Chapter 20 Liver Biochemistry The function of liver
Chapter 20 Liver Biochemistry

The function of liver Liver is the largest and metabolically the most complex organ in our body. It performs the following functions: • It decomposes and cleanses all the toxic substances of the body; • It generates the bile-juice to help digestion; • It regulates the glucose, lipid and protein metabolism;

The function of liver • It manufactures numbers of protein e. g. serum albumin; • It stores fat soluble vitamins, minerals; • It is a major energy consuming organ, hence to maintain the body temperature and the weight of the body, etc.

We will learn: -The Role of liver in metabolism -Hepatic Biotransformation -Metabolism of bile acid -Bile pigment Metabolism and jaundice

the role of liver in metabolism • Carbohydrate metabolism • Lipid metabolism • Protein metabolism

The role in carbohydrate metabolism Keep normal blood sugar • Glycogenesis: after a meal, liver take up excess glucose in blood and synthesize glycogen • Glycogenolysis: when level of blood sugar begin to decline, liver activate glycogenolysis to export glucose back into the blood

The role in carbohydrate metabolism Keep normal blood sugar • Glyconeogenesis: when hepatic glycogen reserves become exhausted, liver begin synthesizing glucose out of such things as amino acids and non-hexose carbohydrates

The role in lipid metabolism • oxidizes triglycerides to produce energy or ketone bodies. • synthesizes lipoproteins • converts excess carbohydrates and proteins into fatty acids and triglyceride, which are then exported and stored in adipose tissue • synthesizes large quantities of cholesterol and phospholipids. Some of them is packaged with lipoproteins, the remainder is excreted in bile as cholesterol or after conversion to bile acids.

The role in protein metabolism • Deamination and transamination of amino acids, followed by conversion of the non-nitrogenous part of those molecules to glucose or lipids. • Removal of ammonia from the body by synthesis of urea. • Synthesis of non-essential amino acids. • Synthesis of most of the plasma proteins.

Section 2 hepatic biotransformation

What is biotransformation? • Nonnutritive compounds Poorly soluble, biologically active, some toxic -endogenous: ammonia, amine, hormones -exogenous: drugs, food additives, pollutants • The liver has the function by which various nonnutritive compounds can be metabolized to form lower toxic or more water-soluble before being excreted from the body, these processes are named biotransformation.

What is biotransformation? • a series of enzyme-catalyzed process in which nonnutritive compounds are added polar group and become more water-soluble and easily to be excreted from kidneys. • Inactivate or detoxicate the nonnutritive compounds, make it easy to be excreted. • Liver is the main site of biotransformation

The basic reactions of biotransformation • Biotransformation processes often have two major phases -Phase I: oxidation, reduction, hydrolysis -Phase II: conjugation compounds + donor substrate polar metabolites
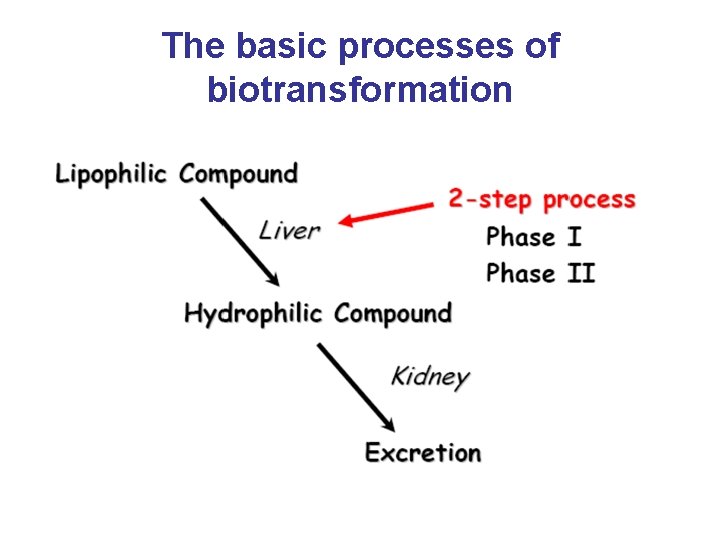
The basic processes of biotransformation

Phase I reaction • Expose a polar group (-OH, -COOH, -NH 2) on the substrate to prepare a lipophilic compound to be hydrophilic • Enzymes are mainly located in liver ER membrane, others in the cytoplasm or mitochondria

