Chapter 23 Endocrine Emergencies National EMS Education Standard









































































































- Slides: 118

Chapter 23 Endocrine Emergencies

National EMS Education Standard Competencies Medicine Integrates assessment findings with principles of epidemiology and pathophysiology to formulate a field impression and implement a comprehensive treatment/disposition plan for a patient with a medical complaint.

National EMS Education Standard Competencies Endocrine Disorders • Awareness that − Diabetic emergencies cause altered mental status. • Anatomy, physiology, pathophysiology, assessment, and management of − Acute diabetic emergencies

National EMS Education Standard Competencies Endocrine Disorders • Anatomy, physiology, epidemiology, pathophysiology, psychosocial impact, presentations, prognosis, and management of − − Acute diabetic emergencies Diabetes Adrenal disease Pituitary and thyroid disorders

Introduction • The endocrine system influences almost every cell, organ, and function of the body. − Disorders often display a broad range of signs and symptoms. − Assess thoroughly and treat immediately to prevent life threats.

Anatomy and Physiology • Endocrine system − Network of glands that produce and secrete hormones − Maintain homeostasis − Promote permanent structural change

Anatomy and Physiology • Exocrine glands − Exo: outside − Secrete chemicals for elimination − Ducts carry secretions • Endocrine glands − Endo: inside − Secrete/release chemicals used inside the body − Release hormones into tissue and blood

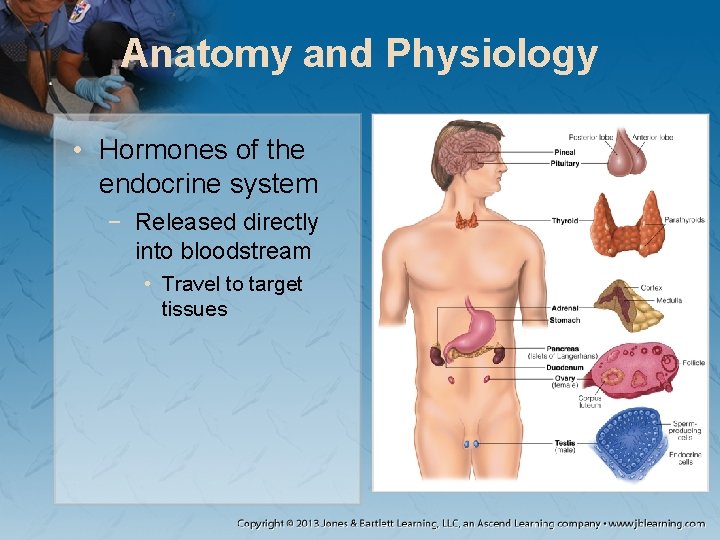
Anatomy and Physiology • Hormones of the endocrine system − Released directly into bloodstream • Travel to target tissues

Anatomy and Physiology • Agonists − Bind to a cell’s receptor − Trigger a response • Antagonists − Bind to a cell’s receptor − Block agonists

Mechanisms of Hormonal Regulation • Hormones operate within feedback systems to maintain an optimal operating environment. • Release of hormones is regulated by: − Chemical and other hormonal factors − Neural control

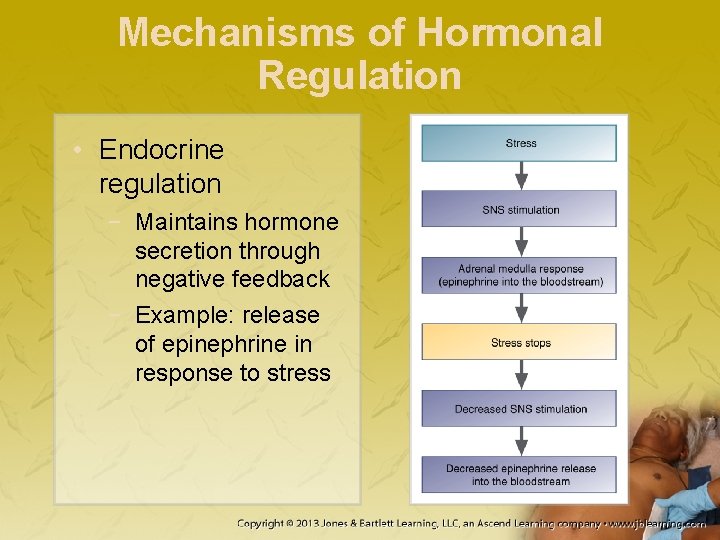
Mechanisms of Hormonal Regulation • Endocrine regulation − Maintains hormone secretion through negative feedback − Example: release of epinephrine in response to stress

Mechanisms of Hormonal Regulation • Disease − Normal cell signaling is interrupted. − Positive feedback is given. − System stops providing negative feedback to regulate function.

