Chapter 14 Immune Response in Space and Time
















- Slides: 26

Chapter 14 Immune Response in Space and Time Dr. Capers IMMUNOLOGY

Kindt • Goldsby • Osborne Kuby IMMUNOLOGY Sixth Edition Chapter 13 Leukocyte Activation and Migration Copyright © 2007 by W. H. Freeman and Company

Invaders infect our bodies Cells of innate immune system arrive first Adaptive immune response provides longer protection Leukocytes are constantly monitoring for infection When detected, cells cross the blood barrier and travel to site of infection

Inflammatory response ○ Redness ○ Heat ○ Swelling ○ Pain Needs controlled migration of leukocyte populations

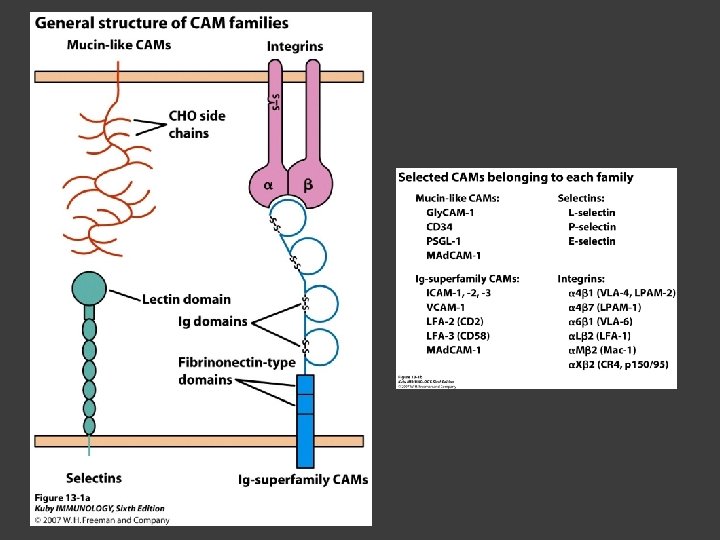
Our tissues are held together by molecular interactions ○ Cell adhesion molecules (CAMs) - Selectins, mucins, integrins, Ig-Superfamily CAMs (ICAMs) Can be used by leukocytes to interact with tissues For leukocytes to enter inflamed tissues, cells must adhere and pass between endothelial cells lining blood vessel - EXTRAVASATION Endothelial cells can express certain leukocyte specific CAMs


CAMs Selectins Membrane glycoproteins Bind to specific carbohydrate groups Interact with mucin-like molecules Example: ○ P-selectin is stored in granule in endothelial cell ○ Upon activation, granule fuses with membrane so that p-selectin is expressed

CAMs Mucins Serine and threonine-rich proteins Binding sites for selectins

CAMs Integrins Consist of α and β chains Bind cell surface molecules involved with cell to cell interactions Leukocyte adhesion deficiency ○ Autosomal recessive disease ○ Characterized by recurrent bacterial infections and slow healing

CAMs Ig-Superfamily CAMs (ICAMs) Immunoglobulin-like domains Bind to various integrin molecules

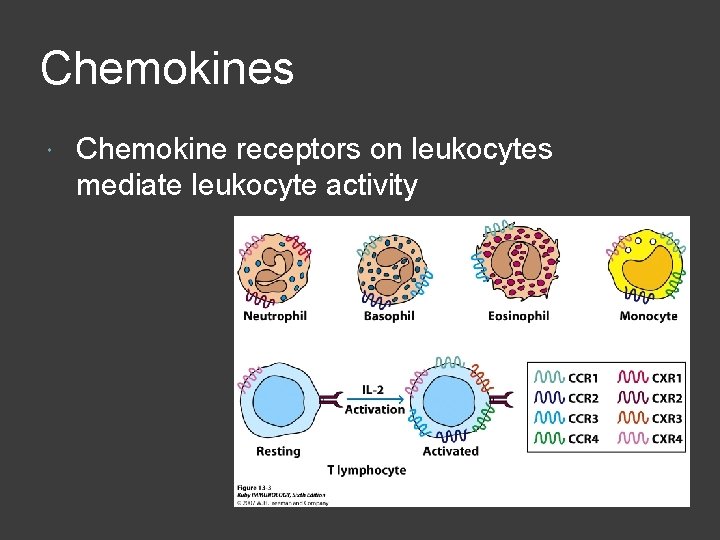
Chemokines Major regulators of leukocyte traffic ○ Cytokines that are responsible for movement of immune cells Small polypeptides Some involved in inflammation, some involved in homeostatic roles (“house keeping”) Induce adherence of leukocytes to endothelial lining

