Chapter 21 Blood Vessels and Circulation BIO 211

Chapter 21: Blood Vessels and Circulation BIO 211 Lecture Instructor: Dr. Gollwitzer 1

• Today in class we will discuss: – The relationship between blood flow and • Cardiac output • Pressure and resistance – Pressure differences in various vessels in the CVS – Blood pressure , mean arterial pressure, and pulse – The basis for systolic pressure and diastolic pressure – Total peripheral resistance and its major components 2

Cardiovascular Physiology • Goal of cardiovascular physiology – To maintain adequate blood flow through peripheral tissues and organs • Cardiovascular system (CVS) continuously adjusted to maintain homeostasis • Contracting ventricle must produce enough tension to force open the semilunar valve and eject blood • Determined by interplay between pressure and resistance in cardiovascular network • If no resistance to blood flow, heart would not have to generate pressure to force blood through pulmonary and systemic circuits 3
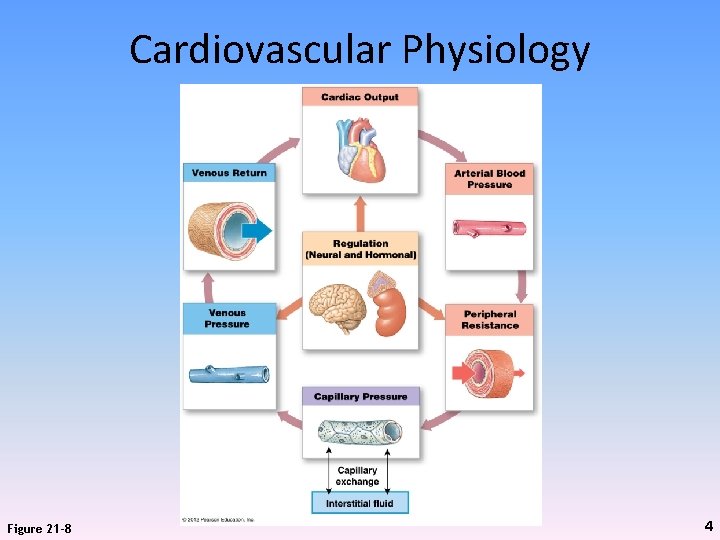
Cardiovascular Physiology Figure 21 -8 4
Cardiovascular Physiology • Cardiac output (CO) – Normally = blood flow – When CO goes up, blood flow through the capillary beds goes up; and vice versa • Blood (arterial) pressure (BP) – Responsible for maintaining blood flow within capillaries • Peripheral resistance controls: – Blood flow – Capillary pressure • Drives exchange via diffusion and osmosis between blood and interstitial fluid • Venous pressure – Due to venoconstriction – Aided by valves, skeletal muscle contraction • Venous return – Brings blood back to heart 5

