Chapter 21 Blood Vessels and Hemodynamics Copyright John
Chapter 21 Blood Vessels and Hemodynamics Copyright © John Wiley & Sons, Inc. All rights reserved.
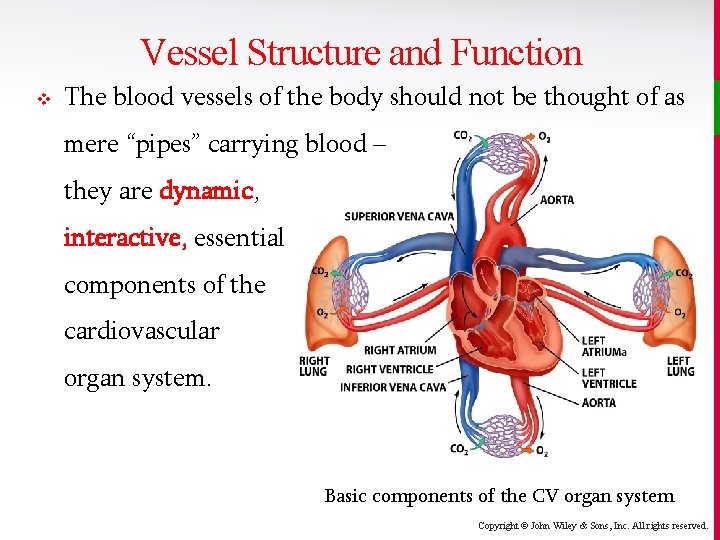
Vessel Structure and Function v The blood vessels of the body should not be thought of as mere “pipes” carrying blood – they are dynamic, interactive, essential components of the cardiovascular organ system. Basic components of the CV organ system Copyright © John Wiley & Sons, Inc. All rights reserved.

Vessel Structure and Function v Blood Vessel Types • Arteries – carry blood away from the heart q Large elastic arteries (>1 cm); medium muscular arteries (0. 1 – 10 mm); arterioles (< 0. 1 mm) • Capillaries – site of nutrient and gas exchange • Veins – carry blood towards the heart q Venules are small veins (< 0. 1 mm) Copyright © John Wiley & Sons, Inc. All rights reserved.
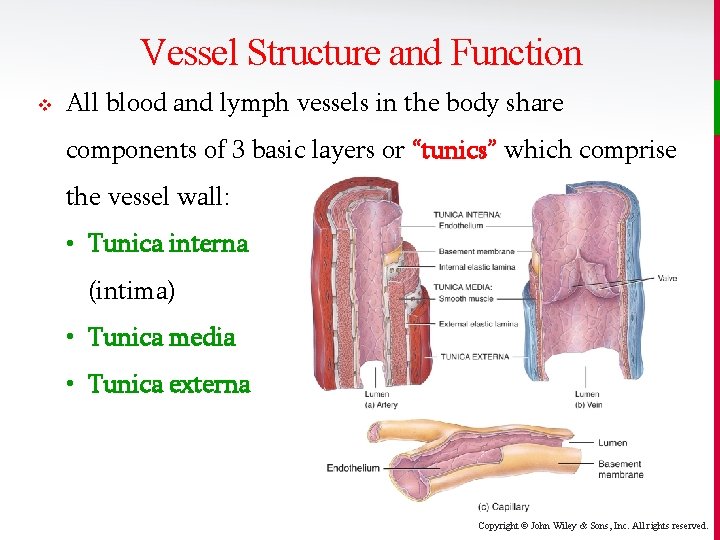
Vessel Structure and Function v All blood and lymph vessels in the body share components of 3 basic layers or “tunics” which comprise the vessel wall: • Tunica interna (intima) • Tunica media • Tunica externa Copyright © John Wiley & Sons, Inc. All rights reserved.

Vessel Structure and Function v The tunica interna is the inner lining in direct contact with blood. • The epithelium of the intima is the same endothelium that makes up the endocardial lining of the heart. • It has an active role in vessel-related activities. v The tunica media is chiefly composed of smooth muscle that regulates the diameter of the vessel lumen. v The tunica externa helps anchor vessel to surrounding tissue through use of elastic and collagen fibers. Copyright © John Wiley & Sons, Inc. All rights reserved.