Phase I reaction • oxidation - Microsomal monooxygenase - Mitochondrial monoamine oxidase (MAO) - alcohol dehydrogenase(ADH) and aldehyde dehydrogenase(ALDH)
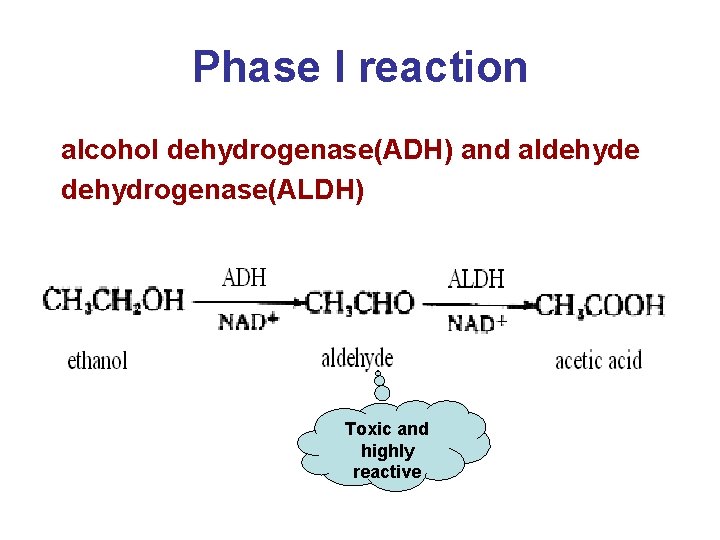
Phase I reaction alcohol dehydrogenase(ADH) and aldehyde dehydrogenase(ALDH) Toxic and highly reactive
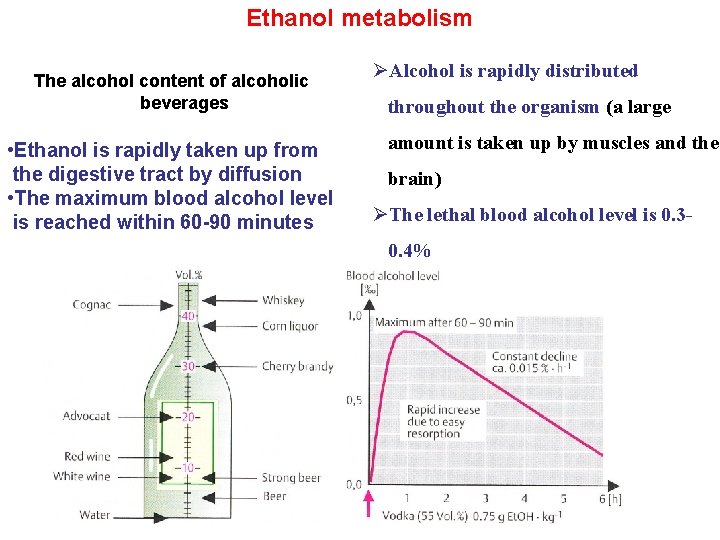
Ethanol metabolism The alcohol content of alcoholic beverages • Ethanol is rapidly taken up from the digestive tract by diffusion • The maximum blood alcohol level is reached within 60 -90 minutes ØAlcohol is rapidly distributed throughout the organism (a large amount is taken up by muscles and the brain) ØThe lethal blood alcohol level is 0. 30. 4%
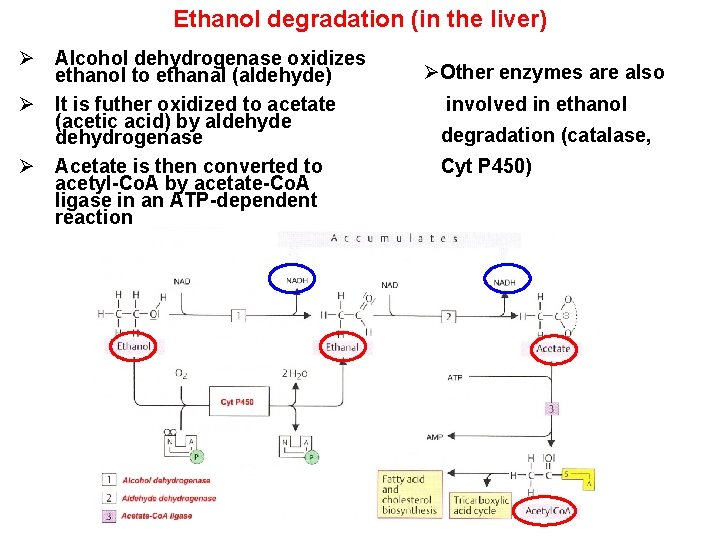
Ethanol degradation (in the liver) Ø Alcohol dehydrogenase oxidizes ethanol to ethanal (aldehyde) Ø It is futher oxidized to acetate (acetic acid) by aldehyde dehydrogenase Ø Acetate is then converted to acetyl-Co. A by acetate-Co. A ligase in an ATP-dependent reaction ØOther enzymes are also involved in ethanol degradation (catalase, Cyt P 450)
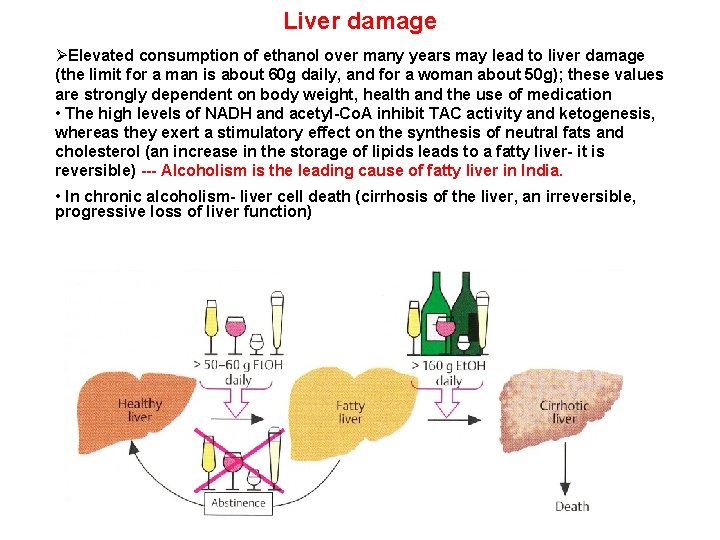
Liver damage ØElevated consumption of ethanol over many years may lead to liver damage (the limit for a man is about 60 g daily, and for a woman about 50 g); these values are strongly dependent on body weight, health and the use of medication • The high levels of NADH and acetyl-Co. A inhibit TAC activity and ketogenesis, whereas they exert a stimulatory effect on the synthesis of neutral fats and cholesterol (an increase in the storage of lipids leads to a fatty liver- it is reversible) --- Alcoholism is the leading cause of fatty liver in India. • In chronic alcoholism- liver cell death (cirrhosis of the liver, an irreversible, progressive loss of liver function)

