Ch 27 The Reproductive System continued partb 20

Ch 27 The Reproductive System continued … part-b 20 Slides Copyright © 2010 Pearson Education, Inc.
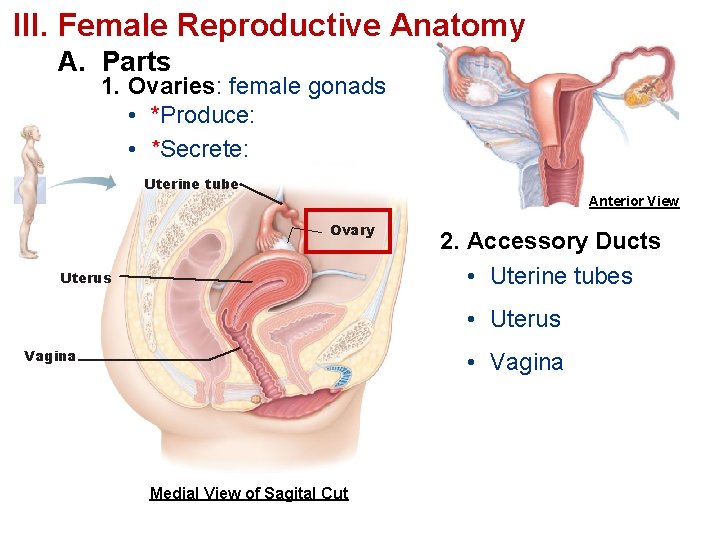
III. Female Reproductive Anatomy A. Parts 1. Ovaries: female gonads • *Produce: • *Secrete: Uterine tube Anterior View Ovary Uterus 2. Accessory Ducts • Uterine tubes • Uterus Vagina • Vagina Medial View of Sagital Cut
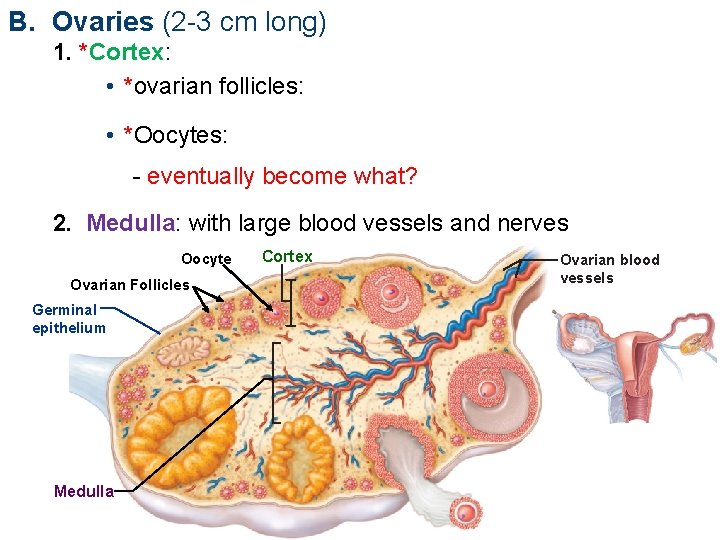
B. Ovaries (2 -3 cm long) 1. *Cortex: • *ovarian follicles: • *Oocytes: - eventually become what? 2. Medulla: with large blood vessels and nerves Oocyte Ovarian Follicles Germinal epithelium Medulla Cortex Ovarian blood vessels
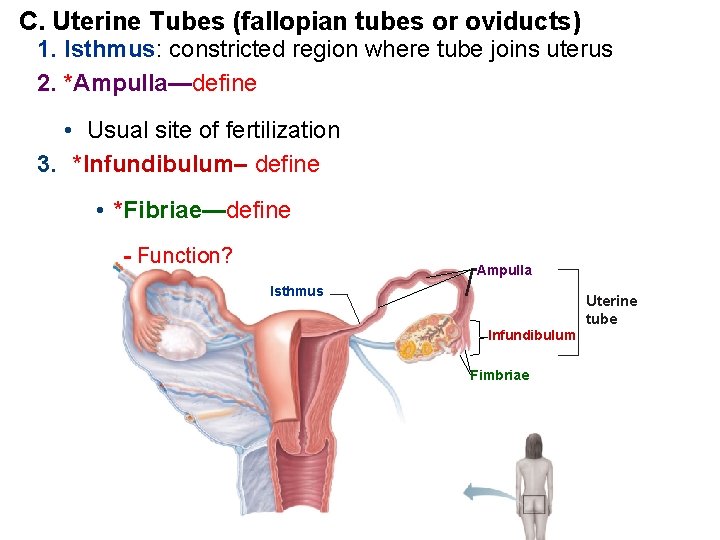
C. Uterine Tubes (fallopian tubes or oviducts) 1. Isthmus: constricted region where tube joins uterus 2. *Ampulla—define • Usual site of fertilization 3. *Infundibulum– define • *Fibriae—define - Function? Ampulla Isthmus Uterine tube Infundibulum Fimbriae
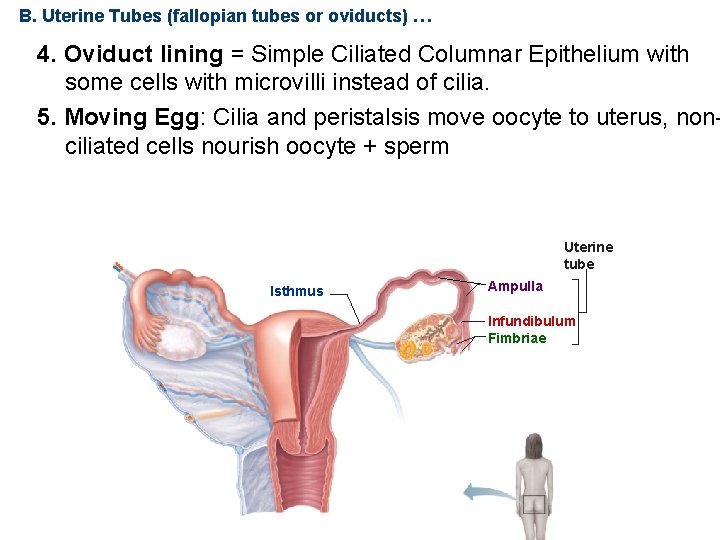
B. Uterine Tubes (fallopian tubes or oviducts) … 4. Oviduct lining = Simple Ciliated Columnar Epithelium with some cells with microvilli instead of cilia. 5. Moving Egg: Cilia and peristalsis move oocyte to uterus, nonciliated cells nourish oocyte + sperm Uterine tube Isthmus Ampulla Infundibulum Fimbriae
