via unpasteurized milk © 2013 Pearson Education, Inc.
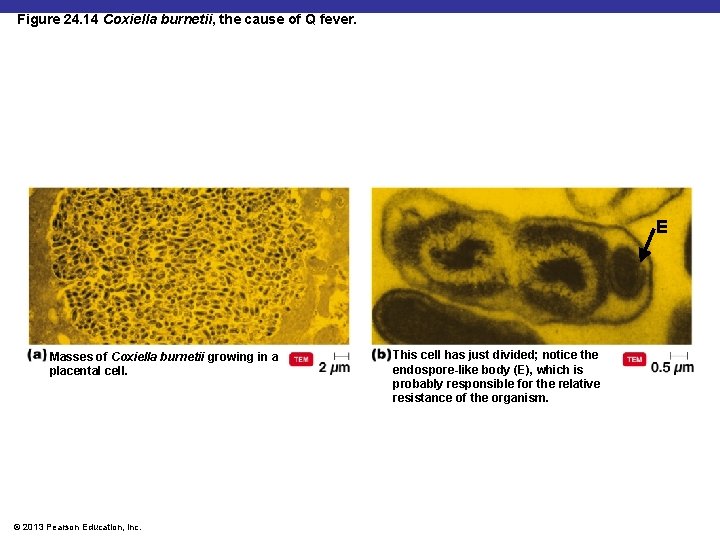
Figure 24. 14 Coxiella burnetii, the cause of Q fever. E Masses of Coxiella burnetii growing in a placental cell. © 2013 Pearson Education, Inc. This cell has just divided; notice the endospore-like body (E), which is probably responsible for the relative resistance of the organism.

Q Fever § Symptoms: mild respiratory disease lasting 1– 2 weeks; occasional complications such as endocarditis occur § Diagnosis: growth in cell culture § Treatment: doxycycline and chloroquine © 2013 Pearson Education, Inc.

Melioidosis § § Causative agent: Burkholderia pseudomallei Reservoir: soil Mainly in southeast Asia and northern Australia Symptoms: pneumonia, or tissue abscesses and severe sepsis § Diagnosis: bacterial culture § Treatment: ceftazidime © 2013 Pearson Education, Inc.

Diseases in Focus: Common Bacterial Pneumonias § A 27 -year-old man with a history of asthma is hospitalized with a 4 -day history of progressive cough and 2 days of spiking fevers. Gram-positive cocci in pairs are cultured from a blood sample. § Can you identify infections that could cause these symptoms? © 2013 Pearson Education, Inc.
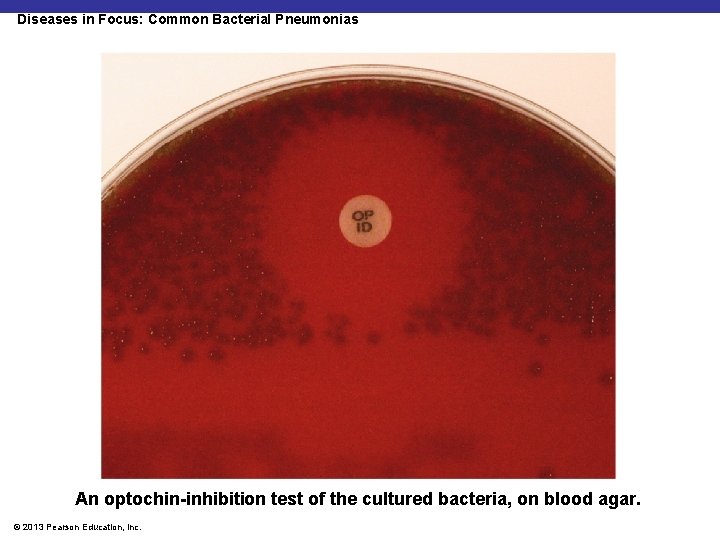
Diseases in Focus: Common Bacterial Pneumonias An optochin-inhibition test of the cultured bacteria, on blood agar. © 2013 Pearson Education, Inc.

