Chapter 16 Lecture Book Title Edition Bleeding and

Chapter 16 Lecture Book Title Edition Bleeding and Shock Slide Presentation prepared by Randall Benner, M. Ed. , NREMT-P © 2012 Pearson Education, Inc.

Learning Objectives • Describe and demonstrate how to control external bleeding with direct pressure, air splints, and tourniquets. • Identify common signs of internal bleeding. • Describe and demonstrate procedures for controlling internal bleeding. © 2012 Pearson Education, Inc.

Learning Objectives • Understand the basic psychopathology of shock, and factors that may influence its severity. • Recognize various types of shock, and identify signs and symptoms. • Describe and demonstrate the management of various types of shock. © 2012 Pearson Education, Inc.

Severity of Bleeding • Depends on – – – – How fast blood is flowing from vessel Size of vessel Whether vessel is a vein or artery Whether bleeding is internal or external Where bleeding originated Victim’s age and weight Victim’s general physical condition Whether bleeding is a threat to airway and respiration © 2012 Pearson Education, Inc.
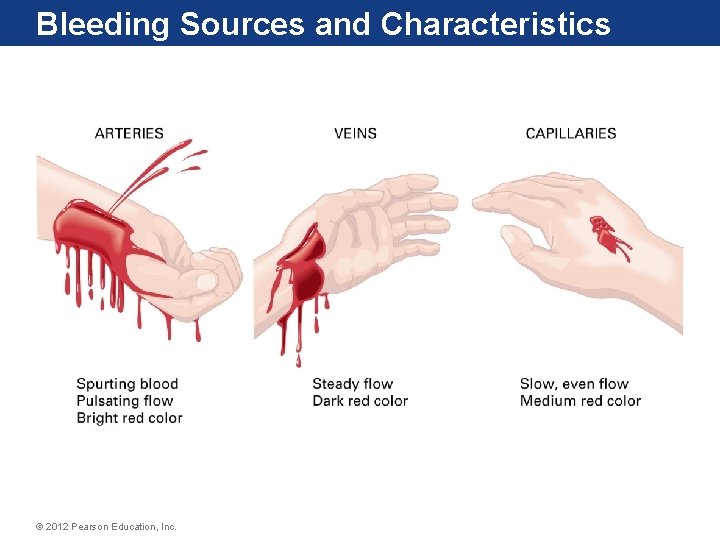
Bleeding Sources and Characteristics © 2012 Pearson Education, Inc.

Control of Bleeding • Steps to follow – Stop the bleeding. – Determine the cause and source of bleeding, and general condition of victim. – Place the victim in a position that minimizes blood loss. – Establish and maintain an open airway. © 2012 Pearson Education, Inc.

Protection from Infectious Disease • Precautions – Place a barrier between yourself and the victim’s blood, such as protective gear. – Don’t touch your mouth, nose, or eyes, or handle food. – When treatment concludes, wash hands thoroughly; brush under fingernails. – Wash thoroughly all items that touched the victim’s blood or body fluids. © 2012 Pearson Education, Inc.

Direct Pressure and Elevation • Best way to control bleeding is applying direct pressure to the wound. • Place a sterile cover wound and press firmly. • Elevation may be used with direct pressure, although its effectiveness has not been proved. • Can also use a cold pack over the wound, along with pressure and elevation. • Check dressing regularly. • Never apply pressure if there is an object in the wound or a protruding bone. © 2012 Pearson Education, Inc.

Other Treatments • If needed, pressure on dressing can be increased by using – A pressure bandage – An air splint – A blood pressure cuff • A tourniquet should be used if direct pressure fails to control bleeding. © 2012 Pearson Education, Inc.
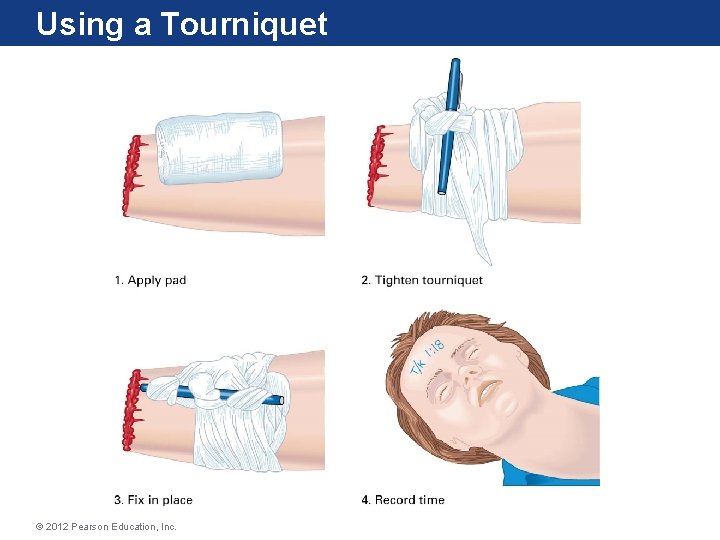
Using a Tourniquet © 2012 Pearson Education, Inc.