Cardiovascular Pressures • General concepts – Liquids, including blood, cannot be compressed – Force exerted against an enclosed liquid (blood in CVS) generates hydrostatic pressure – If pressure gradient exists, hydrostatic pressure will push liquid from an area of higher pressure to an area of lower pressure 6
Cardiovascular Pressures • Pressure gradient of systemic circuit = circulatory pressure (approx 100 mm Hg) – Difference between pressure at base of ascending aorta (100 mm Hg) and entrance to R atrium (2 mm Hg) • This pressure needed to force blood through arterioles (resistance vessels) and into peripheral capillaries 7
Cardiovascular Pressures • 3 components – Blood pressure (BP) • = force exerted against vessel walls by blood in vessels in systemic arterial system • Ranges from 100 at heart to 35 mm Hg at start of capillary network • Capillary blood flow is directly proportional to BP – Capillary hydrostatic pressure • = Pressure in capillary beds • Declines from 35 to 18 mm Hg along length of capillary – Venous pressure • = Pressure in venous system • Pressure gradient from venules to R atrium approx. 18 mm Hg (ranges from 18 to 2 mm Hg) 8
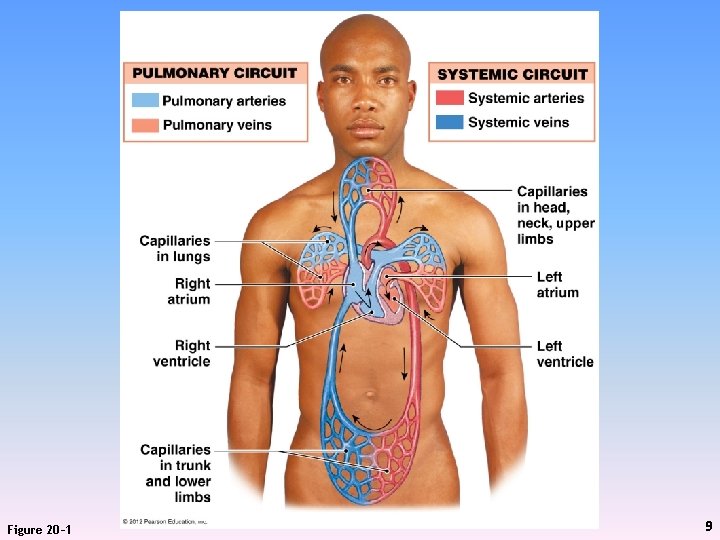
Figure 20– 1 9
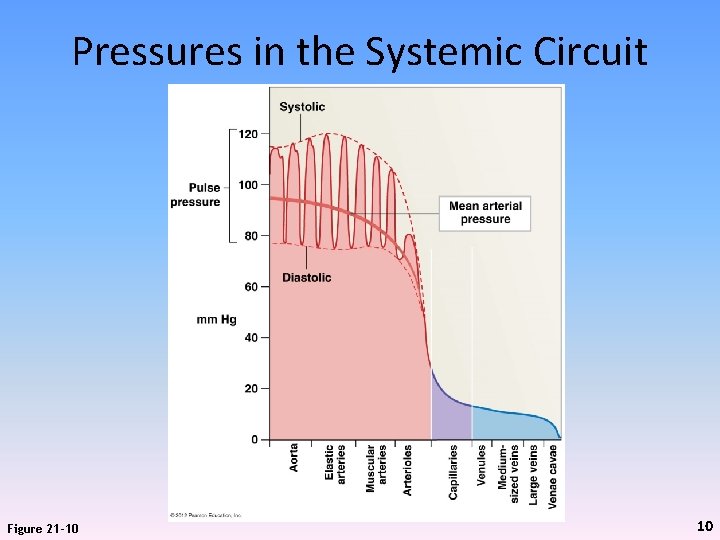
Pressures in the Systemic Circuit Figure 21 -10 10

Arterial Blood Pressure • Important because it maintains blood flow through capillary beds • Must be high enough to overcome peripheral resistance • Not stable – Rises during ventricular systole and falls during ventricular diastole – Systolic pressure (SP) = peak arterial pressure during ventricular systole – Diastolic pressure (DP) = minimum arterial pressure during diastole 11

Arterial Blood Pressure • Measure with sphygmomanometer – Compress brachial artery – Place stethoscope over artery, distal to compress – Inflate cuff until pressure is great enough to collapse artery and blood flow stops, pulse is eliminated – Let air out slowly • When pressure is less than SP = blood enters, pulse appears • When pressure is less than DP = pulse disappears and flow is continuous – Record by separating systolic and diastolic pressures by a slash mark (e. g. , 120/80) – Normal = 120/80 12
Arterial Blood Pressure • Pulse – = Rhythmic pressure oscillation that accompanies each heart beat – Common site: inner wrist (radial artery pressed against radius) • Pulse pressure (PP) – = Difference between systolic and diastolic pressure (i. e. , SP-DP) • Mean arterial pressure (MAP) – = Diastolic pressure + (pulse pressure/3), e. g. , – If SP = 120, DP = 80 • MAP = 80 + ((120 -80)/3) = 80 + 13 = 93 mm Hg 13

Resistance • Any force that opposes movement of fluid – Resistance of CVS • Due to friction between blood and vessel walls • Opposes movement of blood • The greater the resistance, the slower the movement of blood • For circulation to occur, pressure gradient must be great enough to overcome total peripheral resistance = resistance of the entire CVS (mostly arterial resistance b/c venous resistance so low) 14
Peripheral Resistance • = Resistance of the arterial system • For blood to flow into peripheral capillaries the pressure gradient must be great enough to overcome peripheral resistance • 3 sources of peripheral resistance – Vascular resistance (resistance of blood vessels) – Viscosity – Turbulence 15