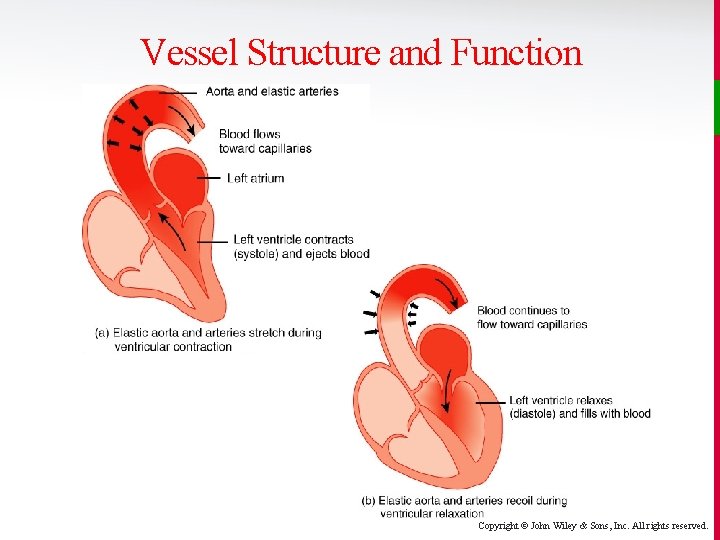
Vessel Structure and Function v The largest arteries are the conducting arteries (elastic arteries), best exemplified by the garden hose-sized aorta. • Their walls are thin compared to their overall size. • Elastic arteries perform the important function of storing mechanical energy during ventricular systole and then transmitting that energy to keep blood moving after the aortic and pulmonary valves close. Copyright © John Wiley & Sons, Inc. All rights reserved.
Vessel Structure and Function Copyright © John Wiley & Sons, Inc. All rights reserved.
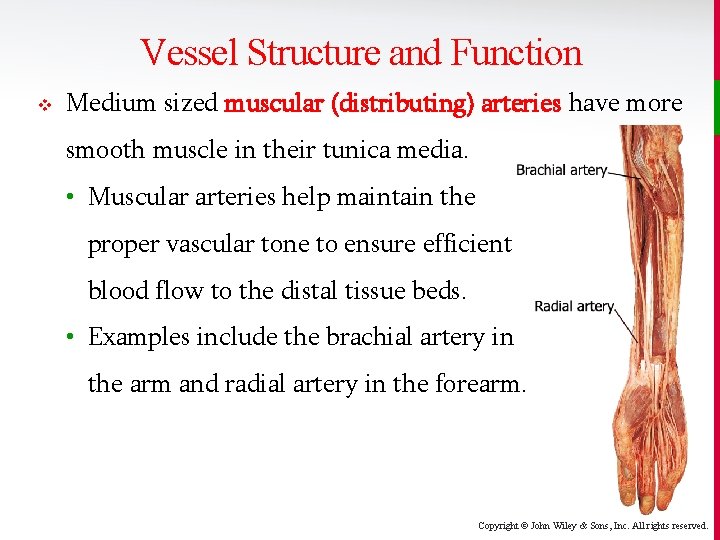
Vessel Structure and Function v Medium sized muscular (distributing) arteries have more smooth muscle in their tunica media. • Muscular arteries help maintain the proper vascular tone to ensure efficient blood flow to the distal tissue beds. • Examples include the brachial artery in the arm and radial artery in the forearm. Copyright © John Wiley & Sons, Inc. All rights reserved.
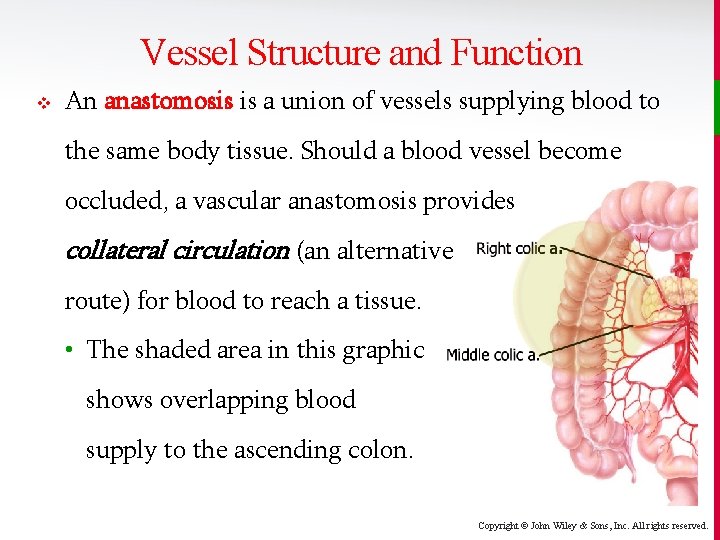
Vessel Structure and Function v An anastomosis is a union of vessels supplying blood to the same body tissue. Should a blood vessel become occluded, a vascular anastomosis provides collateral circulation (an alternative route) for blood to reach a tissue. • The shaded area in this graphic shows overlapping blood supply to the ascending colon. Copyright © John Wiley & Sons, Inc. All rights reserved.
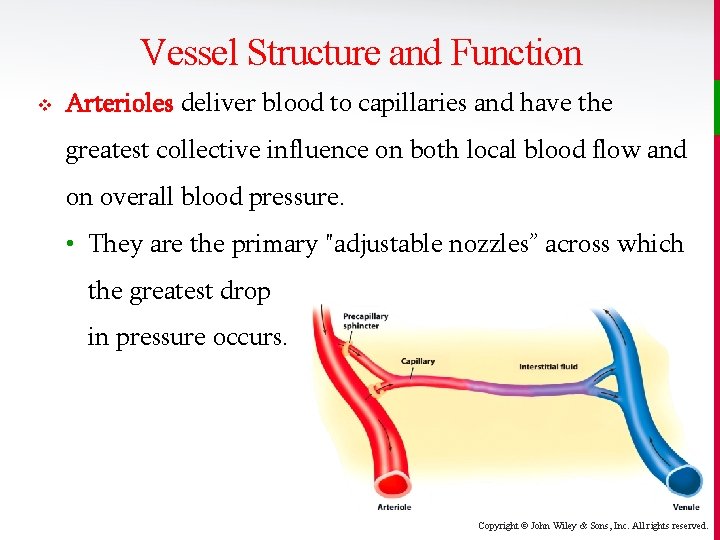
Vessel Structure and Function v Arterioles deliver blood to capillaries and have the greatest collective influence on both local blood flow and on overall blood pressure. • They are the primary "adjustable nozzles” across which the greatest drop in pressure occurs. Copyright © John Wiley & Sons, Inc. All rights reserved.
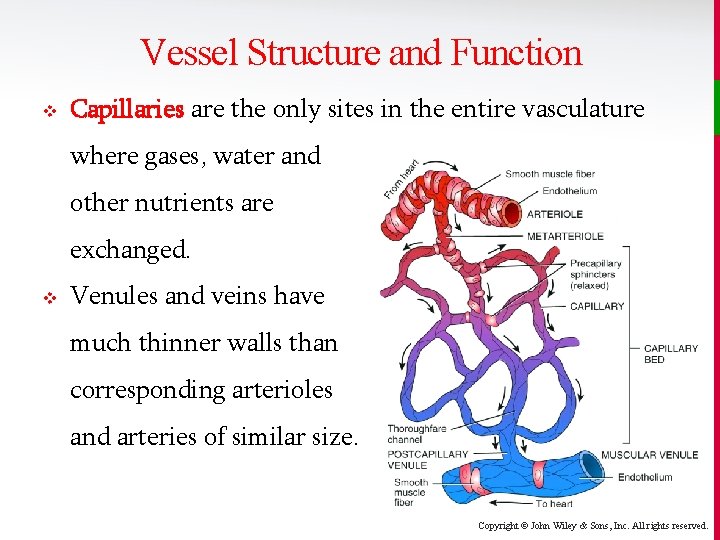
Vessel Structure and Function v Capillaries are the only sites in the entire vasculature where gases, water and other nutrients are exchanged. v Venules and veins have much thinner walls than corresponding arterioles and arteries of similar size. Copyright © John Wiley & Sons, Inc. All rights reserved.
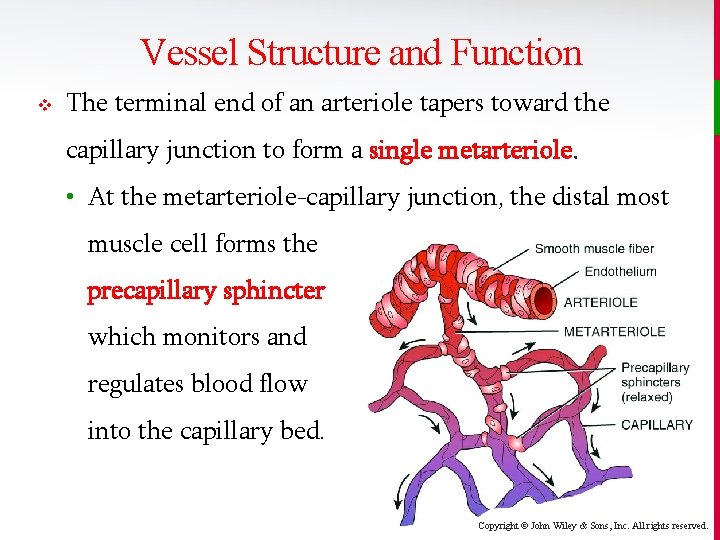
Vessel Structure and Function v The terminal end of an arteriole tapers toward the capillary junction to form a single metarteriole. • At the metarteriole-capillary junction, the distal most muscle cell forms the precapillary sphincter which monitors and regulates blood flow into the capillary bed. Copyright © John Wiley & Sons, Inc. All rights reserved.
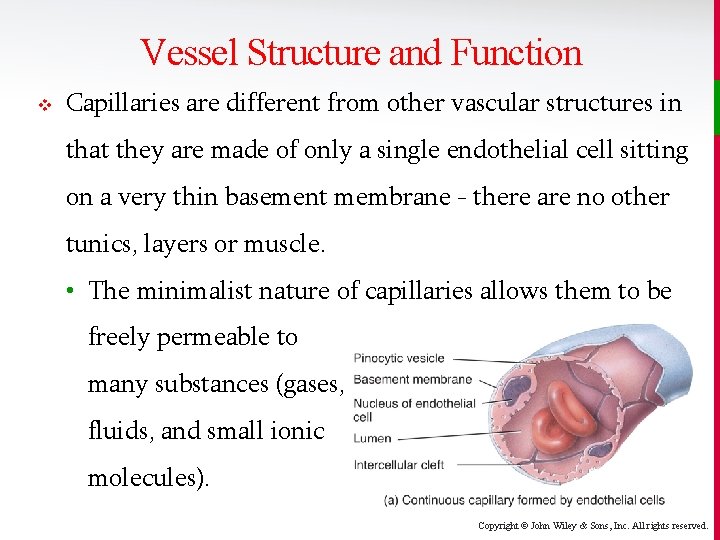
Vessel Structure and Function v Capillaries are different from other vascular structures in that they are made of only a single endothelial cell sitting on a very thin basement membrane - there are no other tunics, layers or muscle. • The minimalist nature of capillaries allows them to be freely permeable to many substances (gases, fluids, and small ionic molecules). Copyright © John Wiley & Sons, Inc. All rights reserved.
Vessel Structure and Function v The body contains three types of capillaries: • Continuous capillaries are the most common with endothelial cells forming a continuous tube, interrupted only by small intercellular clefts. • Fenestrated capillaries (fenestra = windows), found in the kidneys, villi of small intestines, and endocrine glands are much more porous. • Sinusoids form very porous channels through which blood can percolate, e. g. , in the liver and spleen. Copyright © John Wiley & Sons, Inc. All rights reserved.
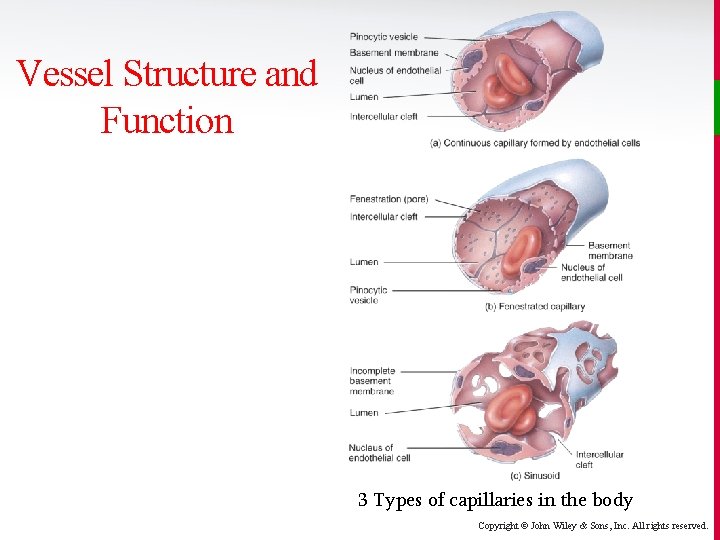
Vessel Structure and Function 3 Types of capillaries in the body Copyright © John Wiley & Sons, Inc. All rights reserved.

