Chapter 15 The Cardiovascular System Heart Introduction to








- Slides: 32

Chapter 15: The Cardiovascular System Heart

Introduction to the Heart � Hold up your clenched fist � Your heart is about the size of your fist ◦ Varies by gender, and age of the owner �Age changes are due to increases in the size of cells, not number of cells � Average mass of a heart 230 -350 grams (0. 5 – 0. 8 pounds)

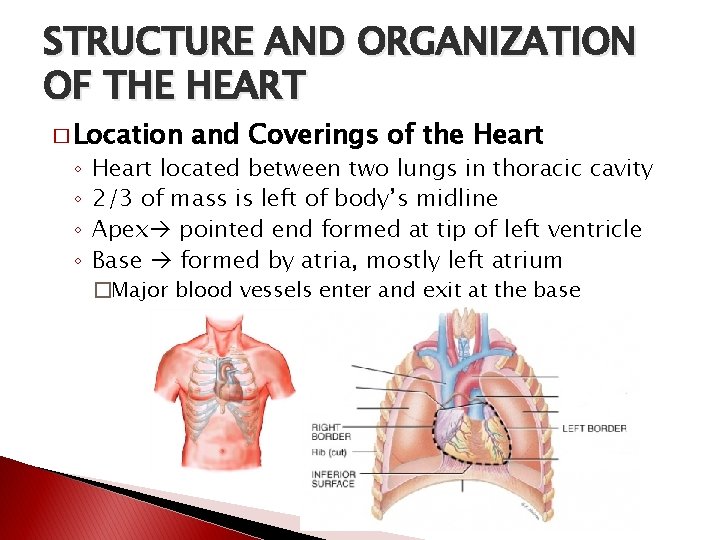
STRUCTURE AND ORGANIZATION OF THE HEART � Location ◦ ◦ and Coverings of the Heart located between two lungs in thoracic cavity 2/3 of mass is left of body’s midline Apex pointed end formed at tip of left ventricle Base formed by atria, mostly left atrium �Major blood vessels enter and exit at the base

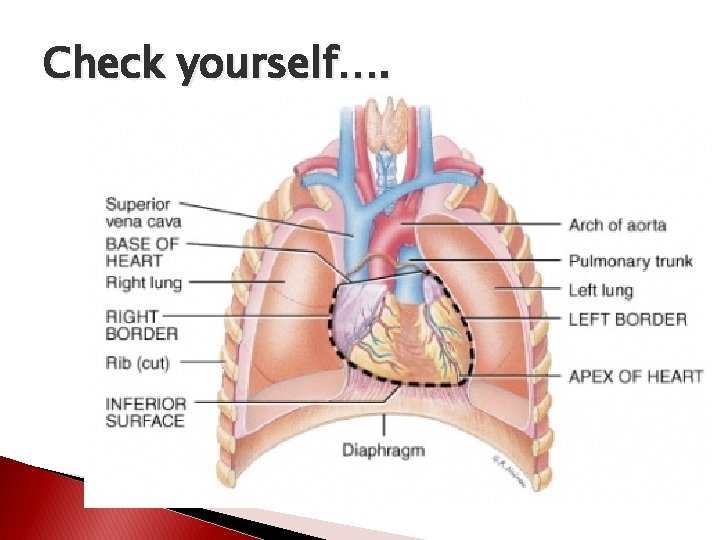
Check yourself….

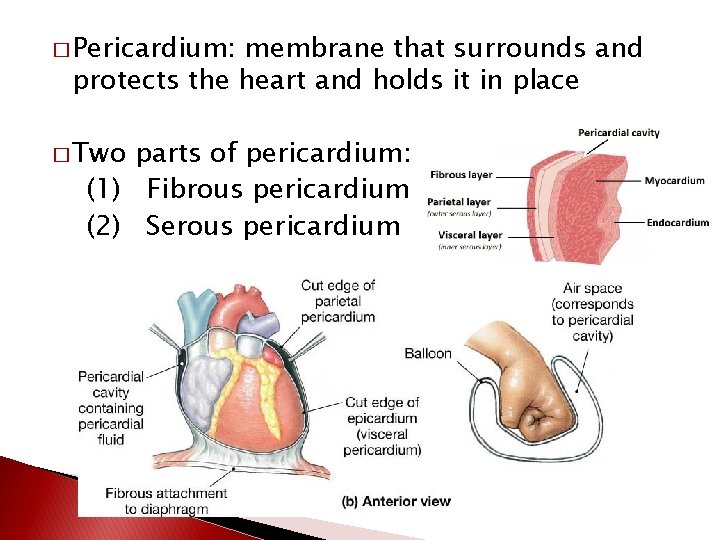
� Pericardium: membrane that surrounds and protects the heart and holds it in place � Two parts of pericardium: (1) Fibrous pericardium (2) Serous pericardium

