Chapter 11 Emergencies By Jahangir Moini M D

Chapter 11 Emergencies By Jahangir Moini, M. D. , M. P. H. and Morvarid Moini, D. M. D. , M. P. H. © 2017 Jahangir Moini

Overview �Medical emergencies involve acute illnesses or injuries �Health care professionals must stay calm, think clearly They must be trained and ready �Fast treatment prevents serious disabilities and death © 2017 Jahangir Moini

Emergency and urgent care �Emergency care – immediate services for sudden, serious conditions Also used for uninsured, underinsured people not actually having an emergency �Medical emergency defined by the prudent layperson standard © 2017 Jahangir Moini

Prudent layperson standard �A condition with acute, severe symptoms that a prudent layperson, with average health/medical knowledge, could expect the lack of quick medical attention to result in: I. Placing health of individual, or unborn child, in jeopardy II. Serious impairment of bodily functions III. Serious dysfunction of a bodily organ or part © 2017 Jahangir Moini

Emergent care �Trauma, other types of care Classified by triage levels �Using the emergency severity index (ESI) � 5 levels of ESI Classified by immediacy of need for treatment © 2017 Jahangir Moini
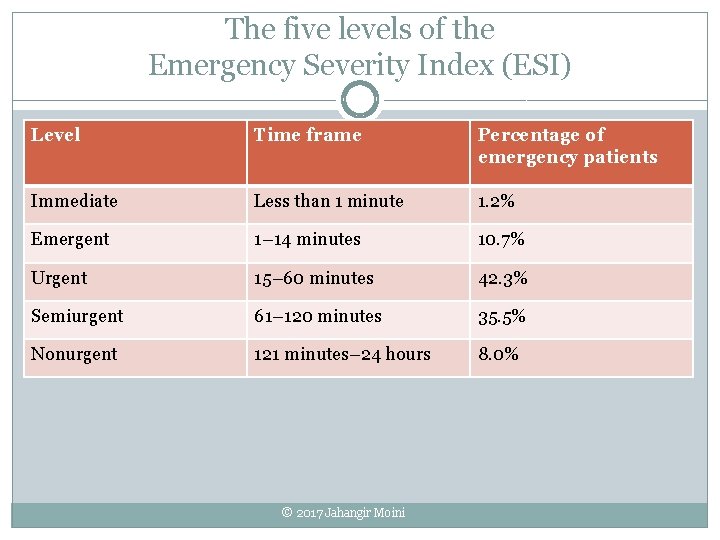
The five levels of the Emergency Severity Index (ESI) Level Time frame Percentage of emergency patients Immediate Less than 1 minute 1. 2% Emergent 1– 14 minutes 10. 7% Urgent 15– 60 minutes 42. 3% Semiurgent 61– 120 minutes 35. 5% Nonurgent 121 minutes– 24 hours 8. 0% © 2017 Jahangir Moini

Emergency and urgent care � 2. 2% of patients at an E. R. require no triage �All presenting patients must be: Screened and evaluated Given necessary stabilizing treatment Admitted to hospital if necessary � Regardless of ability to pay for services �Less than 1 in 4 patients require hospitalization © 2017 Jahangir Moini

Urgent care �Illnesses, injuries, conditions serious enough to require care right away �A type of ambulatory care Patient can walk, unassisted or assisted, into facility Usually involves: � Physicians � Nurse practitioners � Physician assistants © 2017 Jahangir Moini

Triage �When determining which patients require treatment most: Wash hands Put on gloves, personal protective equipment Quick assessments based on injuries Classify patients as: � Emergent � Urgent � Non-urgent � Deceased Label patients using disaster tags and pens © 2017 Jahangir Moini

Labeling patients during triage �#1: Emergent – immediate treatment Hemorrhaging, shock, etc. �#2: Urgent – basic first aid within a few hours Lacerations that can be dressed, sutured later �#3: Non-urgent – provide empathy, refreshments Non-critical �#4: Deceased – moved to separate area Identified later © 2017 Jahangir Moini

