Chapter 13 Health Problems Complicating Pregnancy 1 Copyright

Chapter 13 Health Problems Complicating Pregnancy 1 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

Complications of Pregnancy 2 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

3 Objectives – Define key terms listed. – Discuss three causes of spontaneous abortion. – Describe ectopic pregnancy. – Describe placenta previa and state the characteristic symptom. – Explain five nursing measures for the care of a woman who is hemorrhaging. Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

4 Objectives (cont. ) – Compare two types of abruptio placentae. – Review the cause of coagulation defects in pregnancy. – List five causes of high-risk pregnancies and three leading causes of maternal death. – Recognize four factors that increase the risk for gestational hypertension. Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

5 Effects of a High-Risk Pregnancy on the Family – Disruption of usual roles – May require strict bed rest – May have to find alternate child care – Financial difficulties – Delayed attachment to infant Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

6 Bleeding Disorders – Abnormal in pregnancy and should be investigated – Maternal blood loss decreases oxygen-carrying capacity to fetus Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

7 Causes of Bleeding in Early Pregnancy – Spontaneous abortion – Cervical polyps – Uterine fibroids – Ectopic pregnancy – Hydatidiform mole Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

8 Abortion – Intentional or unintentional ending of a pregnancy before 20 weeks gestation – Miscarriage is a lay term for spontaneous abortion – Artificial or mechanical means for therapeutic or elective reasons can also be performed Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

9 Classification and Management of Abortions – Causes of spontaneous abortion – Genetic defects – Defective ovum or sperm – Defective implantation – Uterine fibroids – Maternal factors Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

10 Maternal Factors – Chronic conditions – Acute infections – Nutritional deficiencies – Abnormalities of maternal reproductive organs – Endocrine deficiencies – Blood group dyscrasias (ABO incompatibility) Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

11 Nursing Interventions – Monitor vital signs – Observe for signs of shock – Weigh perineal pads – Prepare for IV therapy – Assess fetal heart rate – Provide supplemental oxygen – Obtain history and laboratory results – Provide emotional support for woman and partner Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

12 Incompetent Cervix – Cervix dilates without perceivable contractions – Internal os dilates – Incapable of supporting increasing weight and pressure of growing fetus – Cervix may need to be reinforced through a cerclage procedure Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.
13 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.
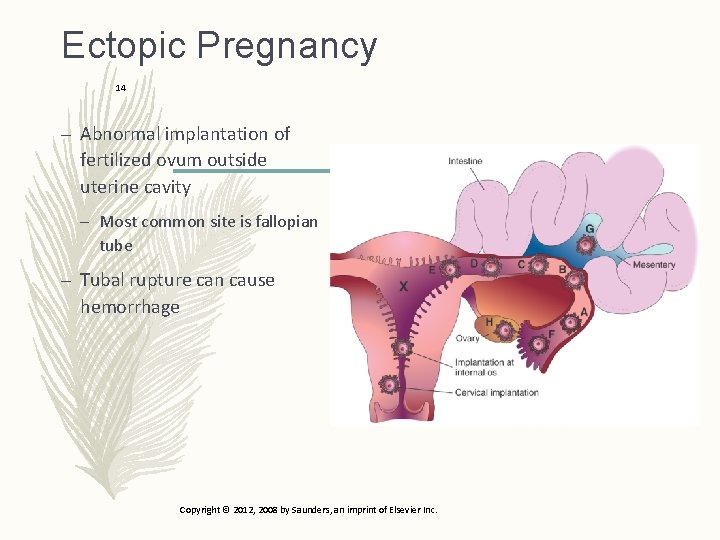
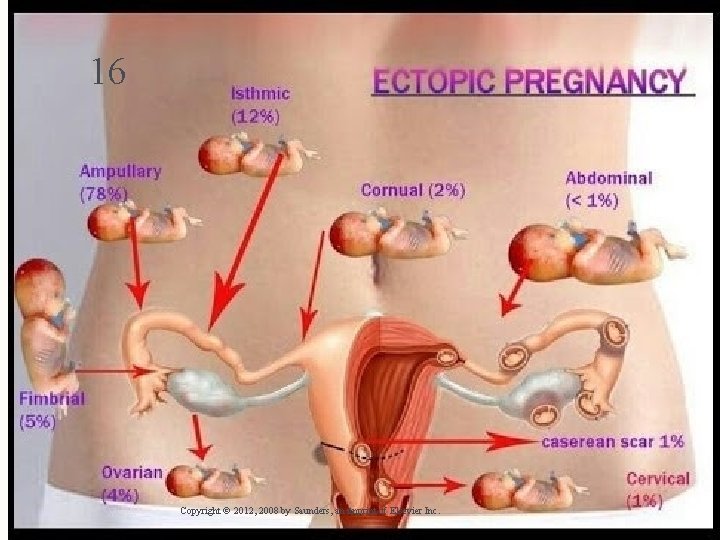
Ectopic Pregnancy 14 – Abnormal implantation of fertilized ovum outside uterine cavity – Most common site is fallopian tube – Tubal rupture can cause hemorrhage Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