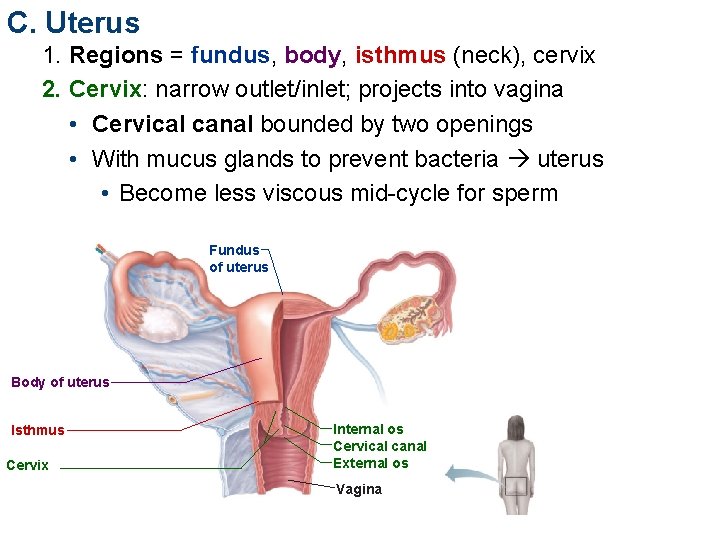
C. Uterus 1. Regions = fundus, body, isthmus (neck), cervix 2. Cervix: narrow outlet/inlet; projects into vagina • Cervical canal bounded by two openings • With mucus glands to prevent bacteria uterus • Become less viscous mid-cycle for sperm Fundus of uterus Body of uterus Isthmus Cervix Internal os Cervical canal External os Vagina
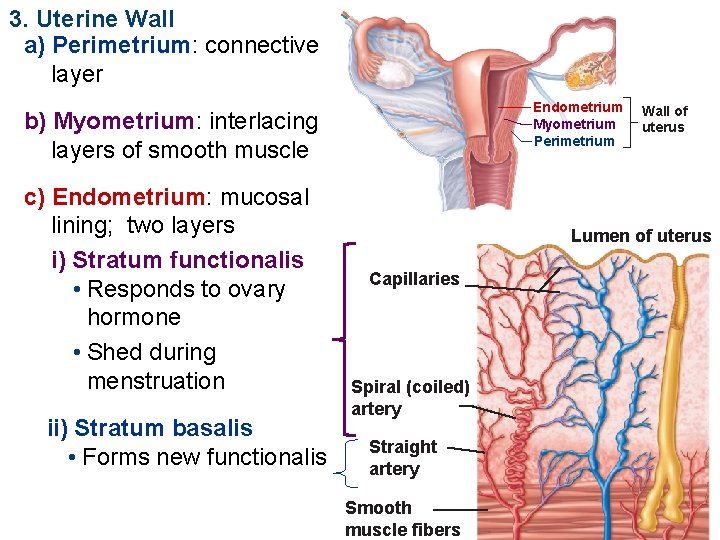
3. Uterine Wall a) Perimetrium: connective layer Endometrium Myometrium Perimetrium b) Myometrium: interlacing layers of smooth muscle c) Endometrium: mucosal lining; two layers i) Stratum functionalis • Responds to ovary hormone • Shed during menstruation ii) Stratum basalis • Forms new functionalis Wall of uterus Lumen of uterus Capillaries Spiral (coiled) artery Straight artery Smooth muscle fibers
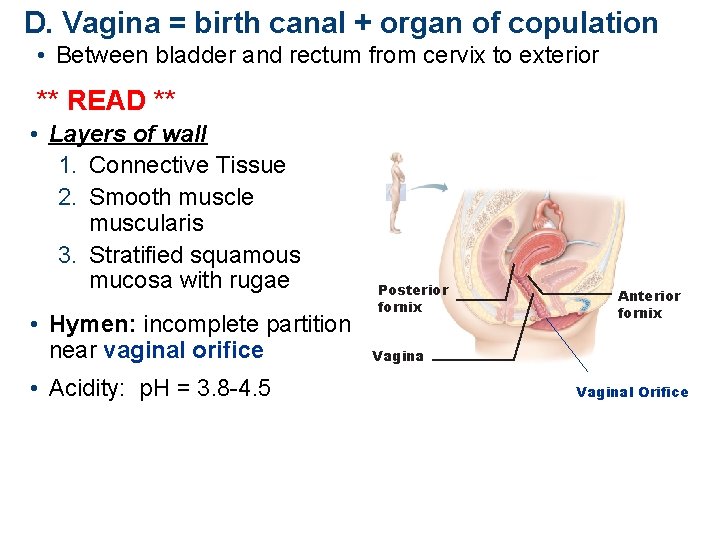
D. Vagina = birth canal + organ of copulation • Between bladder and rectum from cervix to exterior ** READ ** • Layers of wall 1. Connective Tissue 2. Smooth muscle muscularis 3. Stratified squamous mucosa with rugae • Hymen: incomplete partition near vaginal orifice • Acidity: p. H = 3. 8 -4. 5 Posterior fornix Anterior fornix Vaginal Orifice