Phase II reaction • The function of Phase II reaction: inactivate biologically active substances of form more polar (more easily excretable) derivatives. • Conjugate compound to a water soluble adduct using the polar handle from Phase I (containing -OH, -COOH, -NH 2 ) • Donor substrate: Glucuronic acid, Sulfate, acetate, Glutathione, Glycine
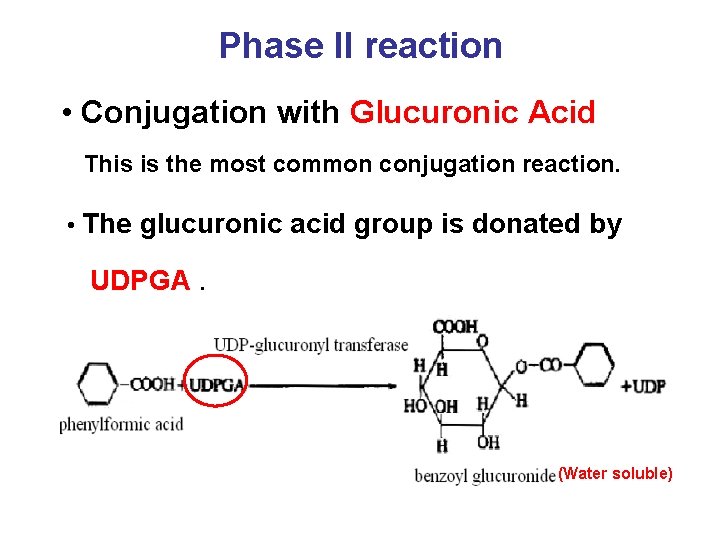
Phase II reaction • Conjugation with Glucuronic Acid This is the most common conjugation reaction. • The glucuronic acid group is donated by UDPGA. (Water soluble)

Characteristics of biotransformation • Continuity of the reactions • Variety of the types of reactions • Duality of deintoxication and causing toxin

Influence factors of biotransformation • Many factors can influence the effectiveness of biotransformation. • Such as age, gender, genetic variability, nutrition, disease, exposure to other chemicals, dose level, etc. • Biotransformation capabilities are decreased in the new-borns and the aged.

Section 3 The metabolism of bile acids

bile • Produce: from liver • Store: in gallbladder • Function: digest fatty food

bile • During interdigestive period (between meal) Bile is stored in the gallbladder, and concentrated. • In the fed state (after meal) The gallbladder contracts, forcing bile into the duodenum to digest fatty food.

bile • Hepatic bile: just secreted from liver. it is pellucid • Gallbladder bile: hepatic bile passed into the gallbladder, the gallbladder concentrates this bile, and secret some mucus into it, make the bile more potent, then the bile is named as gallbladder bile • Solids: bile acid(50%-70%), lecithin, cholesterol, bilirubin

