Chapter 1 Cerebrovascular Infarct From Diseases of the

Chapter 1 Cerebrovascular Infarct From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved.
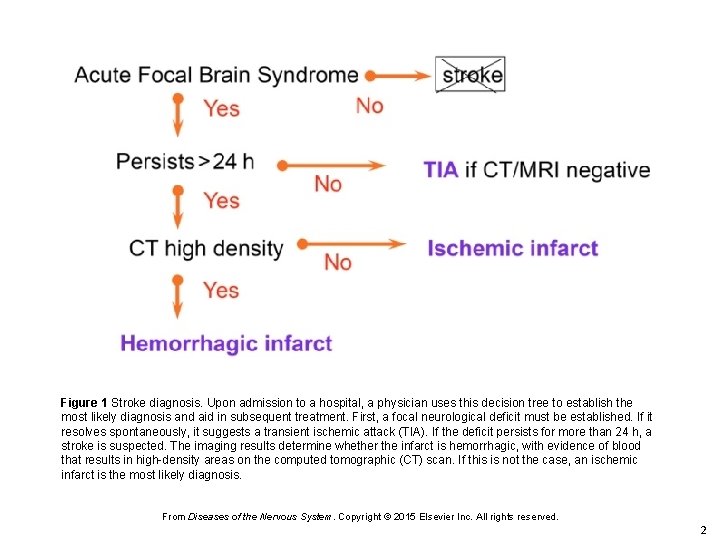
Figure 1 Stroke diagnosis. Upon admission to a hospital, a physician uses this decision tree to establish the most likely diagnosis and aid in subsequent treatment. First, a focal neurological deficit must be established. If it resolves spontaneously, it suggests a transient ischemic attack (TIA). If the deficit persists for more than 24 h, a stroke is suspected. The imaging results determine whether the infarct is hemorrhagic, with evidence of blood that results in high-density areas on the computed tomographic (CT) scan. If this is not the case, an ischemic infarct is the most likely diagnosis. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 2
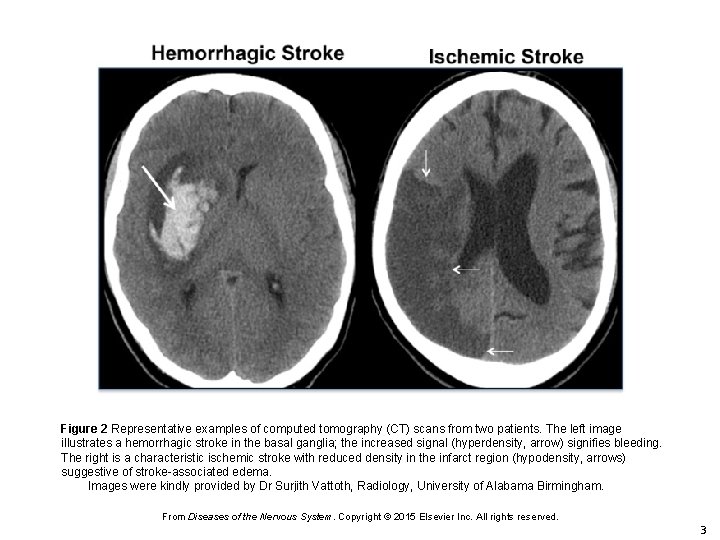
Figure 2 Representative examples of computed tomography (CT) scans from two patients. The left image illustrates a hemorrhagic stroke in the basal ganglia; the increased signal (hyperdensity, arrow) signifies bleeding. The right is a characteristic ischemic stroke with reduced density in the infarct region (hypodensity, arrows) suggestive of stroke-associated edema. Images were kindly provided by Dr Surjith Vattoth, Radiology, University of Alabama Birmingham. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 3
