Chapter 20 The GramNegative Bacilli of Medical Importance

Chapter 20 The Gram-Negative Bacilli of Medical Importance

Aerobic Gram-Negative Bacilli • Large, diverse group of non-spore-forming bacteria • Wide range of habitats – – Zoonotic Respiratory Soil Water • All have outer membrane lipopolysaccharide of the cell wall – endotoxin 2

Aerobic Gram-Negative, Non-enteric Bacilli • Pseudomonas– opportunistic pathogens • Francisella – zoonotic pathogens • Bordetella and Legionella – mainly human pathogens 3

Pseudomonas aeruginosa Copyright © The Mc. Graw-Hill Companies, Inc. Permission required for reproduction or display. • Important decomposers and bioremediators • Reservoir: soil and water • Use aerobic respiration; do not ferment carbohydrates • Produce oxidase and catalase • Intestinal resident in 10% normal people • Resistant to soaps, dyes, quaternary ammonium disinfectants, drugs, drying • Frequent contaminant of ventilators, IV solutions, anesthesia equipment • Opportunistic pathogen © Science VU/Visuals Unlimited © Bottone E. J. and Perez A. A. , II, The Mount Sinai Hospital New York 4
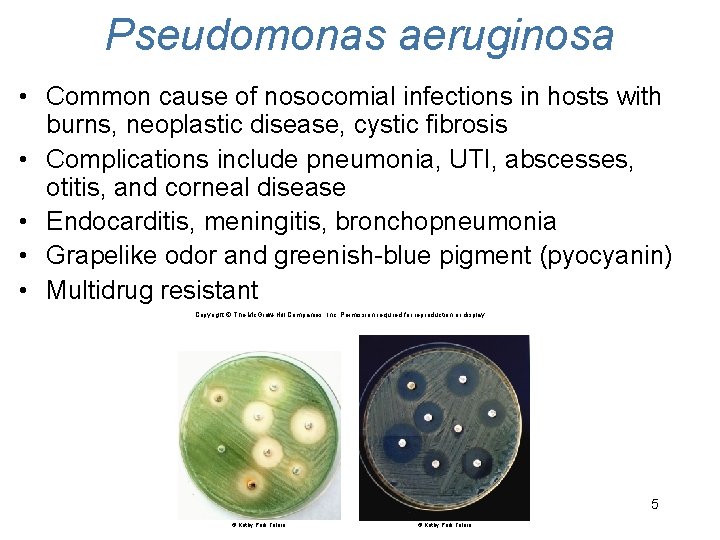
Pseudomonas aeruginosa • Common cause of nosocomial infections in hosts with burns, neoplastic disease, cystic fibrosis • Complications include pneumonia, UTI, abscesses, otitis, and corneal disease • Endocarditis, meningitis, bronchopneumonia • Grapelike odor and greenish-blue pigment (pyocyanin) • Multidrug resistant Copyright © The Mc. Graw-Hill Companies, Inc. Permission required for reproduction or display. 5 © Kathy Park Talaro

Concept Check: The main reservoir for Pseudomonas aeruginosa is A. Soil and Water B. Infected Individuals C. Asymptomatic Carriers D. Wild Animals

