Ch 4 Skin and Body Membranes Epithelial Membranes

Ch. 4 Skin and Body Membranes
Epithelial Membranes Cutaneous membrane (skin) (a) Cutaneous membrane (the skin) covers the body surface. Figure 4. 1 a

Epithelial Membranes �Mucous membranes �Mucosa �Lines body cavities that open to exterior (e. g. , digestive and respiratory tracts)
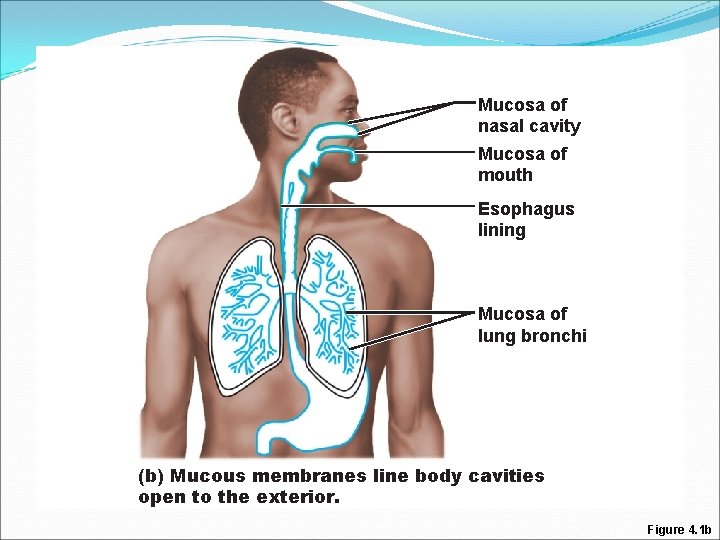
Mucosa of nasal cavity Mucosa of mouth Esophagus lining Mucosa of lung bronchi (b) Mucous membranes line body cavities open to the exterior. Figure 4. 1 b

Epithelial Membranes �Serous Membranes �Paired membranes that line closed ventral body cavities �Parietal layer –lines body walls �Visceral layer- covers internal organs � Serous Membranes are named based on their location: �Pleural membranes surround: lungs �Pericardial membranes surround: heart �Peritoneal membranes surround: viscera
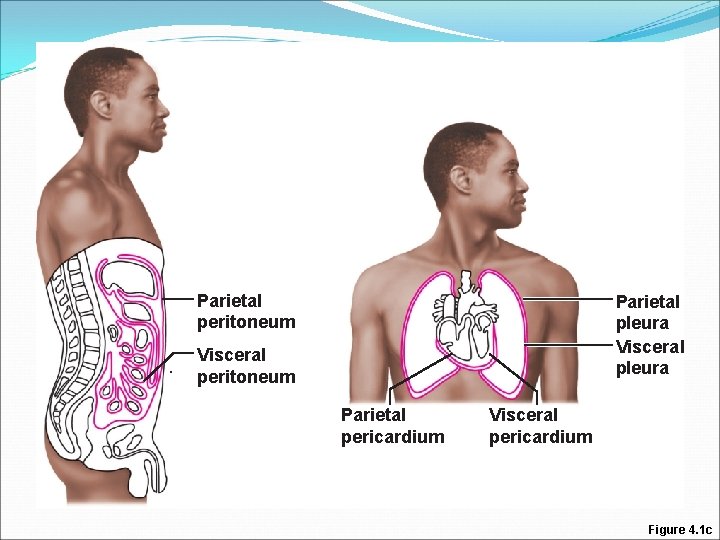
Parietal peritoneum Parietal pleura Visceral peritoneum Parietal pericardium Visceral pericardium Figure 4. 1 c