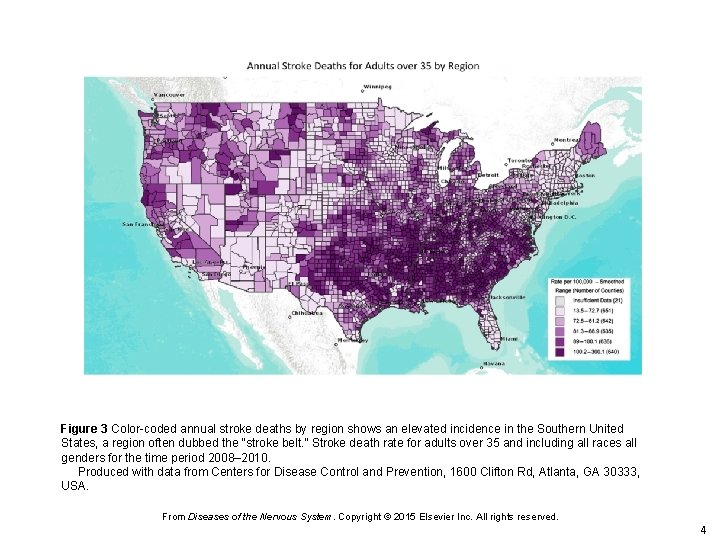
Figure 3 Color-coded annual stroke deaths by region shows an elevated incidence in the Southern United States, a region often dubbed the “stroke belt. ” Stroke death rate for adults over 35 and including all races all genders for the time period 2008– 2010. Produced with data from Centers for Disease Control and Prevention, 1600 Clifton Rd, Atlanta, GA 30333, USA. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 4
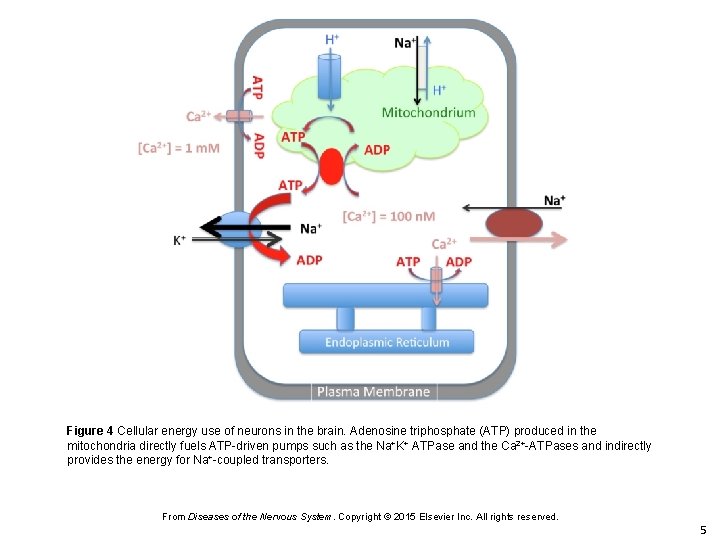
Figure 4 Cellular energy use of neurons in the brain. Adenosine triphosphate (ATP) produced in the mitochondria directly fuels ATP-driven pumps such as the Na+K+ ATPase and the Ca 2+-ATPases and indirectly provides the energy for Na+-coupled transporters. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 5
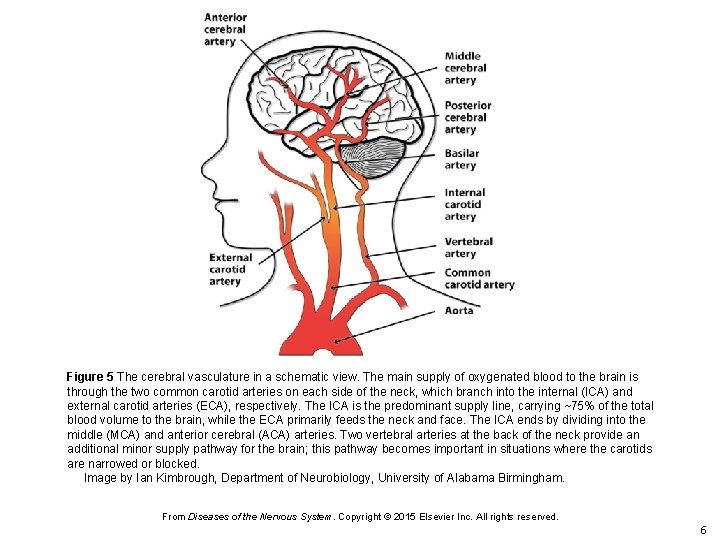
Figure 5 The cerebral vasculature in a schematic view. The main supply of oxygenated blood to the brain is through the two common carotid arteries on each side of the neck, which branch into the internal (ICA) and external carotid arteries (ECA), respectively. The ICA is the predominant supply line, carrying ~75% of the total