Natural and man-made disasters �Disaster: Anything causing damage, death, poor health and services, serious ecological destruction � Natural or man-made � Result in human suffering and need for help Man-made disasters: � Use of chemical weapons � Industrial accidents © 2017 Jahangir Moini

Bioterror �Germs, or other biological substances, released to harm others: Tularemia Anthrax (killed 5 people in 2001) Smallpox Botulinum toxin Bubonic plague Viral hemorrhagic fevers (such as Ebola) © 2017 Jahangir Moini

Complex humanitarian emergency (CHE) �Due to civil wars, other man-made disasters: Complex, multi-party, intra-state conflict � Results in a disaster affecting human security Deaths of many people Displaced people; political refugees © 2017 Jahangir Moini

Examples of man-made and natural disasters Man-made disasters Natural disasters Liberia – civil war – 500, 000 displaced San Francisco – earthquake – 9 deaths Nepal – conflicts – 200, 000 displaced New Orleans – hurricane – more than 1, 200 deaths New York City, Washington, D. C. – terrorist attacks – more than 3, 000 deaths Pakistan – flooding – more than 1, 600 deaths Gulf of Mexico – oil spill – 11 deaths USA – hurricane – 56 deaths; Philippines – tropical storm – 1, 268 deaths Syria – civil war – 6. 5 million displaced internally, 2. 8 million refugees Pakistan – avalanche – 140 deaths; Russia – flooding – 172 deaths; USA - hurricane – more than 100 deaths Libya – conflicts – 80, 000 displaced Philippines – earthquake – 144 deaths; Philippines – typhoon – 4, 011 deaths, 1, 602 missing Paris – terrorist attack – 129 deaths, © 2017 Jahangir India/Pakistan – flooding – 557 deaths; Moini 350 injuries China – earthquakes – 617 deaths

Natural disasters �More predictable where there are earthquakes, hurricanes, typhoons, flooding, volcanic eruptions West Coast of USA: � Trained disaster teams are ready to act � Help people prepare, reduce impact on health © 2017 Jahangir Moini

Disaster preparedness plan �Identification of the area’s vulnerabilities �What might occur, and how likely �Explain roles people will play �Train first responders, disaster management teams © 2017 Jahangir Moini

Long-term disaster preparedness �Improve construction of infrastructure �Determine best methods of bringing assistance �Build temporary, strong buildings to serve as hospitals �Create lists of most-needed items © 2017 Jahangir Moini

Impact of natural disasters �Long-term effects due to: Toxins Pathogens Unsanitary conditions � 90% of related deaths occur in poorer countries Due to lower-quality construction © 2017 Jahangir Moini

Health care during natural disasters �Differs based on type of disaster People displaced from homes Water, food supplies unsafe; famine occurs Mental health problems due to shock Infections, epidemics Health conditions need quick assessment Additional shelter may be needed © 2017 Jahangir Moini

Health care during natural disasters �Providers may also be displaced �Health systems may collapse or be ineffective �Theft of medical supplies, equipment �Inadequate drug supplies �Reduced access to care, or lower quality © 2017 Jahangir Moini

Emergency procedures �Care given before trained personnel arrive: Assess environment � Safe to approach victim; monitor scene safety � Call for help or EMS as soon as possible Accuracy with 9 -1 -1 operator Obtain consent � Obtain consent if victim is conscious Identify yourself � Work with parents, guardians of children © 2017 Jahangir Moini

Emergency procedures Determine what has occurred � Ask victim what happened, or look for clues: Medications, containers, substances, alert bracelets, other victims � Inform EMS of what you find Follow standard precautions � Must occur if in contact with body fluids � Carry gloves, barrier devices, first aid kit © 2017 Jahangir Moini

Emergency procedures Get help from others � Most experienced assists victim � Others call for help Direct traffic, move onlookers, search for clues, assist others Keep victim in one place � Spine straightly aligned � Only turn body as one unit; support limbs Remain calm � Stay calm at all times � Reassure others � Think clearly © 2017 Jahangir Moini

Good Samaritan Act �Protects caregivers and rescuers when helping in emergencies No gross negligence Nothing willfully done to harm victim Generally, prevents caregivers/rescuers from liability while trying to help Civil, other damages not brought against them © 2017 Jahangir Moini