Peripheral Resistance: Vascular Resistance • • = Resistance of blood vessels Largest component of peripheral resistance Due to friction between blood and vessel wall Depends on: – Vessel length – Vessel diameter 16

Peripheral Resistance: Vascular Resistance • Vessel length – Resistance directly proportional to length, i. e. , pulmonary vs. systemic circuit – Constant in adults • Vessel diameter – Much greater effect on resistance – Effects of friction occur in zone close to vessel wall • In large diameter vessel, blood near center does not encounter resistance • In small diameter vessel, nearly all blood is slowed by friction with walls – Increases exponentially as vessel diameter decreases • ½ diameter = 16 X resistance – Mechanisms that alter diameter of arterioles provide control over peripheral resistance and blood flow • Vessel diameter varies by vasodilation (bigger) and vasoconstriction (smaller) – Most resistance occurs in arterioles (smallest diameter) = resistance vessels 17
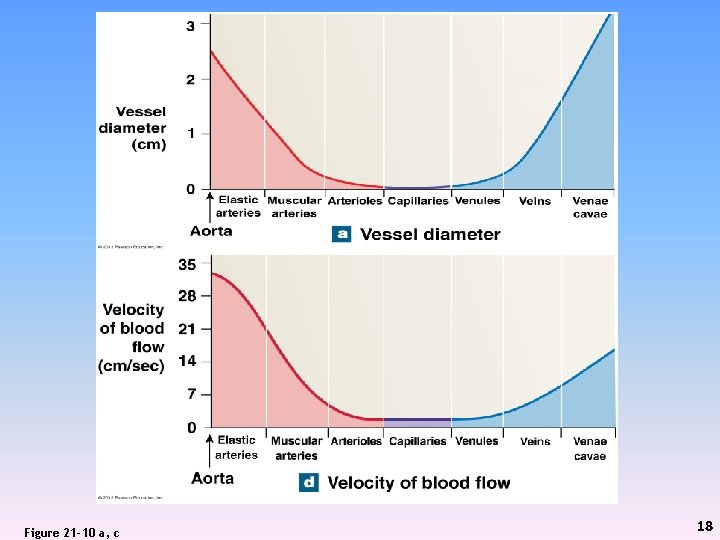
Figure 21 -10 a, c 18

Peripheral Resistance: Viscosity • = Resistance to flow caused by interactions among molecules in a liquid • Low viscosity liquids (water) flow at low pressure • Blood is 4 X as viscous as water due to presence of plasma proteins and blood cells • Viscosity remains stable except in anemia, polycythemia (elevated hematocrit) and other disorders that affect hematocrit 19