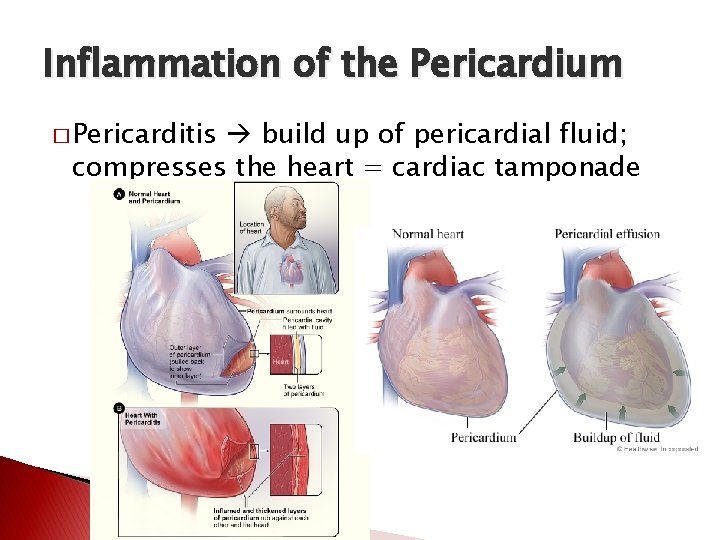
Inflammation of the Pericardium � Pericarditis build up of pericardial fluid; compresses the heart = cardiac tamponade

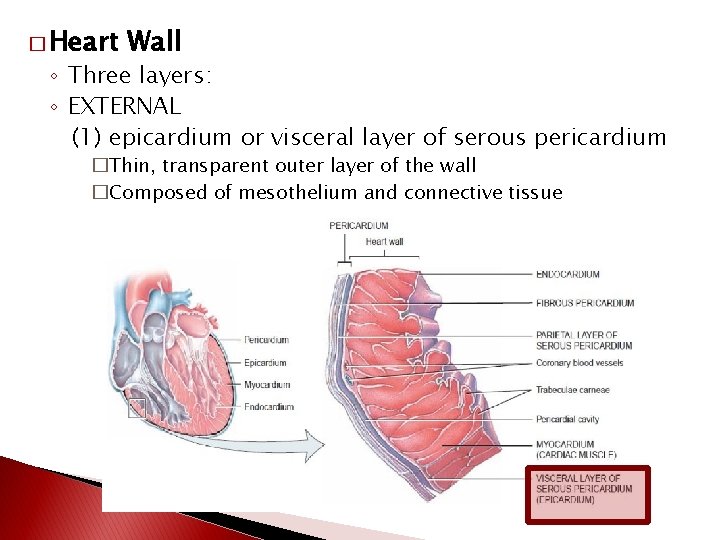
� Heart Wall ◦ Three layers: ◦ EXTERNAL (1) epicardium or visceral layer of serous pericardium �Thin, transparent outer layer of the wall �Composed of mesothelium and connective tissue

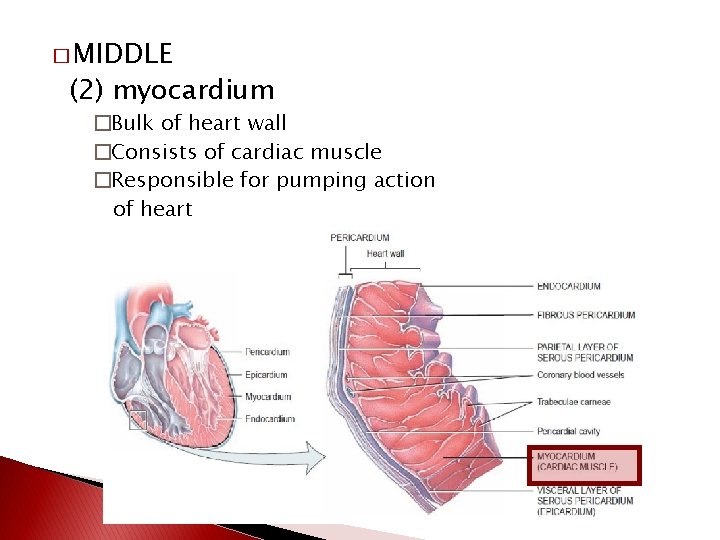
� MIDDLE (2) myocardium �Bulk of heart wall �Consists of cardiac muscle �Responsible for pumping action of heart

