Chapter 21 Burns Copyright 2017 Elsevier Inc All

Chapter 21 Burns Copyright © 2017 Elsevier Inc. All rights reserved.

Quick Quiz! Approximately how many burn injuries require acute hospitalization annually in the United States? 28, 000 B. 40, 000 C. 63, 000 D. 92, 000 A. Copyright © 2017 Elsevier Inc. All rights reserved. 2

Introduction Initial management affects long-term outcome Burn centers Multiprofessional team approach Highest morbidity Burns covering more than 50% of body surface area Ø Inhalation injuries Ø Very young and elderly patients Ø Copyright © 2017 Elsevier Inc. All rights reserved. 3

Integumentary System Skin composed of two layers Epidermis Ø Dermis Ø Subcutaneous fat tissue layer Copyright © 2017 Elsevier Inc. All rights reserved. 4
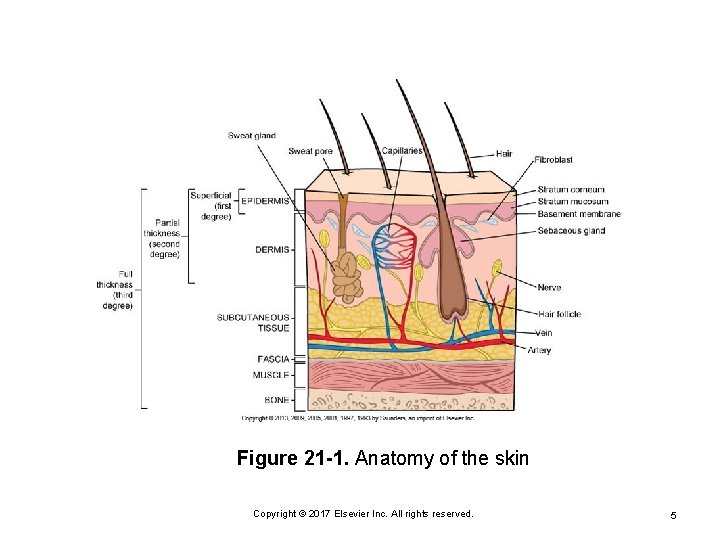
Figure 21 -1. Anatomy of the skin Copyright © 2017 Elsevier Inc. All rights reserved. 5

Integumentary System Functions Protection from infection Prevention of loss of body fluids Thermoregulation Production of vitamin D Excretion Determination of identity Sensation reception Copyright © 2017 Elsevier Inc. All rights reserved. 6

Effects of Aging Flattened dermal-epidermal junction Dermal and subcutaneous atrophy Reduced microcirculation Consequence is thinned skin, predisposition to deeper burns, and delayed or poor healing Complicated by decreased ability to tolerate burn stress Copyright © 2017 Elsevier Inc. All rights reserved. 7

Mechanisms of Burn Injury Thermal Chemical Electrical Inhalation injury Ø 20% to 50% Copyright © 2017 Elsevier Inc. All rights reserved. 8

Thermal Injury Skin damaged by contact with heat Flame Ø Scalding liquids Ø Heat source Ø Copyright © 2017 Elsevier Inc. All rights reserved. 9

Thermal Injury (Cont. ) Severity of injuries Duration of contact Ø Temperature of agent • ↑Risk of injury temperature > 40° C (104° F) Ø Amount of tissue exposed Ø Age of patient Ø Copyright © 2017 Elsevier Inc. All rights reserved. 10

Quick Quiz! What is the average temperature of a water heater? 100° F B. 120° F C. 140° F D. 160° F A. Copyright © 2017 Elsevier Inc. All rights reserved. 11

Critical Thinking Challenge What are examples of thermal injury? Why are the young and elderly at increased risk? Copyright © 2017 Elsevier Inc. All rights reserved. 12

Chemical Injury Methods of injury Contact Ø Inhalation of fumes Ø Ingestion or injection Ø Copyright © 2017 Elsevier Inc. All rights reserved. 13

Chemical Injury (Cont. ) Systemic and local effects Must be completely removed or neutralized or damage continues Material Safety Data Sheets (MSDSs) Copyright © 2017 Elsevier Inc. All rights reserved. 14

Chemical Injury (Cont. ) Severity of injuries Type of agent Ø Volume of agent Ø Duration of contact Ø Concentration of agent Ø Types Alkalies Ø Acids Ø Organic compounds Ø Copyright © 2017 Elsevier Inc. All rights reserved. 15

Chemical Injury (Cont. ) Methamphetamine-related chemical burn injury Ø Clandestine “laboratories” Thermal and chemical burn injury pattern Assess for: A vague or inconsistent injury history Ø Burns to the face and hands Ø Signs of agitation or substance withdrawal Ø Copyright © 2017 Elsevier Inc. All rights reserved. 16

Electrical Injuries High versus low voltage High > 1000 volts Ø Low < 1000 volts Ø Energy is converted into heat AC versus DC Ø AC higher probability of producing cardiac arrest Copyright © 2017 Elsevier Inc. All rights reserved. 17

Electrical Injuries (Cont. ) Factors Type and path of current Ø Duration of contact Ø Environmental • Lightning strikes Ø Tissue resistance Ø Copyright © 2017 Elsevier Inc. All rights reserved. 18