Peripheral Resistance: Turbulence • = Swirling action disturbs smooth flow of blood • Created by: – High flow rates • Between atria and ventricles • Between ventricles and trunks • In aorta – Irregular surfaces, e. g. , • Scar tissue • Atherosclerotic plaques – Sudden changes in vessel diameter, e. g. , • Vasoconstriction • Slows flow and increases resistance • Does not develop in small vessels except when damaged 20
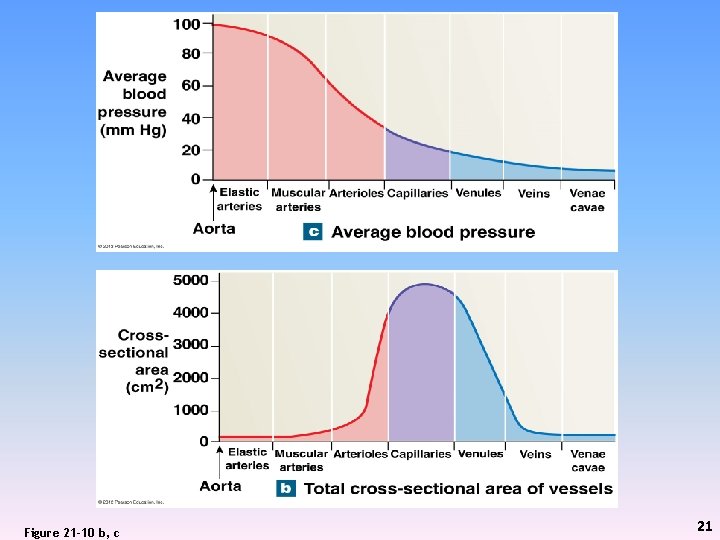
Figure 21 -10 b, c 21
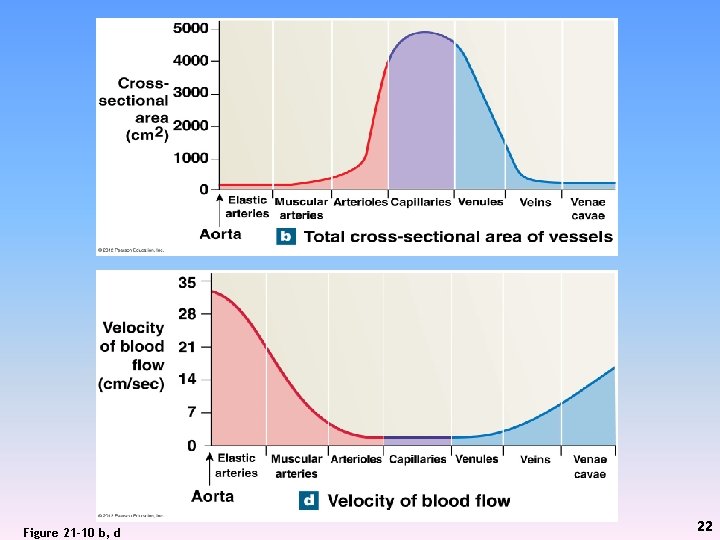
Figure 21 -10 b, d 22
Vascular Pathology • Arteriosclerosis – = Thickening and toughening of arterial walls; hardening of the arteries – Complications account for half of all deaths in US – CAD (coronary artery disease) = arteriosclerosis of coronary vessels – Stroke = result of arteriosclerosis of arteries supplying brain 23

Vascular Pathology • Arteriosclerosis (Cont. ) – 2 Forms of arteriosclerosis • Focal calcification – = Gradual degeneration of smooth muscle in tunica media and deposition of Ca 2+ salts – Typically involves arteries of limbs and genitals – Rapid and severe calcification may occur as complication of diabetes mellitus • Atherosclerosis – Aka: Fatty degeneration – = Damage to endothelial lining and formation of lipid deposits (plaque) in tunica media – Most common form of arteriosclerosis 24

Vascular Pathology • Arteriosclerosis (Cont. ) – Factors involved in development • Lipid levels; high cholesterol – High lipids in blood for an extended period of time – Monocytes begin removing them and become filled with lipid droplets (foam cells) – Attach to endothelial walls, release growth factors that stimulate smooth muscle to divide near the tunica interna, thickening the vessel wall, decreasing diameter – Other monocytes migrate resulting in a fatty mass of tissue (plaque) that projects into lumen – Because cells swollen with lipids, gaps appear in endothelial lining – Platelets appear to repair, clot forms which further restricts blood flow • High blood pressure, smoking, diabetes mellitus, obesity, stress, chronic bacterial infection, chronic inflammation 25
Vascular Pathology • Hypertension – = Abnormally high BP (>140/90) – Increases workload on heart, L ventricle gradually enlarges, more muscle mass – Greater O 2 demand, coronary circulation can’t keep pace, eventually coronary ischemia (inadequate blood supply) – Increases stress on walls of blood vessels, accelerates development of arteriosclerosis and aneurysms • Hypotension – Abnormally low BP (SP < 90 mm Hg) 26

• Today in class we will discuss: – The importance of maintaining adequate blood flow through the capillaries and the mechanisms involved in capillary exchange – Venous return and its role in moving blood – How autoregulatory, neural, and hormonal mechanisms compensate for a reduction in blood flow and blood pressure – How the cardiovascular system responds to hemorrhage 27