Mechanisms of Hormonal Regulation • The hypothalamus and pituitary gland − Related through the vascular system − Hypothalamic–pituitary system controls peripheral endocrine organs − Hypothalamus produces its own regulatory hormones

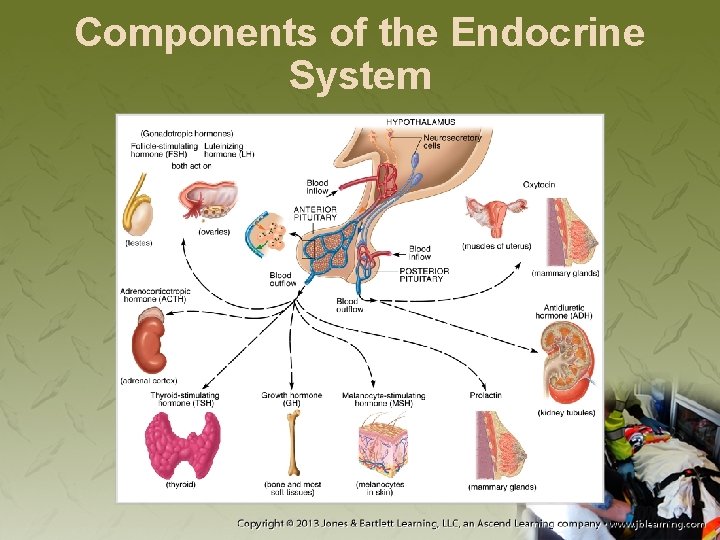
Components of the Endocrine System • Hypothalamus − Small region of the brain − Helps control body functions and emotions − Links endocrine and nervous systems

Components of the Endocrine System • Pineal gland − Located in the posterior of the brain’s third ventricle − Synthesizes and secretes melatonin

Components of the Endocrine System • Pituitary gland − Secretions control other glands − Located at the base of the brain − Two lobes: anterior and posterior

Components of the Endocrine System

Components of the Endocrine System • Thyroid gland − Secretes thyroxine • Stimulates energy production in cells − Secretes calcitonin • Helps maintain calcium levels in the blood

Components of the Endocrine System • Thymus gland − Helps identify and destroy foreign intruders − Lymphocytes: white blood cells that assist with immunity • Killer T cells • Helper T cells • Suppressor T cells

Components of the Endocrine System • Parathyroid glands − Help regulate calcium − Secrete PTH when blood calcium is low • PTH decreases calcium released in urine.

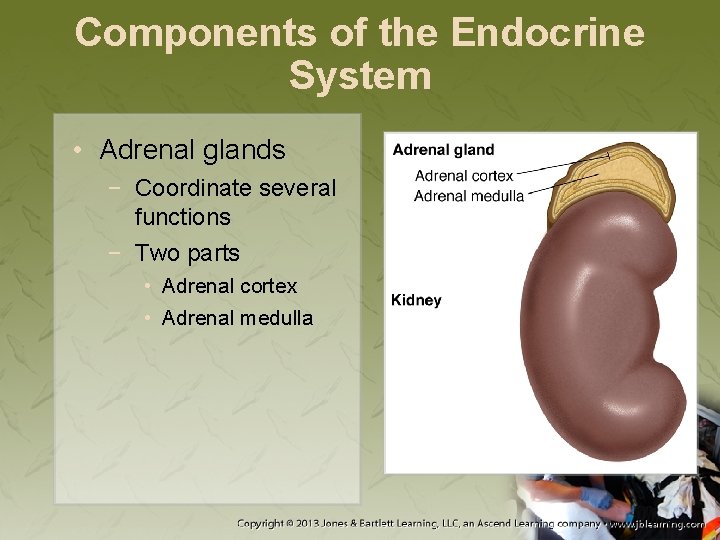
Components of the Endocrine System • Adrenal glands − Coordinate several functions − Two parts • Adrenal cortex • Adrenal medulla

Components of the Endocrine System • Adrenal glands (cont’d) − Both parts produce different hormones.