Inhalation Injury Inhalation of hot smoke, chemical toxins, and products of incomplete combustion Carbon monoxide and cyanide poisoning Classified Systemic injury due to exposure to toxic gases Ø Supraglottic injury Ø Subglottic injury Ø Copyright © 2013, 2009, 2005, 2001, 1997, 1993 by Saunders, an imprint of Elsevier Inc. 19

Burn Classification and Severity Type of burn injury Burn wound characteristics Depth Ø Extent Ø Body part burned Ø Concomitant injuries Patient age Pre-existing health status Copyright © 2017 Elsevier Inc. All rights reserved. 20
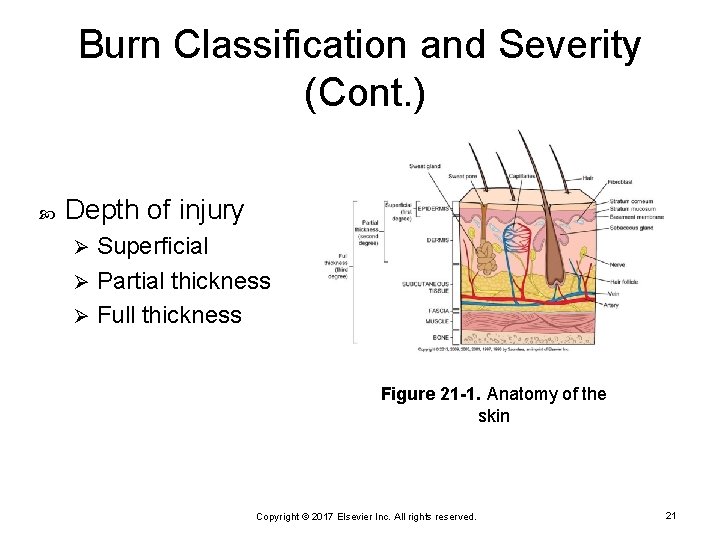
Burn Classification and Severity (Cont. ) Depth of injury Superficial Ø Partial thickness Ø Full thickness Ø Figure 21 -1. Anatomy of the skin Copyright © 2017 Elsevier Inc. All rights reserved. 21

Burn Classification and Severity (Cont. ) Superficial (first degree) Epidermis only or small depth of dermis Ø Heals in 3 to 5 days without treatment Ø Erythema Ø Not calculated for fluid resuscitation Ø Copyright © 2017 Elsevier Inc. All rights reserved. 22

Burn Classification and Severity (Cont. ) Partial thickness (second degree) Ø Epidermis and most of dermis Superficial partial thickness Epidermis and limited portion of the dermis Ø Heals in 7 to 10 days Ø Deep partial thickness Epidermis and most of dermis Ø Heals within 2 to 4 weeks Ø Copyright © 2017 Elsevier Inc. All rights reserved. 23

Burn Classification and Severity (Cont. ) Full thickness (third degree) Destruction of all layers down to or past fat, fascia, muscle, or bone Ø Thick, dry, leathery appearance Ø Insensate (no pain) Ø Copyright © 2017 Elsevier Inc. All rights reserved. 24

Quick Quiz! A 54 -year-old male was working on his car, and the carburetor exploded. He presents with singed nose hairs and red, painful blisters on his face and bilateral forearms and hands. What type and depth of burn injury do you suspect? A. B. C. D. Inhalation injury below the glottis with superficial burns Inhalation injury above the glottis with superficial partialthickness burns Deep partial-thickness burns and carbon monoxide poisoning Full-thickness burns and inhalation injury above the glottis Copyright © 2017 Elsevier Inc. All rights reserved. 25

Zones of Injury Zone of hyperemia Ø Zone of stasis Ø Potentially reversible damage Zone of coagulation Ø Minimal injury Greatest injury Goal: prevent secondary insults Copyright © 2017 Elsevier Inc. All rights reserved. 26
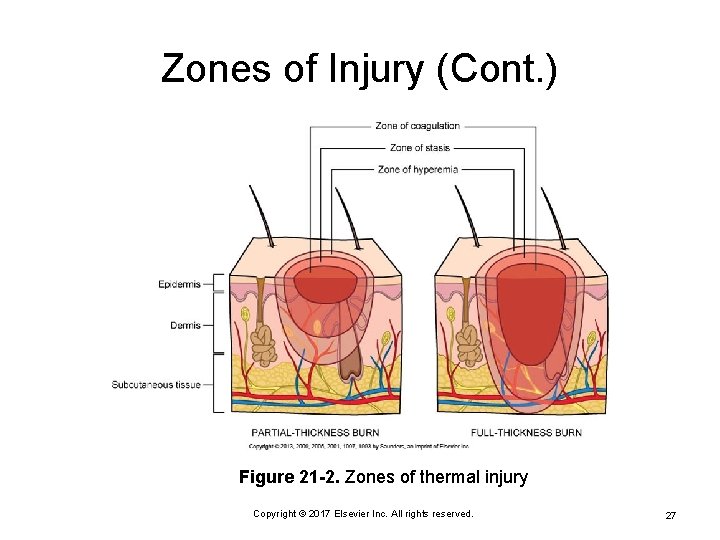
Zones of Injury (Cont. ) Figure 21 -2. Zones of thermal injury Copyright © 2017 Elsevier Inc. All rights reserved. 27