Vessel Structure and Function v Veins have thinner walls, less muscle and elastic tissue, and are designed to operate at much lower pressures. • Intravenous pressure in venules (16 mm. Hg) is less than half that of arterioles (35 mm. Hg), and drops to just 1 -2 mm. Hg in some larger veins. • Because intravenous pressure is so low, veins have valves to keep blood flowing in only 1 direction. q When exposed to higher than normal pressures, veins can become incompetent (varicose veins). Copyright © John Wiley & Sons, Inc. All rights reserved.
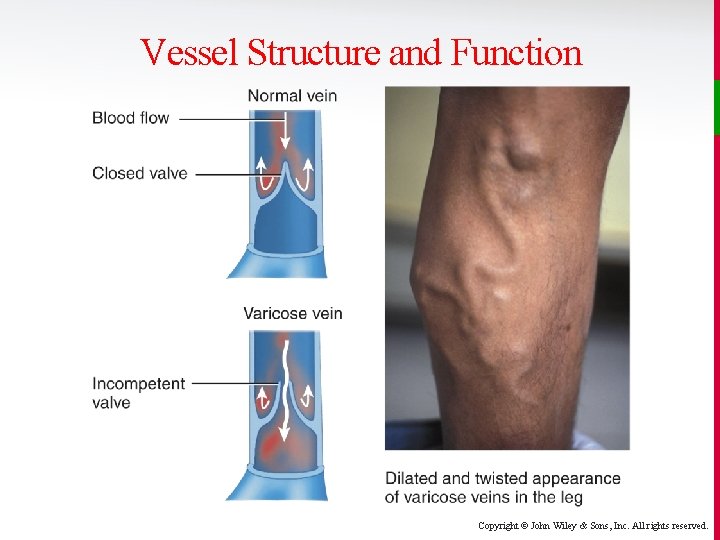
Vessel Structure and Function Copyright © John Wiley & Sons, Inc. All rights reserved.
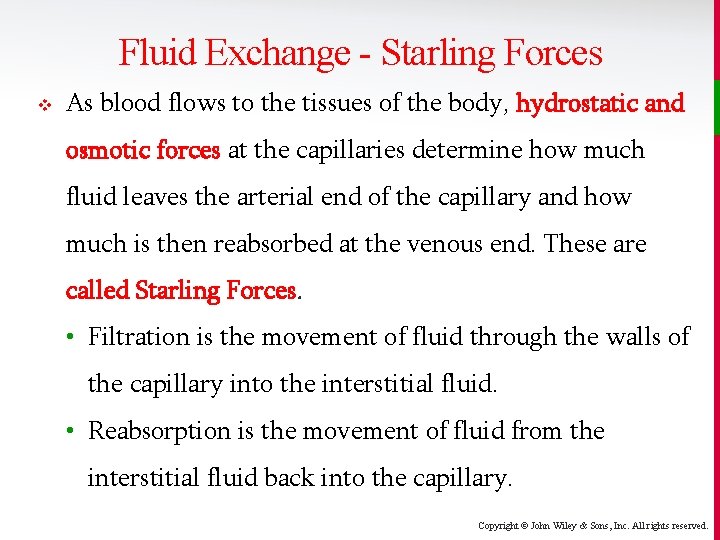
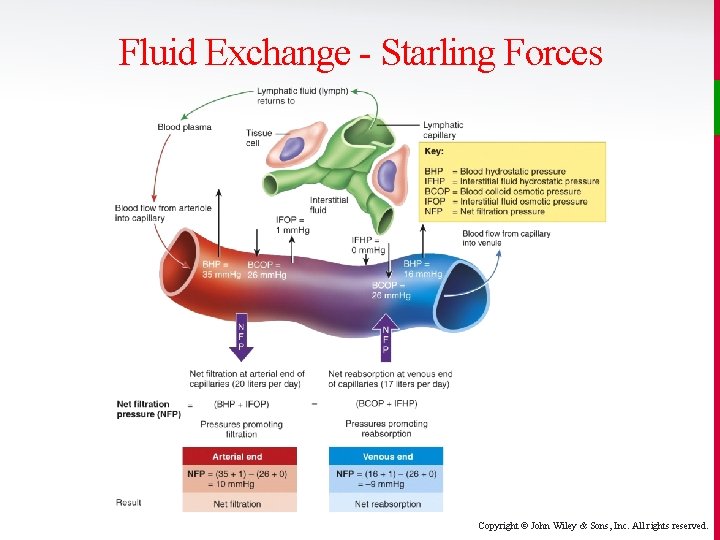
Fluid Exchange - Starling Forces v As blood flows to the tissues of the body, hydrostatic and osmotic forces at the capillaries determine how much fluid leaves the arterial end of the capillary and how much is then reabsorbed at the venous end. These are called Starling Forces. • Filtration is the movement of fluid through the walls of the capillary into the interstitial fluid. • Reabsorption is the movement of fluid from the interstitial fluid back into the capillary. Copyright © John Wiley & Sons, Inc. All rights reserved.
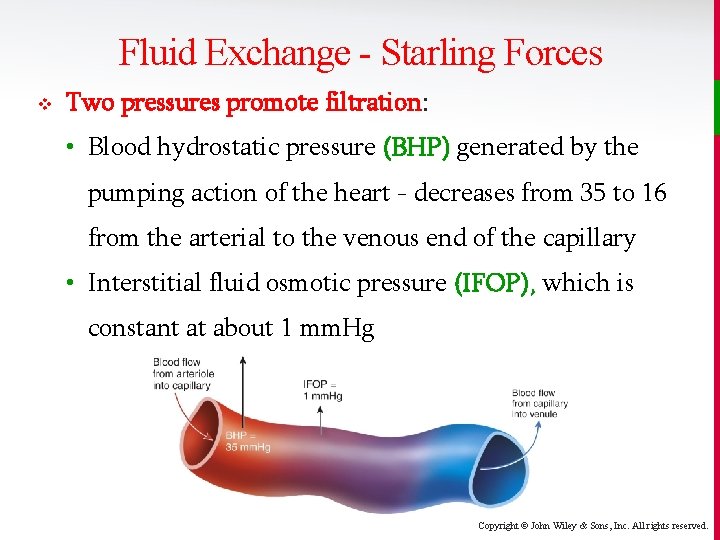
Fluid Exchange - Starling Forces v Two pressures promote filtration: • Blood hydrostatic pressure (BHP) generated by the pumping action of the heart - decreases from 35 to 16 from the arterial to the venous end of the capillary • Interstitial fluid osmotic pressure (IFOP), which is constant at about 1 mm. Hg Copyright © John Wiley & Sons, Inc. All rights reserved.
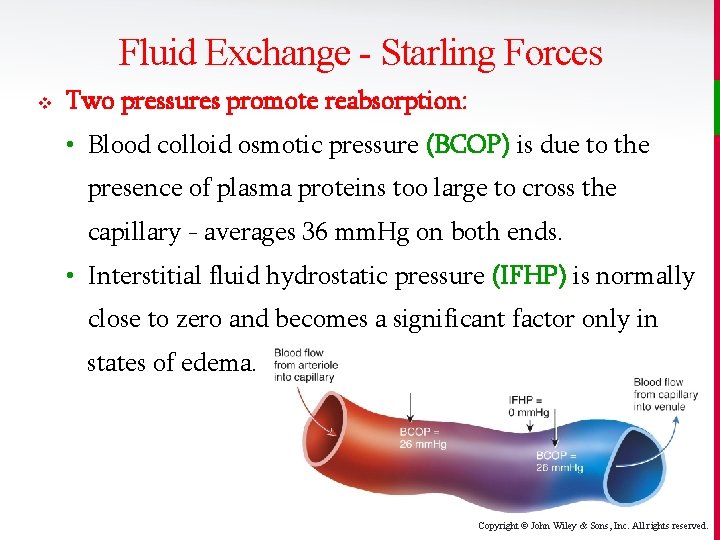
Fluid Exchange - Starling Forces v Two pressures promote reabsorption: • Blood colloid osmotic pressure (BCOP) is due to the presence of plasma proteins too large to cross the capillary - averages 36 mm. Hg on both ends. • Interstitial fluid hydrostatic pressure (IFHP) is normally close to zero and becomes a significant factor only in states of edema. Copyright © John Wiley & Sons, Inc. All rights reserved.
Fluid Exchange - Starling Forces Copyright © John Wiley & Sons, Inc. All rights reserved.

Fluid Exchange - Starling Forces v Normally there is nearly as much fluid reabsorbed as there is filtered. • At the arterial end, net pressure is outward at 10 mm. Hg and fluid leaves the capillary (filtration). • At the venous end, net pressure is inward at – 9 mm. Hg (reabsorption). • On average, about 85% of fluid filtered is reabsorbed. Copyright © John Wiley & Sons, Inc. All rights reserved.
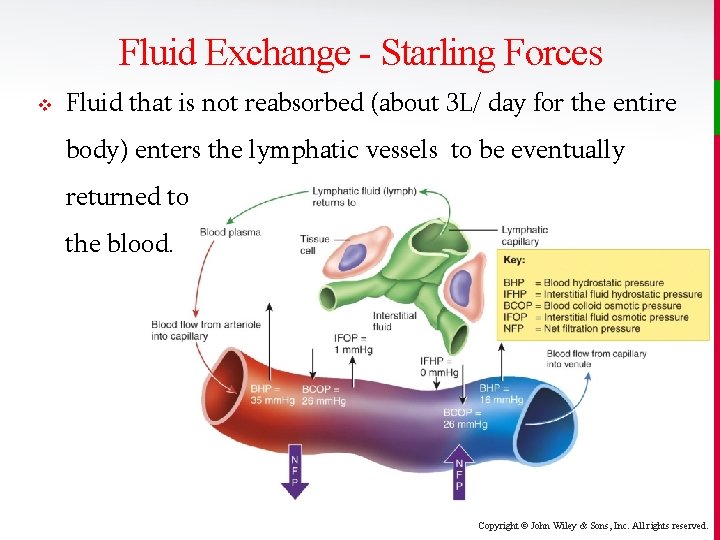
Fluid Exchange - Starling Forces v Fluid that is not reabsorbed (about 3 L/ day for the entire body) enters the lymphatic vessels to be eventually returned to the blood. Copyright © John Wiley & Sons, Inc. All rights reserved.

Gas And Nutrient Exchange v In contrast to the bulk flow of fluids at the capillaries, the exchange of gases and small particles (like certain nutrients and wastes) is a purely passive diffusion process. • Gases and these other substances simply move into or out of the capillary down their concentration gradient. Copyright © John Wiley & Sons, Inc. All rights reserved.