Bile acid According to its structure • free bile acids: cholic acid, chenodeoxycholic acid, lithocholic acid • conjugated bile acids: free bile acids conjugate with glycine or taurine to form conjugated bile acids.
Bile acid Glycocholic acids Taurocholic acids Glycochenodeoxycholic acids conjugated bile acids Taurochenodeoxycholic acids Glycodeoxycholic acids Taurodeoxycholic acids Glycolithocholic acids Taurolithocholic acids
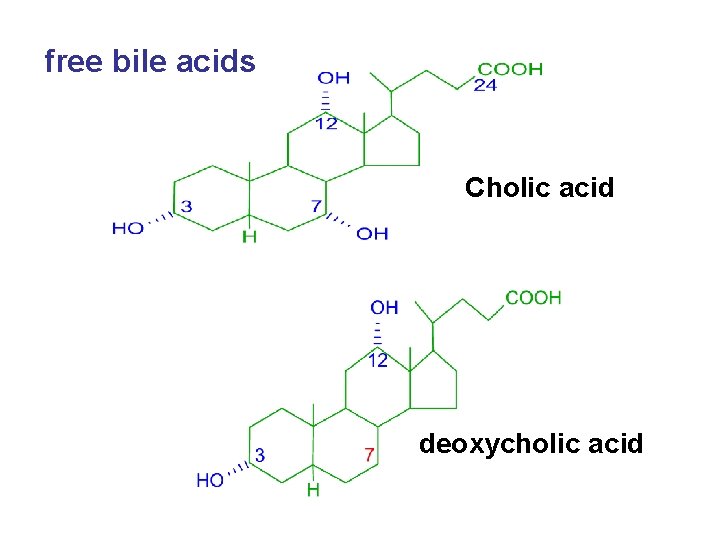
free bile acids Cholic acid deoxycholic acid
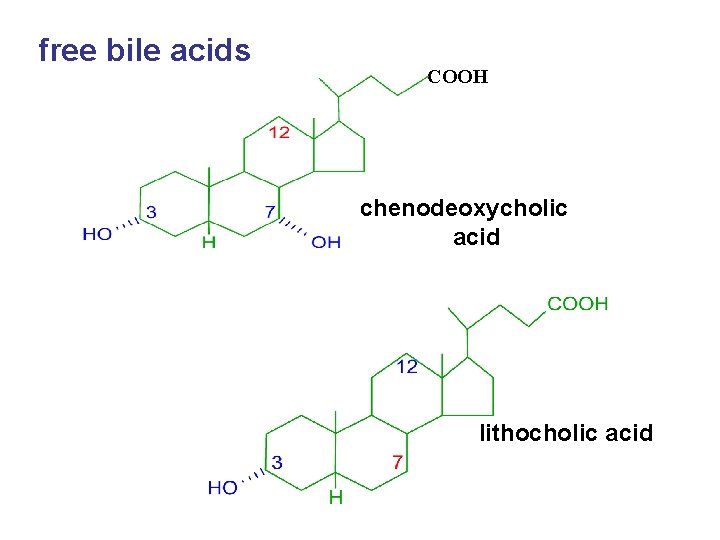
free bile acids COOH chenodeoxycholic acid lithocholic acid
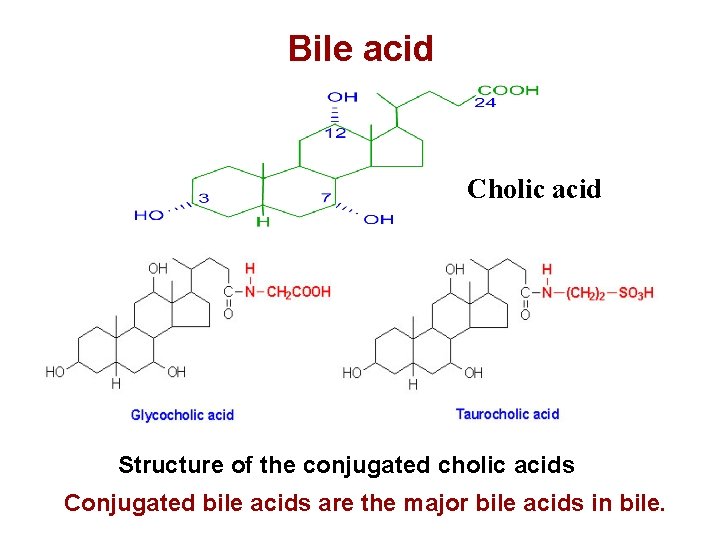
Bile acid Cholic acid Structure of the conjugated cholic acids Conjugated bile acids are the major bile acids in bile.

Bile acid According to its origin • primary bile acids: synthesized in hepatic cells, including cholic acid, chenodeoxycholic acid and their conjugated form. • secondary bile acids : produced in small intestine from primary bile, including deoxycholic acid, lithocholic acid and their conjugated form.
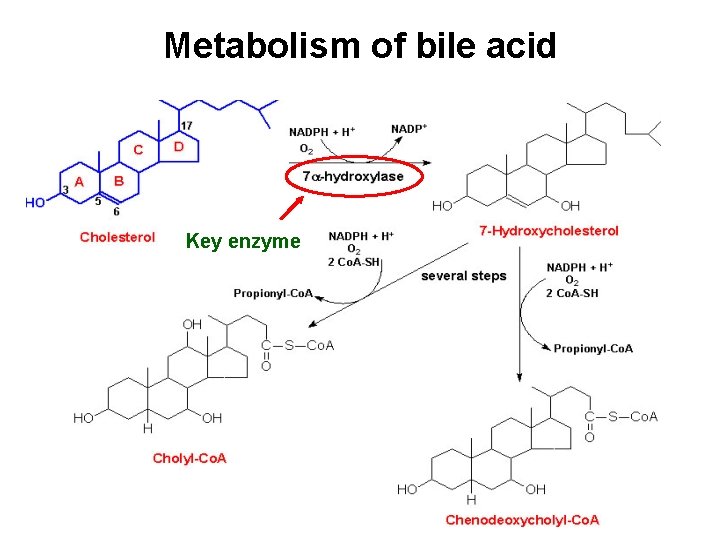
Metabolism of bile acid Key enzyme