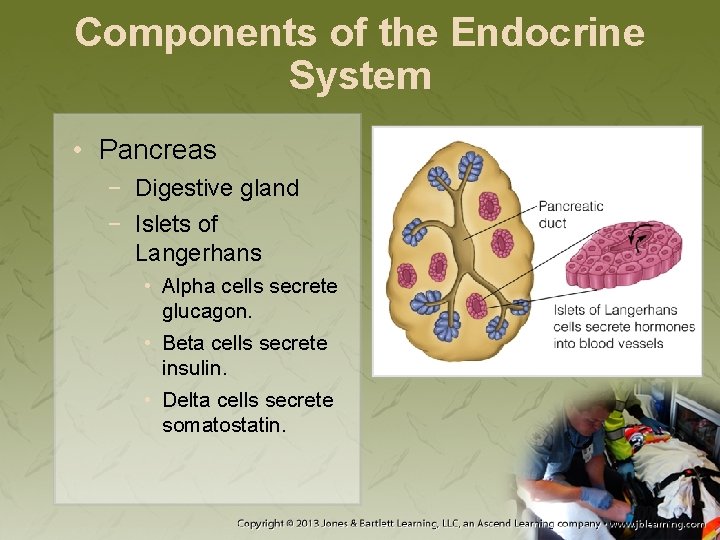
Components of the Endocrine System • Pancreas − Digestive gland − Islets of Langerhans • Alpha cells secrete glucagon. • Beta cells secrete insulin. • Delta cells secrete somatostatin.

Components of the Endocrine System • Pancreas (cont’d) − When blood glucose level falls, glucagon is secreted. − When blood glucose level rises, insulin is secreted.

Components of the Endocrine System • Gonads − Main source of sex hormones • Testes in men • Ovaries in women

Patient Assessment • Endocrine emergencies tend to affect many organ systems. − Do not take endocrine emergencies lightly.

Scene Size-Up • Address hazards. • Follow standard precautions. • Check the home for medications.

Primary Assessment • Identify and manage life threats. • Form a general impression. − Signs and symptoms depend on affected hormone. − Position may indicate severity of the condition. − Diaphoresis is a sign of severe distress.

Primary Assessment • Airway and breathing − Ensure a patent airway. − Investigate abnormal breathing sounds. − Administer oxygen if the rate is: • Greater than 24 breaths/min • Less than 8 breaths/min

Primary Assessment • Circulation − Assess skin color, moisture, and temperature. − Obtain blood pressure. − If necessary: • Administer IV. • Replenish blood component.

Primary Assessment • Transport decision − Many patients should be transported to a specialty facility. − Provide rapid transport to the closest facility if the patient is unstable.

History Taking • Consider signs and symptoms. − Undiagnosed or poorly managed diabetes may include: • Polyphagia • Polyuria • Polydipsia

History Taking • Ascertain any allergies prior to administering medication. • Document all medications being taken. • Ask females about their LMP.

Secondary Assessment • Physical exam − Observe appearance and position. − Identify atypical findings. − Finer abnormalities will help determine treatment.

Secondary Assessment • Goals with comatose patients: − Determine level of consciousness. − Look for the source of coma.

Secondary Assessment • Vital signs − Look for hypertension and bradycardia. − Be alert for abnormal respiratory patterns. − Look for pararespiratory motions.

Reassessment • Continually reassess the patient. − Critical patients at least every 5 minutes − Noncritical every 15 minutes • Manage ABCs. • Obtain blood specimens early in patients with diabetes.

Reassessment • Altered mental status − Establish either: • An IV with 0. 9% NS • A saline lock − Immediately determine blood glucose level. • Initiate treatment if less than 60 mg/d. L.

Reassessment • Provide emotional support. • Monitor comatose patient’s cardiac rhythm. • Recheck vital signs, pupils, and level of consciousness every 5– 15 minutes. • Record findings accurately and thoroughly.

Emergency Medical Care • Transport for comatose patients − Intubated: supine with cervical collar − Not intubated: stable side position − Increasing intracranial pressure: head elevated to 30– 45 degrees and midline

Glucose Metabolic Derangements • Endocrine disorders are caused by: − Hypersecretion of a gland − Insufficient secretion of a gland • Glucose metabolic derangements − Caused by dysfunction of the pancreas

Glucose Metabolic Derangements • Most endocrine emergencies result in: − − Compromise of the ABCs Improper fluid balance Deteriorating mental status Abnormal vital signs and blood glucose levels