Venous Reserve v Because systemic veins and venules contain a large percentage of the blood volume (about 64% at rest), they function as blood reservoirs from which blood can be diverted quickly if needed. • To counteract a drop in BP, stimulation of the sympathetic NS will cause venoconstriction, allowing a greater volume of blood to flow to skeletal muscles. Copyright © John Wiley & Sons, Inc. All rights reserved.
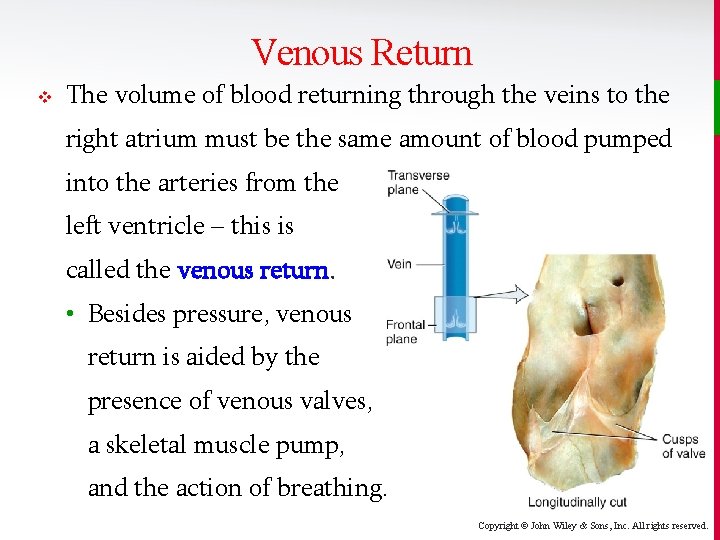
Venous Return v The volume of blood returning through the veins to the right atrium must be the same amount of blood pumped into the arteries from the left ventricle – this is called the venous return. • Besides pressure, venous return is aided by the presence of venous valves, a skeletal muscle pump, and the action of breathing. Copyright © John Wiley & Sons, Inc. All rights reserved.
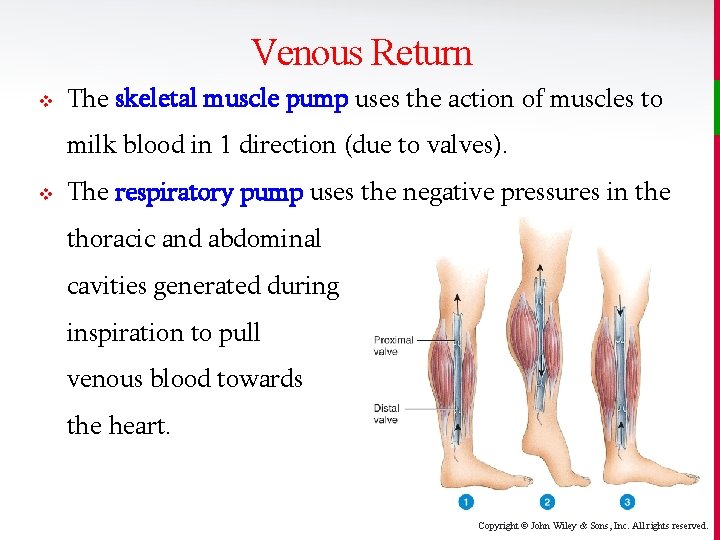
Venous Return v The skeletal muscle pump uses the action of muscles to milk blood in 1 direction (due to valves). v The respiratory pump uses the negative pressures in the thoracic and abdominal cavities generated during inspiration to pull venous blood towards the heart. Copyright © John Wiley & Sons, Inc. All rights reserved.
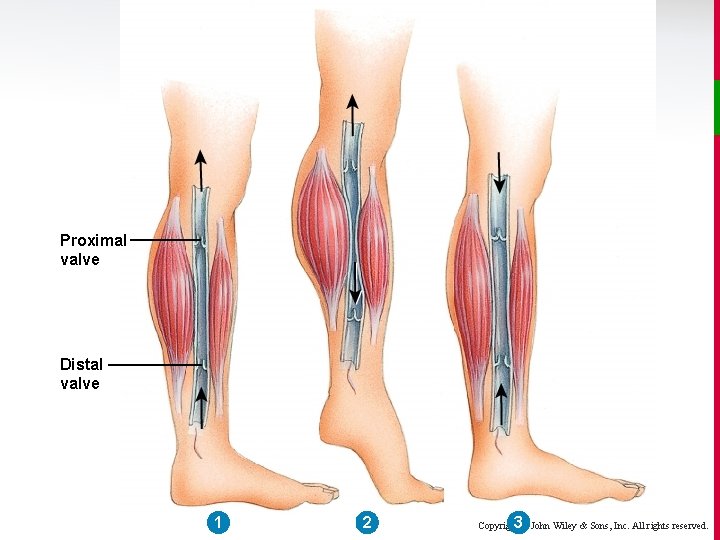
Proximal valve Distal valve 1 2 3 Copyright © John Wiley & Sons, Inc. All rights reserved.
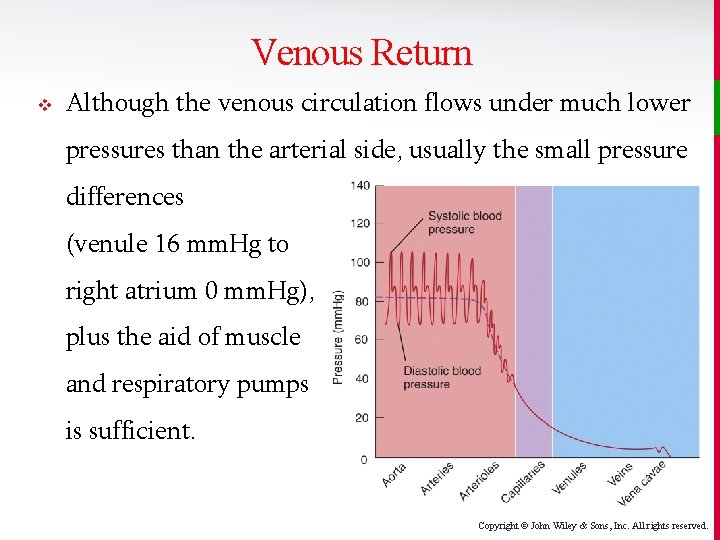
Venous Return v Although the venous circulation flows under much lower pressures than the arterial side, usually the small pressure differences (venule 16 mm. Hg to right atrium 0 mm. Hg), plus the aid of muscle and respiratory pumps is sufficient. Copyright © John Wiley & Sons, Inc. All rights reserved.
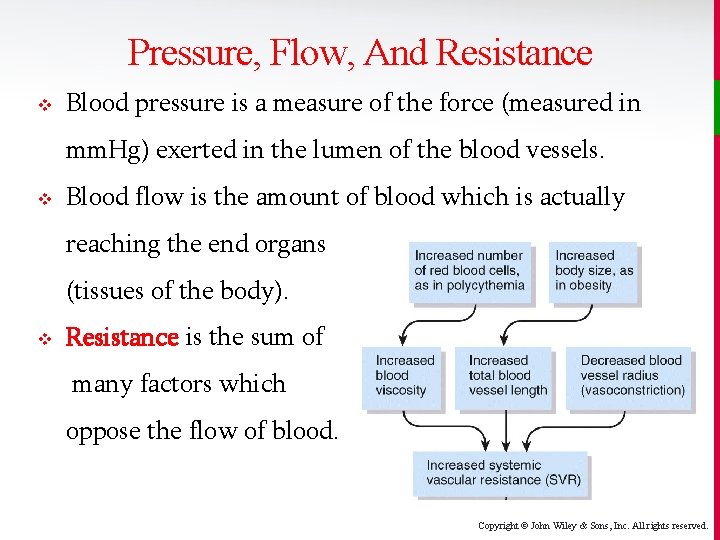
Pressure, Flow, And Resistance v Blood pressure is a measure of the force (measured in mm. Hg) exerted in the lumen of the blood vessels. v Blood flow is the amount of blood which is actually reaching the end organs (tissues of the body). v Resistance is the sum of many factors which oppose the flow of blood. Copyright © John Wiley & Sons, Inc. All rights reserved.

Pressure, Flow, And Resistance v Cardiovascular homeostasis is mainly dependent on blood flow… but blood flow is hard to measure. • Clinically, we check blood pressure because it is easier to measure, and it is related to blood flow. • The relationship between blood flow, blood pressure, and peripheral resistance follows a simple formula called Ohms Law. BP = Flow x Resistance Copyright © John Wiley & Sons, Inc. All rights reserved.
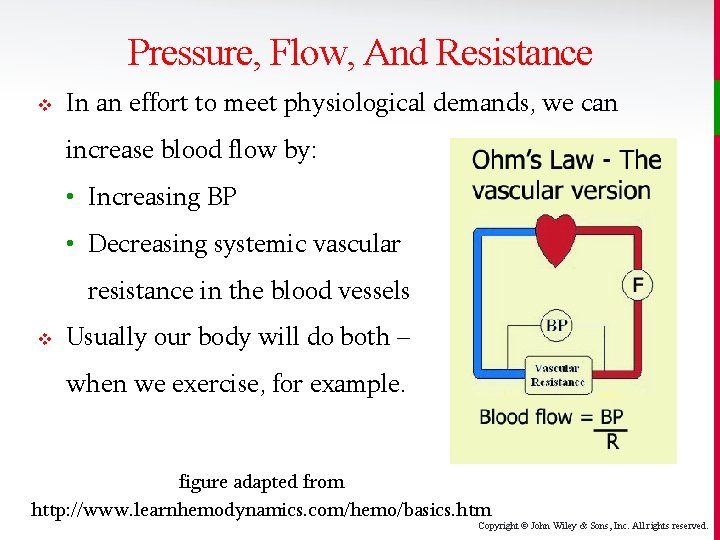
Pressure, Flow, And Resistance v In an effort to meet physiological demands, we can increase blood flow by: • Increasing BP • Decreasing systemic vascular resistance in the blood vessels v Usually our body will do both – when we exercise, for example. figure adapted from http: //www. learnhemodynamics. com/hemo/basics. htm Copyright © John Wiley & Sons, Inc. All rights reserved.

Pressure, Flow, And Resistance v As we have already seen, peripheral resistance is itself dependent on other factors like the viscosity of blood, the length of all the blood vessels in the body (body size), and the diameter of a vessel. v The first two of these factors (viscosity and the length of blood vessels) are unchangeable from moment to moment. • The diameter, however, is readily adjusted if the body needs to change blood flow to a certain capillary bed. Copyright © John Wiley & Sons, Inc. All rights reserved.

Pressure, Flow, And Resistance v Copyright © John Wiley & Sons, Inc. All rights reserved.
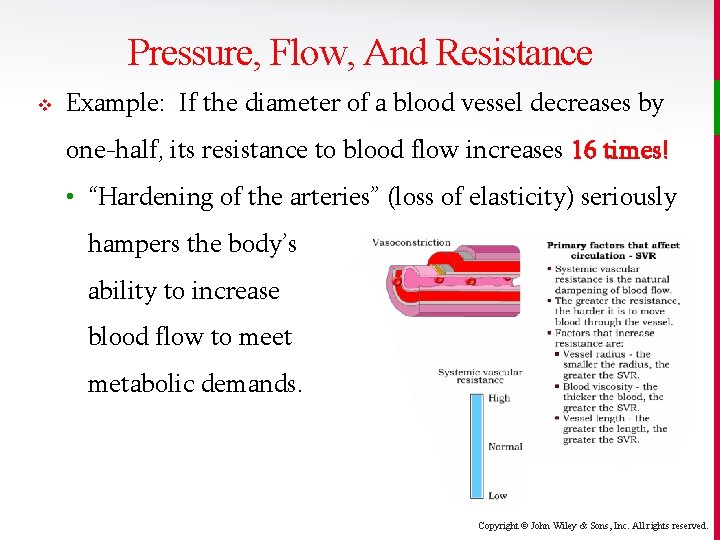
Pressure, Flow, And Resistance v Example: If the diameter of a blood vessel decreases by one-half, its resistance to blood flow increases 16 times! • “Hardening of the arteries” (loss of elasticity) seriously hampers the body’s ability to increase blood flow to meet metabolic demands. Copyright © John Wiley & Sons, Inc. All rights reserved.
Pressure, Flow, And Resistance (Interactions Animation) v Vascular Regulation You must be connected to the internet to run this animation Copyright © John Wiley & Sons, Inc. All rights reserved.