Metabolism of bile acid The further transformation of cholyl-Co. A and chenodeoxycholyl-Co. A is to form cholic acid, chenodeoxycholic acid • Primary bile acids are mainly conjugated form. • primary bile acids pass into small intestine, part of them turn into secondary bile acids by 7αdehydroxylation. • Bile salts: bile acids always exist in a salt form.
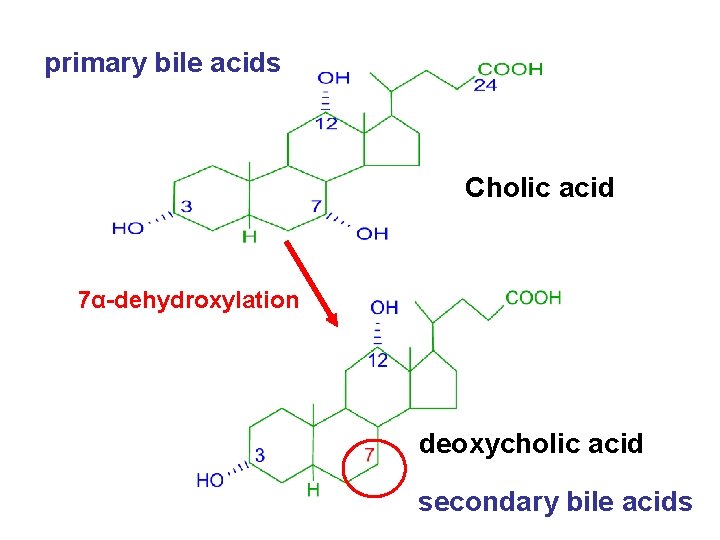
primary bile acids Cholic acid 7α-dehydroxylation deoxycholic acid secondary bile acids
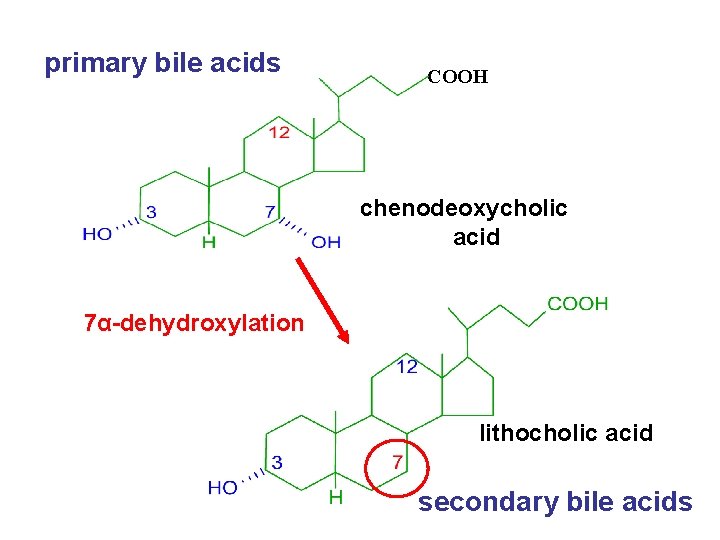
primary bile acids COOH chenodeoxycholic acid 7α-dehydroxylation lithocholic acid secondary bile acids
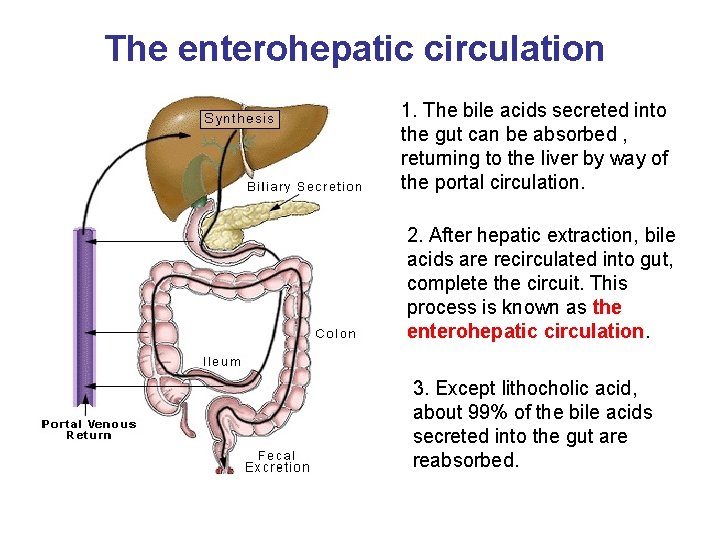
The enterohepatic circulation 1. The bile acids secreted into the gut can be absorbed , returning to the liver by way of the portal circulation. 2. After hepatic extraction, bile acids are recirculated into gut, complete the circuit. This process is known as the enterohepatic circulation. 3. Except lithocholic acid, about 99% of the bile acids secreted into the gut are reabsorbed.

