Challenges in endstage heart failure Compliance Fabienne Dobbels

Challenges in end-stage heart failure: Compliance Fabienne Dobbels, Ph. D

Heart failure: A chronic disease • Requires ongoing management over a period of years • Cannot be cured • May lead to disability, or the short- or long-term reduction of a person’s activity • Goal of treatment: = to improve patients’ ability to live a productive and pain free life to get rid of the disease!!!
Treatment of heart failure: A complex therapeutic regimen Management of heart failure Prescription of multiple drugs - fluid restrictions - diet (< salt) - weighing +exercise -… Optimal treatment of co-morbidities

Management of patient with heart failure: Psychological Dimension Behavioral Dimension Physical Dimension Goal = to optimize outcomes!

Non-adherence: the Achilles heel of heart failure treatment v Definition v Prevalence v Consequences v Risk factors v Interventions Peter Paul Rubens 1630

Eve and the Apple in the Garden of Eden. . . . the first case of nonadherence?

Compliance = adherence = concordance = “The extent to which a person’s behavior corresponds with the agreed recommendations from a health care provider” (Sabate. WHO report 2003) = “Is a behavioral process, strongly influenced by the environment in which the patient lives, including the healthcare practices and system. Adherence assumes that a patient has the knowledge, motivation, skills and resources required to follow the recommendations of a healthcare professional. (AHA expert panel. Miller et al. 1997)
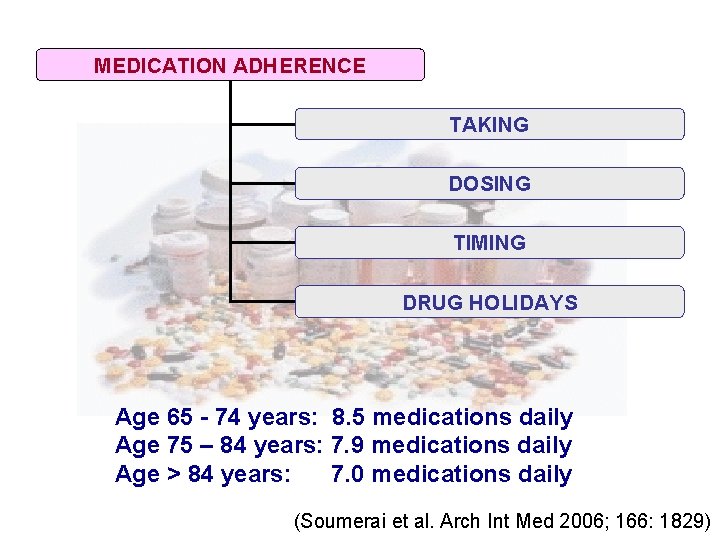
MEDICATION ADHERENCE TAKING DOSING TIMING DRUG HOLIDAYS Age 65 - 74 years: 8. 5 medications daily Age 75 – 84 years: 7. 9 medications daily Age > 84 years: 7. 0 medications daily (Soumerai et al. Arch Int Med 2006; 166: 1829)

Prevalence of non-adherence (NA) in elderly with heart failure • Medication taking: 1 - 90% • Fluid restrictions: 27 - 77% • Sodium restrictions: 27 – 87% • Daily weighing: 21 – 88% Large variation depending on operational definition and measurement method used (van der Wal et al. Int J Cardiol 2008; 125: 203)

Prevalence of adherence Disease HIV Arthritis Cancer Cardiovascular disease* End-stage renal disease Pulmonary disease Diabetes Mean (%) adherence 88. 3 81. 2 Random effects 95% CI (78. 9; 95. 2) (71. 9; 89. 0) 79. 1 76. 6 70. 0 68. 8 67. 5 (75. 9; 84. 2) (73. 4; 79. 8) (56. 8; 81. 6) (61. 1; 76. 2) (58. 5; 75. 8) * Numbers for hypertension similar to other cardiovascular diseases (Di. Matteo MR. Med Care 2004; 42(3): 200 -209)

Estimated NA of elderly patients with hear disease in Belgium Estimations (2004): - 10 318 000 inhabitants - 1 754 060 (17%) > 65 years - 261 355 (14. 9%) serious heart disease or heart attack in past 12 months - 23. 4% non-adherent 61 680 PATIENTS WITH HEART DISEASE NONADHERENT!!! (Belgian Health Interview Survey 2004, www. iph. fgov. be) (Di. Matteo MR. Med Care 2004; 2: 200)

NA is a prevalent problem: so what? ? ?

