Chapter 24 Management of Patients With Chronic Pulmonary
































- Slides: 44

Chapter 24 Management of Patients With Chronic Pulmonary Disease Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

COPD: (Chronic Obstructive Pulmonary Disease) • A disease state characterized by airflow limitation that is not full reversible (decreased vital capacity and forced expiratory volume). • Progressive, associated with an abnormal inflammatory response of the lung to noxious particles or gases • COPD includes diseases that cause airflow obstruction (emphysema, chronic bronchitis) or a combination of these disorders. • Asthma is now considered a separate disorder but can coexist with COPD. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Pathophysiology of COPD • Inflammatory response occurs throughout the airways, lung parenchyma, and pulmonary vasculature. • chronic inflammation + the body’s attempts to repair it ---- Scar tissue and narrowing occurs in airways. • In large diameter airways (trachea and bronchi) -- increased numbers of goblet cells and enlarged submucosal glands hypersecretion of mucus. • In the small diameter airways, inflammation causes thickening of the airway wall, peribronchial fibrosis, exudate, and overall airway narrowing (obstructive bronchiolitis). Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

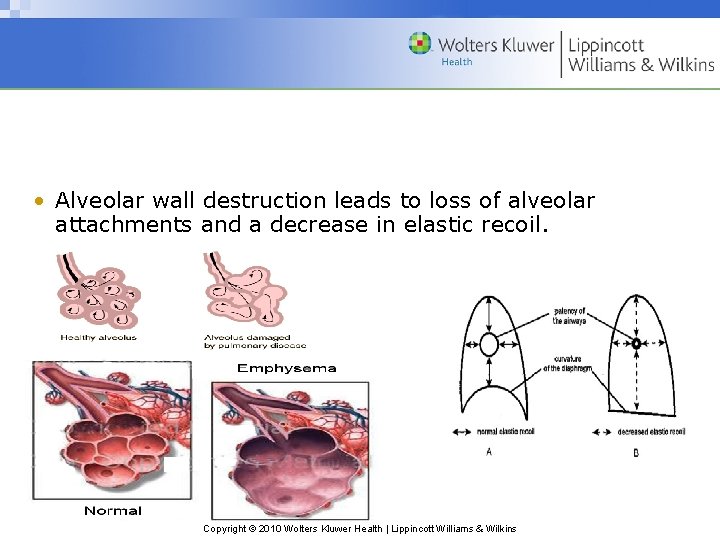
• Alveolar wall destruction leads to loss of alveolar attachments and a decrease in elastic recoil. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

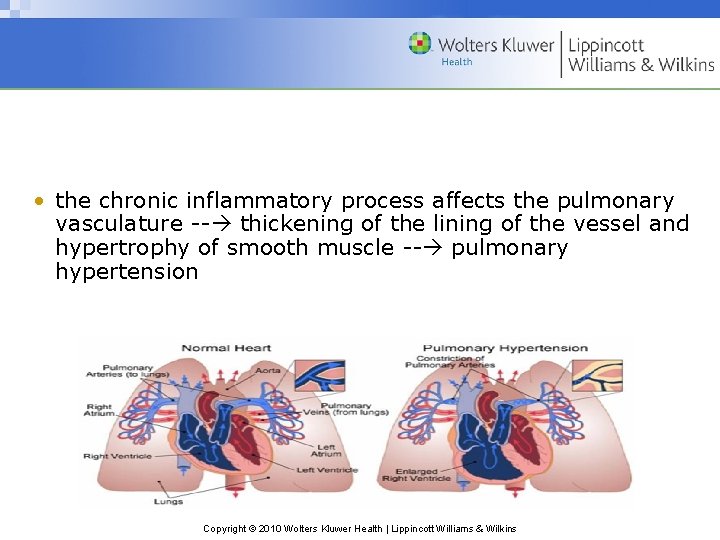
• the chronic inflammatory process affects the pulmonary vasculature -- thickening of the lining of the vessel and hypertrophy of smooth muscle -- pulmonary hypertension Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

