Cerebrovascular disease CVD CVA STROKE Brain Attack Rapidly


Cerebrovascular disease CVD (CVA) STROKE Brain Attack “Rapidly developed clinical signs of focal(global) disturbance of cerebral function lasting more than 24 hours or leading to death, with no apparent cause other than a vascular origin. ”

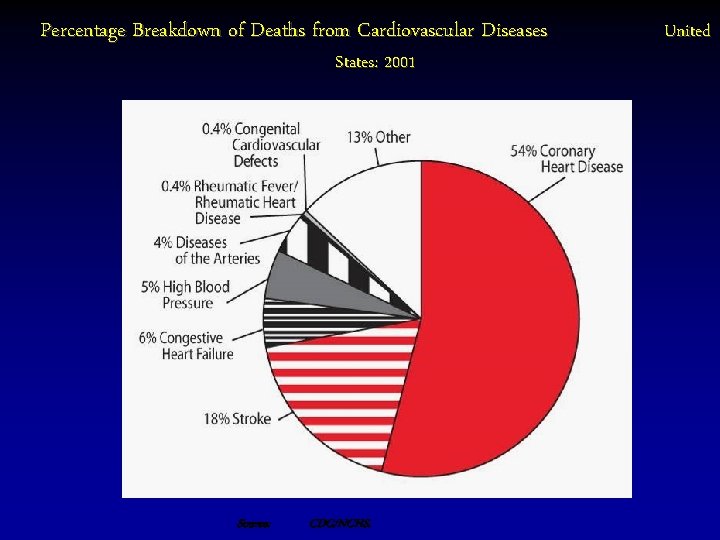
Percentage Breakdown of Deaths from Cardiovascular Diseases States: 2001 Source: CDC/NCHS. United
Magnitude of disease o Vascular disease in USA / Europe 3: 1
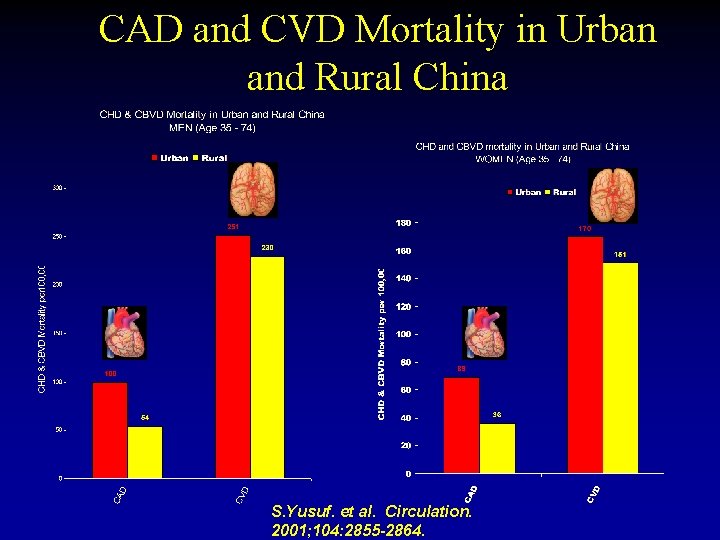
CAD and CVD Mortality in Urban and Rural China S. Yusuf. et al. Circulation. 2001; 104: 2855 -2864.
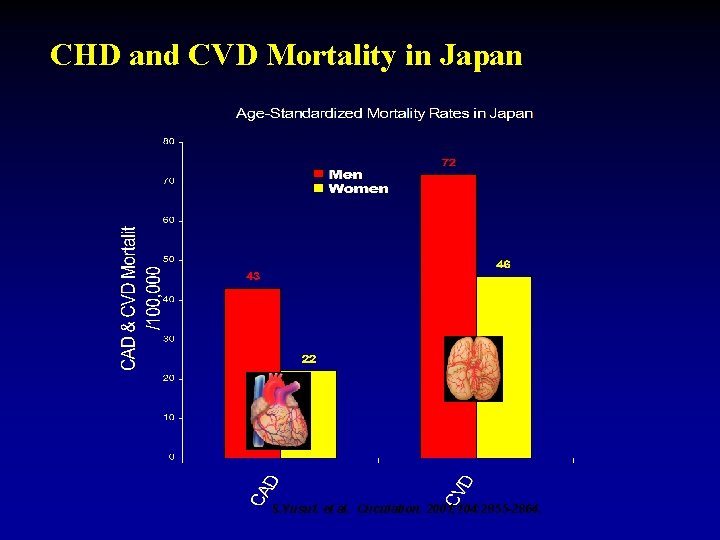
CHD and CVD Mortality in Japan S. Yusuf. et al. Circulation. 2001; 104: 2855 -2864.