“Drugs don’t work in patients who don’t take them” (C Everett Koop M. D. ) Clinical Economic consequences

NA associated with poor clinical outcomes in heart failure • Absence of the intended effect of the drugs • Higher number of hospitalizations • More visits to the emergency department • Adverse effects (rebound effect) (Hope et al. Am J Health-Syst Pharm 2004; 61: 2043) (Vinson et al. Am J Geriatr Soc 1990; 38: 1290)
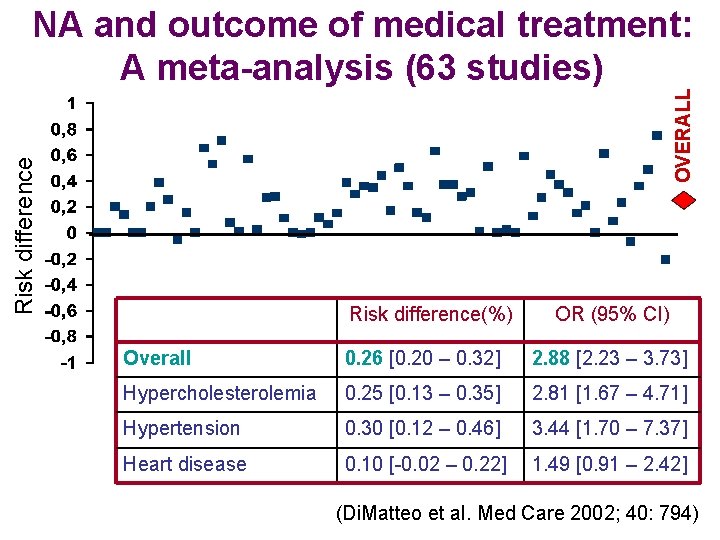
Risk difference OVERALL NA and outcome of medical treatment: A meta-analysis (63 studies) Risk difference(%) OR (95% CI) Overall 0. 26 [0. 20 – 0. 32] 2. 88 [2. 23 – 3. 73] Hypercholesterolemia 0. 25 [0. 13 – 0. 35] 2. 81 [1. 67 – 4. 71] Hypertension 0. 30 [0. 12 – 0. 46] 3. 44 [1. 70 – 7. 37] Heart disease 0. 10 [-0. 02 – 0. 22] 1. 49 [0. 91 – 2. 42] (Di. Matteo et al. Med Care 2002; 40: 794)
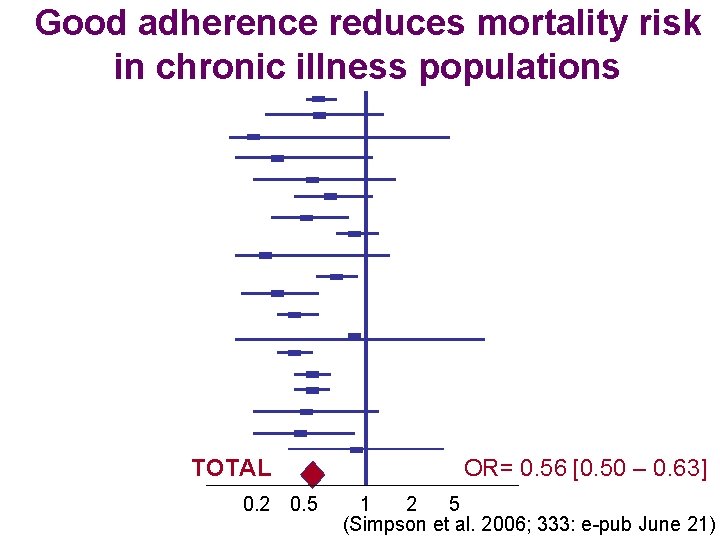
Good adherence reduces mortality risk in chronic illness populations TOTAL 0. 2 0. 5 OR= 0. 56 [0. 50 – 0. 63] 2 5 1 (Simpson et al. 2006; 333: e-pub June 21)
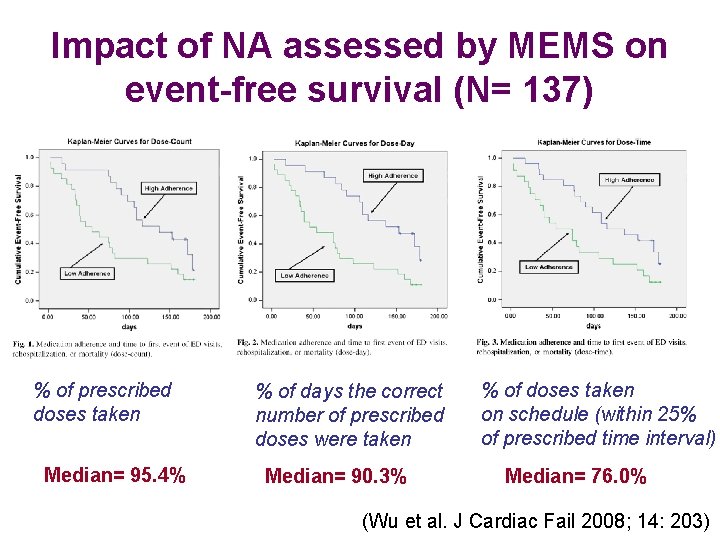
Impact of NA assessed by MEMS on event-free survival (N= 137) % of prescribed doses taken Median= 95. 4% % of days the correct number of prescribed doses were taken Median= 90. 3% % of doses taken on schedule (within 25% of prescribed time interval) Median= 76. 0% (Wu et al. J Cardiac Fail 2008; 14: 203)

