Chapter 17 Documenting Reporting Conferring and Using Informatics






























- Slides: 31

Chapter 17 Documenting, Reporting, Conferring, and Using Informatics Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Characteristics of Effective Documentation • Consistent with professional and agency standards • Complete • Accurate • Concise • Factual • Organized and timely • Legally prudent • Confidential Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

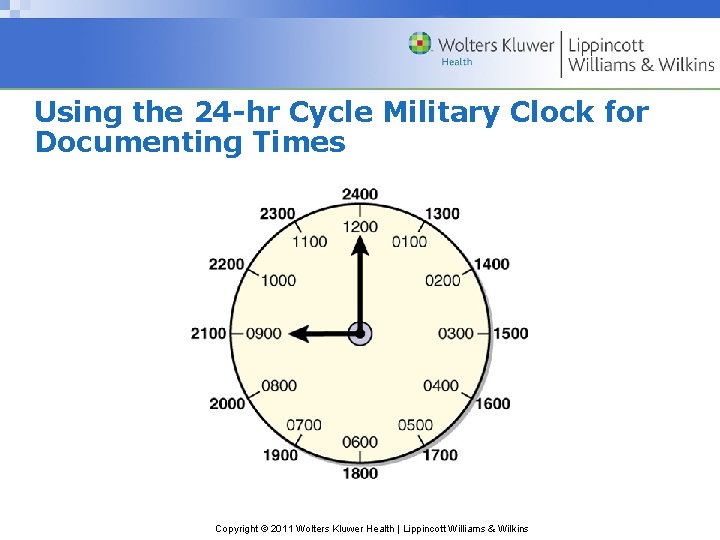
Using the 24 -hr Cycle Military Clock for Documenting Times Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

What Is Confidential? • All information about patients written on paper, spoken aloud, saved on computer – Name, address, phone, fax, social security – Reason the person is sick – Treatments patient receives – Information about past health conditions Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Potential Breaches in Patient Confidentiality • Displaying information on a public screen • Sending confidential e-mail messages via public networks • Sharing printers among units with differing functions • Discarding copies of patient information in trash cans • Holding conversations that can be overheard • Faxing confidential information to unauthorized persons • Sending confidential messages overheard on pagers Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Patient Rights • See and copy their health record • Update their health record • Get a list of disclosures • Request a restriction on certain uses or disclosures • Choose how to receive health information Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Policy for Receiving Verbal Orders in an Emergency • Record the orders in patient’s medical record. • Read back the order to verify accuracy. • Date and note the time orders were issued in emergency. • Record VO, the name of the physician followed by nurse’s name and initials. Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Policy for Physician Review of Verbal Orders • Review orders for accuracy. • Sign orders with name, title, and pager number. • Date and note time orders signed. Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Duties of RN Receiving a Telephone Order • Record the orders in patient’s medical record. • Read orders back to practitioner to verify accuracy. • Date and note the time orders were issued. • Record TO, full name and title of physician or nurse practitioner who issued orders. • Sign the orders with name and title. Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question Tell whether the following statement is true or false. One of the purposes of creating a patient record is to evaluate the quality of care patients have received and the competence of the nurses providing that care. A. True B. False Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer: A. True One of the purposes of creating a patient record is to evaluate the quality of care patients have received and the competence of the nurses providing that care. Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Purposes of Patient Records • Communication with other healthcare professionals • Record of diagnostic and therapeutic orders • Care planning • Quality of care reviewing • Research • Decision analysis • Education • Legal and historical documentation • Reimbursement Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Purposes of Recording Data • Facilitate patient care. • Serve as a financial and legal record. • Help in clinical research. • Support decision analysis. Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Methods of Documentation • Source-oriented records • Problem-oriented medical records • PIE charting • Focus charting • Charting by exception • Case management model • Computerized documentation • Electronic medical records (EMRs) Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question Which of the following methods of documentation is unique in that it does not develop a separate plan of care but instead incorporates the plan of care into the progress notes? A. Source-oriented records B. Problem-oriented records C. PIE (problem, intervention, evaluation) D. Focus charting Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer: C. PIE (problem, intervention, evaluation) Rationale: PIE charting incorporates the plan of care into progress notes in which problems are identified by number. In source-oriented records, each healthcare group keeps data on its own separate form. Problem-oriented records are organized around patient problems rather than around sources of information. Focus charting brings the focus of care back to the patient and the patient’s concerns. Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Sample PIE Patient Care Note Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Sample Focus Patient Care Notes Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Case Management Models • Collaborative pathways • Variance charting Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Major Components of POMR • Defined database • Problem list • Care plans • Progress notes Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Formats for Nursing Documentation • Initial nursing assessment • Kardex and patient care summary • Plan of nursing care • Critical collaborative pathways • Progress notes • Flow sheets • Discharge and transfer summary • Home healthcare documentation • Long-term care documentation Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Types of Flow Sheets • Graphic record • 24 -hour fluid balance record • Medication record • 24 -hour patient care records and acuity charting forms Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question PIE notes, SOAP notes, focus charting, and charting by exception are examples of which of the following formats for nursing documentation? A. Critical/collaborative pathways B. Progress notes C. Flow sheets D. Discharge summary Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer: B. Progress notes Rationale: Progress notes inform caregivers of the progress a patient is making using the specified formats. Critical/collaborative pathways are standardized plans of care developed for a patient with designated diagnoses. Flow sheets are documentation tools included in the progress notes that record routine aspects of care. Discharge summaries are clinical reports written to summarize the patient record. Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Medicare Requirements for Home Healthcare • Patient is homebound and still needs skilled nursing care. • Rehabilitation potential is good (or patient is dying). • The patient’s status is not stabilized. • The patient is making progress in expected outcomes of care. Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Four Basic Components of RAI (Resident Assessment Tool) • Minimum data set • Triggers • Resident assessment protocols • Utilization guidelines Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Benefits of RAI • Residents respond to individualized care. • Staff communication becomes more effective. • Resident and family involvement increases. • Documentation becomes clearer. Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Change of Shift Report • Basic identifying information about each patient • Current appraisal of each patient’s health status – Changes in medical conditions and patient response to therapy – Where patient stands in relation to identified diagnoses and goals • Current orders (nurse and physician) and unfilled orders • Summary of each newly admitted patient • Report on patient transferred or discharged Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Two Nurses Confer at Change of Shift Report Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Methods of Reporting • Face-to-face meetings • Telephone conversations • Written messages • Audio-taped messages • Computer messages Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins

Conferring About Care • Consultations and referrals • Nursing and interdisciplinary team care conferences • Nursing care rounds Copyright © 2011 Wolters Kluwer Health | Lippincott Williams & Wilkins