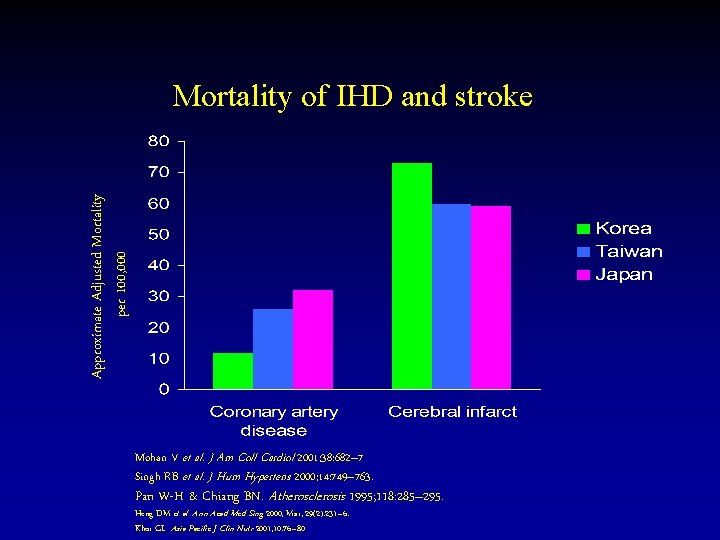
Approximate Adjusted Mortality per 100, 000 Mortality of IHD and stroke Mohan V et al. J Am Coll Cardiol 2001; 38: 682– 7 Singh RB et al. J Hum Hypertens 2000; 14: 749– 763. Pan W-H & Chiang BN. Atherosclerosis 1995; 118: 285– 295. Heng DM et al. Ann Acad Med Sing 2000; Mar; 29(2): 231– 6. Khor GL. Asia Pacific J Clin Nutr 2001; 10: 76– 80
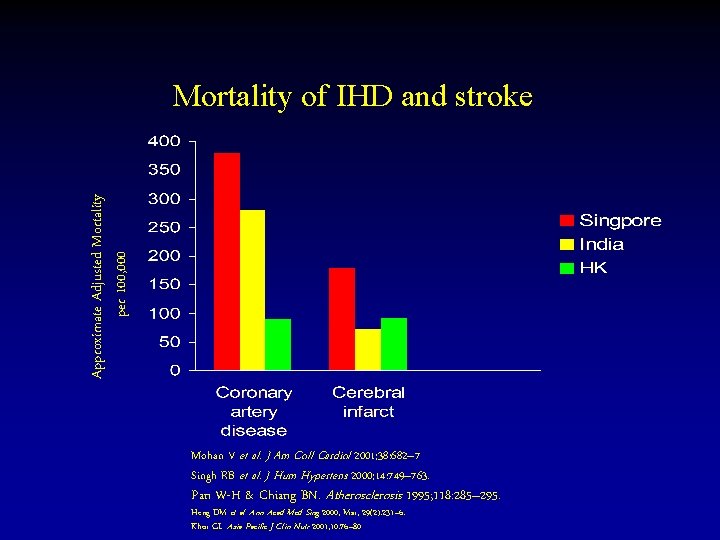
Approximate Adjusted Mortality per 100, 000 Mortality of IHD and stroke Mohan V et al. J Am Coll Cardiol 2001; 38: 682– 7 Singh RB et al. J Hum Hypertens 2000; 14: 749– 