CHAPTER 13 Bipolar and Related Disorders Copyright 2014

CHAPTER 13 Bipolar and Related Disorders Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc.

Clinical Picture • Bipolar I disorder • Bipolar II disorder • Cyclothymia Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 2

Bipolar Disorder – DSM V • A distinct period of abnormally & persistently elevated, expansive, or irritable mood and persistently increased goal-directed activity or energy, lasting at least one week and present most of the day, nearly every day • Or any duration if hospitalization is required in bipolar disorder, type 1 3

Bipolar Disorder – DSM V (continued) During the period of mood disturbance, 3 or more of the following have persisted (4 if the mood is only irritable): ◦ Inflated self-esteem or grandiosity ◦ Decreased need for sleep ◦ More talkative or pressured speech ◦ Flight of ideas or subjective feeling of racing thoughts ◦ Distractibility ◦ Increased goal-directed activity or psychomotor agitation ◦ Excessive involvement in pleasurable activities that have a high potential for painful consequences 4

Hypomania • Unequivocal change uncharacteristic of person when not symptomatic • Observable by others known to patient • Absence of marked impairment in social or occupational functioning • Hospitalization not indicated • Not due to substance abuse, medication, or other medical condition 5

Mania • Behavior severe enough to cause marked impairment in occupational activities, usual social activities, or relationships • Necessitates hospitalization to prevent harm to self or others, or there are psychotic features • Symptoms not due to substance abuse, medications or other medical condition 6
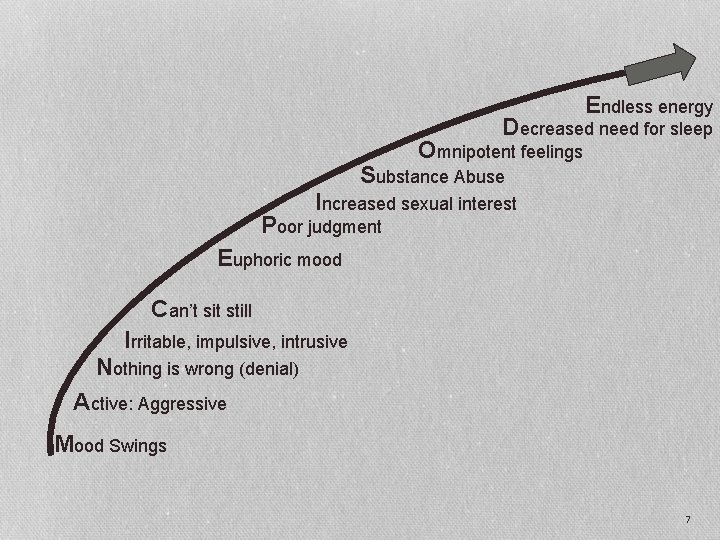
Endless energy Decreased need for sleep Omnipotent feelings Substance Abuse Increased sexual interest Poor judgment Euphoric mood Can’t sit still Irritable, impulsive, intrusive Nothing is wrong (denial) Active: Aggressive Mood Swings 7

8

Case Study • A patient was just admitted to your unit with bipolar disorder I and is in the manic state. • What symptoms might you expect to see? Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 9

Epidemiology • Lifetime prevalence of bipolar disorder in the United States is 5. 1% • Bipolar I – more common in males • Bipolar II – more common in females • Cyclothymia – usually begins in adolescence or early adulthood Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 10

50% have co-morbidities • Panic attacks • Substance abuse • Social Phobia • Specific Phobia • Borderline Personality disorder • Seasonal Affective disorder 11

Etiology • Biological factors • Genetic • Neurobiological • Neuroendocrine 12

Psychosocial & Environmental Factors • Stress • Education • Occupation • Economic status • Creativity 13

Assessment • Mood • Behavior • Appearance • Speech • Thought processes • Flight of ideas • Clang associations • Grandiosity • Cognitive functioning Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 14

Case Study (Cont. ) • What are some problems that can be avoided if your manic patient gets proper treatment? Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 15

Self-Assessment • Manic patient • Manipulative • Aggressively demanding • Splitting • Staff member actions • Frequent staff meetings to deal with patient behavior and staff response • Set limits consistently Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 16

Assessment Guidelines Bipolar Disorder • Danger to self or others • Need for protection from uninhibited behaviors • Need for hospitalization • Medical status • Coexisting medical conditions • Family’s understanding Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 17

Nursing Diagnosis Risk for suicide Risk for violence Ø Other-directed Ø Self-directed Risk for injury Defensive / Ineffective coping Disturbed thought process Situational Low Self-esteem 18

Outcomes Identification • Acute phase • Prevent injury • Continuation phase • Relapse prevention • Maintenance phase • Limit severity and duration of future episodes • Continuation of relapse prevention • Education for interpersonal strategies to improve relationships and quality of life Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 19

Planning • Acute phase • Medical stabilization • Maintaining safety • Self-care needs • Continuation phase • Maintain medication adherence • Psychoeducational teaching • Referrals • Maintenance phase • Prevent relapse Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 20

Implementation • Acute phase • Depressive episodes • Manic episodes • Continuation phase • Prevent relapse with follow-up care • Maintenance phase • Prevent recurrence Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 21

Intervention: Acute Phase • Communication • Structure in a safe milieu • Physiological safety • Self-care needs 22

Communication with Manic Patient • Use firm, calm approach • Use short and concise explanations • Remain neutral: avoid power struggles • Be consistent in approach and expectations • Firmly redirect energy into more appropriate areas • Act on legitimate complaints • Convey limits, consequences 23

