Chapter 15 AUTONOMIC NERVOUS SYSTEM By Yvan Rostand

Chapter 15 AUTONOMIC NERVOUS SYSTEM By Yvan Rostand S. MD Copyright © Mc. Graw-Hill Education. Permission required for reproduction or display. 1

15. 1 a Functional Organization • Somatic nervous system (SNS) – Consciously perceived or controlled processes Somatic sensory portion detects signals from special senses (vision, hearing, equilibrium, smell, taste) and from skin and proprioceptors Somatic motor portion sends signals from CNS to skeletal muscles o Voluntary movements involve cerebrum o Reflexive movements involve brainstem and spinal cord Copyright © 2016 Mc. Graw-Hill Education. All rights reserved. No reproduction or distribution without the prior written consent of Mc. Graw-Hill Education 2
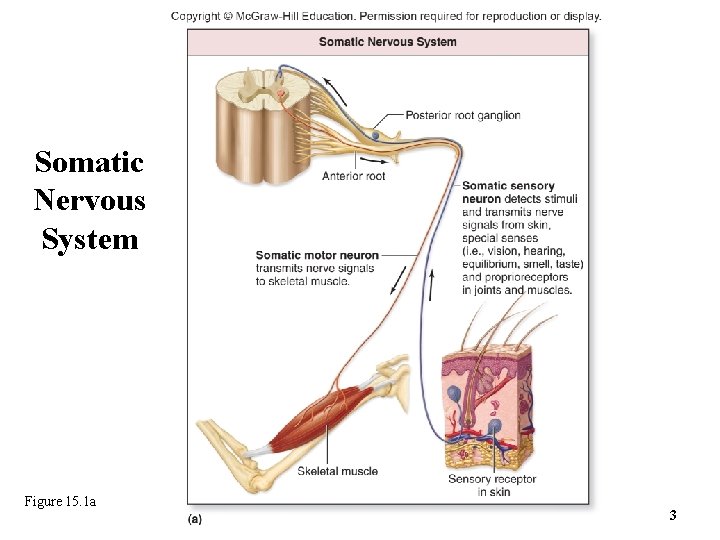
Somatic Nervous System Figure 15. 1 a 3

15. 1 a Functional Organization • Autonomic nervous system (ANS) – – Also called autonomic motor or visceral motor system Processes regulated below conscious level Transmits signals from CNS to heart, smooth muscle, glands Responds to visceral sensory inputs (e. g. , from blood vessels) o Those sensory neurons are not considered part of ANS – Functions to maintain homeostasis o Keeps conditions inside body within optimal ranges 4
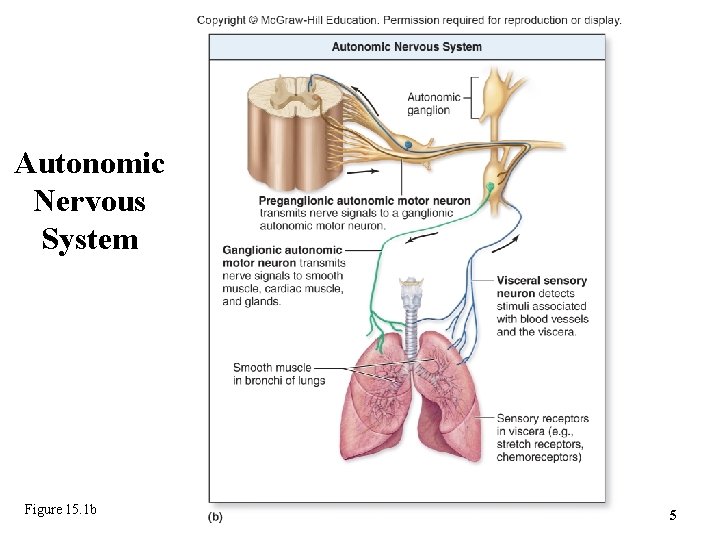
Autonomic Nervous System Figure 15. 1 b 5

15. 1 b Lower Motor Neurons of the Somatic Versus Autonomic Nervous System • Lower motor neurons of somatic nervous system – A ‘single’ lower motor neuron extends from CNS to skeletal muscle fibers o Cell body within brainstem or spinal cord o Myelinated axon with large diameter o Releases acetylcholine (ACh) from synaptic knob to excite muscle fiber 6

15. 1 b Lower Motor Neurons of the Somatic Versus Autonomic Nervous System • Lower motor neurons of autonomic nervous system – ANS uses a chain of ‘two’ motor neurons to reach effector – First is the preganglionic neuron o Cell body within brainstem or spinal cord o Thin, myelinated axon projects to autonomic ganglion in peripheral nervous system o Releases ACh from synaptic knob to excite second motor neuron – Second is the ganglionic (postganglionic) neuron o Cell body within autonomic ganglion o Very thin, unmyelinated axon projects to cardiac muscle, smooth muscle, or gland o Releases ACh or norepinephrine (NE) from synaptic knob to either excite or inhibit the effector (effectors have a variety of receptor types) 7

Lower Motor Neurons of the Autonomic Nervous System Figure 15. 2 8

15. 1 b Lower Motor Neurons of the Somatic Versus Autonomic Nervous System • Lower motor neurons of ANS (continued ) – What advantages are there for the ANS to use a chain of two neurons instead of just one neuron? o Allows for neuronal convergence: multiple preganglionic neurons synapsing on one ganglionic neuron o Allows for neuronal divergence: branches of axon from one preganglionic neuron synapsing with numerous ganglionic neurons 9

15. 1 c CNS Control of the Autonomic Nervous System • ANS is regulated by parts of brain and spinal cord • Hypothalamus is crucial (contains nuclei controlling both divisions of the ANS) – Crucial for emotional ANS processes such as fight-or-flight – Can be influenced by areas of cortex, thalamus, limbic system • Brainstem nuclei mediate visceral reflexes – E. g. , maintenance of blood pressure • Spinal cord governs some ANS reflexes – E. g. , defecation and urination as controlled by the parasympathetic nervous system 10
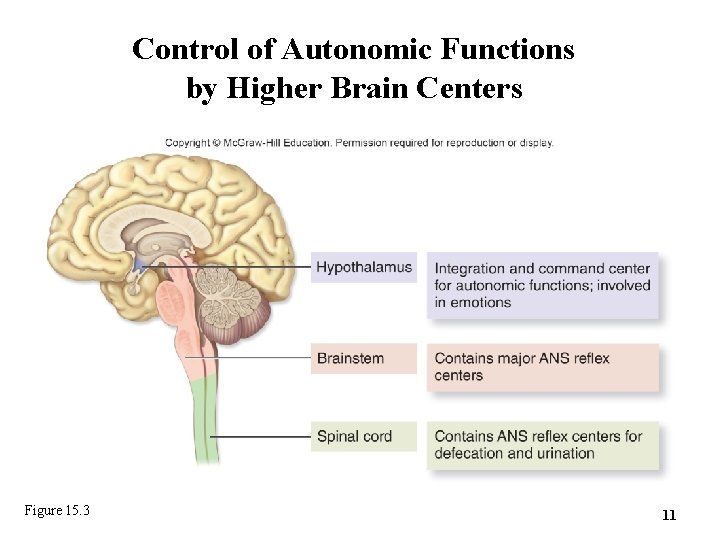
Control of Autonomic Functions by Higher Brain Centers Figure 15. 3 11

