Chapter 14 Cardiovascular Physiology Heart Circulation Deoxygenated blood
Chapter 14 Cardiovascular Physiology
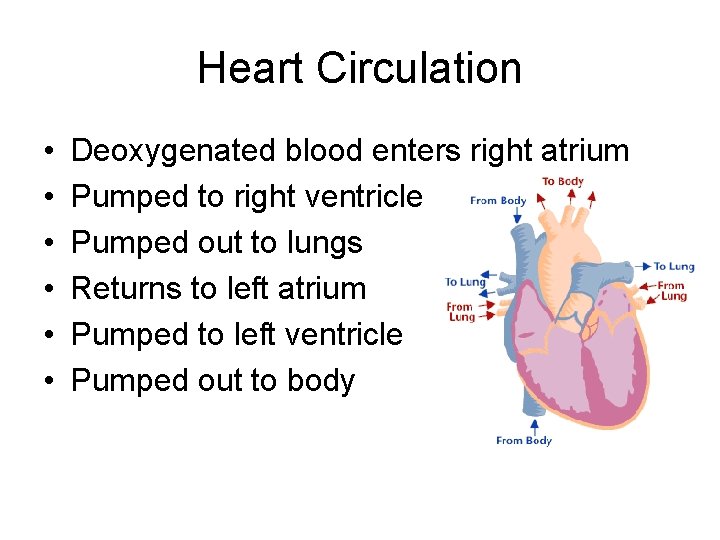
Heart Circulation • • • Deoxygenated blood enters right atrium Pumped to right ventricle Pumped out to lungs Returns to left atrium Pumped to left ventricle Pumped out to body
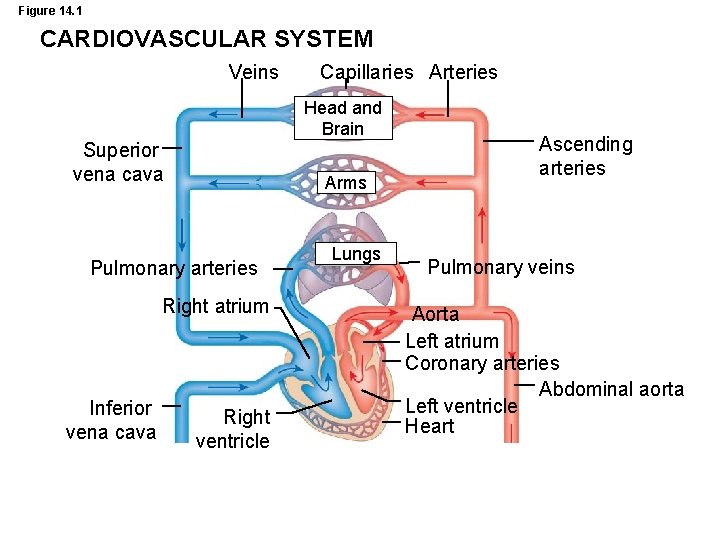
Figure 14. 1 CARDIOVASCULAR SYSTEM Veins Capillaries Arteries Head and Brain Superior vena cava Arms Pulmonary arteries Right atrium Inferior vena cava Right ventricle Lungs Ascending arteries Pulmonary veins Aorta Left atrium Coronary arteries Abdominal aorta Left ventricle Heart
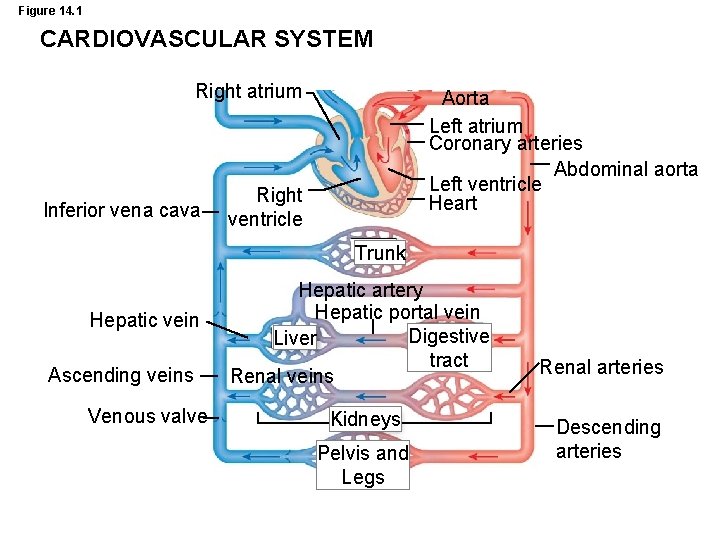
Figure 14. 1 CARDIOVASCULAR SYSTEM Right atrium Inferior vena cava Aorta Left atrium Coronary arteries Abdominal aorta Left ventricle Heart Right ventricle Trunk Hepatic vein Ascending veins Venous valve Hepatic artery Hepatic portal vein Digestive Liver tract Renal veins Kidneys Pelvis and Legs Renal arteries Descending arteries

Let’s think about fluid dynamics • What makes a better water gun: – wide/narrow barrel? – long/short barrel?

Concentration Gradients • Fluid flows down concentration gradients – Flows from area of high pressure to area of low pressure • Flow = ∆P (difference in pressure) – If the pressure is the same at both ends of the tube, no flow

Fluid Pressure • Fluid pressure is the force exerted by the fluid on its container – measured in mm Hg • Hydrostatic pressure is the pressure of a fluid that is not moving

Resistance • Resistance is tendency to oppose flow – related to tube diameter, length, and viscosity of fluid – narrow tubes exert more resistance on fluid because of friction

Resistance •

Flow •

Measuring Flow •

Measuring Flow • Flow rate = how much blood flows past a point • Velocity = how fast blood flows past a point
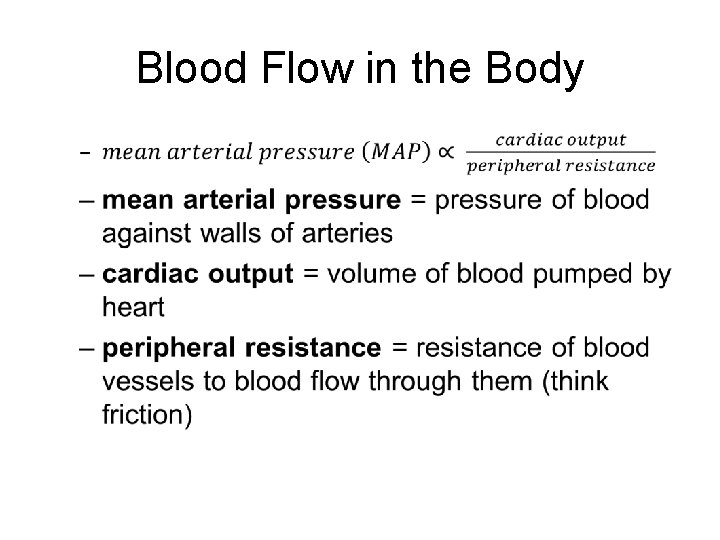
Blood Flow in the Body •
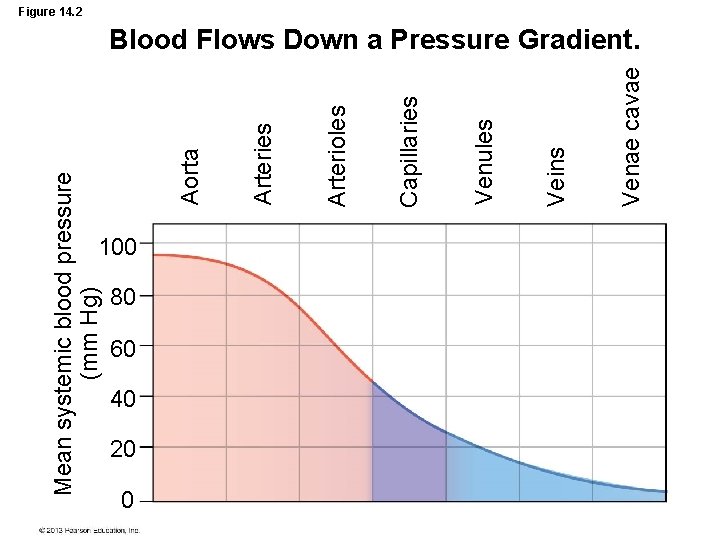
100 80 60 40 20 0 Venae cavae Veins Venules Capillaries Arterioles Arteries Aorta Mean systemic blood pressure (mm Hg) Figure 14. 2 Blood Flows Down a Pressure Gradient.