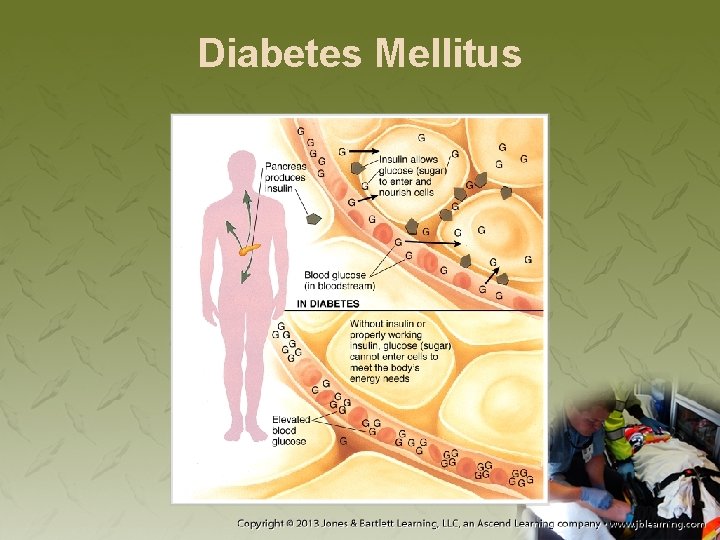
Diabetes Mellitus • Impaired ability to metabolize glucose • Characterized by • Polyphagia • Polydipsia • Polyuria • Glucose: fuel for cellular metabolism

Diabetes Mellitus • Insulin assists in: − Metabolism of carbohydrates − Transport of glucose into the cells • Patients have a flaw in production or function of insulin.

Diabetes Mellitus

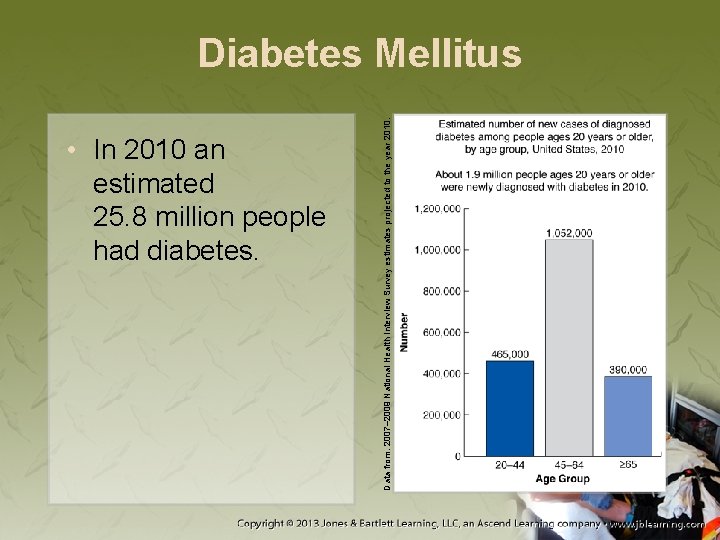
• In 2010 an estimated 25. 8 million people had diabetes. Data from: 2007– 2009 National Health Interview Survey estimates projected to the year 2010. Diabetes Mellitus

Life-Altering Complications from Diabetes • Kidney failure − Glomeruli become sclerotic. • Necrosis of the papillary tissue • Nephropathy • Renal failure • Heart disease or stroke − Lipolysis raises fat level in the blood. • Increased risk of atherosclerosis and coronary artery disease − Microangiopathy restricts blood flow

Life-Altering Complications from Diabetes • Cerebrovascular disease, stroke, and hypertension − Microangiopathy is associated with cerebrovascular disease, stroke − Hypertension is often present. • Eyes − High blood glucose levels damage vessels. − Cataracts form from fructose and sorbitol in the lens.

Life-Altering Complications from Diabetes • Neuropathy − Often affects peripheral nerves • Diminished sensation and function in the extremities • Many conditions can be delayed or prevented with lifestyle changes and continued management.

Type 1 Diabetes Mellitus • Pathophysiology − − Generally affects children Environmental factors may be part of the cause. Islets of Langerhans do not produce insulin. Daily insulin is required by injection or pump.

Type 1 Diabetes Mellitus • Assessment − Assess compliance with disease management. − With altered mental status, suspect low blood glucose level. − Look for sores or infections.

Type 1 Diabetes Mellitus • Management − Some patients use an insulin pump. • Alternative to injections • Controls blood glucose levels − Several types of insulin are available.

