Chapter 11 Gastrointestinal Drugs Dr Dipa Brahmbhatt VMD

Chapter 11 Gastrointestinal Drugs Dr. Dipa Brahmbhatt VMD Mp. H dbrahmbhatt@vettechinstitute. edu

Basic Anatomy and Physiology • The term gastrointestinal (GI) tract describes a long, muscular tube that begins at the mouth and ends at the anus. • Structures: – – – Oral cavity Esophagus Stomach Small intestine Large intestine • Structures vary from monogastric animals with simple stomachs to ruminant animals with multichambered forestomachs – Unobstructed and regulated flow
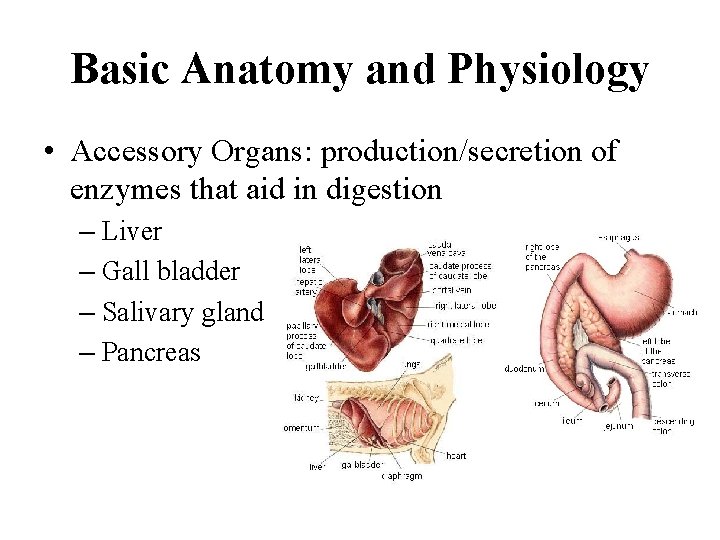