Autoregulation v Homeostasis in the body tissues requires the cardiovascular system to adjust pressure and resistance to maintain adequate blood flow to vital organs at all times – a process called autoregulation. v Autoregulation is controlled through negative feedback loops. Copyright © John Wiley & Sons, Inc. All rights reserved.
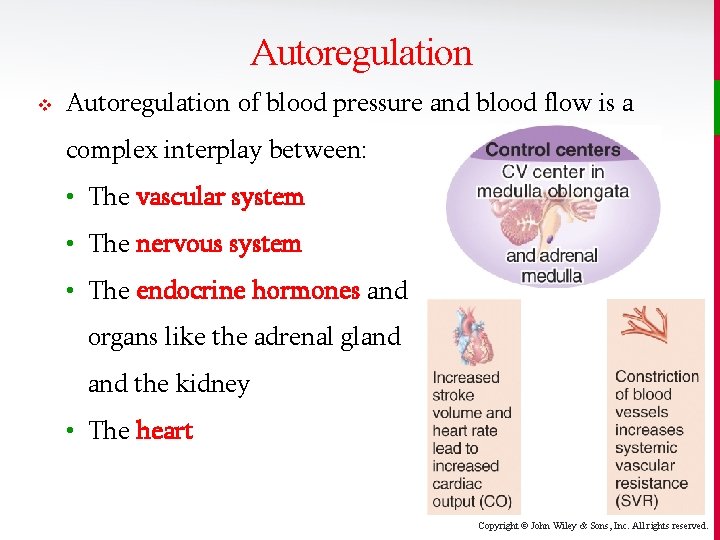
Autoregulation v Autoregulation of blood pressure and blood flow is a complex interplay between: • The vascular system • The nervous system • The endocrine hormones and organs like the adrenal gland the kidney • The heart Copyright © John Wiley & Sons, Inc. All rights reserved.
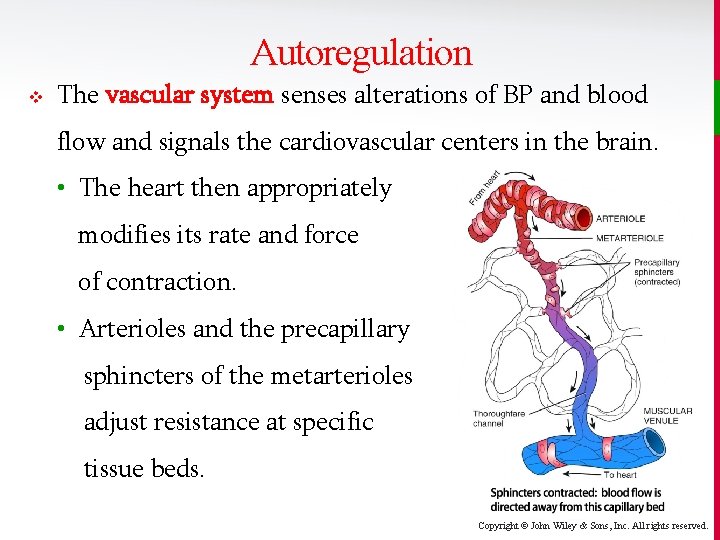
Autoregulation v The vascular system senses alterations of BP and blood flow and signals the cardiovascular centers in the brain. • The heart then appropriately modifies its rate and force of contraction. • Arterioles and the precapillary sphincters of the metarterioles adjust resistance at specific tissue beds. Copyright © John Wiley & Sons, Inc. All rights reserved.

Autoregulation v For example, during emergencies, the autonomic nervous system will vasodilate the precapillary sphincters of metarterioles in the skeletal muscles, lungs, and brain, while constricting the precapillary sphincters found in tissues such as the skin, GI tract, and kidneys. • This sends the majority of the cardiac output (blood flow) to those organs important in a fight or flight response, while temporarily depriving (through vasoconstriction) the nonessential organs. Copyright © John Wiley & Sons, Inc. All rights reserved.
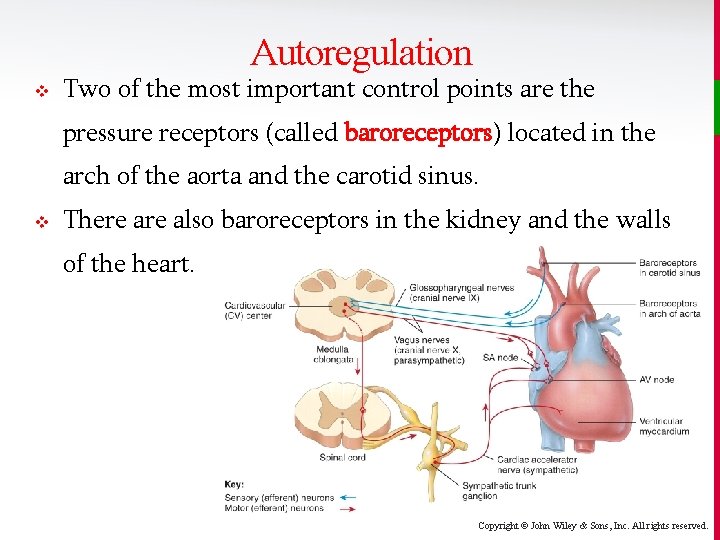
Autoregulation v Two of the most important control points are the pressure receptors (called baroreceptors) located in the arch of the aorta and the carotid sinus. v There also baroreceptors in the kidney and the walls of the heart. Copyright © John Wiley & Sons, Inc. All rights reserved.
Autoregulation v Stimulation of the baroreceptors in the carotid sinus is called the carotid sinus reflex , and it helps normalize blood pressure in the brain. Stimulation of the aortic baroreceptors helps normalize the systemic BP. • When the blood pressure falls, baroreceptors are stretched less, and the input is sensed in the cardiovascular centers of the brain which respond with decreased parasympathetic and increased sympathetic stimulation. Blood pressure increases do the opposite. Copyright © John Wiley & Sons, Inc. All rights reserved.
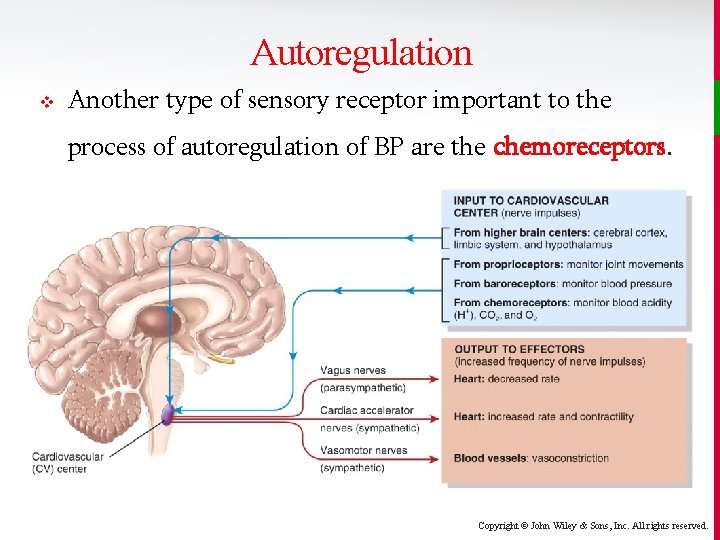
Autoregulation v Another type of sensory receptor important to the process of autoregulation of BP are the chemoreceptors. Copyright © John Wiley & Sons, Inc. All rights reserved.

Autoregulation v Chemoreceptors are found in the carotid bodies (located close to baroreceptors of carotid sinus) and aortic bodies (located in the aortic arch). v When they detect hypoxia (low O 2), hypercapnia (high CO 2), or acidosis (high H+), they signal the cardiovascular centers. • They increase sympathetic stimulation increasing heart rate and respiratory rate, and vasoconstricting the vessels (arterioles and veins) to increase BP. Copyright © John Wiley & Sons, Inc. All rights reserved.

Autoregulation v The Renin-angiotensin-aldosterone (RAA) system is an important endocrine component of autoregulation. • Renin is released by kidneys when blood volume falls or blood flow decreases. • It is subsequently converted into the active hormone angiotensin II which raises BP by vasoconstriction and by stimulating secretion of aldosterone from the adrenal glands. Copyright © John Wiley & Sons, Inc. All rights reserved.

Autoregulation v Epinephrine and norepinephrine are also released from the adrenal medulla as an endocrine autoregulatory response to sympathetic stimulation. • They increase cardiac output by increasing rate and force of heart contractions. v Antidiuretic hormone (ADH) is released from the posterior pituitary gland in response to dehydration or decreased blood volume. Copyright © John Wiley & Sons, Inc. All rights reserved.

Autoregulation v Atrial Naturetic Peptide (ANP) is a natural diuretic polypeptide hormone released by cells of the cardiac atria. • ANP participates in autoregulation by: q Lowering blood pressure (it causes a direct vasodilation) q Reducing blood volume (by promoting loss of salt and water as urine) Copyright © John Wiley & Sons, Inc. All rights reserved.