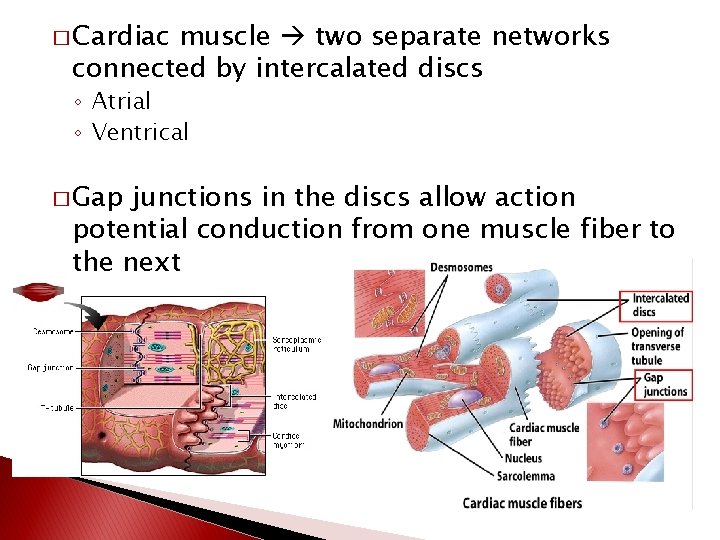
� Cardiac muscle two separate networks connected by intercalated discs ◦ Atrial ◦ Ventrical � Gap junctions in the discs allow action potential conduction from one muscle fiber to the next

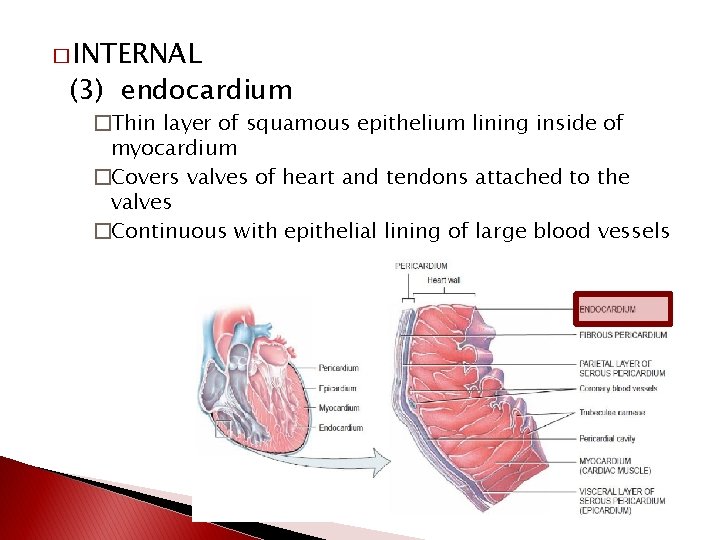
� INTERNAL (3) endocardium �Thin layer of squamous epithelium lining inside of myocardium �Covers valves of heart and tendons attached to the valves �Continuous with epithelial lining of large blood vessels

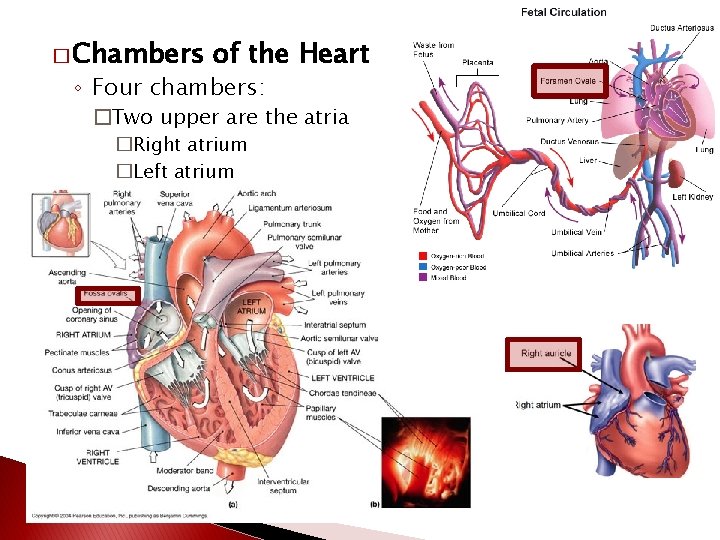
� Chambers of the Heart ◦ Four chambers: �Two upper are the atria �Right atrium �Left atrium

