Chapter 2 Patient Safety Culture SAFEQI Chapter 2













- Slides: 21

Chapter 2 Patient Safety Culture @SAFE_QI

Chapter 2: Theories of Patient Safety To create sustainable improvements in safety, it is necessary to create a culture of safety. This chapter introduced the key theories and approaches to developing a safety-based culture locally. @SAFE_QI

Why is safety ‘culture’? “The safety culture of an organisation is the product of individual and group values, attitudes, perceptions, competencies and patterns of behaviour that determine the commitment to, and the style and proficiency of, an organisation’s health and safety management. ” @SAFE_QI

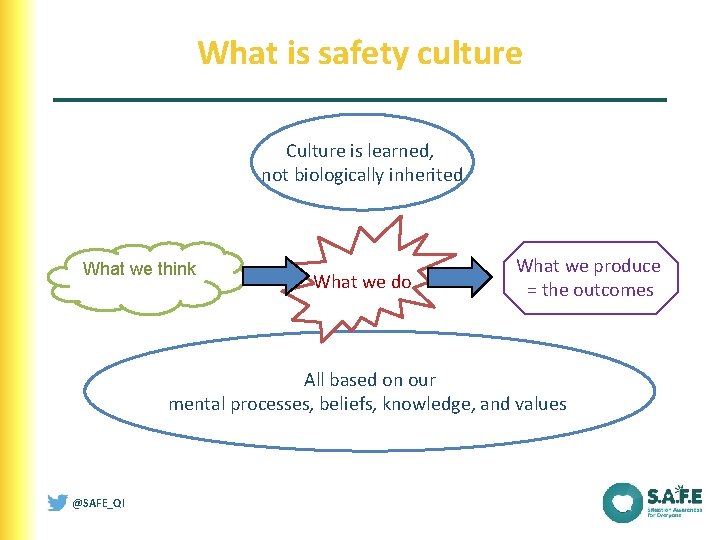
What is safety culture Culture is learned, not biologically inherited What we think What we do What we produce = the outcomes All based on our mental processes, beliefs, knowledge, and values @SAFE_QI Adapted from Reason

WHAT WE PERMIT WE PROMOTE @SAFE_QI

Key characteristics of safety culture… Mutual trust Safety culture Shared perceptions on the importance of safety Confidence in the efficacy of preventive measures @SAFE_QI

Resources • • Manchester Patient Safety Scales (Ma. PSaf) Sexton Safety Attitudes Survey Experience of Care Survey SHINE Tool @SAFE_QI

The Model for Safety Culture • No time for safety or investment into improvement Pathological Reactive • Safety occurs in response to an incident Bureaucratic Proactive Generative @SAFE_QI • Safety is driven by management systems and imposed on the workforce • There is value placed in safety with continually improving systems • The ideal, where safety is an integral part of everyday life in all staff Hudson P. Applying the lessons of high risk industries to health care Qual Saf Health Care 2003

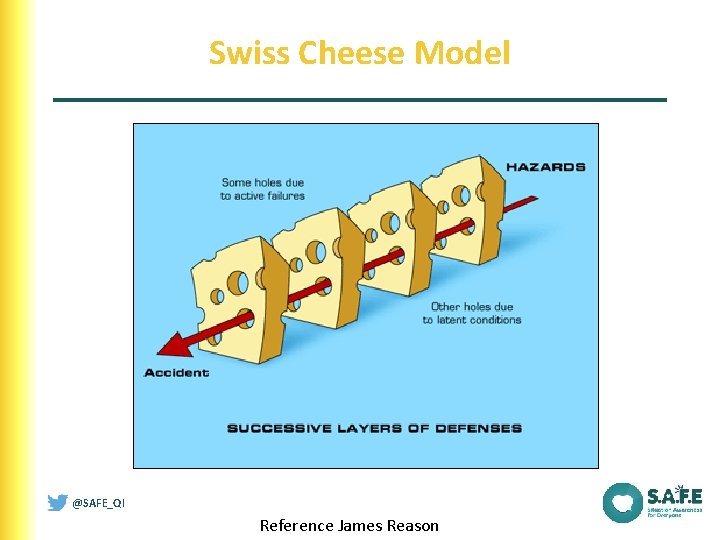
Swiss Cheese Model @SAFE_QI Reference James Reason