Extent of Injury Expressed as percentage of total body surface area (%TBSA) Several methods for estimating Rule of nines Ø Patient’s palm method Ø Lund and Browder chart Ø Differences between adults and children Copyright © 2017 Elsevier Inc. All rights reserved. 28
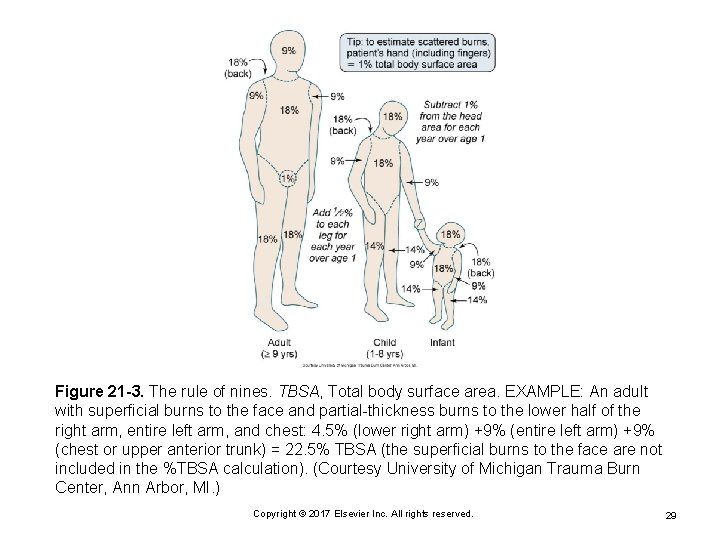
Figure 21 -3. The rule of nines. TBSA, Total body surface area. EXAMPLE: An adult with superficial burns to the face and partial-thickness burns to the lower half of the right arm, entire left arm, and chest: 4. 5% (lower right arm) +9% (entire left arm) +9% (chest or upper anterior trunk) = 22. 5% TBSA (the superficial burns to the face are not included in the %TBSA calculation). (Courtesy University of Michigan Trauma Burn Center, Ann Arbor, MI. ) Copyright © 2017 Elsevier Inc. All rights reserved. 29
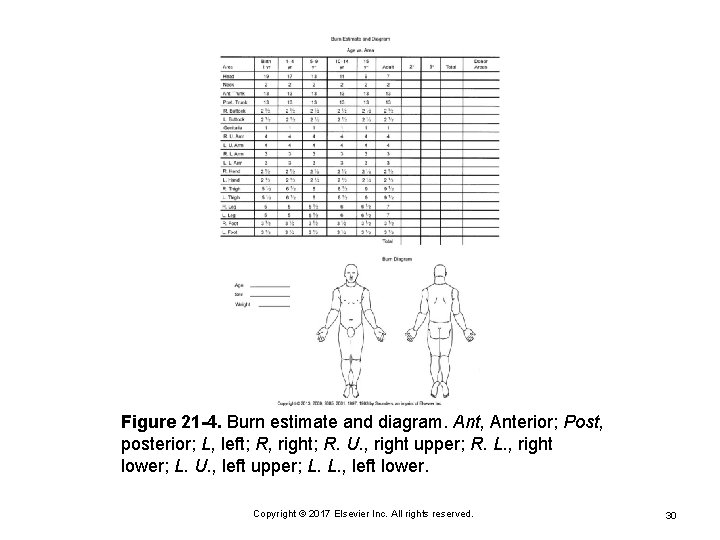
Figure 21 -4. Burn estimate and diagram. Ant, Anterior; Post, posterior; L, left; R, right; R. U. , right upper; R. L. , right lower; L. U. , left upper; L. L. , left lower. Copyright © 2017 Elsevier Inc. All rights reserved. 30

Physiological Response to Burns Acute inflammation Intravascular coagulation Cellular enzymes and vasoactive substances Activation of complement Altered vascular permeability Copyright © 2017 Elsevier Inc. All rights reserved. 31

Fluid Shifts Fluid shifts to extravascular space Burns greater than 20% total body surface area Ø Edema in burned and unburned areas Maximum edema 24 to 48 hours postburn Copyright © 2017 Elsevier Inc. All rights reserved. 32

Systemic Response to Burns Cardiovascular Loss of intravascular volume Ø Decreased cardiac output Ø Tachycardia and vasoconstriction Ø Loss of volume decreases cardiac output and oxygen delivery Ø Catecholamine release causes tachycardia and vasoconstriction Ø Myocardial depression with negative inotropic effect Ø Cardiac output increase 48 hours after injury leads to diuresis Ø Copyright © 2017 Elsevier Inc. All rights reserved. 33

Systemic Response to Burns (Cont. ) Host defense mechanisms Immune suppression Ø Increased risk of infection Ø Pulmonary hypertension Ø Effect of direct injury Ø Renal Sensitive to decreased cardiac output Ø Initial decrease in urine output related to decreased glomerular filtration rate Ø Followed by diuresis as fluids shift Ø Copyright © 2017 Elsevier Inc. All rights reserved. 34

Systemic Response to Burns (Cont. ) Gastrointestinal (GI) Ischemia due to redistribution of blood to brain and heart Ø Curling’s ulcers Ø Paralytic ileus Ø Metabolic Hypermetabolic state Ø Metabolic rates are 100% to 200% above basal rates Ø Lasts up to 9 to 12 months after burn Ø Copyright © 2017 Elsevier Inc. All rights reserved. 35