15 Assessment of Tubal Pregnancy – Transvaginal ultrasound – Serum hormone levels – Progesterone – β-h. CG (beta-human chorionic gonadotropin) – Shoulder pain – Signs of shock out of proportion with visible blood loss Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.
16 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

17 Management of Tubal Pregnancy – Preserve fallopian for chance of future pregnancies – Depends on status of tube: ruptured or unruptured – Methotrexate – Interferes with cell reproduction – Surgical interventions – salpingectomy Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

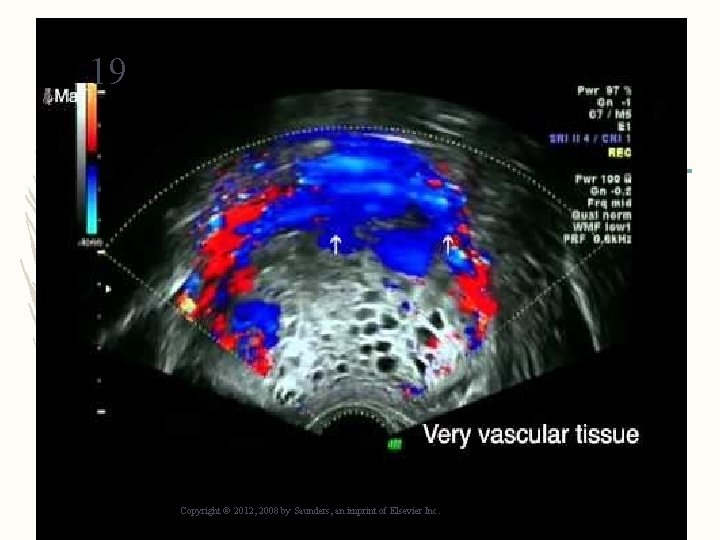
18 Gestational Trophoblastic Disease – Hydatidiform mole – Trophoblastic tissue proliferates – Chorionic villi of placenta swell with fluid; can look like grapes – Invasive mole – Choriocarcinoma Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.
19 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

20 Gestational Trophoblastic Disease (cont. ) – Two types – Complete – Chromosome banding and enzyme analysis show all genetic material is paternally derived – No inner cell mass develops – No fetal vascularization – Partial – Genetic material maintained – Fetus abnormal, usually aborts Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

21 Assessment of Molar Pregnancy – Uterus grows more rapidly than in a normal pregnancy – Brown vaginal bleeding (looks like prune juice) – Hyperemesis gravidarum – If gestational hypertension occurs before 24 weeks gestation, strongly suggests molar pregnancy – Serial β-h. CG levels and ultrasound Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

22 Management of Molar Pregnancy – Evacuation by suction aspiration – Follow-up is essential due to increased risk of developing choriocarcinoma – Serum h. CG levels monitored for 1 year until serum titers return to normal – Should delay pregnancy until h. CG has returned to normal Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.
23 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