Significance of the enterohepatic circulation Limited bile acids can be fully utilized. The enterohepatic circulation of the bile salts is so efficient that each day the relatively small pool of bile acids (about 3~5 g) can be cycled through the intestine 6~10 times with only a small amount lost, which can meet the needs of fat digestion.

Functions of Bile acids perform four physiologically significant functions: • eliminate of excess cholesterol. • prevent the precipitation of cholesterol in the gallbladder. Gallstones ? ? • facilitate the digestion of dietary triacylglycerols by acting as emulsifying agents that render fats accessible to pancreatic lipases. • facilitate the intestinal absorption of fat-soluble vitamins.
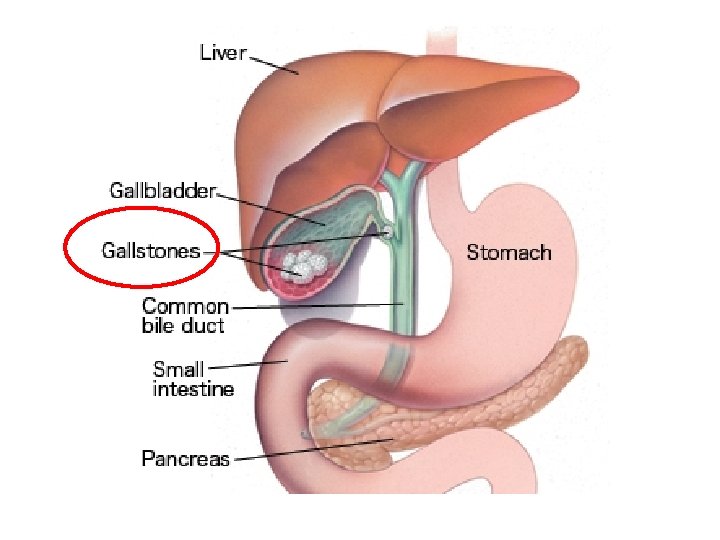

Gallstones

Functions of Bile The formation of gallstones • The solubility of cholesterol in bile depends on the relative proportion of bile salt, lecithin and cholesterol. • When bile is supersaturated with cholesterol, the excess cholesterol is precipitated to form crystals. • The crystals may grow to form stones.

Section 4 Bile pigment metabolism and jaundice

What is Bile pigment • It is the main catabolic product of iron porphyrin compounds in the body. • Including bilirubin, biliverdin, bilinogen and bilin. All except bilinogen present certain color, so collectively call them bile pigment. • Bilirubin is the major pigment in bile which is yellow, and its metabolism is the center of metabolism of bile pigment. • Liver has a central role in metabolism of the bile pigment.

Formation of bilirubin The source of bilirubin • The compounds involving iron porphyrin in the body are hemoglobin, myoglobin, cytochrome, catalase, and peroxidase, etc. • Hemoglobin is the main source of bile pigment.
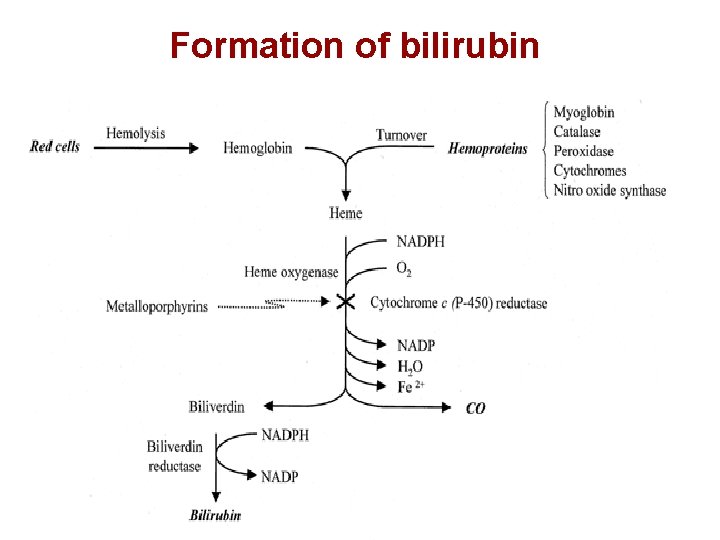
Formation of bilirubin

Metabolism of Bilirubin • Transportation of bilirubin in blood • Bilirubin metabolism in liver • Bilirubin metabolism in intestine

Transportation of bilirubin in blood Unconjugated bilirubin(UCB) liberated into the plasma is bound to albumin then presented to the liver.

