CHAPTER 2 INFLAMMATION AND REPAIR Mr Ahmed Abdirizak


CHAPTER 2 INFLAMMATION AND REPAIR Mr Ahmed Abdirizak

INFLAMMATION Inflammation: Inflammation is the reaction of blood vessels, leading to the accumulation of fluid (Serum) and leukocytes in extra vascular tissue.

Types Of Inflammation is divided into I - Acute inflammation, which occurs over seconds, minutes, hours, and days. II - Chronic inflammation, which occurs over longer times, days & months.

GENERAL CONCEPTS OF ACUTE AND CHRONIC INFLAMMATION The body must undergo changes locally through vasodilation and increased vascular permeability in the area of the agent inciting the inflammatory reaction to allow white blood cells to accumulate. The white blood cells must then leave the blood vessel, cross the basement membrane, and be drawn to the area where they are needed. The process by which white blood cells are drawn to the area where they are needed is referred to as chemotaxis. Acute inflammation has a rapid onset, lasts for minutes to days, and is characterized by exudation of fluid and protein from vessels and emigration of neutrophils.

Acute inflammation is a protective process that is designed to rid the body of the inciting agent and set up the process of repair. Chronic inflammation has a longer time course (days to years) and involves different cell types than does acute inflammation (lymphocytes and macrophages versus neutrophils). Also, in chronic inflammation, tissue repair coexists with tissue destruction.

Sign & Symptoms Of Inflammation These are: Fever (increase temperature). Pain. Tissue damage. Swelling of tissue. Redness of tissue. Loss of movements or restricted movement, if near joints.

Causes of inflammation Bacterial Viral Protozoal Metazoal Fungal Immunological Tumours Chemicals, toxins etc Radiation 2 nd Yr Pathology 2010
Response Of Inflammation The main processes are: I - Increased blood flow. II - Increased permeability. III - Migration of neutrophils. IV - Chemotaxis. V - Leucocytes recruitment & activation.

Response Of Inflammation The main processes are: I - Increased blood flow due to dilation of blood vessels (arterioles) supplying the region. II - Increased permeability of the capillaries, allowing fluid and blood proteins to move into the interstitial spaces

Response Of Inflammation III - Migration of neutrophils (and perhaps a few macrophages) out of the venules and into interstitial spaces.

Response Of Inflammation IV - Chemotaxis Once outside the blood vessel, a neutrophil is guided towards an infection by various diffusing chemotactic factors. Examples include the chemokines and the complement peptide C 5 a, which is released when the complement system is activated either via specific immunity or innate immunity.

Response Of Inflammation V - Leucocytes recruitment & activation. This is the first step is the binding of the neutrophils to the endothelium of the blood vessels. The binding is due to molecules, called cell adhesion molecules (CAMs), found on the surfaces of neutrophils and on endothelial cells in injured tissue.

Response of Inflammation V - Leucocytes recruitment & activation (contd. ) The binding of leukocytes occur in two steps: In the first step, adhesion molecules called selectins tightly gather the neutrophil to the endothelium, so that it begins rolling along the surface.

Response of Inflammation V - Leucocytes recruitment & activation (contd). In a second step, a much tighter binding occurs through the interaction of ICAMs on the endothelial cells with integrins on the neutrophil.

Response of Inflammation Eosinophils. However, in some circumstances eosinophils rather than neutrophils predominate in acute inflammation. This tends to occur with parasites (worms), against which neutrophils have little success.
Response of Acute Inflammation Increased Blood Flow, increased permeability and Edema in Inflammation: The increased blood flow & increased permeability are readily visible within a few minutes following a scratch that does not break the skin.

Response of Acute Inflammation At first, there is pale red line of scratch. Later on there is accumulation of inflammatory cells lead swelling, (inflammation). Finally, there is accumulation of interstitial fluid cause edema.