Basic Anatomy and Physiology • Accessory Organs: production/secretion of enzymes that aid in digestion – Liver – Gall bladder – Salivary gland – Pancreas
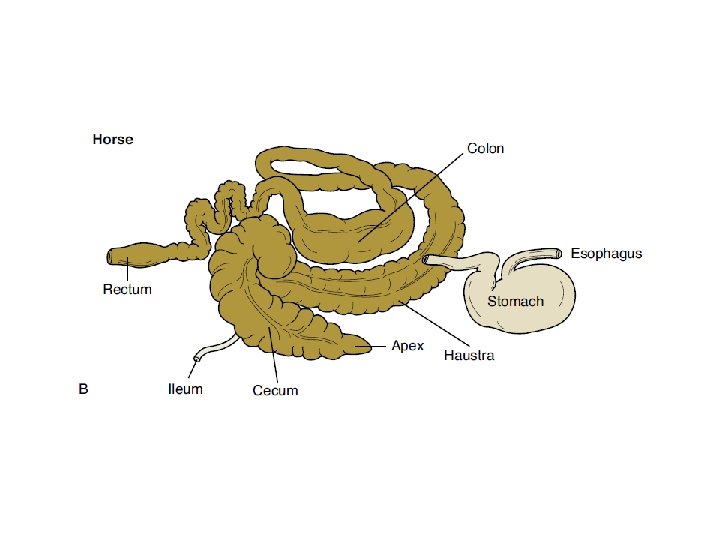
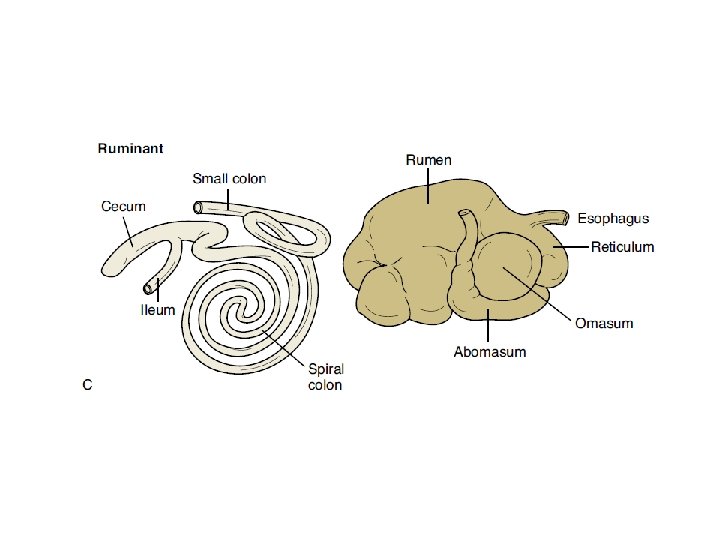
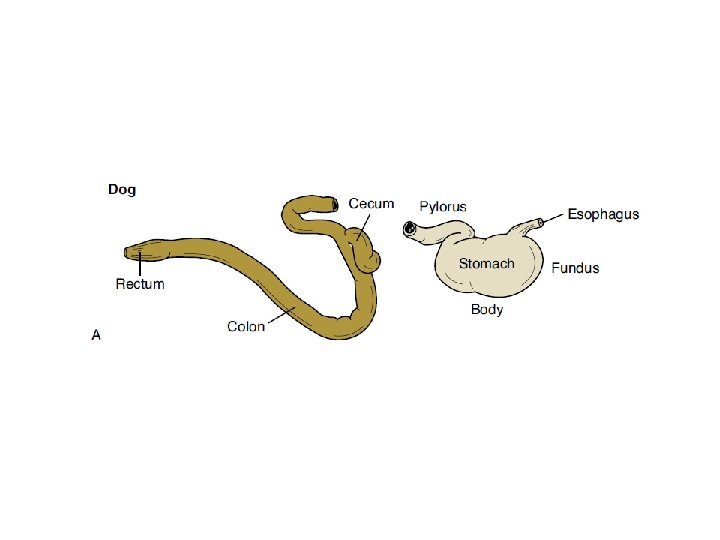
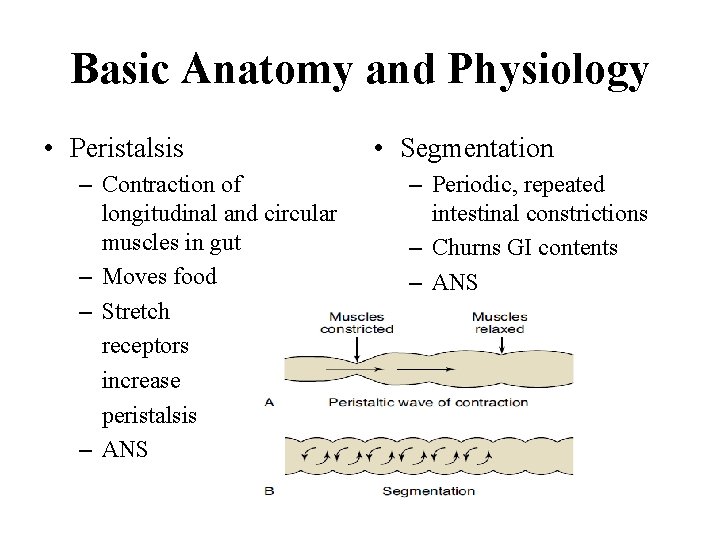
Basic Anatomy and Physiology • Peristalsis – Contraction of longitudinal and circular muscles in gut – Moves food – Stretch receptors increase peristalsis – ANS • Segmentation – Periodic, repeated intestinal constrictions – Churns GI contents – ANS