763. Pan W-H & Chiang BN. Atherosclerosis 1995; 118: 285– 295. Heng DM et al. Ann Acad Med Sing 2000; Mar; 29(2): 231– 6. Khor GL. Asia Pacific J Clin Nutr 2001; 10: 76– 80

The top killers in Thailand 1999 (Male) Diseases Deaths % 1. HIVAIDS 40, 064 18 2. Traffic accidents 21, 901 10 3. Stroke 18, 286 8 4. Liver cancer 13, 774 6 5. COPD 10, 977 5 6. Ischemic heart disease 9, 734 4 7. Homicide/Violence 6, 786 3 8. Suicides 6, 671 3 9. Lung cancer 6, 461 3 10. Diabetes 6, 223 3 ����� : Burden of disease and injuries in Thailand: Minstry of Public Health Nov 2002 (http: //203: 157. 191/index-burden. htm)

Top 10 killers in Thailand 1999 (Female) Diseases 1. Stroke 2. HIVIAIDS 3. Diabetes 4. Ischemic heart disease 5. Liver cancer 6. Lower respiratory tract infection 7. Traffic accident 8. COPD 9. Tuberculosis 10. Nephritis & Nephrosis Deaths 23, 433 16, 443 12, 235 8, 089 7, 938 5, 521 5, 330 5, 132 4, 413 4, 123 % 14 10 7 5 3 3 3 2 ����� : Burden of disease and injuries in Thailand: Minstry of Public Health Nov 2002 (http: //203: 157. 191/index-burden. htm)
Magnitude of disease o Vascular disease in Asia (Chinese / Japanese / Korea/Thai) 1: 3

