Chapter 19 Infection Control 2 Learning Objectives Define

Chapter 19 Infection Control

2

Learning Objectives § Define and spell key terms § Identify the role of the medical assistant in infection control § Identify disease-producing microorganisms § List common infectious diseases § Identify the links in the chain of infection 3

Learning Objectives § Differentiate between the stages of disease § Describe the body’s defense mechanisms § Demonstrate the performance of handwashing with soap and water § Demonstrate the performance of hand sanitization with an alcohol-based hand rub § Explain standard precautions 4

Learning Objectives § List common types of personal protective equipment § Describe strategies to increase health and safety in the workplace § Differentiate medical asepsis and surgical asepsis § Differentiate sanitization, disinfection, and sterilization 5

Learning Objectives § Demonstrate equipment and instrument sanitization § Demonstrate equipment and instrument disinfection § Demonstrate wrapping a pack for sterilization 6

Learning Objectives § Demonstrate the performance of sterilization using an autoclave § Educate patients regarding methods to reduce disease transmission 7

Microorganisms and Pathogens § A microorganism is a microscopic organism seen only by using a microscope § Not all microorganisms cause disease § Harmless microorganisms on our body are called “normal flora” § Microorganisms that cause disease are called “pathogens” 8

Pathogens § Require nutrients, moisture, warmth, and neutral p. H to grow and thrive § Aerobic pathogens require oxygen to survive § Anaerobic pathogens require oxygenfree environment to survive 9

Types of Pathogens § Five main types of pathogens: § Bacteria § Rickettsia § Virus § Fungus § Protozoa 10

Bacteria § One-celled organisms § Three types: cocci—round shape, bacilli — rod shape, spirilla—spiral shape § Bacterial infections include staph infections, strep throat, Lyme disease, and gonorrhea 11

Rickettsia (parasite) § Parasitic nature—organism depends on host to survive § Spread to humans via vectors: lice, ticks, fleas § Infections include Rocky Mountain spotted fever, and typhus 12

Virus § Pathogen that grows and reproduces after infecting a host cell § More than 400 types § Smallest of all pathogens § Viral infections include common cold, hepatitis, chicken pox, and HIV 13

Fungus § § Yeast, mold, and mushroom Many present in body’s normal flora Many do not cause disease Fungal infections include athlete’s foot, ringworm, and yeast infections 14

Protozoa § Live mainly in soil § Spread through fecal–oral route by ingested contaminated food or water § Some spread by mosquitoes or other insects § Protozoan infections include malaria, Giardia, and trichomoniasis 15
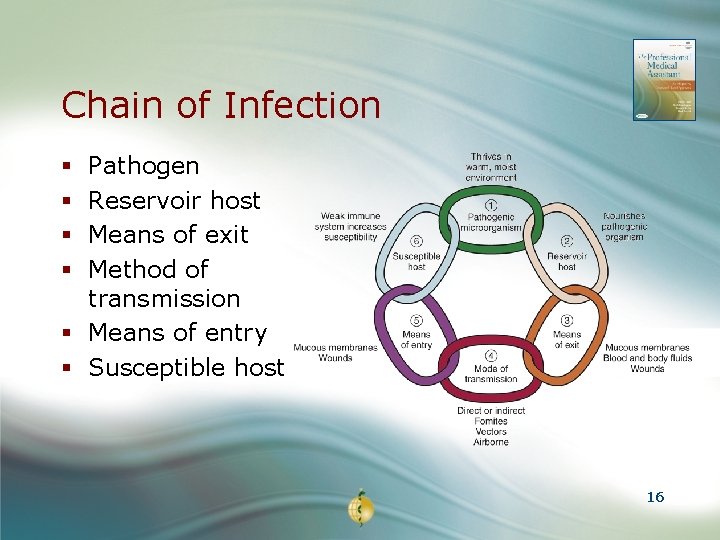
Chain of Infection Pathogen Reservoir host Means of exit Method of transmission § Means of entry § Susceptible host § § 16