What did you learn? • Since thick, myelinated axons conduct the fastest, and since synapses cause delays, which sends motor signals more rapidly, the SNS or ANS? • What neurotransmitter is released by preganglionic neurons of the ANS? Copyright © 2016 Mc. Graw-Hill Education. All rights reserved. No reproduction or distribution without the prior written consent of Mc. Graw-Hill Education 12

15. 2 a Functional Differences • Parasympathetic and sympathetic divisions of ANS have complimentary functions – Parasympathetic division: “rest-and-digest” o For conserving energy, replenishing nutrients – Sympathetic division: “fight-or-flight” o For exercise, excitement, emergency 13

15. 2 b Anatomic Differences in Lower Motor Neurons • Parasympathetic – Craniosacral division – Preganglionic neurons in brainstem or S 2–S 4 spinal cord – Preganglionic axons are long, postganglionic axons are short o Ganglia are close to or within the effector organ – Preganglionic axons have few branches • Sympathetic – Thoracolumbar division – Preganglionic neuron in lateral horns of T 1–L 2 – Preganglionic axons are short, postganglionic axons are long o Ganglia are close to spinal cord (lateral or anterior to it) – Preganglionic axons have many branches 14

Comparison of Parasympathetic and Sympathetic Divisions Figure 15. 4 15
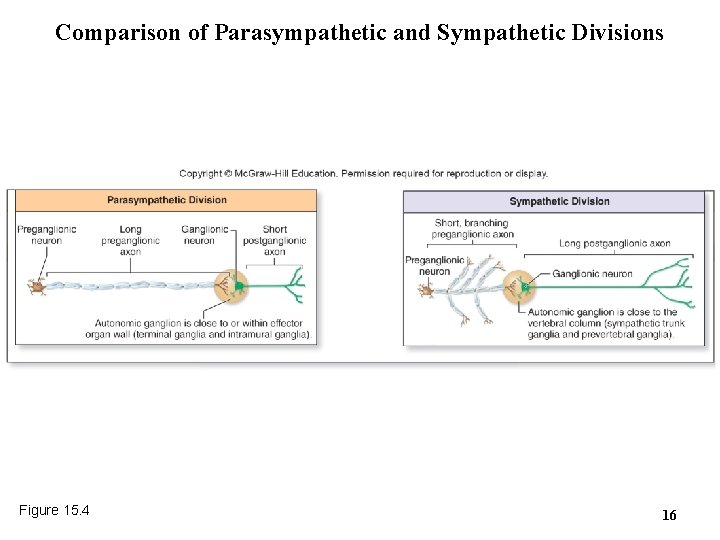
Comparison of Parasympathetic and Sympathetic Divisions Figure 15. 4 16

15. 2 c Degree of Response • Parasympathetic activity is fairly localized – Long preganglionic axons with limited branches influence only one or a few effectors at the same time • Sympathetic activity often facilitates mass activation – Short preganglionic axons with many branches simultaneously influence several effectors o Exercise or fear can stimulate changes in many organ systems – Sympathetic stimulation of the release of adrenal medulla hormones facilitates this – Sometimes, however, a single effector can be engaged o E. g. , sympathetic activity triggering just pupil dilation in low light 17

What did you learn? • Which ANS division is for “flight-or-flight”? • The vagus nerve contains many parasympathetic preganglionic axons. Are these axons long or short? • Which ANS division tends to cause more localized physiological changes? 18 Copyright © 2016 Mc. Graw-Hill Education. All rights reserved. No reproduction or distribution without the prior written consent of Mc. Graw-Hill Education

15. 3 Parasympathetic Division • Parasympathetic function: maintain homeostasis at rest • Craniosacral anatomical origin • Ganglia found in two types of locations – Terminal ganglia located close to effector – Intramural ganglia located within wall of target organ 19

15. 3 a Cranial Components • Four cranial nerves convey (assoc. ) parasympathetic signals – Oculomotor, facial, glossopharyngeal, and vagus nerves 1 - Oculomotor Nerve (CN III) – Preganglionic axons from cell bodies in midbrain nuclei extend to ciliary ganglion within the orbit o Postganglionic axons control ciliary muscle (lens focus for near objects) and pupil constriction (iris sphincter) 2 - Facial Nerve (CN VII) – Preganglionic axons with cell bodies in pons extend to pterygopalatine and submandibular ganglia o Postganglionic axons from pterygopalatine ganglion control lacrimal glands and small glands of nose and mouth o Postganglionic axons from submandibular glands control submandibular and sublingual salivary glands 20

15. 3 a Cranial Components 3 - Glossopharnygeal Nerve (CN IX) – Preganglionic axons from cell bodies in medulla extend to otic ganglion near o Postganglionic axons control parotid salivary gland 4 - Vagus Nerve (CN X) – Preganglionic axons from cell bodies in medulla project extensively to a variety of ganglia in thorax and abdomen o Postganglionic axons have a variety of functions including: slowing heart rate, constricting lung bronchioles, increasing digestive secretions, storing carbohydrates 21