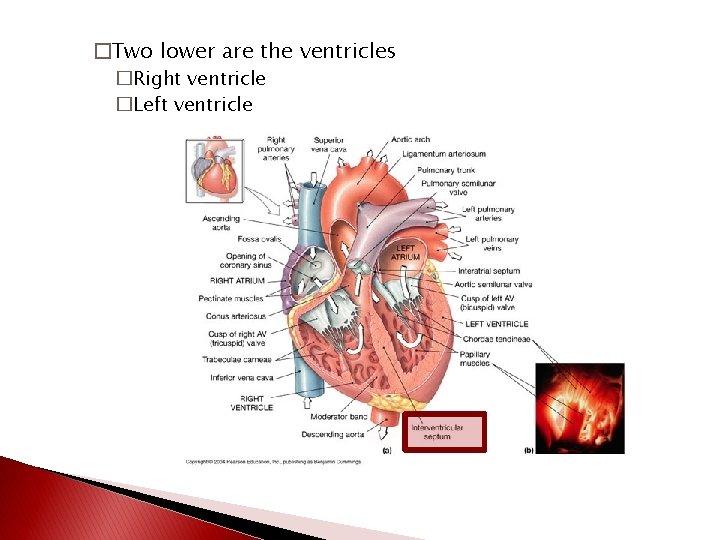
�Two lower are the ventricles �Right ventricle �Left ventricle

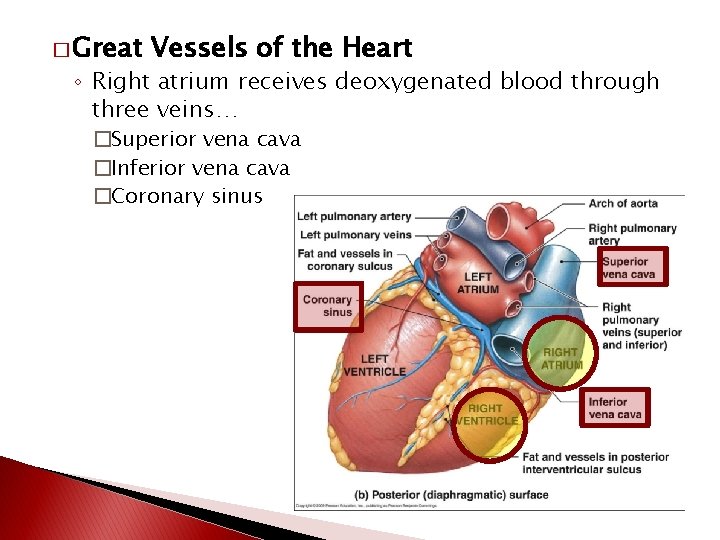
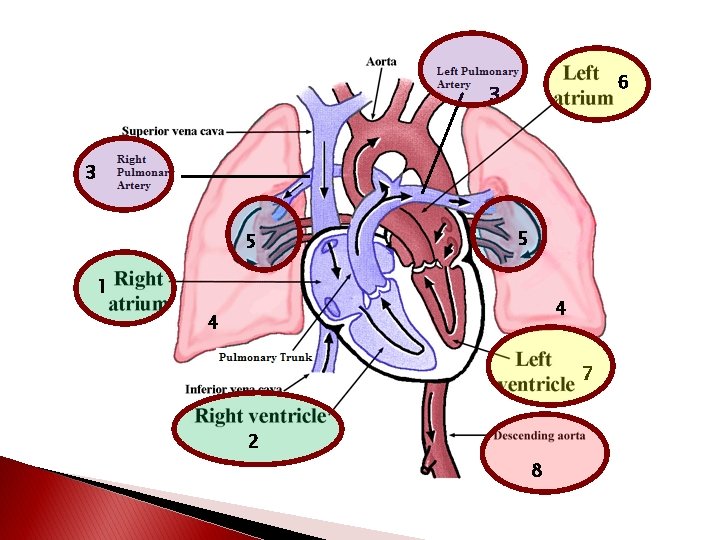
� Great Vessels of the Heart ◦ Right atrium receives deoxygenated blood through three veins… �Superior vena cava �Inferior vena cava �Coronary sinus