Cardiac Muscle • Cells smaller than skeletal muscles • Each cell has one nucleus • Connected by intercalated disks with gap junctions and desmosomes • Large t-tubules, smaller SR – cells rely on extracellular Ca 2+ • Lots of mitochondria
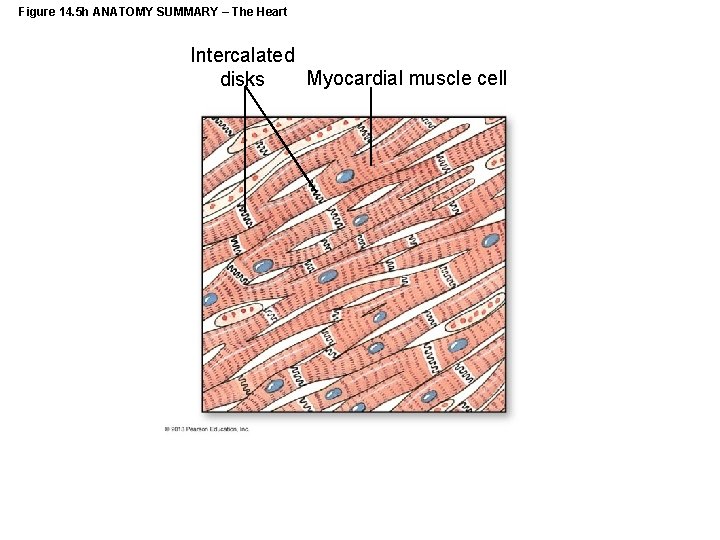
Figure 14. 5 h ANATOMY SUMMARY – The Heart Intercalated Myocardial muscle cell disks
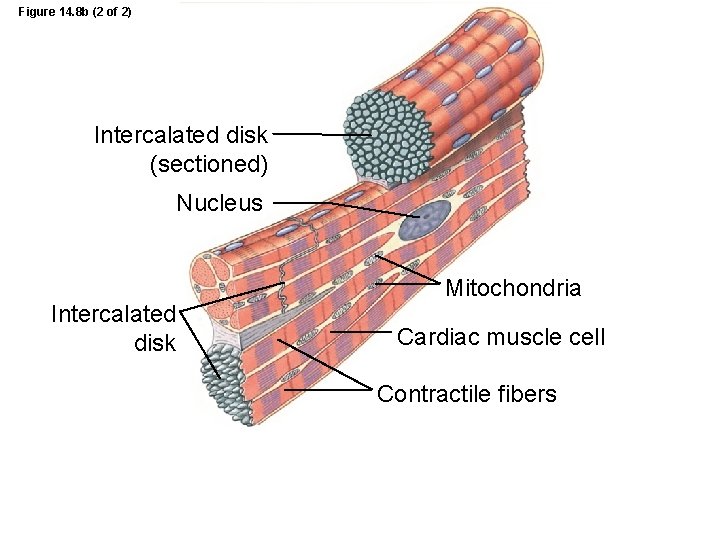
Figure 14. 8 b (2 of 2) Intercalated disk (sectioned) Nucleus Intercalated disk Mitochondria Cardiac muscle cell Contractile fibers
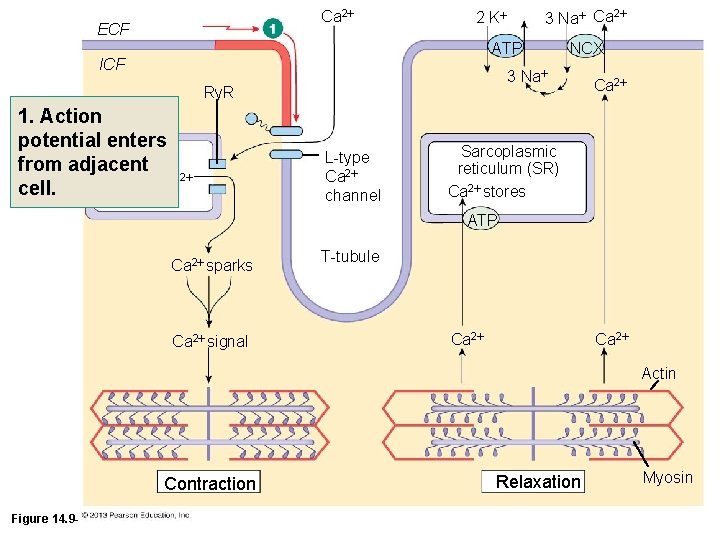
Ca 2 ECF 3 Na Ca 2 2 K ATP ICF 3 Na Ry. R 1. Action potential enters SR from adjacent Ca 2 cell. NCX L-type Ca 2 channel Ca 2 Sarcoplasmic reticulum (SR) Ca 2 stores ATP Ca 2 sparks Ca 2 signal T-tubule Ca 2 Actin Contraction Figure 14. 9 -1 (1 of 10) Relaxation Myosin
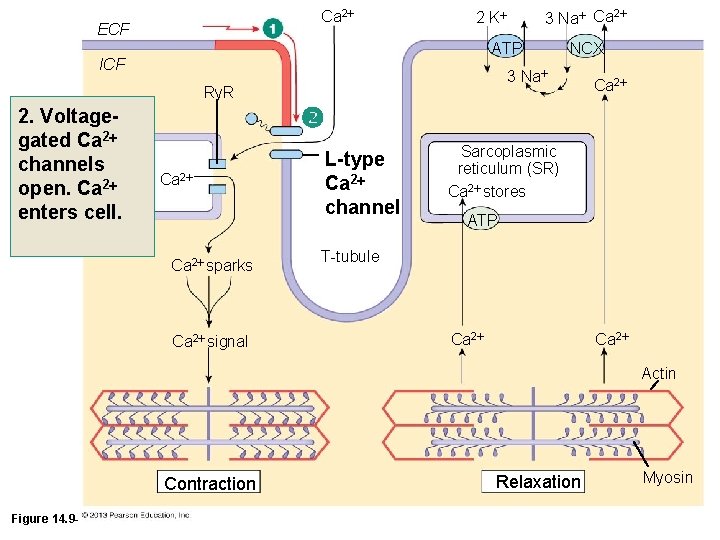
Ca 2 ECF ATP ICF NCX 3 Na Ry. R 2. Voltagegated Ca 2 SR channels open. Ca 2 enters cell. 3 Na Ca 2 2 K Ca 2 sparks Ca 2 signal L-type Ca 2 channel Sarcoplasmic reticulum (SR) Ca 2 stores ATP T-tubule Ca 2 Actin Contraction Figure 14. 9 -1 (1 of 10) Relaxation Myosin
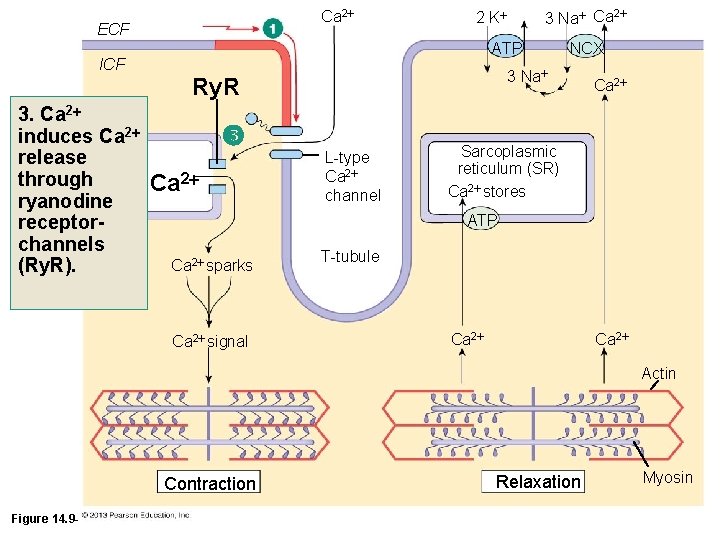
Ca 2 ECF ATP ICF Ca 2 NCX 3 Na Ry. R 3. Ca 2 induces Ca 2 release SR through ryanodine receptorchannels (Ry. R). 3 Na Ca 2 2 K L-type Ca 2 channel Ca 2 Sarcoplasmic reticulum (SR) Ca 2 stores ATP Ca 2 sparks Ca 2 signal T-tubule Ca 2 Actin Contraction Figure 14. 9 -1 (1 of 10) Relaxation Myosin
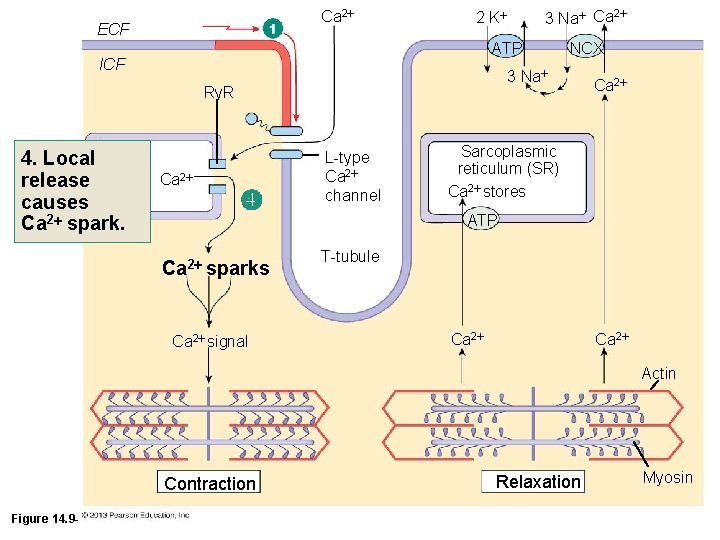
Ca 2 ECF ATP ICF Ca 2 NCX 3 Na Ry. R 4. Local SR release causes Ca 2 spark. 3 Na Ca 2 2 K Ca 2 sparks Ca 2 signal L-type Ca 2 channel Ca 2 Sarcoplasmic reticulum (SR) Ca 2 stores ATP T-tubule Ca 2 Actin Contraction Figure 14. 9 -1 (1 of 10) Relaxation Myosin
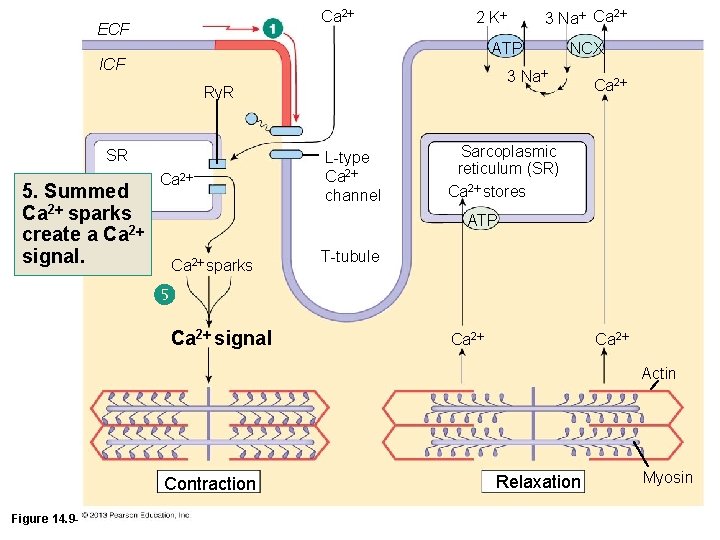
Ca 2 ECF ATP ICF SR Ca 2 NCX 3 Na Ry. R 5. Summed Ca 2 sparks create a Ca 2 signal. 3 Na Ca 2 2 K L-type Ca 2 channel Ca 2 Sarcoplasmic reticulum (SR) Ca 2 stores ATP Ca 2 sparks T-tubule Ca 2 signal Ca 2 Actin Contraction Figure 14. 9 -1 (1 of 10) Relaxation Myosin
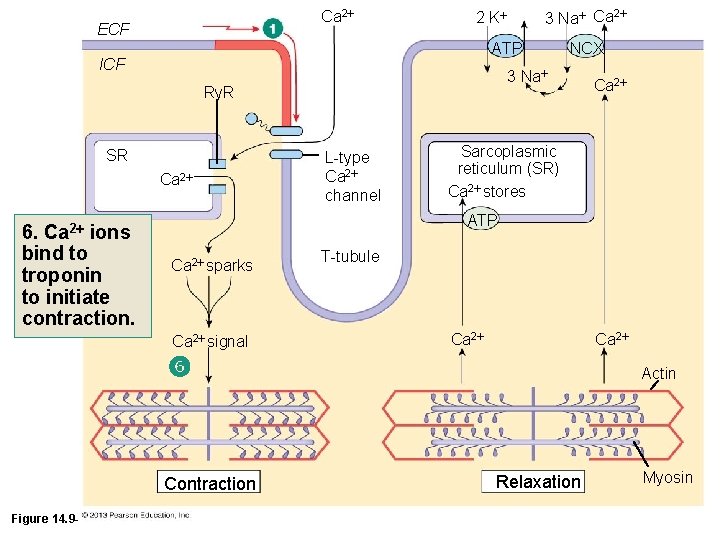
Ca 2 ECF ATP ICF SR Ca 2 NCX 3 Na Ry. R 6. Ca 2 ions bind to troponin to initiate contraction. 3 Na Ca 2 2 K L-type Ca 2 channel Sarcoplasmic reticulum (SR) Ca 2 stores ATP Ca 2 sparks Ca 2 signal T-tubule Ca 2 Contraction Figure 14. 9 -1 (1 of 10) Ca 2 Actin Relaxation Myosin
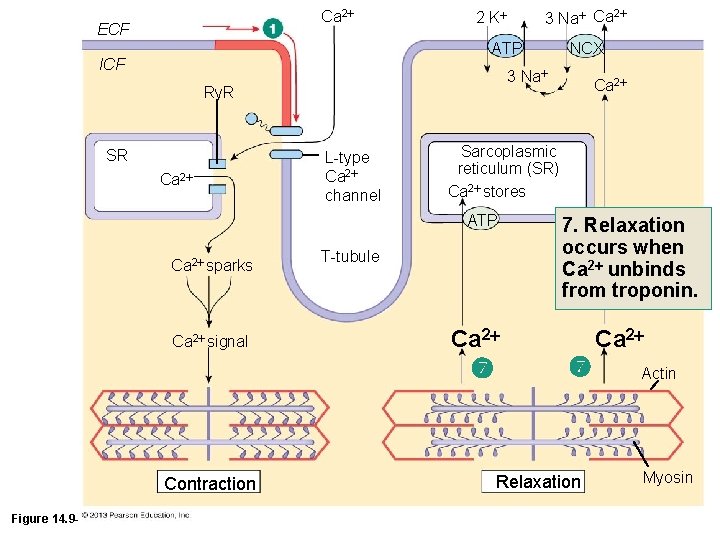
Ca 2 ECF ATP ICF SR Ca 2 L-type Ca 2 channel Ca 2 signal T-tubule Ca 2 Contraction Ca 2 Sarcoplasmic reticulum (SR) Ca 2 stores ATP Ca 2 sparks NCX 3 Na Ry. R Figure 14. 9 -1 (1 of 10) 3 Na Ca 2 2 K 7. Relaxation occurs when Ca 2 unbinds from troponin. Relaxation Ca 2 Actin Myosin
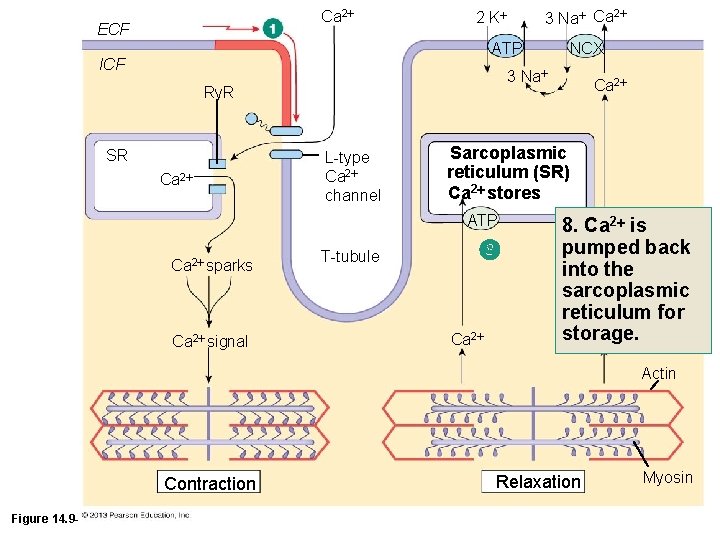
Ca 2 ECF 3 Na Ca 2 2 K ATP ICF 3 Na Ry. R SR Ca 2 L-type Ca 2 channel Ca 2 signal T-tubule Ca 2 Sarcoplasmic reticulum (SR) Ca 2 stores ATP Ca 2 sparks NCX Ca 2 8. Ca 2 is pumped back into the sarcoplasmic reticulum for storage. Ca 2 Actin Contraction Figure 14. 9 -1 (1 of 10) Relaxation Myosin
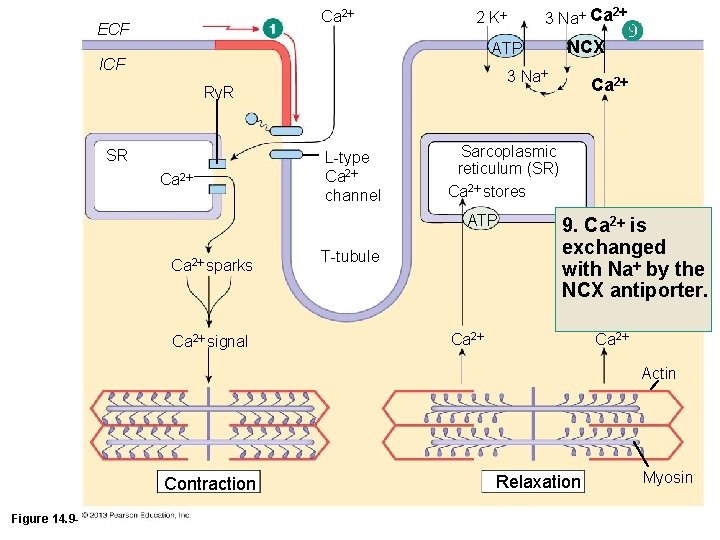
Ca 2 ECF 3 Na Ca 2 2 K ATP ICF 3 Na Ry. R SR Ca 2 L-type Ca 2 channel Ca 2 signal Ca 2 Sarcoplasmic reticulum (SR) Ca 2 stores ATP Ca 2 sparks NCX T-tubule 9. Ca 2 is exchanged with Na by the NCX antiporter. Ca 2 Actin Contraction Figure 14. 9 -1 (1 of 10) Relaxation Myosin
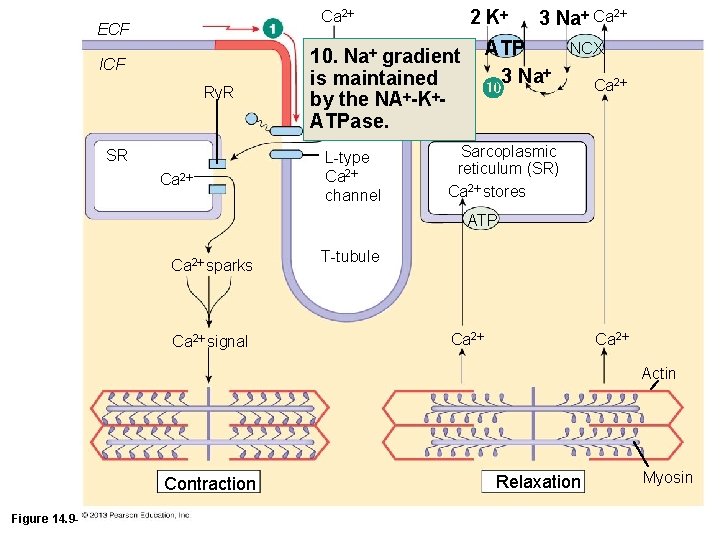
2 K Ca 2 ECF ICF Ry. R SR Ca 2 10. Na gradient is maintained by the NA -K ATPase. L-type Ca 2 channel 3 Na Ca 2 ATP 3 Na NCX Ca 2 Sarcoplasmic reticulum (SR) Ca 2 stores ATP Ca 2 sparks Ca 2 signal T-tubule Ca 2 Actin Contraction Figure 14. 9 -1 (1 of 10) Relaxation Myosin