Circulation v In an autoregulatory response, important differences exist between the pulmonary and systemic circulations: • Systemic blood vessel walls dilate in response to hypoxia (low O 2) or acidosis to increase blood flow. • The walls of the pulmonary blood vessels constrict to a hypoxic or acidosis stimulus to ensure that most blood flow is diverted to better ventilated areas of the lung. Copyright © John Wiley & Sons, Inc. All rights reserved.
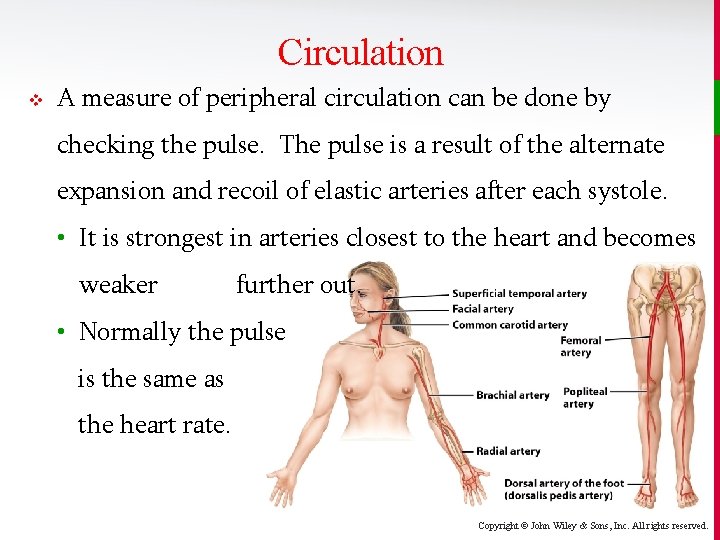
Circulation v A measure of peripheral circulation can be done by checking the pulse. The pulse is a result of the alternate expansion and recoil of elastic arteries after each systole. • It is strongest in arteries closest to the heart and becomes weaker further out. • Normally the pulse is the same as the heart rate. Copyright © John Wiley & Sons, Inc. All rights reserved.
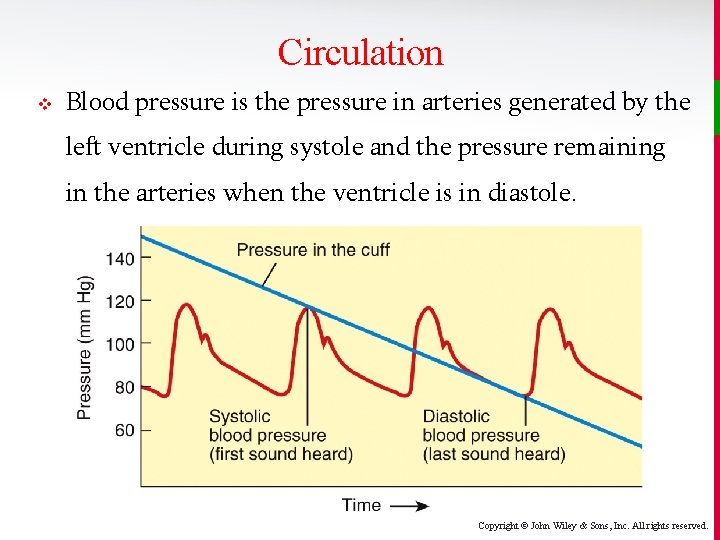
Circulation v Blood pressure is the pressure in arteries generated by the left ventricle during systole and the pressure remaining in the arteries when the ventricle is in diastole. Copyright © John Wiley & Sons, Inc. All rights reserved.
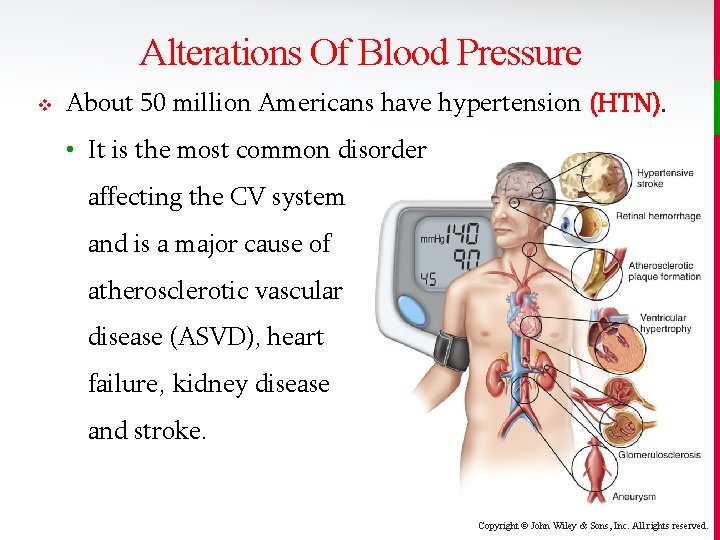
Alterations Of Blood Pressure v About 50 million Americans have hypertension (HTN). • It is the most common disorder affecting the CV system and is a major cause of atherosclerotic vascular disease (ASVD), heart failure, kidney disease and stroke. Copyright © John Wiley & Sons, Inc. All rights reserved.
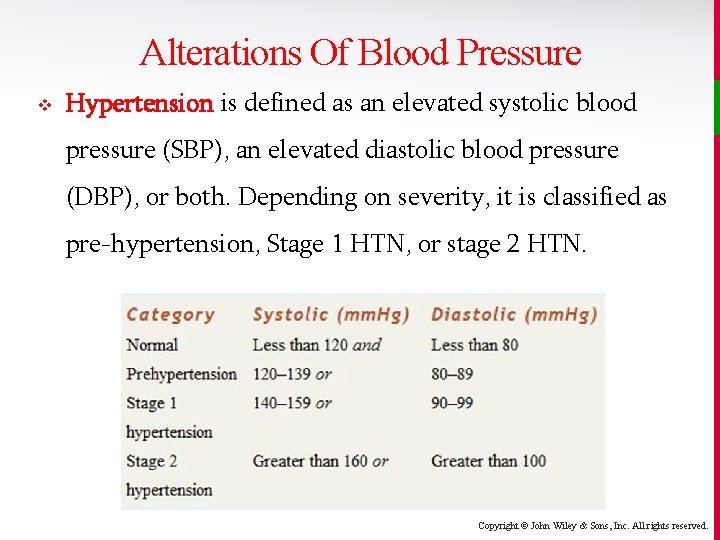
Alterations Of Blood Pressure v Hypertension is defined as an elevated systolic blood pressure (SBP), an elevated diastolic blood pressure (DBP), or both. Depending on severity, it is classified as pre-hypertension, Stage 1 HTN, or stage 2 HTN. Copyright © John Wiley & Sons, Inc. All rights reserved.

Alterations Of Blood Pressure v Hypotension is defined as any blood pressure too low to allow sufficient blood flow (hypo-perfusion) to meet the body's metabolic demands (to maintain homeostasis). v Many persons, especially some thin, young women, have very low BP, yet experience no dizziness, fatigue, or other symptoms – they are not hypotensive, and in fact are probably very healthy (cardiovascular wise). v Hypotension leading to hypo-perfusion (pressure and flow are related) of critical organs results in shock Copyright © John Wiley & Sons, Inc. All rights reserved.

Shock And Homeostasis v The 4 basic types of shock are: • Hypovolemic shock, due to decreased blood volume • Cardiogenic shock, due to poor heart function • Obstructive shock, due to obstruction of blood flow • Vascular shock, due to excess vasodilation - as seen in cases of a massive allergy (anaphylaxis) or sepsis. In the U. S. , septic shock causes >100, 000 deaths/yr. and is the most common cause of death in hospital critical care units. Copyright © John Wiley & Sons, Inc. All rights reserved.

Shock And Homeostasis v The same negative feedback mechanism discussed in autoregulation of blood pressure/flow is activated to restore blood and nutrient flow in cases of shock. • Heart will respond with rate and force of contraction. • Selective tissue beds will vasoconstrict to shunt blood flow to those tissue most necessary to life (brain). • The other neural, hormonal, and chemical pathways will be recruited to restore balance. Copyright © John Wiley & Sons, Inc. All rights reserved.
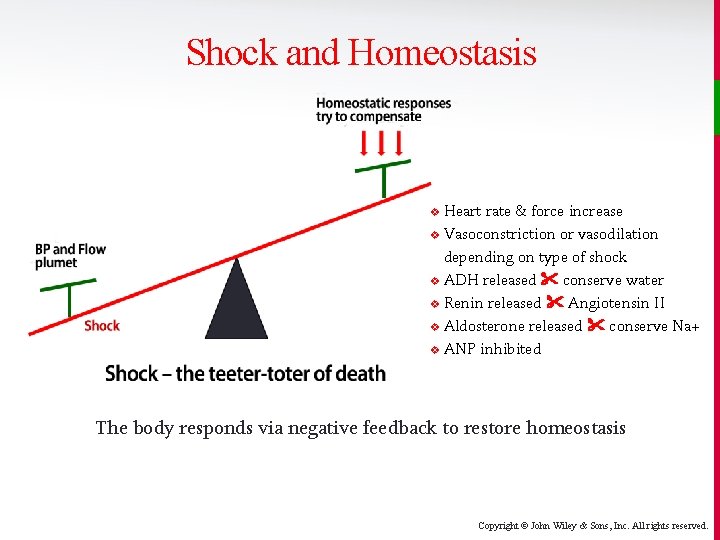
Shock and Homeostasis Heart rate & force increase v Vasoconstriction or vasodilation depending on type of shock v ADH released conserve water v Renin released Angiotensin II v Aldosterone released conserve Na+ v ANP inhibited v The body responds via negative feedback to restore homeostasis Copyright © John Wiley & Sons, Inc. All rights reserved.

Shock And Homeostasis v Most cases of shock call for the administration of extra fluids and emergency medications like epinephrine to help restore perfusion to the tissues. v If the body is not able to do this quickly, with or without outside help, organs will fail (kidney failure, liver failure, coma) and damage may become permanent. Copyright © John Wiley & Sons, Inc. All rights reserved.

Circulatory Routes v Blood vessels are organized into circulatory routes that carry blood to specific parts of the body. • The pulmonary circulation leaves the right heart to allow blood to be re-oxygenated and to off-load CO 2. • The systemic circulation leaves the left side of the heart to supply the coronary, cerebral, renal, digestive and hepatic circulations (among others). The bronchial circulation provides oxygenated blood to the lungs, not the pulmonary circulation, which oxygenates blood! Copyright © John Wiley & Sons, Inc. All rights reserved.