Acute Inflammation Acute inflammation, begins within seconds to minutes following the injury of tissues. The damage may be purely physical, or it may involve the activation of an immune response.
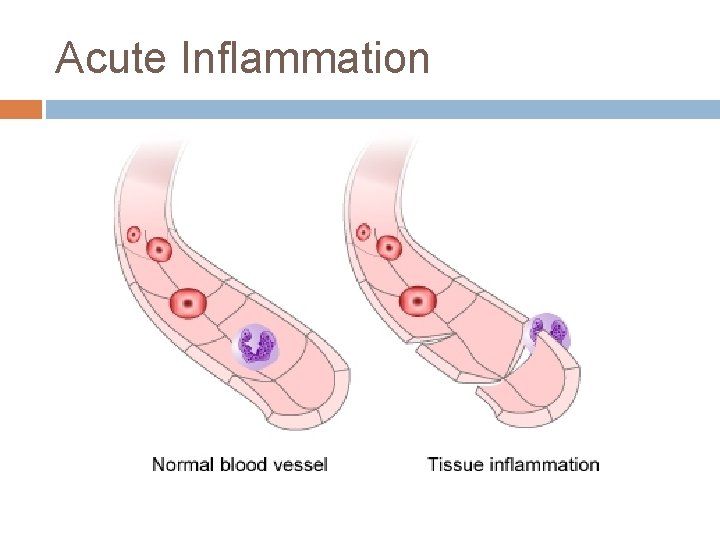
Acute Inflammation
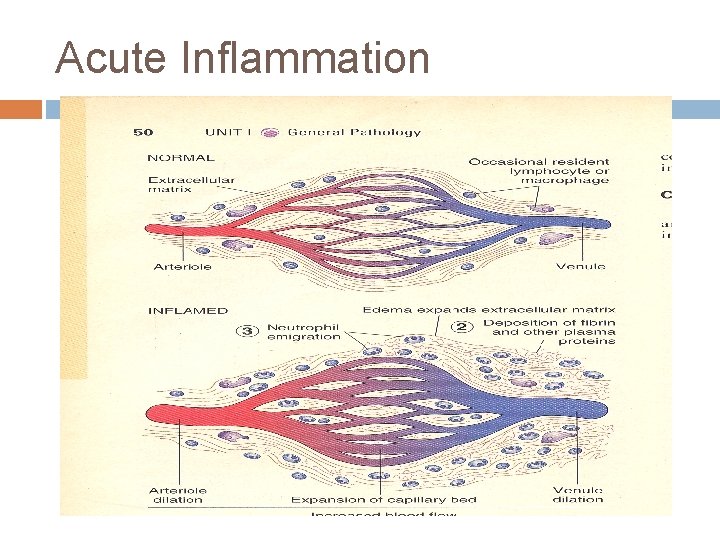
Acute Inflammation

Cardinal signs of acute inflammation: § § § Cardinal signs of acute inflammation: Rubor (red discoloration), calor (heat), dolor (pain), tumor (mass effect), and loss of function.

MORPHOLOGY OF ACUTE INFLAMMATION Types of acute inflammation include § serous § fibrinous § purulent however, mixed forms with features of one or more of these types may be seen.
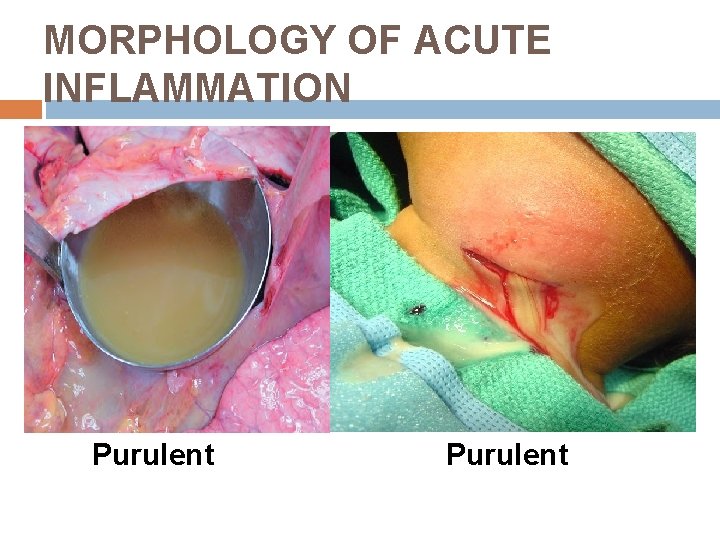
MORPHOLOGY OF ACUTE INFLAMMATION Purulent
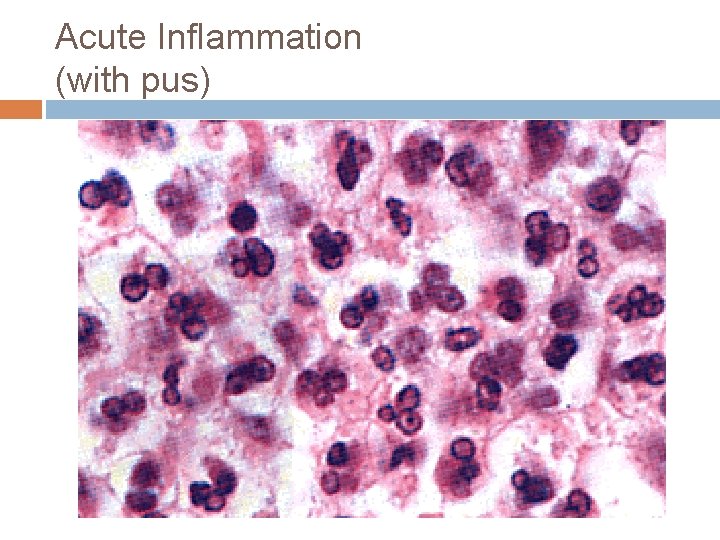
Acute Inflammation (with pus)

