Chapter 19 Bowel Elimination and Gastric Intubation Copyright

Chapter 19 Bowel Elimination and Gastric Intubation Copyright © 2016 by Mosby, an imprint of Elsevier Inc.

Diet and Bowel Elimination Dietary fiber, which is found in fruits, vegetables, whole grains, and legumes, is an excellent food source for relieving constipation. Ø Foods containing fiber offer other health benefits, such as helping to maintain a healthy weight and lowering a person’s risk for diabetes and heart disease. Diet is just one of a myriad of factors that affect bowel elimination in patients. Ø Patients’ physical conditions, psychological factors, fluid intake, life style, as well as medications influence bowel function. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 2

Diet and Bowel Elimination (Cont. ) Disorders of the bowel requiring direct nursing intervention include diarrhea, constipation, and bowel incontinence. Left unrecognized or untreated, constipation progresses to fecal impaction, in which stool blocks the intestinal lumen. Ø Fecal impaction can potentially result in bowel obstruction. Ø When patients undergo surgery or experience an alteration in gastrointestinal peristalsis, the insertion of a nasogastric tube is needed for gastric decompression. Ø Gastric decompression reduces nausea and vomiting by keeping the stomach empty. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 3

Patient-Centered Care It is important to show respect for a patient’s privacy, provide necessary comfort and hygiene measures, and attend to each patient’s emotional needs when performing required skills. Assist immobilized patients with the elimination process by helping them on and off bedpans. Provide patient-centered care by determining a patient’s normal pattern of bowel elimination and accommodate that pattern while in a health care setting. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 4

Patient-Centered Care (Cont. ) Be aware of a patient’s cultural practices. Provide gender-congruent care for patients from cultures that emphasize separate gender roles and female modesty. Also be aware of patients’ unique hygiene needs. Ø For example, some patients who are Hindus and Muslims have distinct hygiene practices. • The left hand is designated for unclean procedures such as practices associated with bowel elimination. • Use the right hand to first touch the patient and assist with other aspects of care and use the left for handling the bedpan and perineal cleansing following bowel elimination. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 5

Safety Safe patient-handling techniques, used when positioning a patient for removal of a fecal impaction or administering an enema, are essential. Ø It is important that a patient understand the need to maintain the position and try to relax. When removing a fecal impaction, there additional safety issues. Ø If your patient has a history of cardiac dysrhythmias, there is a risk for procedural-associated bradycardia because of stimulation of the sacral branch of the vagus nerve. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 6

Evidence-Based Practice Choose the correct size of medical device(s) to fit the individual Cushion and protect the skin (when possible) with dressings in high-risk areas (e. g. , nasal bridge) Remove or move the device daily to assess skin Avoid placement of device(s) over sites of prior or existing pressure ulceration Educate staff on correct use of devices and prevention of skin breakdown Be aware of edema under device(s) and potential for skin breakdown Confirm that tubing of devices is not placed directly under an individual who is bedridden or immobile Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 7

Procedural Guideline 19 -1: Providing a Bedpan A patient restricted to bed uses a bedpan for bowel elimination. Regular bedpan vs. Fracture bedpan Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 8

Procedural Guideline 19 -1: Providing a Bedpan (Cont. ) Delegation and Collaboration The skill of providing a bedpan can be delegated to nursing assistive personnel. Ø Instruct the NAP about the following: • Correct positioning guidelines for patients with mobility Ø restrictions or for those who have therapeutic equipment such as wound drains, intravenous (IV) catheters, or traction • To provide perineal and hygiene for patient as necessary after using the bedpan Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 9

Quick Quiz! The nurse is assisting a patient in using a regular bedpan. How will the nurse position the bedpan? A. Wide end under the patient’s buttocks B. Tapered end at the small of the patient’s back C. Wide end in line with patient’s thighs D. Tapered end low on the thighs, near the knees Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 10