Systemic Circulation - Arteries v Aorta (one) v Radial v Brachiocephalic (one) v Ulnar v Common Carotid v Bronchial (usually 3) v External Carotid v Renal v Internal Carotid v Iliac (common, internal, v Subclavian v Axillary v Femoral v Brachial v Popliteal external) Copyright © John Wiley & Sons, Inc. All rights reserved.
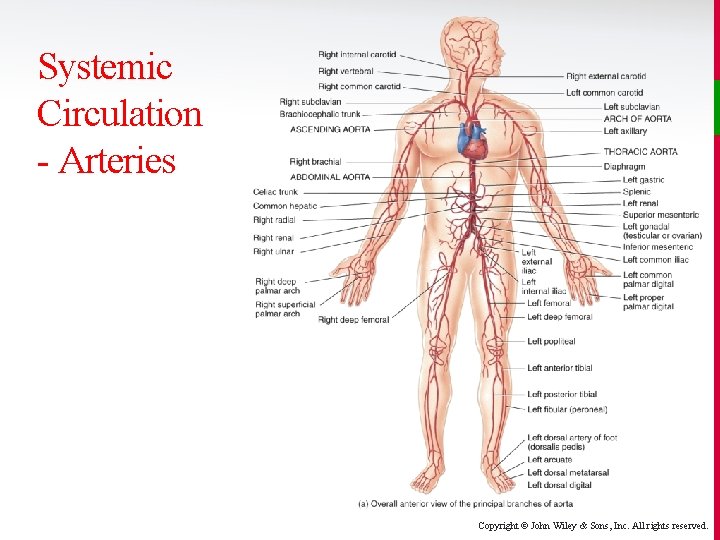
Systemic Circulation - Arteries Copyright © John Wiley & Sons, Inc. All rights reserved.
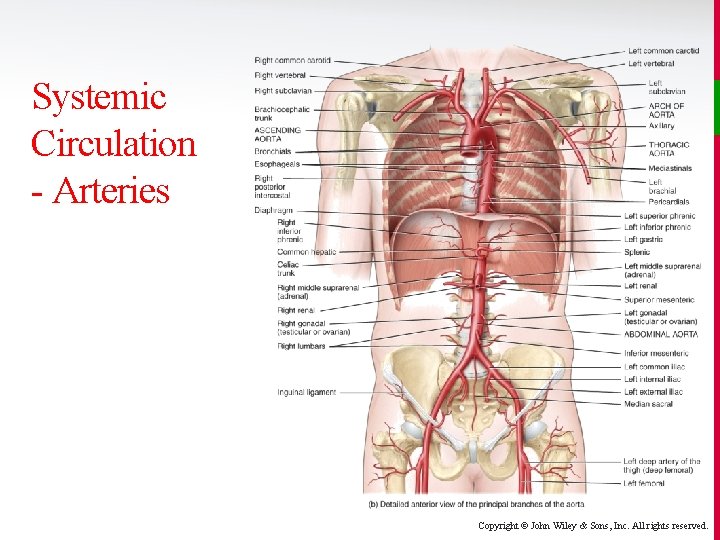
Systemic Circulation - Arteries Copyright © John Wiley & Sons, Inc. All rights reserved.
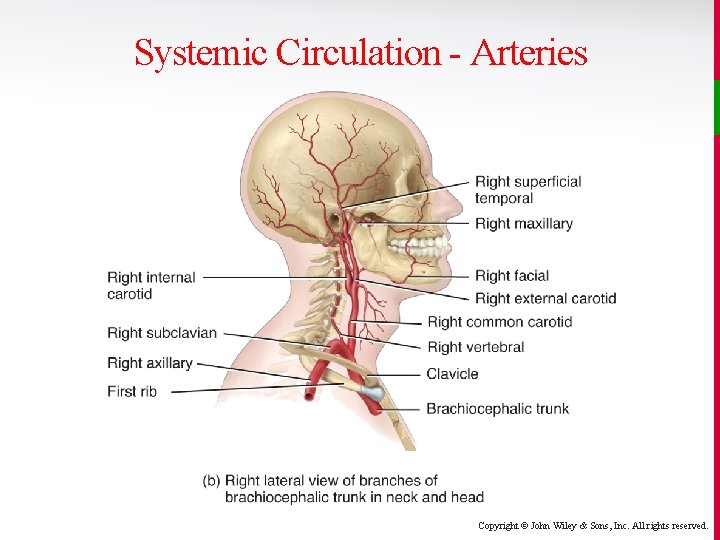
Systemic Circulation - Arteries Copyright © John Wiley & Sons, Inc. All rights reserved.
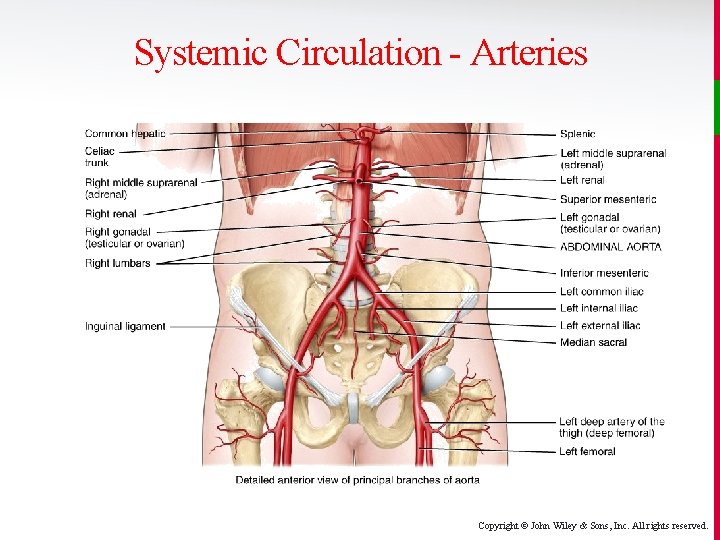
Systemic Circulation - Arteries Copyright © John Wiley & Sons, Inc. All rights reserved.