Type 2 Diabetes Mellitus • Pathophysiology − − Blood glucose levels are elevated. Typically develops later in life May be related to metabolic syndrome Many with the disease are insulin resistant.

Type 2 Diabetes Mellitus • Assessment − Symptoms may include: • • • Frequent urination Thirst Blurred vision Frequent infections Unresponsiveness

Type 2 Diabetes Mellitus • Management − − Weight loss helps to control the disease. Food intake must be spread throughout the day. Medication/insulin required daily. Oral medications are used with some patients.

Gestational Diabetes • Pathophysiology − − Form of glucose intolerance during pregnancy Increases risk of type 2 diabetes Resolves before delivery for most women May result in large babies

Gestational Diabetes • Assessment − High levels of glucose in the fetus cause increased production of insulin. − Often requires cesarean sections • Management − Stabilize blood glucose levels. − Diet, exercise, blood glucose testing

Hypoglycemia • Pathophysiology − In persons with insulin-dependent diabetes, often results from: • Too much insulin • Too little food • Both

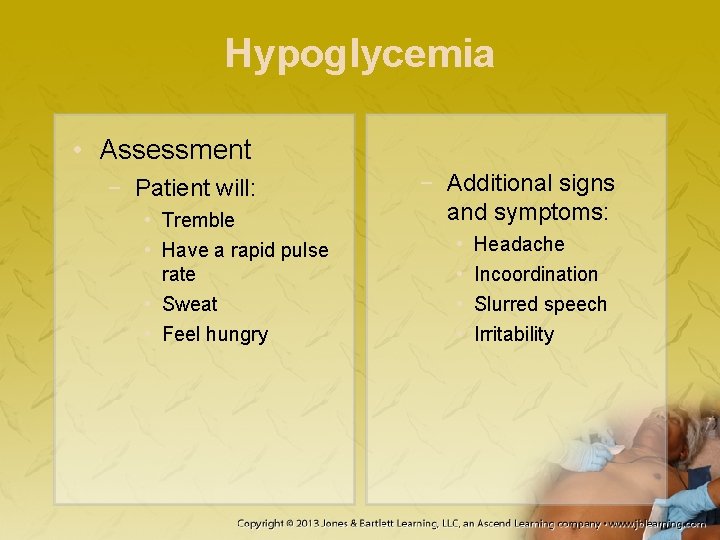
Hypoglycemia • Assessment − Patient will: • Tremble • Have a rapid pulse rate • Sweat • Feel hungry − Additional signs and symptoms: • • Headache Incoordination Slurred speech Irritability

Hypoglycemia • Assessment (cont’d) − Blood glucose level drops to 45 mg/d. L or less − Suspect in any diabetic patient with: • Bizarre behavior • Neurologic signs • Coma

• Management − Treat immediately. − Measure blood glucose. − Administration of glucose with stroke may exacerbate cerebral damage. Courtesy of Paddock Laboratories, Inc. Hypoglycemia

Hypoglycemia • Management (cont’d) − Rule out hypoglycemia with a field glucose test. − Administer sugar if alert and able to swallow. − Do not use an advanced airway until you have given the patient D 50. • 12. 5 to 25 g, over at least 3 minutes

Hypoglycemia • Management (cont’d) − Administer glucagon IM if you cannot obtain IV access. − Type 1 diabetes requires oral carbohydrates or additional glucose administration.

Hyperglycemia and Diabetic Ketoacidosis • Pathophysiology − Hyperglycemia: classic symptom of diabetes • Early signs: excessive thirst and urination • Occurs when blood glucose exceeds 120 mg/d. L • Onset may be rapid or gradual.

• Pathophysiology (cont’d) − Untreated hyperglycemia will progress to DKA. • Occurs when certain acids accumulate because insulin is not available Courtesy of Leonard Crowley Hyperglycemia and Diabetic Ketoacidosis

Hyperglycemia and Diabetic Ketoacidosis • Assessment − Hyperglycemia usually progresses slowly. − Patients in DKA are seldom deeply comatose. − Rely on clinical presentation.

Hyperglycemia and Diabetic Ketoacidosis • Assessment (cont’d) − Signs and symptoms of DKA include: • Polyuria, polydipsia, polyphagia • Fruity odor on the breath • Abdominal pain

Hyperglycemia and Diabetic Ketoacidosis • Management − Insulin therapy may be delivered at the hospital. − Monitor cardiac rhythm. • Sharply peaked T waves may require administration of sodium bicarbonate. • Sine wave may require administration of calcium chloride or gluconate.