Structure - Milieu • Low level of stimuli • Structured solitary activities or with staff • Redirect violent behavior • Minimize physical harm – medication, seclusion, restraints • Observe for medication side effects/toxicity • Protect from consequences of behavior • Such as giving away possessions, spending all money, disrobing 24

Interventions: Physiologic Safety/ Self-Care Needs • Monitor vital signs, I & O if indicated • Nutrition • Offer frequent mobile high calorie foods or protein drinks • Elimination • Sleep • Avoid caffeine, reduce stimulation, encourage rest, other sleep-inducing interventions • Hygiene • May need supervision, step by step reminders • Minimize choices 25

Bipolar Disorder Psychopharmacology • Mood stabilizers • Antipsychotics • Anxiolytics • Antidepressants 26

Pharmacological Interventions • Lithium carbonate • First-line agent • Therapeutic and toxic levels • Therapeutic blood level: 0. 8 to 1. 4 m. Eq/L • Maintenance blood level: 0. 4 to 1. 3 m. Eq/L • Toxic blood level: 1. 5 m. Eq/L and above • Takes 7 to 14 days to reach therapeutic levels in blood Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 27

Initial Treatment of Acute Mania Until Lithium Takes Effect • Antipsychotics • Slow speech • Inhibit aggression • Decrease psychomotor activity • Antipsychotic or benzodiazepine to prevent: • Exhaustion • Coronary collapse • Death 28

Lithium: Expected Side Effects • Blood level: <0. 4 to 1. 0 m. Eq/L • Signs • Fine hand tremor • Polyuria • Mild thirst • Mild nausea • General discomfort • Weight gain 29

Lithium: Expected Side Effects • Blood level: <0. 4 to 1. 0 m. Eq/L • Signs • Fine hand tremor • Polyuria • Mild thirst • Mild nausea • General discomfort • Weight gain 30

Lithium: Early Signs of Toxicity • Blood level: 1. 5 m. Eq/L • Signs • Nausea • Vomiting • Diarrhea • Thirst • Polyuria • Slurred speech • Muscle weakness 31

Lithium: Advanced Signs of Toxicity • Blood level: 1. 5 to 2. 0 m. Eq/L • Signs • • • Coarse hand tremor Persistent gastrointestinal upset Mental confusion Muscle hyperirritability Incoordination 32

Lithium: Severe Toxicity Blood level: 2. 0 to 2. 5 m. Eq/L Signs ◦ ◦ ◦ ◦ ◦ Ataxia Blurred vision Clonic movements Large output of dilute urine Seizures Stupor Severe hypotension Coma Death 33

Lithium: Severe Toxicity - Continued Blood level: >2. 5 m. Eq/L Signs ◦ ◦ ◦ ◦ ◦ Confusion Incontinence of urine or feces Coma Cardiac arrhythmias Peripheral circulatory collapse Abdominal pain Proteinuria Oliguria Death 34

Lithium: Major Long-Term Risks • Hypothyroidism • Impairment of kidneys’ ability to concentrate urine 35

Contraindications to Lithium • Cardiovascular disease • Brain damage • Renal disease • Thyroid disease • Myasthenia gravis • Pregnancy • Breastfeeding mothers • Children younger than 12 years 36

Patient and Family Teaching for Lithium Therapy • Effects of treatment • Need to monitor lithium blood levels • Side effects and toxic effects • Effects of dietary salt and dehydration • Check with physician before taking OTC medications • Take with food to decrease stomach irritation 37

Anticonvulsant Drugs • • • Valproate (Depakote, Depakene) Carbamazepine (Tegretol) Lamotrigine (Lamictal) Gabapentin (Neurontin) Topiramate (Topamax) Oxcarbazepine (Trileptal) Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 38

Antianxiety Drugs • Clonazepam (Klonopin) • Lorazepam (Ativan) • Atypical antipsychotics • Olanzapine (Zyprexa) • Risperidone (Risperdal) Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 39

Other Treatments • Electroconvulsive therapy (ECT) • • Severe manic behavior Rapid cycling (four or more cycles/yr) Paranoid, catatonic, destructive features Acutely suicidal behavior Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 40

Milieu Therapy: Seclusion Room or Restraints • Used in an emergency for patient when: • Clear risk of harm to patient or others • Patient's behavior has continued despite use of less restrictive methods to keep patient and others safe 41

Advanced Practice Interventions • Psychotherapy • Cognitive-behavioral therapy (CBT) • Interpersonal and social rhythm therapy Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 42

Evaluation • Evaluate outcome criteria • Reassess care plan • Revise care plan if indicated Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 43

Audience Response Questions 1. Which anticonvulsant medication might be prescribed for a patient with bipolar disorder? A. Divalproex sodium (Depakote) B. Clonazepam (Klonopin) C. Olanzapine (Zyprexa) D. Lithium (Lithobid) Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 44

Audience Response Questions 2. Lithium toxicity may result in which one of the following? A. Neuroleptic malignant syndrome B. Dystonia C. Blurred vision D. Akathisia • All Elsevier items and derived items © 2013, 2009 by Saunders, an imprint of Elsevier Inc. 45

Case Study (Cont. ) • Your patient with mania has been started on lithium. • What patient teaching about this medication should the nurse provide before the patient is discharged? Copyright © 2014, 2010, 2006 by Saunders, an imprint of Elsevier Inc. 46
- Slides: 46