Stroke Mortality in Thailand • A leading cause of serious, long-term disability • >40, 000 new or recurrent strokes occur per year in Thailand • 1 death due to stroke every 12 minutes
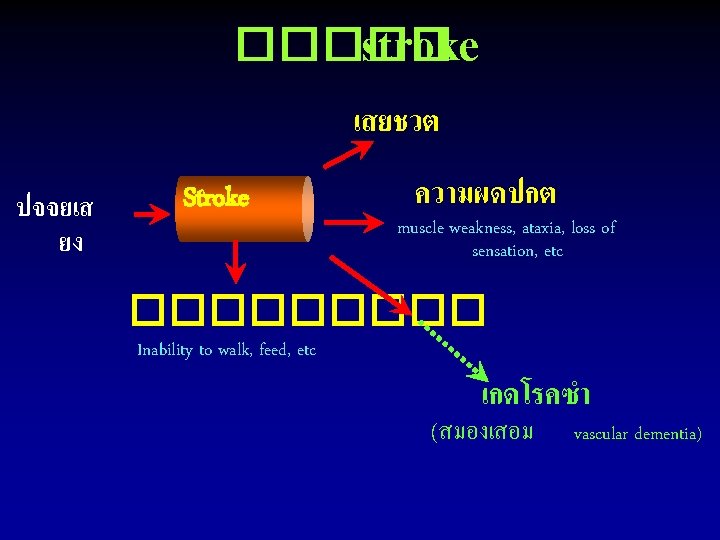
����� stroke เสยชวต ปจจยเส ยง Stroke ความผดปกต muscle weakness, ataxia, loss of sensation, etc ����� Inability to walk, feed, etc เกดโรคซำ (สมองเสอม vascular dementia)



Epidemiology of stroke in the elderly Thailand Viriyavejakul A, Senanarong V, Prayoonwiwat N. J Med Assoc Thai 1998; 81(7) 497 • • 3036 Thai elderly (>60 years old) from 4 regions Nakhonpathom, Lampang, Sakonnakon, Ranong Aug 1994 -oct 1996 34 strokes were identified (Prevalence 1. 12%) =112/100, 000 + fatal cases