Economic consequences

Economic consequences of NA Direct costs • cost of non-taken medication • cost for treatment of morbidity • cost of avoidable hospitalizations Indirect costs • Missed work days • Cost for transportation, household, home care • quality of life • cost of evolving more potent medications
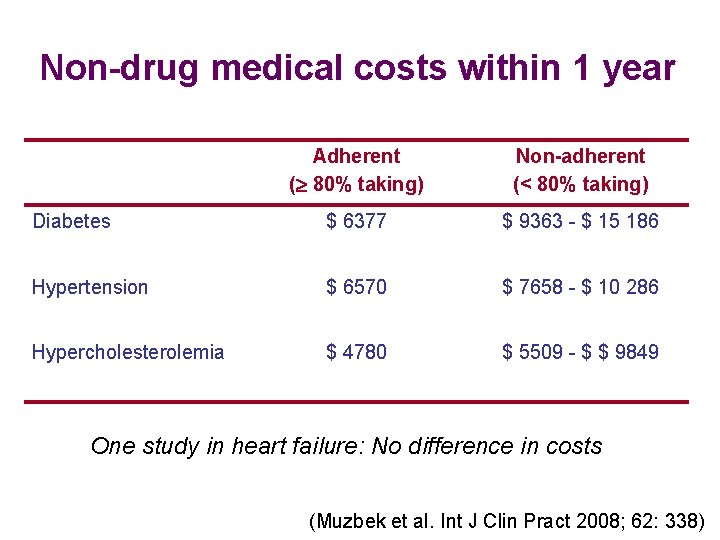
Non-drug medical costs within 1 year Adherent ( 80% taking) Non-adherent (< 80% taking) Diabetes $ 6377 $ 9363 - $ 15 186 Hypertension $ 6570 $ 7658 - $ 10 286 Hypercholesterolemia $ 4780 $ 5509 - $ $ 9849 One study in heart failure: No difference in costs (Muzbek et al. Int J Clin Pract 2008; 62: 338)