Related Gram-Negative Aerobic Rods • Genera Acinetobacter & Stenotrophomonas • Similar to pseudomonads • Wide variety of habitats in soil, water, and related environments • Obligate aerobes; do not ferment sugars • Motile, oxidase positive • Opportunistic 7
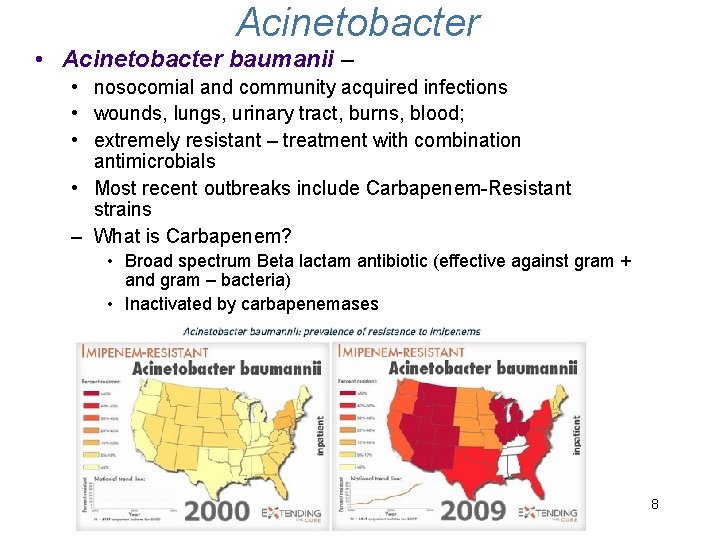
Acinetobacter • Acinetobacter baumanii – • nosocomial and community acquired infections • wounds, lungs, urinary tract, burns, blood; • extremely resistant – treatment with combination antimicrobials • Most recent outbreaks include Carbapenem-Resistant strains – What is Carbapenem? • Broad spectrum Beta lactam antibiotic (effective against gram + and gram – bacteria) • Inactivated by carbapenemases 8
Stenotrophomonas • Stenotrophomonas maltophilia – • nosocomial and community acquired infections • forms biofilms; • Contaminant of disinfectants (can grow in anti-microbial soap containing triclosan) • Contaminant of dialysis equipment, respiratory equipment, and catheters; water dispensers • clinical isolate in respiratory soft tissue, blood, CSF; • high resistance to multiple drugs 9
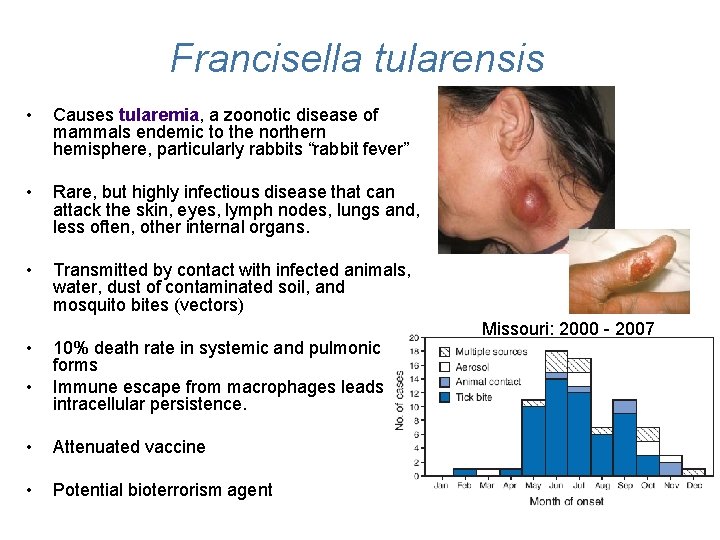
Francisella tularensis • Causes tularemia, a zoonotic disease of mammals endemic to the northern hemisphere, particularly rabbits “rabbit fever” • Rare, but highly infectious disease that can attack the skin, eyes, lymph nodes, lungs and, less often, other internal organs. • Transmitted by contact with infected animals, water, dust of contaminated soil, and mosquito bites (vectors) • • 10% death rate in systemic and pulmonic forms Immune escape from macrophages leads to intracellular persistence. • Attenuated vaccine • Potential bioterrorism agent Missouri: 2000 - 2007 10