blood volume to the brain, while the ECA primarily feeds the neck and face. The ICA ends by dividing into the middle (MCA) and anterior cerebral (ACA) arteries. Two vertebral arteries at the back of the neck provide an additional minor supply pathway for the brain; this pathway becomes important in situations where the carotids are narrowed or blocked. Image by Ian Kimbrough, Department of Neurobiology, University of Alabama Birmingham. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 6
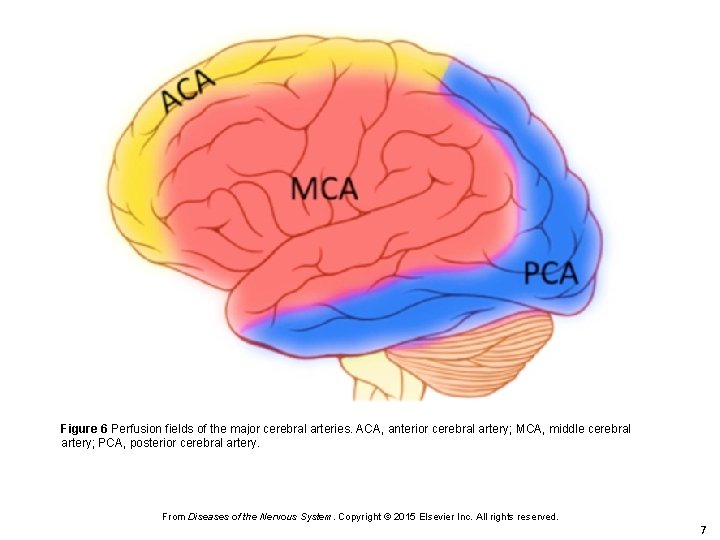
Figure 6 Perfusion fields of the major cerebral arteries. ACA, anterior cerebral artery; MCA, middle cerebral artery; PCA, posterior cerebral artery. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 7
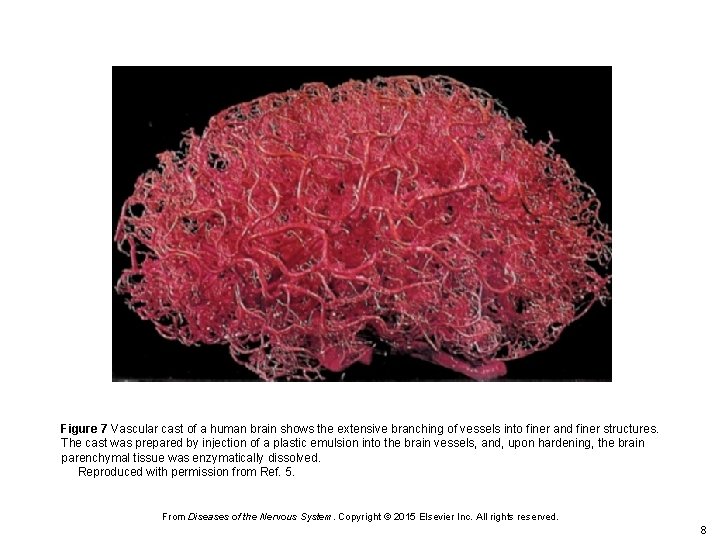
Figure 7 Vascular cast of a human brain shows the extensive branching of vessels into finer and finer structures. The cast was prepared by injection of a plastic emulsion into the brain vessels, and, upon hardening, the brain parenchymal tissue was enzymatically dissolved. Reproduced with permission from Ref. 5. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 8
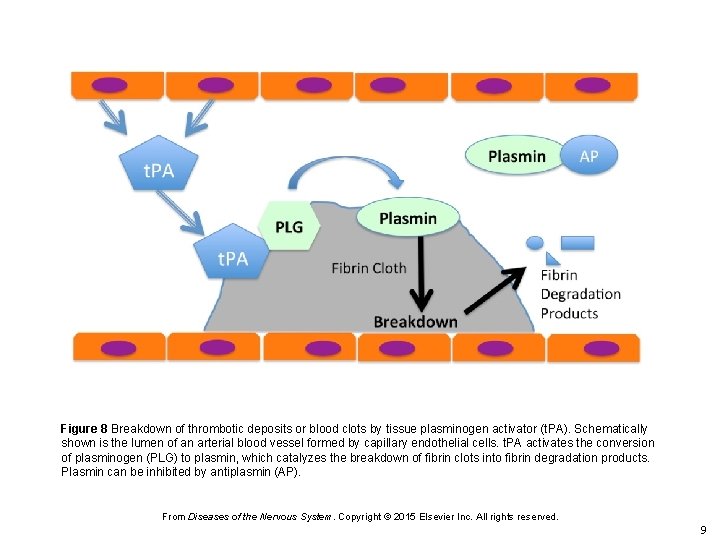