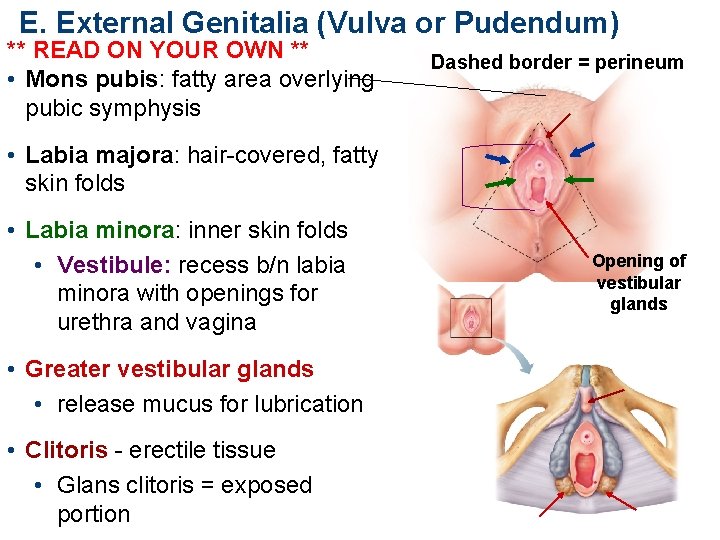
E. External Genitalia (Vulva or Pudendum) ** READ ON YOUR OWN ** • Mons pubis: fatty area overlying pubic symphysis Dashed border = perineum • Labia majora: hair-covered, fatty skin folds • Labia minora: inner skin folds • Vestibule: recess b/n labia minora with openings for urethra and vagina • Greater vestibular glands • release mucus for lubrication • Clitoris - erectile tissue • Glans clitoris = exposed portion Opening of vestibular glands
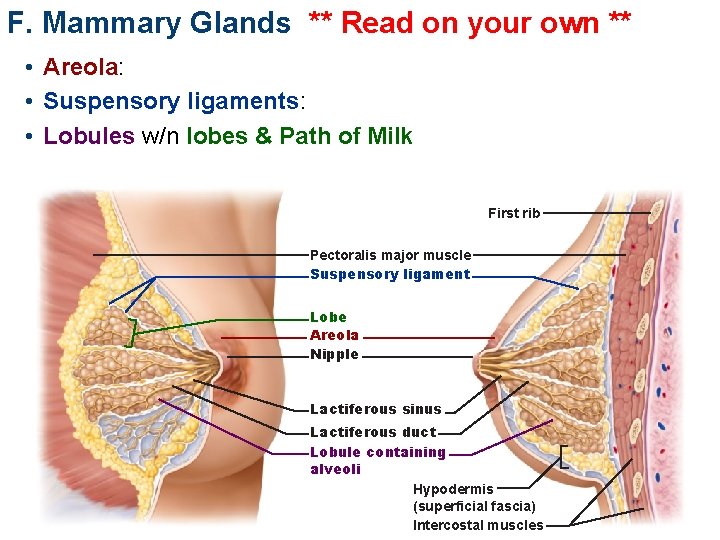
F. Mammary Glands ** Read on your own ** • Areola: • Suspensory ligaments: • Lobules w/n lobes & Path of Milk First rib Pectoralis major muscle Suspensory ligament Lobe Areola Nipple Lactiferous sinus Lactiferous duct Lobule containing alveoli Hypodermis (superficial fascia) Intercostal muscles

IV. Physiology of the Female Reproductive System Introduction • Oogenesis • 7 Million potential eggs at birth are in growth area called-- Follicle • ¼ Million left by puberty • 500 will ovulate during lifetime • Ovarian Cycle: Events associated with the maturation of an egg • Occurs Monthly • Uterine Cycle: Series of cyclic changes that the uterus undergoes each month • Occurs Monthly Copyright © 2010 Pearson Education, Inc.