Cost of stroke • Acute hospitalization – 10, 000 -200, 000 Bht • Cost of medicine and rehabilitation after discharge • Indirect costs

Transient Ischemic Attack (TIA) • Episodes of temporary and focal cerebral dysfunction of vascular (occlusive) origin. • Lasting < 24 hours
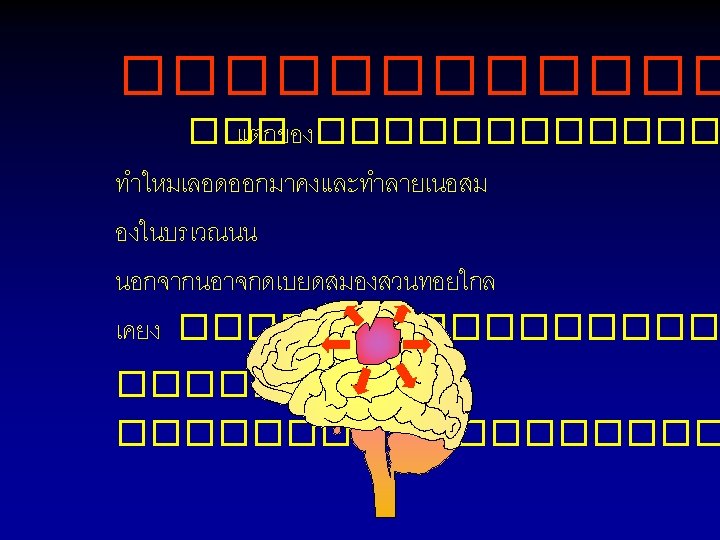
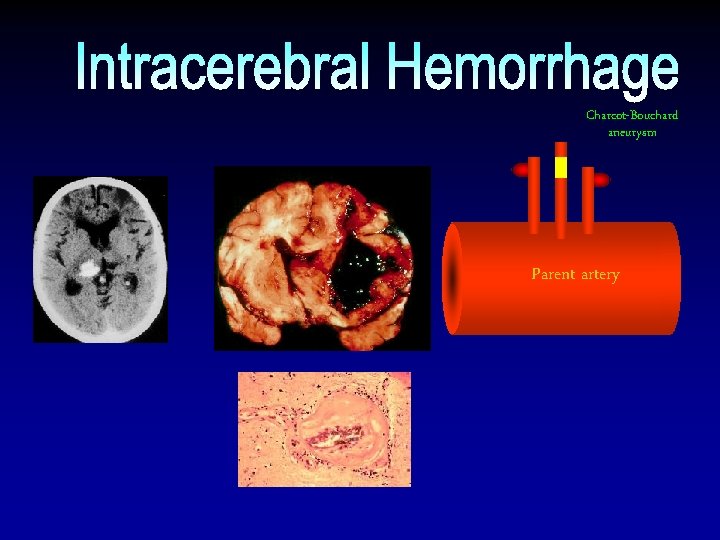
Charcot-Bouchard aneurysm Parent artery



�������� Non-modifiable Stroke Factors Age, Gender, Risk Race, Heredity ������� Modifiable Medical Conditions • • • Hypertension