Figure 8 Breakdown of thrombotic deposits or blood clots by tissue plasminogen activator (t. PA). Schematically shown is the lumen of an arterial blood vessel formed by capillary endothelial cells. t. PA activates the conversion of plasminogen (PLG) to plasmin, which catalyzes the breakdown of fibrin clots into fibrin degradation products. Plasmin can be inhibited by antiplasmin (AP). From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 9
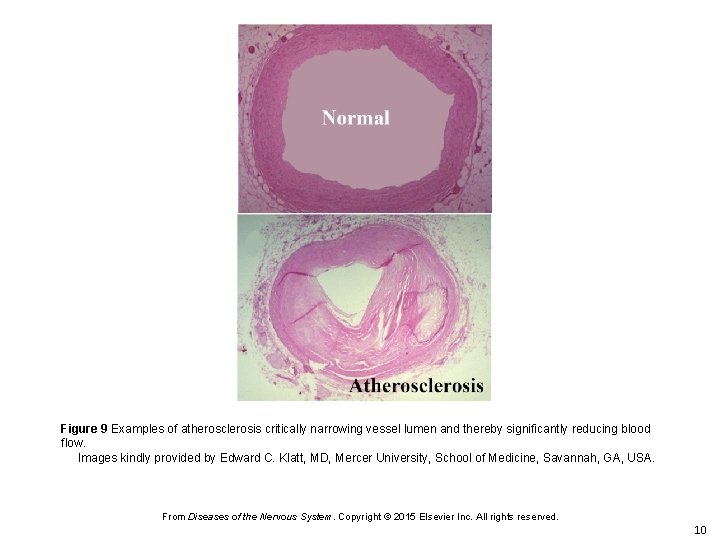
Figure 9 Examples of atherosclerosis critically narrowing vessel lumen and thereby significantly reducing blood flow. Images kindly provided by Edward C. Klatt, MD, Mercer University, School of Medicine, Savannah, GA, USA. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 10
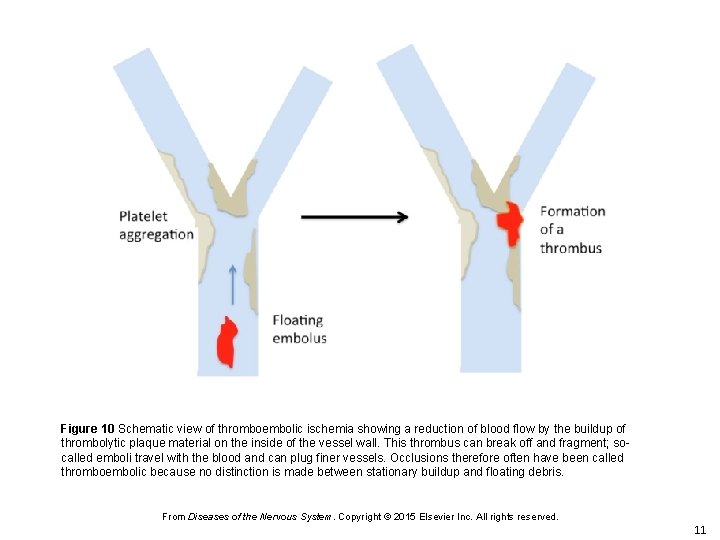
Figure 10 Schematic view of thromboembolic ischemia showing a reduction of blood flow by the buildup of thrombolytic plaque material on the inside of the vessel wall. This thrombus can break off and fragment; socalled emboli travel with the blood and can plug finer vessels. Occlusions therefore often have been called thromboembolic because no distinction is made between stationary buildup and floating debris. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 11
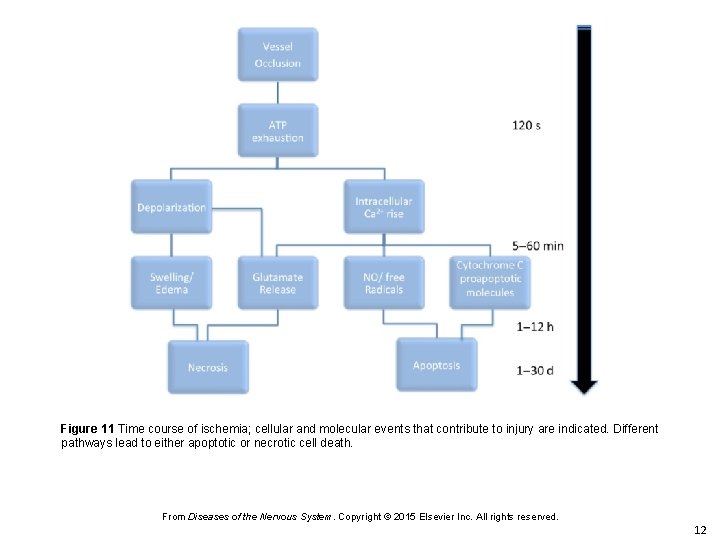