Viral Pneumonia § Viral pneumonia occurs as a complication of influenza, measles, or chickenpox § Viral etiology suspected if no other cause is determined © 2013 Pearson Education, Inc.

Respiratory Syncytial Virus (RSV) § § Common in infants; 4500 deaths annually Causes cell fusion (syncytium) in cell culture Symptoms: pneumonia in infants Diagnosis: serological test for viruses and antibodies § Treatment: ribavirin, palivizumab © 2013 Pearson Education, Inc.

Influenza (Flu) § Symptoms: chills, fever, headache, and muscle aches § No intestinal symptoms § 1% mortality, very young and very old § Treatment: zanamivir and oseltamivir inhibit neuraminidase § Prophylaxis: multivalent vaccine © 2013 Pearson Education, Inc.
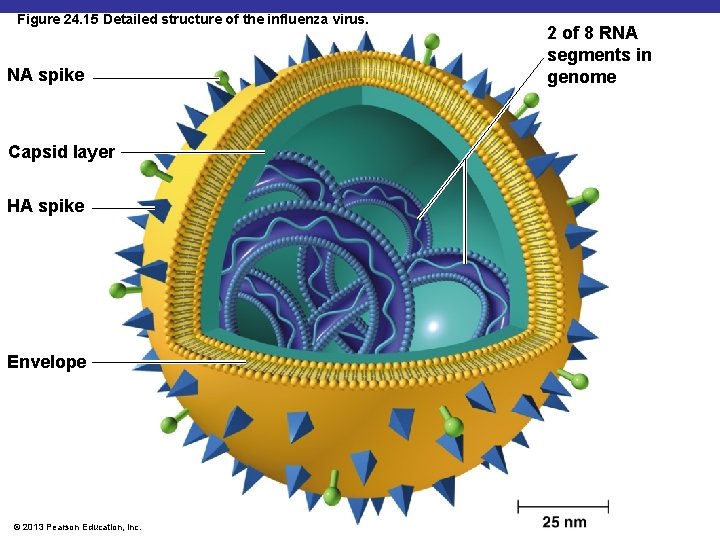
Figure 24. 15 Detailed structure of the influenza virus. NA spike Capsid layer HA spike Envelope © 2013 Pearson Education, Inc. 2 of 8 RNA segments in genome