A. Oogenesis = production of female gametes 1. Fetus • Oogonia (2 n ovarian stem cells) multiply and store nutrients • Primary oocytes develop in primordial follicles • Primary oocytes begin meiosis but do not finish 2. Infancy and Meiotic events Follicle development in ovary Before birth Childhood: Oogonium (stem cell) • ovary is inactive and Mitosis produces very low Infancy and Estrogen Primary oocyte Primordial follicle childhood) (arrested in prophase I; • low levels inhibit present at birth) release of Gn. RH At Puberty 3. Puberty a) Hypothalamus releases Gn. RH (Day 1) i) Pituitary hormones LH and FSH are then released and a few primary oocytes starts up their development ii) Puberty Only If adequate fat present (produces Leptin) ↑ Leptin stops estrogen inhibition of hypoth. Follicle cells Oocyte Primary oocyte Each month from puberty to menopause
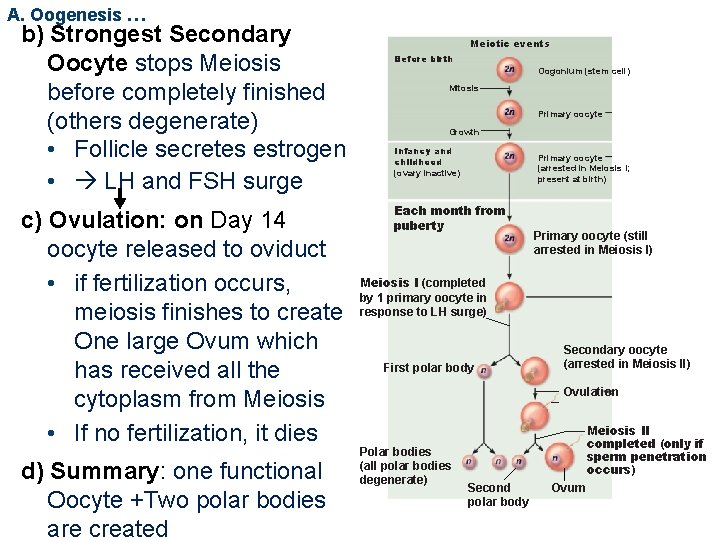
A. Oogenesis … b) Strongest Secondary Oocyte stops Meiosis before completely finished (others degenerate) • Follicle secretes estrogen • LH and FSH surge c) Ovulation: on Day 14 oocyte released to oviduct • if fertilization occurs, meiosis finishes to create One large Ovum which has received all the cytoplasm from Meiosis • If no fertilization, it dies d) Summary: one functional Oocyte +Two polar bodies are created Meiotic events Before birth Oogonium (stem cell) Mitosis Primary oocyte Growth Infancy and childhood (ovary inactive) Primary oocyte (arrested in Meiosis I; present at birth) Each month from puberty Primary oocyte (still arrested in Meiosis I) Meiosis I (completed by 1 primary oocyte in response to LH surge) First polar body Secondary oocyte (arrested in Meiosis II) Ovulation Polar bodies (all polar bodies degenerate) Meiosis II completed (only if sperm penetration occurs) Second polar body Ovum
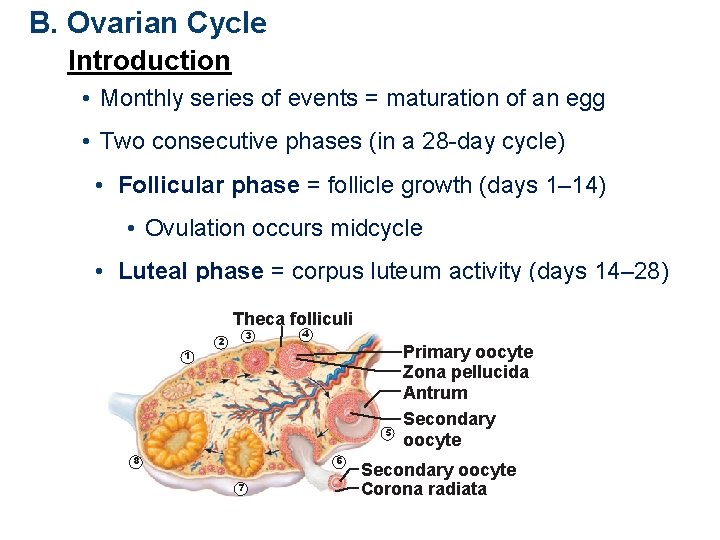
B. Ovarian Cycle Introduction • Monthly series of events = maturation of an egg • Two consecutive phases (in a 28 -day cycle) • Follicular phase = follicle growth (days 1– 14) • Ovulation occurs midcycle • Luteal phase = corpus luteum activity (days 14– 28) Theca folliculi 3 2 4 1 5 6 8 7 Primary oocyte Zona pellucida Antrum Secondary oocyte Corona radiata