Figure 11 Time course of ischemia; cellular and molecular events that contribute to injury are indicated. Different pathways lead to either apoptotic or necrotic cell death. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 12
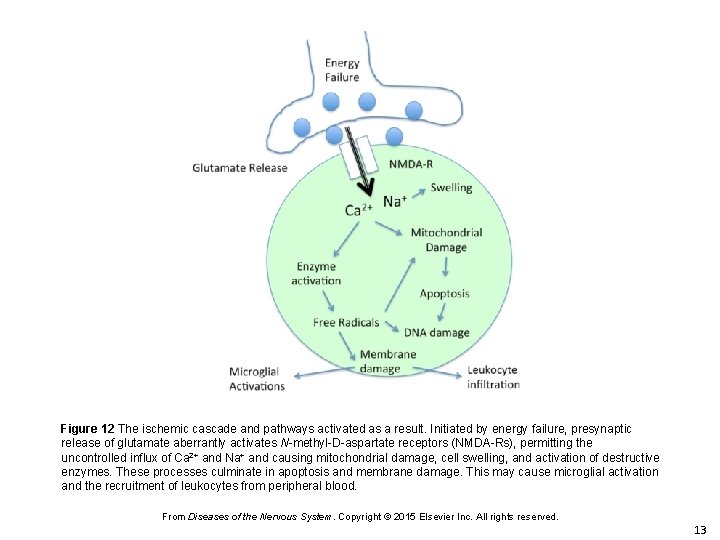
Figure 12 The ischemic cascade and pathways activated as a result. Initiated by energy failure, presynaptic release of glutamate aberrantly activates N-methyl-D-aspartate receptors (NMDA-Rs), permitting the uncontrolled influx of Ca 2+ and Na+ and causing mitochondrial damage, cell swelling, and activation of destructive enzymes. These processes culminate in apoptosis and membrane damage. This may cause microglial activation and the recruitment of leukocytes from peripheral blood. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 13
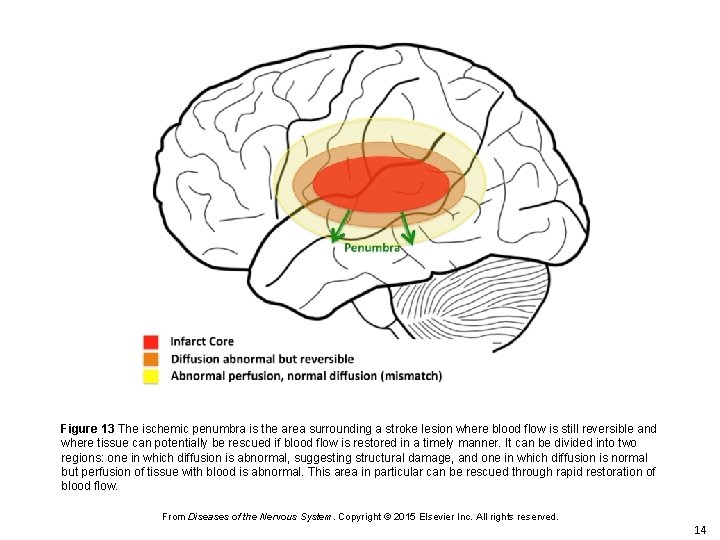
Figure 13 The ischemic penumbra is the area surrounding a stroke lesion where blood flow is still reversible and where tissue can potentially be rescued if blood flow is restored in a timely manner. It can be divided into two regions: one in which diffusion is abnormal, suggesting structural damage, and one in which diffusion is normal but perfusion of tissue with blood is abnormal. This area in particular can be rescued through rapid restoration of blood flow. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 14