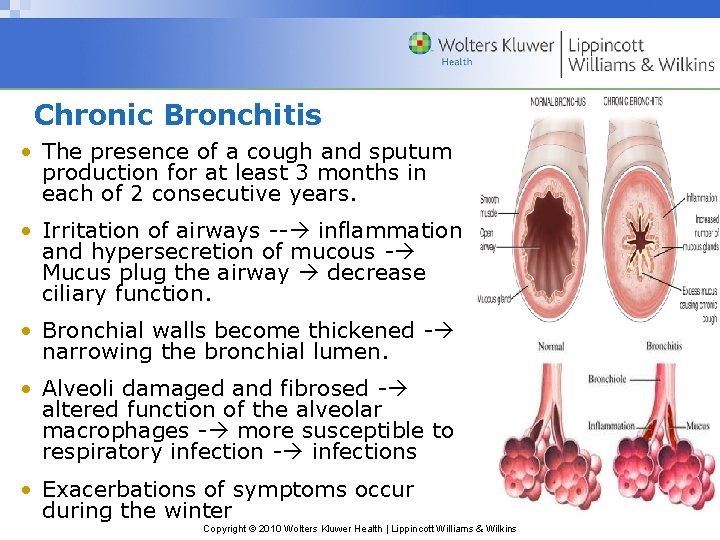
Chronic Bronchitis • The presence of a cough and sputum production for at least 3 months in each of 2 consecutive years. • Irritation of airways -- inflammation and hypersecretion of mucous - Mucus plug the airway decrease ciliary function. • Bronchial walls become thickened - narrowing the bronchial lumen. • Alveoli damaged and fibrosed - altered function of the alveolar macrophages - more susceptible to respiratory infection - infections • Exacerbations of symptoms occur during the winter Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Emphysema: • Abnormal distention of air spaces beyond the terminal bronchioles with destruction of the walls of the alveoli. • Decreased alveolar surface area - the pulmonary capillaries continually decreases - an increase in “dead space” and impaired oxygen diffusion. • In the later stages: impaired CO 2 elimination � hypercapnia � respiratory acidosis. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

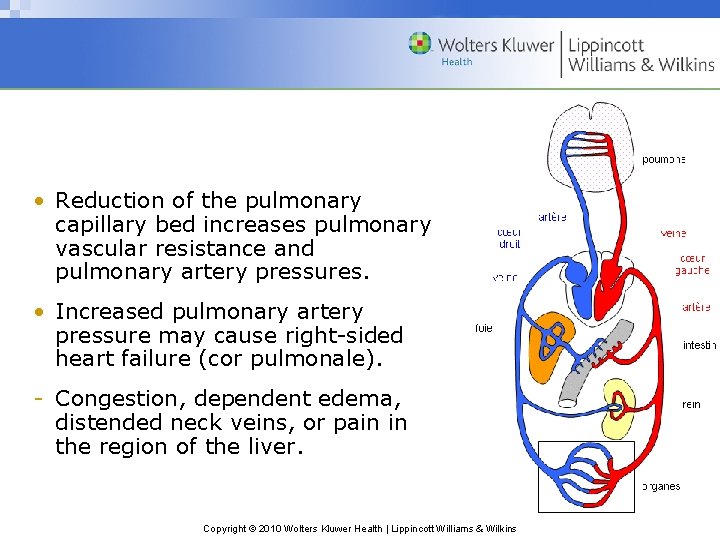
• Reduction of the pulmonary capillary bed increases pulmonary vascular resistance and pulmonary artery pressures. • Increased pulmonary artery pressure may cause right-sided heart failure (cor pulmonale). - Congestion, dependent edema, distended neck veins, or pain in the region of the liver. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

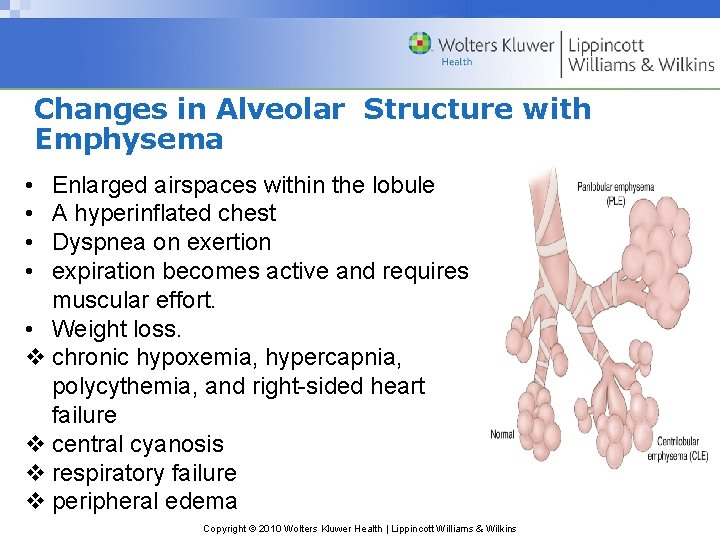
Changes in Alveolar Structure with Emphysema • • Enlarged airspaces within the lobule A hyperinflated chest Dyspnea on exertion expiration becomes active and requires muscular effort. • Weight loss. v chronic hypoxemia, hypercapnia, polycythemia, and right-sided heart failure v central cyanosis v respiratory failure v peripheral edema Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Risk Factors for COPD - Environmental: • Tobacco smoke causes 80 -90% of COPD cases! • Passive smoking • Occupational exposure • Ambient air pollution • Genetic abnormalities – Alpha 1 -antitrypsin Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