Figure 14. 10 Membrane potential (m. V) ACTION POTENTIAL OF A CARDIAC CONTRACTILE CELL PNa 20 PX Permeability to ion X PK and PCa 0 20 PK and PCa 40 60 PNa 80 Phase*Membrane channels Na channels open Na channels close Ca 2 channels open; fast K channels close Ca 2 channels close; slow K channels open Resting potential *The phase numbers are a convention. 100 0 100 200 Time (msec) 300

Myocardial Action Potential • Longer than skeletal muscle action potential – prevents tetanus
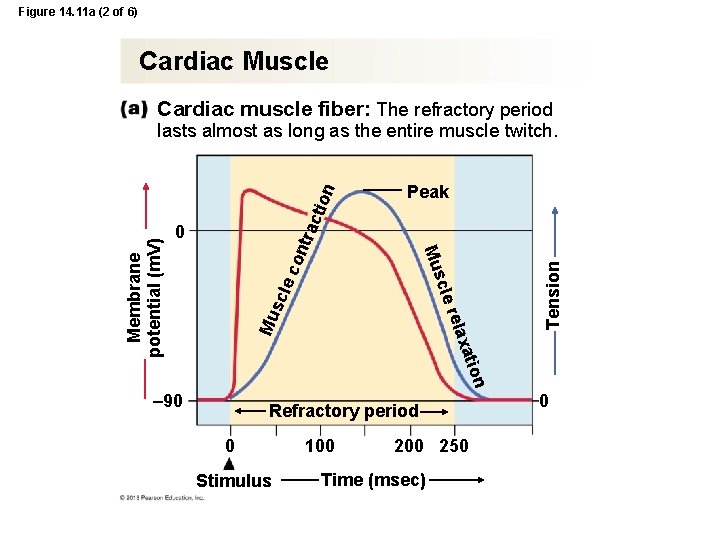
Figure 14. 11 a (2 of 6) Cardiac Muscle Cardiac muscle fiber: The refractory period on xati rela Mu scl cle ec 0 Tension ont rac t Peak Mus Membrane potential (m. V) ion lasts almost as long as the entire muscle twitch. 90 Refractory period 0 Stimulus 100 250 Time (msec) 0
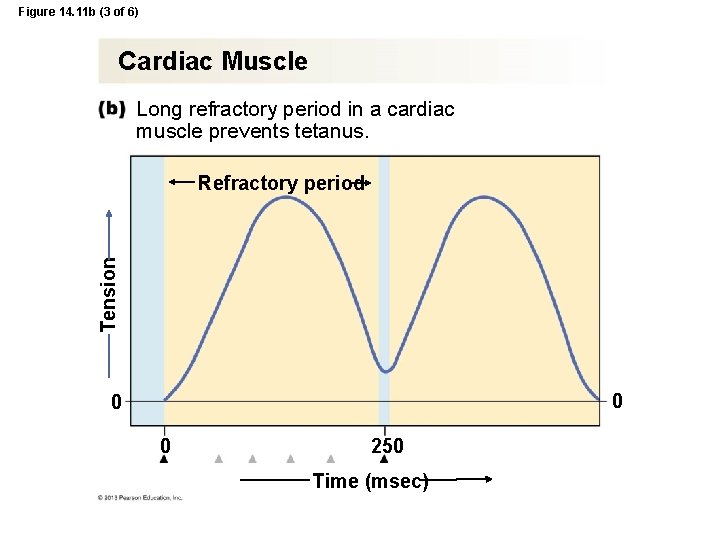
Figure 14. 11 b (3 of 6) Cardiac Muscle Long refractory period in a cardiac muscle prevents tetanus. Tension Refractory period 0 0 0 250 Time (msec)
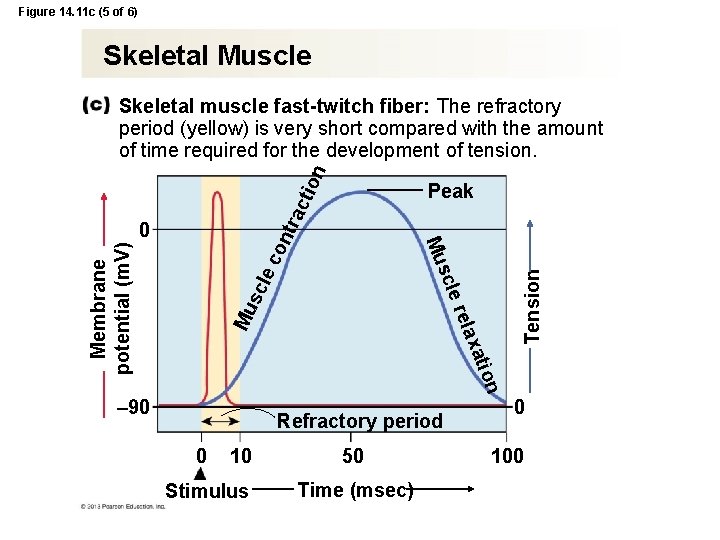
Figure 14. 11 c (5 of 6) Skeletal Muscle ion Skeletal muscle fast-twitch fiber: The refractory period (yellow) is very short compared with the amount of time required for the development of tension. xat ela Mu le r scl ec Membrane potential (m. V) sc Mu on tr 0 Tension act Peak ion 90 Refractory period 0 10 Stimulus 50 Time (msec) 0 100
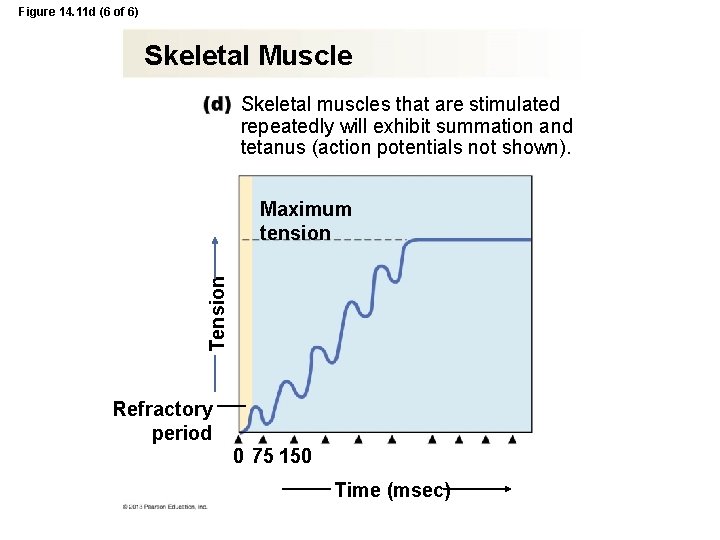
Figure 14. 11 d (6 of 6) Skeletal Muscle Skeletal muscles that are stimulated repeatedly will exhibit summation and tetanus (action potentials not shown). Tension Maximum tension Refractory period 0 75 150 Time (msec)