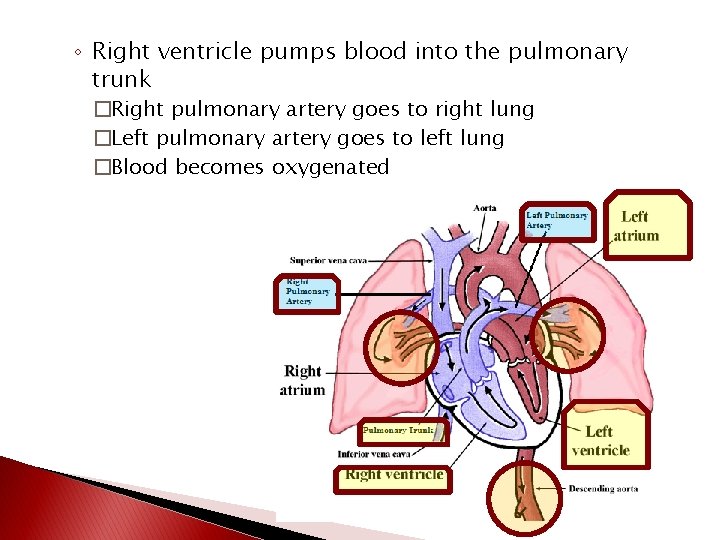
◦ Right ventricle pumps blood into the pulmonary trunk �Right pulmonary artery goes to right lung �Left pulmonary artery goes to left lung �Blood becomes oxygenated

6 3 3 5 5 1 4 4 7 2 8


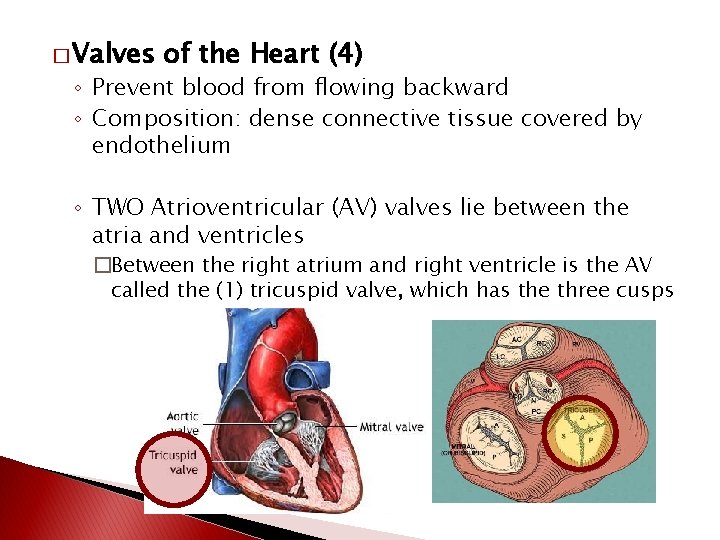
� Valves of the Heart (4) ◦ Prevent blood from flowing backward ◦ Composition: dense connective tissue covered by endothelium ◦ TWO Atrioventricular (AV) valves lie between the atria and ventricles �Between the right atrium and right ventricle is the AV called the (1) tricuspid valve, which has the three cusps

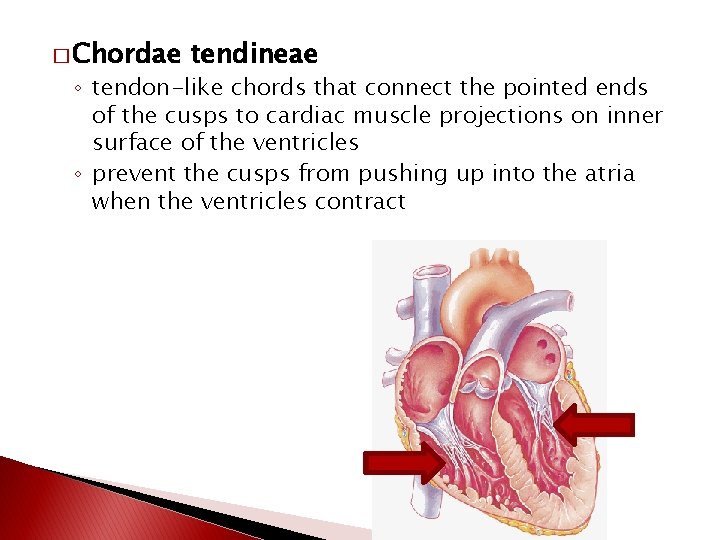
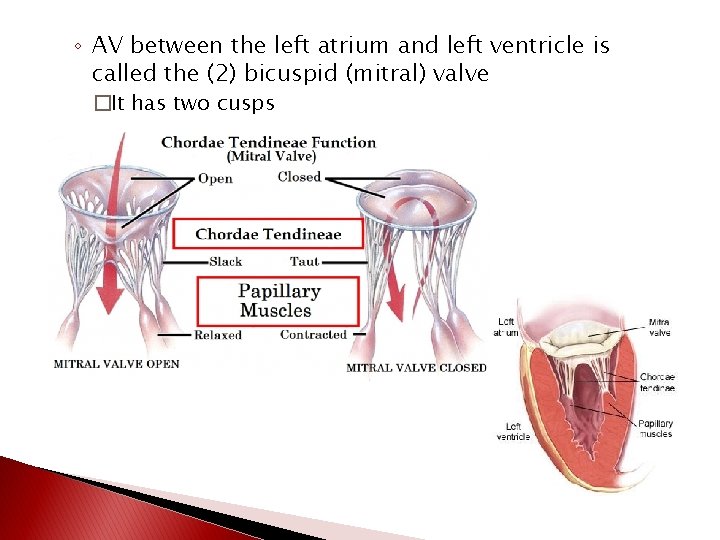
� Chordae tendineae ◦ tendon-like chords that connect the pointed ends of the cusps to cardiac muscle projections on inner surface of the ventricles ◦ prevent the cusps from pushing up into the atria when the ventricles contract