Autonomic Nervous System Sympathetic = “Fight or Flight” Parasympathetic = homeostatic Eat turkey and sleep it off
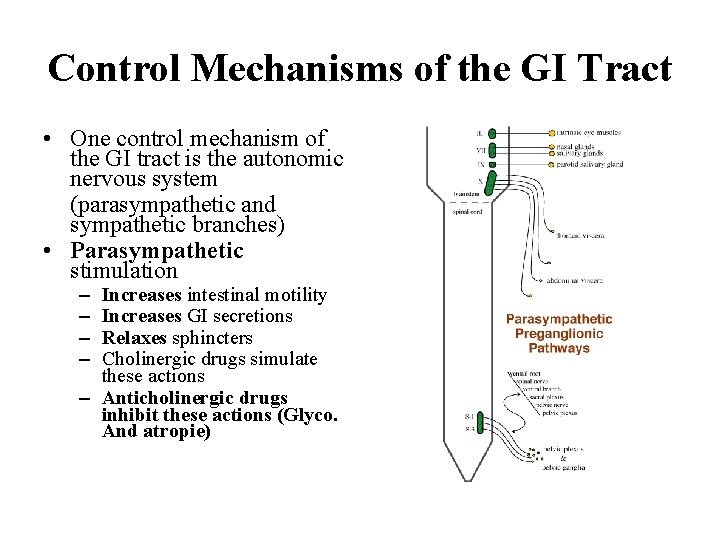
Control Mechanisms of the GI Tract • One control mechanism of the GI tract is the autonomic nervous system (parasympathetic and sympathetic branches) • Parasympathetic stimulation – – Increases intestinal motility Increases GI secretions Relaxes sphincters Cholinergic drugs simulate these actions – Anticholinergic drugs inhibit these actions (Glyco. And atropie)
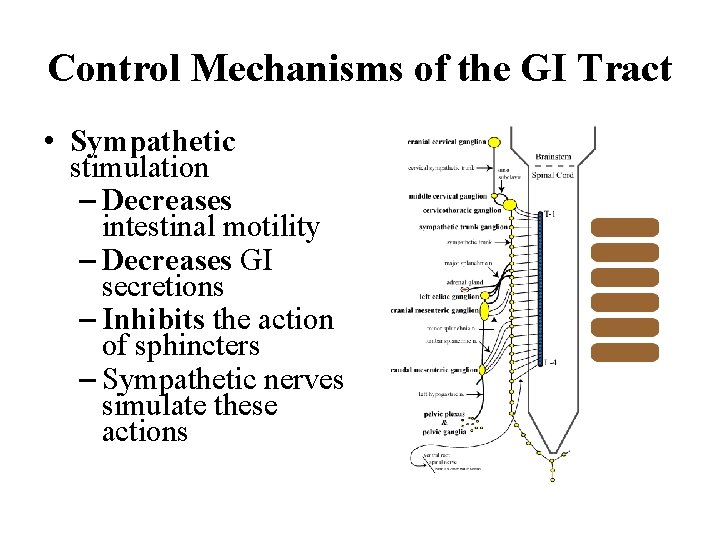
Control Mechanisms of the GI Tract • Sympathetic stimulation – Decreases intestinal motility – Decreases GI secretions – Inhibits the action of sphincters – Sympathetic nerves simulate these actions
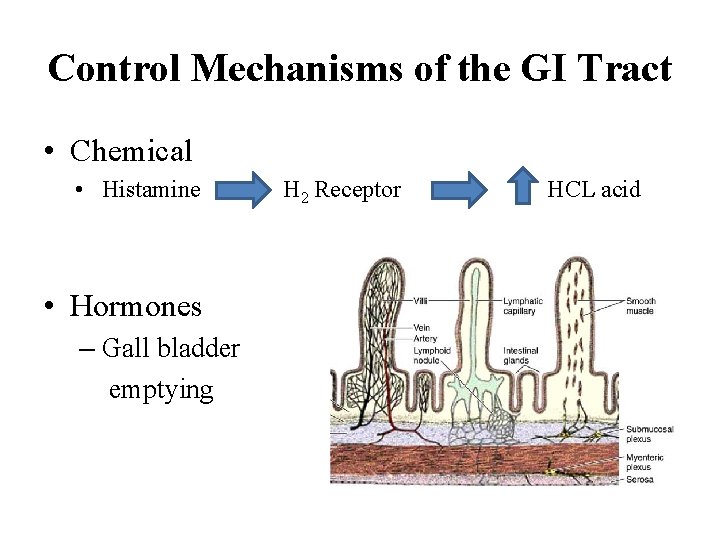
Control Mechanisms of the GI Tract • Chemical • Histamine • Hormones – Gall bladder emptying H 2 Receptor HCL acid