The Influenza Virus § Hemagglutinin (HA) spikes used for attachment to host cells § Neuraminidase (NA) spikes used to release virus from cell § Antigenic shift § Changes in HA and NA spikes § Probably due to genetic recombination between different strains infecting the same cell § Antigenic drift § Point mutations in genes encoding HA or NA spikes § May involve only one amino acid § Allows virus to avoid mucosal Ig. A antibodies © 2013 Pearson Education, Inc.
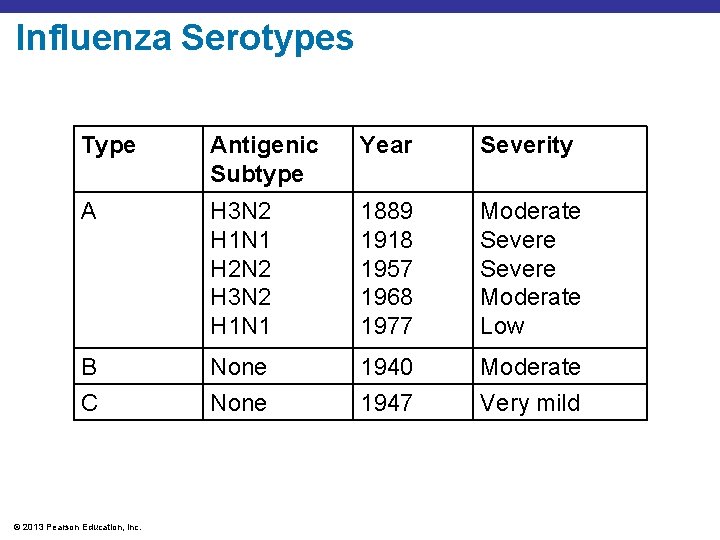
Influenza Serotypes Type Antigenic Subtype Year Severity A H 3 N 2 H 1 N 1 H 2 N 2 H 3 N 2 H 1 N 1 1889 1918 1957 1968 1977 Moderate Severe Moderate Low B None 1940 Moderate C None 1947 Very mild © 2013 Pearson Education, Inc.
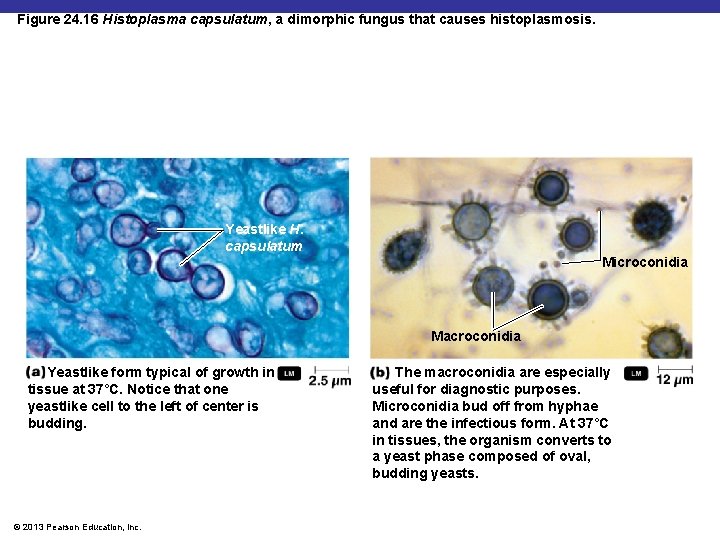
Figure 24. 16 Histoplasma capsulatum, a dimorphic fungus that causes histoplasmosis. Yeastlike H. capsulatum Microconidia Macroconidia Yeastlike form typical of growth in tissue at 37°C. Notice that one yeastlike cell to the left of center is budding. © 2013 Pearson Education, Inc. The macroconidia are especially useful for diagnostic purposes. Microconidia bud off from hyphae and are the infectious form. At 37°C in tissues, the organism converts to a yeast phase composed of oval, budding yeasts.
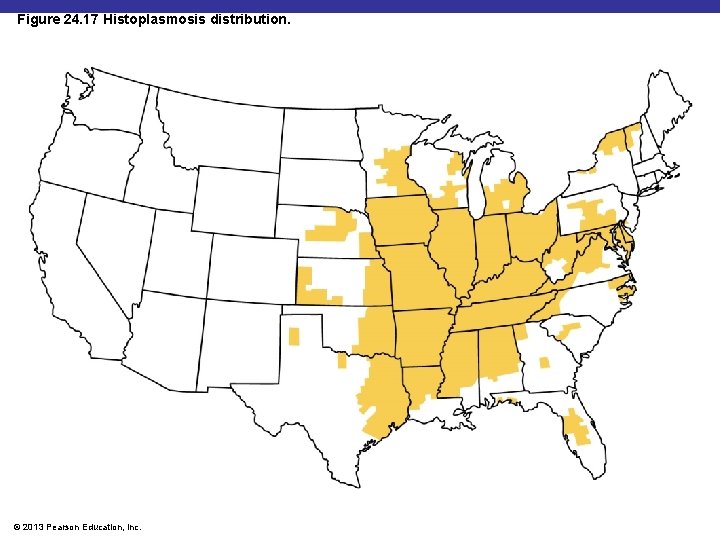
Figure 24. 17 Histoplasmosis distribution. © 2013 Pearson Education, Inc.