Bordetella pertussis • Minute, encapsulated coccobacillus • Causes pertussis or whooping cough, a communicable childhood affliction • Acute respiratory syndrome • Often severe, life-threatening complications in babies • Reservoir – apparently healthy carriers • Transmission by direct contact or inhalation of aerosols Copyright © The Mc. Graw-Hill Companies, Inc. Permission required for reproduction or display. 11 CDC
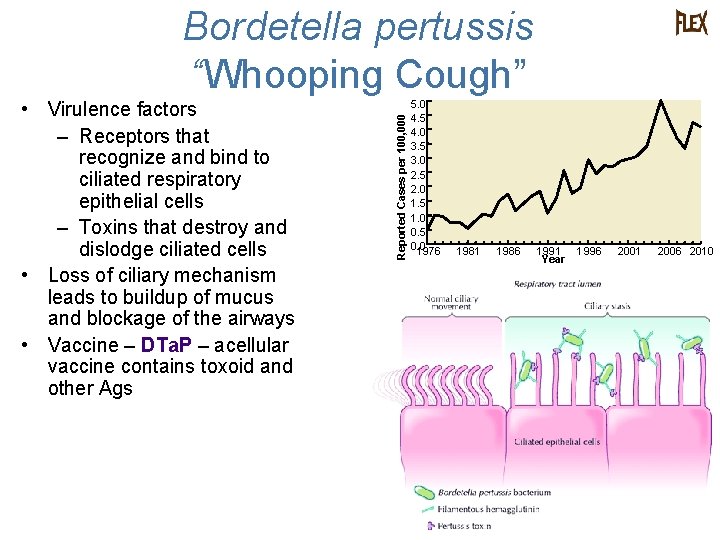
• Virulence factors – Receptors that recognize and bind to ciliated respiratory epithelial cells – Toxins that destroy and dislodge ciliated cells • Loss of ciliary mechanism leads to buildup of mucus and blockage of the airways • Vaccine – DTa. P – acellular vaccine contains toxoid and other Ags Reported Cases per 100, 000 Bordetella pertussis “Whooping Cough” 5. 0 4. 5 4. 0 3. 5 3. 0 2. 5 2. 0 1. 5 1. 0 0. 5 0. 0 1976 1981 1986 1991 Year 1996 2001 2006 2010
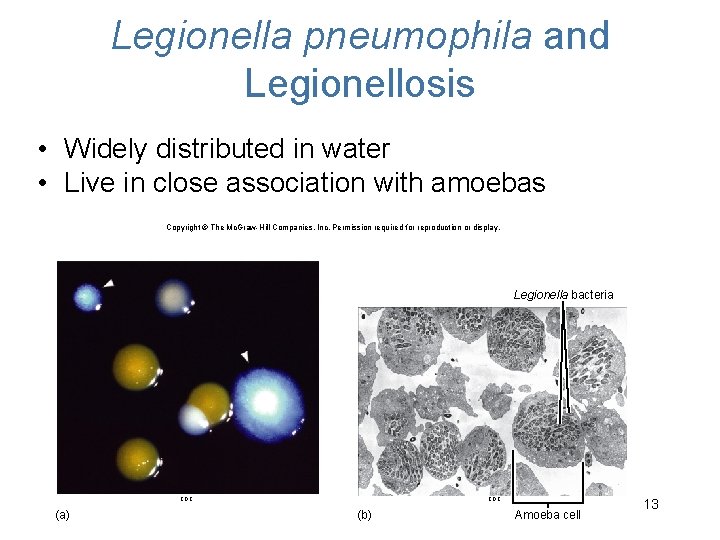
Legionella pneumophila and Legionellosis • Widely distributed in water • Live in close association with amoebas Copyright © The Mc. Graw-Hill Companies, Inc. Permission required for reproduction or display. Legionella bacteria CDC (a) CDC (b) Amoeba cell 13
Legionella pneumophila Legionellosis • 1976 epidemic of pneumonia afflicted 200 American Legion members attending a convention in Philadelphia and killed 29 (source: hotel air conditioner) • http: //www. nytimes. com/2006/08/01/heal th/01 docs. html? pagewanted=all&_r=0 • Not communicable • Sources: contaminated hot tubs, cooling towers, hot water tanks, plumbing systems, and decorative fountains • Nosocomial disease in elderly patients (most prevalent in males over 50) • Legionnaires disease – • • Pneumonia, Cough, Shortness of breath, High fever, Muscle aches, Headaches Pontiac fever – – Milder form of Legionaires disease, lacking pneumonia and lasting only 2 -5 days • • Fatality rate of 3 -30% Treatment: Azithromycin 14