Skin (Integument) � Consists of three major regions 1. Epidermis—superficial region 2. Dermis—middle region 3. Hypodermis —deepest region � Mostly adipose tissue
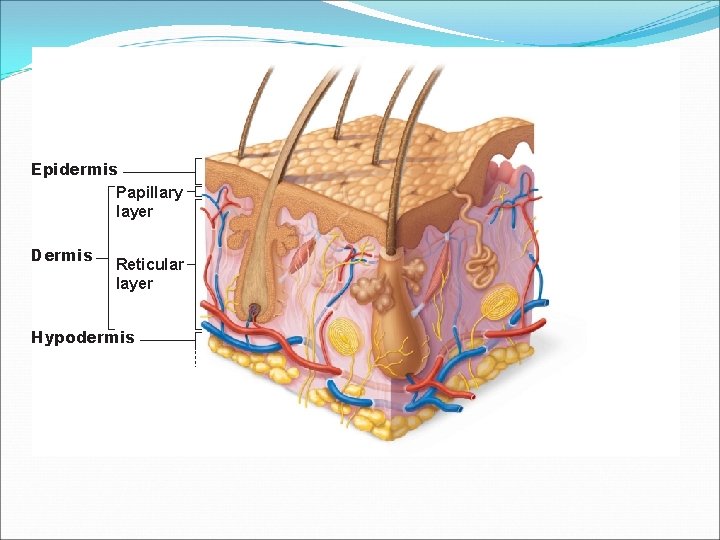
Epidermis Papillary layer Dermis Reticular layer Hypodermis

Epidermis �Keratinized stratified squamous epithelium �Cells of epidermis �Keratinocytes—produce fibrous protein keratin �Melanocytes � Produce pigment melanin
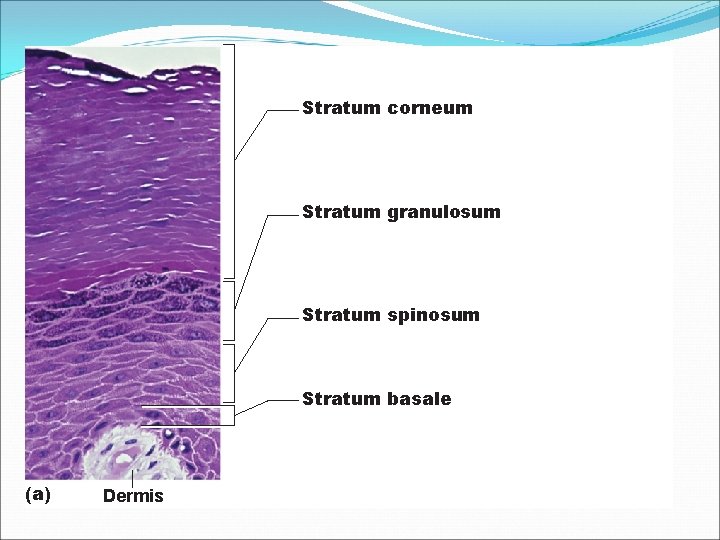
Stratum corneum Stratum granulosum Stratum spinosum Stratum basale (a) Dermis

Layers of the Epidermis: Stratum Basale �Deepest epidermal layer firmly attached to dermis �One cell layer �Cells undergo rapid division and then travel from basal layer to surface �Takes 25– 45 days �Contains melanocytes

Layers of the Epidermis: Stratum Spinosum �~5 -6 cell layers �Flatter cells increasingly filled with keratin

Layers of the Epidermis: Stratum Granulosum � 2 -3 cell layers �Thin layer of flat cells increasingly filled with keratin

Layers of the Epidermis: Stratum Lucidum �A few rows of flat, dead keratinocytes �Thin, transparent band superficial to the stratum granulosum �Only in soles and palms

Layers of the Epidermis: Stratum Corneum � 20– 30 rows of dead, flat, keratinized cells �Three-quarters of the epidermal thickness �Functions �Protects from abrasion and penetration �Waterproofs skin
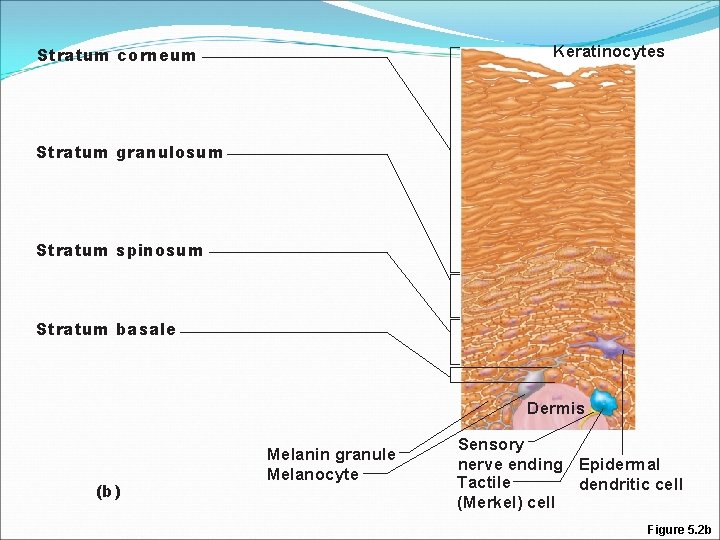
Keratinocytes Stratum corneum Stratum granulosum Stratum spinosum Stratum basale Dermis (b) Melanin granule Melanocyte Sensory nerve ending Epidermal Tactile dendritic cell (Merkel) cell Figure 5. 2 b