15. 3 b Pelvic Splanchnic Nerves • Pelvic splanchnic nerves – Preganglionic axons from cell bodies in lateral gray regions of S 2–S 4 project to ganglionic neurons in terminal or intramural ganglia – Contribute to superior and inferior hypogastric plexuses – Postganglionic axons go to abdominal and pelvic effectors o Effects include: smooth muscle contraction, increased secretions in urinary and digestive systems; penile, clitoral erection 22
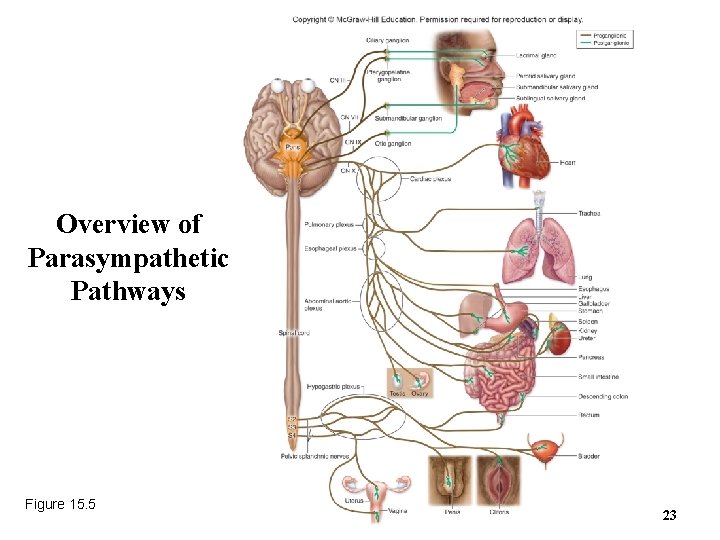
Overview of Parasympathetic Pathways Figure 15. 5 23

What did you learn? • Which ganglion innervates nasal glands and tear glands (and would be overactive in hay fever sufferers)? • What happens to heart rate when the vagus nerve fires more action potentials? • Which part of the spinal cord contains cell bodies of parasympathetic preganglionic neurons? Copyright © 2016 Mc. Graw-Hill Education. All rights reserved. No reproduction or distribution without the prior written consent of Mc. Graw-Hill Education 24

15. 4 Sympathetic Division • Sympathetic function: exercise and emergency • Thoracolumbar anatomical origin • Ganglia are close to CNS, but anatomical pathways are complex 25

15. 4 a Organization and Anatomy of the Sympathetic Division • Sympathetic preganglionic neurons – Cell bodies housed in lateral horn of T 1–L 2 – Myelinated axons course through anterior roots of T 1–L 2 spinal nerves, then branch off • Sympathetic trunks and ganglia – Left and right trunks just lateral to the vertebral column – Trunk resembles a pearl necklace o “String” composed of axons o “Pearls” composed of sympathetic trunk ganglia housing cell bodies 26

15. 4 a Organization and Anatomy of the Sympathetic Division • Sympathetic trunks and ganglia (continued ) – Generally one ganglion associated with each spinal nerve – But cervical portion of trunk has only three ganglia: superior, middle, inferior o Superior cervical ganglion cells have postganglionic axons going to head, neck, thoracic viscera – Targets include: sweat glands, blood vessels, dilator pupillae muscle of eye, superior tarsal muscle of eyelid o Middle and inferior cervical ganglion cells have postganglionic axons that innervate thoracic viscera* 27
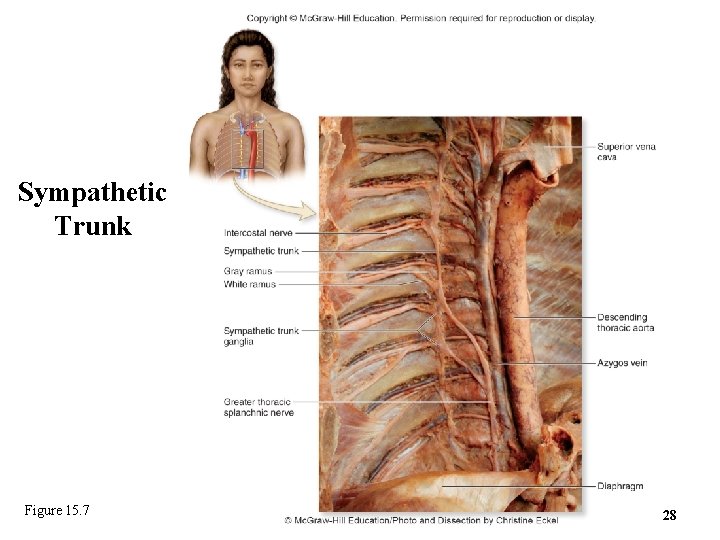
Sympathetic Trunk Figure 15. 7 28

15. 4 a Organization and Anatomy of the Sympathetic Division • White and gray rami – Connect spinal nerves to sympathetic trunk Ø White rami communicantes o Carry myelinated preganglionic sympathetic axons from T 1–L 2 nerves to trunk o “Entrance ramps” to trunk Ø Gray rami communicantes o Carry unmyelinated postganglionic sympathetic axons from trunk to all spinal nerves o “Exit ramps” from trunk 29

15. 4 a Organization and Anatomy of the Sympathetic Division • Sympathetic splanchnic nerves – Preganglionic sympathetic axons not synapsing in sympathetic trunk – Run anteriorly from sympathetic trunk, typically terminate in prevertebral ganglia o Prevertebral ganglia – Located anterior to vertebral column on surface of aorta; within abdominopelvic cavity – Include celiac, superior mesenteric, and inferior mesenteric ganglia 30
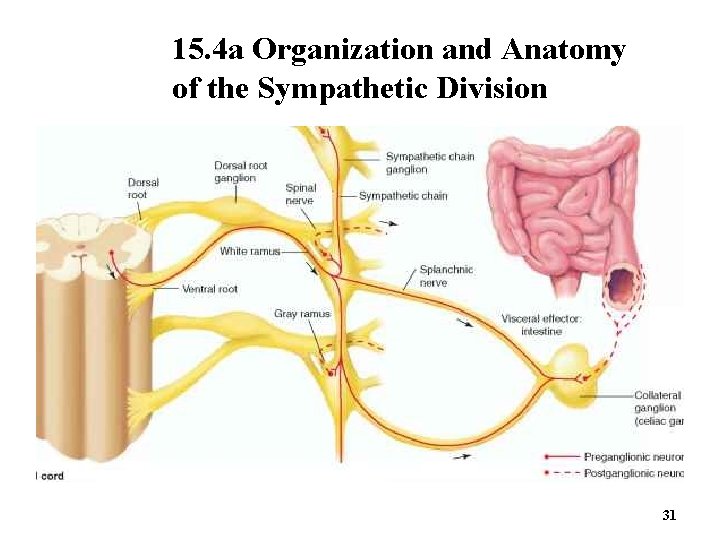
15. 4 a Organization and Anatomy of the Sympathetic Division 31

