Chapter 16 Fluid and Chemical Balance Copyright 2009

Chapter 16 Fluid and Chemical Balance Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Body Fluid • Body fluid is a mixture of: – Water – Electrolytes – Nonelectrolytes – Blood cells Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Fluid Transport Mechanisms • Osmosis • Filtration • Passive diffusion • Facilitated diffusion • Active transport Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Assessing a Client’s Fluid Status • Signs of deficit or excess • Physical assessment • Measurement of intake • Output volumes • Intake and output (I&O) tool • Loss over 24 -hour period Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Common Fluid Imbalances • Hypovolemia: low volume in extracellular fluid compartments • Hypervolemia: excess water in intravascular fluid compartment • Third-spacing: movement of intravascular fluid to nonvascular fluid compartments Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Restoring Fluid Volume • Treating the cause of hypovolemia • Increasing oral intake • Administering IV fluid replacements • Controlling fluid losses • Using a combination of these measures Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Reducing Fluid Volume • Treating the disorder contributing to the increased fluid volume • Restricting or limiting oral fluids • Reducing salt consumption • Discontinuing IV fluid infusions or reducing the infusing volume • Administering drugs that promote urine elimination • Using a combination of the above interventions Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Administering Intravenous Fluids • Maintain or restore fluid balance when oral replacement is inadequate or impossible • Maintain or replace electrolytes • Administer water-soluble vitamins • Provide a source of calories • Administer drugs • Replace blood and blood products Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question • Is the following statement true or false? Reducing salt consumption helps restore fluid volume. Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer False. Reducing salt consumption helps reduce fluid volume. Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Crystalloid and Colloid Solutions Crystalloid solutions are made of water and other uniformly dissolved crystals such as salt and sugar Colloid solutions are made of water and molecules of suspended substances such as blood cells and blood products (such as albumin) Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Types of Intravenous Solutions • Isotonic: contains the same concentration of dissolved substances as normally found in plasma • Hypotonic: contains fewer dissolved substances than normally found in plasma • Hypertonic: more concentrated than body fluid and draws cellular and interstitial water into the intravascular compartment Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins
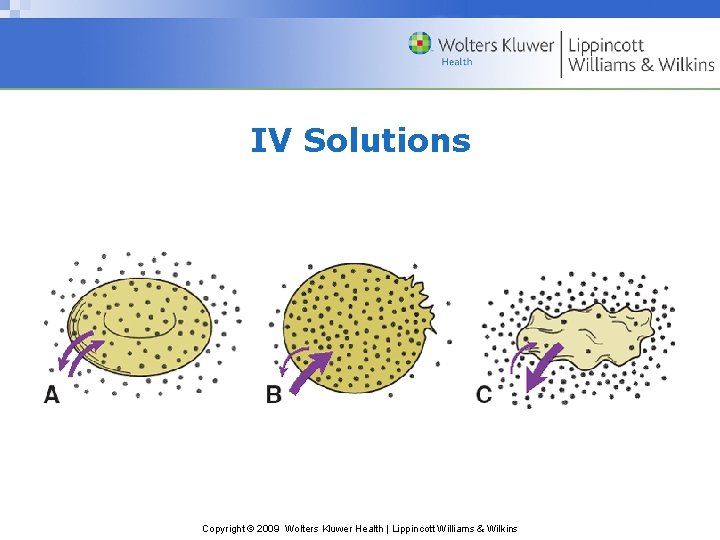
IV Solutions Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question • Is the following statement true or false? Blood is an example of crystalloid solution. Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer False. Blood is an example of colloid solution. Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Types of Tubing • Primary or secondary tubing • Vented or unvented tubing • Microdrip or macrodrip chamber • Unfiltered or filtered tubing • Needle or needleless access ports Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Unvented and Vented Tubing Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Techniques for Infusing Intravenous Solutions • Gravity infusion • Electronic infusion devices • Infusion pumps • Volumetric controllers Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins
Vein Selection • Venipuncture device is inserted in veins of: – Hand in adults – Scalp in child – Forearm in adults Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Complications With IV Administration • Circulatory overload • Infiltration • Phlebitis • Thrombus formation • Pulmonary embolus • Infection • Air embolism Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Inserting an Intermittent Venous Access Device • When client no longer needs continuous infusions of fluid • When client needs intermittent IV medication • When client needs emergency IV fluid or medications Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins
Intermittent Venous Access Device Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Blood Administration • Blood collection and storage • Blood safety • Blood compatibility • Blood transfusion equipment – Catheter or needle gauge – Blood transfusion tubing Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Transfusion Reactions • Febrile nonhemolytic transfusion reaction • Viral infection • Bacterial infection • Acute hemolytic reaction • Anaphylactic reaction Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Parenteral Nutrition • Intravenous administration of nutrients such as protein, carbohydrate, fat, vitamins, minerals, and trace elements – Peripheral parenteral nutrition – Total parenteral nutrition – Lipid emulsions Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Question • Is the following statement true or false? The venipuncture device is inserted in hand veins in infants or small children. Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

Answer False. The venipuncture device is inserted in scalp veins in infants or small children. Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

General Gerontologic Considerations • Older adults at risk for fluid and electrolyte imbalances due to cardiac meds and chronic conditions – Encourage fluid intake to keep oral mucosa moist and provides hydration • Offer noncaffeinated beverages; offer fluids at non-meal times • When fasting before procedures, ensure prior increased oral fluid intake Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

General Gerontologic Considerations (cont’d) • Indicators of dehydration – Test skin turgor over sternum – Mental status changes – Increased pulse and respiration rates – Decreased blood pressure – Dark, concentrated urine with high specific gravity Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins

General Gerontologic Considerations (cont’d) • Indicators of dehydration (cont’d) – Dry mucous membranes – Warm skin, furrowed tongue – Low urine output – Hardened stools Copyright © 2009 Wolters Kluwer Health | Lippincott Williams & Wilkins
- Slides: 30