Phases of Burn Care Acute phase Onset of diuresis to wound closure Ø Approx. 48 -72 hours postinjury until wounds close Ø Rehabilitative phase Ø Restore to functional status Copyright © 2017 Elsevier Inc. All rights reserved. 36

Resuscitative Phase Prehospital Interventions Stop the burning process Identify life-threatening injuries ABCs and cervical spine Oxygen at 100%; intubation if needed Assess circulation Assess for additional trauma Minimize time on the scene Copyright © 2017 Elsevier Inc. All rights reserved. 37

Prehospital Interventions (Cont. ) Remove the patient from thermal source Cover and prevent hypothermia Remove jewelry, belts, and clothing that may retain heat Scalds, tar, asphalt burns: cool with water Copyright © 2017 Elsevier Inc. All rights reserved. 38

Prehospital Interventions (Cont. ) Large-bore IV catheters and fluids Pain management with narcotics Vital signs and baseline assessment Copyright © 2017 Elsevier Inc. All rights reserved. 39
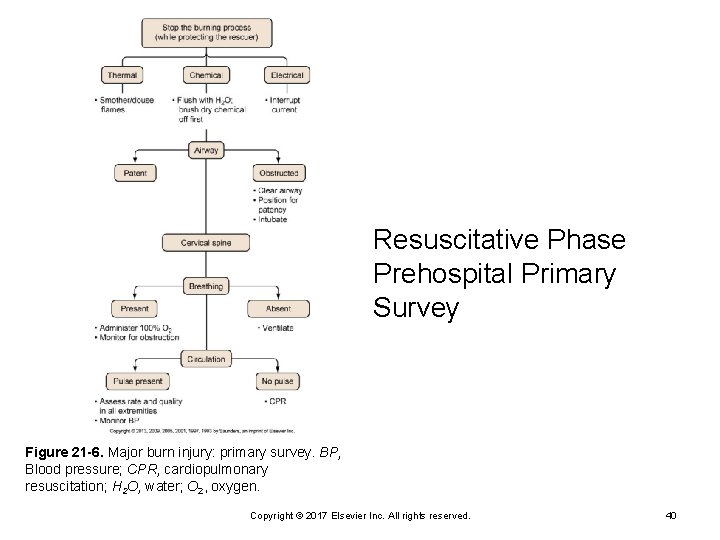
Resuscitative Phase Prehospital Primary Survey Figure 21 -6. Major burn injury: primary survey. BP, Blood pressure; CPR, cardiopulmonary resuscitation; H 2 O, water; O 2, oxygen. Copyright © 2017 Elsevier Inc. All rights reserved. 40

Assessment in Resuscitative Phase Respiratory Assess for hypoxemia Ø Carbon monoxide poisoning Ø Assess for direct injury Ø Maintain cervical spine precautions Ø Copyright © 2017 Elsevier Inc. All rights reserved. 41

Quick Quiz! What is an appropriate intervention in the prehospital setting in the management of an unconscious patient who was pulled from a house fire. His vital signs are BP 100/82 mm Hg, HR 122 beats/min, RR 26 breaths/min, Sp. O 2 100%. Monitor vital signs every 15 minutes. B. Cover the patient with warm blankets. C. Apply 100% humidified oxygen. D. Place the patient in a side-lying position. A. Copyright © 2017 Elsevier Inc. All rights reserved. 42

Critical Thinking Challenge What are cues for thermal injury to the airway? If tracheal edema is suspected, what is the best way to manage the airway? Copyright © 2017 Elsevier Inc. All rights reserved. 43

Assessment in Resuscitative Phase Cardiovascular Assess for fluid volume status Ø Vital signs Ø Prevent heat loss Ø Copyright © 2017 Elsevier Inc. All rights reserved. 44

Assessment in Resuscitative Phase (Cont. ) Neurological Ø Renal Ø Changes in level of consciousness Urine output GI Ø Assess for occult bleeding Copyright © 2017 Elsevier Inc. All rights reserved. 45

Assessment in Resuscitative Phase (Cont. ) Integumentary Document extent of injury Ø Measure severity of burn (rule of nines or patient’s palm method) Ø Psychosocial Assess response to injury Ø Pain assessment Ø Copyright © 2017 Elsevier Inc. All rights reserved. 46

Assessment in Resuscitative Phase (Cont. ) Monitor serum electrolytes Sodium Ø Potassium Ø Blood urea nitrogen Ø Glucose Ø Lactate Ø Copyright © 2017 Elsevier Inc. All rights reserved. 47

Critical Thinking Challenge Why is it important to remove all clothing and jewelry early? Why is it important to start IV lines immediately? Why is pain treated with IV narcotics? Copyright © 2017 Elsevier Inc. All rights reserved. 48

Emergency Department Interventions Primary survey Secondary survey ABCs and C-spine evaluation Chest and other x-rays Evaluation of TBSA and depth of burn injuries Calculation of fluid requirements Tetanus toxoid immunization Copyright © 2017 Elsevier Inc. All rights reserved. 49