15. 4 a Organization and Anatomy of the Sympathetic Division o Prevertebral ganglia (continued ) – Celiac ganglia are adjacent to celiac artery o Greater thoracic splanchnic nerves enter o Postganglionic axons innervate stomach, duodenum, spleen, liver, gallbladder, pancreas – Superior mesenteric ganglia are adjacent to superior mesenteric artery o Lesser and least thoracic splanchnic nerves enter o Postganglionic axons innervate small intestine, large intestine, pancreas, kidneys, ureters 32

15. 4 a Organization and Anatomy of the Sympathetic Division • Prevertebral ganglia (continued ) – Inferior mesenteric ganglia are adjacent to inferior mesenteric artery o Lumbar splanchnic nerves enter o Postganglionic axons innervate large intestine, rectum, bladder, ureters, reproductive organs 33
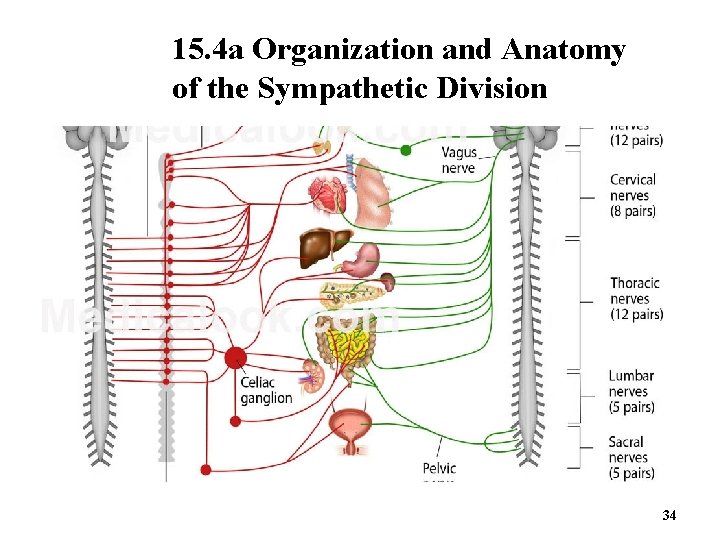
15. 4 a Organization and Anatomy of the Sympathetic Division 34

Clinical View: Horner Syndrome • Injury of cervical sympathetic trunk or T 1 trunk ganglion • Ptosis – Drooping of superior eyelid due to paralysis of superior tarsal muscle • Miosis – Constricted pupil due to paralysis of pupil dilator muscle • Anhydrosis – Lack of sweating because sweat glands not receiving sympathetic innervation • Facial flushing – Due to lack of sympathetic innervation, vasodilation results 35

15. 4 b Sympathetic Pathways • Axons exit the sympathetic trunk by one of four pathways – – Spinal nerve pathway Postganglionic sympathetic pathway Splanchnic nerve pathway Adrenal medulla pathway 36

15. 4 b Sympathetic Pathways • Spinal nerve pathway – For skin effectors (e. g. , sweat glands) of neck, torso and limbs – Preganglionic neuron enters sympathetic trunk ganglion and synapses with ganglionic neuron – Postganglionic axon travels through gray ramus at same spinal level as ganglion, joins that level’s spinal nerve and extends to effector 37
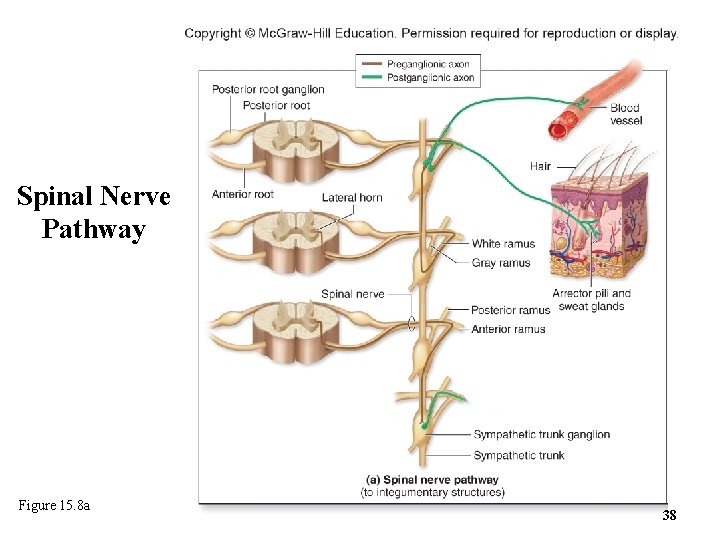
Spinal Nerve Pathway Figure 15. 8 a 38

15. 4 b Sympathetic Pathways • Postganglionic sympathetic nerve pathway – For effectors that are internal organs of thorax and neck (e. g. , heart and esophagus); skin effectors of head and neck; eyelid and dilator pupillae muscles – Preganglionic neuron enters and synapses in sympathetic trunk ganglion – Postganglionic axon goes directly from trunk ganglion to effector o Does not leave trunk via grey ramus 39
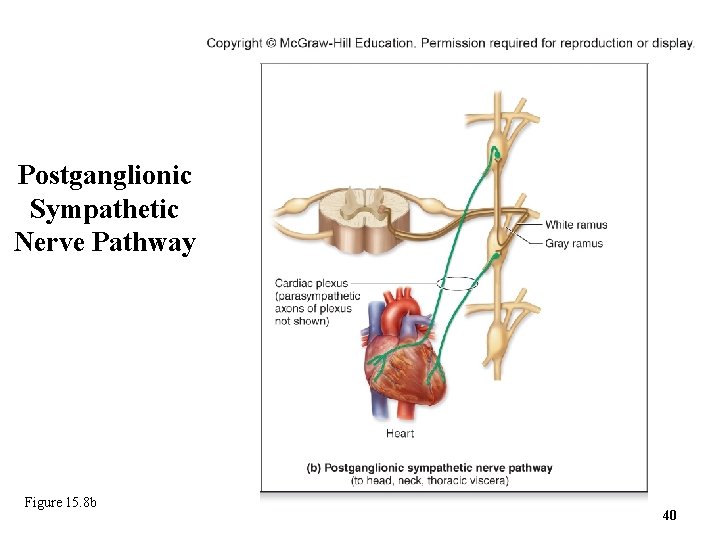
Postganglionic Sympathetic Nerve Pathway Figure 15. 8 b 40