Dermis �Made up of Two layers: �Papillary Layer �Reticular Layer
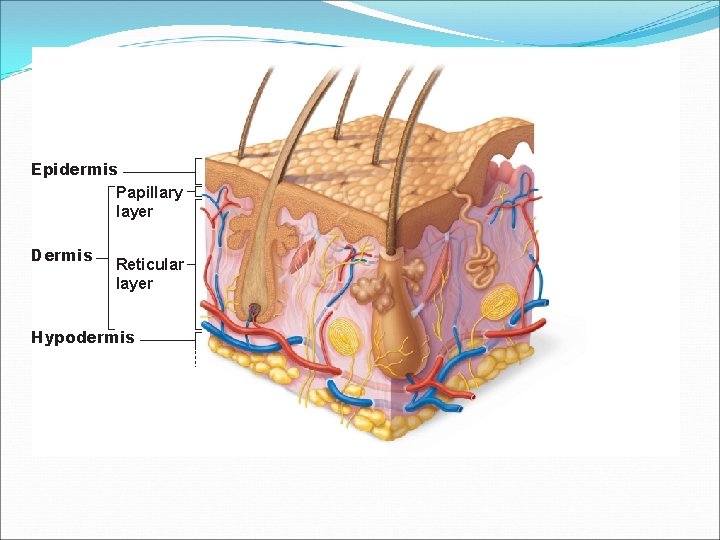
Epidermis Papillary layer Dermis Reticular layer Hypodermis

Layers of the Dermis: Papillary Layer �Papillary layer �Composed of: �Contains dermal papillae which may have: �Capillary loops �Meissner’s Corpuscles �Free nerve endings
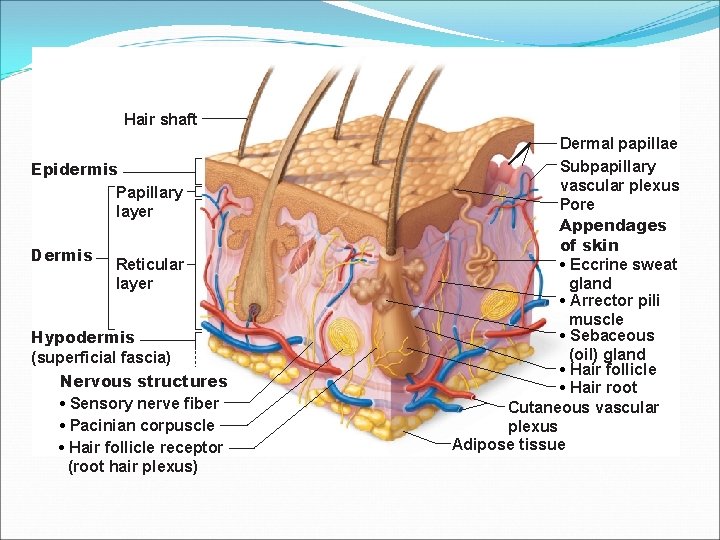
Hair shaft Epidermis Papillary layer Dermis Reticular layer Hypodermis (superficial fascia) Nervous structures • Sensory nerve fiber • Pacinian corpuscle • Hair follicle receptor (root hair plexus) Dermal papillae Subpapillary vascular plexus Pore Appendages of skin • Eccrine sweat gland • Arrector pili muscle • Sebaceous (oil) gland • Hair follicle • Hair root Cutaneous vascular plexus Adipose tissue

Layers of the Dermis: Reticular Layer �Reticular layer �Composed of: �Most glands, hair follicles, emerge from dermis

Skin Color � Three pigments contribute to skin color: 1. Melanin � Yellow to reddish-brown to black, responsible for dark skin colors

Skin Color 2. Carotene � Yellow to orange, most obvious in the palms and soles 3. Hemoglobin � Responsible for the pinkish hue of skin

Appendages of the Skin �Derived from the epidermis �Sweat glands �Oil glands �Hairs and hair follicles �Nails