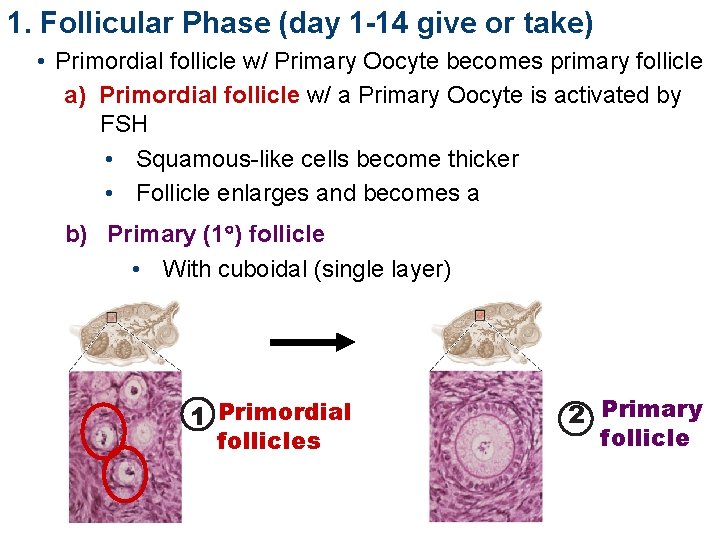
1. Follicular Phase (day 1 -14 give or take) • Primordial follicle w/ Primary Oocyte becomes primary follicle a) Primordial follicle w/ a Primary Oocyte is activated by FSH • Squamous-like cells become thicker • Follicle enlarges and becomes a b) Primary (1 ) follicle • With cuboidal (single layer) 1 Primordial follicles 2 Primary follicle
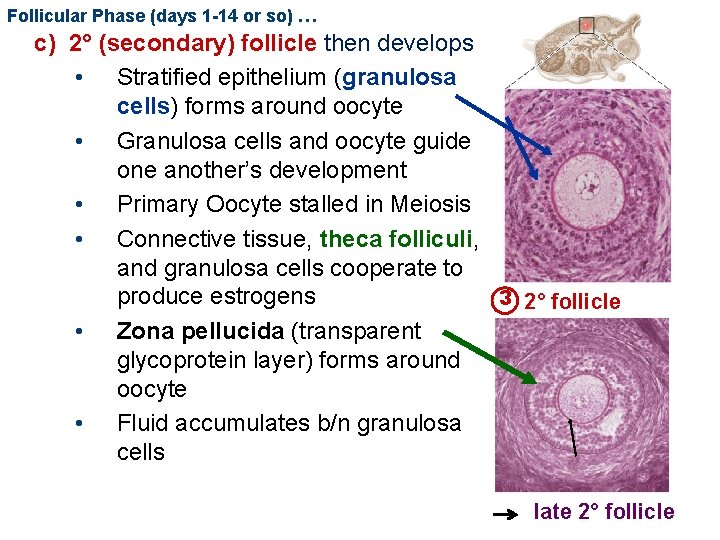
Follicular Phase (days 1 -14 or so) … c) 2° (secondary) follicle then develops • Stratified epithelium (granulosa cells) forms around oocyte • Granulosa cells and oocyte guide one another’s development • Primary Oocyte stalled in Meiosis • Connective tissue, theca folliculi, and granulosa cells cooperate to produce estrogens 3 2° follicle • Zona pellucida (transparent glycoprotein layer) forms around oocyte • Fluid accumulates b/n granulosa cells late 2° follicle
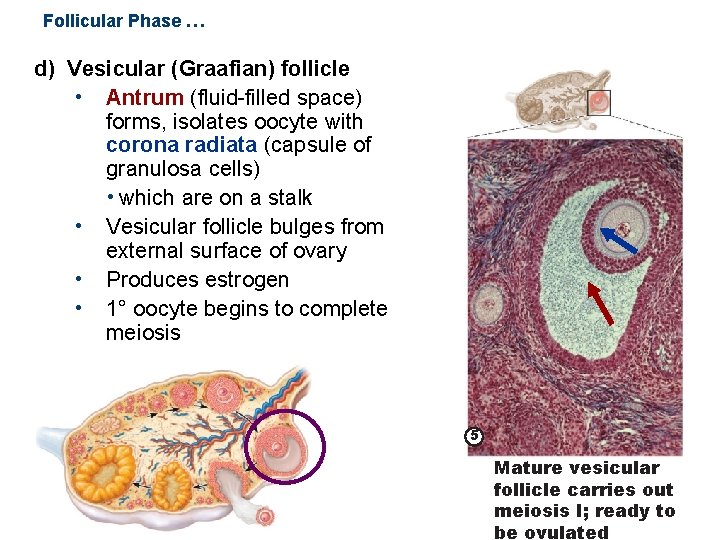
Follicular Phase … d) Vesicular (Graafian) follicle • Antrum (fluid-filled space) forms, isolates oocyte with corona radiata (capsule of granulosa cells) • which are on a stalk • Vesicular follicle bulges from external surface of ovary • Produces estrogen • 1° oocyte begins to complete meiosis 5 Mature vesicular follicle carries out meiosis I; ready to be ovulated

2. Ovulation a) Just before Ovulation, Primary Oocyte becomes a Secondary Oocyte • But still does not complete Meiosis b) Ovary wall ruptures, expels 2°oocyte with Corona Radiata • Triggered by LH surge Theca folliculi 3 2 4 1 6 8 7 Primary oocyte Zona pellucida Antrum Secondary 5 oocyte 6 Follicle ruptures; secondary oocyte Secondary oocyte Corona radiata ovulated
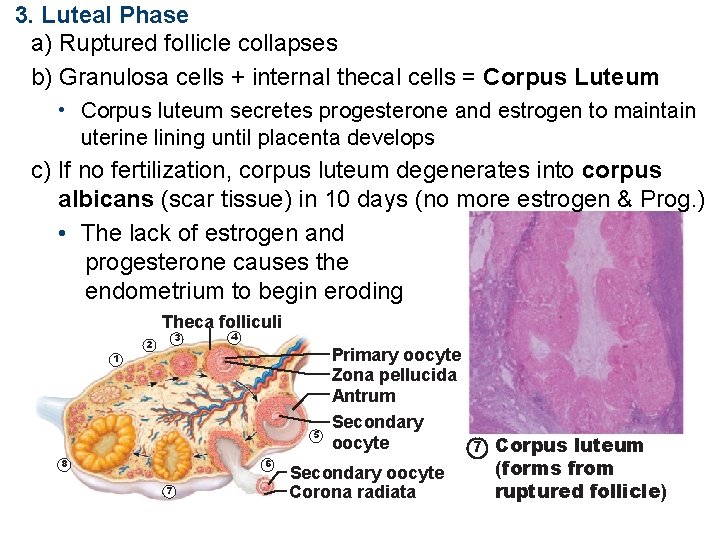
3. Luteal Phase a) Ruptured follicle collapses b) Granulosa cells + internal thecal cells = Corpus Luteum • Corpus luteum secretes progesterone and estrogen to maintain uterine lining until placenta develops c) If no fertilization, corpus luteum degenerates into corpus albicans (scar tissue) in 10 days (no more estrogen & Prog. ) • The lack of estrogen and progesterone causes the endometrium to begin eroding Theca folliculi 3 2 4 1 6 8 7 Primary oocyte Zona pellucida Antrum Secondary 5 oocyte 7 Corpus luteum (forms from Secondary oocyte ruptured follicle) Corona radiata