◦ AV between the left atrium and left ventricle is called the (2) bicuspid (mitral) valve �It has two cusps

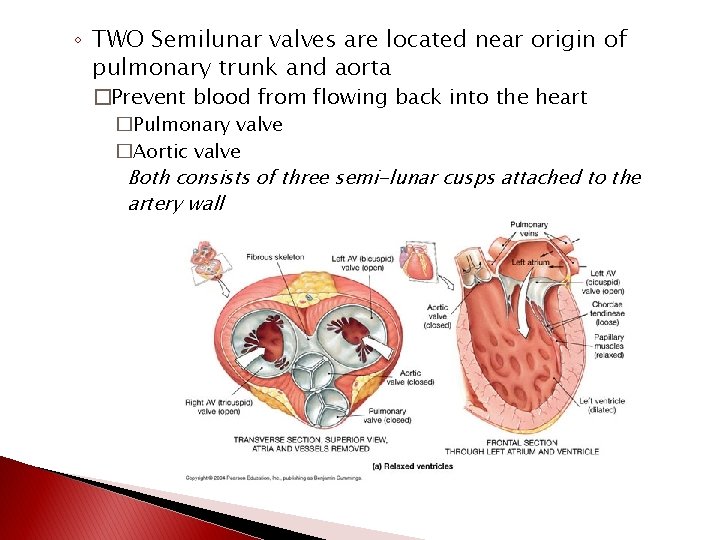
◦ TWO Semilunar valves are located near origin of pulmonary trunk and aorta �Prevent blood from flowing back into the heart �Pulmonary valve �Aortic valve Both consists of three semi-lunar cusps attached to the artery wall

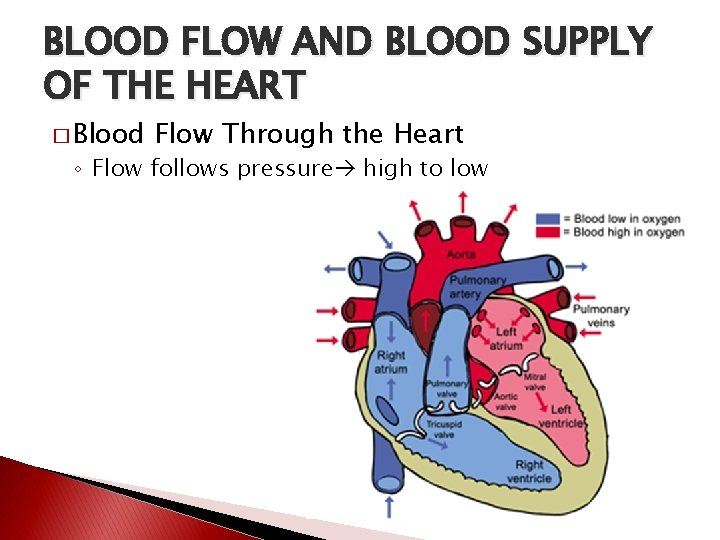
BLOOD FLOW AND BLOOD SUPPLY OF THE HEART � Blood Flow Through the Heart ◦ Flow follows pressure high to low