OUTCOMES OF ACUTE INFLAMMATION Outcomes of acute inflammation include Ø resolution Ø abscess formation, Ø ulcers, Ø fistula formation, Ø chronic inflammation, and Ø scar formation.

Chronic inflammation It is the inflammation of prolong duration (weeks or months). It is occurred as: Following acute inflammation. Occurs, incidentally as active inflammation. With tissue destruction. With repair process.
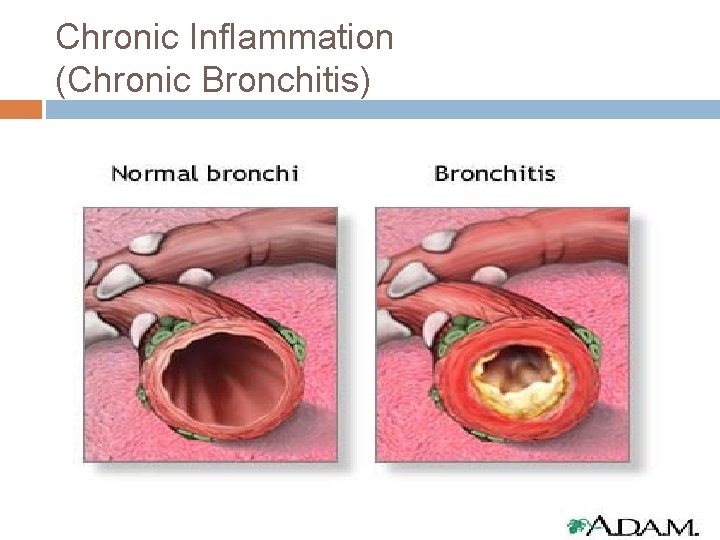
Chronic Inflammation (Chronic Bronchitis)
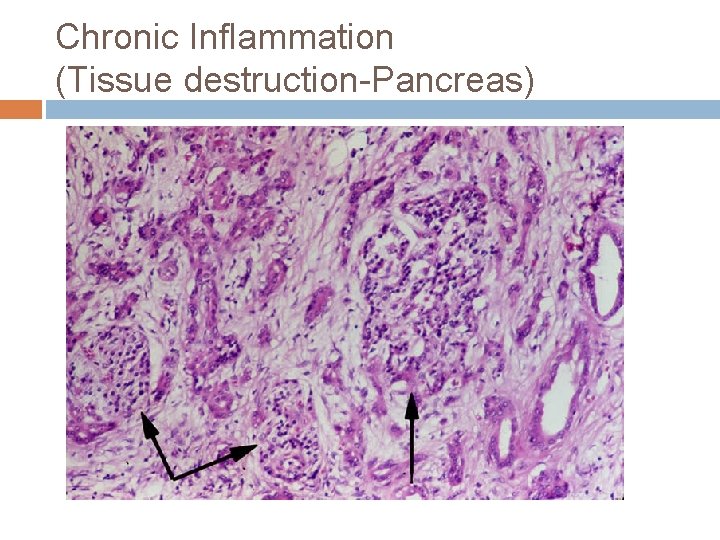
Chronic Inflammation (Tissue destruction-Pancreas)

Causes of Chronic inflammation I - Persistent infection. II - Prolonged exposure to potentially toxic agents. III - Autoimmunity.

Causes of Chronic inflammation I - Persistent infection: Bacteria. Viruses. Fungi. Parasites

Causes of Chronic inflammation III - Autoimmunity: Occurs in: Rheumatoid arthritis. Lupus erythmatosus.

important type of chronic inflammation: Granulomatous inflammation Collection of epithelioid histiocytes. Morphology of granuloma: Collection of activated macrophages (i. e. , epithelioid histiocytes); can have multinucleated giant cells (Figure 2 -6). Causes: Mycobacteria, fungi, foreign material, sarcoidosis, and silica. .