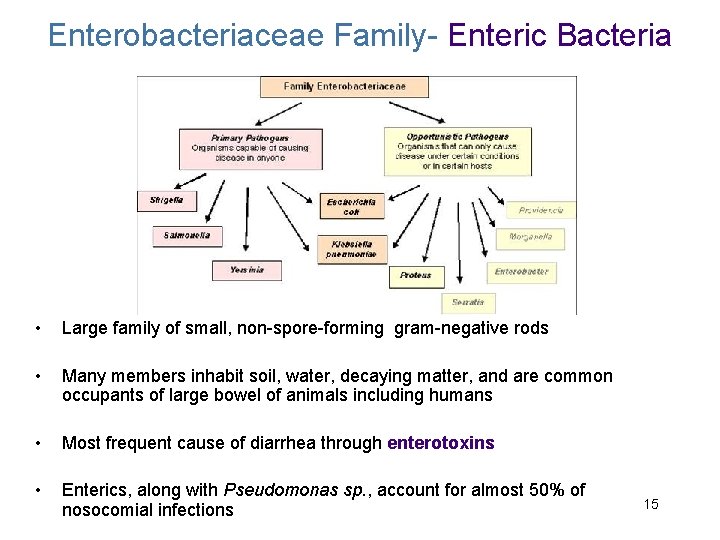
Enterobacteriaceae Family- Enteric Bacteria • Large family of small, non-spore-forming gram-negative rods • Many members inhabit soil, water, decaying matter, and are common occupants of large bowel of animals including humans • Most frequent cause of diarrhea through enterotoxins • Enterics, along with Pseudomonas sp. , account for almost 50% of nosocomial infections 15
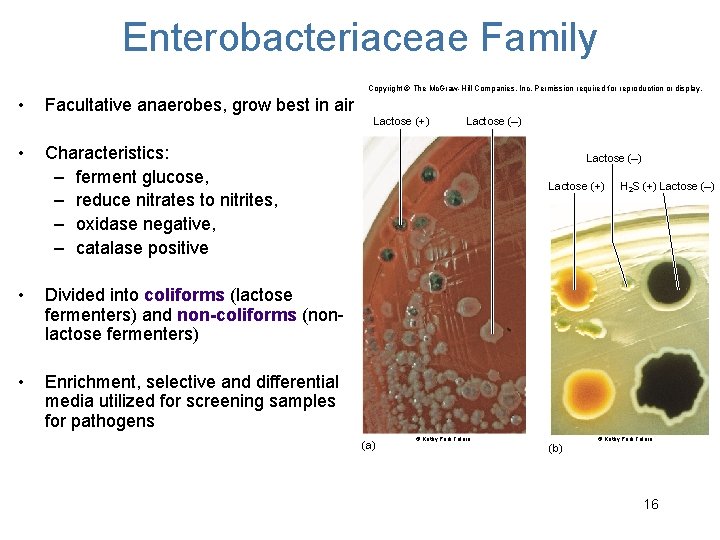
Enterobacteriaceae Family Copyright © The Mc. Graw-Hill Companies, Inc. Permission required for reproduction or display. • Facultative anaerobes, grow best in air • Characteristics: – ferment glucose, – reduce nitrates to nitrites, – oxidase negative, – catalase positive Lactose (+) • Divided into coliforms (lactose fermenters) and non-coliforms (nonlactose fermenters) • Enrichment, selective and differential media utilized for screening samples for pathogens Lactose (–) Lactose (+) (a) © Kathy Park Talaro H 2 S (+) Lactose (–) © Kathy Park Talaro (b) 16
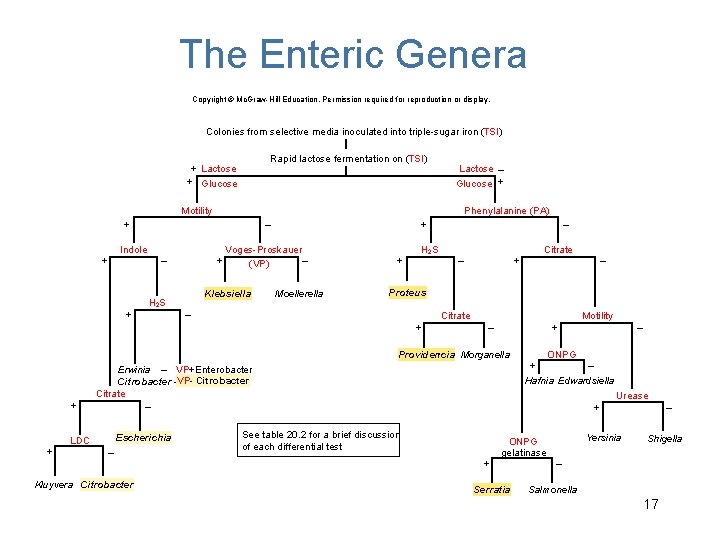
The Enteric Genera Copyright © Mc. Graw-Hill Education. Permission required for reproduction or display. Colonies from selective media inoculated into triple-sugar iron (TSI) Rapid lactose fermentation on (TSI) + Lactose + Glucose Lactose – Glucose + Motility Phenylalanine (PA) + Indole + + – Klebsiella H 2 S + Voges-Proskauer – (VP) Moellerella + – H 2 S + – – Citrate Motility + – Providencia Morganella Erwinia – VP+Enterobacter Citrobacter –VP- Citrobacter Citrate – Escherichia LDC + – – ONPG + – Hafnia Edwardsiella Urease + See table 20. 2 for a brief discussion of each differential test Yersinia ONPG gelatinase + Kluyvera Citrobacter – Proteus + + Citrate Serratia – Shigella – Salmonella 17
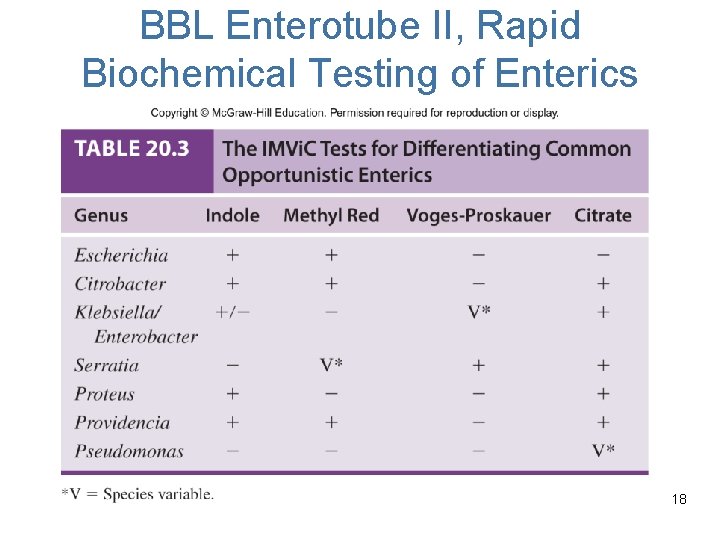
BBL Enterotube II, Rapid Biochemical Testing of Enterics 18