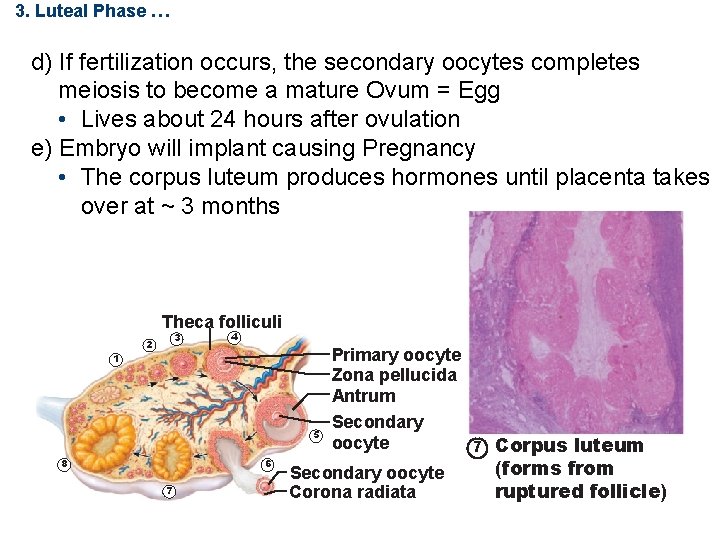
3. Luteal Phase … d) If fertilization occurs, the secondary oocytes completes meiosis to become a mature Ovum = Egg • Lives about 24 hours after ovulation e) Embryo will implant causing Pregnancy • The corpus luteum produces hormones until placenta takes over at ~ 3 months Theca folliculi 3 2 4 1 6 8 7 Primary oocyte Zona pellucida Antrum Secondary 5 oocyte 7 Corpus luteum (forms from Secondary oocyte ruptured follicle) Corona radiata
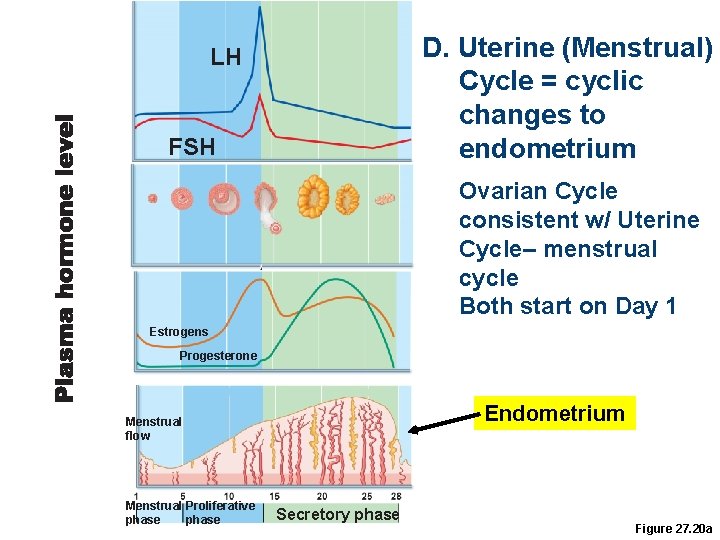
D. Uterine (Menstrual) Cycle = cyclic changes to endometrium LH FSH Ovarian Cycle consistent w/ Uterine Cycle– menstrual cycle Both start on Day 1 Estrogens Progesterone Endometrium Menstrual flow Menstrual Proliferative phase Secretory phase Figure 27. 20 a

D. Uterine (Menstrual) Cycle … Three phases 1. Days 1– 5: menstrual phase – low hormone levels stratum functionalis is shed 2. Days 6– 14: proliferative (preovulatory) phase – estrogen ↑, new functional layer develops (w/ progesterone receptors) 3. Days 15– 28: secretory (postovulatory) phase – progesterone ↑ = glands secrete glycogen, mucus plug reforms (endometrium prepared for implantation) • If no pregnancy, cycle begins again Endometrial glands Spiral Arteries Menstrual Flow = shed stratum functionalis Functional layer Basal layer Days Menstrual phase Proliferative phase Secretory phase
E. Effects of Sex Hormones ** Read On Your Own ** 1. Effects of Estrogens • Promote oogenesis and follicle growth • Maturation of female reproductive tract/breasts • Induce 2°sex characters – widened, lightened pelvis; subcutaneous fat deposits of hips/breasts • Support growth spurt at puberty • Enhances Ca 2+ uptake 2. Effects of Progesterone • Works w/ estrogen to regulate uterine cycle • During Pregnancy: placental progesterone • Inhibits uterine motility • Helps prepare breasts for lactation

F. Female Sexual Response ** READ ** • Clitoris, vaginal mucosa, and breasts engorge with blood (sensitive like head of penis) • Vestibular gland lubricates vestibule • Orgasm occurs, but not required for conception; • Function