Skill 19 -1: Removing Fecal Impaction Fecal impaction: the inability to pass a hard collection of stool commonly found in the lower colon and rectum. Fecal impaction occurs when there is a history of constipation (infrequent stools). Ø A consensus definition of functional constipation includes two or more of the following factors for at least 3 months: 1) 2) 3) 4) straining with defecation at least ¼ of the time lumpy or hard stools (or both) at least ¼ of the time sensation of incomplete evacuation at least ¼ of the time two or fewer bowel movements in a week Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 11

Skill 19 -1: Removing Fecal Impaction (Cont. ) Symptoms: constipation rectal discomfort anorexia, nausea, vomiting, abdominal pain, diarrhea (leaking around the impacted stool) Ø urinary frequency Ø Ø Ø Prevention is the key to managing fecal impaction. However, once it occurs, digital removal of the stool is a treatment option. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 12

Skill 19 -1: Removing Fecal Impaction (Cont. ) Prior to performing the invasive intervention, a nurse needs to do the following: Ø Ø Ø assess each patient’s risk factors determine religious and cultural beliefs obtain informed consent (follow hospital policy). Digital removal of an impaction is embarrassing and uncomfortable for patients. Ø Excessive rectal manipulation may cause irritation to the mucosa and subsequent bleeding or vagus nerve stimulation, which can produce a reflex slowing of heart rate. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 13

Skill 19 -1: Removing Fecal Impaction (Cont. ) Assessment Identify the patient using two identifiers (i. e. , name and birthday or name and account number, according to facility policy). Ø Ask patient about normal and current bowel elimination pattern, including frequency and characteristics of stool; use of laxatives, enemas, and other medications; level of regular exercise; urge to defecate but inability to do so; presence of hemorrhoids; abdominal discomfort, especially when attempting to defecate; feelings of incomplete emptying; and sensations of bloating, cramping, or excessive gas. Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 14

Skill 19 -1: Removing Fecal Impaction (Cont. ) Assessment (Cont. ) Inspect patient’s abdomen for distention. Auscultate all four quadrants for presence of bowel sounds. Ø Palpate patient’s abdomen for distention, discomfort, or masses. Ø Observe the anal area for signs of irritation from passing stool or hemorrhoids. Ø Measure patient’s current heart rate and comfort level on a scale of 0 to 10. Ø Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 15

Skill 19 -1: Removing Fecal Impaction (Cont. ) Assessment (Cont. ) Perform hand hygiene and apply clean gloves. Observe consistency of stool, seepage of liquid stool, or continual passage of small amounts of hard stool. Remove gloves and perform hand hygiene. Ø Determine if patient is receiving anticoagulant therapy. Ø Check patient’s record for health care provider’s order for digital removal of impaction. Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 16

Skill 19 -1: Removing Fecal Impaction (Cont. ) Planning/Expected Outcomes Delegation and Collaboration The skill of removing an impaction cannot be delegated to nursing assistive personnel. Ø Instruct the NAP about the following: • Assisting the RN in positioning patient for the procedure • What to observe for (e. g. , color and consistency of any Ø evacuated stool, rectal bleeding, or bloody mucus) and report back to nurse • Providing frequent perineal care to patient Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 17

Skill 19 -1: Removing Fecal Impaction (Cont. ) Evaluation Unexpected Outcomes Patient experiences bradycardia, decrease in blood pressure, and decrease in level of consciousness as a result of vagus nerve stimulation. Ø Patient has seepage of liquid fecal material after removal of impaction. Ø Patient has trauma to the rectal mucosa as evidenced by blood on the gloved finger. Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 18

Recording and Reporting • Record patient’s tolerance to procedure, amount and consistency of stool removed, vital signs, pain level on a scale of 0 to 10, and adverse effects. • Report any changes in vital signs or adverse effects to nurse in charge or health care provider. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 19