Capillary Exchange • As blood flows through peripheral tissues, BP forces water and solutes out of plasma, across capillary walls • Most of water is reabsorbed by capillaries • A portion (approx. 3. 6 L) enters the lymphatic system and eventually re-enters bloodstream 28

Blood-lymph Cycle • = Continuous movement of water out of the capillaries, through peripheral walls, to lymphatics, then back to bloodstream • Has 4 important functions – Ensures plasma and interstitial fluid are in constant communication – Accelerates distribution of nutrients, hormones, dissolved gases through tissues – Transports insoluble lipids and tissue proteins that can’t cross capillary walls – Flushes bacterial toxins and chemicals into immune system tissues 29

Capillary Exchange • 3 processes involved in moving materials across capillary walls – Filtration – Diffusion – Reabsorption 30
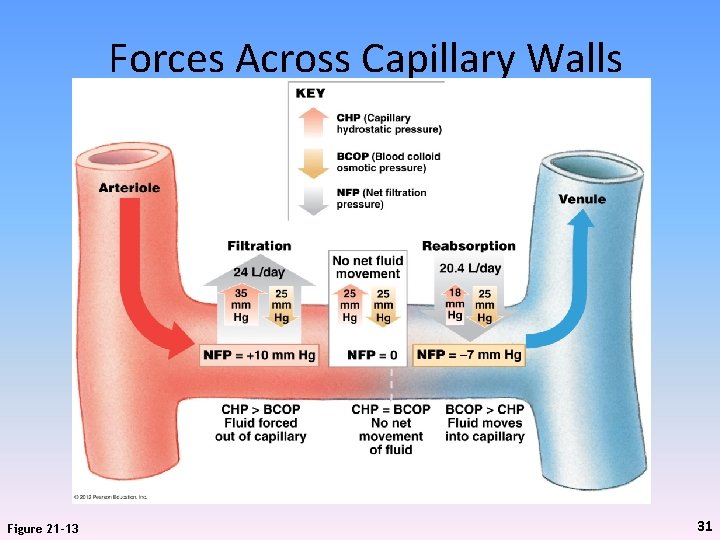
Forces Across Capillary Walls Figure 21 -13 31

Capillary Exchange • Filtration – Driving force is hydrostatic pressure • Forces water out of a solution from high to low pressure area (35 mm Hg in capillaries vs. 25 mm Hg in tissues) – When water is forced out of capillary walls, small solute particles travel with the water – Larger molecules and protein stay in bloodstream – Because BP drops from 35 to 18 mm Hg in capillaries, filtration occurs mostly at the arterial end 32

Capillary Exchange • Diffusion – = Movement of ions or molecules from high to low concentration – Does not involve pressure effects – Primary route for capillary exchange 33

Capillary Exchange • Capillary diffusion occurs by 5 routes – Between endothelial cells, e. g. , water, ions, small organic compounds (glucose, amino acids, urea) – Through channels in cell membrane, e. g. , water, Na+, K+, Ca 2+, Cl- ions – At fenestrated capillaries, e. g. , above and large watersoluble compounds otherwise unable to leave bloodstream • Found in hypothalamus, kidneys, endocrine organs, intestinal tract – Through endothelial cell membranes, e. g. , lipids (FAs, steroids), lipid-soluble materials including gases (O 2 and CO 2 – In sinusoids, e. g. , where plasma proteins are produced and enter bloodstream in liver 34

Capillary Exchange • Reabsorption – Result of osmosis = diffusion of water across membrane toward higher solute concentration, e. g, blood + plasma proteins – From arterial to venous ends of capillaries, rates of filtration and reabsorption change at about 25 mm Hg • Filtration higher at beginning and reabsorption higher at end – Of the 24 L of fluid that moves out of capillaries every day, 85% is reabsorbed – Remainder enters lymphatic vessels and eventually venous system 35

Capillary Exchange • Summary – Hydrostatic pressure • Forces water and solutes out of capillaries • Into interstitial fluid • At arterial end of capillary – Osmotic pressure • Pulls water and solutes into capillaries • Out of interstitial fluid • At venous end of capillary 36