Gastrointestinal Disorders • Are the most common complains in vet. medicine • Underlying causes include: – Infectious sources • Gram negative bacterial endotoxin increases b. v. permeability, increased fluid loss – Dietary excess – Adverse drug effects – Systemic disease • Liver disease affects bile production and fat digestion
Gastrointestinal Disorders • These disorders result in clinical signs such as: – – – Diarrhea Constipation Vomiting Bloat Ulcer development Pain

Drugs Affecting the GI Tract • Antisialogues – Drugs that decrease salivary flow – Used to limit the flow of excess saliva, which often occurs secondary to anesthetic drug use • Examples include anticholinergics such as glycopyrrolate and atropine – These drugs can also affect peristalsis because they are also used to treat vomiting, diarrhea, and excess gastric secretion • Decreases intestinal motility • Decreases GI secretions • Does not relax sphincters


Glycopyrrolate (Robinul) and Atropine Use Glycopyrrolate in Pregnant animals it does not appreciably cross CNS or placenta Atropine comes in Two concentration: 0. 5 mg/m. L (injectable-SA) and 2. 0 mg/m. L (injectable-LA)

Diarrhea – Diarrhea: abnormal frequency and liquidity of fecal material due to GI tract unable to absorb fluid – Dehydration and electrolyte imbalance – Decrease uptake of nutrients – Muscle weakness – Acid-base disturbances – Causes • • • Infectious Foreign body Toxins Inflammatory Neoplasm
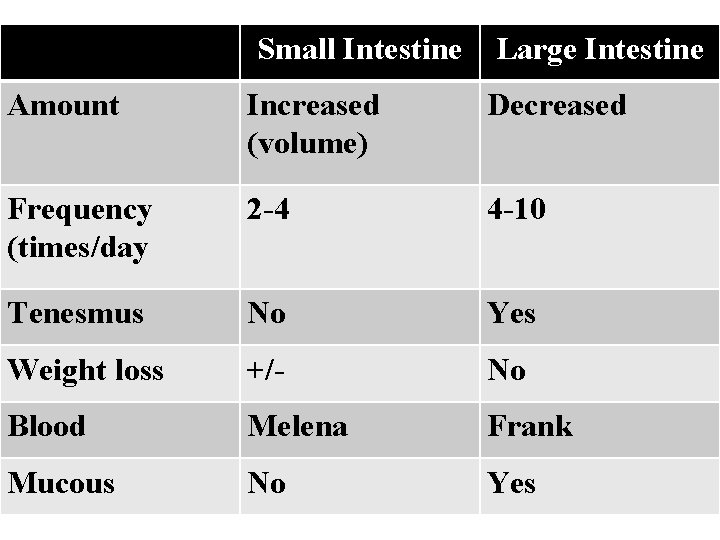
Small Intestine Large Intestine Amount Increased (volume) Decreased Frequency (times/day 2 -4 4 -10 Tenesmus No Yes Weight loss +/- No Blood Melena Frank Mucous No Yes

Antidiarrheals – Antidiarrheals are drugs that decrease peristalsis, thereby allowing fluid absorption from the intestinal contents – Examples: • • • Anticholinergics Protectants/adsorbents Opiate-related agents Probiotics Metronidazole
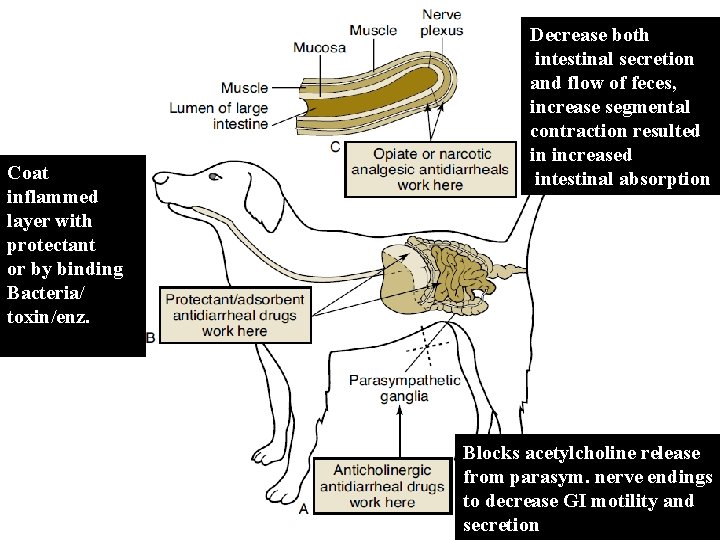
Coat inflammed layer with protectant or by binding Bacteria/ toxin/enz. Decrease both intestinal secretion and flow of feces, increase segmental contraction resulted in increased intestinal absorption Blocks acetylcholine release from parasym. nerve endings to decrease GI motility and secretion

Antidiarrheals Anticholinergics are used to treat tenesmus (colitis) and vomiting (colonic irritation) – Examples: • Atropine (Injectable. SA) • Aminopentamide (Centrine) • Isopropamide • Propantheline (Pro. Banthine) - IBD • Methscopolamine (Biosol-M) • Side effects of anticholinergics • Dry mouth • Constipation • CNS stimulation • Tachycardia • Pupillary dilation