Fluid Resuscitation Based on %TBSA IV fluid resuscitation is instituted for patients with greater than 20% TBSA Consensus formula (Parkland) Ø 4 m. L/kg per %TBSA burned Administer half of total fluids during first 8 hours from time of injury Administer the other half over the next 16 hours from time of injury Copyright © 2017 Elsevier Inc. All rights reserved. 50

Quick Quiz! Calculate the volume of IV fluid needed for the first 8 hours after burn injury: 60 years old, 82 kg, 42% TBSA. 3, 444 m. L B. 6, 888 m. L C. 13, 776 m. L D. 19, 456 m. L A. Copyright © 2017 Elsevier Inc. All rights reserved. 51

Fluid Guidelines for Adults Maintain urine output of 30 to 50 m. L/hr Place IV access in nonburned areas Hold colloids for 8 to 12 hours after injury Inhalation injury Copyright © 2017 Elsevier Inc. All rights reserved. 52

Fluid Guidelines: Electrical Patients with electrical injury need higher volumes of fluid Keep urine output at 75 to 100 m. L/hr Risk: myoglobinuria Copyright © 2017 Elsevier Inc. All rights reserved. 53

Peripheral Circulation Circumferential full-thickness burns Compartment syndrome Neurovascular assessment Ø Peripheral pulse assessment Ø Escharotomy or fasciotomy Copyright © 2017 Elsevier Inc. All rights reserved. 54

Intraabdominal Hypertension Circumferential torso injury Aggressive fluid resuscitation Intraabdominal pressure (IAP) ≥ 12 mm Hg Abdominal compartment syndrome Ø IAP ≥ 20 mm Hg Tense abdomen, decreasing urine output, hypoxia, hypercarbia Copyright © 2017 Elsevier Inc. All rights reserved. 55

Critical Thinking Challenge If fluid resuscitation was not started until 2 hours after the burn, how does that affect fluid administration? Copyright © 2017 Elsevier Inc. All rights reserved. 56
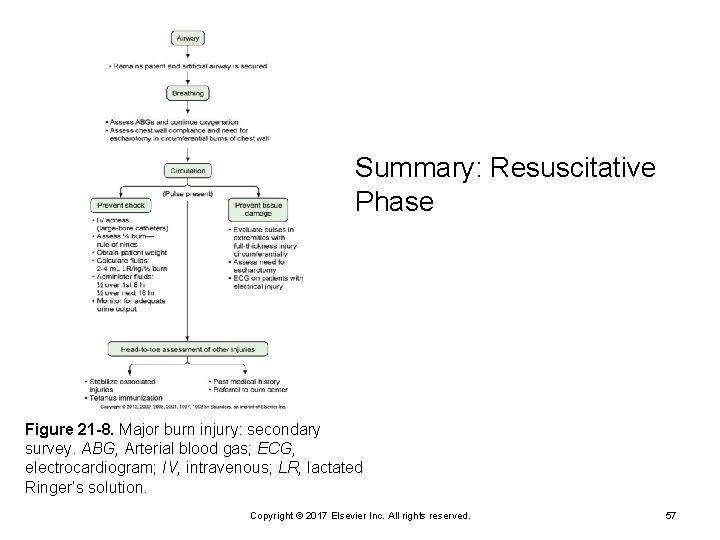
Summary: Resuscitative Phase Figure 21 -8. Major burn injury: secondary survey. ABG, Arterial blood gas; ECG, electrocardiogram; IV, intravenous; LR, lactated Ringer’s solution. Copyright © 2017 Elsevier Inc. All rights reserved. 57

Transfer to Burn Center Transfer patient to burn center early, according to criteria Partial thickness > 10% TBSA Ø Full-thickness burns Ø Burns on face, hands, feet, genitalia, perineum, and joints Ø Chemical and electrical Ø Inhalation Ø Comorbidities Ø Associated trauma Ø Copyright © 2017 Elsevier Inc. All rights reserved. 58

Acute Phase Begins 48 to 72 hours after injury Continue with assessments performed during resuscitative phase Focus of interventions is to: Ø Ø Ø Promote wound healing Prevent complications Improve function of body systems (systemic response to burn injury) Copyright © 2017 Elsevier Inc. All rights reserved. 59

Acute Phase Assessment Respiratory system Signs of respiratory compromise • Pneumonia • Acute respiratory failure/ARDS Ø Chest x-rays Ø Fever Ø Secretions Ø WBC count Ø Copyright © 2017 Elsevier Inc. All rights reserved. 60

Acute Phase Assessment (Cont. ) Cardiovascular Maintain fluid requirement Ø Monitor intake and output Ø Monitor weight Ø Neurological status Ø Changes in level of consciousness Renal status Ø Urine output Copyright © 2017 Elsevier Inc. All rights reserved. 61

Acute Phase Assessment (Cont. ) GI system Stress ulcer Ø Nutritional considerations Ø Integumentary system Wound healing Ø Infection Ø Copyright © 2017 Elsevier Inc. All rights reserved. 62

Acute Phase Assessment (Cont. ) Blood and electrolytes Fluid shifts Ø Electrolyte imbalances • Hemodilution: hemoglobin/hematocrit • Sodium • Potassium • Glucose • Serum protein • WBC • Coagulation studies • Acid-base balance Ø Copyright © 2017 Elsevier Inc. All rights reserved. 63