15. 4 b Sympathetic Pathways • Splanchnic nerve pathway – For effectors in abdominal and pelvic viscera – Preganglionic axons pass sympathetic trunk without synapsing o Axons travel in splanchnic nerves to prevertebral ganglia where they make synapses – Postganglionic axons innervate effectors 41
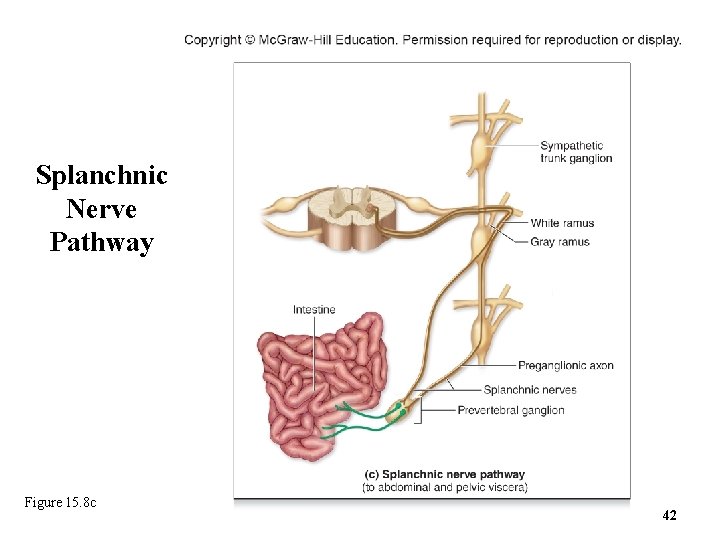
Splanchnic Nerve Pathway Figure 15. 8 c 42

15. 4 b Sympathetic Pathways • Adrenal medulla pathway – For central region of adrenal gland (its medulla) – Preganglionic sympathetic axons extend through sympathetic trunk and prevertebral ganglia without synapsing in either – Preganglionic cells stimulate adrenal medulla cells to release epinephrine and norepinephrine into the blood o These hormones potentiate and prolong the fight-or-flight response 43
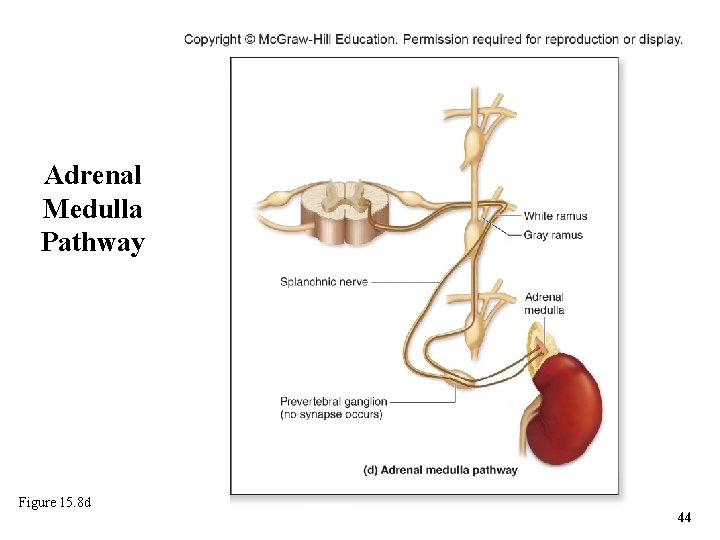
Adrenal Medulla Pathway Figure 15. 8 d 44
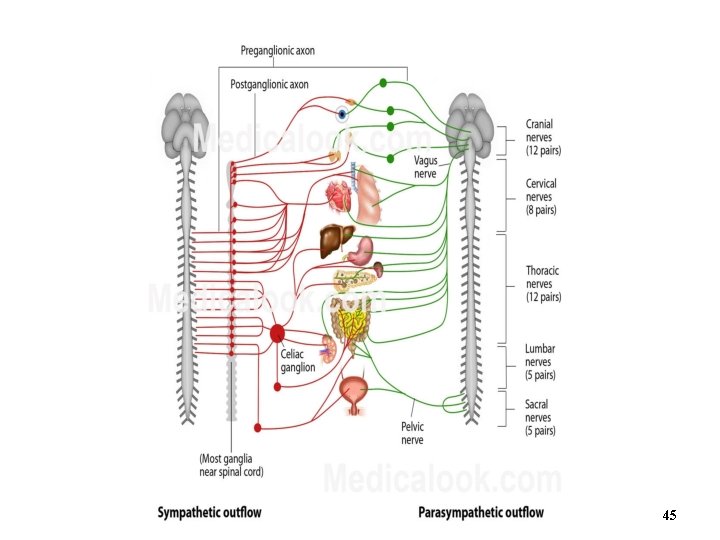
45

What did you learn? • Where are the cell bodies of sympathetic preganglionic neurons? • Do the white rami contain preganglionic or postganglionic axons? • Where are the target organs for the splanchnic nerve pathway? 46 Copyright © 2016 Mc. Graw-Hill Education. All rights reserved. No reproduction or distribution without the prior written consent of Mc. Graw-Hill Education

15. 5 a Overview of ANS Neurotransmitters • ANS uses acetylcholine (ACh) and norepinephrine (NE) • Either transmitter can cause stimulation or inhibition, depending on the postsynaptic receptor • Cells that release ACh are cholinergic neurons – Cholinergic neurons include o All ANS preganglionic neurons o All parasympathetic ganglionic neurons o Sympathetic ganglionic neurons innervating sweat glands and blood vessels in skeletal muscle – Target cells have cholinergic receptors 47

15. 5 a Overview of ANS Neurotransmitters • Cells that release norepinephrine (NE) are adrenergic neurons – Most sympathetic ganglionic neurons are adrenergic – Target cells have adrenergic receptors 48

Comparison of Neurotransmitters in the Autonomic Nervous System Figure 15. 9 49
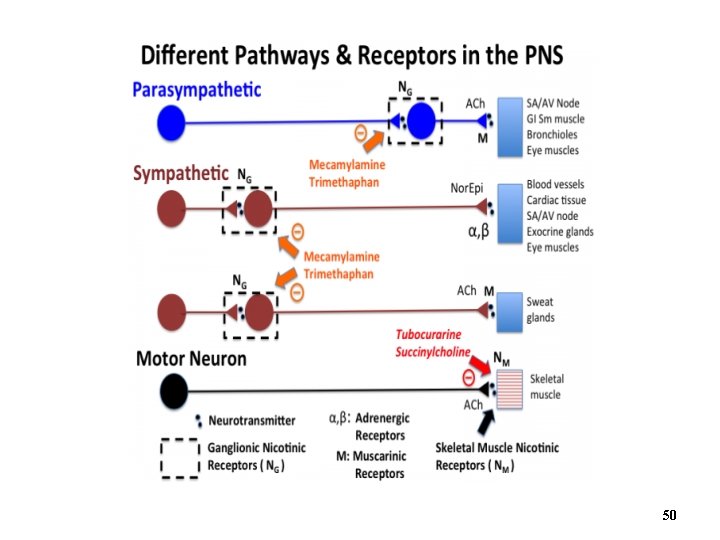
50