Noncompliance: a major and important problem Can / will health care provider do something. . . Or will we expel patients from Paradise?
What can be done to improve adherence ? Identifying patients at risk for NA Implementation of interventions Determinants of NA Randomized controlled trials

Measurement of nonadherence Clinical nonadherence A. Direct methods B. - observation C. D. - assay - objective tests Sub-clinical nonadherence B. Indirect methods – pill count – prescription refill – clinical judgement – electronic monitoring – self-report No gold standard: combine measures to increase accuracy (Osterberg et al. N Engl J Med 2005; 353)

5 interrelated categories of determinants Socio-economic factors Condition related factors Health professional and setting-related Patient related factors Treatment related factors (Sabate E. WHO report 2003)

Determinants in patients with HF Socio-economic Condition related Poor socioeconomic status Low education/illiterate Depression Cognitive dysfunction Cost of medication Higher co-morbidity Poor social support Living alone Treatment related Patient related Complex regimen Side effects Poor knowledge Lack of motivation Lifelong duration of treatment Health beliefs/ attitudes Frequent changes Interference with socialization (van der Wal et al. Int J Cardiol 2008; 125: 203)

Impact of the health care provider and setting related factors Macro level Policy Meso level Health care organizations and community Micro level patient-provider interaction - reimbursement and insurance policy - no funding for chronic disease management programs or prevention - Short consultations - Lack of follow-up / cooperation with community services - Uni-disciplinary treatment - Poor knowledge about adherence - lack of trust - poor communication style

Interventions…
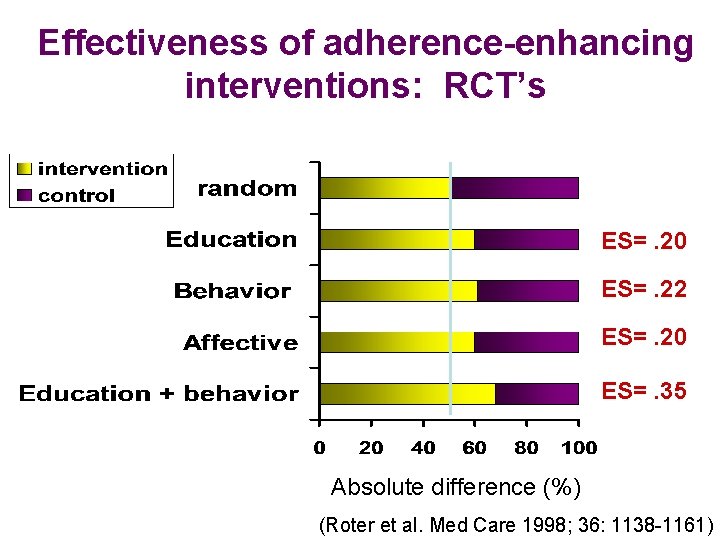
Effectiveness of adherence-enhancing interventions: RCT’s ES=. 20 ES=. 22 ES=. 20 ES=. 35 Absolute difference (%) (Roter et al. Med Care 1998; 36: 1138 -1161)

Typical reaction if treatment is not working: the radar syndrome The patient appears… Find the problem and fix it, by: - increasing the dose - switching to another drug - adding another drug But nonadherence frequently ignored!