Acute Care Interventions Primary and secondary surveys Ongoing assessment Vital signs Ø Pulses Ø Urine output Ø Pulse oximetry Ø Copyright © 2017 Elsevier Inc. All rights reserved. 64

Acute Care Interventions (Cont. ) Hemodynamic monitoring Central venous line Ø Pulmonary artery catheter Ø Gastric p. H; occult blood Prevent hypothermia VTE prophylaxis Maintain joint function and mobility Copyright © 2017 Elsevier Inc. All rights reserved. 65

Critical Thinking Challenge List at least two interventions for ongoing monitoring related to the systems below: Respiratory Ø Cardiovascular Ø Renal Ø GI Ø Neurological Ø Copyright © 2017 Elsevier Inc. All rights reserved. 66

Special Concerns Facial burns: risk of respiratory injury; oral hygiene; promote healing Ears: prevent infection and breakdown Eyes: ophthalmology consult as needed; keep moist Copyright © 2017 Elsevier Inc. All rights reserved. 67

Special Concerns (Cont. ) Hands and feet or major joints: adequate circulation; maintain function Genitalia and perineum: meticulous wound care to prevent infection Copyright © 2017 Elsevier Inc. All rights reserved. 68
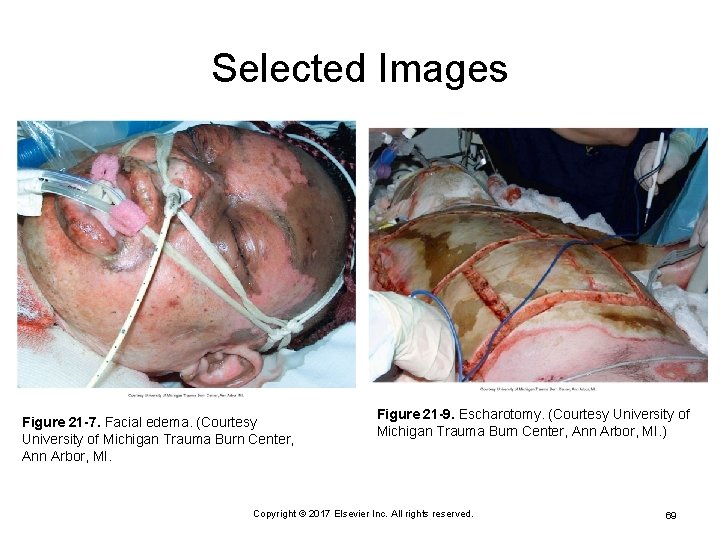
Selected Images Figure 21 -7. Facial edema. (Courtesy University of Michigan Trauma Burn Center, Ann Arbor, MI. Figure 21 -9. Escharotomy. (Courtesy University of Michigan Trauma Burn Center, Ann Arbor, MI. ) Copyright © 2017 Elsevier Inc. All rights reserved. 69

Abuse Vulnerable population Children Ø Geriatric Ø Disabled Ø Mentally impaired Ø Identification of potential cases Elicit history Ø Note wound appearance and pattern Ø Take photos Ø Observe interaction Ø Assess for other injuries Ø Copyright © 2017 Elsevier Inc. All rights reserved. 70
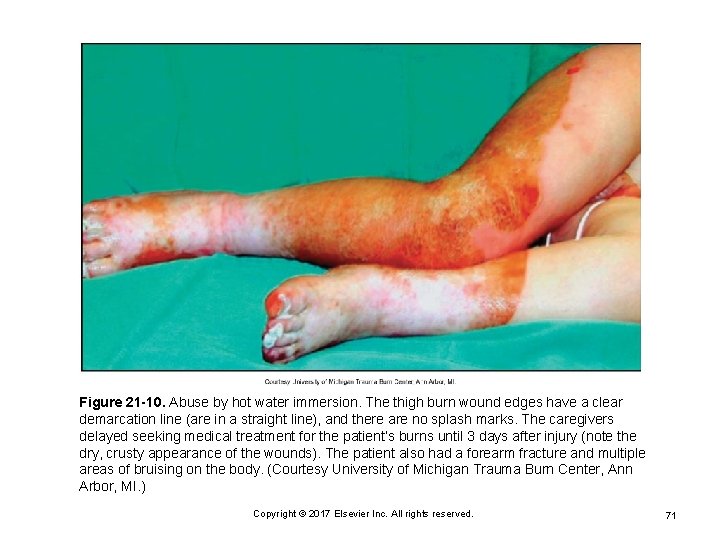
Figure 21 -10. Abuse by hot water immersion. The thigh burn wound edges have a clear demarcation line (are in a straight line), and there are no splash marks. The caregivers delayed seeking medical treatment for the patient’s burns until 3 days after injury (note the dry, crusty appearance of the wounds). The patient also had a forearm fracture and multiple areas of bruising on the body. (Courtesy University of Michigan Trauma Burn Center, Ann Arbor, MI. ) Copyright © 2017 Elsevier Inc. All rights reserved. 71

Pain Control Adequate, accurate assessment tools Opiates; IV route PCA may be useful Nonpharmacological strategies Copyright © 2017 Elsevier Inc. All rights reserved. 72

Critical Thinking Challenge Identify three procedures that can increase pain in the patient with burns. When should pain medication be administered to prevent pain? Copyright © 2017 Elsevier Inc. All rights reserved. 73