15. 5 b Cholinergic Receptors • Two main types of cholinergic receptors: nicotinic and muscarinic • Nicotinic receptors (sensitive to nicotine) – Found on all ganglionic neurons and adrenal medulla cells o Also on skeletal muscle cells at neuromuscular junction – When ACh binds nicotinic receptor it opens cation channel o Na+ moves into cell (a lesser amount of K+ moves out of cell) o Cell depolarizes: excitatory postsynaptic potential produced – Subtypes of nicotinic receptors o E. g. , receptors at neuromuscular junction are blocked by curare but receptors on ganglionic neurons are not 51

15. 5 b Cholinergic Receptors • Muscarinic receptors (sensitive to muscarine toxin) – Found in all target organs of parasympathetic division and a few of sympathetic division o Sympathetic effectors with muscarinic receptors include sweat glands and blood vessels in skeletal muscle – All muscarinic receptors use second messengers, but different subtypes of receptor have different effects o When ACh binds to muscarinic receptors of smooth muscle in GI tract it is stimulated to contract more o When ACh binds to muscarinic receptors on cardiac muscle the heart rate decreases 52

15. 5 c Adrenergic Receptors • NE is a catecholamine – Catecholamines are a chemical subtype of biogenic monoamines o Ligands that bind to membrane receptors o Norepinephrine and epinephrine are both catecholamines that bind to adrenergic receptors • Two main types of adrenergic receptors are alpha (α) and beta (β) receptors – Cells with α receptors are typically stimulated by NE – Cells with β receptors may be stimulated or inhibited by NE 53

15. 5 c Adrenergic Receptors • Alpha receptors – α 1 receptors o Stimulatory receptors found on most smooth muscle cells o Located in most blood vessels (vasoconstriction); arrector pili muscle (goose bumps), uterus (contraction), ureters, internal urethral sphincter (closing), dilator pupillae (pupil dilation) – α 2 receptors o Located throughout CNS, in pancreas (inhibit insulin secretion), GI tract sphincters (constriction) 54

15. 5 c Adrenergic Receptors • Beta receptors – β 1 receptors o Primarily stimulatory o Located in heart (increase heart rate and force) and in kidney (stimulate renin secretion) – β 2 receptors o Primarily inhibitory o Located in smooth muscle of vessels to heart, liver, and skeletal muscle (cause vessel dilation); lung (bronchodilation); uterine and GI tract smooth muscle (relaxation); detrusor muscle of bladder (relaxation) – β 3 receptors o May be stimulatory (or inhibitory) o Located in adipose (triglyceride breakdown for fuel); urinary bladder smooth muscle (relaxation) 55
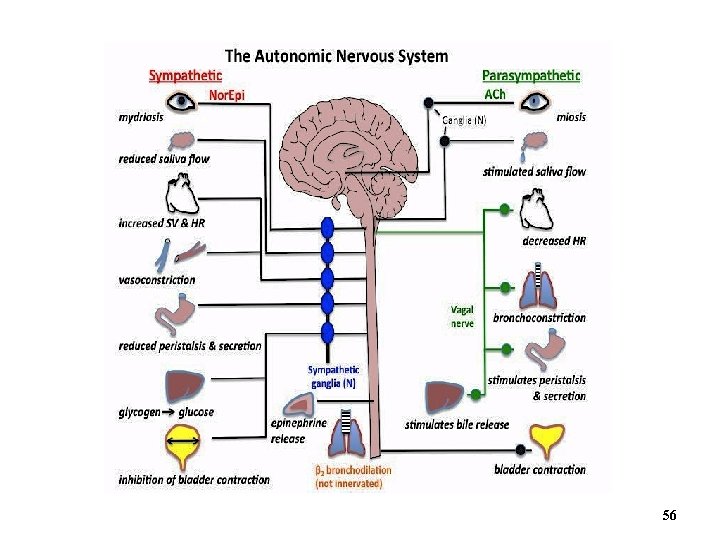
56

Clinical View: Epinephrine for Treatment of Asthma • Asthma attacks narrow the bronchioles • Bronchioles contain β 2 receptors • Epinephrine binds to β 2 receptors more effectively than does norepinephrine • Epinephrine is used to treat asthma attack as it is a more potent relaxant of smooth muscles in bronchioles (more dilation) 57

What did you learn? • What neurotransmitter is released by preganglionic neurons of both ANS divisions? • Activation of which type of cholinergic receptor causes the heart to slow down? • Activation of which type of adrenergic receptor causes the heart to speed up? Copyright © 2016 Mc. Graw-Hill Education. All rights reserved. No reproduction or distribution without the prior written consent of Mc. Graw-Hill Education 58

15. 6 Interactions Between the Parasympathetic and Sympathetic Divisions Learning Objectives: Discuss the nature of autonomic tone and its effects. 2. Explain what is meant by dual innervation. 3. Describe the antagonistic and cooperative effects of dual innervation. 4. Describe the systems innervated only by the sympathetic division and how they function. 1. Copyright © 2016 Mc. Graw-Hill Education. All rights reserved. No reproduction or distribution without the prior written consent of Mc. Graw-Hill Education 59

15. 6 a Autonomic Tone • Most effectors are innervated by both divisions of ANS • Both continuously release neurotransmitter – Generate autonomic tone • In some instances, only one division controls the status of an effector – E. g. , blood vessels usually in a partially constricted state due to sympathetic tone o Vessel constricts if sympathetic activity increases; vessel dilates if sympathetic activity decreases 60

15. 6 b Dual Innervation • Dual innervation: organ receives input from both the sympathetic and parasympathetic divisions – Two divisions may have antagonistic or cooperative effects ü Antagonistic effects – Commonly the two divisions oppose each other – Parasympathetic activity slows heart rate; sympathetic activity increases heart rate o Cardiac cells have both cholinergic and adrenergic receptors 61

15. 6 b Dual Innervation • Antagonistic effects (continued ) – Parasympathetic activity increases GI tract motility; sympathetic activity decreases motility o GI smooth muscle cells have both types of receptors – Parasympathetic activity decreases pupil diameter; sympathetic activity dilates pupil o Parasympathetic fibers innervate circular iris muscles; sympathetic fibers innervate radial iris muscles 62