Special Considerations Geriatric Many adults are especially prone to dysrhythmias and other problems related to vagal stimulation; monitor heart rate and rhythm closely. Ø In North America, 27% of the general population reportedly are constipated as a result of insufficient dietary bulk, inadequate fluid intake, laxative abuse, diminished muscle tone and motor function, decreased defecation reflex, mental or physical illness, and medications. Ø Institute a diet adequate in dietary fiber. Ø Consider development of regular toileting routine that includes responding to the urge to defecate. Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 20

Special Considerations (Cont. ) Pediatric Ø Digital removal of stool is not recommended in pediatrics because of risk for anal fissures and pain that trigger stool withholding Home Care Patients who have had a fecal impaction will need a bowel-retraining program. Ø Consider having patient or family caregiver keep a week’s diary of meals and fluid intake. Determine if dietary pattern contributes to constipation. Ø Have patient or family caregiver maintain a weekly bowel diary. Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 21

Quick Quiz! Which of the following factors is an indication of functional constipation? A. B. C. D. Loose, watery stools Four bowel movements per week Feeling of complete evacuation Straining with defecation Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 22

Skill 19 -2: Administering An Enema Enema: the instillation of a solution into the rectum and sigmoid colon to promote defecation by stimulating peristalsis. Enemas treat constipation or empty the bowel before diagnostic procedures or abdominal surgeries. Preoperative enemas are common for some gastrointestinal surgeries. Teach your patients not to rely on enemas to maintain bowel regularity because they do not treat the cause of irregularity or constipation. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 23
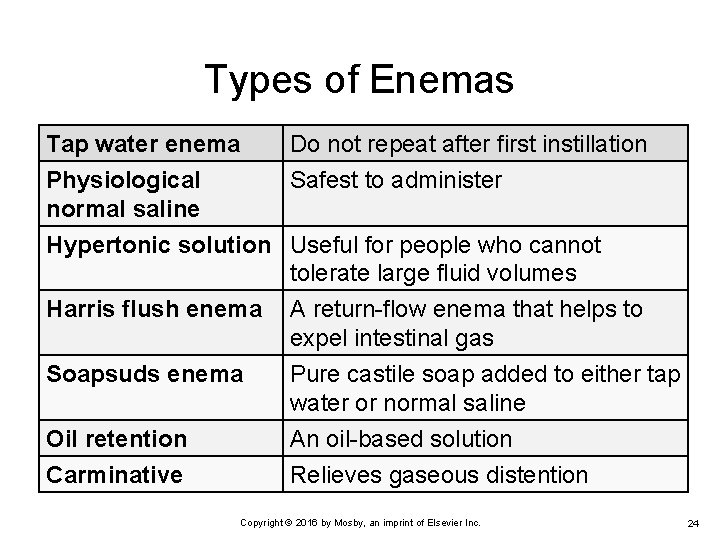
Types of Enemas Tap water enema Physiological normal saline Do not repeat after first instillation Safest to administer Hypertonic solution Useful for people who cannot tolerate large fluid volumes Harris flush enema Soapsuds enema Oil retention Carminative A return-flow enema that helps to expel intestinal gas Pure castile soap added to either tap water or normal saline An oil-based solution Relieves gaseous distention Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 24

Skill 19 -2: Administering An Enema (Cont. ) Assessment Identify the patient using two identifiers (i. e. , name and birthday or name and account number, according to facility policy). Ø Review health care provider’s order for enema and clarify reason for enema administration. Ø Determine patient’s level of understanding of purpose of enema. Ø Inspect abdomen for distention and auscultate for bowel sounds. Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 25

Skill 19 -2: Administering An Enema (Cont. ) Assessment (Cont. ) Assess medical history for presence of undiagnosed gastrointestinal disease, cardiac disease, dehydration, or recent abdominal, rectal, or prostate surgery. Ø Assess patient for allergy to any active ingredients of a Fleet’s enema. Ø Assess last bowel movement, normal versus most recent bowel elimination pattern, presence of hemorrhoids, mobility, and presence of abdominal pain or cramping. Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 26