Internal Bleeding • The result of blunt or penetrating trauma, or fractures • Although not visible, it can be serious or fatal • Signs and Symptoms – Injury evidence such as bruising to abdomen or chest, or deformed upper thigh – Evidence of shock (restlessness, anxiety; cool, clammy skin; weak, rapid pulse; rapid breathing) – Other signs depend on source of bleeding; see Table 6. 2 in text © 2012 Pearson Education, Inc.

Internal Bleeding: First Aid Care • Activate EMS first. • Establish and maintain open airway, and monitor ABCDs (see Chapter 3). • Assess for fractures; apply a splint if needed. • Keep the victim quiet. • Position and treat the victim for shock; keep victim warm. • If the victim vomits, place in recovery/coma position. • Monitor symptoms every five minutes until EMS personnel arrive. © 2012 Pearson Education, Inc.
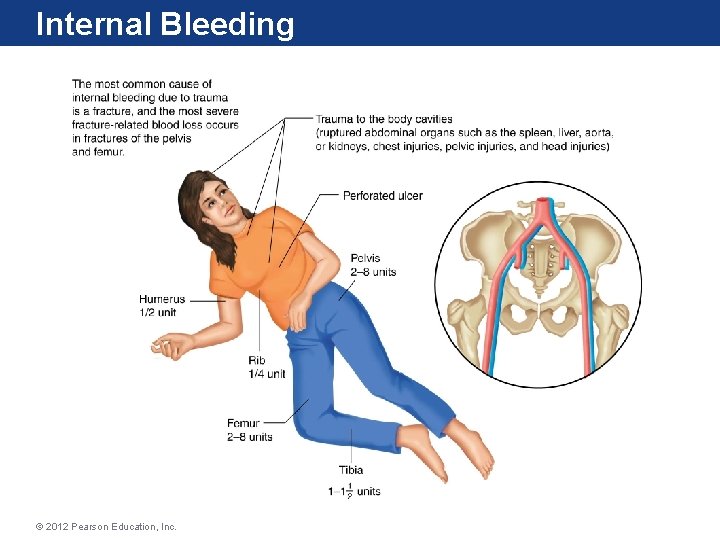
Internal Bleeding © 2012 Pearson Education, Inc.

Nosebleed • Assess for fractures; apply a splint if needed. • Results from injury, disease, activity, temperature extremes, or other causes • If severe or uncontrolled, it can lead to shock • If a skull fracture is suspected, do NOT try to stop the flow of blood; instead, cover opening loosely with dry and sterile dressing, activate EMS, and treat for skull fracture (see Chapter 13) © 2012 Pearson Education, Inc.

Shock • Inadequate delivery of blood (oxygen) and glucose (nutrients) to the cells • Fatal if left untreated • A progressive process that can be either gradual or rapid • Throughout the progression of shock, the victim’s condition constantly changes • The body cells most sensitive to lack of oxygen are in the heart, brain, and lungs © 2012 Pearson Education, Inc.
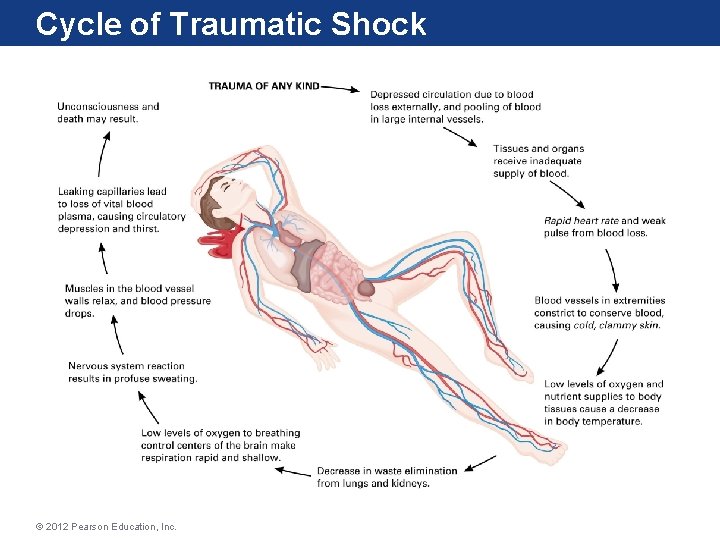
Cycle of Traumatic Shock © 2012 Pearson Education, Inc.