15. 6 b Dual Innervation ü Cooperative effects – Seen when parasympathetic and sympathetic stimulation have different effects that are part of an overall (same) response – E. g. , male sexual function o Penis erection due to parasympathetic activity o Ejaculation due to sympathetic activity 63

15. 6 c Systems Controlled Only by the Sympathetic Division • Opposing effects can be achieved without dual innervation – Blood vessels constrict with increased sympathetic activity; they dilate with decreased sympathetic activity • Examples of effectors innervated only* by the sympathetic division – Sweat glands in the trunk – Arrector pili muscles in the skin – Adrenal medulla neurosecretory cells 64

Clinical View: Raynaud Syndrome • • • Sudden constriction of small arteries of digits Results in loss of normal hue of distal skin Accompanied by pain Triggered by cold or emotional stress Due to exaggerated local sympathetic response More common in women+++ 65
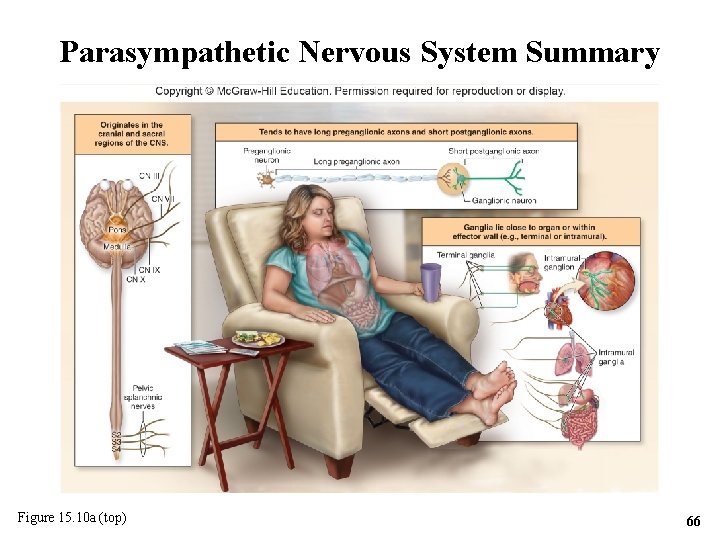
Parasympathetic Nervous System Summary Figure 15. 10 a (top) 66
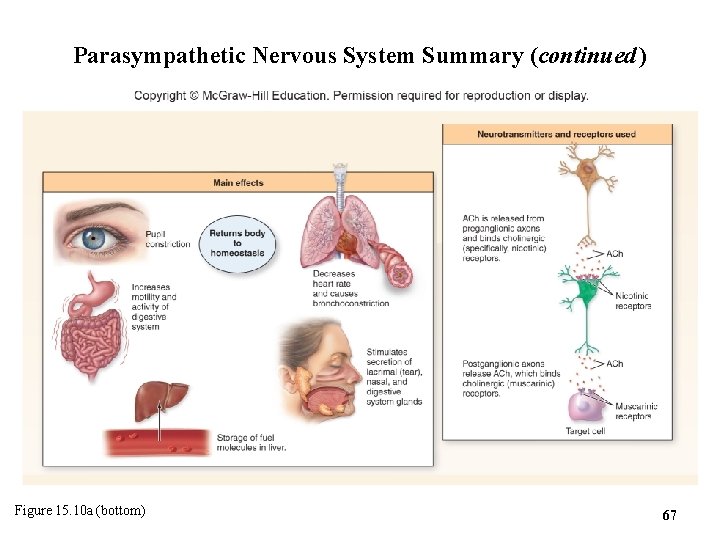
Parasympathetic Nervous System Summary (continued ) Figure 15. 10 a (bottom) 67
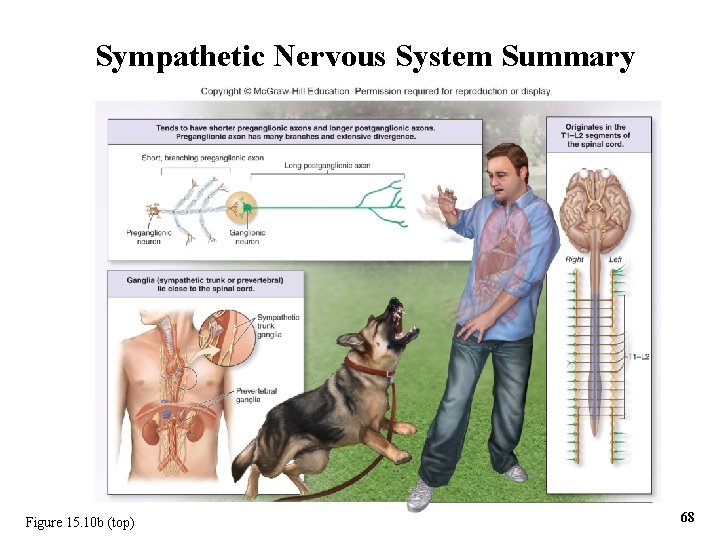
Sympathetic Nervous System Summary Figure 15. 10 b (top) 68
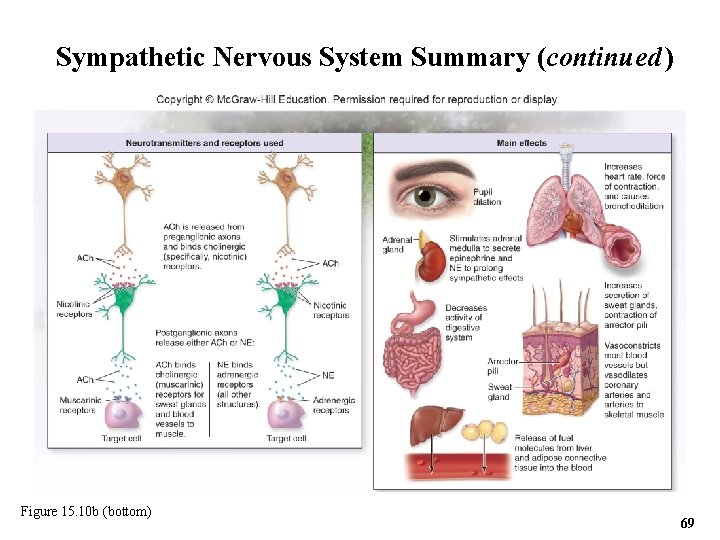
Sympathetic Nervous System Summary (continued ) Figure 15. 10 b (bottom) 69

What did you learn? • How do the sympathetic and parasympathetic divisions influence GI tract motility? • How does autonomic activity regulate blood vessel diameter? Copyright © 2016 Mc. Graw-Hill Education. All rights reserved. No reproduction or distribution without the prior written consent of Mc. Graw-Hill Education 70