Transportation of bilirubin in blood • Unconjugated bilirubin in plasma is protein-bound, specifically to albumin. • Bilirubin bound to albumin is loose with low-affinity, which is easy to detached and diffused into tissues. • Some compounds such as antibodies and drugs can compete with for the high-affinity to albumin. • Binding to albumin can protect many organs from the potentially toxic effects of bilirubin. Especially, it can limit bilirubin cross the blood-brain barrier, reducing brain damage.
After presented to liver, there are three processes: • Uptake of bilirubin by liver cells. • Conjugation of bilirubin in the endoplasmic reticulum of liver cells. • Secretion of conjugated bilirubin into the bile.

Bilirubin metabolism in liver Uptake • the bilirubin is uptaked by hepatocyte, and separated from albumin, then transported to microsome of smooth surface endoplasmic reticulum

Bilirubin metabolism in liver Conjugation • Bilirubin bind to glucuronic acid donated by UDPGA, generating conjugated bilirubin(CB); • Conjugated bilirubin: bilirubin monoglucuronide and bilirubin diglucuronide, which can increase the water solubility; • Most conjugated bilirubin is bilirubin diglucuronide.

Bilirubin metabolism in liver Secretion • conjugated bilirubin is secreted into bile capillaries.

Bilirubin metabolism in intestine • Conjugated bilirubin reaches the terminal ileum and the large intestine, the glucuronides are removed by specific bacterial enzyme • Unconjugated bilirubin is reduced to a group of colorless tetrapyrrolic compounds called urobilinogens. • Large part: urobilinogen is oxidized to urobilin, which contribute to the yellow color of urine. • small part: entero-hepatic cycle of urobilinogen.

Bilirubin metabolism in intestine entero-hepatic cycle of urobilinogen • A small fraction of urobilinogen is reabsorbed into the liver. • Then most is excreted in the bile, some reached the systemic circulation and is excreted in the urine.
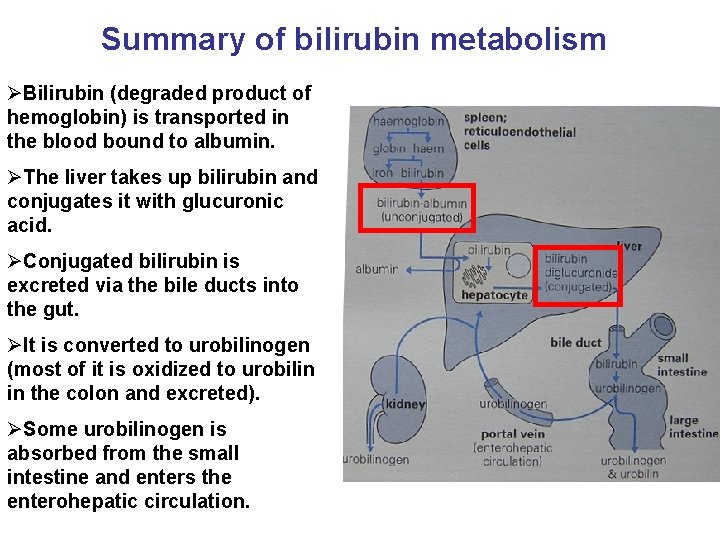
Summary of bilirubin metabolism ØBilirubin (degraded product of hemoglobin) is transported in the blood bound to albumin. ØThe liver takes up bilirubin and conjugates it with glucuronic acid. ØConjugated bilirubin is excreted via the bile ducts into the gut. ØIt is converted to urobilinogen (most of it is oxidized to urobilin in the colon and excreted). ØSome urobilinogen is absorbed from the small intestine and enters the enterohepatic circulation.

Serum Bilirubin and Jaundice

Direct bilirubin and indirect bilirubin • Direct bilirubin: in liver, bilirubin conjugated glucuronic acid. It is water-soluble, which can react directly with diazo reagent to form a purple Bound to compound. conjugated bilirubin albumin • Indirect bilirubin: free or unconjugated bilirubin, it is lipid-soluble, which can not react with the diazo reagents until alcohol or methanol is added • Measuring serum bilirubin can be used for identifying the classes of jaundice.

Serum bilirubin and jaundice • Normal total serum bilirubin ranges from 3. 4~ 17. 1 mol/L. Among which, 80% is unconjugated bilirubin, 20% is conjugated bilirubin. • Hyperbilirubinemia: when serum bilirubin exceeds 17. 1 mol/L, • When serum bilirubin is greater than 34. 2 mol/L, jaundice is clinically apparent. • The serum bilirubin between 17. 1~ 34. 2 mol/L is called latent jaundice, without yellow physical sign.

Serum bilirubin and jaundice • Jaundice: the yellow color of skin, sclera, mucous membranes, body fluid, and the other tissue in associated with an elevation in serum bilirubin.