Cardiac Muscle • Most cardiac tissue is contractile • ~1% of myocardial cells generate action potentials spontaneously – autorhythmic cells, aka pacemakers

Myocardial Autorhythmic Cells • Unstable membrane potential = pacemaker potential – starts at -60 m. V – If channels permeable to K+ and Na+ open • close as membrane potential becomes more positive, Ca 2+ channels open – gradually drifts upward, never “rests”
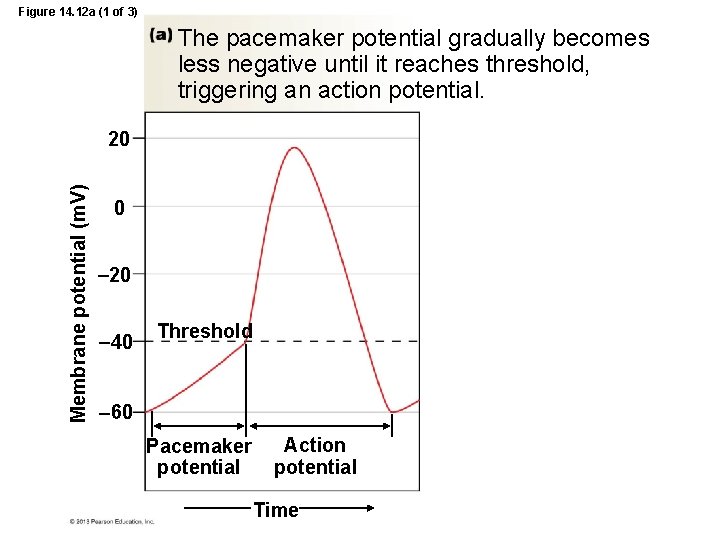
Figure 14. 12 a (1 of 3) The pacemaker potential gradually becomes less negative until it reaches threshold, triggering an action potential. Membrane potential (m. V) 20 0 20 40 Threshold 60 Pacemaker potential Action potential Time
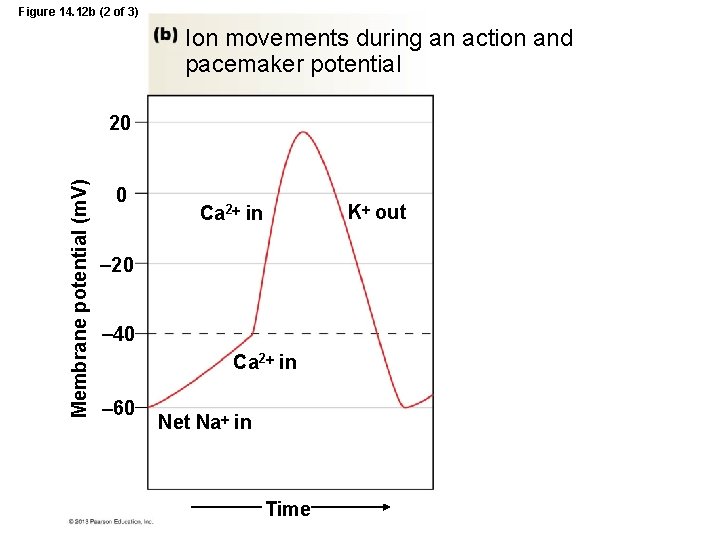
Figure 14. 12 b (2 of 3) Ion movements during an action and pacemaker potential Membrane potential (m. V) 20 0 K out Ca 2 in 20 40 Ca 2 in 60 Net Na in Time
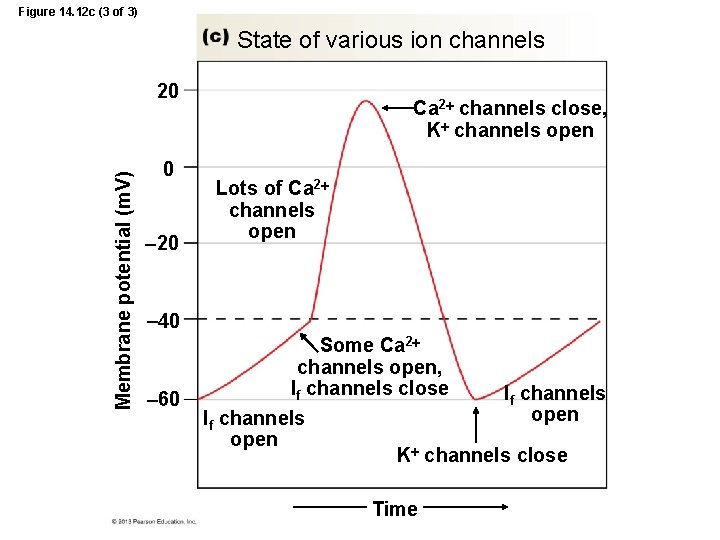
Figure 14. 12 c (3 of 3) State of various ion channels Membrane potential (m. V) 20 0 20 Ca 2 channels close, K channels open Lots of Ca 2 channels open 40 60 Some Ca 2 channels open, If channels close If channels open K channels close Time