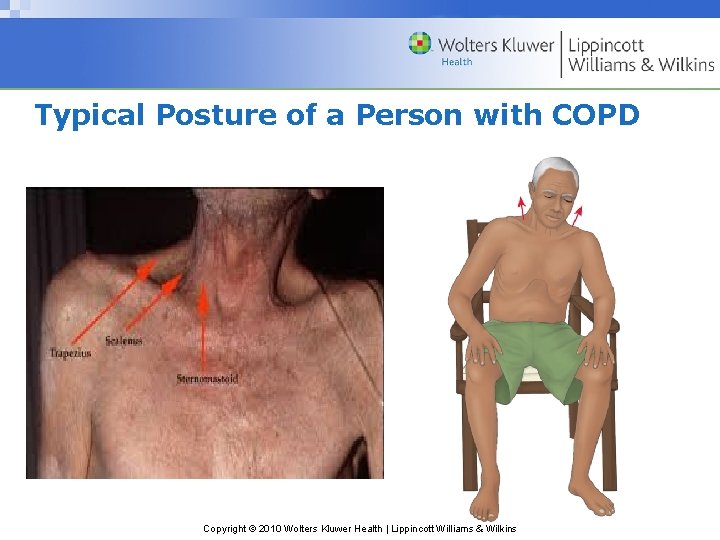
Clinical Manifestations: COPD • progressive disease - 3 primary symptoms: – chronic cough – sputum production – Dyspnea on exertion, later: dyspnea at rest • Weight loss • respiratory infections • barrel chest (hyperinflation) • Retraction of the supraclavicular fossae on inspiration, so the shoulders to pulled upward Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

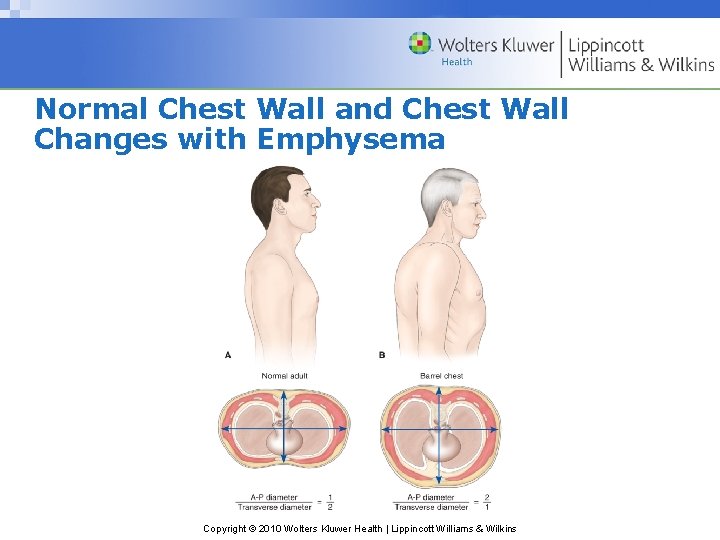
Normal Chest Wall and Chest Wall Changes with Emphysema Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Typical Posture of a Person with COPD Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Assessment & Diagnostics: COPD • health history (past medical history, risk factors, family history, history of symptoms) • Pulmonary function test; Spirometry is used to evaluate airflow obstruction • Arterial blood gases to assess oxygenation and gas exchange • chest x-ray to exclude alternative diagnoses. • chest CT scan in the differential diagnosis. • screening for alpha 1 -antitrypsin deficiency for patients younger than 45 years of age and for those with a strong family history of COPD. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Stages: COPD – Stage I (mild) – Stage II (moderate) – Stage III (severe) – Stage IV (very severe) • survival of COPD: - history of cigarette smoking, - pulmonary artery pressure, - passive smoking exposure, - age, - rate of decline of FEV 1, - resting heart rate, - weight loss, - reversibility of airflow obstruction - hypoxemia, Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Complications: COPD • Respiratory failure are major life-threatening complications. • Infections • Pneumonia • chronic atelectasis • Pneumothorax • pulmonary arterial hypertension (corpulmonale). Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