Enteric Antigenic Structures and Virulence Factors Complex surface antigens contribute to pathogenicity and trigger immune response: • H – flagellar Ag • K – capsule and/or fimbrial Ag • O – somatic or cell wall Ag – all have • Endotoxin • Exotoxins Copyright © The Mc. Graw-Hill Companies, Inc. Permission required for reproduction or display. Capsule (K antigen, or Vi in Salmonella Somatic (O antigen, or cell wall antigen) Flagellar (H antigen) 19

Concept Check: Which of the following is true of the enterics? A. Some are normal flora B. Some release endotoxin C. Some release enterotoxins D. All of the above are true 20
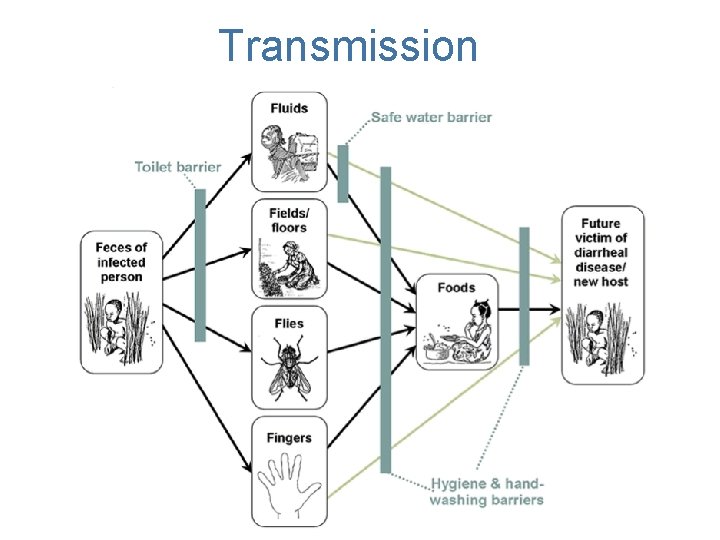
Transmission 21
Escherichia coli: The Most Prevalent Enteric Bacillus • Most common aerobic and nonfastidious bacterium in gut • 150 strains • Some have developed virulence through plasmid transfer, others are opportunists 22
Escherichia coli • Pathogenic strains frequent agents of infantile diarrhea – greatest cause of mortality among babies • Causes ~70% of traveler’s diarrhea • Causes 50 -80% UTI • Coliform count – indicator of fecal contamination in water 23