Chemokines Chemokine receptors on leukocytes mediate leukocyte activity

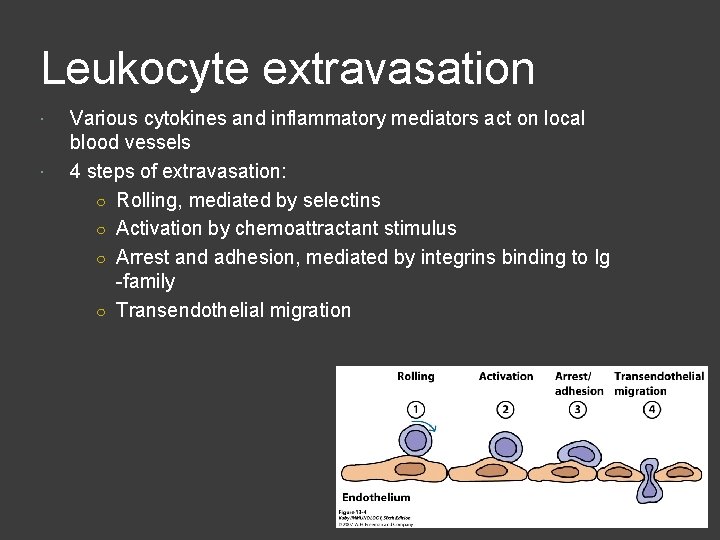
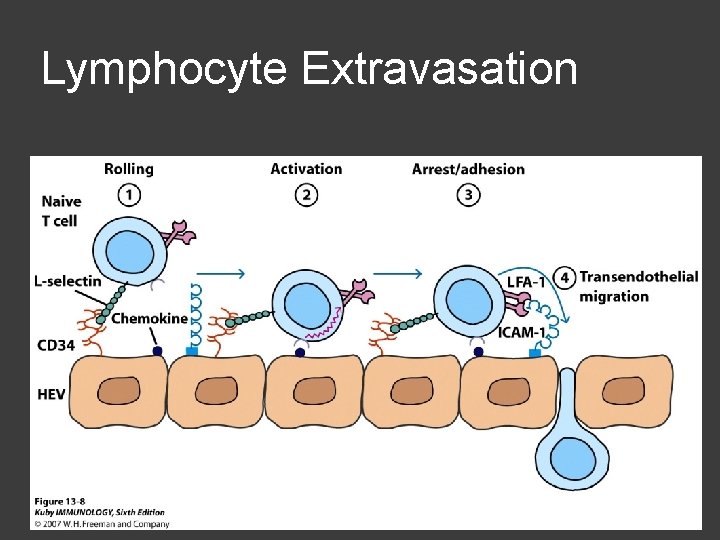
Leukocyte extravasation Various cytokines and inflammatory mediators act on local blood vessels 4 steps of extravasation: ○ Rolling, mediated by selectins ○ Activation by chemoattractant stimulus ○ Arrest and adhesion, mediated by integrins binding to Ig -family ○ Transendothelial migration


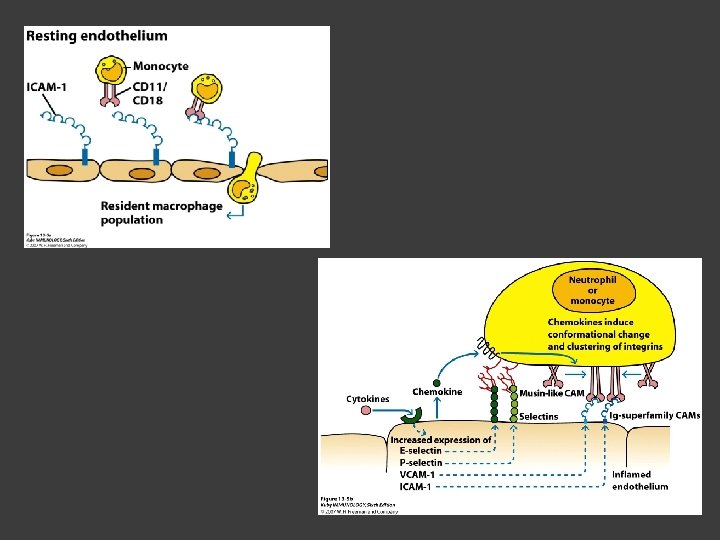
Extravasation Neutrophils are generally first Bind to endothelium when E-selectin and P- selectin are expressed by endothelium Monocytes Come in much later This is because it takes time for inflamed endothelial cells to express CAMs (such as ICAM-1 and VCAM-1)