Sweat Glands � Two main types of sweat glands 1. Eccrine sweat glands—abundant on palms, soles, and forehead � � � Sweat: 99% water, Na. Cl, vitamin C, antibodies, metabolic wastes Ducts connect to pores Function in thermoregulation
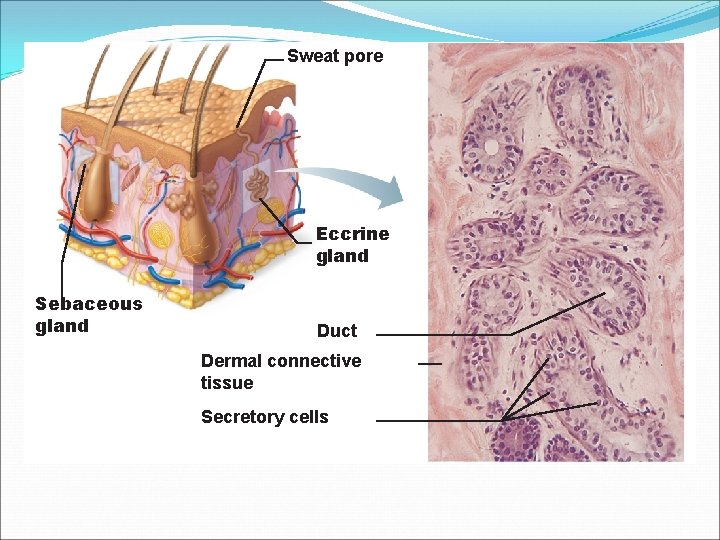
Sweat pore Eccrine gland Sebaceous gland Duct Dermal connective tissue Secretory cells

Sweat Glands 2. Apocrine sweat glands—confined to axillary and anogenital areas � Sebum: sweat + fatty substances and proteins � Ducts connect to hair follicles � Functional from puberty onward

Sebaceous (Oil) Glands �Most develop from hair follicles �Secrete Sebum: �Oily secretion �Bactericidal �Softens hair and skin
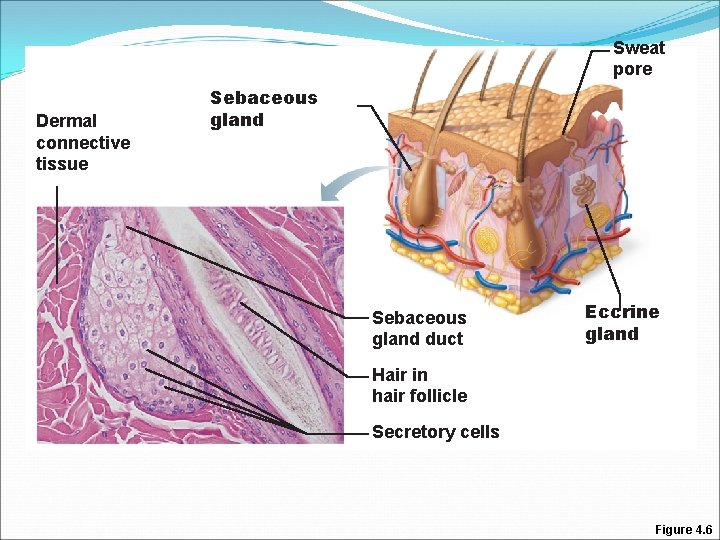
Sweat pore Dermal connective tissue Sebaceous gland duct Eccrine gland Hair in hair follicle Secretory cells Figure 4. 6

Hair �Functions �Alerting the body to presence of objects on the skin �Guarding the scalp against physical trauma, heat loss, and sunlight �Consists of three layers of squamous keratinocytes: cuticle (outermost layer), cortex, medulla surrounded by a hair follicle
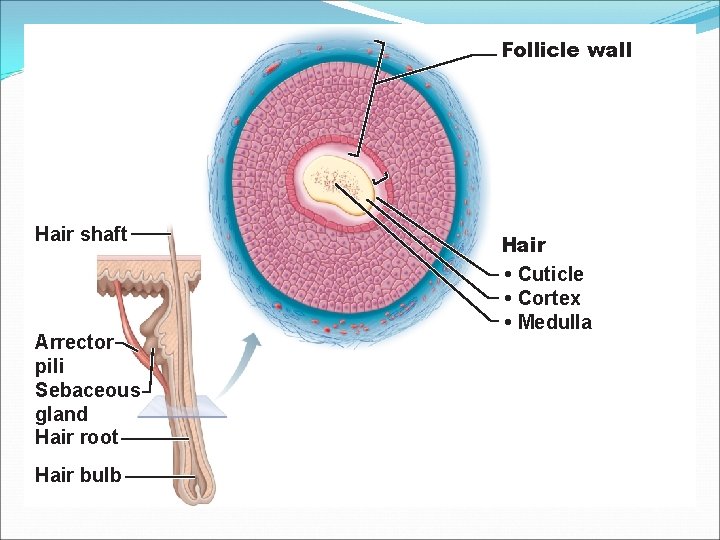
Follicle wall Hair shaft Arrector pili Sebaceous gland Hair root Hair bulb Hair • Cuticle • Cortex • Medulla

