Chapter 11 57 By Dominique Stephanie Lauryn White

Chapter 11: 57 By Dominique, Stephanie, Lauryn

White Blood Cells 11 -5 - Circulate for only a short portion of their life-span. - Travel through the loose and dense connective tissue. - When an injury is detected the WBCs leave the bloodstream and immediately go to the injured area.
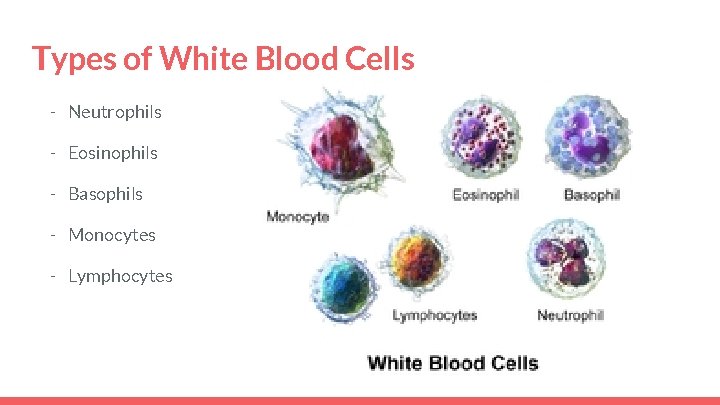
Types of White Blood Cells - Neutrophils - Eosinophils - Basophils - Monocytes - Lymphocytes
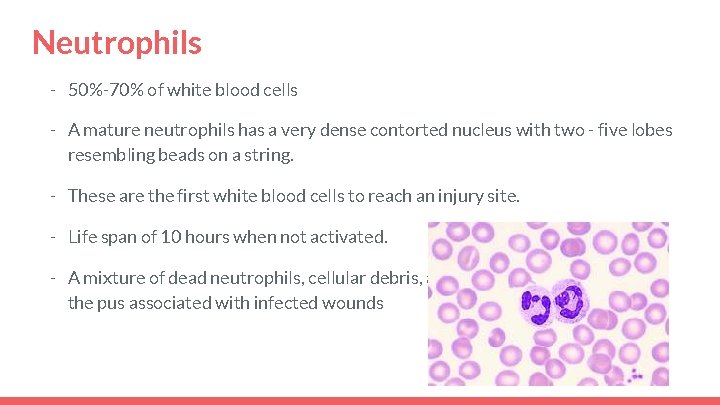
Neutrophils - 50%-70% of white blood cells - A mature neutrophils has a very dense contorted nucleus with two - five lobes resembling beads on a string. - These are the first white blood cells to reach an injury site. - Life span of 10 hours when not activated. - A mixture of dead neutrophils, cellular debris, and other waste products form the pus associated with infected wounds

Eosinophils - They were named because of their granules that stain darkly with the red dye eosin - Usually represents 2%-4%circulating white blood cells - Similar in size to Neutrophils - Attack objects coated with antibodies - Numbers increase dramatically during a parasitic infection or an allergic reaction.