24 Bleeding in Late Pregnancy – May be from increased vascularization of cervix, cervical polyps, or cervicitis – If in second or third trimester, may be caused by – Placenta previa – Abruptio placentae – Disseminated intravascular coagulation (DIC) Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

25 Placenta Previa – Placenta abnormally implants near or over cervical os – Increased risk of occurrence if – Defective vascularity of decidua – Previous infection in upper uterine segment – Uterine scarring Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.
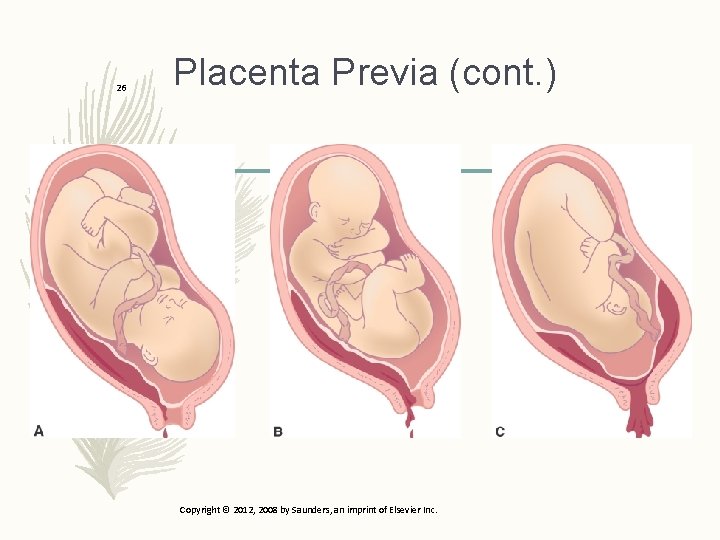
26 Placenta Previa (cont. ) Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

27 Assessment and Management – Ultrasound can detect presence – Suspect if onset of painless bleeding occurs after 24 weeks gestation – Bleeding occurs most often in third trimester as cervix prepares for delivery – Monitor vital signs and amount of blood loss, including fetal heart rate – Do not perform vaginal examination Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

28 Home Management – If following criteria are met, woman can be sent home – Maintain strict bed rest and no coitus – Must have around-the-clock transportation and communication available – Compliant with oral tocolytic therapy – Hematocrit above 30% – Can be followed closely (e. g. , ultrasound, nonstress test, biophysical profiles) Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

29 Potential Complications – Hemorrhage for woman – Hypoxia or death of fetus – Hypovolemic shock and death of mother – Postpartum infection Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.
30 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

31 Abruptio Placentae – Premature separation of placenta – Partial or total detachment – Occurs after 20 weeks gestation – Bleeding is painful – Risks include – Maternal hypertension – Prior abruption – High parity – Degree of compromise depends on extent of separation and blood loss Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.
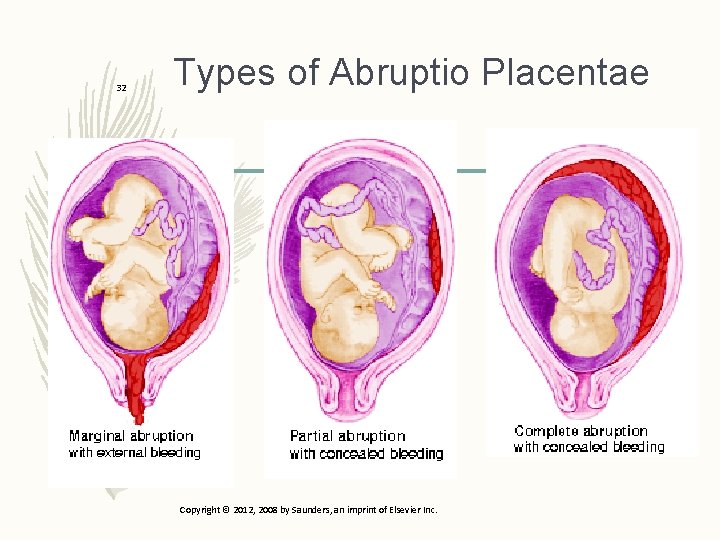
32 Types of Abruptio Placentae Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