Pathogenic Strains of E. coli • Enterotoxigenic E. coli causes severe diarrhea due to heat-labile toxin and heat-stable toxin – “Traveler’s diarrhea” – Onset within 5 -7 days – stimulate secretion and fluid loss; also has fimbriae • Enteroinvasive E. coli causes inflammatory disease of the large intestine – Enteroinvasive dysentery similar to Shigella dysentery • Enteropathogenic E. coli linked to wasting form infantile diarrhea – Etiology less understood 24

Pathogenic Strains of E. coli • Enterohemorrhagic E. coli, causes hemorrhagic syndrome and kidney damage – Prototypical strain: O 157: H 7 – Shiga toxin – 10% of cases lead to hemolytic uremic syndrome (HUS) – Abnormal and premature lysis of RBCs clog filtering system in the kidney – More prevalent in children – Onset after 2 -14 days of bloody diarrhea – Infectious dose: 100 cells 25
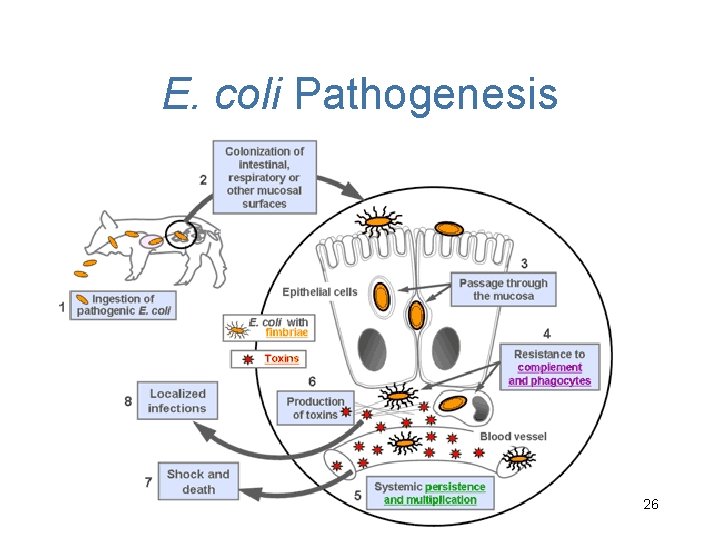
E. coli Pathogenesis 26
Opportunistic Coliforms • Klebsiella pneumoniae – normal inhabitant of respiratory tract, has large capsule, cause of nosocomial pneumonia, meningitis, bacteremia, wound infections, and UTIs 27
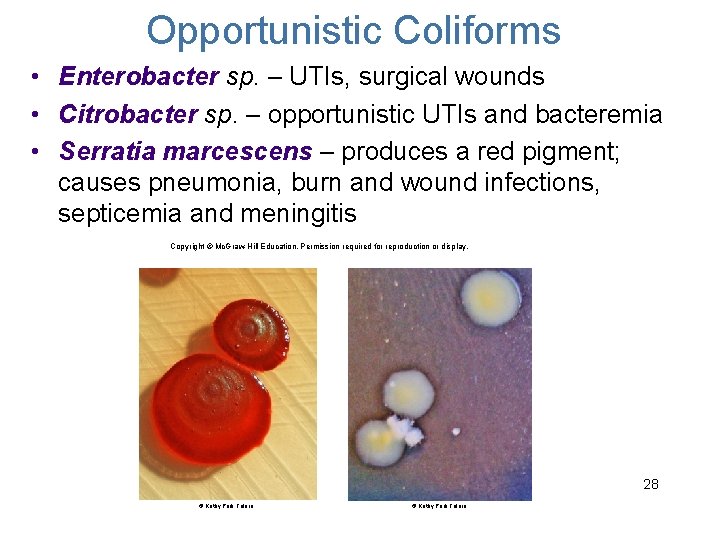
Opportunistic Coliforms • Enterobacter sp. – UTIs, surgical wounds • Citrobacter sp. – opportunistic UTIs and bacteremia • Serratia marcescens – produces a red pigment; causes pneumonia, burn and wound infections, septicemia and meningitis Copyright © Mc. Graw-Hill Education. Permission required for reproduction or display. 28 © Kathy Park Talaro