Hair Follicle �Two layered wall consisting of CT and ET �Hair bulb: expanded deep end �Hair follicle receptor (root hair plexus): �Sensory nerve endings around each hair bulb

Hair Follicle �Arrector pili �Smooth muscle attached to follicle �Contraction of these muscles causes the hairs to stand on end
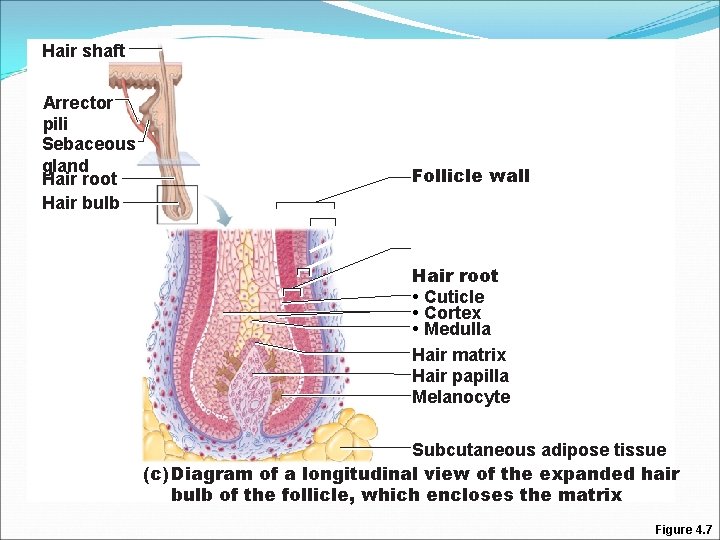
Hair shaft Arrector pili Sebaceous gland Hair root Hair bulb Follicle wall Hair root • Cuticle • Cortex • Medulla Hair matrix Hair papilla Melanocyte Subcutaneous adipose tissue (c) Diagram of a longitudinal view of the expanded hair bulb of the follicle, which encloses the matrix Figure 4. 7

Structure of a Nail �Scalelike modification of the epidermis �Structures of the nail: Nail matrix, nail bed, hyponichium, eponichium,
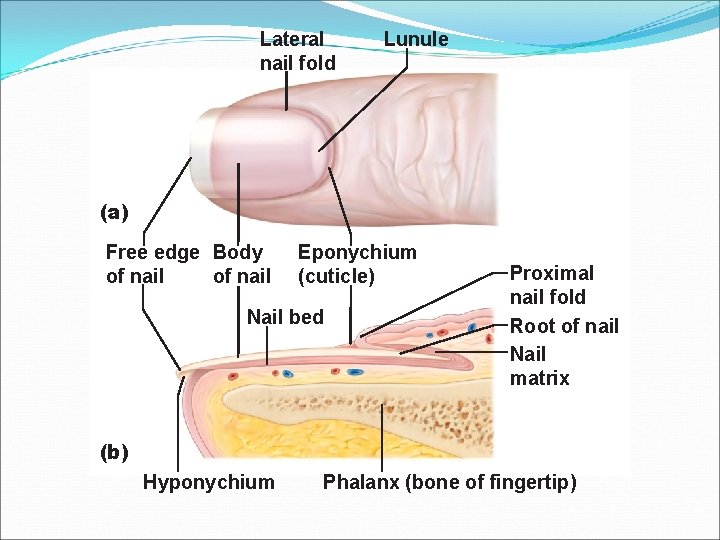
Lateral nail fold Lunule (a) Free edge Body of nail Eponychium (cuticle) Nail bed Proximal nail fold Root of nail Nail matrix (b) Hyponychium Phalanx (bone of fingertip)