33 Complications – Inability of uterus to contract – Trapping of blood may release thromboplastin into maternal circulation – Can lead to DIC Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

34 Assessment and Management – Dark red vaginal bleeding – Uterine rigidity – Severe abdominal pain – Maternal hypovolemia – Signs of fetal distress – Excessive bleeding – Coagulation profile – Prepare for cesarean delivery if hemorrhage severe or fetal distress evident Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.
35 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

36 Disseminated Intravascular Coagulation (DIC) – Blood cannot clot – Overstimulation of normal coagulation process – Massive, rapid fibrin formation – Depleted platelets and clotting factors – Does not occur as primary disorder but secondary to another complication Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

37 Assessment and Management – Monitor coagulation studies closely – Correct underlying cause – Terminate pregnancy – Administer blood products – Do not give heparin Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.
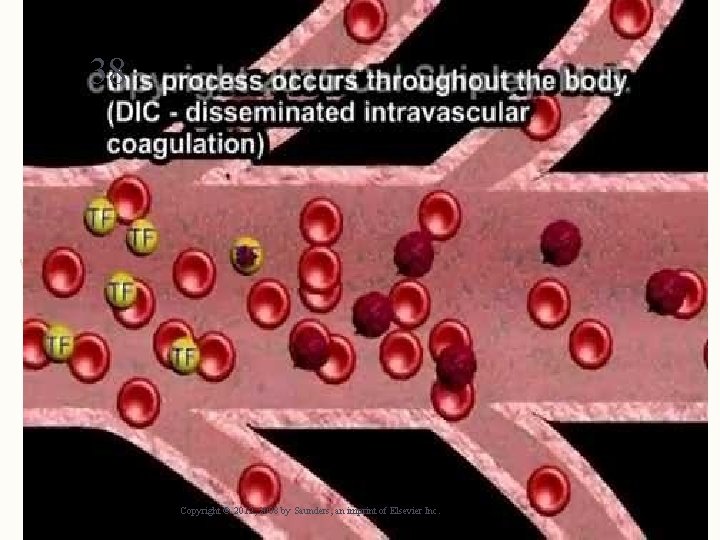
38 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

39 Blood Incompatibility (Isoimmunization) – Placenta can allow maternal and fetal blood to mix due to small “leaks” – If maternal and fetal blood compatible, no issues – If not compatible, mother’s body produces antibodies to destroy foreign fetal RBCs Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

40 Rh Incompatibility – Rh-positive blood type is dominant trait – If father is Rh positive and mother is Rh negative, good chance fetus will be Rh positive – If leakage occurs, mother starts making antibodies to destroy the Rh-positive erythrocytes, which also destroy fetal RBCs Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

41 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

42 ABO Incompatibility – Woman has group O blood – Fetus has group A, B, or AB blood – Anti-A and anti-B antibodies – Few cross placenta, so treatment not required during pregnancy – First pregnancy most often affected – Newborn may develop jaundice within 24 hours of birth – Provide phototherapy Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

43 Audience Response System Question 1 In the presence of Rh incompatibility, an amniocentesis can be done to determine if what is present? A. Fetal hemolysis B. A congenital anomaly C. Alpha-fetoprotein levels D. Genetic disorders Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

Cardiovascular and Endocrine Complications 44 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

45 Objectives – Discuss three signs that a pregnant hypertensive woman should report immediately to her physician. – Identify the antihypertensive drug most commonly given to women with gestational hypertension and its antidote. – Compare the effects of the physiologic changes in pregnancy related to thromboembolic disease. Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

46 Objectives (cont. ) – Discuss heart disease in pregnancy. – Explain hyperemesis gravidarum. – Explain three ways diabetes mellitus affects pregnancy. – Review four aspects of self-care for the diabetic woman. Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

Cardiovascular Disorders 47 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

48 Gestational Hypertension – Types – Gestational hypertension – Preeclampsia – Eclampsia – Chronic hypertension – Preeclampsia with superimposed chronic hypertension Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