Serum bilirubin and jaundice • The reasons of hyperbilirubinemia (1)production of more bilirubin, which exceeds the ability of uptake and excretion of normal liver; (2)the production of bilirubin is normal, but function of liver is damaged; (3)the function of liver is normal, but the excretory ducts of liver are obstructed, which prevents the excretion of bilirubin.
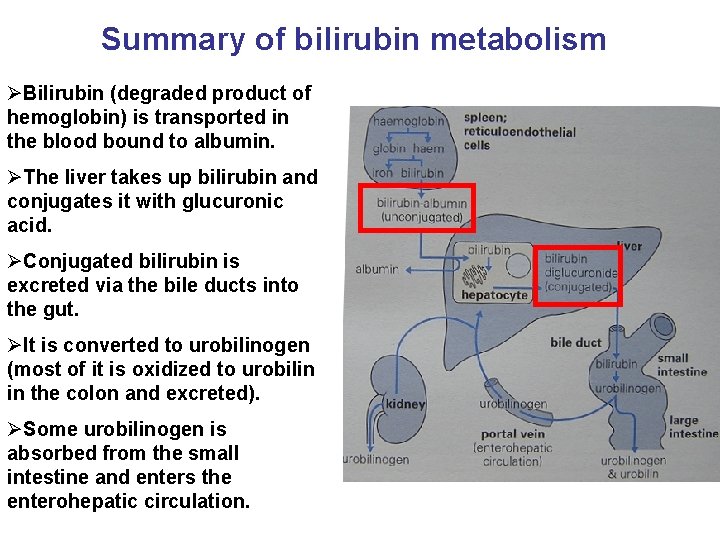
Summary of bilirubin metabolism ØBilirubin (degraded product of hemoglobin) is transported in the blood bound to albumin. ØThe liver takes up bilirubin and conjugates it with glucuronic acid. ØConjugated bilirubin is excreted via the bile ducts into the gut. ØIt is converted to urobilinogen (most of it is oxidized to urobilin in the colon and excreted). ØSome urobilinogen is absorbed from the small intestine and enters the enterohepatic circulation.

Classification of jaundice • Hemolytic(prehepatic) jaundice: due to the excess production of bilirubin by increased degradation of erythrocytes. (total and indirect bilirubin ) • Hepatic (medical) jaundice: due to dysfunction of liver (hepatitis, liver toxic damage, cirrhosis, hepatic failure). (total , indirect and direct bilirubin , urine bilirubin ) • Extrahepatic (surgical) jaundice: namely obstructive jaundice, due to blockage of bile drainage (due to gallstones, inflammation of biliary tract). (total and direct bilirubin , urine bilirubin , Kaolin-like feces)

Problems for Chapter 20 Liver biochemistry I. Term definition 1. biotransformation 2. bile pigment II. Answer the following questions • What is the purpose of biotransformation? The reaction types of it? • How many bile acids are there according to their structure or origin? • According to the mechanism, how many jaundice is there? How does blood bilirubin change in them?

• Which the following statements about biotransformation is not right? A. It is a series of enzyme-catalyzed process. B. The purpose is to add polar group on nonnutritive compounds and make it more water-soluble and easily to be excreted. C. All the transformation reactions are deintoxication. D. Transformation reactions are continuous. E. Many factors can effect transformation.

There are two phases reactions in transformation, they are and , the former includes , , and reactions, the later includes reaction. During transformation phase II reactions, Conjugation with is the most common conjugation reaction, which is donated by Bile is produced in bile is to. , stored in . . The role of

Free bile acids include , , and. The conjugated forms are free bile acids conjugating with or. According to the origin, bile acids can be divided Into and bile acids. the former includes , and their conjugated forms; the later includes , and conjugated forms. The Significance of the enterohepatic circulation is.

Bile pigment includes , , and. They are the main catabolic product of compounds in the body. is the main source of bile pigment production. Conjugated bilirubin is bilirubin binding to by UDPGA donated

• Which the following statements about metabolism of bilirubin is not right? A. Unconjugated bilirubin liberated into the plasma is bound to albumin. B. Conjugated bilirubin can cross the blood-brain barrier, resulting in brain damage. C. Bilirubin is uptaked by hepatocyte, and separated from albumin. D. In liver, bilirubin forms conjugated then secreted into bile capillaries E. There is entero-hepatic cycle of urobilinogen during metabolism of bilirubin.

When serum bilirubin exceeds hyperbilirubinemia mol/L is called According to the reasons of hyperbilirubinemia, there are 3 types jaundice, they are , , and.

• Which the following statements about jaundice are right? A. Direct bilirubin means bilirubin can react directly with diazo reagent, which is the conjugated bilirubin. B. In prehepatic jaundice, total and indirect blood bilirubin are increased. C. In hepatic jaundice, besides total blood bilirubin, both indirect and direct blood bilirubin are increased. D. Blockage of bile drainage can lead to extrahepatic jaundice. The patient may appear Kaolin-like feces. E. Elevated urine bilirubin can be detected in three types of jaundice.
- Slides: 73