Edema • = Abnormal accumulation of interstitial fluid (ECF) – Filtration out > reabsorption in – Results from a disturbance between hydrostatic and osmotic forces at capillary level – Causes • Damage to capillary, increase BP from heart problems, blockage of lymphatic vessels, kidney failure 37
Venous Pressure and Venous Return • BP very low at venules (18 mm Hg), but they provide very little resistance • As blood approaches heart – Veins become larger – Resistance drops even more – Velocity of blood increases • When individual stands, venous blood entering IVC must overcome gravity 38

Venous Pressure and Venous Return • 2 factors help venous blood overcome gravity – Muscular compression • Muscular contraction near vein push blood toward heart because of 1 -way valves • Is why standing still for long time results in little blood flow to the brain and person faints – Respiratory pump • When inhale: – – Thoracic cavity expands Pressure in pleural cavities drops Pulls air into lungs Also pulls blood into IVC and R atrium from smaller veins in abdominal cavity • When exhale: – Pressure in pleural cavities rises – Pushes blood into R atrium – Important during heavy exercise 39

Cardiovascular Regulation • 3 Regulatory mechanisms control cardiovascular function, i. e, CO and BP – Autoregulation • Local factors at tissue level cause immediate, localized adjustments – Neural mechanisms • Respond quickly to changes at specific sitesflex control – Endocrine mechanisms • Direct long-term changes 40
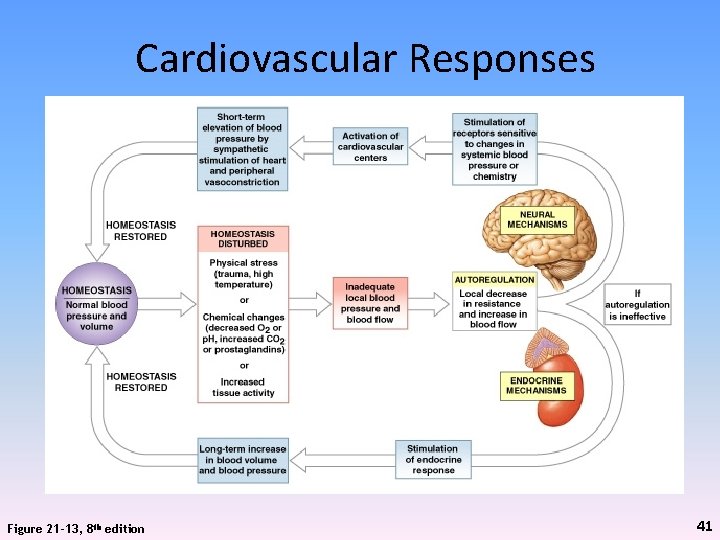
Cardiovascular Responses Figure 21 -13, 8 th edition 41

Cardiovascular Regulation: Autoregulation • Local factors change pattern of blood flow in capillary bed in response to chemical changes in interstitial fluid • Affect precapillary sphincters – Local vasodilators – dilate sphincters • Accelerate blood flow through tissues brings O 2, other nutrients to restore homeostasis • e. g. , low O 2 or high CO 2, lactic or other acid, NO, high K+ or H+, histamine, high temperatures – Local vasoconstrictors – constrict sphincters – e. g. , compounds produced by platelets and damaged tissues (antihemorrhage prostaglandins and thromboxanes from platelets and WBCs) • Cause immediate, localized hemostatic adjustments • If this fails, then neural and endocrine factors activated 42