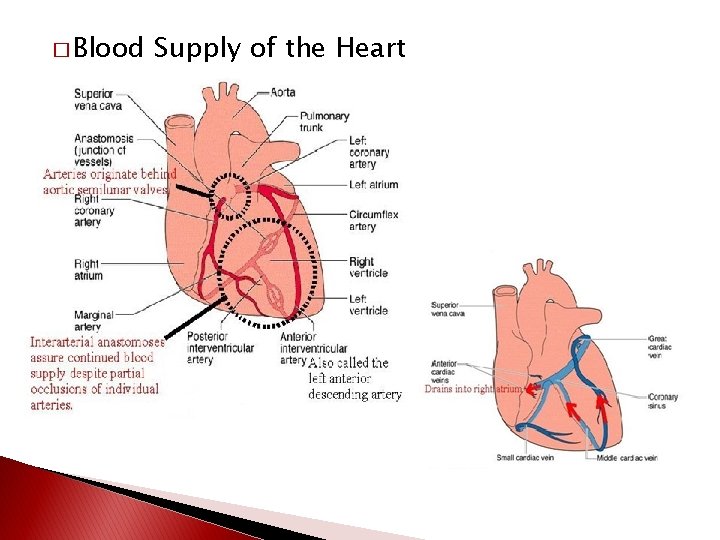
� Blood Supply of the Heart

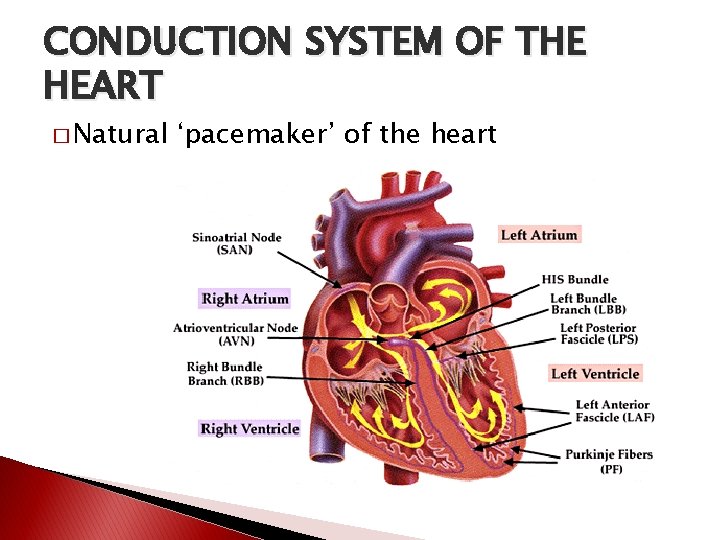
CONDUCTION SYSTEM OF THE HEART � Natural ‘pacemaker’ of the heart

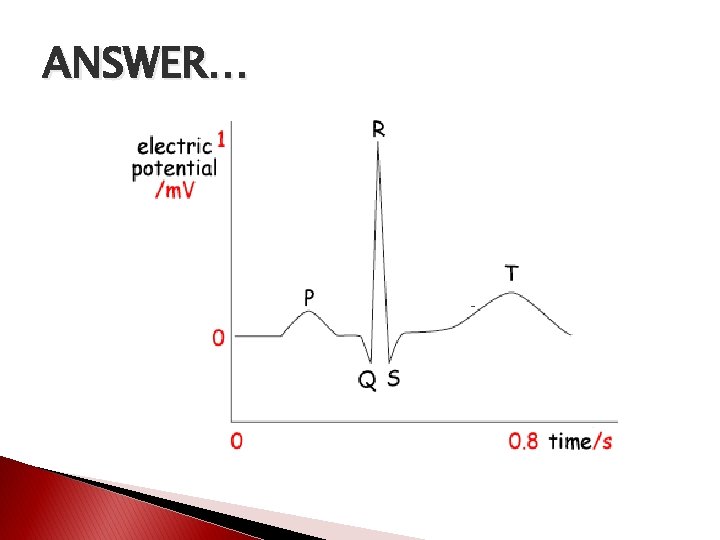
ELECTROCARDIOGRAM � Recordings of the electrical changes that accompany the heartbeat are called electrocardiograms or EKG or ECG