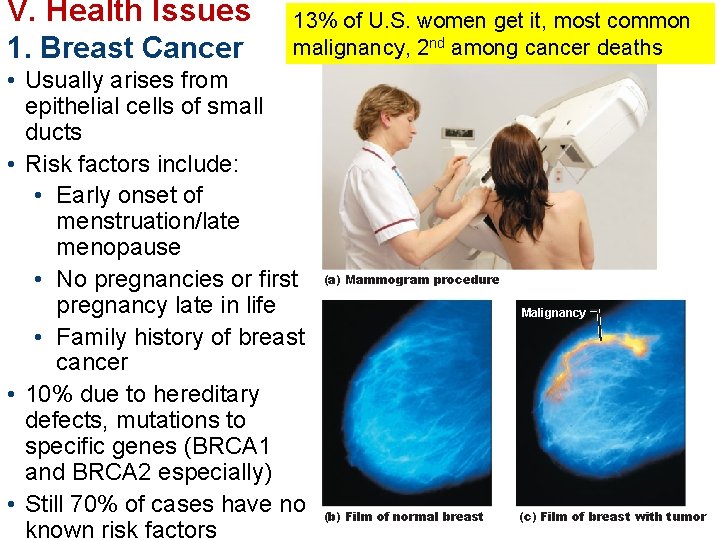
V. Health Issues 1. Breast Cancer 13% of U. S. women get it, most common malignancy, 2 nd among cancer deaths • Usually arises from epithelial cells of small ducts • Risk factors include: • Early onset of menstruation/late menopause • No pregnancies or first pregnancy late in life • Family history of breast cancer • 10% due to hereditary defects, mutations to specific genes (BRCA 1 and BRCA 2 especially) • Still 70% of cases have no known risk factors (a) Mammogram procedure Malignancy (b) Film of normal breast (c) Film of breast with tumor

2. Menopause ** READ ** • = Menses cease for entire year and no more ovulation: WHY? > 55 pregnancy is much more dangerous • No equivalent in males • Declining estrogen levels • Atrophy: of reproductive organs/breasts • Mood: Irritability and depression in some • Blood Vessels: Hot flashes as skin blood vessels undergo intense vasodilation • Loss of cells: Gradual thinning of skin and bone loss • Increased cholesterol levels/falling HDL
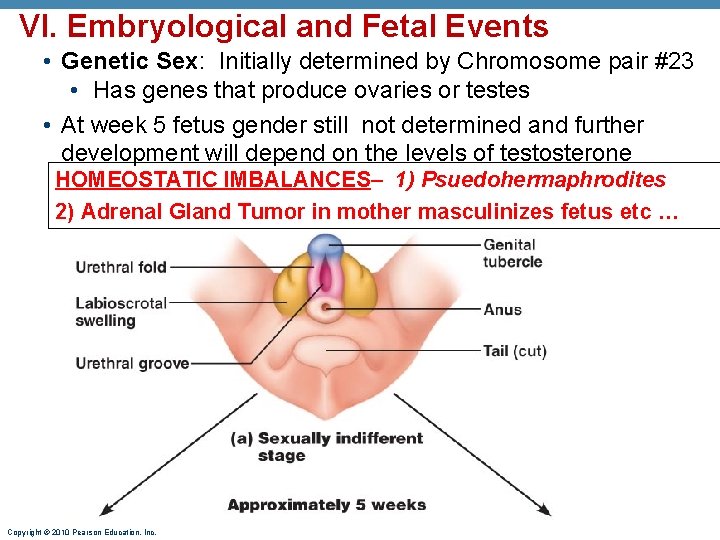
VI. Embryological and Fetal Events • Genetic Sex: Initially determined by Chromosome pair #23 • Has genes that produce ovaries or testes • At week 5 fetus gender still not determined and further development will depend on the levels of testosterone HOMEOSTATIC IMBALANCES– 1) Psuedohermaphrodites 2) Adrenal Gland Tumor in mother masculinizes fetus etc … Copyright © 2010 Pearson Education, Inc.
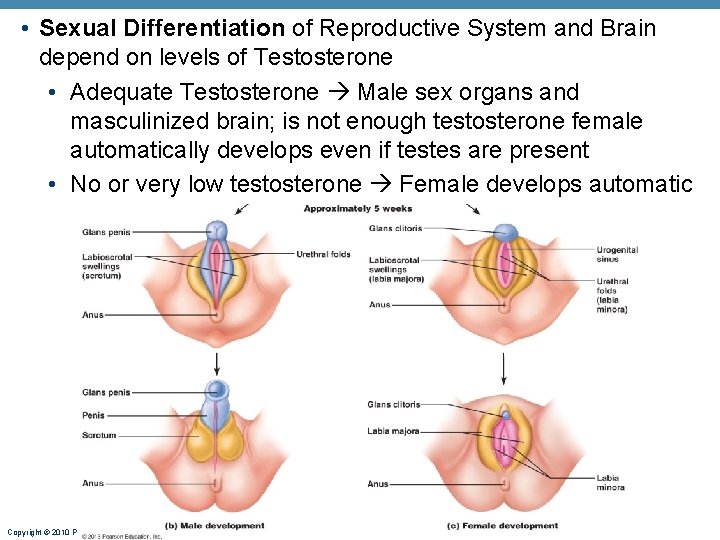
• Sexual Differentiation of Reproductive System and Brain depend on levels of Testosterone • Adequate Testosterone Male sex organs and masculinized brain; is not enough testosterone female automatically develops even if testes are present • No or very low testosterone Female develops automatic Copyright © 2010 Pearson Education, Inc.

• END Copyright © 2010 Pearson Education, Inc.
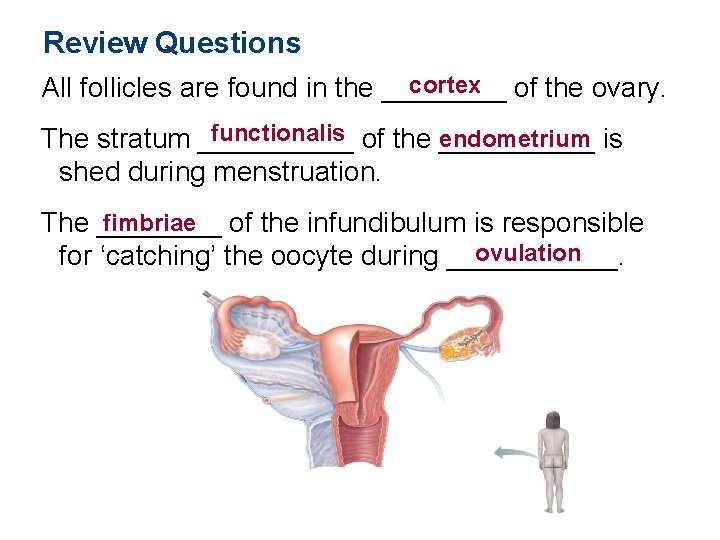
Review Questions cortex of the ovary. All follicles are found in the ____ functionalis of the endometrium The stratum __________ is shed during menstruation. fimbriae of the infundibulum is responsible The ____ ovulation for ‘catching’ the oocyte during ______.