Cardiovascular Regulation: Neural Mechanisms • Reflexes regulated through negative feedback loop • 2 types of reflex control – Baroreceptor reflexes – Chemoreceptor reflexes 43
Cardiovascular Regulation • Special cardiovascular receptors monitor conditions – Baroreceptors • Monitor and respond to stretch in blood vessels and atrium – Chemoreceptors • Monitor composition of arterial blood and CSF • Respond to changes in CO 2, or p. H in blood • Found near carotid sinus (carotid bodies) and aortic arch (aortic bodies) • Receptors trigger neural reflex arcs to neurons in cardiovascular centers in medulla oblongata 44
Cardiovascular Regulation: Neural Mechanisms • Baroreceptor reflexes – Stretch receptors respond to changes in BP – Found in vessel walls and heart (carotid sinuses, R atrium, aortic sinuses) – Controlled by ANS – When BP increases, CV centers • Dec HR • Cause peripheral vasodilation dec BP – When BP decreases, CV centers • Inc HR and stroke volume • Cause peripheral vasoconstriction inc BP – Maintains normal/adequate arterial pressure 45
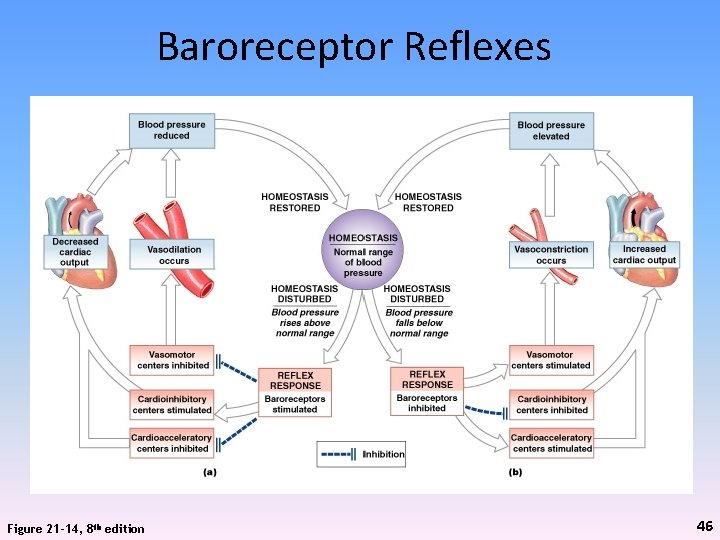
Baroreceptor Reflexes Figure 21 -14, 8 th edition 46

Cardiovascular Regulation: Neural Mechanisms • Chemoreceptor reflexes – Receptors respond to changes in O 2, CO 2 levels and p. H in blood and CSF – Found in aortic bodies, carotid bodies, and medulla oblongata – Lead to increased HR and BP by sympathetic activation or decreased by parasympathetic activation 47
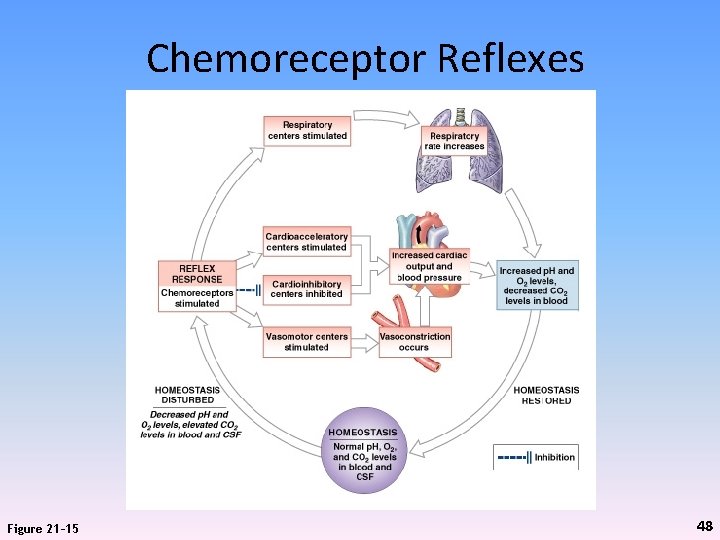
Chemoreceptor Reflexes Figure 21– 15 48

Cardiovascular Regulation: Endocrine Mechanisms • Short-term regulation – Of cardiac output and peripheral vasoconstriction (resistance) – With E and NE • Long-term regulation – Of BP and/or volume – With: • • ADH – increases BP and volume Angiotensin II – increases BP and volume Erythropoietin – increases volume Atrial natriuretic peptide (ANP) - decreases volume 49

Cardiovascular Regulation: Endocrine Mechanisms • ADH – Released from post pit in response to: • Low blood volume • High plasma Na+ • Angiotensin II – Immediate result is vasoconstriction that increases BP – Stimulates conservation of water at kidneys which prevents further drop in blood volume 50