What did you learn? • How do the sympathetic and parasympathetic divisions influence GI tract motility? • How does autonomic activity regulate blood vessel diameter? Copyright © 2016 Mc. Graw-Hill Education. All rights reserved. No reproduction or distribution without the prior written consent of Mc. Graw-Hill Education 71

15. 7 a Autonomic Plexuses • Autonomic plexuses: networks of nerves within thoracic and abdominopelvic cavities – Contain sympathetic postganglionic axons, parasympathetic preganglionic axons, and some visceral sensory axons v. Cardiac plexus o Includes sympathetic axons from cervical and thoracic trunk (quicken heart rate) and parasympathetic axons from vagus nerve (slow the heart) v. Pulmonary plexus o Includes sympathetic axons from cervical and thoracic trunk (bronchodilation) and parasympathetic axons from vagus nerve (bronchoconstriction) 72

15. 7 a Autonomic Plexuses • Autonomic plexuses (continued ) v. Esophageal plexus o Includes sympathetic axons from cervical and thoracic trunk (decrease motility) and parasympathetic axons from vagus nerve (coordinate opening of cardiac sphincter with swallowing) v. Abdominal aortic plexus o Consists of celiac (solar) plexus, superior mesenteric plexus, and inferior mesenteric plexus – Sympathetic postganglionic axons from prevertebral ganglia – Parasympathetic preganglionic axons from vagus or pelvic splanchnic nerves o Innervates all abdominal and some pelvic organs 73

15. 7 a Autonomic Plexuses • Autonomic plexuses (continued ) v. Hypogastric plexus o Consists of sympathetic axons from aortic plexus and sympathetic trunk, parasympathetic axons from pelvic splanchnic nerves o Innervates viscera within pelvic region 74
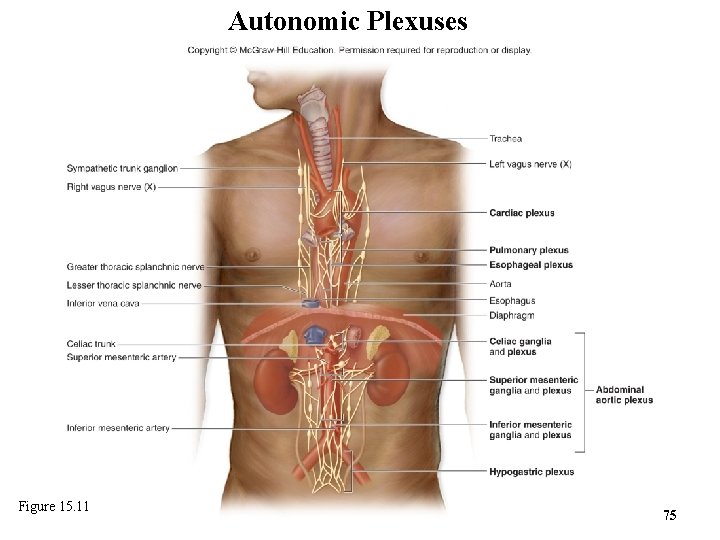
Autonomic Plexuses Figure 15. 11 75

15. 7 b Autonomic Reflexes • Autonomic reflexes (visceral reflexes) – Pre-programmed response to a stimulus generated by a reflex arc o Arc includes: receptor, sensory relay to CNS, CNS integration center, motor neuron, effector o ANS effectors are cardiac muscle, smooth muscle, or glands 76
15. 7 b Autonomic Reflexes • Cardiovascular reflex (blood pressure) – Stretch receptors in vessel walls respond to pressure elevation – Signals sent to cardiac center in medulla oblongata – Inhibit sympathetic and activate parasympathetic output to heart – Slow heart rate, decrease volume of blood ejected o Decrease blood pressure 77

15. 7 b Autonomic Reflexes • Gastrointestinal reflex (defecation) – Sensory neurons in rectum respond to stretch by fecal matter – Signals sent to spinal cord – Signals sent through motor neurons stimulate rectum to contract and internal anal sphincter to relax 78

15. 7 b Autonomic Reflexes • Micturition reflex (urination) – Stretch receptors signal when bladder fills with urine – Signals sent to sacral spinal cord – In infant this results in reflexive contraction of smooth muscles in bladder and relaxation of urinary sphincters o Once toilet trained, signals through the pons allow for voluntary control of the external urethral sphincter 79
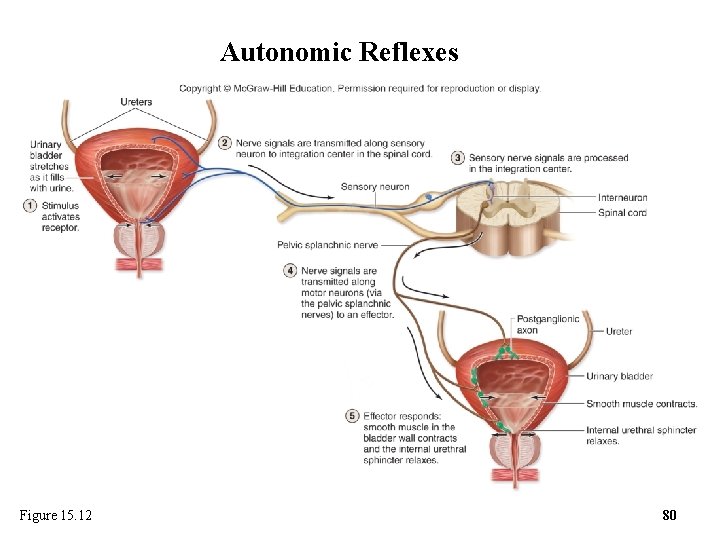
Autonomic Reflexes Figure 15. 12 80

Clinical View: Autonomic Dysreflexia • Causes blood pressure to rise profoundly • Stimulates a sympathetic reflex – Causes systemic vasoconstriction and large increase in blood pressure • Caused by hyperactivity of ANS after a spinal cord injury • Initial response to injury is spinal shock, with loss of autonomic reflexes • Abnormal response to lack of innervation, denervation hypersensitivity – E. g. , involuntary relaxation of internal urethral sphincter due to spinal cord reflex 81

What did you learn? • What types of axons are found in the pulmonary plexus? • What types of effectors are parts of autonomic reflex arcs? • What is the stimulus for the micturition reflex? Copyright © 2016 Mc. Graw-Hill Education. All rights reserved. No reproduction or distribution without the prior written consent of Mc. Graw-Hill Education 82
- Slides: 82