Where is healthcare? We embrace procedures Self-reflection is encouraged Safety tends to come from management @SAFE_QI

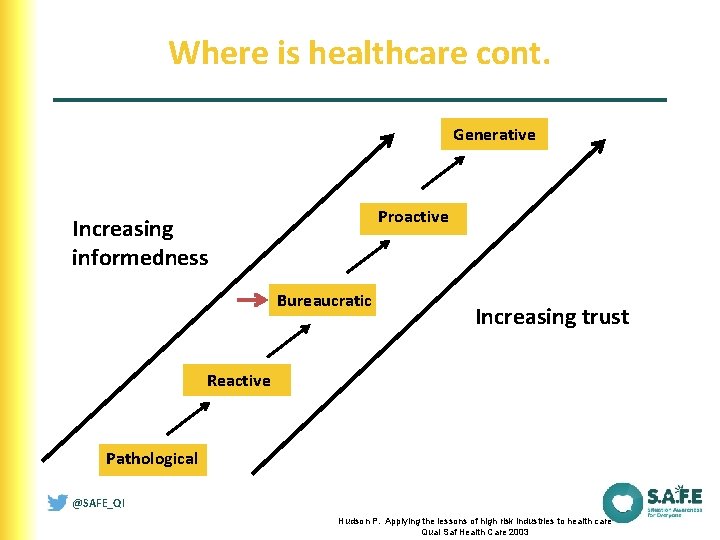
Where is healthcare cont. Generative Proactive Increasing informedness Bureaucratic Increasing trust Reactive Pathological @SAFE_QI Hudson P. Applying the lessons of high risk industries to health care Qual Saf Health Care 2003

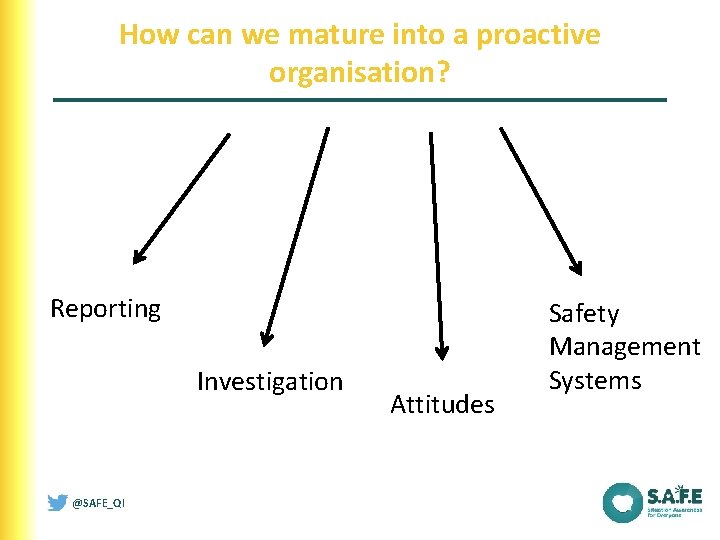
How can we mature into a proactive organisation? Reporting Investigation @SAFE_QI Attitudes Safety Management Systems

How can we map progress? Manchester Patient Safety Framework (Ma. PSa. F) • Facilitate reflection on patient safety culture • Stimulate discussion about the strengths and weaknesses of the patient safety culture • Reveal any differences in perceptions between staff groups • Help understand how a more mature safety culture might look • Help evaluate any specific intervention needed to change the patient safety culture @SAFE_QI www. nrls. npsa. nhs. uk › Home › Patient safety resources