SYSTEMIC EFFECTS OF INFLAMMATIONS The systemic effects of inflammation include: a. Fever b. Endocrine & metabolic responses c. Autonomic responses d. Behavioral responses e. Leukocytosis f. Leukopenia g. Weight loss

REPAIR The process of repair begins very early. Repair involves regeneration of the parenchyma or replacement of damaged tissue with a scar if regeneration is not possible. The process of complete regeneration (i. e. , resolution of acute inflammation) requires an organ that is composed of cells that can divide and an intact basement membrane and connective tissue scaffolding.

Tissue Repair may start early after tissue damage regeneration � by parenchymal cells of the same type reparation � replacement � result - scar by connective tissue (fibrosis)

Regeneration and Reparation regeneration � restoration of normal structure and function � persistence of supportive „tissue skeleton“ necessary BM of epithelia reticulin frame in liver reparation � restoration of normal shape x function is impaired or lost � parenchyma replaced by fibrous tissue

Tissue types permanent � � stable � � � nonproliferative in postnatal life neurons (? ), cardiomyocytes (? ) regeneration as response to injury parenchyma – liver, pancreas, renal tubules mesenchymal cells, endothelium labile � � � continuous regeneration from stem cells (self-renewal) hematopoietic cells in bone marrow surface epithelia – skin, oral cavity, vagina, cervix duct epithelia – salivary glands, pancreas, biliary tract mucosas – GIT, uterus, fallopian tubes, urinary bladder
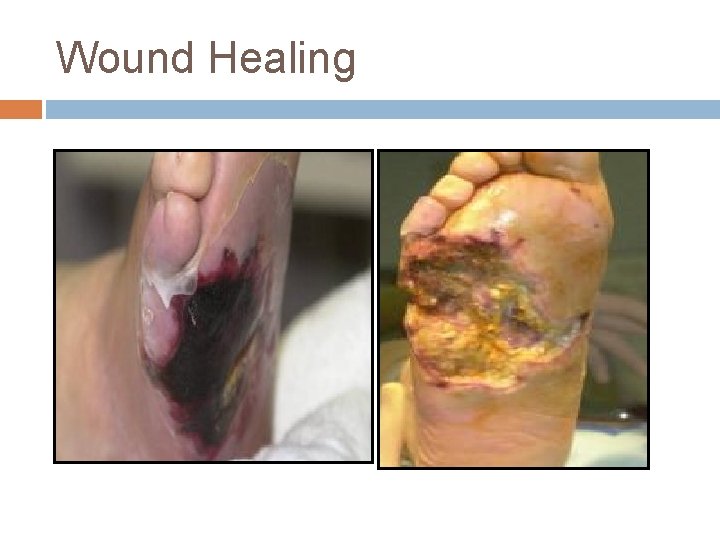
Wound Healing

Healing Definition of healing The word healing, used in a pathological context, refers to the body’s replacement of destroyed tissue by living tissue.

Healing Definitions: Healing versus regeneration Regeneration is complete replacement of damaged cells, with no scar formation. Can occur in renewing tissues (e. g. , gastrointestinal tract and skin). Can occur in stable tissues (e. g. , compensatory growth in the liver and kidney). Regeneration requires an intact connective tissue scaffold.

Components of healing Induction of inflammatory process to deal with the source of injury (cell injury is prequel to healing). The inflammatory process acts to contain damage, remove injuring substance, remove dead tissue, and start deposition of extracellular matrix. q Formation of new blood vessels. q Production of extracellular matrix, including collagen. q Tissue remodeling. q Wound contracture. q Increasing wound strength.

Factors that influence wound healing Local Factors v Type of the wound v Size of the wound v and location of the wound Systemic Factors v Circulatory status v Infection : Systemic infections delay wound healing. v Nutritional deficiencies v Hormones
Replacement by scar: The following four processes occur. 1. Formation of new blood vessels (i. e. , angiogenesis). 2. Migration and proliferation of fibroblasts. 3. Deposition of extracellular matrix. 4. Maturation and reorganization of fibrous tissue. Tissue remodeling is a balance between extracellular matrix synthesis and degradation. Extracellular matrix is degraded by matrix metalloproteinases (e. g. , collagenases, gelatinases).
- Slides: 44