Skill 19 -2: Administering An Enema (Cont. ) Planning/Expected Outcomes Delegation and Collaboration The skill of enema administration can be delegated to nursing assistive personnel. Ø Instruct the NAP about the following: • How to properly position patients with therapeutic Ø equipment such as drains, IV catheters, or traction • How to properly position patients with mobility restrictions • Informing the nurse immediately about the presence of blood in the stool or around rectal area, any change in vital signs, abdominal pain, abdominal cramping, or distention Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 27

Skill 19 -2: Administering An Enema (Cont. ) Evaluation Unexpected Outcomes Patient is unable to hold enema solution. Severe cramping, bleeding, or sudden severe abdominal pain occurs and is unrelieved by temporarily stopping or slowing flow of solution. Ø With an order for “enemas until clear, ” after three enemas the water is highly colored or contains solid fecal material. Ø Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 28

Recording and Reporting • Record the time, type, and volume of enema administered; patient’s signs and symptoms; response to enema; and results, including color, amount, and appearance of stool. Document your evaluation of patient learning. • Report failure of patient to defecate or any adverse reactions to health care provider. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 29

Special Considerations Geriatric Older adults may tire more quickly and are at greater risk for fluid and electrolyte imbalances; use caution when administering enemas “until clear. ” Ø Teach older adults and their family caregivers dietary and activity measures to avoid constipation. Ø Older adults may have difficulty in retaining enema solution. Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 30

Special Considerations (Cont. ) Pediatric Ø The use of oral stool softeners is the initial recommended treatment of constipation in children. Home Care Assess patient’s and family caregiver’s ability and motivation to administer enema in the home and provide instruction as needed. Ø Assess patient’s ability to manipulate equipment to self-administer enema. Ø Instruct patient and family caregiver not to exceed number and volume of enemas. Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 31

Quick Quiz! What action can the nurse take to make a metal bedpan more comfortable for the patient? A. Store the pan in a cool area for 30 minutes B. Rub petroleum jelly on the top of the pan C. Place the pan under warm, running water for few seconds D. Wrap gauze dressings around the base of the pan Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 32

Procedural Guideline 19 -2: Applying a Fecal Continence Device A fecal-containment device is a useful intervention for patients with severe fecal incontinence, such as those with Clostridium difficile associated diarrhea. Fecal-containment devices are an effective way to prevent skin damage due to moisture and enzyme action on perianal tissues. A risk associated with use of an indwelling device is a mucosal pressure ulcer, in this case inside the rectal wall. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 33

Procedural Guideline 19 -2: Applying a Fecal Continence Device (Cont. ) Delegation and Collaboration The skill of applying a topical (external) fecalcontainment device cannot be delegated to nursing assistive personnel. The NAP can assist the nurse by helping with positioning of a patient during device application. Ø The nurse directs the NAP about: • Reporting to the nurse any instances of leakage or Ø change in appearance of skin around device noted during routine care. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 34

Skill 19 -3: Insertion, Maintenance, and Removal of a Nasogastric Tube for Gastric Decompression At times normal peristalsis is altered temporarily, either following major surgery or from conditions affecting the GI tract. When peristalsis is slowed or absent, a patient cannot eat or drink fluids without causing abdominal distention. The temporary insertion of a nasogastric (NG) tube into the stomach serves to decompress the stomach, keeping it empty until normal peristalsis returns. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 35

Skill 19 -3: Insertion, Maintenance, and Removal of a Nasogastric Tube for Gastric Decompression (Cont. ) An NG tube is a hollow, pliable tube inserted through a patient’s nasopharynx into the stomach to allow for the removal of gastric secretions and the introduction of solutions into the stomach. . Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 36

Skill 19 -3: Insertion, Maintenance, and Removal of a Nasogastric Tube for Gastric Decompression (Cont. ) The Salem sump tube is preferable for stomach decompression. Never clamp off the air vent, connect to suction, or use for irrigation. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 37