Antidiarrheals - Anticholinergics

Antidiarrheals • Protectants & Adsorbents – Protectants coat inflamed intestinal mucosa with a protective layer – Adsorbents bind bacteria and/or digestive enzymes and/or toxins to protect intestinal mucosa from damaging effects – Examples: • Bismuth subsalicylate (bismuth + aspirin-like product) – DON’T USE IN CATS – Not specific – Pepto bismol, corrective mixture (w/opium) • Kaolin/pectin (Kao-forte, kaopectilin) • Activated charcoal (toxiban, liqui-char) – Side effects include constipation

Antidiarrheals • Opiate-related agents – Narcotic analgesics control diarrhea by decreasing both intestinal secretions and the flow of feces and increasing segmental contractions – Examples: • Diphenoxylate (Lomotil, lonox, diphenatol). C-V • Loperamide (Imodium): least CNS depression • Paregoric: C-III – Side effects include CNS depression (excitement: horses & cats), ileus, urine retention, bloat, and constipation

Antidiarrheals • Probiotics – Probiotics seed the GI tract with beneficial bacteria; use is based on theory that some forms of diarrhea are caused by disruption of the normal bacterial flora of the GI tract – Must be refrigerated to maintain the viability of the bacteria – Examples: • Plain yogurt with active cultures • Variety of trade-name products
Probiotics Lactobacillus spp. Enterococcus faecium Bifidobacterium spp.

Antidiarrheals • Metronidazole – A theory regarding the development of diarrhea is that anaerobic bacteria may increase due to disruption of normal GI flora – One way to treat this is to use an antibiotic effective against anaerobic bacteria – Metronidazole is an example of an antibiotic used to treat diarrhea
Metronidazole

Passage of feces is slowed or nonexistent

Laxatives – Loosens the bowel contents and encourages evacuation of stool – Evacuate without excessive straining – Treat chronic constipation from nondietary causes and movable intestinal blockages (hair balls) – Evacuate the GI tract before surgery, radiography, or diagnostic procedures – Cathartics are harsher laxatives: soft/watery stool, abd. cramping – Purgatives are harsh cathartics

Laxatives • Types of Laxatives include: – Osmotic – Stimulant – Bulk-forming – Emollients
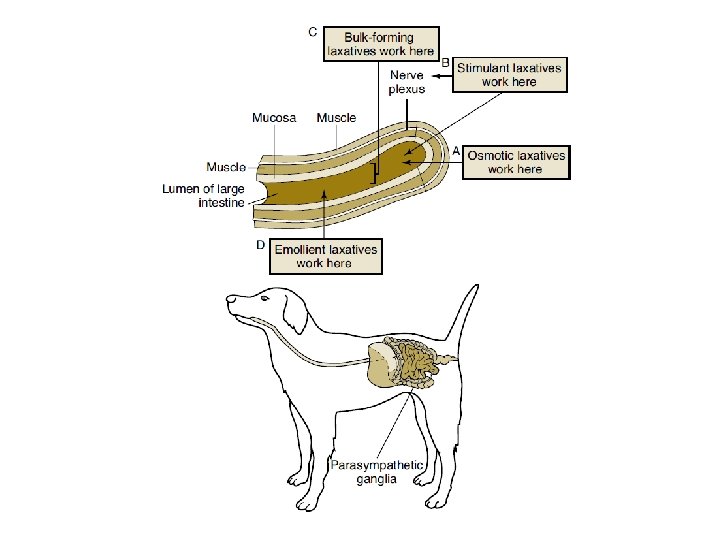

Laxatives • Osmotic • Pull water into the colon and increase water content in the feces, thereby increasing bulk and stimulating peristalsis • Are salts or saline product that may cause electrolyte imbalances if absorbed systemically Enema • Examples include: lactulose, sodium phosphate with per sodium biphosphate (Fleet Enema, Gent-L-Tip, rectum magnesium sulfate (Epsom salts), magnesium hydroxide (Milk of Magnesia) • NOT IN CATS, caution in heart and renal failure

Laxatives • Stimulant • Increase peristalsis by chemically irritating sensory nerve endings in the intestinal mucosa • Many are absorbed systemically and cause a variety of side effects • Examples include bisacodyl (Dulcolax): enteric coating, phenolphthalein, and castor oil (ricinoleic acid)