Disease management programs in heart failure populations • Integrated programs with focus on - detailed assessment of the patient DISEASE MANAGEMENT - patient education about treatment regimen - optimizing medications Education Monitoring - regular monitoring by health professionals (Health and health care 2010 – The Forecast – the Challenge Institute of the future 2003)
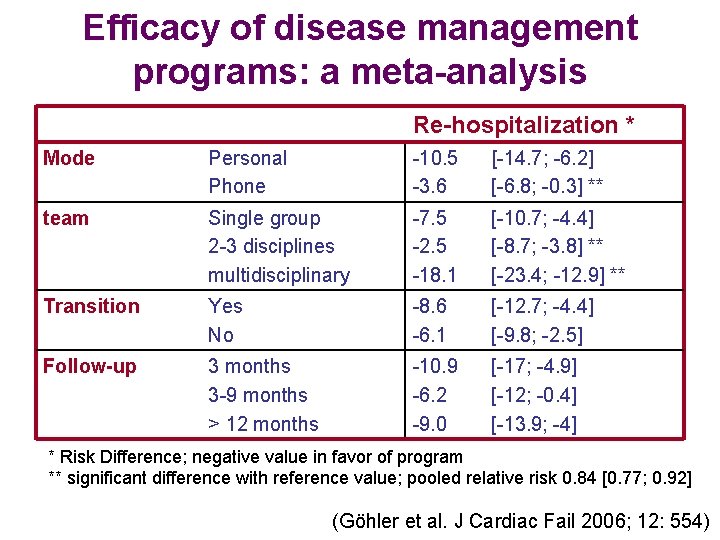

Efficacy of disease management programs: a meta-analysis Re-hospitalization * Mode Personal Phone -10. 5 -3. 6 [-14. 7; -6. 2] [-6. 8; -0. 3] ** team Single group 2 -3 disciplines multidisciplinary -7. 5 -2. 5 -18. 1 [-10. 7; -4. 4] [-8. 7; -3. 8] ** [-23. 4; -12. 9] ** Transition Yes No -8. 6 -6. 1 [-12. 7; -4. 4] [-9. 8; -2. 5] Follow-up 3 months 3 -9 months > 12 months -10. 9 -6. 2 -9. 0 [-17; -4. 9] [-12; -0. 4] [-13. 9; -4] * Risk Difference; negative value in favor of program ** significant difference with reference value; pooled relative risk 0. 84 [0. 77; 0. 92] (Göhler et al. J Cardiac Fail 2006; 12: 554)

Cost-effectiveness of disease management programs • Mean age at onset 67 years (35% female) – Quality adjusted life expectancy: 2. 64 years for standard care 2. 83 years for disease management program – Additional lifetime cost for 84 days difference: 1700 Euro (i. e. 9800 Euro per QALY gained) Beneficial impact on clinical outcomes but expensive… (Göhler et al. Eur J Heart Failure 2008; e-pub)
Problem of disease management problems 20% 3 o 2 o 1 o Patient preferences Readiness for treatment Compliance Symptom management … Providing professional patient care

The majority of care is taking place outside the hospital setting 20% 80% 3 o 2 o 1 o Patient preferences Readiness for treatment Compliance Symptom management … Providing professional patient care Fostering patient self-management