Skill 19 -3: Insertion, Maintenance, and Removal of a Nasogastric Tube for Gastric Decompression (Cont. ) NG tube insertion requires clean technique. During insertion patients experience a burning sensation as the tube passes through the sensitive nasal mucosa. One of the greatest nursing care challenges is keeping the patient comfortable during the procedure and after tube placement. An NG tube often causes a medical device–related pressure ulcer. Ø Routinely assess the condition of the naris and mucosa for inflammation and excoriation when a tube is in place. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 38

Skill 19 -3: Insertion, Maintenance, and Removal of a Nasogastric Tube for Gastric Decompression (Cont. ) Assessment Identify the patient using two identifiers. Inspect condition of patient’s nasal and oral cavity. Ask if patient has had history of nasal surgery or congestion and allergies and note if deviated nasal septum is present. Ø Auscultate for bowel sounds. Palpate patient’s abdomen for distention, pain, and rigidity. Ø Assess patient’s level of consciousness and ability to follow instructions. Ø Ø Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 39

Skill 19 -3: Insertion, Maintenance, and Removal of a Nasogastric Tube for Gastric Decompression (Cont. ) Assessment (Cont. ) Determine if patient had previous NG tube and which naris was used. Ø Safe Patient Care: If patient is confused, disoriented, or unable to follow commands, obtain assistance from another staff member to insert the tube. Verify order for type of NG tube to be placed and whether tube is to be attached to suction or drainage bag. Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 40

Skill 19 -3: Insertion, Maintenance, and Removal of a Nasogastric Tube for Gastric Decompression (Cont. ) Planning/Expected Outcomes Delegation and Collaboration Ø The skill of inserting and maintaining an NG tube cannot be delegated to nursing assistive personnel. Instruct the NAP about the following: • When to measure and record the drainage from an NG tube • How often to provide oral hygiene • Selected comfort measures such as positioning or offering ice chips if allowed • How to correctly anchor a tube to the patient’s gown during routine care to prevent accidental displacement and pulling on the naris Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 41

Skill 19 -3: Insertion, Maintenance, and Removal of a Nasogastric Tube for Gastric Decompression (Cont. ) Evaluation Unexpected Outcomes Patient’s abdomen is distended and painful. Patient complains of sore throat from dry, irritated mucous membranes. Ø Patient develops irritation or pressure ulcer of skin around naris. Ø Patient develops signs and symptoms of pulmonary aspiration: fever, shortness of breath, or pulmonary congestion. Ø Tube slips or is pulled out Ø Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 42

Recording and Reporting • Record length, size, type of gastric tube inserted, and naris in which tube was introduced. Also record patient’s tolerance of procedure, confirmation of tube placement, character and p. H of gastric contents, results of x-ray film, whether the tube is clamped or connected to drainage bag or to suction, and amount of suction supplied. • Record difference between amount of normal saline instilled and amount of gastric aspirate removed on I&O sheet. Record amount and character of contents draining from NG tube every shift in nurses’ notes or flow sheet. • • Record removal of tube “intact, ” patient’s tolerance to procedure, and final amount and character of drainage. Report occurrence of abdominal distention, unexpected increase or sudden stoppage in gastric drainage, and patient complaining of gastric distress to health care provider. Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 43

Special Considerations Pediatric For children consider the use of sedation before tube insertion. Ø Consider the child’s developmental stage and prepare child and family before initiating the procedure. Never surprise the child with this procedure. Ø Geriatric Check for ill-fitting dentures and remove them for patient’s safety and comfort during the insertion. Ø Oral and nasal mucosal drying is sometimes present. Adequately lubricate the tube for insertion. Ø If patient wears a hearing aid, be sure that the aid is in place during preprocedure explanation and insertion of the tube so patient is able to hear any instructions. Ø Copyright © 2016 by Mosby, an imprint of Elsevier Inc. 44
- Slides: 44