Pathogen § Disease-producing § Pathogens need an microorganism; environment that bacteria, virus, fungus, enables them to protozoa, and survive, grow, and rickettsia multiply § Present in blood or § The human body is a body fluids, called perfect environment “bloodborne pathogens” 17

Reservoir Host § Human, animal, or insect that is infected with disease § Other reservoirs may be water, food, and contaminated objects § Host may be symptomatic or asymptomatic § Reservoir host is contagious even though he or she may not appear ill 18

Means of Exit § Pathogen must be able to exit reservoir host § Any body opening lined with mucous membranes: eyes, nose, throat, vagina, rectum, penis § Injury or surgery § Blood, body fluids: vaginal secretions, semen, urine, feces 19

Mode of Transmission § Direct contact— person-to-person contact or skin-toskin contact § Handshaking, kissing, and sexual contact § Indirect contact— fomites; ticks, fleas, lice, and countertops § Indirect contact includes airborne and droplet infection— sneezing, coughing, and talking 20

Means of Entry § Pathogen must find entry into new host § Any opening in the body lined with mucous membranes: nose, mouth, throat, vagina, penis, rectum § Wounds to the skin 21

Susceptible Host § Weakened immune system § Poor hygiene § Inadequate nutrition § Stress § Chronic disease § Poor environmental conditions § Elderly § Very young § Certain medications § Smoking § Alcohol abuse 22
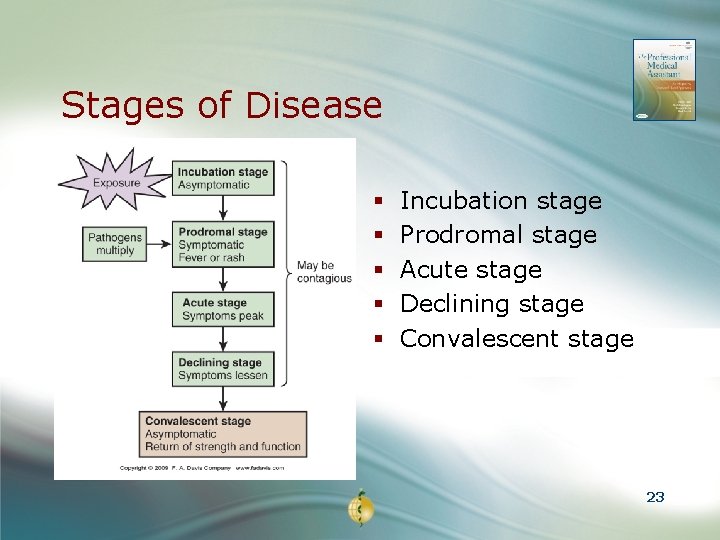
Stages of Disease § § § Incubation stage Prodromal stage Acute stage Declining stage Convalescent stage 23
Incubation Stage § Beginning stage of infection (latent) § Starts when person first contacts pathogen § Person may be asymptomatic § Person is contagious § First appearance of symptoms 24

Prodromal Stage § § Earliest symptoms Fever (febrile) or rash Person may state “I just don’t feel right” Person is contagious 25

Acute Stage § § Symptoms are at their worst Person is obviously ill Person is contagious During this time the patient should take medications, rest, and avoid contact with others 26

Declining Stage § Acute stage ends § Symptoms begin to decrease § Patient starts to feel better 27

Convalescent Stage § Symptoms are gone § Recovery time § Continues until patient regains homeostasis 28

Defense Mechanisms § The body has natural defense mechanisms to protect itself against disease: § Mechanical § Chemical § Cellular 29

Mechanical Defenses § First line of defense against pathogens is “intact” skin § Serves as barrier to environment § Cilia movement in lower airways § Coughing and sneezing § Eyelashes and eyebrows 30