Basophils -Have numerous granules that stain darkly with basic dyes. - In a standard blood smear the granules are purple or blue - The cells are smaller than eosinophils and neutrophils - They are relatively rare, accounting for less than 1% of the circulating white blood cell population. - Migrate to sites of injury and cross the capillary wall to accumulate within damaged tissue - The granules contain heparin which prevents blood clotting and histamine which enhances the local inflammation initiated by mast cells
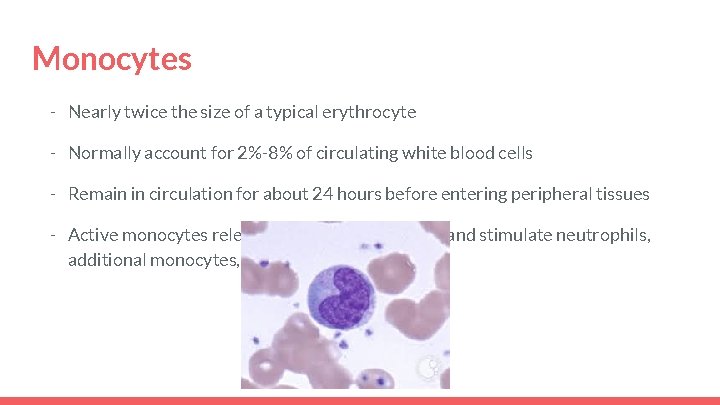
Monocytes - Nearly twice the size of a typical erythrocyte - Normally account for 2%-8% of circulating white blood cells - Remain in circulation for about 24 hours before entering peripheral tissues - Active monocytes release chemicals that attract and stimulate neutrophils, additional monocytes, and other phagocytes
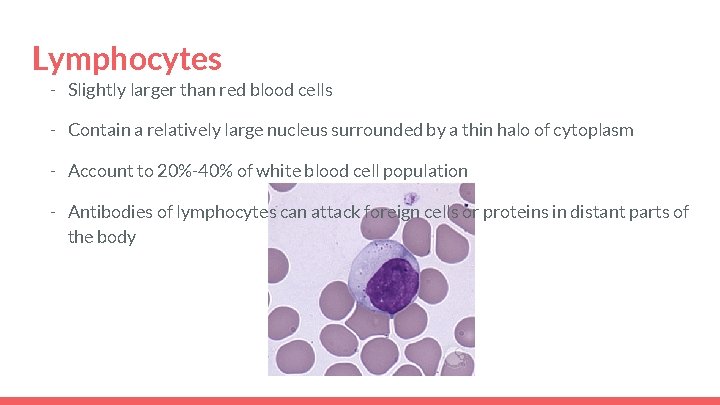
Lymphocytes - Slightly larger than red blood cells - Contain a relatively large nucleus surrounded by a thin halo of cytoplasm - Account to 20%-40% of white blood cell population - Antibodies of lymphocytes can attack foreign cells or proteins in distant parts of the body
Platelets 11 -6 Thrombocytes - The function is homeostasis - - They clump together and stick to vessel wall These are found in nonmammalian vertebrate - Are nucleated cells - Activate an intrinsic pathway of coagulation phase - Produced by megakaryocytes in red bone marrow - Red bone marrow containing enormous cells with large nuclei - Initiates the clotting process and helps close injured blood vessels - Continuously shed cytoplasm in small membrane enclosed packets Megakaryocytes

Phases of Homeostasis 11 -7 - Stop bleeding and prevent blood loss 1. Vascular phase 2. Platelet phase 3. Coagulation phase
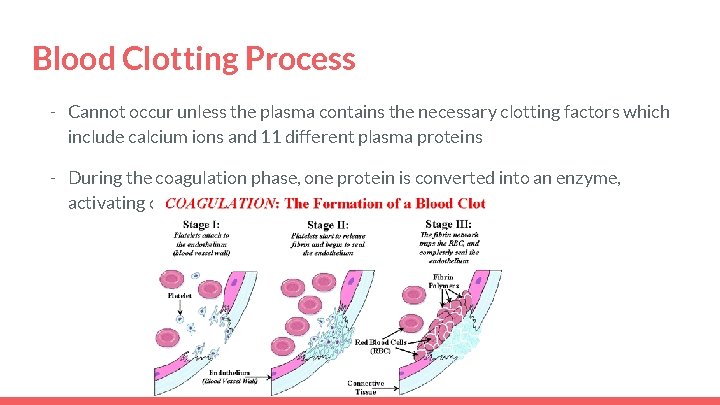
Blood Clotting Process - Cannot occur unless the plasma contains the necessary clotting factors which include calcium ions and 11 different plasma proteins - During the coagulation phase, one protein is converted into an enzyme, activating other proteins causing a chain reaction.

Extrinsic Pathways - Begins the release of a lipoprotein called tissue factor by damaged endothelial cells or peripheral tissues. - The greater the damage, the more tissue factor is released and the faster clotting occurs Intrinsic Pathways - Beings with the activation of protein enzymes exposed to collagen fibers at the injury site - Proceeds with the assistance of a platelet factor released by aggregating platelets. Common Pathways - Begins when enzymes from either the extrinsic or the intrinsic pathway activate factor X, forming the enzyme prothrombinase. - Calcium ions and a single vitamin K affect almost every aspect of the blood clotting process. - Inadequate amounts of vitamin K leads to breakdown of the common pathway, inactivating the clotting system.
- Slides: 12