Coccidioidomycosis § § § Causative agent: Coccidioides immitis Reservoir: desert soils of American Southwest Symptoms: fever, coughing, weight loss Diagnosis: serological tests Treatment: amphotericin B © 2013 Pearson Education, Inc.
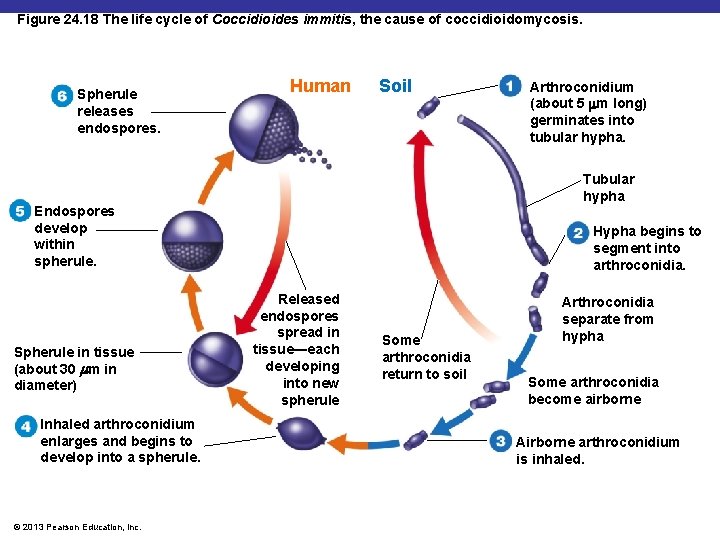
Figure 24. 18 The life cycle of Coccidioides immitis, the cause of coccidioidomycosis. Spherule releases endospores. Human Soil Tubular hypha Endospores develop within spherule. Spherule in tissue (about 30 mm in diameter) Inhaled arthroconidium enlarges and begins to develop into a spherule. © 2013 Pearson Education, Inc. Arthroconidium (about 5 mm long) germinates into tubular hypha. Hypha begins to segment into arthroconidia. Released endospores spread in tissue—each developing into new spherule Some arthroconidia return to soil Arthroconidia separate from hypha Some arthroconidia become airborne Airborne arthroconidium is inhaled.
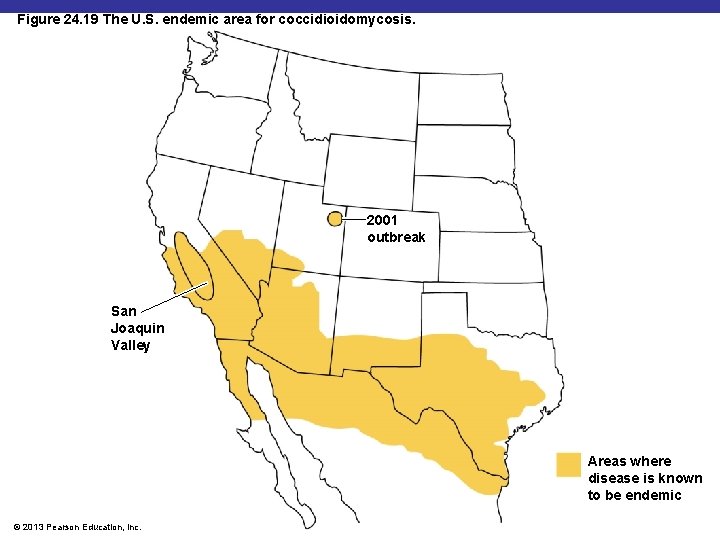
Figure 24. 19 The U. S. endemic area for coccidioidomycosis. 2001 outbreak San Joaquin Valley Areas where disease is known to be endemic © 2013 Pearson Education, Inc.