Chemical Defenses § § Sebaceous glands Stomach fluids Tears and saliva contain lyzozyme Interferons have antiviral activity 31

Cellular Defenses § Various cells also act to protect the body from pathogens § Inflammatory response § Cell-mediated immunity § Antibody-mediated immunity 32

Inflammatory Response § Inflammation occurs when damage or trauma is done to tissues § Body responds by releasing chemical substances such as histamine, prostaglandins, and kinins 33
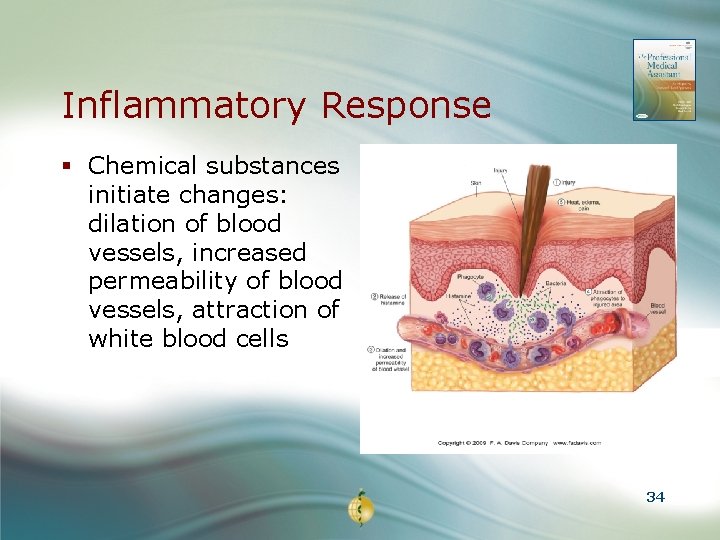
Inflammatory Response § Chemical substances initiate changes: dilation of blood vessels, increased permeability of blood vessels, attraction of white blood cells 34
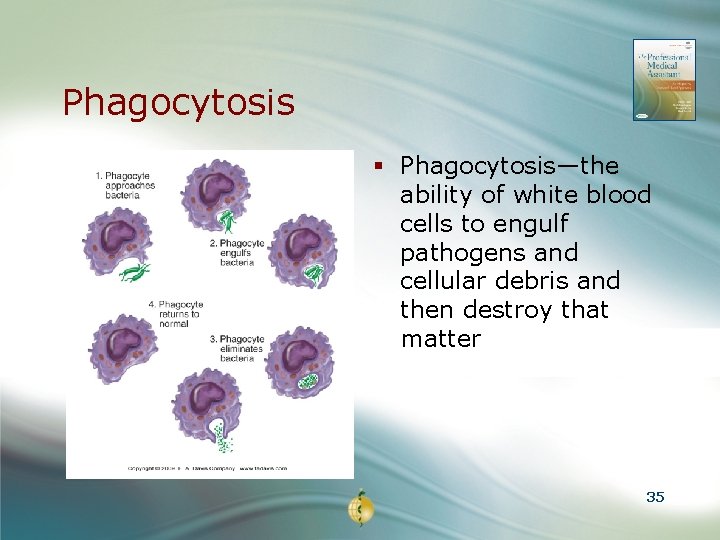
Phagocytosis § Phagocytosis—the ability of white blood cells to engulf pathogens and cellular debris and then destroy that matter 35

Immunity § Protection from infectious disease § Active or passive § Further categorized as acquired naturally or passively 36

Active Natural Immunity § Develops when body is exposed to pathogenic microorganisms § Microorganisms contain antigens (cell markers) § White blood cells develop antibodies § Antibodies protect during second exposure 37

Active Artificial Immunity § Develops when antigen is purposely introduced into body § Vaccine § Live, weakened, dead microorganism § Stimulates antibody formation without causing disease 38

Passive Natural Immunity § Develops when antibodies from mother cross placenta to fetus § Provide protection to fetus for several months § Additional antibodies are found in breastmilk 39