Lymphocyte Recirculation ○ Unlike other leukocytes, lymphocytes recirculate continuously from blood to tissues to lymph (1 to 2 times a day) ○ Lymphocytes are antigenically committed ○ This recirculation increases chances of lymphocyte coming into contact with particular antigen

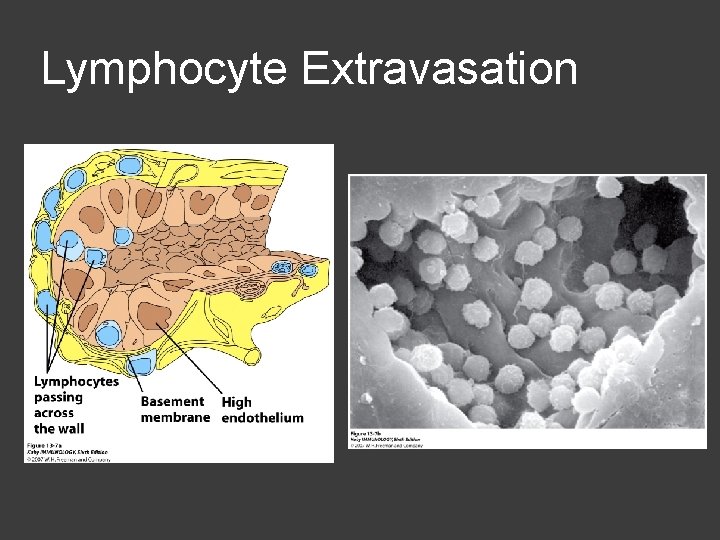
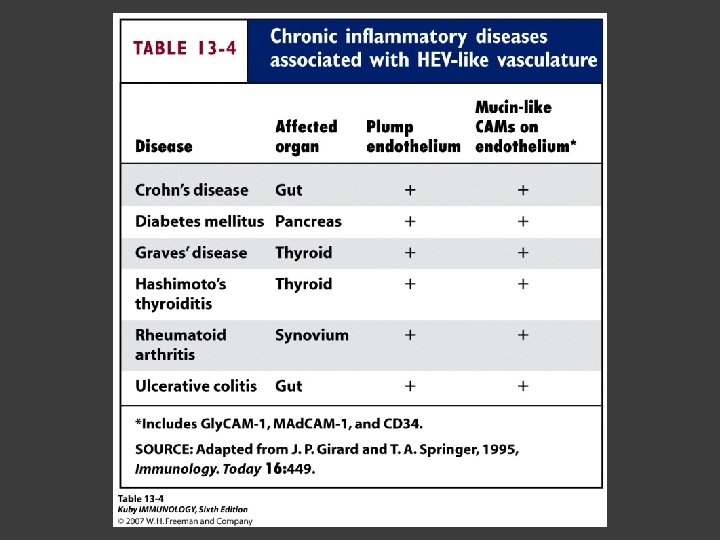
Lymphocyte Extravasation ○ Involves interaction of CAMs ○ Ensures proper populations of B and T cell make it into certain tissues ○ Capillaries Flattened endothelial cells HEVs – high endothelial venules - Areas of capillaries that have cells that are more cubodial in shape - Express variety of CAMs

Lymphocyte Extravasation

Lymphocyte Extravasation

Although lymphocyte extravasation is similar to neutrophils, different subsets of lymphocytes must make it into different tissues ○ Naïve lymphocytes Migrate to secondary lymphoid tissue to encounter antigen ○ Effector and memory lymphocytes Home to regions of infection Memory cells will tend to home to tissues in which they first encountered antigen