Cardiovascular Regulation: Endocrine Mechanisms • Angiotensin II – Responds to decreased renal BP – Stimulates production of • Aldosterone from adrenal cortex which causes Na (and water) retention and K loss at kidneys • ADH production which causes water retention – Stimulates thirst – Increases CO – Stimulates vasoconstriction 51

Cardiovascular Regulation: Endocrine Mechanisms • Erythropoietin – Released at kidneys – Responds to low BP or O 2 – Stimulates RBC production and maturation which increases blood volume and improves O 2 carrying capacity 52

Cardiovascular Regulation: Endocrine Mechanisms • Atrial natriuretic peptide (ANP) – Natural diuretic produced by cardiac muscle cells in R atrium – Respond to excessive stretch during diastole – Reduces stress on heart • Decreases blood volume and BP by increasing Na loss at kidneys, promoting water loss, decreasing thirst 53
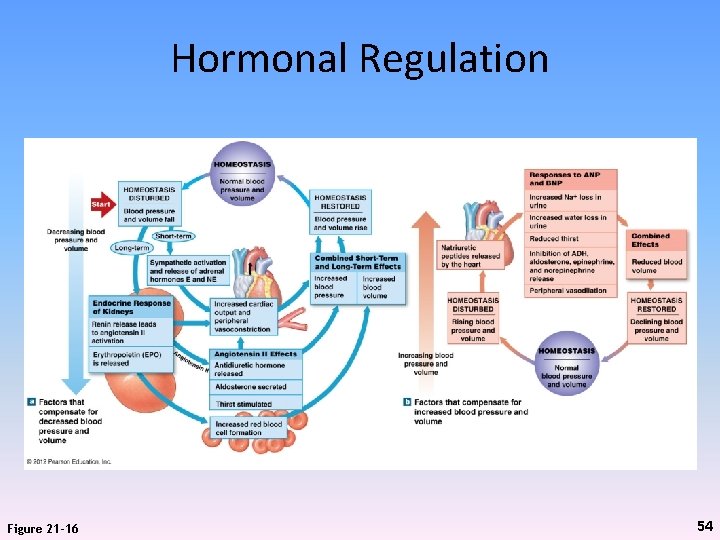
Hormonal Regulation Figure 21 -16 54

Circulatory Shock • Acute circulatory crisis marked by: – Low BP (hypotension) – Inadequate peripheral blood flow • Severe, potentially fatal symptoms develop as vital tissues become starved for O 2 and nutrients • Causes: – – Blood fluid loss (hemorrhage, dehydration, severe burns) Extensive peripheral vasodilation Heart damage External pressure on heart 55

Circulatory Shock • Symptoms – Hypotension (SP < 90 mm Hg) – Pale, cool (due to vasoconstriction), moist (clammy) skin (sweat glands activated) – Confusion, disorientation (due to dec. BP in brain) – Increased heart rate; rapid, weak pulse – Cessation of urination (due to reduced blood flow to kidneys) – Dec. blood p. H (acidosis) (due to lactic acid formed by O 2 starved tissues) 56

Circulatory Shock • When BP declines more than 35%: – Normal homeostatic mechanisms can no longer handle: • Sustained vasoconstriction • Mobilization of venous return – BP remains low damage to myocardium decreased CO decreased BP decreased flow to brain 57

Circulatory Shock • When MAP < 50 mm Hg – Carotid sinus baroreceptors massive activation of vasomotor centers in brain stem maximal vasoconstriction (central ischemic response) • Goal: preserve circulation to brain at expense of other tissues – May progress to irreversible shock • In absence of treatment, CV damage becomes irreversible • Conditions in heart, liver, kidneys, CNS deteriorate to point at which death will occur, even with medical treatment • Results in widespread peripheral vasodilation and immediate, fatal decline in BP (circulatory collapse) due to capillary collapse cell death 58

Circulatory Shock • Treatment – Prevent further fluid losses – Transfuse whole blood, plasma expanders, or blood substitutes 59

Age-related Changes • Linked to arteriosclerosis • Sudden pressure increase in (more inelastic) artery walls may cause aneurysm – Stroke – Myocardial infarction – Massive hemorrhage • Ca 2+ salts deposit on vessel walls – Stroke – Myocardial infarction • Thrombi form at atherosclerotic plaques 60
- Slides: 60