Cardiopulmonary resuscitation (CPR) �CPR given when: Victim not breathing, does not have a pulse �Immediate CPR can save a life: Chest compressions With or without rescue breathing � Based on training © 2017 Jahangir Moini

Cardiopulmonary resuscitation (CPR) �Chest compressions circulate oxygenated blood Until heartbeat, breathing are restored �Rescue breathing provides oxygen to lungs �All citizens should receive training in CPR Increases likelihood of saving more lives © 2017 Jahangir Moini

Steps of CPR �Is victim breathing? If not – chest compressions immediately �Check for pulse only if you are trained �Untrained people: give chest compressions only No rescue breathing unless trained © 2017 Jahangir Moini

Steps of CPR �Chest compressions: Place heel of one hand on sternum (breastbone) Other hand directly on top of first hand Position body above victim’s chest Rapid, hard compressions (100 -120 per minute) Chest should depress at least 2 inches with each Allow chest to rise between compressions © 2017 Jahangir Moini

Steps of CPR �If trained, after 30 compressions: Tilt victim’s head back Lift the chin Give 2 rescue breaths (use barrier device if there) � If no device, cover victim’s mouth tightly with yours � Pinch victim’s nose closed � Give 2 breaths, one second each Chest should rise with each breath © 2017 Jahangir Moini

Steps of CPR �Cycles of: 30 chest compressions, 2 breaths, should continue Until: � The victim starts breathing, or � EMS personnel arrive © 2017 Jahangir Moini
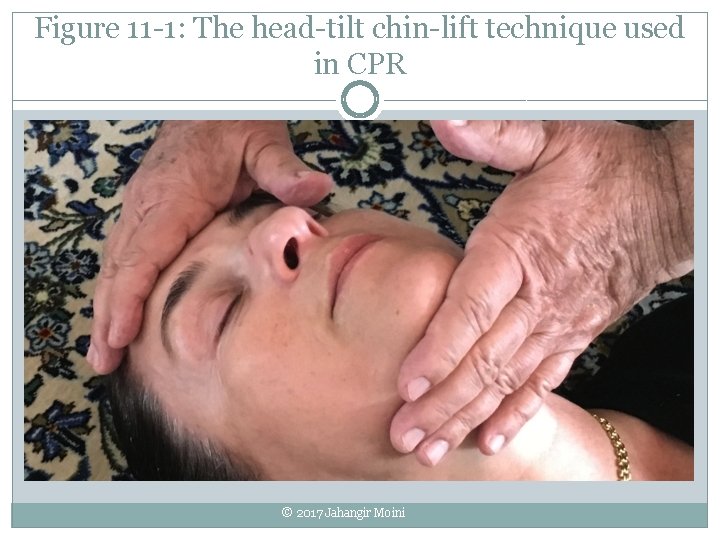
Figure 11 -1: The head-tilt chin-lift technique used in CPR © 2017 Jahangir Moini

Automatic external defibrillator (AED) �Should be used, with CPR, if victim is: Not breathing normally Unresponsive �AED: portable machine, monitors heart rhythm Introduces an electric shock to restore normal rhythm © 2017 Jahangir Moini

Automatic external defibrillator (AED) �Simple to use without training: Determine responsiveness (shaking; “Are you okay? ”) If not breathing: � Begin CPR immediately as AED is brought � Ask for help from others � Turn on AED, follow instructions � Another person can continue CPR as you prepare © 2017 Jahangir Moini

Automatic external defibrillator (AED) �Remove victim’s shirt �Prepare chest: Dry the skin Remove transdermal patches Clean, trim excessive hair �Remove metal necklaces or underwire bras �Verify no implanted pacemaker or similar device �Check for medical alert bracelets, body piercings © 2017 Jahangir Moini

Automatic external defibrillator (AED) �Remove electrode pad paper backings �Place pads per instructions �Connect wires from pads to AED if needed �As AED analyzes heart rhythm: Follow instructions Do not touch victim Stop CPR © 2017 Jahangir Moini