Systemic Circulation - Veins v Vena Cava v Median Cubital v Brachiocephalic (two) v Iliac (common, v External Jugular v Internal Jugular v Femoral v Subclavian v Popliteal v Axillary v Saphenous v Brachial v Hepatic portal internal, external) Copyright © John Wiley & Sons, Inc. All rights reserved.
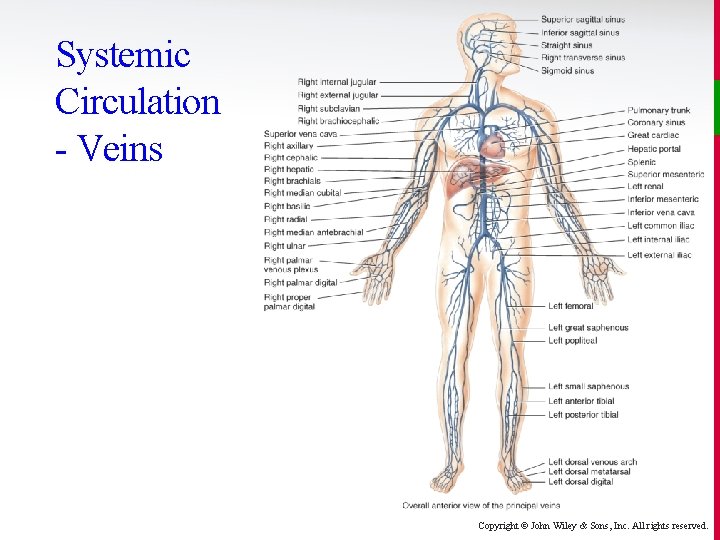
Systemic Circulation - Veins Copyright © John Wiley & Sons, Inc. All rights reserved.
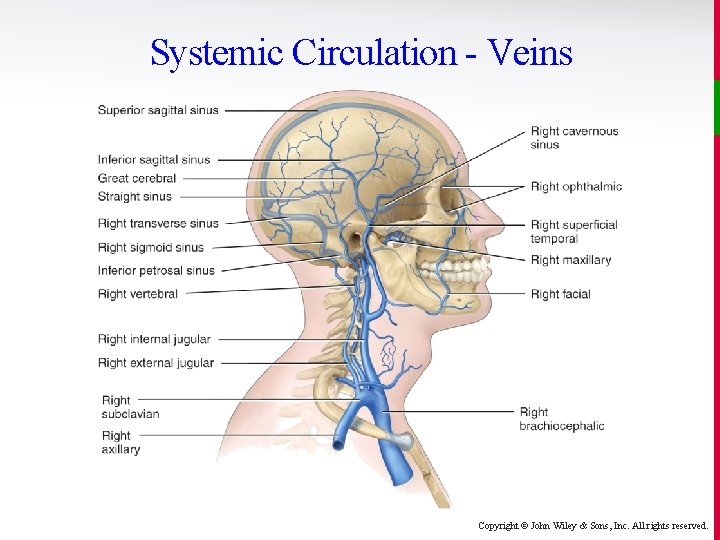
Systemic Circulation - Veins Copyright © John Wiley & Sons, Inc. All rights reserved.
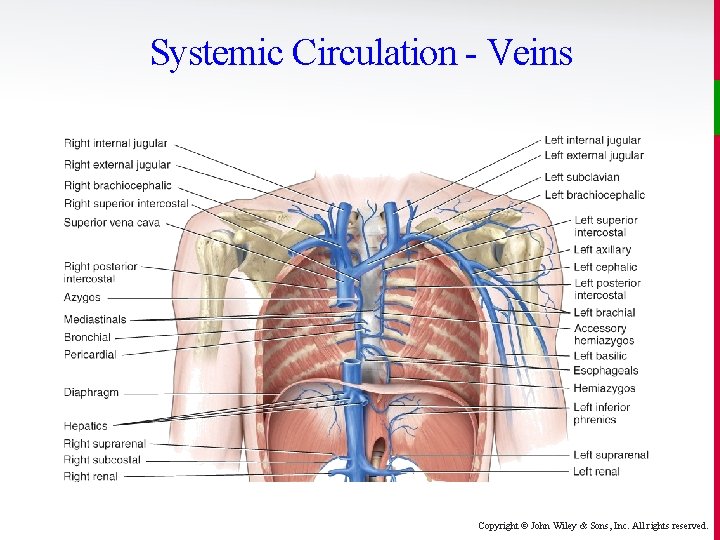
Systemic Circulation - Veins Copyright © John Wiley & Sons, Inc. All rights reserved.
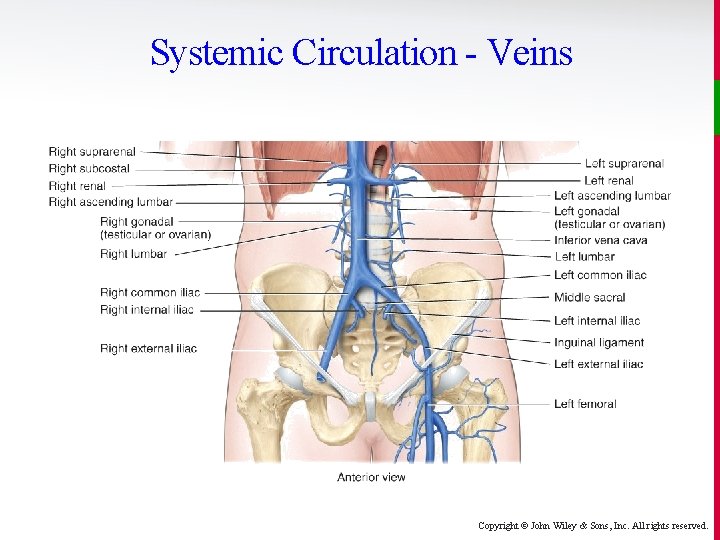
Systemic Circulation - Veins Copyright © John Wiley & Sons, Inc. All rights reserved.
Portal Circulation v The hepatic portal system is designed to take nutrientrich venous blood from the digestive tract capillaries, and transport it to the sinusoidal capillaries of the liver. • As it percolates through the liver sinusoids, the hepatocytes of the liver, acting as the chemical factories of the body, extract and add what they wish to maintain homeostasis (extracting sugars, fats, proteins when appropriate and then dumping them back into the circulation when necessary). Copyright © John Wiley & Sons, Inc. All rights reserved.
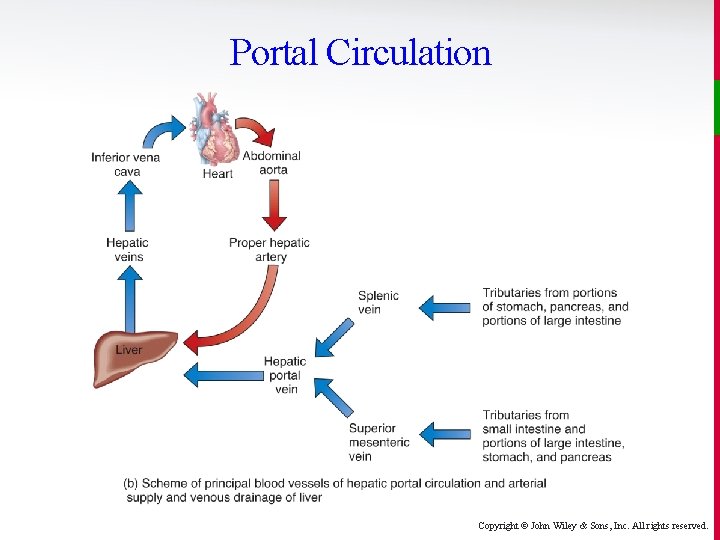
Portal Circulation Copyright © John Wiley & Sons, Inc. All rights reserved.
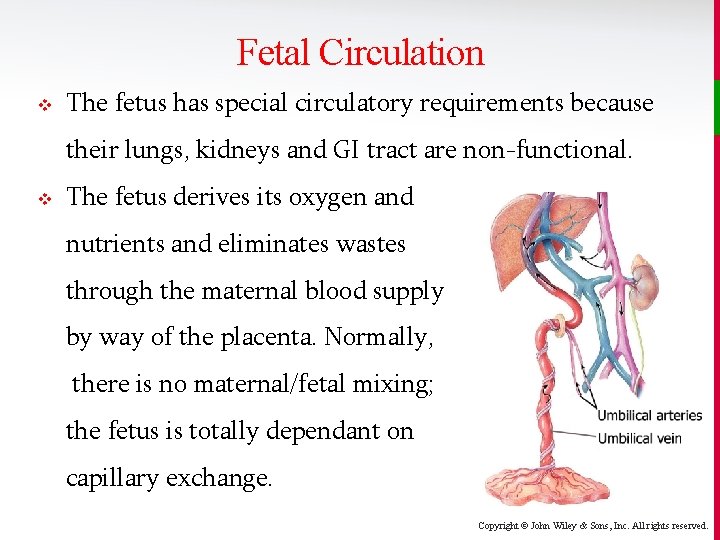
Fetal Circulation v The fetus has special circulatory requirements because their lungs, kidneys and GI tract are non-functional. v The fetus derives its oxygen and nutrients and eliminates wastes through the maternal blood supply by way of the placenta. Normally, there is no maternal/fetal mixing; the fetus is totally dependant on capillary exchange. Copyright © John Wiley & Sons, Inc. All rights reserved.
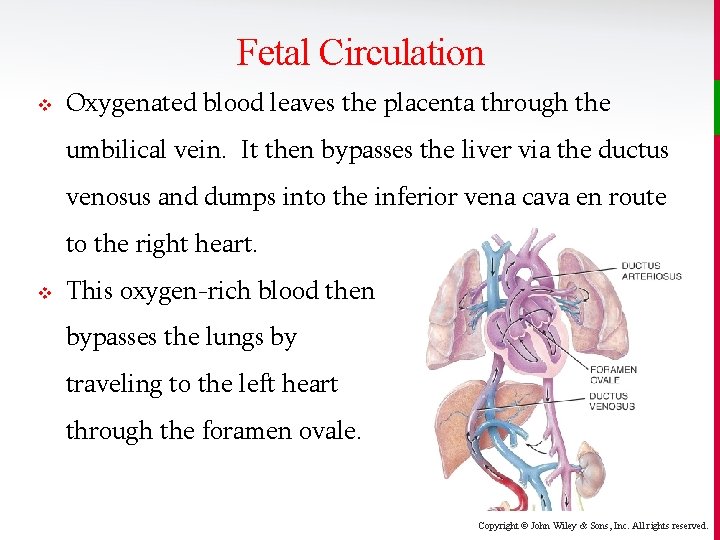
Fetal Circulation v Oxygenated blood leaves the placenta through the umbilical vein. It then bypasses the liver via the ductus venosus and dumps into the inferior vena cava en route to the right heart. v This oxygen-rich blood then bypasses the lungs by traveling to the left heart through the foramen ovale. Copyright © John Wiley & Sons, Inc. All rights reserved.
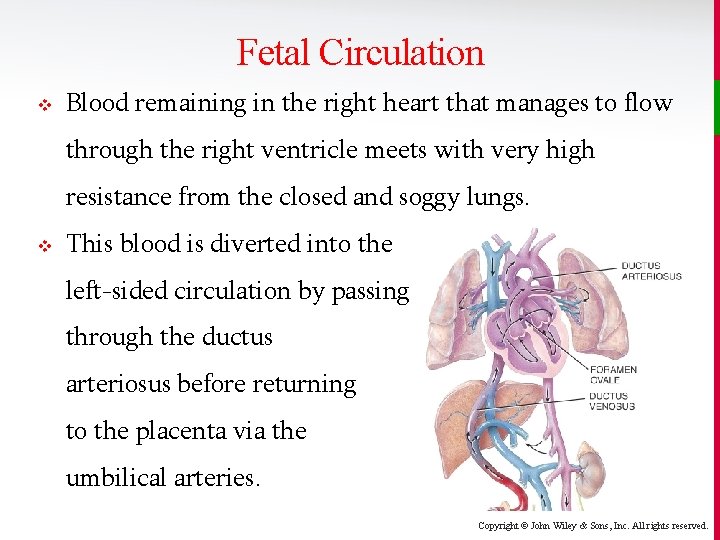
Fetal Circulation v Blood remaining in the right heart that manages to flow through the right ventricle meets with very high resistance from the closed and soggy lungs. v This blood is diverted into the left-sided circulation by passing through the ductus arteriosus before returning to the placenta via the umbilical arteries. Copyright © John Wiley & Sons, Inc. All rights reserved.
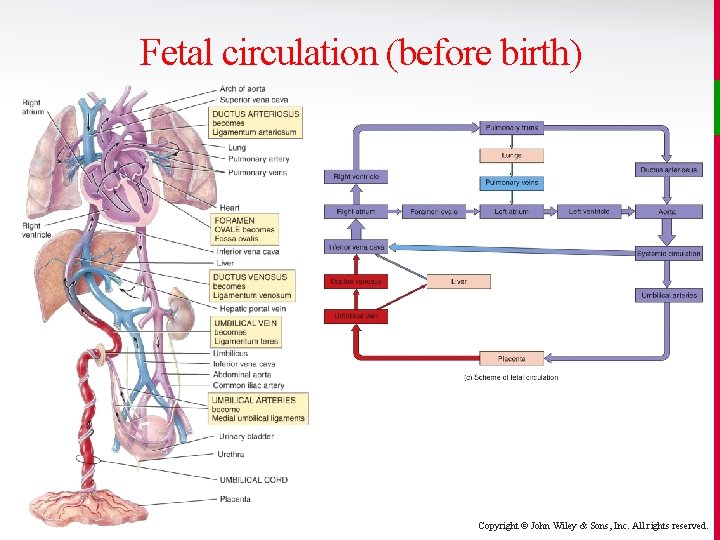
Fetal circulation (before birth) Copyright © John Wiley & Sons, Inc. All rights reserved.
Neonatal Circulation After Birth v At birth, the neonate’s lungs open and in just a few seconds, there is a massive drop in pulmonary vascular resistance. • Blood now entering the right heart now sees lower pressure looking into the lungs and has no “incentive” to flow through the foremen ovale or the ductus arteriosus. v Another change also occurs very rapidly - the umbilical cord is severed. • And so begins the adult pattern of blood flow. Copyright © John Wiley & Sons, Inc. All rights reserved.

Neonatal Circulation After Birth v Within hours, days, or weeks after birth, the umbilical vein atrophies to become the ligamentum teres. • The ductus venosus atrophies to become the ligamentum venosum. • The foramen ovale becomes the closed fossa ovale. • The ductus arteriosus atrophies to become the ligamentum arteriosum. • Umbilical arteries atrophy to become the medial umbilical ligaments. Copyright © John Wiley & Sons, Inc. All rights reserved.
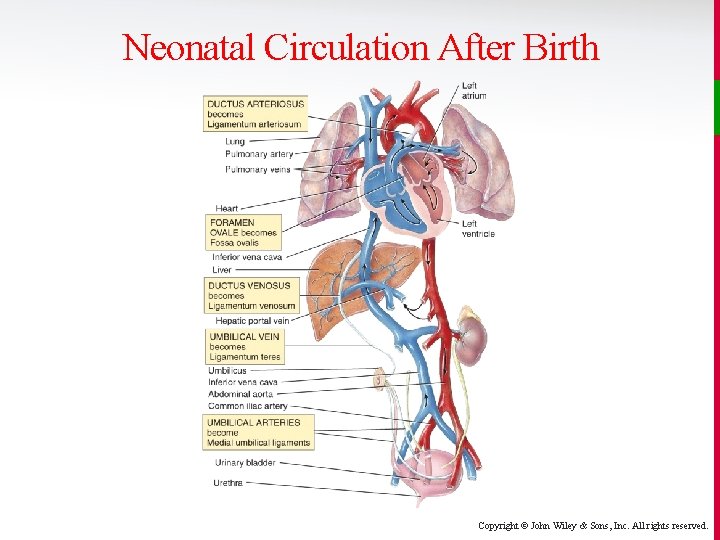
Neonatal Circulation After Birth Copyright © John Wiley & Sons, Inc. All rights reserved.

End of Chapter 21 Copyright 2012 John Wiley & Sons, Inc. All rights reserved. Reproduction or translation of this work beyond that permitted in section 117 of the 1976 United States Copyright Act without express permission of the copyright owner is unlawful. Request for further information should be addressed to the Permission Department, John Wiley & Sons, Inc. The purchaser may make back-up copies for his/her own use only and not for distribution or resale. The Publisher assumes no responsibility for errors, omissions, or damages caused by the use of these programs or from the use of the information herein. Copyright © John Wiley & Sons, Inc. All rights reserved.
- Slides: 78