Pneumocystis Pneumonia § § § Causative agent: Pneumocystis jirovecii Reservoir: unknown; possibly humans or soil Symptoms: pneumonia Diagnosis: microscopy Treatment: trimethoprim © 2013 Pearson Education, Inc.
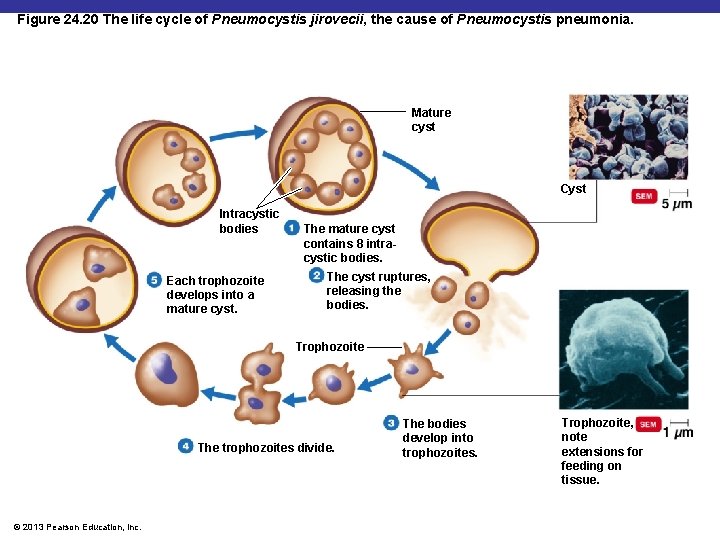
Figure 24. 20 The life cycle of Pneumocystis jirovecii, the cause of Pneumocystis pneumonia. Mature cyst Cyst Intracystic bodies Each trophozoite develops into a mature cyst. The mature cyst contains 8 intracystic bodies. The cyst ruptures, releasing the bodies. Trophozoite The trophozoites divide. © 2013 Pearson Education, Inc. The bodies develop into trophozoites. Trophozoite, note extensions for feeding on tissue.

Blastomycosis § § § Causative agent: Blastomyces dermatitidis Reservoir: soil in Mississippi valley area Symptoms: abscesses; extensive tissue damage Diagnosis: isolation of pathogen Treatment: amphotericin B © 2013 Pearson Education, Inc.

Other Fungi Involved in Respiratory Disease § Systemic § Predisposing factors: § Immunocompromised state § Cancer § Diabetes § Aspergillus fumigatus § Mucor § Rhizopus © 2013 Pearson Education, Inc.

Diseases in Focus: Diseases of the Lower Respiratory System § A worker is hospitalized for acute respiratory illness. He had been near a colony of bats. The mass is surgically removed. Microscopic examination of the mass reveals ovoid yeast cells. § Can you identify infections that could cause these symptoms? © 2013 Pearson Education, Inc.
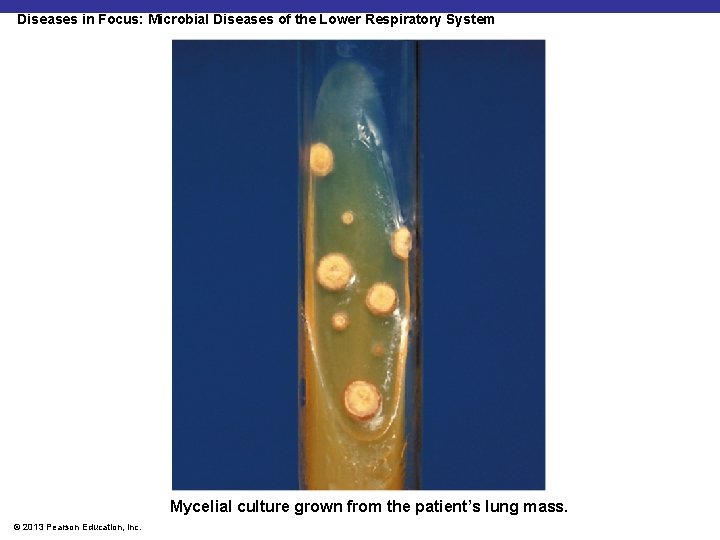
Diseases in Focus: Microbial Diseases of the Lower Respiratory System Mycelial culture grown from the patient’s lung mass. © 2013 Pearson Education, Inc.
- Slides: 69