Laxatives • Bulk-forming • Substances that absorb water into the intestine, increase fecal bulk, and stimulate peristalsis, resulting in large, soft stool production (which tends to look normal) • Are not systemically absorbed, so side effects are rare • Examples include psyllium hydrophilic mucilloid, polycarbophil, and bran FREE ACCESS TO WATER

Laxatives • Emollients • Can be stool softeners (reduce stool surface tension and reduce water absorption through the colon), lubricants (facilitate the passage of fecal material, increasing water retention in stool), or fecal wetting agents (detergentlike drugs that permit easier penetration and mixing of fats and fluid with the fecal mass) • Examples include docusate sodium, docusate calcium, docusate potassium, and petroleum products

Horse s, Cattle rabbits an d don’t eject rats don’t vom Often vomiting can be controlled by NPO and correcting dehydration it Vomiting: expulsion of stomach (+/duodenal) through mouth
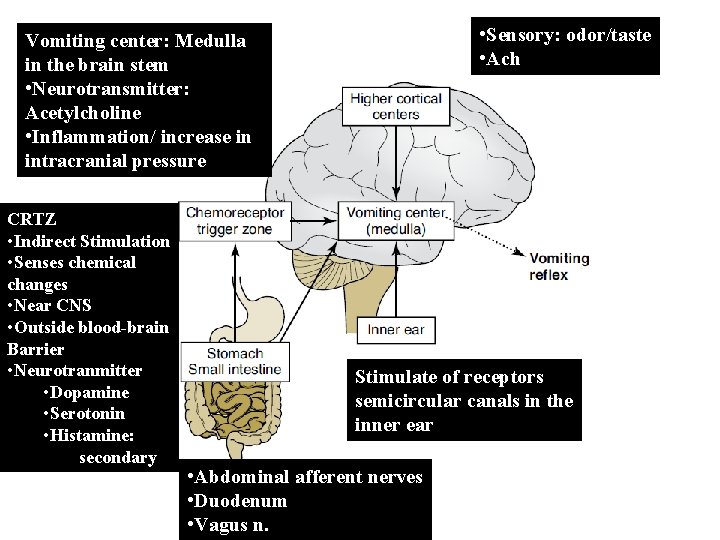
• Sensory: odor/taste • Ach Vomiting center: Medulla in the brain stem • Neurotransmitter: Acetylcholine • Inflammation/ increase in intracranial pressure CRTZ • Indirect Stimulation • Senses chemical changes • Near CNS • Outside blood-brain Barrier • Neurotranmitter • Dopamine • Serotonin • Histamine: secondary Stimulate of receptors semicircular canals in the inner ear • Abdominal afferent nerves • Duodenum • Vagus n.
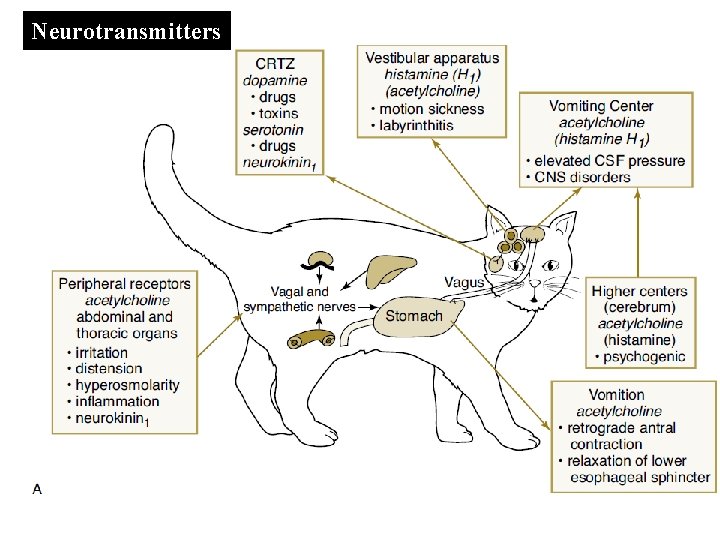
Neurotransmitters
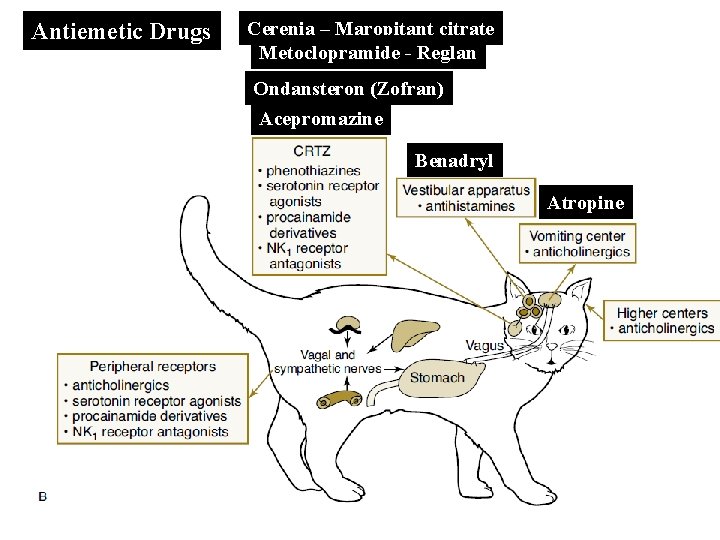
Antiemetic Drugs Cerenia – Maropitant citrate Metoclopramide - Reglan Ondansteron (Zofran) Acepromazine Benadryl Atropine