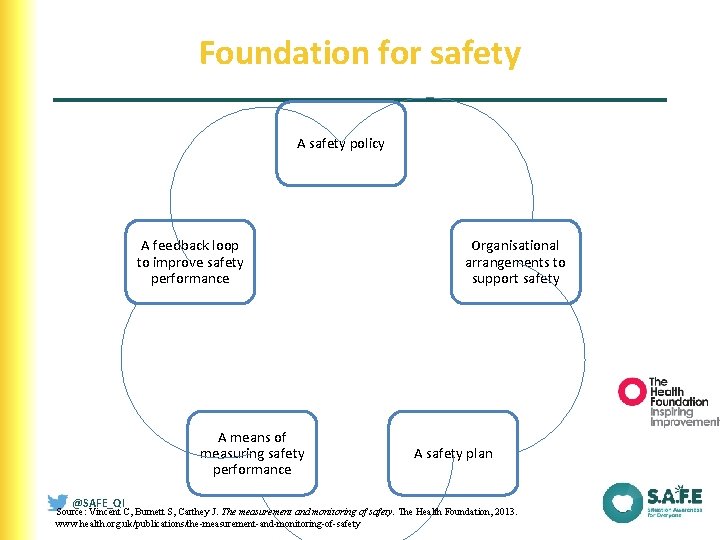
Foundation for safety A safety policy A feedback loop to improve safety performance A means of measuring safety performance @SAFE_QI Organisational arrangements to support safety A safety plan Source: Vincent C, Burnett S, Carthey J. The measurement and monitoring of safety. The Health Foundation, 2013. www. health. org. uk/publications/the-measurement-and-monitoring-of-safety

A framework for the measurement and monitoring of safety Past Harm Integration and learning Reliability Past harm Anticipation and preparedness Sensitivity to operations @SAFE_QI Source: Vincent C, Burnett S, Carthey J. The measurement and monitoring of safety. The Health Foundation, 2013. www. health. org. uk/publications/the-measurement-and-monitoring-of-safety

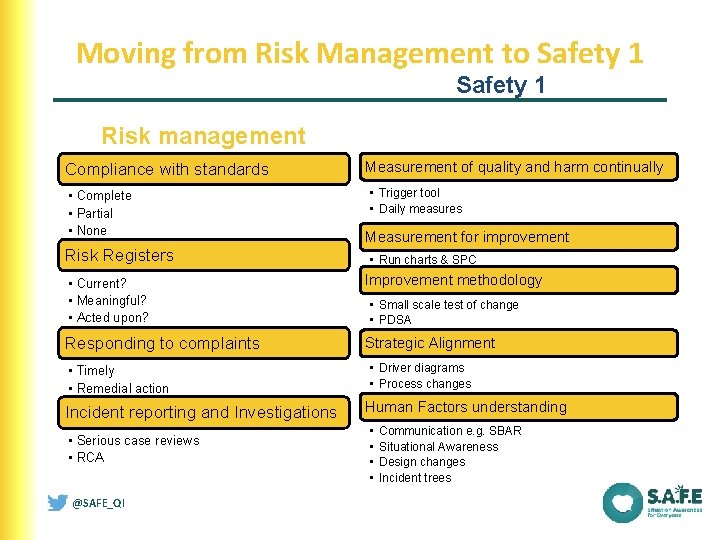
Moving from Risk Management to Safety 1 Risk management Compliance with standards • Complete • Partial • None Risk Registers Measurement of quality and harm continually • Trigger tool • Daily measures Measurement for improvement • Run charts & SPC • Current? • Meaningful? • Acted upon? Improvement methodology Responding to complaints Strategic Alignment • Timely • Remedial action Incident reporting and Investigations • Serious case reviews • RCA • Small scale test of change • PDSA • Driver diagrams • Process changes Human Factors understanding • • Communication e. g. SBAR Situational Awareness Design changes Incident trees @SAFE_QI NHS III