Functions of the Integumentary System 1. Protection—three types of barriers � Chemical � Low p. H secretions retard bacterial activity �Physical/mechanical barriers �Keratin and glycolipids block most water and water- soluble substances �Biological barriers �Macrophages

Functions of the Integumentary System 2. Body temperature regulation � 3. At elevated temperature, dilation of dermal vessels and increased sweat gland activity cool the body Cutaneous sensations � Temperature, touch, and pain

Functions of the Integumentary System 4. Metabolic functions � Synthesis of vitamin D precursor 5. Blood reservoir—up to 5% of body’s blood volume 6. Excretion—nitrogenous wastes and salt in sweat

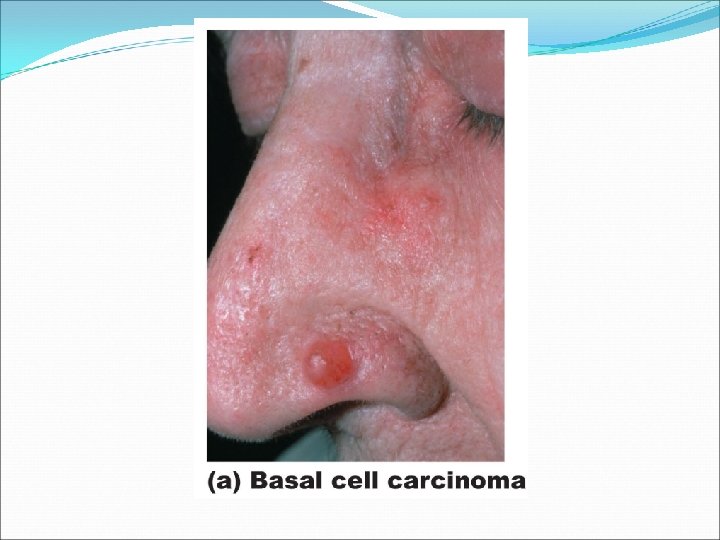
Basal Cell Carcinoma �Least malignant, most common �Appearance: Red, shiny, raised nodule �Stratum basale cells proliferate and slowly invade dermis and hypodermis �Cured by surgical excision in 99% of cases

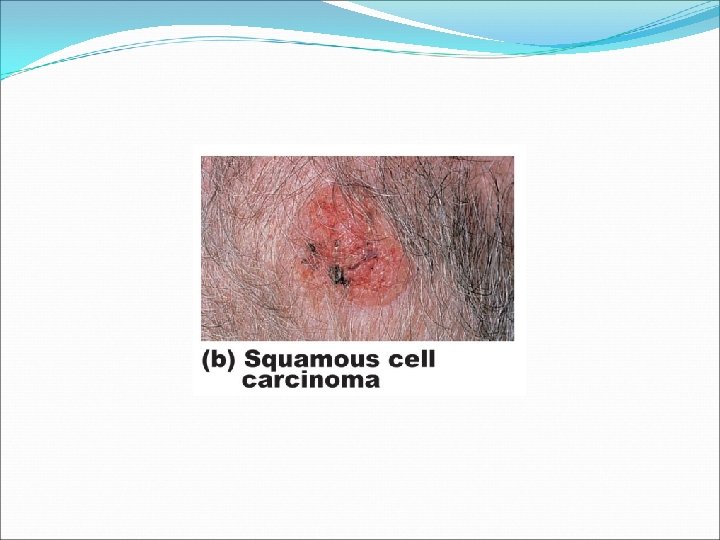
Squamous Cell Carcinoma �Second most common �Appearance: flat and scaly �Involves keratinocytes of stratum spinosum �Good prognosis if treated by radiation therapy or removed surgically

Melanoma �Most dangerous type �Appearance: black/brown spreading patch; may develop from pre-existing moles �Highly metastatic and resistant to chemotherapy; most dangerous �Treated by wide surgical excision accompanied by immunotherapy