49 Classification and Risk Factors – Preeclampsia—renal involvement leads to proteinuria – Eclampsia—CNS involvement leads to seizures and chronic HTN with superimposed eclampsia – HELLP syndrome—disease is dominated by hematologic and hepatic clinical manifestations Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

50 Pathophysiology of Preeclampsia – Thought to start with placental implantation – May not be evident until 20 weeks gestation – Loss of resistance to angiotensin II – Prostacyclin (vasodilator) decreases – Thromboxane (vasoconstrictor) increases – Leads to increased vasospasms – Condition reverses once placenta is delivered Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

51 – Mother Effects on the Mother and Fetus – DIC – Uteroplacental perfusion – Immunologic response may trigger preeclampsia – Increased risk of abruptio placentae – HELLP – Fetal distress from hypoxia – Nausea, vomiting, malaise – Preterm birth – Intrauterine growth restriction – Later: hematuria, jaundice, generalized abdominal pain Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

52 Assessment and Management – If occurs before 34 weeks gestation, screen for presence of antiphospholipid antibodies – If present, increases risk of recurrent severe gestational hypertension in future pregnancies – Closely monitor blood pressure, proteinuria, renal and hepatic function – If severe, may have to terminate pregnancy/deliver – Should not go beyond 40 weeks gestation due to placental insufficiency – Magnesium sulfate infusion – Toxicity treated with calcium gluconate Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

53 Clinical Manifestations of Gestational Hypertension (GH) – Expedient delivery if – Maternal oliguria – Renal failure – HELLP syndrome – Magnesium sulfate therapy should be stopped if – Loss of deep tendon reflexes (DTRs) – Respiratory rate < 12/min – Decreased urine output of < 30 m. L/hr Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

54 Prenatal Nursing Assessment and Management – If mother received magnesium sulfate, can cause respiratory depression in newborn – Evaluate deep tendon reflexes – A mild form of preeclampsia may rapidly progress to a severe form, including seizures – Management depends on symptoms, aggressiveness of physician, and understanding and compliance of the patient – Calcium gluconate is used to treat magnesium sulfate toxicity Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

55 Education, Self-Care, Home Management – Important to know baseline blood pressure – Increases in systolic by 30 mm Hg and diastolic by 15 mm Hg above baseline places woman in high-risk category – Careful teaching, guidance, and compliance are critical to the woman, the developing fetus, and family – If on home management, woman must have a means of communication and transportation Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

56 Hospitalization and Management of Preeclampsia and Eclampsia – Quiet room – Left side-lying – To optimize placental blood flow – Frequent monitoring of blood pressure – Urine evaluated every 4 hours for protein and specific gravity – Accurate I&O Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

57 Emergency Care – Equipment to have readily available – Oral airway – Ambu bag – Symptoms that may precede seizures – Rise in blood pressure – Oxygen – Epigastric pain – Suction equipment – Severe headache – Ophthalmoscope – Apprehension – Medications – Pulse oximetry – Electrocardiography Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc. – Twitching – Hyperirritability of muscles

58 Chronic Hypertensive Disease – Blood pressure of 140/90 mm Hg or higher before pregnancy or before 20 weeks gestation – Goal is to prevent preeclampsia, ensure normal fetal growth and development – Antihypertensive may be prescribed for blood pressure over 160/100 mm Hg Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

59 Chronic Hypertension with Superimposed Preeclampsia – First 48 hours after delivery require careful monitoring – After 48 hours, assessments may be decreased – Monitor uterine tones and fundus to prevent postpartum bleeding – Baseline blood pressure usually returns within 2 weeks Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

60 Thromboembolic Disease – Pregnancy increases risk of superficial thrombophlebitis, deep vein thrombosis, and pulmonary embolism (PE) – PE leading cause of maternal death – Risk factors – Venous stasis – Normal changes in coagulability and fibrinolysis during pregnancy – Use of oral contraceptives before pregnancy – Sitting for extended periods – Over 30 – Obese Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