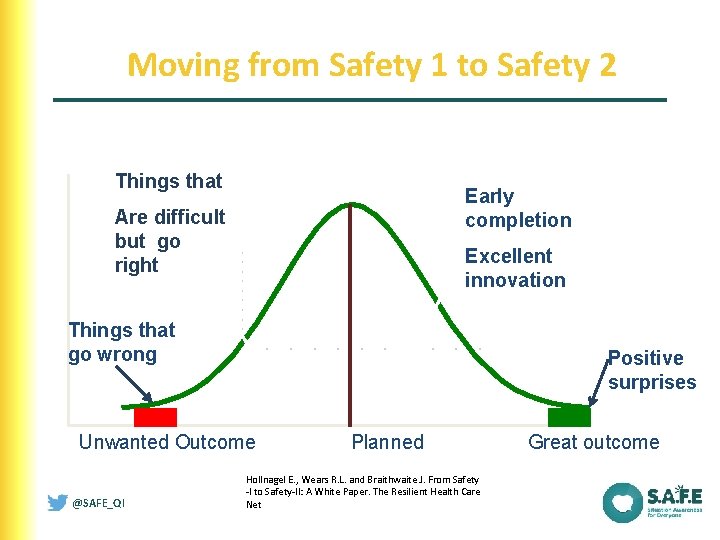
Moving from Safety 1 to Safety 2 Things that Early completion Are difficult but go right Excellent innovation Things that go wrong Positive surprises Unwanted Outcome @SAFE_QI Planned Hollnagel E. , Wears R. L. and Braithwaite J. From Safety -I to Safety-II: A White Paper. The Resilient Health Care Net Great outcome

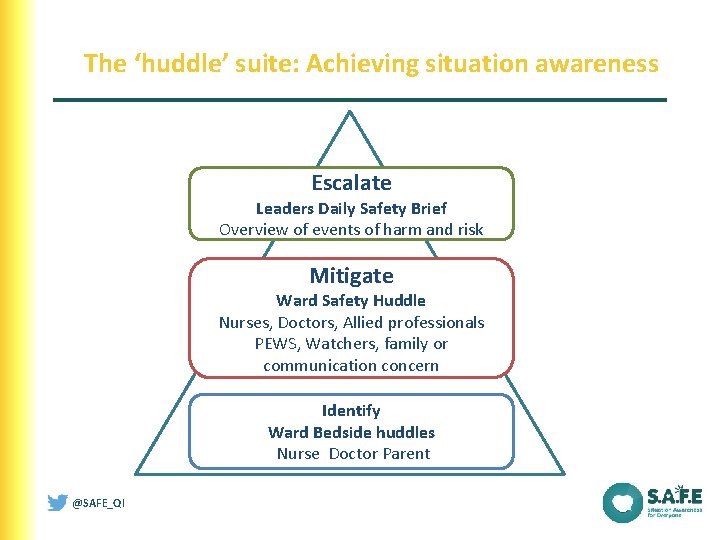
The ‘huddle’ suite: Achieving situation awareness Escalate Leaders Daily Safety Brief Overview of events of harm and risk Mitigate Ward Safety Huddle Nurses, Doctors, Allied professionals PEWS, Watchers, family or communication concern Identify Ward Bedside huddles Nurse Doctor Parent @SAFE_QI

Reliable Communication I-S-B-A-R • • • Identify Situation Background Assessment Recommendation and Read back @SAFE_QI

Ten suggestions for harm-free paediatrics Fitzsimons J and Vaughan D Patient Safety (P Lachman, Section Editor) Current Treatment Options in Pediatrics December 2015, Volume 1, Issue 4, pp 275 -285 1. No or minimal pain and distress 2. No tissue injury—extravasation, pressure ulcer or other tissue injury 3. No hospital-acquired infections 4. No medication or fluid injuries 5. Early recognition and management of procedural or surgical complications 6. Early recognition and management of sepsis or other life-threatening illnesses 7. Early recognition and management of in-hospital deterioration 8. Early recognition and management of safeguarding concerns 9. No unnecessary admissions, investigations, procedures or treatments 10. No psychological harm—provide a positive experience @SAFE_QI

Daily questions to ask at all levels • What did we do well? – So we can replicate • Past harm – Has patient care been safe in the past? • Reliability – Are our clinical systems and processes reliable • Sensitivity to operations – Is care safe today? • Anticipation and preparedness – Will care be safe in the future? • Integration and learning – Are we responding and improving? @SAFE_QI