Coordination of Contraction • Signal starts with depolarization of autorhythmic cells in sinoatrial node (SA node) in right atrium • Signal passes through internodal pathway to atrioventricular node (AV node) • Purkinje fibers carry signals down atrioventricular bundle (AV bundle, aka bundle of His) in ventricular septum • Within septum, AV bundle fibers divide into right and left bundle branches, continue to apex of heart • Purkinje fibers spread out among contractile cells. Ventricles contract from apex upward
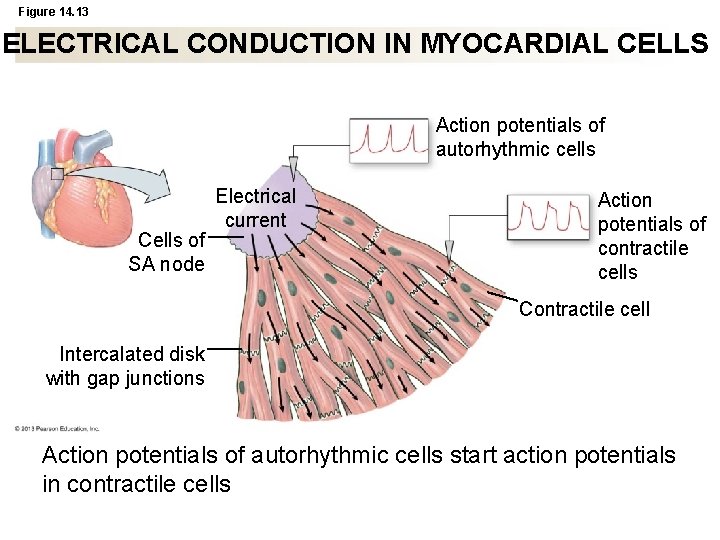
Figure 14. 13 ELECTRICAL CONDUCTION IN MYOCARDIAL CELLS Action potentials of autorhythmic cells Cells of SA node Electrical current Action potentials of contractile cells Contractile cell Intercalated disk with gap junctions Action potentials of autorhythmic cells start action potentials in contractile cells
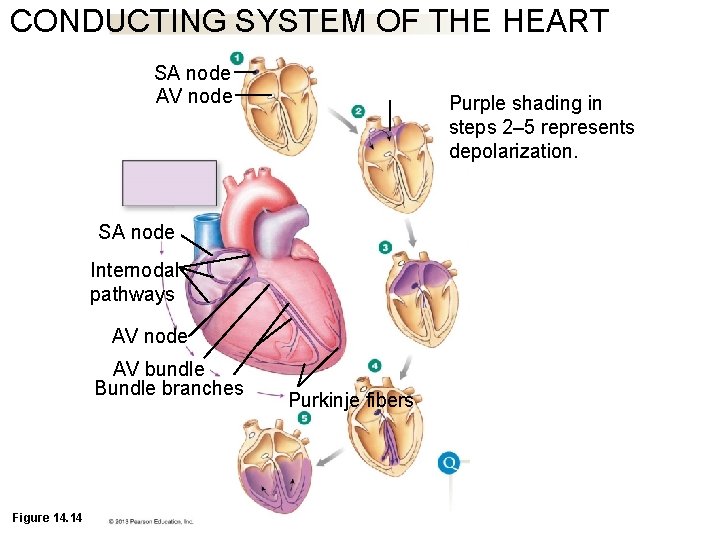
CONDUCTING SYSTEM OF THE HEART SA node AV node Purple shading in steps 2– 5 represents depolarization. SA node Internodal pathways AV node AV bundle Bundle branches Figure 14. 14 Purkinje fibers
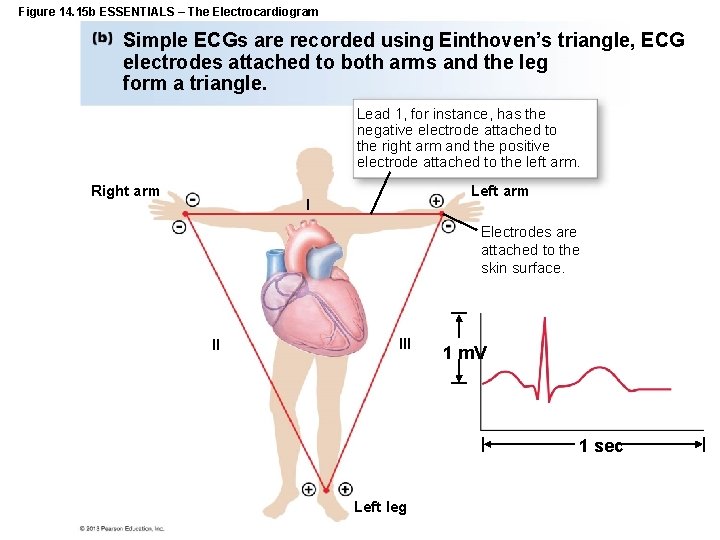
Figure 14. 15 b ESSENTIALS – The Electrocardiogram Simple ECGs are recorded using Einthoven’s triangle, ECG electrodes attached to both arms and the leg form a triangle. Lead 1, for instance, has the negative electrode attached to the right arm and the positive electrode attached to the left arm. Right arm Left arm I Electrodes are attached to the skin surface. II III 1 m. V 1 sec Left leg
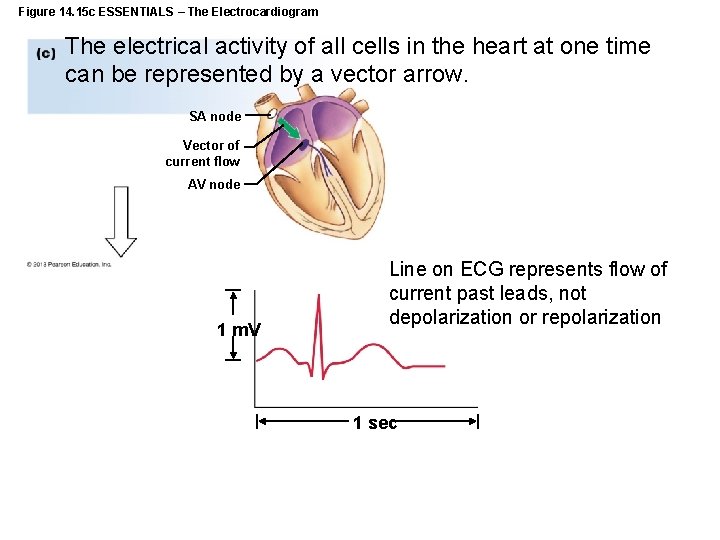
Figure 14. 15 c ESSENTIALS – The Electrocardiogram The electrical activity of all cells in the heart at one time can be represented by a vector arrow. SA node Vector of current flow AV node 1 m. V Line on ECG represents flow of current past leads, not depolarization or repolarization 1 sec