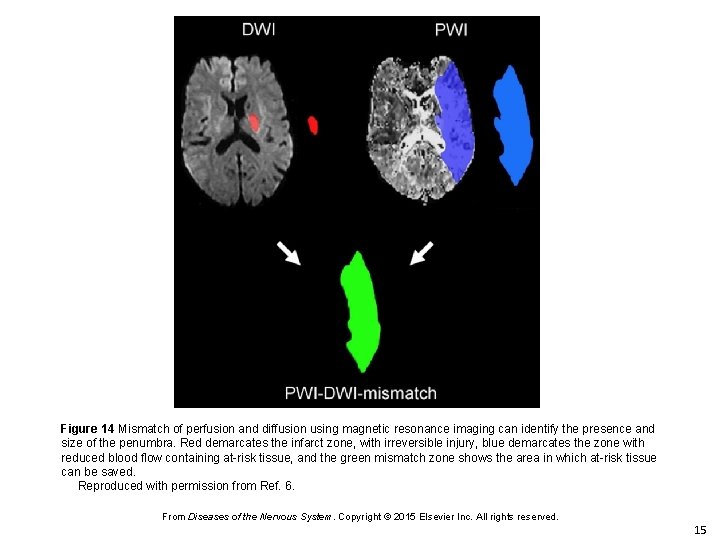
Figure 14 Mismatch of perfusion and diffusion using magnetic resonance imaging can identify the presence and size of the penumbra. Red demarcates the infarct zone, with irreversible injury, blue demarcates the zone with reduced blood flow containing at-risk tissue, and the green mismatch zone shows the area in which at-risk tissue can be saved. Reproduced with permission from Ref. 6. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 15
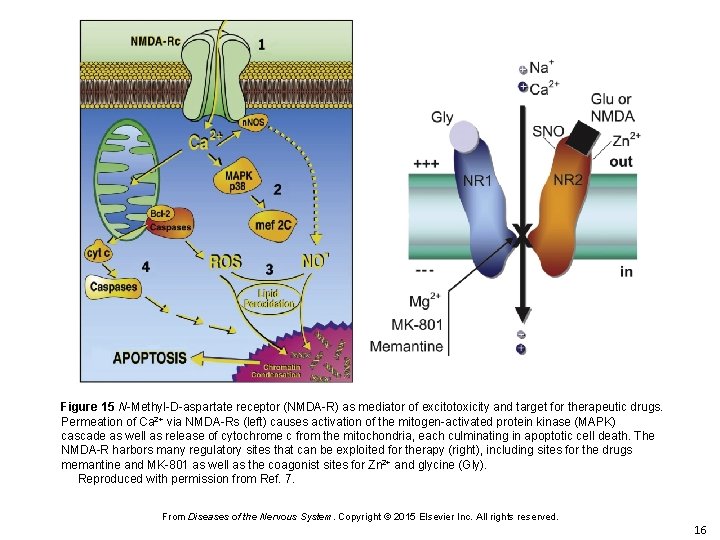
Figure 15 N-Methyl-D-aspartate receptor (NMDA-R) as mediator of excitotoxicity and target for therapeutic drugs. Permeation of Ca 2+ via NMDA-Rs (left) causes activation of the mitogen-activated protein kinase (MAPK) cascade as well as release of cytochrome c from the mitochondria, each culminating in apoptotic cell death. The NMDA-R harbors many regulatory sites that can be exploited for therapy (right), including sites for the drugs memantine and MK-801 as well as the coagonist sites for Zn 2+ and glycine (Gly). Reproduced with permission from Ref. 7. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 16
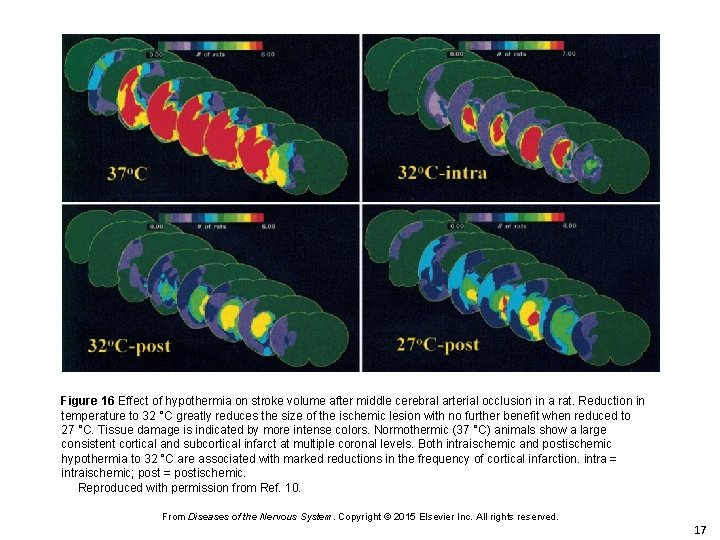