Automatic external defibrillator (AED) �If shock is necessary: Make sure no one touches victim or anything victim is lying on � Except for floor or ground �Some AEDs give shock automatically Some require you to press a button �Keep following instructions until EMS arrives © 2017 Jahangir Moini

Figure 11 -2: Automatic external defibrillator © 2017 Jahangir Moini

First aid �Emergency care after an accident or sudden illness �Minimizes harm until a physician can intervene �Everyone should receive first aid training �Golden rule: Do no further harm Do not attempt anything in which you are unskilled Seek help immediately instead © 2017 Jahangir Moini

Seizures �Uncontrolled muscle movements �Abnormal sensations �Partial or complete loss of consciousness �Caused by abnormal discharges of electrical signals in the brain �May signify: Epilepsy Drug toxicity Head injuries Other conditions © 2017 Jahangir Moini

Seizures �Symptoms before a seizure: Bitter or metallic taste in mouth Visual abnormalities � Flashing lights � Hallucinations � Blurred vision �Symptoms during a seizure: Muscle twitching or tightening Sudden loss of muscular control �Often, no memory of a specific period of time © 2017 Jahangir Moini

Seizures �To treat seizure victim: Move harmful objects away Protect neck and spine Check responsiveness, airway, breathing Help victim roll on one side so that vomit, other secretions can drain from mouth © 2017 Jahangir Moini
Shock �Sudden reduction in blood flow �Deprives vital organs of oxygen �Related to: Heart disease Hemorrhage Infections Other conditions �If tissue and organ damage becomes severe: Shock is irreversible Victim will die © 2017 Jahangir Moini

Signs and symptoms of shock �Low blood pressure �Weak, rapid pulse �Restless or signs of fever �Nausea �Thirst �Cool, clammy, pale skin Lips, earlobes appear bluish in color © 2017 Jahangir Moini

Treating shock �Call EMS immediately �Monitor victim’s airway; keep it open �Control bleeding �Administer oxygen (if directed by physician) �Immobilize victim to protect spine �Splint fractured bones �Cover victim with a blanket, especially if cold �Elevate legs and feet to help circulation © 2017 Jahangir Moini

Diabetic emergencies �Dysregulation of blood sugar: Hypoglycemia (low blood sugar) Hyperglycemia (high blood sugar) � Both can cause coma and death if untreated �Causative factors: Incorrect amount of synthetic insulin Excessive or inadequate food or exercise Physical stress (cold, flu, other illness) Mental or emotional stress © 2017 Jahangir Moini

Hypoglycemia �Occurs more quickly than hyperglycemia �Hunger, sweating, confusion, pallor, lack of coordination �Give sweetened drink or snack Usually effective in 5 to 15 minutes �Immediate treatment required if: Victim becomes unconscious � Glucagon injection or � Emergency department treatment © 2017 Jahangir Moini

Hyperglycemia �“Fruity” smell to the breath �Extreme thirst or hunger, extreme urination �Vomiting �Flushed skin �Confusion �Rapid pulse © 2017 Jahangir Moini

Hyperglycemia �Is the person diabetic? Insulin injection; assist if needed Have another person call EMS Remain with the person Monitor vital signs © 2017 Jahangir Moini
Fainting �Brief loss of consciousness not caused by trauma �Usually sudden �Often due to low blood sugar or excessive standing �Orthostatic hypotension Fainting after sitting, then standing up too quickly �Loss of consciousness also occurs after a head injury Such as a concussion © 2017 Jahangir Moini

Fainting �Warning signs: Dizziness, nausea, weakness, blurred vision �Help victim lie on the floor, face up Legs elevated above heart Loosen clothing so breathing is not restricted Turn head to one side to keep airway clear �Victim should awaken in under 5 minutes If not, call EMS © 2017 Jahangir Moini

Fractures �Broken bones, usually due to external injury �Also occur in thin or brittle bones from osteoporosis �Closed fractures – skin not broken �Open fractures – bone breaks through skin �Signs: Pain Swelling Loss of function Deformation of affected area © 2017 Jahangir Moini