Passive Artificial Immunity § Develops when preformed antibodies from animal or human are then injected into an individual with known exposure § Antiserum provides temporary passive immunity § Helps in cases of exposure to rabies, botulism, venomous snake or spider bites, hepatitis, and diptheria 40

Standard Precautions § Centers for Disease Control and Prevention (CDC) § Occupational Safety and Health Administration (OSHA) § Workplace guidelines to promote safety § Bloodborne pathogens § Personal protective equipment 41

Personal Protective Equipment § Degree of risk to exposure § Gloves, masks, eye protection, shoe covers, and gowns 42

Disposal of Biohazardous Waste § Containers that hold blood or body fluids § Containers are required to have biohazardous labels 43

Sharps and Needlestick Safety § “Sharps”—needles, scalpel blades, capillary tubes, and broken glass or slides § Dispose of in puncture-resistant containers § Never recap an uncapped needle § Replace biohazard containers when full 44

Vaccinations § If no Hepatitis B vaccination prior to employment, the employer must provide it for the employee within 10 days of employment at no cost to employee § Series of three injections § Documentation § Test for TB exposure 45

Exposure Control § All employers must have exposure control plan and review with employees § Exposure incident is any contact with blood or body fluid, and any accidental injury § Report exposure to employer immediately § Follow policy and procedure for your facility 46

Biohazard Spill § Protect yourself with PPE, control spill with paper towels § Cover entire spill with 10% bleach solution and let stand for 20 minutes § Clean up spill with mechanical device, do not use hands § Repeat bleach application, wait another 20 minutes 47

Asepsis § § Condition free from pathogens Handwashing Sanitization Disinfection 48

Hand Sanitization § Single most effective way to prevent the spread of disease § Soap and warm water, rub vigorously 15 seconds § Antiseptic hand wash, cover all surfaces of hands, and air dry 49

Typical Times to Wash Hands § Beginning work § Before and after rooming patients § Before and after cleaning exam rooms § Before and after assisting the physician with procedures § Before and after cleaning equipment § Before and after using the restroom § Before and after taking a break or eating lunch § At the end of the day 50

Sanitization of Equipment § Inactivating or removing microorganisms on reusable equipment and surfaces to a safe level § Chemicals, heat, and gas are used § Low-suds detergents are commonly used § Read labels, follow manufacturer’s directions, rinse all instruments, and protect yourself 51

Disinfection § More thorough than sanitization § Kills bacteria and most microorganisms but not spores § Use different disinfectants for surfaces and equipment vs. skin surfaces § Read labels and follow manufacturer’s directions § Iodine, household bleach, and 70% alcohol 52

Sterilization § Complete destruction of all microorganisms including spores § Autoclave sterilization involves heat, pressure, steam, and time § Sanitize and disinfect instruments and equipment before sterilizing § All surfaces of instruments must be exposed 53

Sterile Packs § Sanitize and disinfect instruments prior to wrapping § Hinged instruments should be left open, surfaces of instruments should not be touching § Use indicator tape and label 54

Chemical Sterilization § Certain instruments should not be autoclaved; for example, fiberoptic endoscopes § Sterilize using chemicals § Solution is caustic; wear PPE § Immerse for a specified time 55

Medical Asepsis § Destruction of pathogenic organisms after they leave the body § Follow standard precautions § Consider specimens to be contaminated 56

Surgical Asepsis § Destroying all pathogenic organisms before they enter the body § Use surgical aseptic technique § Normal protective barriers are punctured or disrupted § Injections, urinary catheterization, wound care, and surgical procedures 57

Discussion § List five types of pathogens § Discuss difference between aerobes and anaerobes § Discuss differences in handwashing with soap and handwashing with alcoholbased hand sanitizer § Identify procedures that require medical asepsis vs. surgical asepsis 58

Credits 59
- Slides: 59