Figure 16 Effect of hypothermia on stroke volume after middle cerebral arterial occlusion in a rat. Reduction in temperature to 32 °C greatly reduces the size of the ischemic lesion with no further benefit when reduced to 27 °C. Tissue damage is indicated by more intense colors. Normothermic (37 °C) animals show a large consistent cortical and subcortical infarct at multiple coronal levels. Both intraischemic and postischemic hypothermia to 32 °C are associated with marked reductions in the frequency of cortical infarction. intra = intraischemic; post = postischemic. Reproduced with permission from Ref. 10. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 17
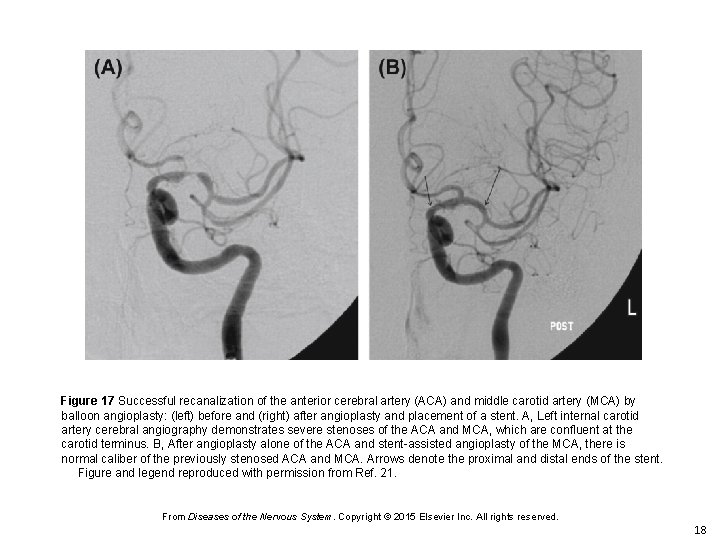
Figure 17 Successful recanalization of the anterior cerebral artery (ACA) and middle carotid artery (MCA) by balloon angioplasty: (left) before and (right) after angioplasty and placement of a stent. A, Left internal carotid artery cerebral angiography demonstrates severe stenoses of the ACA and MCA, which are confluent at the carotid terminus. B, After angioplasty alone of the ACA and stent-assisted angioplasty of the MCA, there is normal caliber of the previously stenosed ACA and MCA. Arrows denote the proximal and distal ends of the stent. Figure and legend reproduced with permission from Ref. 21. From Diseases of the Nervous System. Copyright © 2015 Elsevier Inc. All rights reserved. 18
- Slides: 18