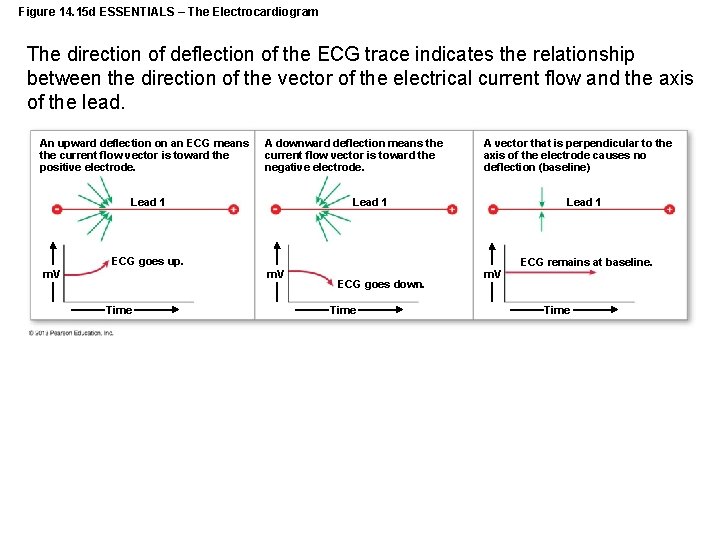
Figure 14. 15 d ESSENTIALS – The Electrocardiogram The direction of deflection of the ECG trace indicates the relationship between the direction of the vector of the electrical current flow and the axis of the lead. An upward deflection on an ECG means the current flow vector is toward the positive electrode. A downward deflection means the current flow vector is toward the negative electrode. Lead 1 A vector that is perpendicular to the axis of the electrode causes no deflection (baseline) Lead 1 ECG goes up. m. V Time ECG goes down. Time m. V ECG remains at baseline. Time
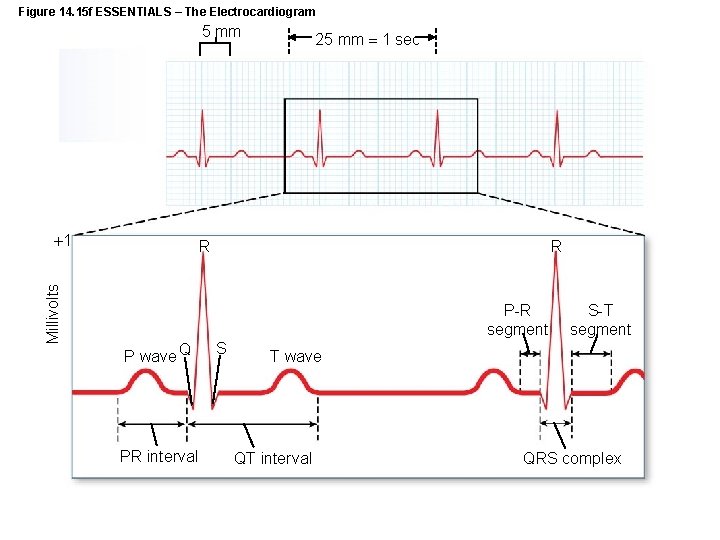
Figure 14. 15 f ESSENTIALS – The Electrocardiogram 5 mm Millivolts 1 25 mm 1 sec R R P-R segment P wave Q PR interval S S-T segment T wave QT interval QRS complex
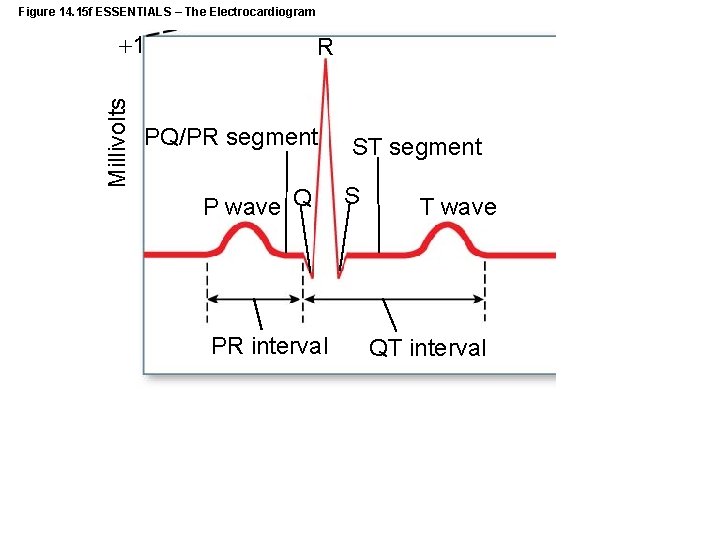
Figure 14. 15 f ESSENTIALS – The Electrocardiogram Millivolts 1 R PQ/PR segment P wave Q PR interval ST segment S T wave QT interval
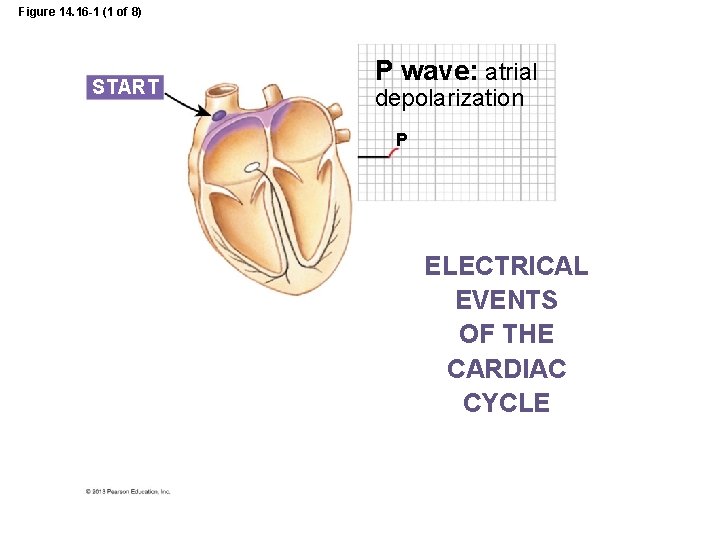
Figure 14. 16 -1 (1 of 8) START P wave: atrial depolarization P ELECTRICAL EVENTS OF THE CARDIAC CYCLE
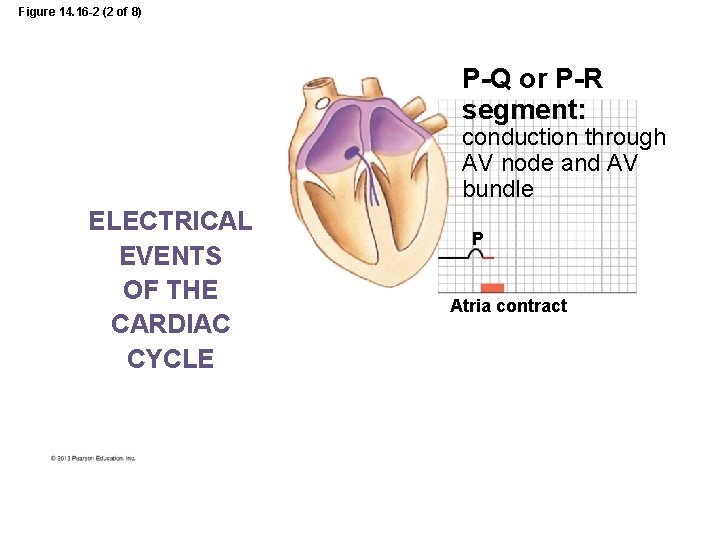
Figure 14. 16 -2 (2 of 8) P-Q or P-R segment: conduction through AV node and AV bundle ELECTRICAL EVENTS OF THE CARDIAC CYCLE P Atria contract
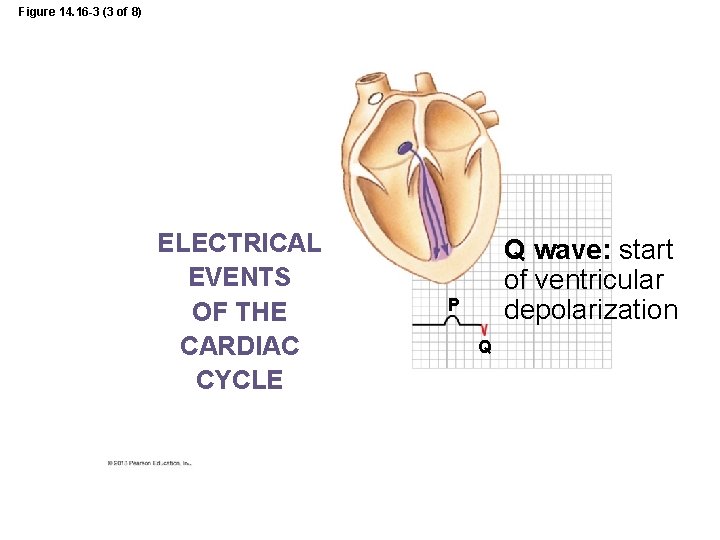
Figure 14. 16 -3 (3 of 8) ELECTRICAL EVENTS OF THE CARDIAC CYCLE Q wave: start of ventricular depolarization P Q
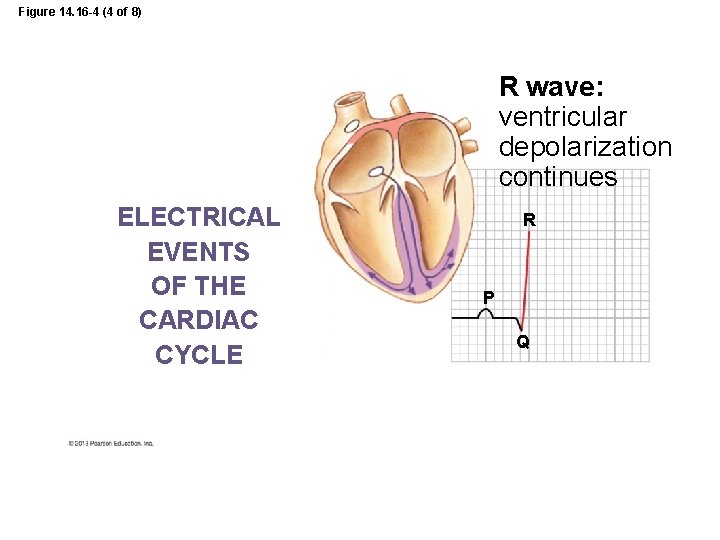
Figure 14. 16 -4 (4 of 8) R wave: ventricular depolarization continues ELECTRICAL EVENTS OF THE CARDIAC CYCLE R P Q
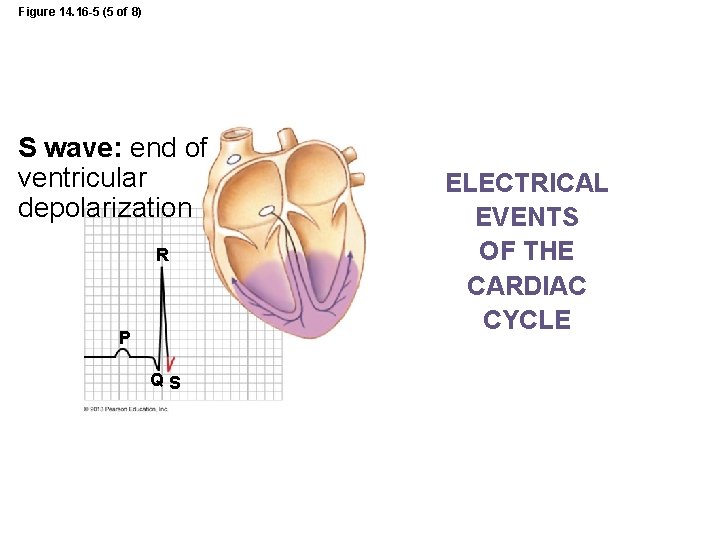