“The most effective approaches have been shown to be multidimensional and multilevel – targeting more than one factor with more than one intervention” (Haynes et al. Cochrane Reviews 2008)
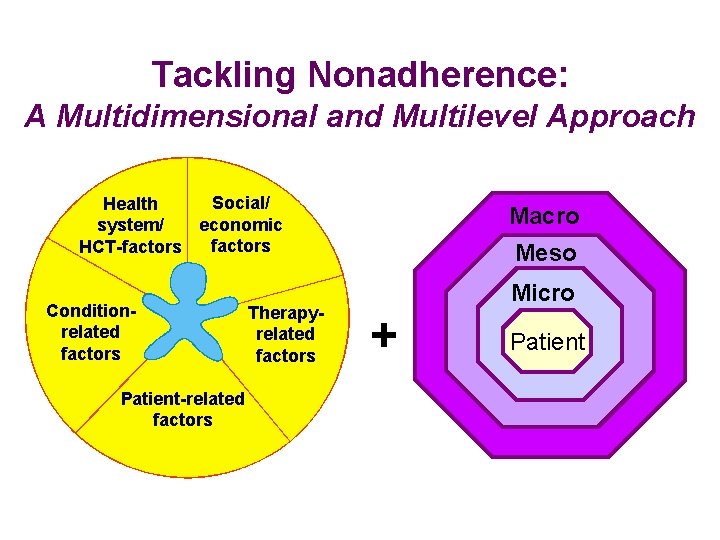
Tackling Nonadherence: A Multidimensional and Multilevel Approach Social/ Health economic system/ factors HCT-factors Conditionrelated factors Patient-related factors Therapyrelated factors Macro Meso Micro + Patient
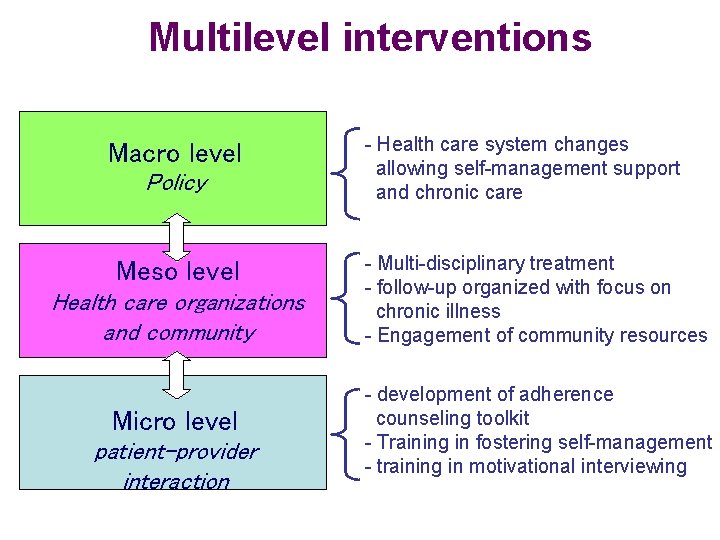
Multilevel interventions Macro level Policy Meso level Health care organizations and community Micro level patient-provider interaction - Health care system changes allowing self-management support and chronic care - Multi-disciplinary treatment - follow-up organized with focus on chronic illness - Engagement of community resources - development of adherence counseling toolkit - Training in fostering self-management - training in motivational interviewing
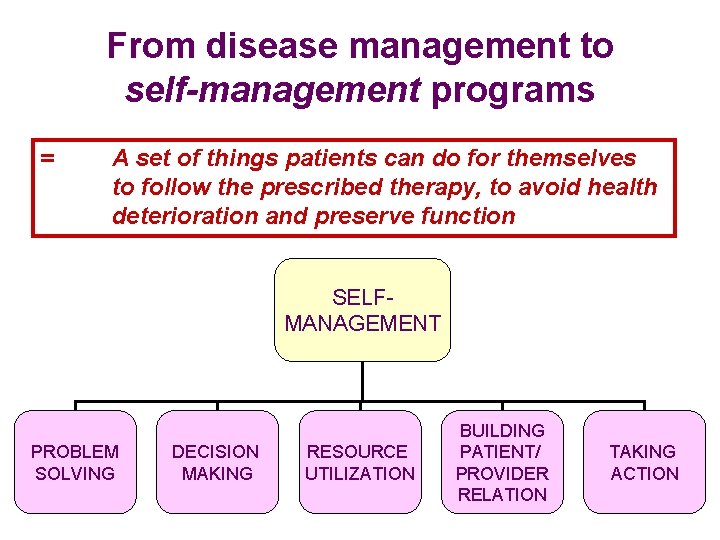
From disease management to self-management programs = A set of things patients can do for themselves to follow the prescribed therapy, to avoid health deterioration and preserve function SELFMANAGEMENT PROBLEM SOLVING DECISION MAKING RESOURCE UTILIZATION BUILDING PATIENT/ PROVIDER RELATION TAKING ACTION