Fractures �Immobilize broken bone with a splint Splints made from twigs, boards Attached with strips of cloth Check circulation so that splint is not too tight �Never attempt to realign bones �Cover open fractures with dressings before immobilizing Do not wash the area © 2017 Jahangir Moini
Figure 11 -3: Immobilizing a broken bone using a splint © 2017 Jahangir Moini
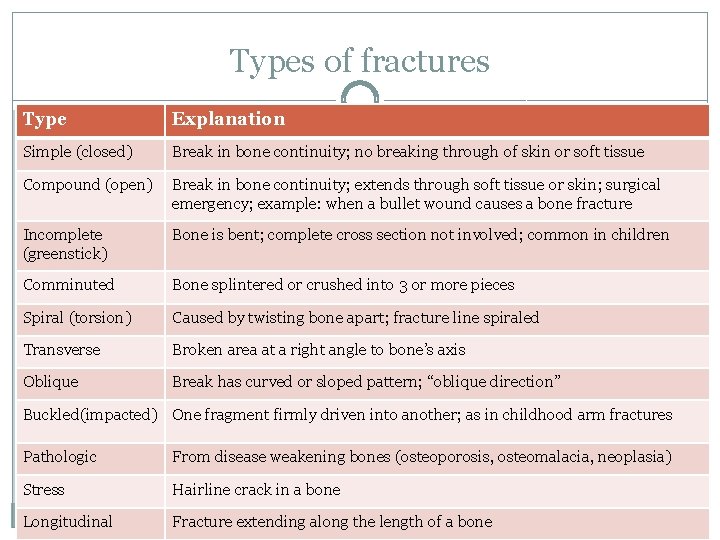
Types of fractures Type Explanation Simple (closed) Break in bone continuity; no breaking through of skin or soft tissue Compound (open) Break in bone continuity; extends through soft tissue or skin; surgical emergency; example: when a bullet wound causes a bone fracture Incomplete (greenstick) Bone is bent; complete cross section not involved; common in children Comminuted Bone splintered or crushed into 3 or more pieces Spiral (torsion) Caused by twisting bone apart; fracture line spiraled Transverse Broken area at a right angle to bone’s axis Oblique Break has curved or sloped pattern; “oblique direction” Buckled(impacted) One fragment firmly driven into another; as in childhood arm fractures Pathologic From disease weakening bones (osteoporosis, osteomalacia, neoplasia) Stress Hairline crack in a bone Longitudinal Fracture extending along the length of a bone © 2017 Jahangir Moini

Sprains �Torn ligament fibers: Cause a joint to become loose, painful, swollen Sprained joints function unless completely torn �Apply cold compresses quickly, every 3– 4 hours 15– 20 minutes each time No ice directly onto skin Elevate sprained limb �Contact physician: Severe pain Loss of function Impaired circulation below injury Area is misshapen © 2017 Jahangir Moini

Strains �Muscle fibers suddenly torn during exertion �Also known as pulled muscles �Victim feels a sudden tearing sensation Followed by pain and swelling �Treated the same way as sprains © 2017 Jahangir Moini

Wounds �Damage to soft tissues due to violence or trauma �Clean area, protect from further damage �Include tears or open areas anywhere on body �Do not clean large wounds Do not remove embedded objects Okay to remove loose debris �Sucking wound: Bubbling from neck or chest Difficulty breathing Must be sealed quickly © 2017 Jahangir Moini

Wounds �Amputation: Part of the body is severed Give first aid �If body part found, save severed part for reattachment Rinse it, wrap in wet cloth, place in a container Place container into another that has ice and water No ice directly on the severed part Put patient’s name and time of accident on container Transport amputated body part with patient © 2017 Jahangir Moini