61 Assessment – May complain of sudden pain with swelling in affected extremity – May be warmth and redness at site – On passive dorsiflexion, pain in calf of leg (Homans’ sign) – Diagnosed via Doppler scanning, MRI – If develops a PE, may have dyspnea, chest pain, hemoptysis, and tachycardia Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

62 Heart Disease: Effects During Pregnancy – Pregnancy results in increased cardiac output, heart rate, blood volume, and stroke volume – Some drugs to help treat are contraindicated in pregnancy – During labor, woman requires careful monitoring due to blood shifts of 300 to 500 m. L – This leads to increased cardiac output by 15% to 20%; could trigger congestive heart failure Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

63 Assessment and Management – May complain of shortness of breath with activity, weight gain, edema; may hear cardiac murmur – Contraindications to planned pregnancy include pulmonary hypertension, aortic coarctation, history of myocardial infarction, and uncorrected tetralogy of Fallot – Goal is to minimize stress on heart – Symptoms of cardiac decompensation can occur slowly during pregnancy Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

64 Anemia – Reduced ability of blood to carry oxygen to cells – In pregnancy, defined by hemoglobin (Hgb) levels less than 10 g/d. L and hematocrit (Hct) levels below 30% – More susceptible to infection, increased risk of complications during pregnancy Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

65 Anemia (cont. ) – Iron deficiency anemia—serum iron of less than 60 mg/d. L with less than 16% transferrin saturation – Folic acid deficiency—may result from inadequate intake, poor absorption or drug interactions; seen in women with vitamin B 12 deficiency – Thalassemia—genetic defect; abnormal Hgb; results in hemolysis and anemia Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

66 Sickle Cell Anemia – Inherited disorder; presence of abnormal Hgb that causes sickling of RBCs – During labor – Oxygen supplementation to mother – Administration of IV fluids – Fetal monitoring – Maternal Hgb monitoring – Administration of prophylactic antibiotics if operative delivery is necessary or urinary tract infection is present Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

67 GI Disorders: Hyperemesis Gravidarum – Nausea and vomiting that can lead to severe dehydration, electrolyte imbalance, starvation, and excessive weight loss before the 20 th week of gestation – Occurs most often with first pregnancy, multifetal pregnancy, hydatidiform mole, and sometimes with psychiatric disorders – Fetus at risk for intrauterine growth restriction (IUGR) Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

68 Assessment and Management – Any specific “triggers” for nausea or vomiting? – Correct fluid and electrolyte imbalance – Parenteral nutrition may be indicated – Record I&O, including weight – Ketonuria suggests fat stores are being used to nourish fetus and meet woman’s energy needs – Low-fat frequent feedings – Positioning and other techniques to reduce nausea and vomiting – Drugs such as pyridoxine, meclizine Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

69 Endocrine Disorders: Diabetes Mellitus (DM) – Affects carbohydrate metabolism – Hyperglycemia; inadequate production or ineffective use of insulin – Pregestational DM: type 1 or 2 – Gestational DM: glucose intolerance first recognized during pregnancy; usually resolves after delivery Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

70 Effect of Pregnancy on Diabetes – Increased need for glucose creates a resistance to insulin – Maternal insulin does not cross placenta – By 10 th week of gestation, fetus is obligated to secrete own insulin to use glucose obtained from mother – Hormone concentration higher in second and third trimesters, which increases insulin resistance – Allows more maternal glucose to be available to fetus; leads to macrosomia Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

71 Pregestational Diabetes Mellitus – Known diabetic before pregnancy – Once pregnant, glycemic control affected – Oral hypoglycemics cannot be taken during pregnancy – First trimester maternal blood glucose usually reduced; need less insulin Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

72 Risk and Complications – First trimester: hyperglycemia can cause fetal anomalies – Second and third trimesters: glucose crosses placenta, increases fetal secretion of insulin – Can lead to macrosomia and impaired fetal lung function – At birth, newborn at risk for hypoglycemia Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