Remember the definition? ? ? = “Is a behavioral process, strongly influenced by the environment in which the patient lives, including the healthcare practices and system. Adherence assumes that a patient has the knowledge, motivation, skills and resources required to follow the recommendations of a healthcare professional. (AHA expert panel. Miller et al. 1997)
![Efficacy and cost of HF selfmanagement programs Odds ratio [95% CI] All-cause readmission in Efficacy and cost of HF selfmanagement programs Odds ratio [95% CI] All-cause readmission in](http://slidetodoc.com/presentation_image_h/e0dd89c4a6de96630a5126704205d89b/image-40.jpg)
Efficacy and cost of HF selfmanagement programs Odds ratio [95% CI] All-cause readmission in 1 year (5 studies) 0. 59 [0. 44; 0. 80] Readmissions due to HF (3 studies) 0. 44 [0. 27; 0. 71] Mortality (3 studies) 0. 95 [0. 57; 1. 51](NS) Adherence (2 studies) Both significant Cost saving (3 studies) after subtracting the intervention cost: $ 1300 - $ 7515 saved per patient annually ONLY POSSIBLE IF YOU HAVE A TRAINED TEAM!!! (Jovicic et al. BMC Cardiovascular Disorders 2006; 6: 43)

Conclusion • HF is a chronic disease requiring a complex management • Nonadherence is a prevalent problem, resulting in poor clinical and economical outcomes • Risk factors are multi-factorial • Interventions should be multidimensional, targeting more than 1 risk factor with more than 1 intervention • A multilevel approach is mandatory, integrating interventions at the patient, health care professional, team and policy level

Take home message “Changing systems of care and applying multidimensional + multilevel adherenceenhancing interventions to improve selfmanagement may have a far greater impact on the health of heart failure patients than any improvement in specific medical treatments” (Haynes et al. Cochrane review 2008)

Increasing adherence with heart failure treatment. . . ITHET IS NEVER TOO IS NOOIT TEEARLY! LAAT!

IT IS NEVER TOO LATE! KEEP ON BELIEVING THAT PEOPLE CAN CHANGE!


Some numbers… • 3. 7% of the Belgian population reported with a serious heart problem or heart attack in the last 12 months (2004) • 21. 9% treated by GP alone • 38. 9% treated by specialist alone • 25. 7% treated by both GP and specialist • • 89. 3% of these patients use medicines for this problem Use of cholesterol reducing agents: 6. 4% Use of cardiac glycosides: 0. 7% Use of anti-arrhytmics: 0. 8% Use of ace-inhibitors: 3. 8% Use of diuretics: 4% Use of beta-blocking agents: 8. 7%

• > 65 years: 3. 4 drugs on average • 14. 9% of > 65 years serious cardiac disease or heart attack in past 12 months – 22. 3% cholesterol reducing agent – 3. 9% cardiac glycosides – 4. 2% anti-arrhytmics – 14. 1% ace-inhibitor – 18. 7% diuretics – 26. 2% beta-blocking agents Belgian Health Interview Survey 2004, Scientific Institute for Public Health www. iph. fgov. be
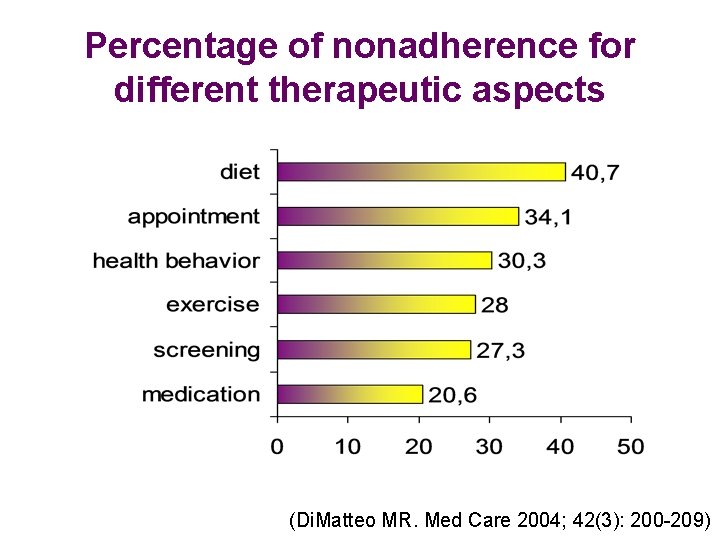
Percentage of nonadherence for different therapeutic aspects (Di. Matteo MR. Med Care 2004; 42(3): 200 -209)
- Slides: 48