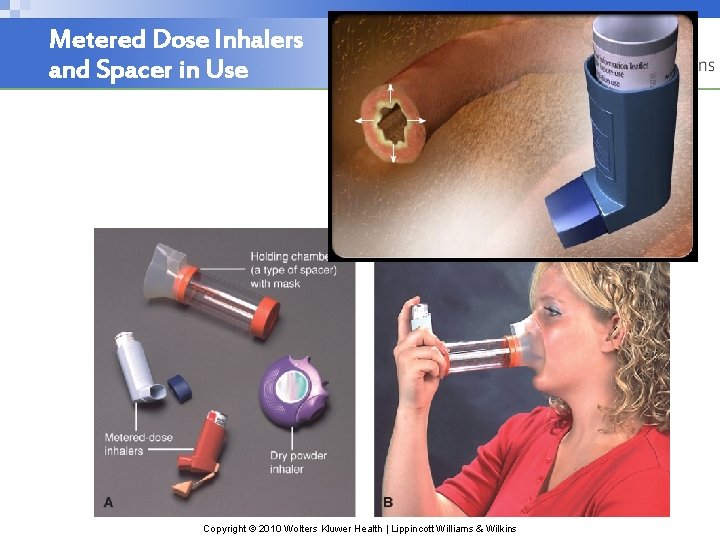
Medical Management: COPD • Risk Reduction – Stop Smoking • Pharmacologic Therapy – Bronchodilators; relieve bronchospasm allowing oxygen distribution throughout the lungs and improve alveolar ventilation. § delivered through an inhaler, nebulization, or oral route in pill or liquid form. § classes of bronchodilators: beta-adrenergic agonists, anticholinergic agents Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Metered Dose Inhalers and Spacer in Use Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Medical Management: COPD • Pharmacologic Therapy – Corticosteroids § symptoms decrease § they do not slow the decline in lung function. § oral corticosteroids is not recommended • Other Medications – alpha -antitrypsin therapy, antibiotic agents, mucolytic agents, antitussive agents, vasodilators, and narcotics. Influenza vaccines 1 Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Management of Exacerbations: COPD • acute change in the patient’s baseline dyspnea, cough, or sputum production beyond the normal day-to-day variations. • causes : infection and air pollution. • oxygen therapy • Optimization of bronchodilator medications = identifying the best medication or combinations of medications taken on a regular schedule for a specific patient. • corticosteroids, antibiotic agents and intensive respiratory interventions Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

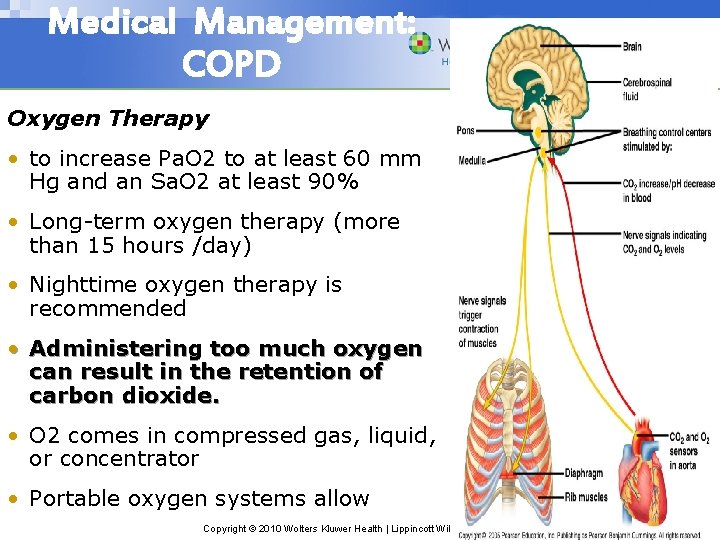
Medical Management: COPD Oxygen Therapy • to increase Pa. O 2 to at least 60 mm Hg and an Sa. O 2 at least 90% • Long-term oxygen therapy (more than 15 hours /day) • Nighttime oxygen therapy is recommended • Administering too much oxygen can result in the retention of carbon dioxide. • O 2 comes in compressed gas, liquid, or concentrator • Portable oxygen systems allow Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Oxygen indication: • a Pa. O 2 of 55 mm Hg or less • evidence of tissue hypoxia • and organ damage such as cor pulmonale, secondary polycythemia, edema from right-sided heart failure, or impaired mental status Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