Burns �Caused by fire, heat, chemicals, electric current, radiation �Severity determined by size, depth, location First-degree (superficial) � Epidermis Second-degree (partial-thickness) � Burn only; skin is red, dry extends to dermis; skin is red, wet, painful, swollen, blistered Third-degree (full-thickness) � Burn extends into deeper tissues; all skin layers � Other structures destroyed; skin is red, brown, black, or charred © 2017 Jahangir Moini
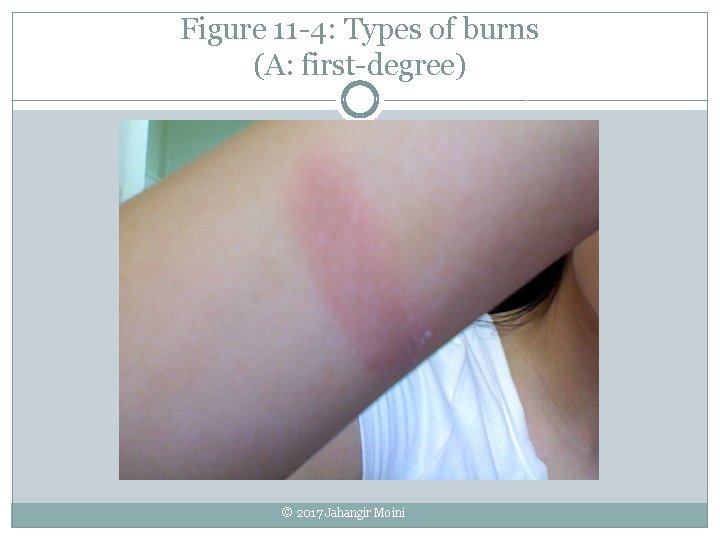
Figure 11 -4: Types of burns (A: first-degree) © 2017 Jahangir Moini
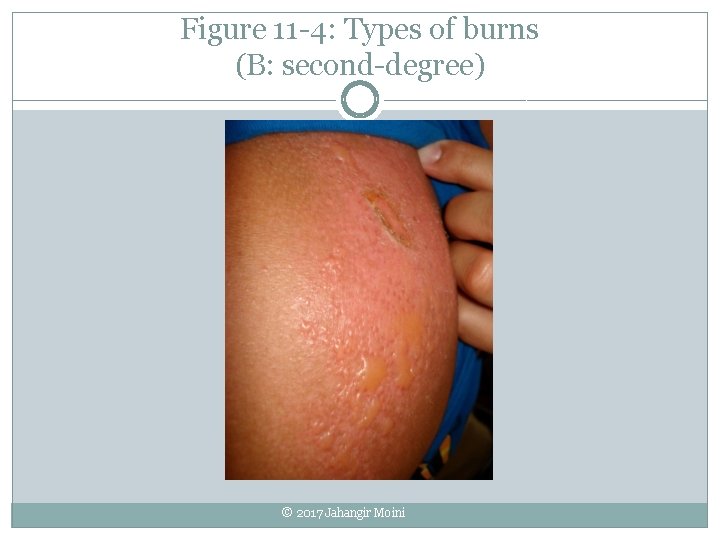
Figure 11 -4: Types of burns (B: second-degree) © 2017 Jahangir Moini
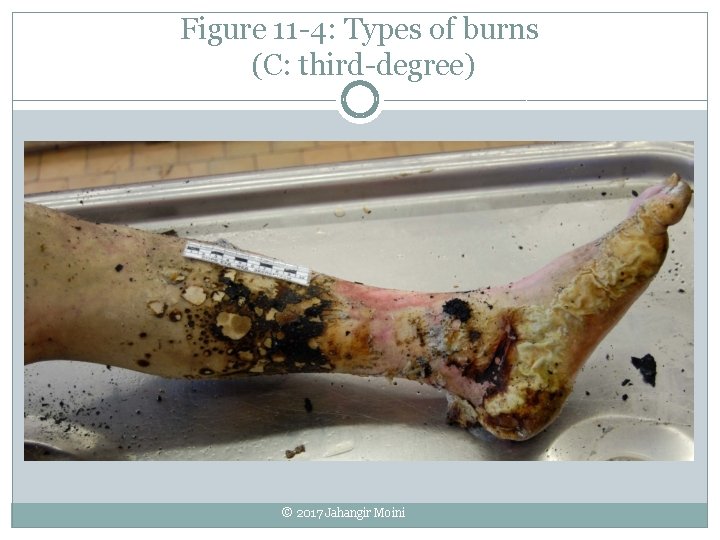
Figure 11 -4: Types of burns (C: third-degree) © 2017 Jahangir Moini