Infection Prevention Burn patient at high risk for infection Higher risk with 30% TBSA burns Ø Altered skin integrity Ø Altered immune response (immunosuppression) Ø Multidrug-resistant organisms Ø Multiple invasive monitoring and treatment procedures Ø Copyright © 2017 Elsevier Inc. All rights reserved. 74

Wound Care Remove nonviable tissue Promote re-epithelialization and wound healing Cover the burned area; graft as needed Copyright © 2017 Elsevier Inc. All rights reserved. 75

Wound Care (Cont. ) Prewarm room prior to wound care Clean and debride wounds Hydrotherapy Application of antimicrobial agents Silver-based agents Ø See Table 21 -4 Ø Open versus closed method Copyright © 2017 Elsevier Inc. All rights reserved. 76

Wound Care (Cont. ) Various types of biological and biosynthetic dressings Biological Dressings: Allograft (homograft) and xenograft (heterograft) Ø Biosynthetic Dressing: Ø Epidermal replacements (Epicel, Epidex, My. Skin, etc. ) Ø Dermal substitutes: Allo. Derm; Integra; Trans. Cyte Ø Bilayer dermo-epidermal substitutes (Apligraf, Or. Cel) Ø Copyright © 2017 Elsevier Inc. All rights reserved. 77
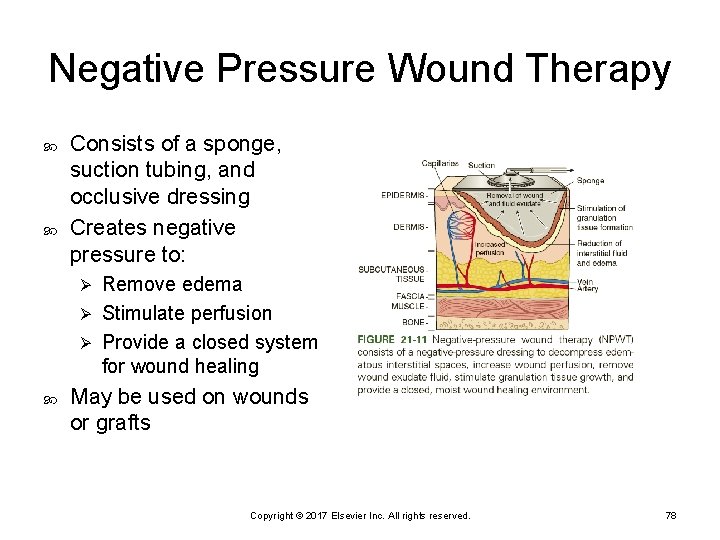
Negative Pressure Wound Therapy Consists of a sponge, suction tubing, and occlusive dressing Creates negative pressure to: Remove edema Ø Stimulate perfusion Ø Provide a closed system for wound healing Ø May be used on wounds or grafts Copyright © 2017 Elsevier Inc. All rights reserved. 78