Hyperosmolar Nonketotic (HONK) Coma • Pathophysiology − Occurs primarily with type 2 diabetes − Characterized by • Hyperglycemia • Hyperosmolarity • Absence of significant ketosis

Hyperosmolar Nonketotic (HONK) Coma • Assessment − Patients do not experience ketoacidosis. − Most have a history of diabetes. − Neurologic changes possible, such as: • Drowsiness and lethargy • Delirium and coma • Focal or generalized seizures

Hyperosmolar Nonketotic (HONK) Coma • Management − Address dehydration and altered mental status. − A bolus of NS is appropriate for nearly all who are clinically dehydrated. − Administer D 50 if the glucose level is less than 60 to 80 mg/d. L.

Pancreatitis • Pathophysiology − Inflammation of the pancreas • Acute form is a medical emergency • Chronic form is a progressive disease

Pancreatitis • Assessment − Patient may present with: • Flank and/or epigastric pain • Nausea and vomiting • Abdominal distention − Organ failure may develop.

Pancreatitis • Management − − Most are managed with supportive care. Transport patients. Pain management may be considered. Lifestyle changes are critical for chronic pancreatitis.

Adrenal Insufficiency • Decreased function of the adrenal cortex − Underproduction of cortisol and aldosterone • Results in weakness, dehydration, inability to maintain blood pressure • Usually well tolerated

Primary Adrenal Insufficiency (Addison Disease) • Pathophysiology − Both adrenal glands atrophied or destroyed • Leads to deficiency of steroid hormones − Occurs when 90% of the adrenal cortex has been destroyed

Primary Adrenal Insufficiency (Addison Disease) • Assessment − Signs of chronic disease include: • • • Fatigue Anorexia Salt craving Muscle, joint pain Increased pigmentation

Primary Adrenal Insufficiency (Addison Disease) • Assessment (cont’d) − Blood volume and pressure fall. − Sodium concentration of the blood falls. − Blood potassium rises.

Primary Adrenal Insufficiency (Addison Disease) • Management − Assess and manage ABCs. − Initiate aggressive fluid replacement. − Hydrocortisone is indicated in the acute management of a crisis.

Secondary Adrenal Insufficiency • Pathophysiology − Characterized by a lack of ACTH secretion from the pituitary gland − May result if a patient abruptly stops taking corticosteroids

Secondary Adrenal Insufficiency • Assessment − May appear suddenly (addisonian crisis) − Chief manifestation is shock − Symptoms may also include: • Confusion • Low blood pressure • Severe pain and/or vomiting

Secondary Adrenal Insufficiency • Management − Maintain ABCs, and have suction ready. − Rehydrate and correct abnormalities. − Check glucose level and cardiac rhythm.

Cushing Syndrome • Pathophysiology − Excess cortisol production or use of corticosteroid hormones − Characteristic changes: • Blood glucose level rises. • Protein synthesis is impaired. • Bones become weaker.

Cushing Syndrome • Assessment − Signs and symptoms include: • • Weakness and fatigue Increased thirst and urination Low blood glucose Thinning and/or darkening of the skin

Cushing Syndrome • Management − Assess and manage ABCs. − Prehospital treatment is generally supportive. − Obtain blood glucose level, and administer D 50 if indicated.

Adrenal Gland Tumor • Pheochromocytoma − Usually in the medulla − Causes excessive release of hormones − Combination of symptoms is common

Congenital Adrenal Hyperplasia (CAH) • Inadequate production of cortisol and aldosterone − Signs may include • Enlarged vagina in female infants • Signs of puberty in male infants • Short stature and severe acne

Congenital Adrenal Hyperplasia (CAH) • Usually requires cortisol and/or aldosterone replacement therapy • Surgery can correct genital deformities. • Dexamethasone may be prescribed to a pregnant woman if diagnosed.