Causes of Shock • Four basic causes – Fluid is lost from circulatory system (often from bleeding, burns, or dehydration) – Heart fails to pump blood effectively – Blood vessels dilate, causing blood to pool in extremities and nonvital areas – Forward movement of blood through the body is obstructed © 2012 Pearson Education, Inc.

Types of Shock • Hypovolemic: Characterized by loss of blood (hemorrhaging) • Cardiogenic: Cardiac muscle (heart) does not pump effectively • Distributive: Extreme blood vessel dilation, often associated with spinal cord injury • Obstructive: Blockage of blood movement, often associated with blood clots © 2012 Pearson Education, Inc.

Stages of Shock • Compensatory: First stage; body tries to use its normal defense mechanisms • Progressive: Second stage; body moves blood toward heart, brain and lungs to preserve functioning; blood pressure drops • Irreversible: Final stage; multiple organs start to fail, death follows © 2012 Pearson Education, Inc.

Signs and Symptoms of Shock • • • Dizziness or fainting Anxious or dull expression Nausea; possible vomiting; extreme thirst Cool, clammy, moist skin Shallow, labored, or grasping breathing In dark-skinned people, skin around the mouth may turn grayish; lips or nail beds may be blue; mucous membranes of the mouth may look pale or waxy • Light-skinned people may have pale, dull skin color © 2012 Pearson Education, Inc.
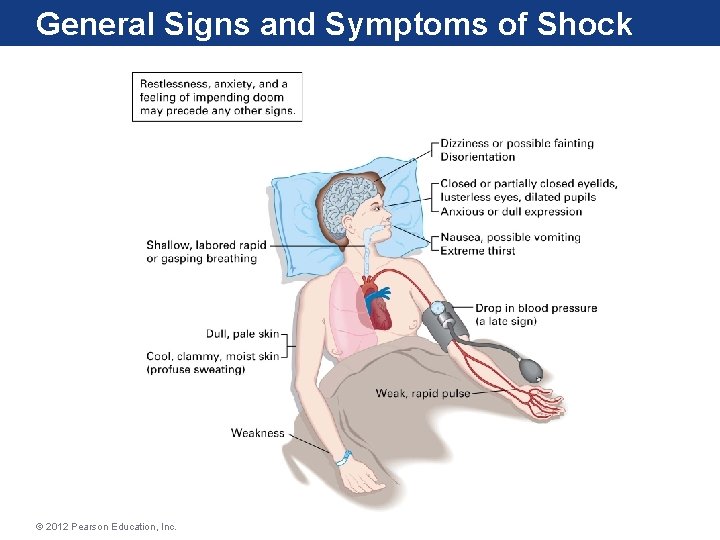
General Signs and Symptoms of Shock © 2012 Pearson Education, Inc.
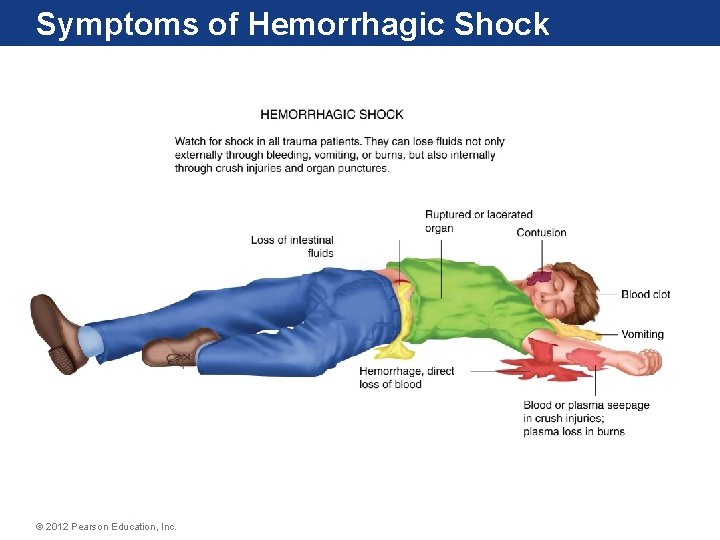
Symptoms of Hemorrhagic Shock © 2012 Pearson Education, Inc.
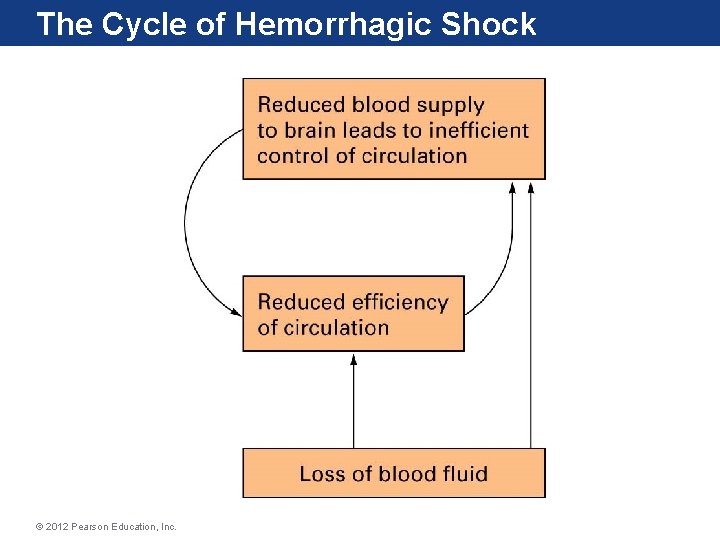
The Cycle of Hemorrhagic Shock © 2012 Pearson Education, Inc.