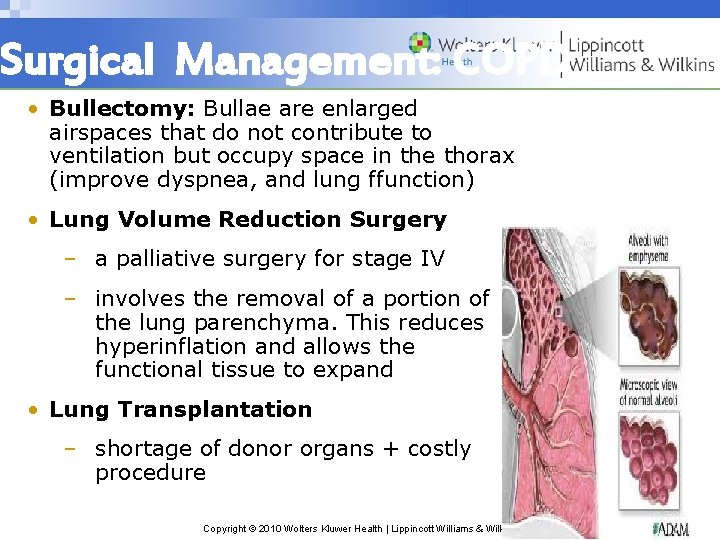
Surgical Management: COPD • Bullectomy: Bullae are enlarged airspaces that do not contribute to ventilation but occupy space in the thorax (improve dyspnea, and lung ffunction) • Lung Volume Reduction Surgery – a palliative surgery for stage IV – involves the removal of a portion of the lung parenchyma. This reduces hyperinflation and allows the functional tissue to expand • Lung Transplantation – shortage of donor organs + costly procedure Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Surgical Management: COPD • Pulmonary Rehabilitation • to reduce symptoms, improve quality of life, and increase physical and emotional participation in everyday activities • include assessment, education, smoking cessation, physical reconditioning, nutritional counseling, skills training, and psychological support. • appropriate for stages II through IV • The minimum length of an effective program is 6 weeks Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Management: COPD Patient Education Topics: • anatomy and physiology, pathophysiology • medications and oxygen therapy • Nutrition • respiratory therapy treatments • symptoms alleviation • smoking cessation, coping with COPD • communicating with the health care team • Planning for the future Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