Figure 14. 16 -5 (5 of 8) S wave: end of ventricular depolarization R P QS ELECTRICAL EVENTS OF THE CARDIAC CYCLE
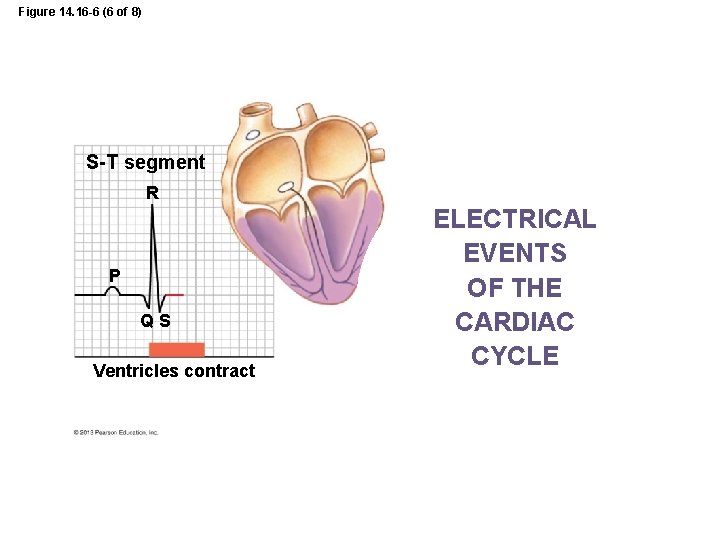
Figure 14. 16 -6 (6 of 8) S-T segment R P QS Ventricles contract ELECTRICAL EVENTS OF THE CARDIAC CYCLE
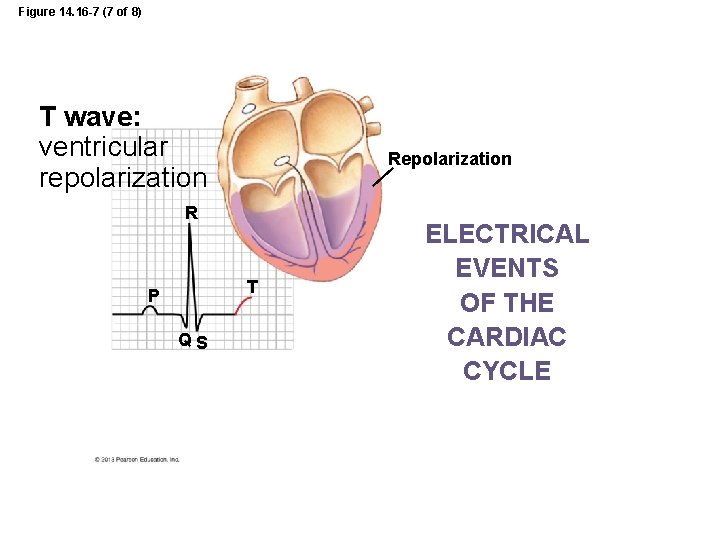
Figure 14. 16 -7 (7 of 8) T wave: ventricular repolarization R T P QS ELECTRICAL EVENTS OF THE CARDIAC CYCLE
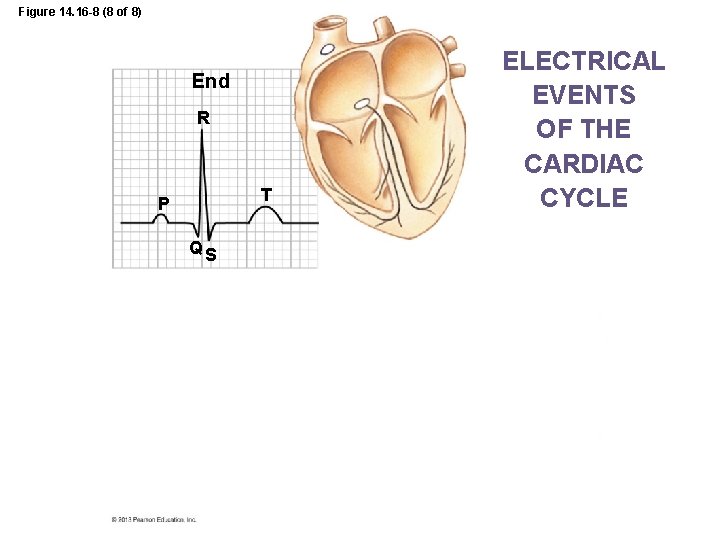
Figure 14. 16 -8 (8 of 8) End R T P QS ELECTRICAL EVENTS OF THE CARDIAC CYCLE
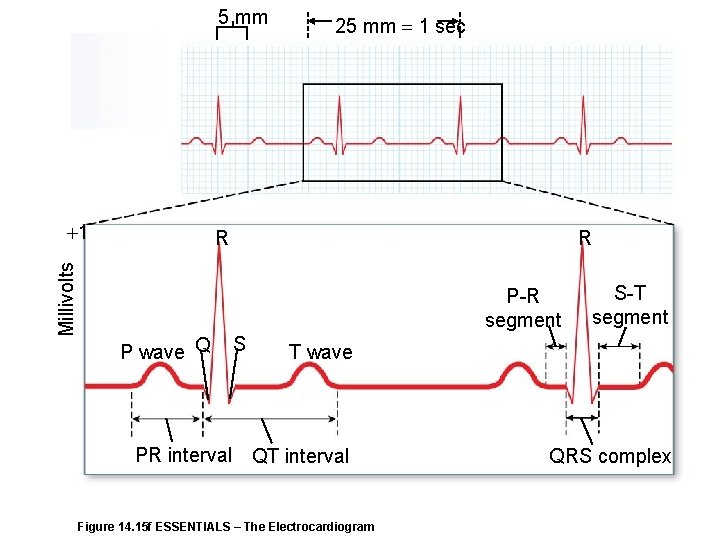
5 mm Millivolts 1 25 mm 1 sec R R P-R segment P wave Q S S-T segment T wave PR interval QT interval Figure 14. 15 f ESSENTIALS – The Electrocardiogram QRS complex
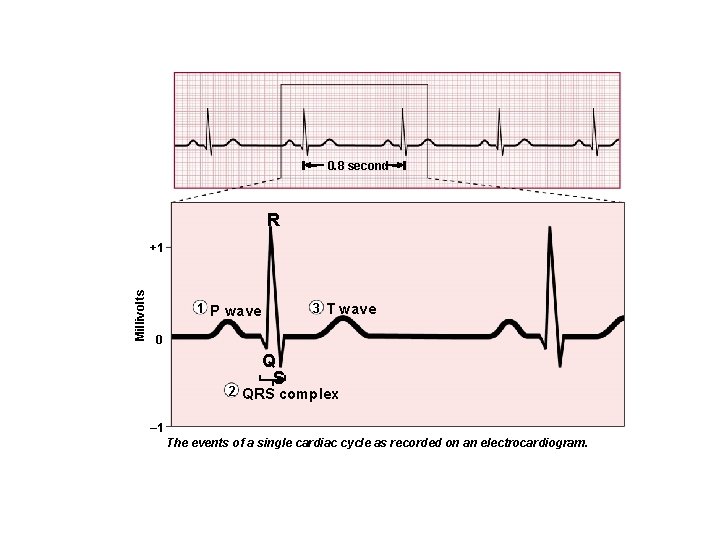
0. 8 second R Millivolts +1 3 T wave 1 P wave 0 Q S 2 QRS complex – 1 The events of a single cardiac cycle as recorded on an electrocardiogram.
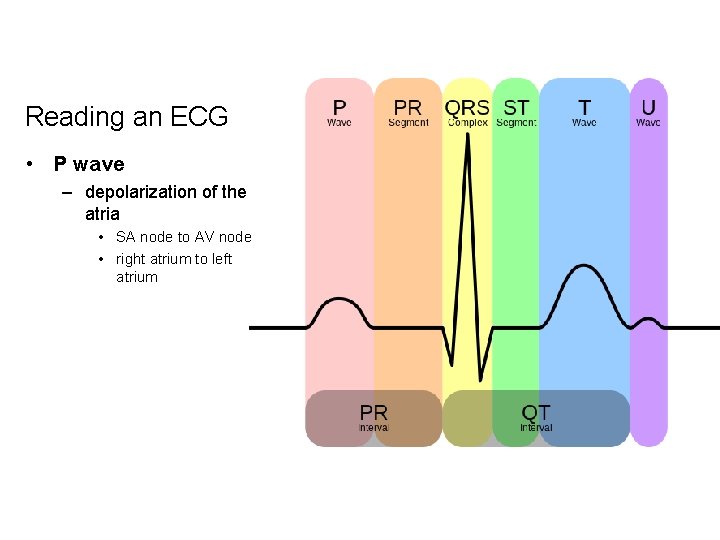
Reading an ECG • P wave – depolarization of the atria • SA node to AV node • right atrium to left atrium
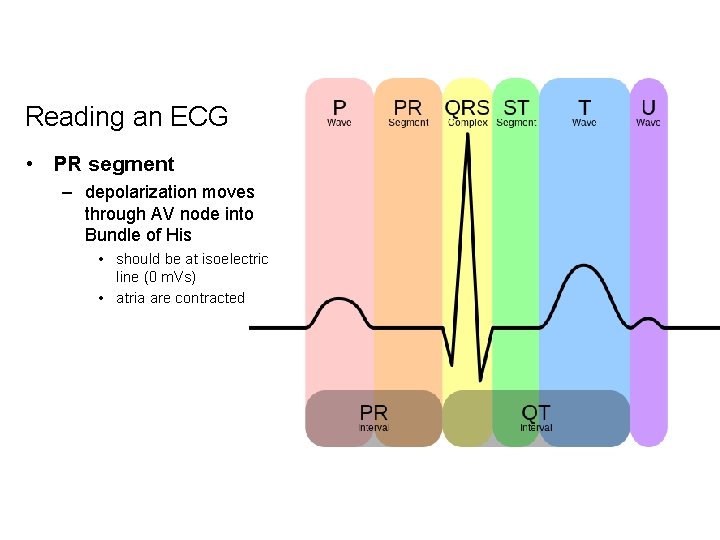
Reading an ECG • PR segment – depolarization moves through AV node into Bundle of His • should be at isoelectric line (0 m. Vs) • atria are contracted
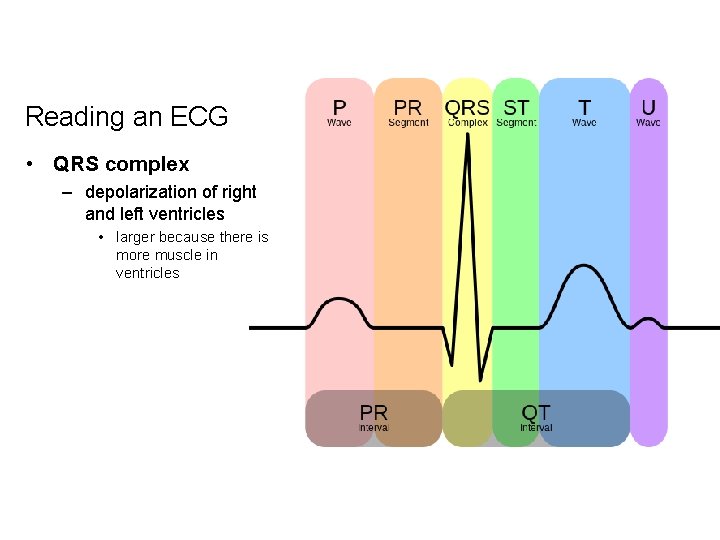
Reading an ECG • QRS complex – depolarization of right and left ventricles • larger because there is more muscle in ventricles
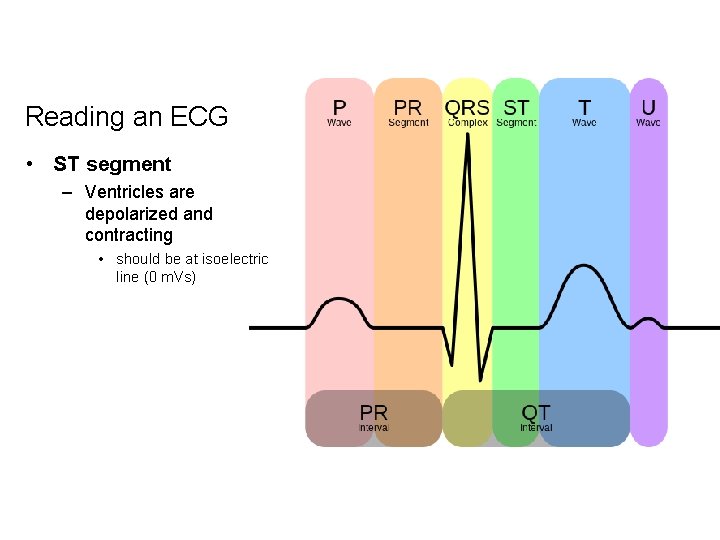
Reading an ECG • ST segment – Ventricles are depolarized and contracting • should be at isoelectric line (0 m. Vs)
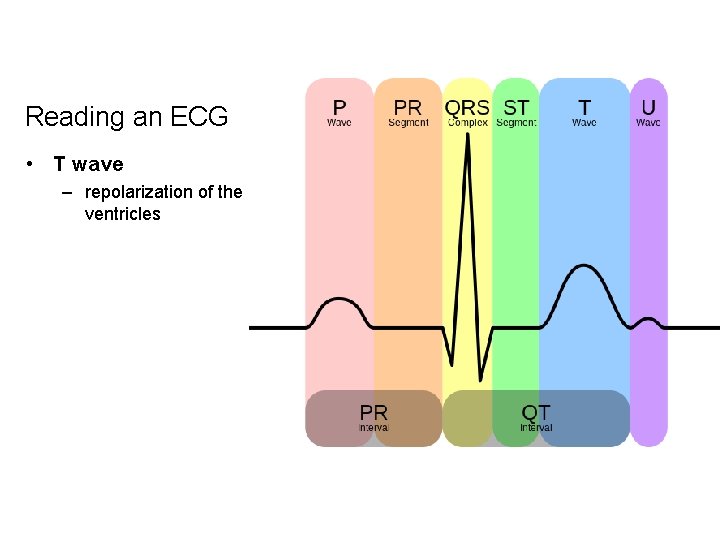
Reading an ECG • T wave – repolarization of the ventricles
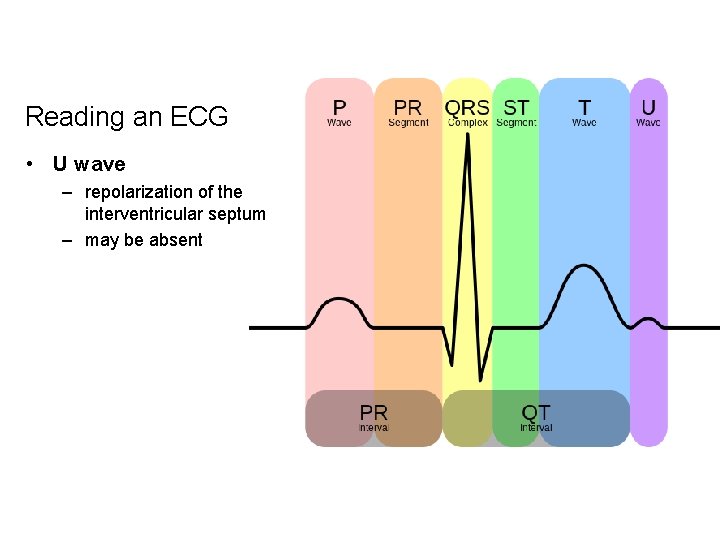
Reading an ECG • U wave – repolarization of the interventricular septum – may be absent