Antiemetics • Antiemetics – Drugs that control vomiting that help alleviate discomfort and help control electrolyte balance – Most are given parenterally, as the patient may vomit the medication before it can be absorbed through the GI tract – Examples: • • • Phenothiazine derivatives Antihistamines Anticholinergics Procainamide derivatives Serotonin receptor antagonists Neurokinin (NK 1) Receptor Antagonists

Antiemetics • Vomiting has many causes including: – Viral and bacterial infections, dietary indiscretion, food intolerance, surgery, pain, GI disease, kidney/liver failure, metabolic conditions (hypoadrenocorticism), CNS disorders or other drugs • The vomiting center of the brain have many inputs that tell it to activate including: – Equilibrium changes in the ear, responses due to pain or fear, intracranial pressure changes, vagus nerve stimulation in the GI tract, and activity in the chemoreceptor trigger zone

Antiemetics • Phenothiazine derivatives (vasodilation, hypotension) • Inhibit dopamine in the chemoreceptor trigger zone, thus decreasing the stimulation to vomit • Side effects include hypotension and sedation • Don’t use with epileptics, vomiting animals or with abnormal GI motility • Hydration has to be good • Examples: – – Acepromazine Chlorpromazine Prochlorperazine Perphenazine

Antiemetics • Antihistamines • Controls vomiting when the vomiting is due to motion sickness, vaccine reactions, or inner ear problems • Work by blocking input from the vestibular system to the CRTZ • A side effect is sedation • Examples: – Trimethobenzamide (Tigan) – Dimenhydrinate (Dramamine) – Diphenhydramine (Benadryl)

Antiemetics • Anticholinergics • Block acetylcholine peripherally, which decreases intestinal motility and secretions • May decrease gastric emptying (which may increase the tendency to vomit) • Side effects include dry mouth, constipation, urinary retention, and tachycardia • Examples: – Aminopentamide – Atropine – Propantheline

Antiemetics • Procainamide derivatives • Work centrally by blocking the CRTZ (dopamine antagonist) and peripherally by speeding gastric emptying, strengthening cardiac sphincter tone, and increasing the force of gastric contractions • Should not be used in animals with GI obstructions, GI perforation, or GI hemorrhage, (Due to peripheral effects: gastric motility) or seizures

Antiemetics • Procainamide derivatives • An example used in veterinary medicine is metoclopramide (Reglan) • PO/SQ/IM/IV • Stimulates motility of upper GI w/o gastric/biliary/pancreatic secretions (used with chemotherapy agents in humans)

Antiemetics • Serotonin receptor antagonists • Work selectively on 5 -HT 3 receptors, which are located peripherally (Vagus n. ) and centrally (CRTZ) • Work on theory that some chemicals (chemotherapeutic agents/ propofol) cause vomiting because they increase serotonin release from small intestinal cells • $$ and GI upset • Examples: – Ondansetron (Zofran) – Dolasetron (Anzemet)

Extra label in cats Antiemetics Oral / SQ • Neurokinin receptor antagonists – Work on NK 1 receptors located in the center of the brain – Work by inhibiting substance P, the key neurotransmitter involved in vomiting – Peripheral and central mediated vomiting • Maropitant citrate (Cerenia®) – Used to prevent acute vomiting and motion sickness – Side effects include: • Pain at the injection site, hypersalivation, pre-travel vomiting (when given at high doses) and diarrhea

Maropitant (Cerenia®)
- Slides: 50