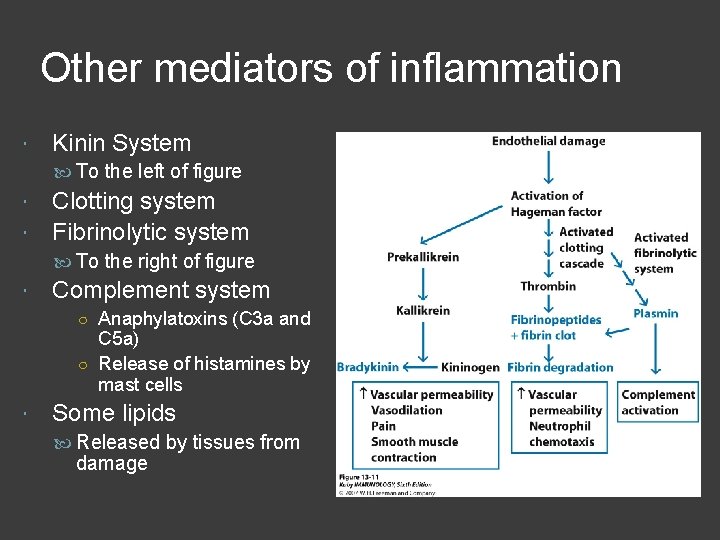
Other mediators of inflammation Kinin System To the left of figure Clotting system Fibrinolytic system To the right of figure Complement system ○ Anaphylatoxins (C 3 a and C 5 a) ○ Release of histamines by mast cells Some lipids Released by tissues from damage

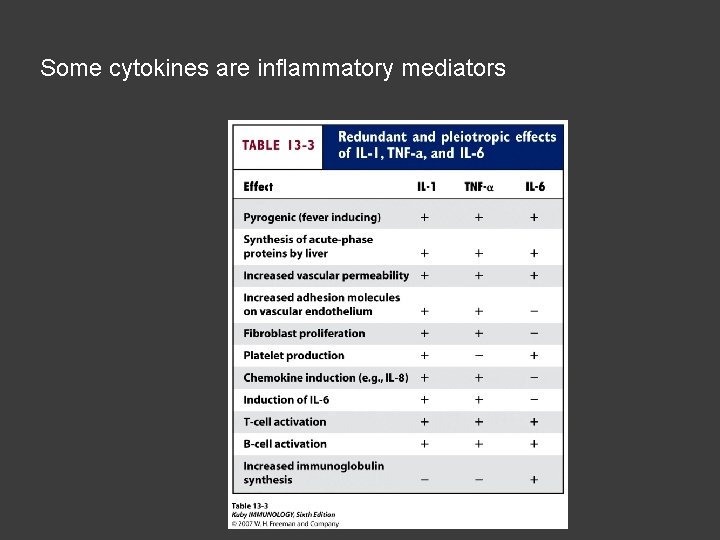
Some cytokines are inflammatory mediators

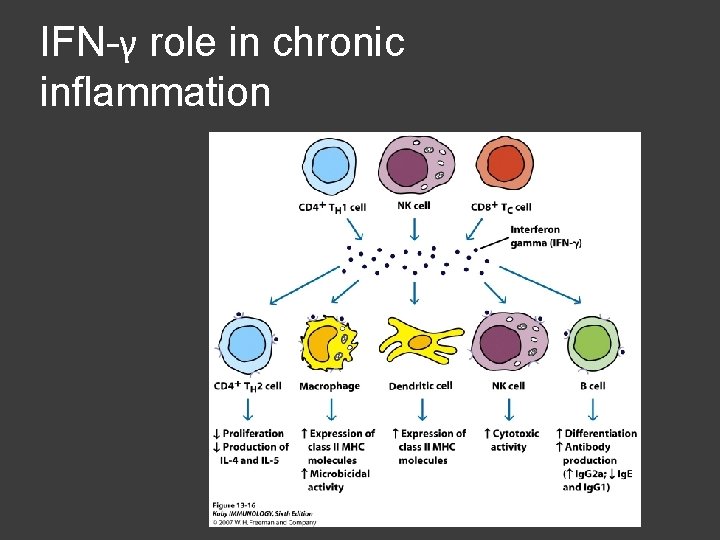
Inflammation response may be localized or systemic Localized Inflammatory Response ○ Duration and intensity must be carefully regulated to control tissue damage Systemic Acute Phase Response ○ Localized accompanied by acute phase response Induction of fever Increased production of WBCs IFN-γ and TNF-α involved in chronic inflammation Contributes to tissue wasting

IFN-γ role in chronic inflammation


Anti-Inflammatory Agents Antibody therapies can reduce leukocyte extravasation ○ Monoclonal Abs to CAMs Corticosteroids ○ Cholesterol derivatives ○ Decreases number of circulating lymphocytes ○ Reduces phagocytosis NSAIDs ○ Found in plants, aspirin ○ Pain and inflammation ○ Reduces prostaglandins, lowers vascular permeability