Hypothyroidism and Hyperthyroidism • Anterior pituitary gland secretes thyroid-stimulating hormone (TSH). • Likely to require supplemental oxygen

Graves Disease • Most common cause of hyperthyroidism • Autoimmune disorder in which the thyroid gland hypertrophies as its activity increases − Produces a visible mass in the neck. − Excessive amount of thyroxine is secreted

Hashimoto Disease • Cause of hyperthyroidism − Result of the infiltration of T lymphocytes and plasma cells • Autoimmune disorder that affects TSH receptors

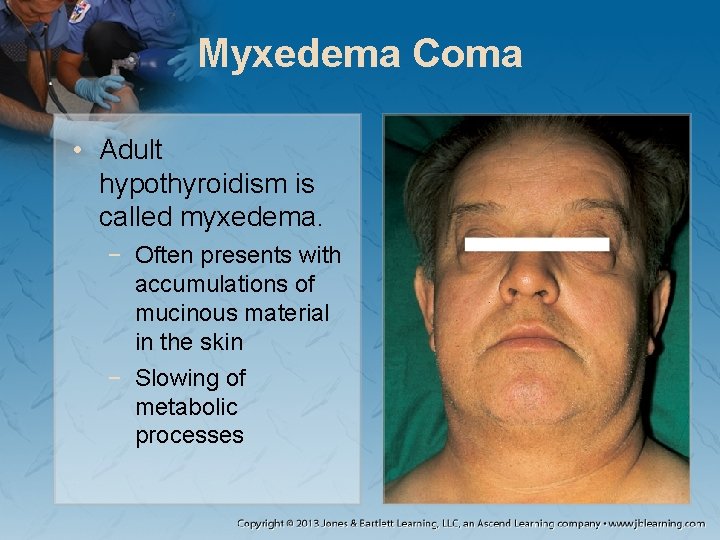
Myxedema Coma • Adult hypothyroidism is called myxedema. − Often presents with accumulations of mucinous material in the skin − Slowing of metabolic processes

Myxedema Coma • Symptoms − Severity is consistent with degree of deficiency. − May include: • Fatigue • Feeling cold • Dry skin

Myxedema Coma • Dropping hormone levels may lead to myxedema coma. − Often precipitated by triggers − Hallmark is deterioration of mental status − Consistent finding is hypothermia

Myxedema Coma • Supplemental oxygen for hypoxia • Intubation, ventilation may be indicated • Monitor cardiac status. • Passive rewarming for hypothermia • Avoid sedatives, narcotics, anesthetics

Thyrotoxicosis • Caused by excessive levels of circulating thyroid hormone • Causes may include: − Hyperthyroidism − Goiters − Autoimmune disorders

Thyroid Storm • Rare, life threatening • Signs and symptoms may include: − − Normal signs, symptoms of hyperthyroidism Fever Severe tachycardia Vomiting

Hyperparathyroidism • Increased parathyroid hormone level − Primary causes result from the gland − Secondary causes occur elsewhere • Most common cause is adenoma.

Hyperparathyroidism • Signs and symptoms − Can be vague − May include fatigue, weakness, vomiting • Definitive management: remove gland • Manage ABCs, provide supportive care

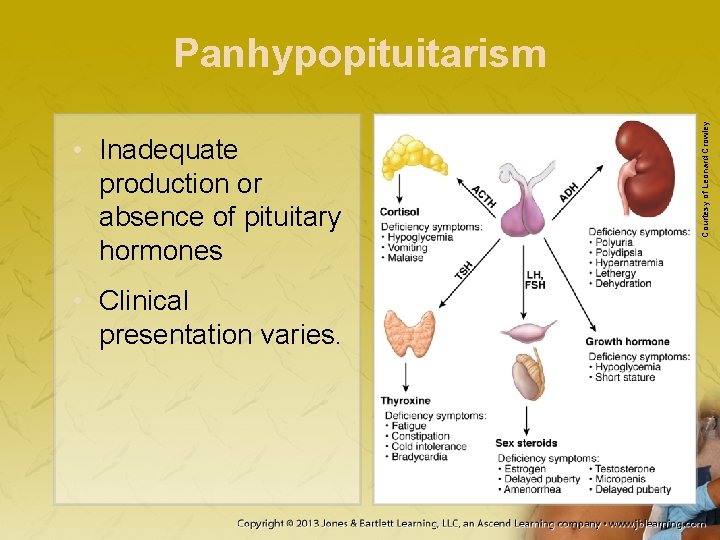
• Inadequate production or absence of pituitary hormones • Clinical presentation varies. Courtesy of Leonard Crowley Panhypopituitarism

Diabetes Insipidus • Unable to regulate fluid due to: − Lack of ADH (central diabetes insipidus) − Kidneys unable to respond appropriately (nephrogenic diabetes insipidus) • Management may include synthetic ADH.

Inborn Errors of Metabolism • Hereditary diseases • Cannot transform food to energy • Two categories of disorders − Toxic accumulations − Energy production or utilization

Summary • The endocrine system influences almost every cell, organ, and function. • Patients exhibit a range of signs and symptoms. Avert life threats with thorough assessment and immediate treatment.