Typhoid Fever • Salmonella typhi – most serious pathogen of the genus; cause of typhoid fever; human host • Flagellated; survive outside the host • Resistant to chemicals – bile and dyes Note the red spots on the skin 29
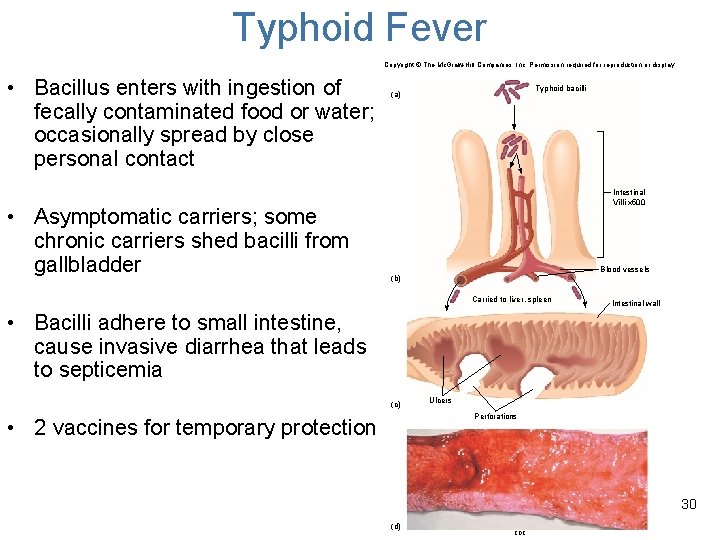
Typhoid Fever Copyright © The Mc. Graw-Hill Companies, Inc. Permission required for reproduction or display. • Bacillus enters with ingestion of fecally contaminated food or water; occasionally spread by close personal contact • Asymptomatic carriers; some chronic carriers shed bacilli from gallbladder Typhoid bacilli (a) Intestinal Villi x 500 Blood vessels (b) Carried to liver, spleen Intestinal wall • Bacilli adhere to small intestine, cause invasive diarrhea that leads to septicemia (c) Ulcers Perforations • 2 vaccines for temporary protection 30 (d) CDC
Salmonelloses • Salmonelloses other than typhoid fever are called enteric fevers, Salmonella food poisoning, and gastroenteritis • Usually less severe than typhoid fever but more prevalent • Enteric fevers are caused by one of many serotypes of Salmonella enteritidis; all zoonotic in origin but humans can become carriers – Cattle, poultry, rodents, reptiles, animal, and dairy products – Fomites contaminated with animal intestinal flora Why would medicines that slow diarrhea not be prescribed for Salmonella poisoning? 31

Shigella sp. • Shigellosis, an incapacitating dysentery – Crippling abdominal cramps – Frequent defecation of watery stool filled with mucus and blood • Etiological agents – Shigella dysenteriae, S. sonnei, S. flexneri, S. boydii • Shigella sp. are primarily human pathogens, though can infect apes

Shigella sp. • Virulence Factor : Shiga-toxin – Injures nerve cells, the intestine, and kidneys • Site of infection – Mucosa of the large intestines – Most initial damage is due to the inflammatory response – Endotoxins promote fever – Enterotoxins damage the intestinal mucosa and villi causing bleeding and heavy mucous secretions

Nonenteric Yersinia pestis and Plague • Nonenteric Copyright © The Mc. Graw-Hill Companies, Inc. Permission required for reproduction or display. • Tiny, gram-negative rod, unusual bipolar staining and capsules • Virulence factors – capsular and envelope proteins protect against phagocytosis and foster intracellular growth CDC – Coagulase – Endotoxin – Murine toxin – highly toxic to mice but necessary for survival in fleas 34