Cardiac disease Atrial fibrillation Dyslipidemia Diabetes mellitus Carotid stenosis Prior TIA or stroke Elevated homocysteine Atherosclerosis of aorta Behaviors l Cigarette smoking l Alcohol abuse l Physical inactivity Sacco RL, et al. Stroke 1997; 28: 1507 -1517. Pancioli AM, et al. JAMA 1998; 279: 1288 -1292.
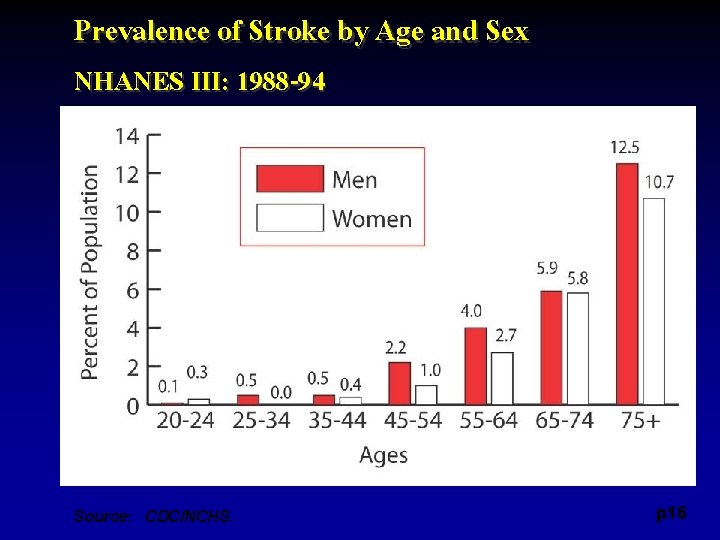
Prevalence of Stroke by Age and Sex NHANES III: 1988 -94 Source: CDC/NCHS. p 16

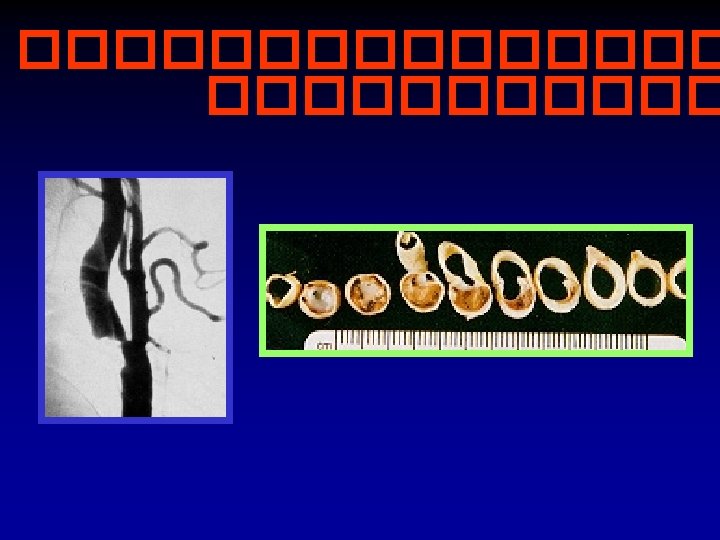

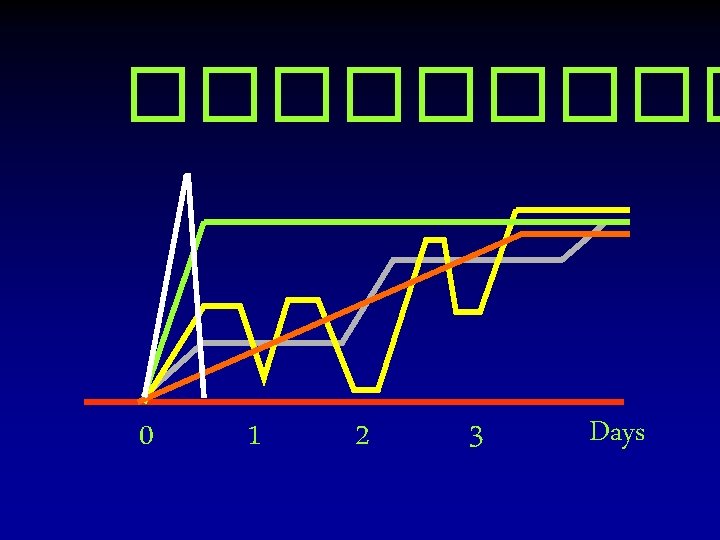
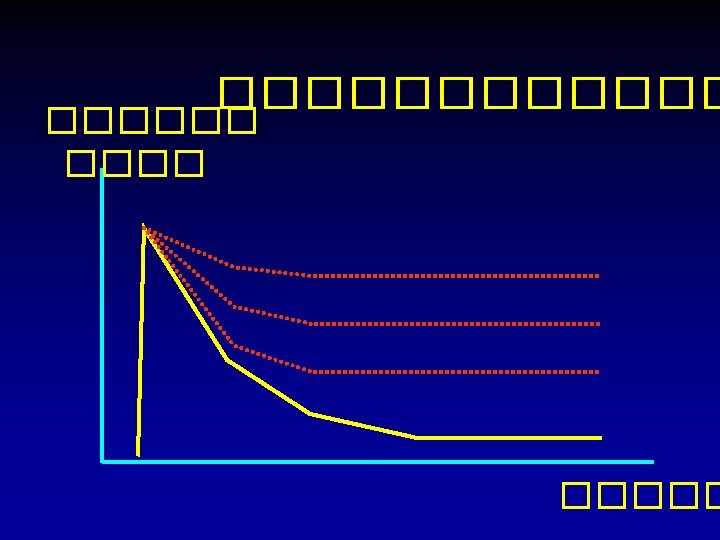
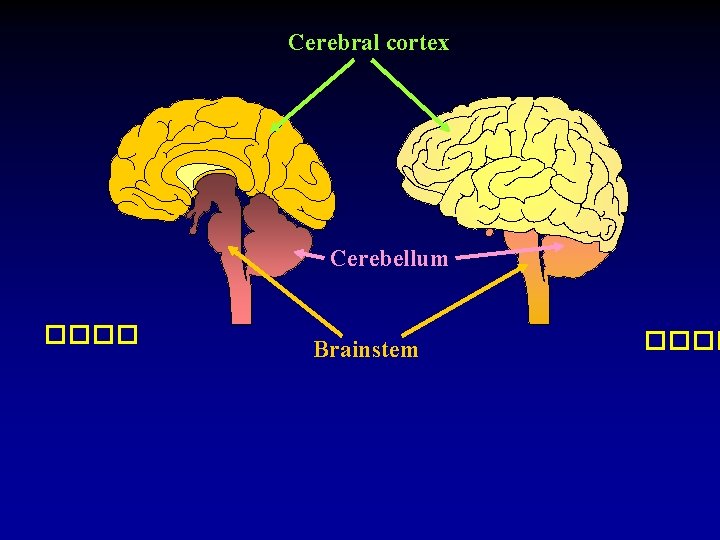
