Chapter 24 Calcium Homeostasis and Hormonal Regulation By

Chapter 24: Calcium Homeostasis and Hormonal Regulation By Josephine Abraham, Dev Abraham Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Calcium Homeostasis • Serum calcium maintained at a constant level • Cellular & tissue effects of calcium depend on blood calcium maintenance within a specific range. • Adult human body contains 1, 000 g of calcium – 99% as hydroxyapatite salt (bone) – 1% in extra-cellular fluids (blood) – which regulates various biochemical events. – Diet is only source of calcium – Urine is only significant “way out” Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins
Calcium • Calcium critical for heart/muscle contractions, blood clotting, bone density, and other functions. • Of the 1% of body calcium in extra-cellular fluids (blood) • 50% is ionized calcium • 40% pound to protein • 10% complexed form (small ions - citrate and phosphate) • Vitamin D and Parathyroid hormone (PTH) – are the two most important hormones that regulate calcium homeostasis. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins
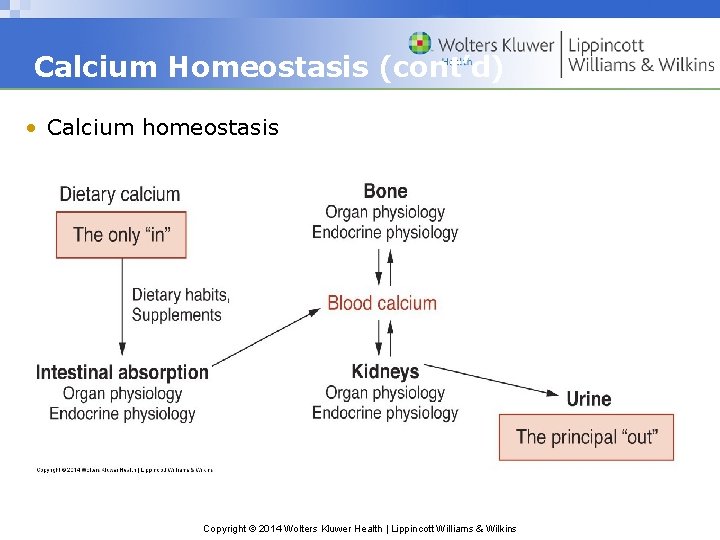
Calcium Homeostasis (cont’d) • Calcium homeostasis Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Hormonal Control of Calcium Metabolism • Vitamin D – Steroid hormone, not actually a vitamin – synthesized by skin from cholesterol following UVB rays from sun. – Serum 25 -hydroxyl Vitamin D is best indicator of body stores therefore, low 25 -hydroxyl Vitamin D in blood = deficiency – Tissues involved in synthesis: skin, liver, kidneys – Tissues it affects: gut, bone, parathyroids – Can also be obtained from dietary sources: fortified milk, multivitamins, cod liver oil – Key point – Vitamin D is steroid hormone derived from cholesterol. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins
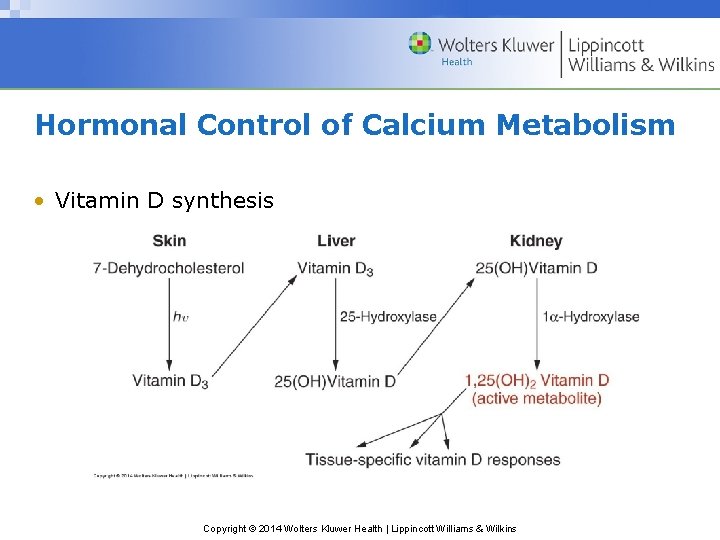
Hormonal Control of Calcium Metabolism • Vitamin D synthesis Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Hormonal Control of Calcium Metabolism • Parathyroid Hormone (PTH) – Secreted from 4 parathyroid glands in region of thyroid gland – Parathyroid glands have calcium-sensing receptors that respond to calcium levels by increasing or decreasing PTH secretion. – Functions • Stimulates bone resorption and release of calcium into blood • Acts on kidney to increase fractional reabsorption of renal tubular calcium & drive production of active metabolite • Promotes intestinal absorption of calcium by activating 1, 25(OH)2 D (Said another way – Vitamin D is enhanced by PTH, which promotes meal-related intestinal absorption of calcium. ) – All functions raise blood calcium & are mediated via a specific PTH receptor. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Parathyroid Hormone and Calcium Levels • When Blood Calcium decreases • PTH is secreted by parathyroid glands • This stimulates Osteoclasts (cells that promote breakdown of bone for Calcium release) and inhibits Osteoblasts (bone building) • When Blood Calcium increases • PTH is suppressed (Negative Feedback Mechanism) • Calcitonin is secreted by thyroid • This stimulates Osteoblasts (bone building cell) and inhibits Osteoclasts (bone breakdown cell) Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Organ Physiology and Calcium Metabolism • Gastrointestinal (GI) tract Regulation of Calcium – Factors required for calcium absorption • Normal intestinal function (short bowel syndrome & genetic or physiologic defects may have negative effect) • Adequate dietary calcium intake • Normal vitamin D availability & metabolism • 1, 25 (OH)2 D controls calcium absorption from the small bowel. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Organ Physiology and Calcium Metabolism • Role of Kidneys in Calcium Metabolism – Diseased kidney impairs calcium and phosphate metabolism. – Impaired hydroxylation of 25 -hydroxyl Vitamin D to form the active 1, 25 (OH)2 D result in poor calcium absorption in the gut. – Serum PTH levels can be elevated (up to 1000 x) in chronic renal failure – leading to hypercalcemia. • Once a critical calcium/phosphate level is reached, they precipitate into tissues with devastating consequences. – Primary hyperparathyroidism (PHPT) – over production of PTH causing hypercalcemia – PHPT patients form calcium kidney stones Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Organ Physiology and Calcium Metabolism • Bone Physiology (Bone contains about 1 kg of calcium) – Bone turnover (remodeling): coupled process of simultaneous bone formation & breakdown occurring throughout life – Bone formation is mediated by osteoblasts. • Alkaline Phosphatase = marker for bone formation – Bone breakdown (resorption) is mediated by osteoclasts. – When resorption exceeds formation, bone mass decreases (increased risk of fracture). – Two main types of bone in skeleton • Cortical: primary type in long bones (femur); strong, rigid • Trabecular: axial skeleton (vertebrae); has many cross-hair type connections (trabeculae), providing strength & elasticity Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Calcium Reference Ranges • Total Calcium - Serum – 8. 6 to 10. 0 mg/d. L • Ionized Calcium – Serum – 4. 6 to 5. 3 mg/d. L • Ionized Calcium – Plasma – 4. 1 to 4. 9 mg/d. L Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Hypercalcemia • Blood calcium levels above expected normal range • Binding of calcium to other substances must be taken into account when considering total calcium levels. – Patient with low serum albumin would be expected to have low total calcium & normal ionized calcium. – Opposite is true for patients with high serum albumin. • PHPT most common cause of hypercalcemia in outpatient setting. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Causes of Hypercalcemia • PHPT—most common • Secondary and tertiary hyperparathyroidism – Chronic Renal Failure – low stimuli causes high PTH which causes high calcium • CSR (calcium sensing receptor) abnormalities • Other endocrine disorders – Adrenal insufficiency, hyperthyroidism, etc. • Cancer-mediated hypercalcemia • Granulomatous diseases – Tuburculosis, leprosy, fungal infections, Crohn disease • Medications – HCTZ, lithium, Vitamin A or D toxicity, etx. • Miscellaneous – Wilson’s Syndrome Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Hypercalcemia • Endocrine Causes of Hypercalcemia – Primary hyperparathyroidism (PHPT) • Most common cause of hypercalcemia in outpatient setting • Hallmark of PHPT is overproduction of PTH caused by a single adenoma(s) in one of the parathyroid glands • Parathyroid carcinoma occurs more commonly in a familial syndrome called hyperparathyroidism-jaw tumor syndrome. – Hypervitaminosis D • Caused by excessive intake of vitamin D or aberrant production of 1, 25(OH)2 D – Cancers (PTHr. P), tumors • Cause release of hormones or hormone-like substances Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Hypercalcemia • Signs and Symptoms – CNS: lethargy, decreased alertness, depression, confusion, forgetfulness, obtundation, coma – GI: anorexia, constipation, nausea & vomiting – Renal: impairs kidney’s ability to concentrate urine, leading to dehydration, increased risk of kidney stones – Skeletal: increased bone resorption, increased bone demineralization & risk of fracture – Cardiovascular: causes or exacerbates hypertension Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Hypercalcemia • Familial Hypocalciuric Hypercalcemia – Benign condition – Germline mutation of CSR (Calcium Sensing Receptors) – Stable, mild hypercalcemia from birth – Hypocalciuria is the hallmark of the disease, along with mild hypercalcemia, mild PTH elevation, and mild elevation of Magnesium. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Hypercalcemia Other causes of hypercalcemia: – Hyperthyroidism – increased resorption (low PTH) – Addison’s disease, Addisonian crisis – Milk-alkali syndrome (Burnett’s syndrome) • Results from ingestion of large amounts of calcium together with an absorbable alkali • PTH level is low. – Renal failure • Renal excretion of both calcium & phosphate is severely impaired. • Production of active form of vitamin D is limited. • PTH secretion is stimulated. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Hypercalcemia • Medications That Can Cause Hypercalcemia – Thiazide diuretics • Used to treat hypertension • Cause retention of glomerularly filtered calcium – Lithium • Used to treat bipolar affective disorder • Appears to shift “set point” at calcium-sensing receptor – Vitamin A • Believed to activate osteoclasts & enhance bone resorption, elevating blood calcium; PTH & 1, 25(OH)2 D are suppressed Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Hypocalcemia • State of blood calcium levels below expected range • Best measured by ionized calcium • Signs and symptoms – Neuromuscular: tetany in hands, feet, legs, back; Chvostek’s sign (twitching at corner of mouth(; numbness & tingling in face, hands, & feet – CNS: irritability, seizures, personality changes, impaired intellectual functioning – Cardiovascular: QT prolongation, electromechanical dissociation Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Hypocalcemia • Causes – Parathyroid glands, when functioning properly, will not only correct falling blood calcium but also prevent it by increasing PTH secretion. – Compensatory rise in PTH secretion is known as secondary hyperparathyroidism. – Features that distinguish secondary hyperparathyroidism from primary: • Parathyroids are functioning properly; increased PTH is appropriate mechanism. • Treatment involves identifying & correcting process threatening hypocalcemia, not removal of parathyroid(s). Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Hypocalcemia • Endocrine Causes of Hypocalcemia – Hypoparathyroidism (lack of PTH) as a result of: • Neck surgery (removal of or damage to parathyroid glands) • Autoimmune destruction of parathyroid tissue • Mutations in PTH gene • Abnormal deposition of copper/aluminum in parathyroids – • Magnesium deficiency Pseudohypoparathyroidism (lack of responsiveness to PTH) (Decreased calcium, elevated phosphorous, elevated PTH) – Vitamin D deficiency (malnutrition, malabsorption, etc) – Tertiary hyperparathyroidism Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Hypocalcemia • Organ System Causes of Hypocalcemia – Intestinal disorders resulting in inadequate calcium or vitamin D absorption • Short bowel syndrome, dumping syndrome, celiac sprue • Threaten hypocalcemia, increased PTH secretion – Renal insufficiency/failure • As a result of hyperphosphatemia & defective metabolism of vitamin D – Genetic defects resulting in impaired ability to recover filtered calcium from tubular fluid Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Hypocalcemia • Medications That Affect Calcium Metabolism – Antiresorptive agents – Medications that stimulate bone resorption – Lithium – Thiazide diuretics – Recombinant human parathyroid hormone Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Metabolic Bone Diseases • Rickets and Osteomalacia – Caused by abnormal bone mineralization & vitamin D deficiency – Rickets • Occurs in growing bone (in children) • Bony deformities from bending of long bones due to gravity – Osteomalacia • Occurs in bone in adults (after closure of epiphyseal plates) • No bony deformities • Alkaline Phosphatase levels are increased – due to increased osteoblastic activity. Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Osteoporosis • Most prevalent metabolic bone disease in adults • Affects estimated 20– 25 million Americans • 4: 1 female: male predominance • Believed to cause 1 -1/2 million fractures annually in U. S. • Diagnosis – Based on clinical characteristics and/or a DEXA scan – Fragility fracture: fracture occurring at an inappropriate degree of trauma Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

Magnesium • Neuromuscular excitability • Decreases in Mg produces neuromuscular excitability • Increased Mg levels (hypermagnesia) – Excessive antacid intake – Enemas – Administration of mg in the presence of renal disease • Intracellular levels are higher than extracellular – Impacted by hemolysis – Hemolysis = falsely elevated Mg results Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins

More, more • Of the following, which has the least influence on serum calcium concentrations when present in physiological amounts? – PTH – Serum phosphorous – Calcitonin – Vitamin D Copyright © 2014 Wolters Kluwer Health | Lippincott Williams & Wilkins
- Slides: 28