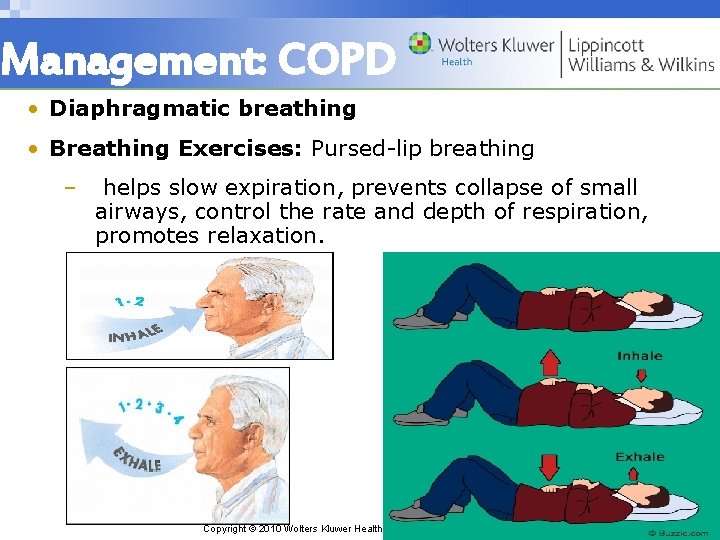
Management: COPD • Diaphragmatic breathing • Breathing Exercises: Pursed-lip breathing – helps slow expiration, prevents collapse of small airways, control the rate and depth of respiration, promotes relaxation. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Management: COPD • Activity Pacing • become fatigued. • moving around for an hour before beginning activity. • planning self-care activities. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Management: COPD • Self-Care Activities – encouraged to increase participation in self-care. – The patient should bathe, dress, and take short walks, resting as needed to avoid fatigue and dyspnea. – Fluids should always be available. – postural drainage Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Management: COPD Physical Conditioning • Breathing exercises and general exercises • Graded exercises; treadmills, stationary bicycles, and measured level walks can improve symptoms • Lightweight portable oxygen systems are available for patients who require O 2 therapy during activity. Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nursing Management: COPD • Assessing the Patient • Achieving Airway Clearance • Improving Breathing Patterns • Improving Activity Tolerance • Monitoring and Managing Complications • Promoting Home and Community-Based Care • Teaching Patients Self-Care Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Achieving Airway Clearance • dyspnea, secretions, and infection. • mucus, decreased mucociliary action - Bronchospasm (wheezing or diminished breath sounds) decreased airflow and decreased gas exchange. • the loss of lung elasticity • monitor the patient for dyspnea and hypoxemia. • administer the medications and be alert for side effects. • the force of expiration, how long it takes to exhale, and the amount of air exhaled • eliminate pulmonary irritants Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

• Instructs the patient in directed or controlled coughing (“Huff” coughing) • Chest physiotherapy with postural drainage, intermittent positive pressure breathing, increased fluid intake, and bland aerosol mists (with normal saline solution or water) Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Improving Breathing Patterns • Dyspnea the ineffective respiratory mechanics of the chest wall and lung - air trapping, ineffective diaphragmatic movement, airway obstruction, the metabolic cost of breathing, and stress. • Training in diaphragmatic breathing • Pursed-lip breathing Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Improving Activity Tolerance • exercise intolerance • promote independence in executing activities of daily living. • upper and lower extremities Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Monitoring and Managing Potential Complications • respiratory failure, respiratory infection and chronic atelectasis • cognitive changes • increasing dyspnea, tachypnea, and tachycardia • monitors pulse oximetry values • Teach patient about signs and symptoms infection respiratory failure (a fever or change in sputum color, character, consistency, or amount. Any worsening of symptoms (increased tightness of the chest, increased dyspnea, and fatigue) Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

• immunized against influenza • Exposure to irritants • evaluate the patient for potential pneumothorax ( assessing the symmetry of chest movement, differences in breath sounds, and pulse oximetry. • Pulmonary hypertension oxygen therapy Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nursing Management: COPD • Promoting Home and Community-Based Care • Teaching Patients Self-Care - Heat and cold - Exercise - Emotional stressors trigger of cough - Smoking Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nursing Process: The Care of Patients with COPD- Assessment • Health history • Inspection and examination findings • Review of diagnostic tests Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nursing Process: The Care of Patients with COPD- Diagnoses • Impaired gas exchange • Impaired airway clearance • Ineffective breathing pattern • Activity intolerance • Deficient knowledge • Ineffective coping Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Nursing Process: The Care of Patients with COPD- Planning • Smoking cessation • Improved activity tolerance • Maximal self-management • Improved coping ability • Adherence to therapeutic regimen and home care • Absence of complications Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Improving Gas Exchange • Proper administration of bronchodilators and corticosteroids • Reduction of pulmonary irritants • Directed coughing, “huff” coughing • Chest physiotherapy • Breathing exercises to reduce air trapping – diaphragmatic breathing – pursed lip breathing • Use of supplemental oxygen Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Improving Activity Tolerance • Focus on rehabilitation activities to improve ADLs and promote independence. • Pacing of activities • Exercise training • Walking aides • Utilization of a collaborative approach Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Other Interventions • Set realistic goals • Avoid extreme temperatures • Enhancement of coping strategies • Monitor for and management of potential complications Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins

Patient Teaching • Disease process • Medications • Procedures • When and how to seek help • Prevention of infections • Avoidance of irritants; indoor and outdoor pollution, and occupational exposure • Lifestyle changes, including cessation of smoking Copyright © 2010 Wolters Kluwer Health | Lippincott Williams & Wilkins