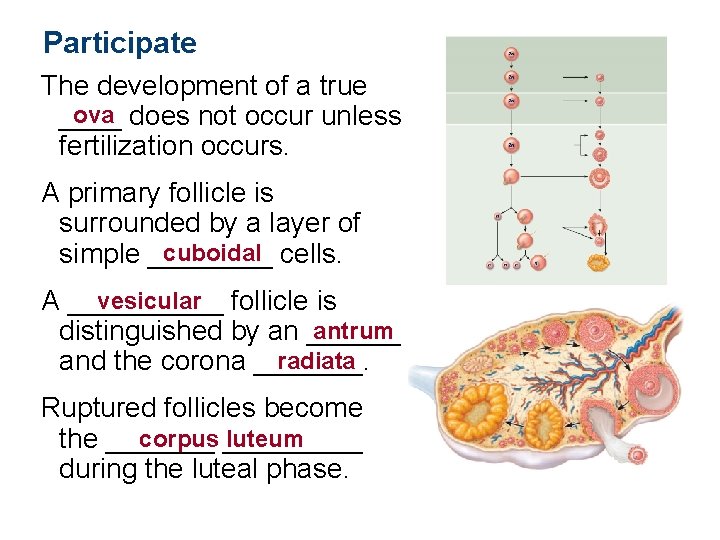
Participate The development of a true ova does not occur unless ____ fertilization occurs. A primary follicle is surrounded by a layer of cuboidal cells. simple ____ vesicular follicle is A _____ antrum distinguished by an ______ radiata and the corona _______. Ruptured follicles become corpus _____ luteum the _______ during the luteal phase.
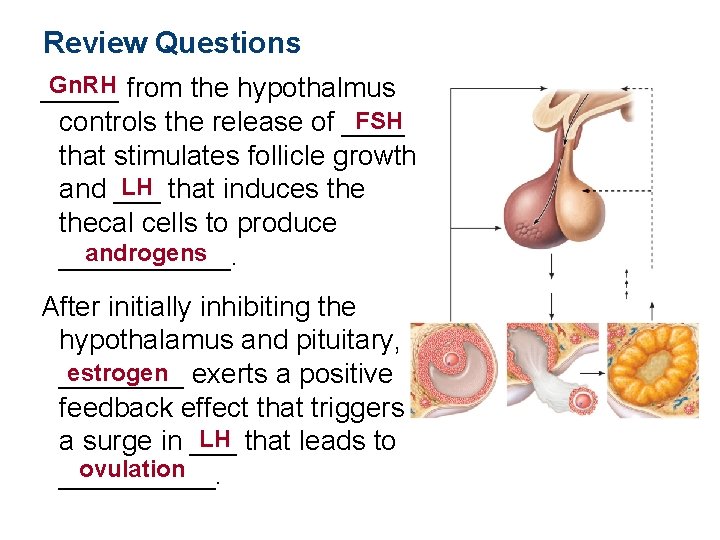
Review Questions Gn. RH from the hypothalmus _____ FSH controls the release of ____ that stimulates follicle growth LH that induces the and ___ thecal cells to produce androgens ______. After initially inhibiting the hypothalamus and pituitary, estrogen exerts a positive ____ feedback effect that triggers LH that leads to a surge in ___ ovulation _____.
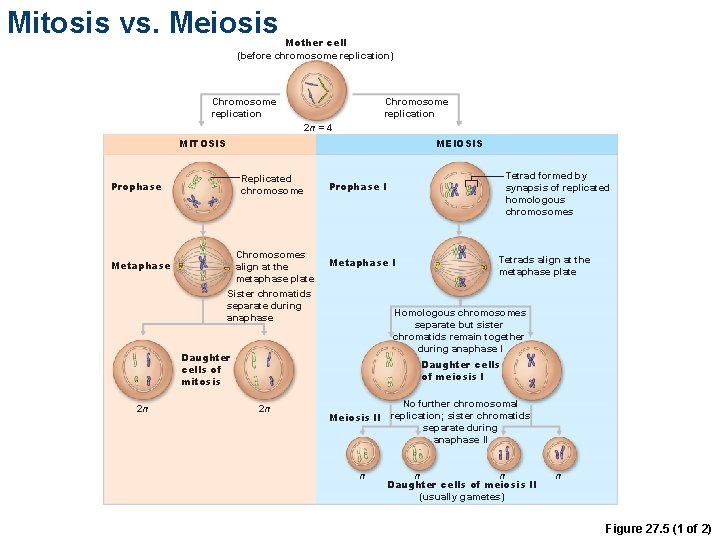
Mitosis vs. Meiosis Mother cell (before chromosome replication) Chromosome replication 2 n = 4 MITOSIS MEIOSIS Replicated chromosome Prophase Metaphase Chromosomes align at the metaphase plate Sister chromatids separate during anaphase Metaphase I Tetrads align at the metaphase plate Homologous chromosomes separate but sister chromatids remain together during anaphase I Daughter cells of mitosis 2 n Tetrad formed by synapsis of replicated homologous chromosomes Prophase I Daughter cells of meiosis I 2 n No further chromosomal replication; sister chromatids Meiosis II separate during anaphase II n n n Daughter cells of meiosis II (usually gametes) n Figure 27. 5 (1 of 2)
- Slides: 33