ANSWER…

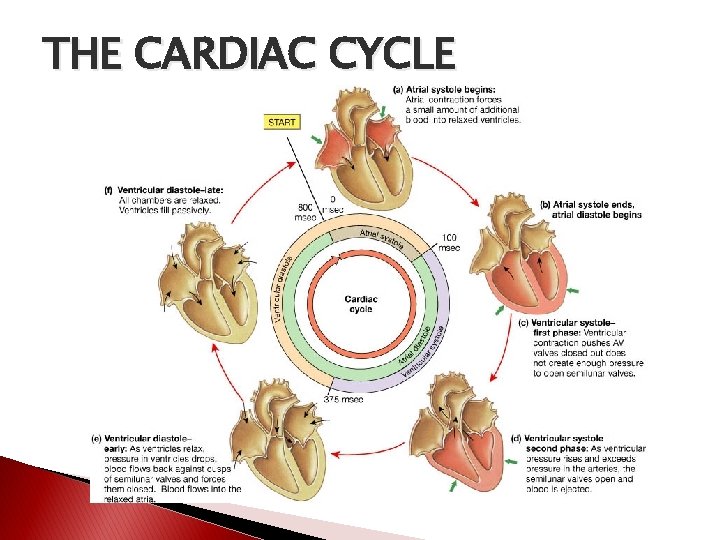
THE CARDIAC CYCLE

� Heart Sounds ◦ Come mainly from turbulence created by blood flow when valves close �First sound lubb �Loud booming sound from AV valves closing after ventricular systole begins �Second sound dubb �Short, sharp sound from SL valves closing at end of ventricular systole � Next a pause…so lubb, dubb, pause, lubb, dubb, pause

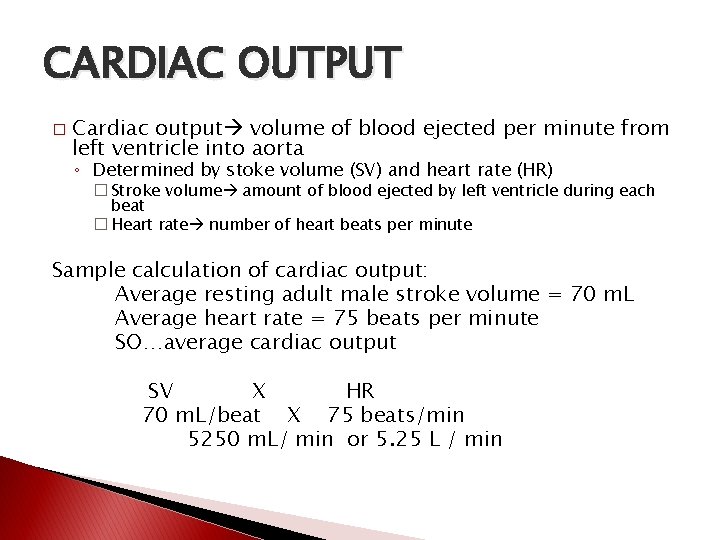
CARDIAC OUTPUT � Cardiac output volume of blood ejected per minute from left ventricle into aorta ◦ Determined by stoke volume (SV) and heart rate (HR) � Stroke volume amount of blood ejected by left ventricle during each beat � Heart rate number of heart beats per minute Sample calculation of cardiac output: Average resting adult male stroke volume = 70 m. L Average heart rate = 75 beats per minute SO…average cardiac output SV X HR 70 m. L/beat X 75 beats/min 5250 m. L/ min or 5. 25 L / min

� Regulation � Three of Stroke Volume factors: ◦ The degree of stretch in the heart before it contracts �More stretch means more forceful contraction ◦ The forcefulness of contraction of individual ventricular muscle fibers ◦ The pressure required to eject blood from the ventricle

� Autonomic Regulation of Heart Rate ◦ Originates in cardiovascular center (CV) in medulla oblongata ◦ Input comes in from a variety of sensory receptors (barorecptors and chemoreceptors) from higher brain centers ◦ Then output is directed through increasing or decreasing frequency of nerve impulses sent to sympathetic and parasympathetic branches �Sympathetic neurons reach heart through cardiac accelerator nerves that innervate conduction system, atria, and ventricles releasing norepinephrine to increase heart rate �Parasympathetic neurons reach heart through vagus (X) nerves that extend conduction system and atria releasing acetylcholine (ACh) to decrease heart rate

� Chemical Regulation of Heart Rate ◦ Hormones �Epinedrine �Norepindrine �Increase heart pumping effectiveness by increasing heart rate and contraction force ◦ Ions �K+ and Na+ �Decrease heart rate and contraction force �Ca+ �Increase heart rate and contraction force

� Other ◦ ◦ Factors in Heart Rate Regulation Age Gender Physical fitness Body temperature