73 Preconceptional Counseling, Assessment, and Management – Woman should normalize blood glucose – Some medications may need to be changed – Close monitoring throughout pregnancy may be needed for both mother and fetus – Management depends on woman’s adherence to treatment plan – Diet: 30 to 35 kcal/kg/day in first trimester, 35 kcal/kg/day in second and third trimesters – Exercise Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

74 Gestational Diabetes Mellitus – Carbohydrate intolerance of variable severity, with first recognition during pregnancy – May have only impaired tolerance to glucose or classic signs of DM (polyuria, polyphagia, polydipsia) – Risk of congenital malformation and spontaneous abortion is less with GDM – Diet often controls blood sugars Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

75 Screening During Pregnancy – Glucose challenge test – Usually between 24 and 28 weeks gestation – Renal threshold lower in pregnancy, causes glucose to spill into urine – Glycosuria is not considered diagnostic for DM but does indicate need for further evaluation – Glucose monitoring daily and with a blood test called Hb. A 1 c – Fetal surveillance: biophysical profile, alpha-fetoprotein, kick count Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

76 Audience Response System Question 2 At what approximate week of development is the fetus obligated to secrete its own insulin? A. 20 weeks B. 30 weeks C. 10 weeks D. 40 weeks Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

Effects of Toxins and Pregnancy Loss 77 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

78 Objectives – Describe rubella and its consequences in pregnancy. – Identify the changes that occur in pregnancy that predispose the woman to urinary tract infections. – Discuss the cause and prevention of toxoplasmosis. – Describe three self-care measures for a pregnant woman with a urinary tract infection. – Describe how the use of nicotine, alcohol, and recreational drugs can affect the fetus. Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

79 Objectives (cont. ) – Discuss the effects of substance abuse on women’s health. – Relate the impact of pregnancy on the woman’s response to bioterrorist agent exposure and treatment protocols. – Recognize the effects of drugs used to treat bioterrorist infections on the developing fetus. – Identify signs of fetal demise. – Recognize stages of grieving and nursing interventions that can assist parents in dealing with fetal loss. Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

80 Infections – TORCH – Can be used to help identify congenital risks – Urinary tract infection (UTI) – Can have asymptomatic infection, cystitis, or pyelonephritis – Symptoms vary – Bacteriuria – Group B streptococci – Bacterial vaginosis Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

81 Substance Abuse – Use of illegal drugs, tobacco, and alcohol can cause serious complications in the developing fetus – IV and intranasal administration crosses placenta more often than other methods – Prenatal care may not occur until late into pregnancy, if at all Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

82 Accidents During Pregnancy – Motor vehicle accidents most common cause of trauma during pregnancy – Blunt trauma can lead to abruptio placentae and fetal demise – Blunt trauma or penetrating wounds can cause shock, preterm labor, spontaneous abortion – ABCs (airway, breathing, circulation) Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

83 Bioterrorism Exposure and Pregnancy – Metabolism and elimination of drugs altered in pregnancy – Protecting life of mother is priority – Vaccines may be needed regardless of pregnancy status – Pregnancy increases susceptibility to infections – Countermeasures include antibiotics, antivirals, antitoxins Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

84 Loss of Expected Birth Experience – Allow parents to remain together in privacy – Accept behaviors related to grieving – Develop care plan to provide support to family – Offer memento and opportunity to hold infant, if parents choose – Preparents for infant’s appearance – Discuss wishes concerning religious and cultural rituals Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

85 Pregnancy Loss: Grief and Bereavement – Perinatal loss after 20 weeks gestation in United States is 6. 8 per 1000 total births – 50% occur before 28 weeks – Causes: physiologic, maladaptation, birth defects, teratogen exposure – Loss includes abortion, fetal or neonatal death, SIDS, and fetal anomalies – Denial, anger, bargaining, depression, acceptance are steps in grieving process – Nurse plays important role Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

86 Audience Response System Question 3 In preeclampsia, the most likely cause of serious end-organ effects or alterations in function during pregnancy is: A. Hemorrhage B. Medications C. Vasospasms D. Hypervolemia Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.

Review Key Points 87 Copyright © 2012, 2008 by Saunders, an imprint of Elsevier Inc.
- Slides: 87