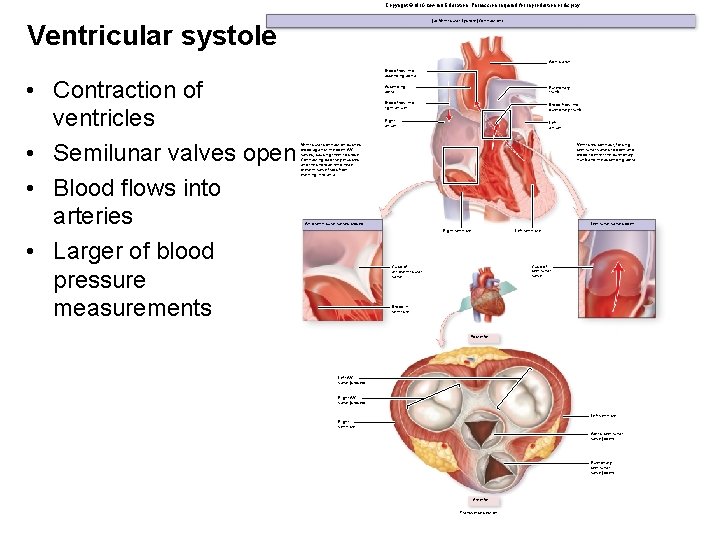
Copyright © Mc. Graw-Hill Education. Permission required for reproduction or display. (a) Ventricular Systole (Contraction) Ventricular systole Aortic arch • Contraction of ventricles • Semilunar valves open • Blood flows into arteries • Larger of blood pressure measurements Blood flow into ascending aorta Ascending aorta Pulmonary trunk Blood flow into right atrium Blood flow into pulmonary trunk Right atrium Left atrium Ventricular contraction pushes blood against the open AV valves, causing them to close. Contracting papillary muscles and the chordae tendineae prevent valve flaps from everting into atria. Ventricles contract, forcing semilunar valves to open and blood to enter the pulmonary trunk and the ascending aorta. Atrioventricular valves closed Semilunar valves open Right ventricle Left ventricle Cusp of semilunar valve Cusp of atrioventricular valve Blood in ventricle Posterior Left AV valve (closed) Right AV valve (closed) Left ventricle Right ventricle Aortic semilunar valve (open) Pulmonary semilunar valve (open) Anterior Transverse section
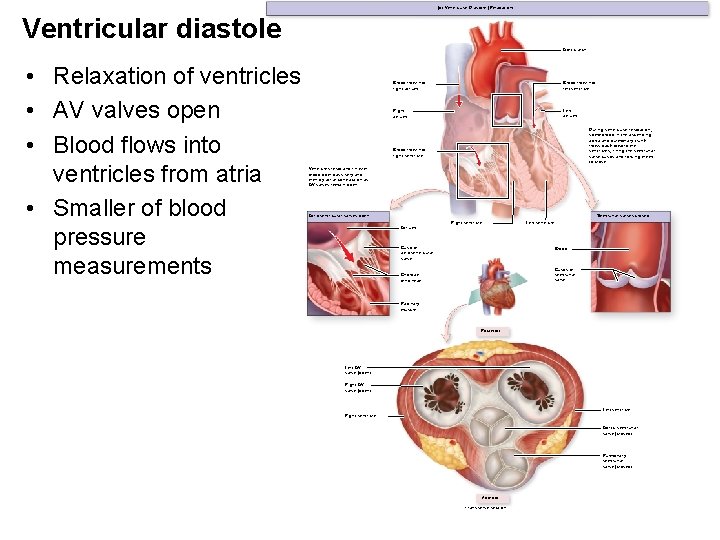
(b) Ventricular Diastole (Relaxation) Ventricular diastole Aortic arch • Relaxation of ventricles • AV valves open • Blood flows into ventricles from atria • Smaller of blood pressure measurements Blood flow into right atrium Blood flow into left ventricle Right atrium Left atrium During ventricular relaxation, some blood in the ascending aorta and pulmonary trunk flows back toward the ventricles, filling the semilunar valve cusps and forcing them to close. Blood flow into right ventricle Ventricles relax and fill with blood both passively and then by atrial contraction as AV valves remain open. Atrioventricular valves open Semilunar valves closed Right ventricle Left ventricle Atrium Cusp of atrioventricular valve Blood Cusps of semilunar valve Chordae tendineae Papillary muscle Posterior Left AV valve (open) Right AV valve (open) Left ventricle Right ventricle Aortic semilunar valve (closed) Pulmonary semilunar valve (closed) Anterior Transverse section
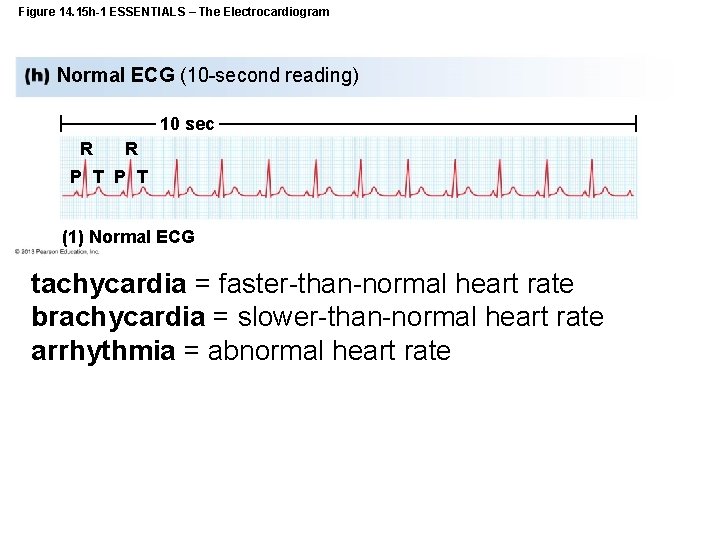
Figure 14. 15 h-1 ESSENTIALS – The Electrocardiogram Normal ECG (10 -second reading) 10 sec R R P T (1) Normal ECG tachycardia = faster-than-normal heart rate brachycardia = slower-than-normal heart rate arrhythmia = abnormal heart rate
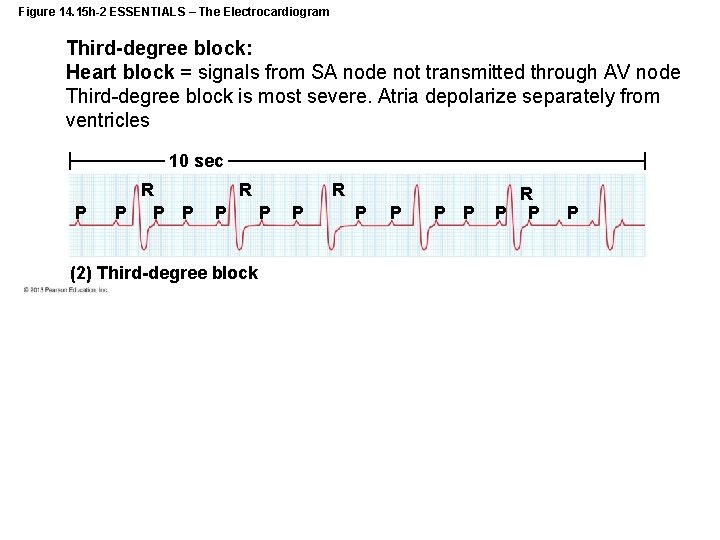
Figure 14. 15 h-2 ESSENTIALS – The Electrocardiogram Third-degree block: Heart block = signals from SA node not transmitted through AV node Third-degree block is most severe. Atria depolarize separately from ventricles 10 sec P R P P P R P (2) Third-degree block R P P P
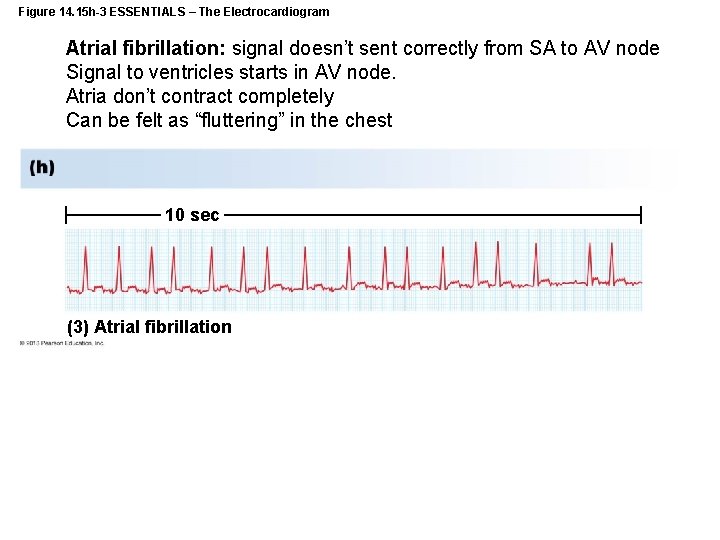
Figure 14. 15 h-3 ESSENTIALS – The Electrocardiogram Atrial fibrillation: signal doesn’t sent correctly from SA to AV node Signal to ventricles starts in AV node. Atria don’t contract completely Can be felt as “fluttering” in the chest 10 sec (3) Atrial fibrillation
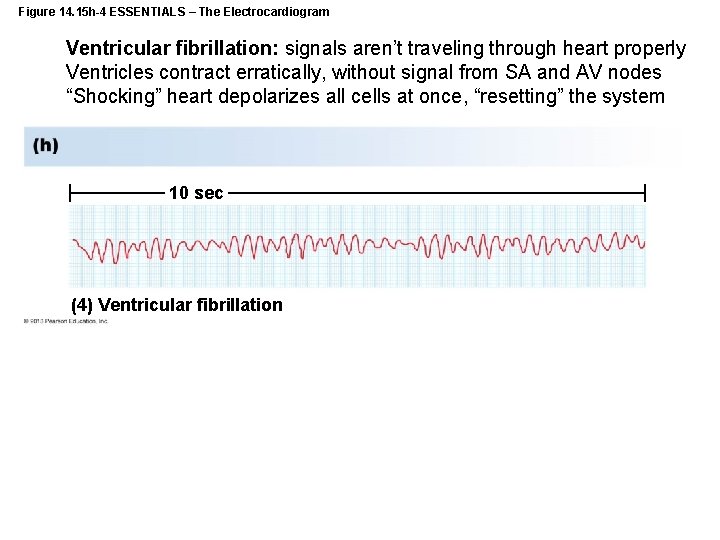
Figure 14. 15 h-4 ESSENTIALS – The Electrocardiogram Ventricular fibrillation: signals aren’t traveling through heart properly Ventricles contract erratically, without signal from SA and AV nodes “Shocking” heart depolarizes all cells at once, “resetting” the system 10 sec (4) Ventricular fibrillation
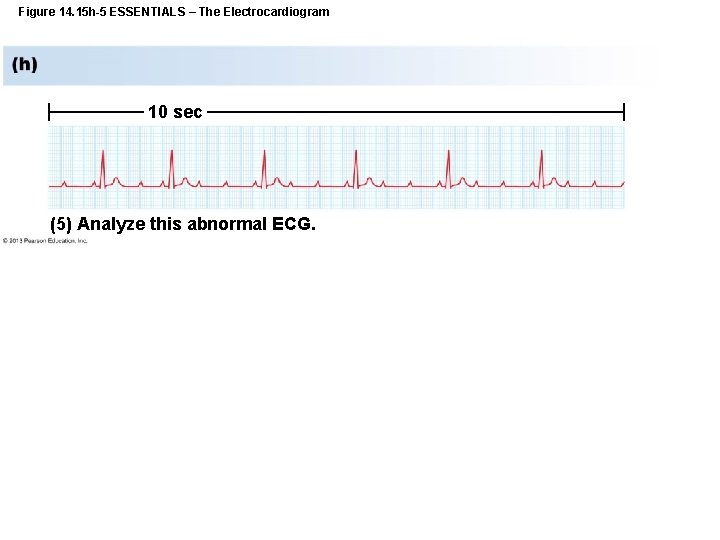
Figure 14. 15 h-5 ESSENTIALS – The Electrocardiogram 10 sec (5) Analyze this abnormal ECG.
Heart Volumes • End-diastolic volume (EDV) = max. volume of blood ventricle will hold when relaxed – ~135 m. L in avg. man • End-systolic volume (ESV) = volume of blood ventricle left in ventricle at end of contraction – ~65 m. L in avg. man

Stroke Volume • Stroke volume = amount of blood pumped by one ventricle during a contraction – measured in m. L/beat

Effectiveness of Heart as Pump •

Neural Control • W/o sympathetic or sympathetic influence, heart rate is 90 -100 bpm • Parasympathetic division releases ACh, slows heart rate – increases K+ permeability, decreases Ca 2+ permeability • Sympathetic releases norepinephrine and epinephrine – increase permeability of Ca 2+ channels and If channels
- Slides: 74