Melanoma �Characteristics (ABCD rule) A: Asymmetry; the two sides of the pigmented area do not match B: Border exhibits indentations C: Color is black, brown, tan, and sometimes red or blue D: Diameter is larger than 6 mm (size of a pencil eraser)
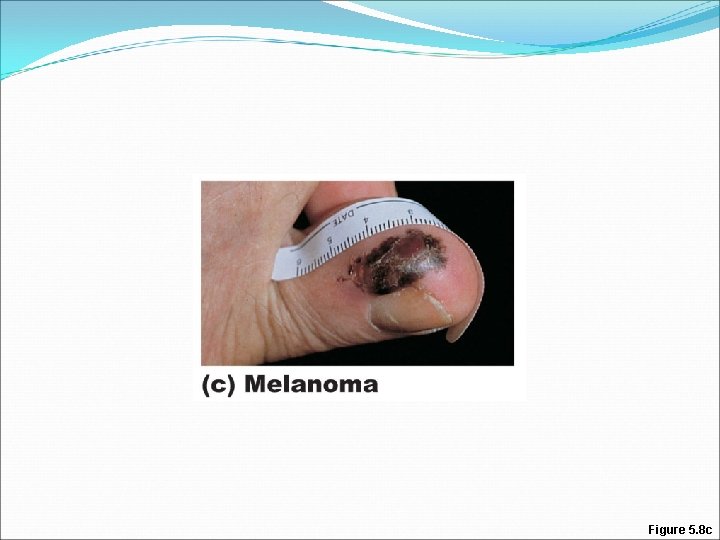
Figure 5. 8 c

Partial-Thickness Burns �First degree �Epidermal damage only �Localized and pain redness, edema (swelling), �Second degree �Epidermal and upper dermal damage �Blisters appear
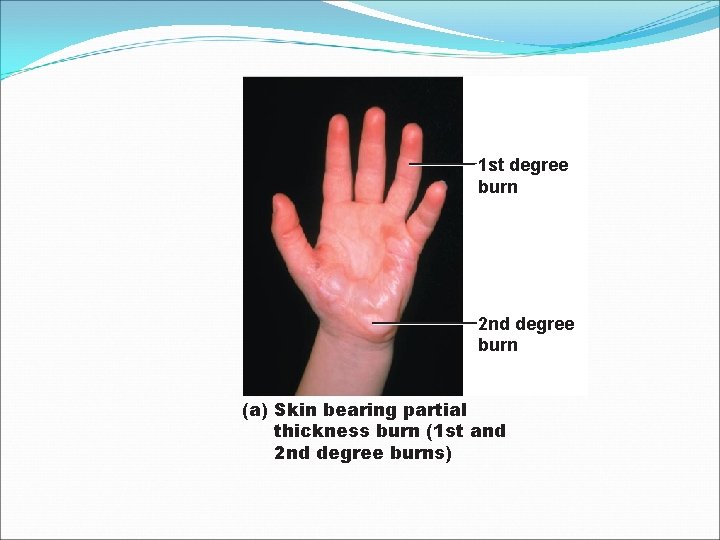
1 st degree burn 2 nd degree burn (a) Skin bearing partial thickness burn (1 st and 2 nd degree burns)

Full-Thickness Burns �Third degree �Entire thickness of skin damaged �Gray-white, cherry red, or black �No initial edema or pain (nerve endings destroyed) �Skin grafting usually necessary
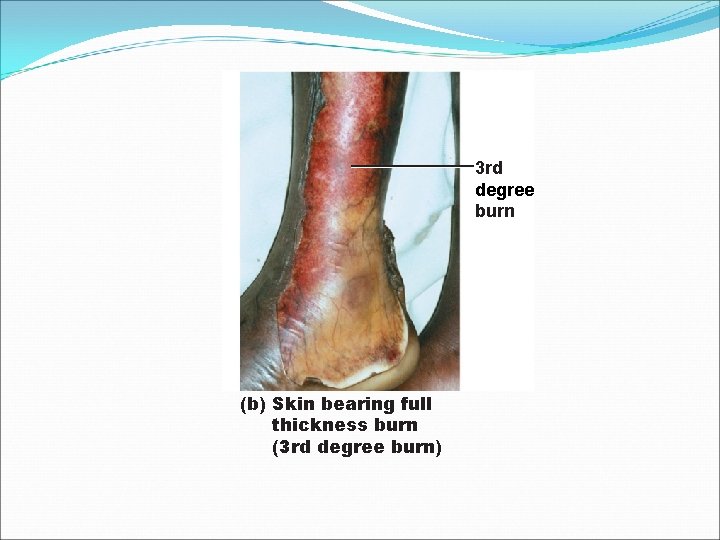
3 rd degree burn (b) Skin bearing full thickness burn (3 rd degree burn)
- Slides: 50