Skin Grafts for deep partial-thickness and fullthickness burns Autograft is the only permanent method of grafting Ø Donor site created: surgical wound Homografts and xenografts Sheet (nonmeshed) grafts used on face and hands Meshed grafts Copyright © 2017 Elsevier Inc. All rights reserved. 79
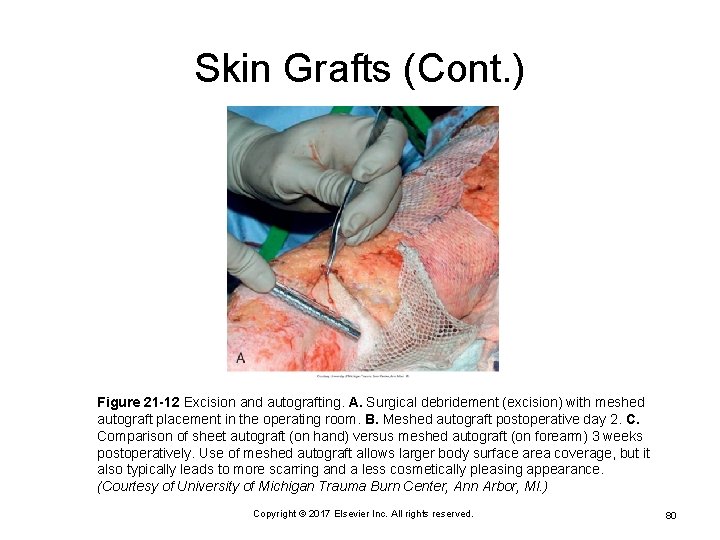
Skin Grafts (Cont. ) Figure 21 -12 Excision and autografting. A. Surgical debridement (excision) with meshed autograft placement in the operating room. B. Meshed autograft postoperative day 2. C. Comparison of sheet autograft (on hand) versus meshed autograft (on forearm) 3 weeks postoperatively. Use of meshed autograft allows larger body surface area coverage, but it also typically leads to more scarring and a less cosmetically pleasing appearance. (Courtesy of University of Michigan Trauma Burn Center, Ann Arbor, MI. ) Copyright © 2017 Elsevier Inc. All rights reserved. 80
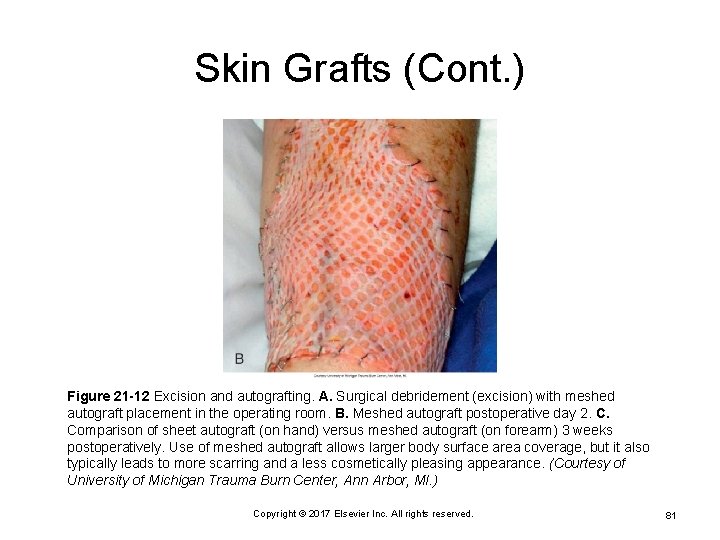
Skin Grafts (Cont. ) Figure 21 -12 Excision and autografting. A. Surgical debridement (excision) with meshed autograft placement in the operating room. B. Meshed autograft postoperative day 2. C. Comparison of sheet autograft (on hand) versus meshed autograft (on forearm) 3 weeks postoperatively. Use of meshed autograft allows larger body surface area coverage, but it also typically leads to more scarring and a less cosmetically pleasing appearance. (Courtesy of University of Michigan Trauma Burn Center, Ann Arbor, MI. ) Copyright © 2017 Elsevier Inc. All rights reserved. 81
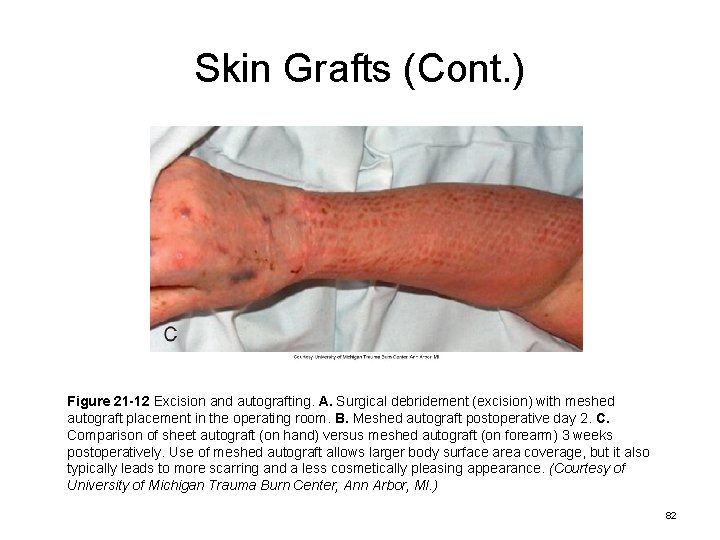
Skin Grafts (Cont. ) Figure 21 -12 Excision and autografting. A. Surgical debridement (excision) with meshed autograft placement in the operating room. B. Meshed autograft postoperative day 2. C. Comparison of sheet autograft (on hand) versus meshed autograft (on forearm) 3 weeks postoperatively. Use of meshed autograft allows larger body surface area coverage, but it also typically leads to more scarring and a less cosmetically pleasing appearance. (Courtesy of University of Michigan Trauma Burn Center, Ann Arbor, MI. ) 82

Nutritional Support Hypermetabolic-catabolic state Consult to determine caloric needs Early enteral nutrition warranted Beta-blockage and anabolic hormones Copyright © 2017 Elsevier Inc. All rights reserved. 83

Psychological Considerations Affects entire family Long-term effects Consider: Preinjury personality Ø Extent of injury Ø Social support system Ø Home environment Ø Copyright © 2017 Elsevier Inc. All rights reserved. 84

Critical Thinking Challenge What are the many psychosocial outcomes of burn injury? What are strategies for addressing the psychosocial needs of the patient with burns? Copyright © 2017 Elsevier Inc. All rights reserved. 85

Geriatric Considerations Older patients are more adversely affected by burn injuries Multiple variables affect outcomes Target interventions to maintaining quality of life Prevention is essential Copyright © 2017 Elsevier Inc. All rights reserved. 86

Nonburn Injury Some syndromes mimic burn-like injury Severe exfoliative disorders Toxic epidermal necrolysis Ø Stevens-Johnson syndrome Ø Erythema multiforme Ø Staphylococcal scalded skin Ø Copyright © 2017 Elsevier Inc. All rights reserved. 87

Nonburn Injury (Cont. ) Necrotizing soft tissue infections (NSTIs) Ø Necrotizing fasciitis Risk factors Rapid progression Pain management Copyright © 2017 Elsevier Inc. All rights reserved. 88

Discharge Planning Evaluate short- and long-term functional disabilities Identify resources (human and financial) Multiprofessional discharge planning Patient, family, community education Copyright © 2017 Elsevier Inc. All rights reserved. 89

Critical Thinking Challenge What are strategies for promoting rehabilitation early in the course of burn management? Which multiprofessional team members participate in burn care management? Copyright © 2017 Elsevier Inc. All rights reserved. 90
- Slides: 90