Summary • The endocrine system is a network of glands that produce and secrete hormones. Its main function is to maintain homeostasis and promote structural changes. • Hormones travel through the bloodstream to target tissues.

Summary • The major components of the endocrine system are the hypothalamus, pineal gland, pituitary, thyroid, thymus, parathyroid, adrenals, pancreas, and reproductive organs. • The hypothalamus links the endocrine and nervous systems. • The pineal gland synthesizes and secretes melatonin.

Summary • The secretions of the pituitary gland regulate other endocrine glands. • Thyroid secretes thyroxine, which stimulates energy production in cells. It also secretes calcitonin, which helps maintain blood calcium levels. • The thymus gland helps the immune system identify and destroy pathogens and disrupt pathogenic processes.

Summary • Three types of T cells evolve in the thymus and help the lymphatic system defend against pathogens: killer T cells, helper T cells, and suppressor T cells. • The parathyroid gland secretes parathyroid hormone, which helps regulate blood calcium levels.

Summary • The adrenal glands consist of the cortex and the medulla. They produce hormones that help regulate metabolism, the balance of salt and water, the immune system, and sexual function. • The pancreas secretes digestive enzymes and the hormones glucagon and insulin. • Gonads include testes and ovaries. They are the main source of sex hormones.

Summary • The testes are in the scrotum and produce androgens, including testosterone, which regulates sexual development. • The ovaries release eggs and secrete estrogen and progesterone, which regulate sexual development and help regulate the menstrual cycle and pregnancy.

Summary • With diabetes the ability to metabolize glucose is impaired. • Endocrine emergencies affect many organ systems. Poor outcomes can result quickly. • Most patients with type 1 diabetes do not produce insulin and require daily injections. • When checking vital signs, watch for increased intracranial pressure, unusual breathing patterns, and pararespiratory motions.

Summary • Management of an endocrine emergency may require intubation, supplemental oxygen, or infusion of dextrose. • In type 1 diabetes, the beta cells in the islets of Langerhans no longer produce insulin. Blood glucose must be monitored and insulin administered daily.

Summary • The most common form of diabetes is type 2 diabetes. • Hypoglycemia in a person with insulindependent diabetes is often the result of too much insulin, too little food, or both. • Hyperglycemia is a classic symptoms of diabetes mellitus. • Untreated hyperglycemia will progress to diabetic ketoacidosis.

Summary • HONK/HHNC is a metabolic derangement that occurs principally with type 2 diabetes. • Gestational diabetes is a form of glucose intolerance during pregnancy. • Primary adrenal insufficiency (Addison disease) is caused by atrophy or destruction of both adrenal glands, leading to deficiency of the hormones they produce.

Summary • Secondary adrenal insufficiency is a lack of adrenocorticotropic hormone secretion from the pituitary gland. • Acute adrenal insufficiency is called an addisonian crisis and may result from an acute exacerbation of chronic insufficiency. • Cushing syndrome is caused by excess cortisol production or by excessive use of corticosteroid hormones.

Summary • Pheochromocytoma is an adrenal gland tumor that causes excessive release of epinephrine and norepinephrine. • With congenital adrenal hyperplasia, the adrenal gland produces insufficient cortisol and aldosterone. • Thyroid hormones are critical for cell metabolism and organ function.

Summary • Graves disease is the most severe and common cause of hyperthyroidism. • Hashimoto disease is an autoimmune disease in which the thyroid gland is enlarged. • Continued decrease of thyroid hormone levels may lead to myxedema coma.

Summary • In a myxedema coma, reduced or absent thyroid hormone slows metabolic processes. • Thyrotoxicosis is caused by excessive levels of circulating thyroid hormone. A thyroid storm may occur with thyrotoxicosis. • In hyperparathyroidism, blood calcium levels increase.

Credits • Chapter opener: © Mark Humphrey/AP Photos • Backgrounds: Blue—Jones & Bartlett Learning. Courtesy of MIEMSS; Gold—Jones & Bartlett Learning. Courtesy of MIEMSS; Red—© Margo Harrison/Shutter. Stock, Inc. ; Green—Courtesy of Rhonda Beck. • Unless otherwise indicated, all photographs and illustrations are under copyright of Jones & Bartlett Learning, courtesy of Maryland Institute for Emergency Medical Services Systems, or have been provided by the American Academy of Orthopaedic Surgeons.