Burns �Amount of pain does not determine severity Deeper burns can be painless due to destruction of nerve endings �Cool burned area Cover with clean, dry dressings �Run cool water over burn for several minutes Or immerse area in cool water �Ice not be applied except for minor first-degree burns Do not break blisters © 2017 Jahangir Moini

Burns �Apply bandages loosely; no cotton dressings �Prevent victim from becoming chilled �Assess for respiratory damage Discolored areas of nose, mouth �Radiation burn Usually a sunburn Also linked to: � Electromagnetic radiation � Radio frequency energy � UV light � Ionizing radiation © 2017 Jahangir Moini

Burns �Chemical burns Move victim to well-ventilated area away from fumes Use cool water to flush burn away from the body If eyes are burned: � Flush continuously with cool water � If one eye is burned, flush from inner to outer aspect So that other eye will not become burned by chemical © 2017 Jahangir Moini

Burns �Electrical burns Never touch victim if still in contact with live wire Turn off electrical power first Only apply clean, dry dressing and prevent chilling Do not move victim because of other possible injuries © 2017 Jahangir Moini
Bleeding �Occurs from damage to blood vessels �Heavy bleeding = hemorrhaging �External bleeding: Blood drains out of body through break in skin Indicates damage to tendons or muscles Loss of sensation distal to wound = nerve damage First aid needed if bleeding does not stop on its own © 2017 Jahangir Moini
Bleeding �Elevate bleeding limb above heart level Unless this causes discomfort, or neck or back is injured �Apply direct pressure Use clean cloth or sterile dressing, once soaked: � Leave in place, cover with another dressing � Do not look under dressing If still bleeding after 15 minutes of direct pressure: Use pressure-point bleeding control � Brachial artery for arms, femoral artery for legs © 2017 Jahangir Moini

Bleeding �Arterial bleeding Bright red, spurts out with every heartbeat May be life-threatening �Venous bleeding Darker, flows evenly; still significant blood loss �Follow universal precautions for all bleeding Call EMS if heavy or other injuries are suspected © 2017 Jahangir Moini

Bleeding �Tourniquets Rarely used in emergencies – potential for additional harm Tight bands placed around arms or legs to stop bleeding from injuries below �Internal bleeding – call EMS quickly: More difficult to detect; may signify serious injury � Blood in stool, urine, vomit, from vagina � Distention � Tenderness � Nausea � Confusion � Weakness � Decreased consciousness © 2017 Jahangir Moini

Bleeding �Possible internal bleeding: Give no food or liquids to patient Place patient on back, knees elevated, pillow under head Cover with blanket for abdominal discomfort Treat patient for shock, stay nearby Apply CPR if required © 2017 Jahangir Moini

Figure 11 -5: Place emergency patients in the shock position, unless they have spinal injury © 2017 Jahangir Moini

Hypothermia � Caused by excessively cold temperatures, wet clothing, or immersion in cold water � Body temperature drops below normal Mild: Cold skin � Shivering � Lack of coordination � Severe: Slurred speech � Drowsiness � Difficulty seeing � Irrational, uncooperative behavior � Slowed heart rate � © 2017 Jahangir Moini

Hypothermia �Untreated severe hypothermia = coma, death �Rescue breathing may be required �Replace wet clothes with loose, dry clothes �No direct heat, use insulated blankets or aluminum foil �Warm, sweet fluids may be administered © 2017 Jahangir Moini

Hyperthermia �Due to very warm temperatures, high humidity �Body temperature raises above normal �Excessive perspiration, loss of salt, dehydration �Aggravated by some conditions and medications © 2017 Jahangir Moini

Hyperthermia �Other causes: Excessive exercise, obesity, alcohol �Heat stroke – most severe form; life-threatening Hot skin, confusion, weakness, seizures, pupil constriction Rapid pulse and breathing, possible unconsciousness � Call EMS immediately, avoid giving any liquids � If no EMS, immerse in cold water, monitor alertness, pulse, respirations �Other forms: heat exhaustion, heat cramps © 2017 Jahangir Moini
- Slides: 76