Yersinia pestis • Responsible for the Bubonic plague also known as the Black Death • Killed an estimated 25 million people, 30 -60% of the European population • Flea vectors – bacteria replicates in gut, coagulase causes blood clotting that blocks the esophagus; flea becomes ravenous • 50 -90% Mortality rate if left untreated • Lives in infamy in a Children’s Rhyme 35
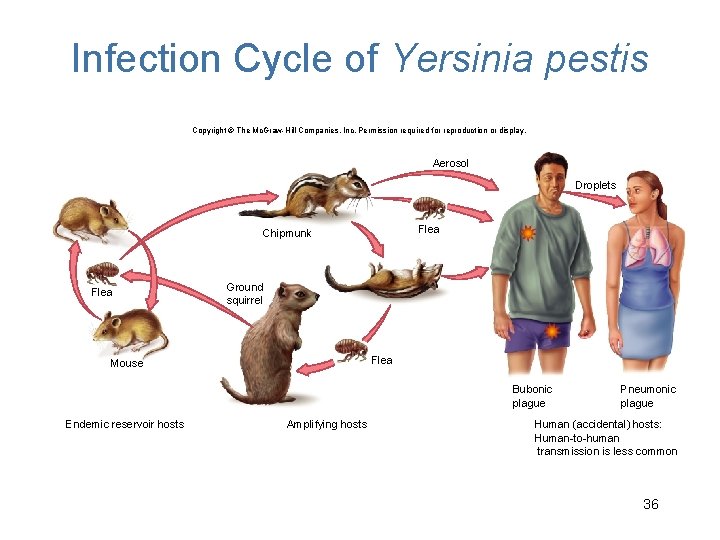
Infection Cycle of Yersinia pestis Copyright © The Mc. Graw-Hill Companies, Inc. Permission required for reproduction or display. Aerosol Droplets Flea Chipmunk Flea Ground squirrel Flea Mouse Bubonic plague Endemic reservoir hosts Amplifying hosts Pneumonic plague Human (accidental) hosts: Human-to-human transmission is less common 36

Pathology of Plague • Infectious Dose: 3 -50 bacilli • Bubonic – bacillus multiplies in flea bite, enters lymph, causes necrosis and swelling called a bubo in groin or axilla • Septicemic – progression to massive bacterial growth; virulence factors cause intravascular coagulation subcutaneous hemorrhage and purpura – black plague • Pneumonic – infection localized to lungs, highly contagious; fatal without treatment 37

Plague as a Biological Weapon – Widespread availability of Y. pestis in microbe banks around the world. – There is widespread natural availability of the Y. pestis bacteria in endemic areas – Reports indicate that techniques for mass production and aerosol dissemination of Y. pestis have been developed. – The fatality rate of pneumonic plague in untreated cases is extremely high. – Plague has the potential for secondary spread from person to person following an attack. – Y. pestis can be disseminated in aerosol form. – Plague has a low infectious dose. – Antibiotic resistant strains of Y. pestis exist in nature. 38
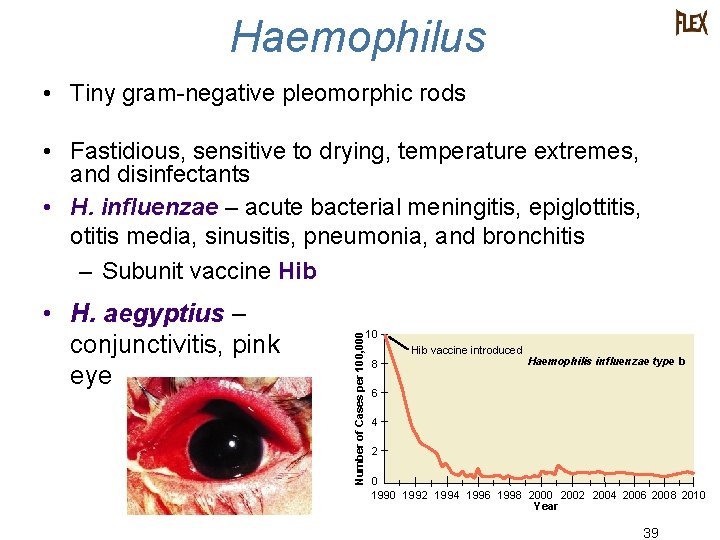
Haemophilus • Tiny gram-negative pleomorphic rods • H. aegyptius – conjunctivitis, pink eye CDC Number of Cases per 100, 000 • Fastidious, sensitive to drying, temperature extremes, and disinfectants • H. influenzae – acute bacterial meningitis, epiglottitis, otitis media, sinusitis, pneumonia, and bronchitis – Subunit vaccine Hib 10 Hib vaccine introduced 8 Haemophilis influenzae type b 6 4 2 0 1992 1994 1996 1998 2000 2002 2004 2006 2008 2010 Year 39

Prevention Food-borne illnesses All communicable illnesses • Prevent pathogen entry into the food chain • Provide adequate sanitation • Proper hand washing • Clean fruits, vegetable and areas where food is consumed • Cook food thoroughly especially meats/eggs • Pasteurize milk 40

Concept Check: The bubo of bubonic plague is a/an A. Ulcer where the flea bite occurred B. Granuloma in the skin C. Enlarged lymph node D. Infected sebaceous gland
- Slides: 41