Preventing Shock • Never wait for signs to develop or worsen; prevention is always best. • Ensure that the victim’s airway is open and breathing is adequate. • Control bleeding. • Splint or immobilize fractures as needed. • Relieve pain via proper wound dressing, bandaging, splinting, and body positioning. • Keep the victim supine. • Keep the victim warm (but not hot). © 2012 Pearson Education, Inc.

Anaphylactic Shock • A severe allergic reaction caused by an immune response • Often the result of insect bites or stings, foods, medicines, or other substances • A dire medical emergency • Generally occurs most rapidly if the allergen/antigen is injected • Untreated victims can die within minutes of contacting the allergen/antigen © 2012 Pearson Education, Inc.

Anaphylactic Shock: Signs and Symptoms • Symptoms can occur in any combination, and affect the skin, heart, blood vessels, respiratory system, gastrointestinal tract, and/or central nervous system • Flushed, itching skin • Sneezing, watery eyes and nose • Skin rash • Swollen airway • “Tickle” or lump in throat that won’t go away • Gastrointestinal complaints © 2012 Pearson Education, Inc.
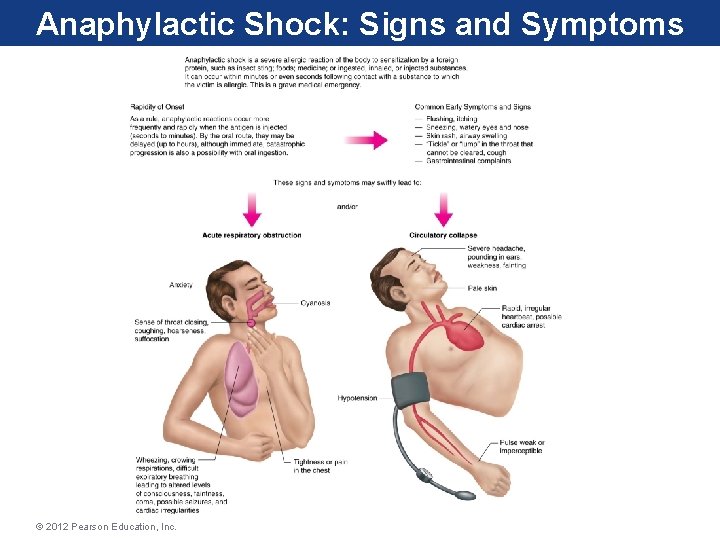
Anaphylactic Shock: Signs and Symptoms © 2012 Pearson Education, Inc.

Anaphylactic Shock Management • • Activate EMS system immediately. Secure and maintain an open airway. If indicated, perform rescue breathing or CPR. If the victim has an epinephrine auto-injector (epi pen), help them to use it if allowed by local protocols. © 2012 Pearson Education, Inc.

Summary • Severity of bleeding depends on multiple factors, including blood speed, source, and origin. • Bleeding can often be effectively controlled through direct pressure in concert with other methods. • Internal bleeding can lead to shock and must be medically treated immediately. • Shock is a serious, progressive condition that can result in death if untreated. • The best approach to shock management is prevention. © 2012 Pearson Education, Inc.
- Slides: 29