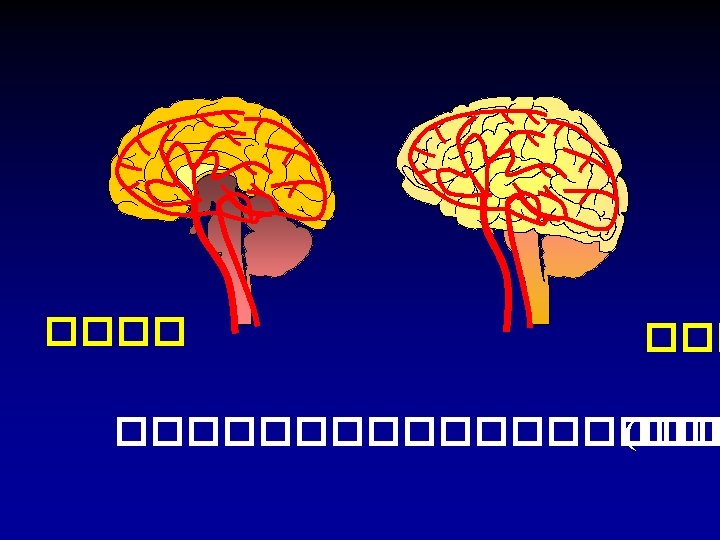
Cerebral cortex Cerebellum ���� Brainstem ����
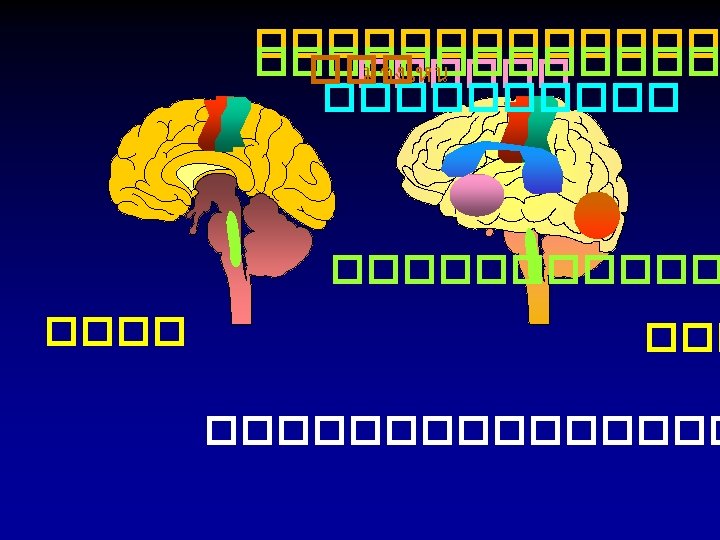






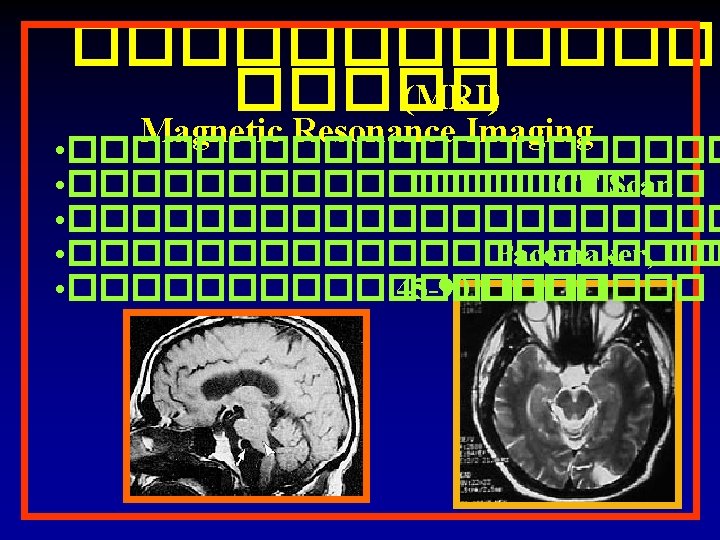
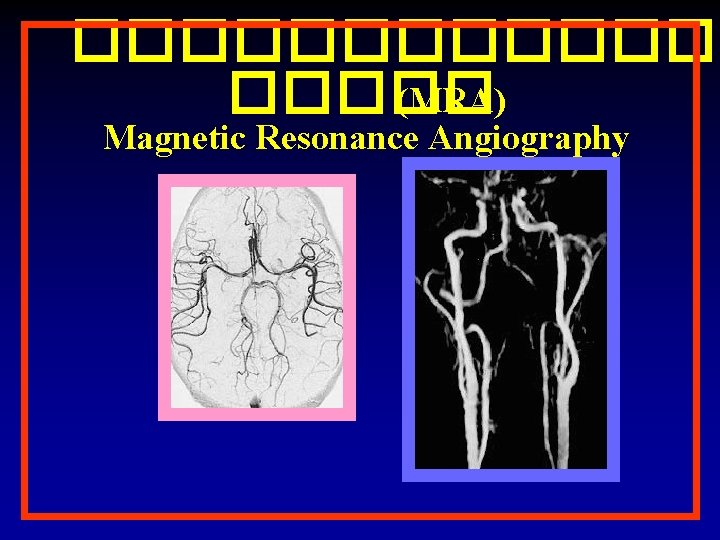
������� (MRA) Magnetic Resonance Angiography
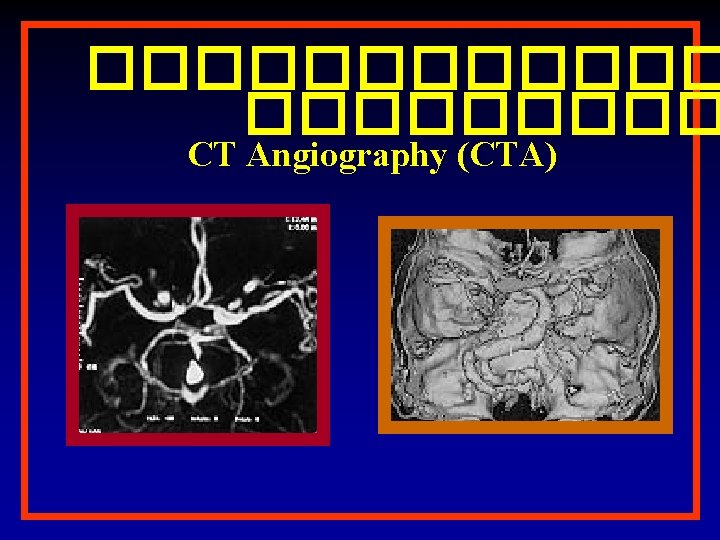
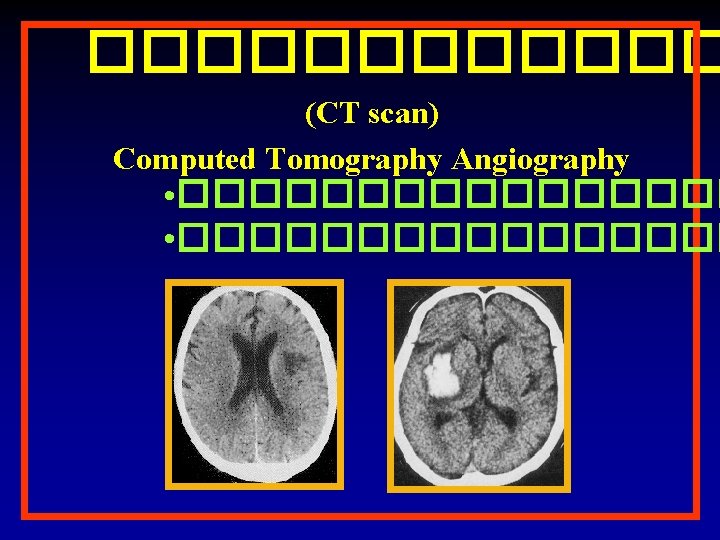
������ CT Angiography (CTA)
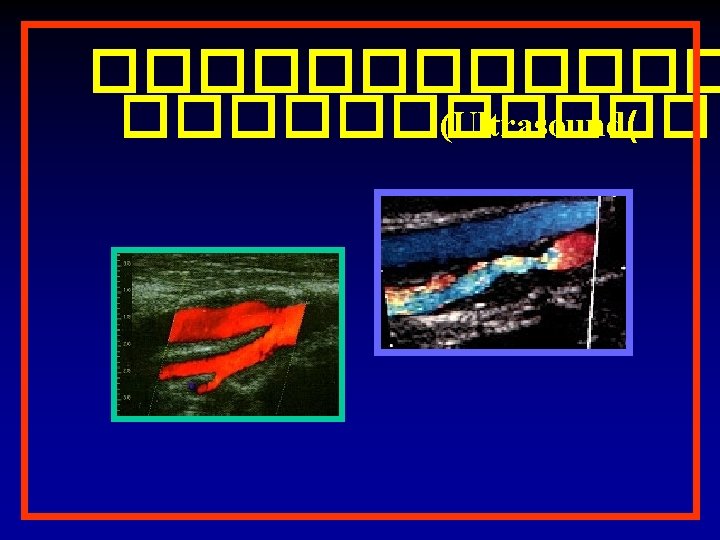
������ (Ultrasound(

Consider Thrombolytic Treatment Onset 3 hr CT neg Inclusion Exclusion
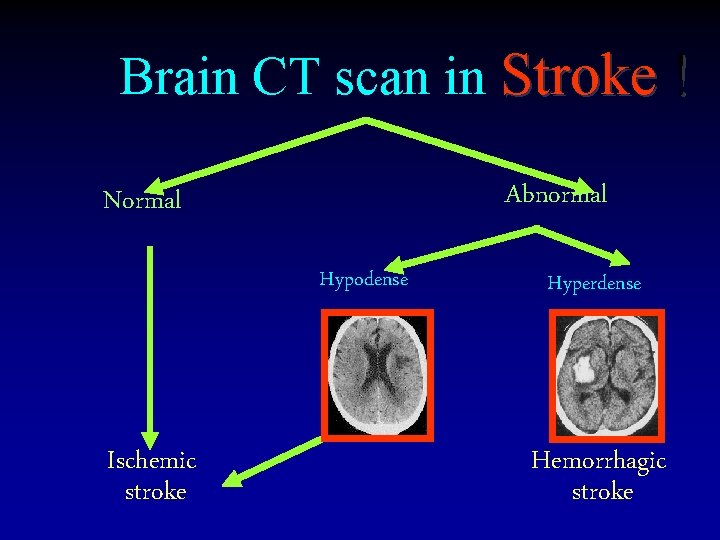
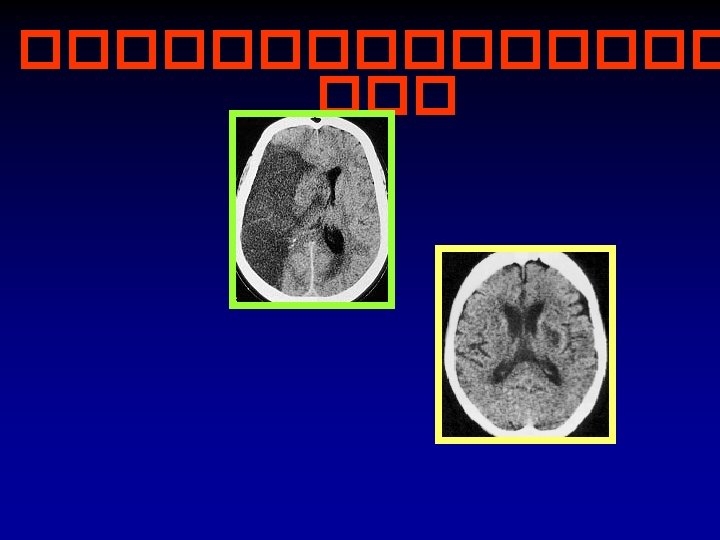
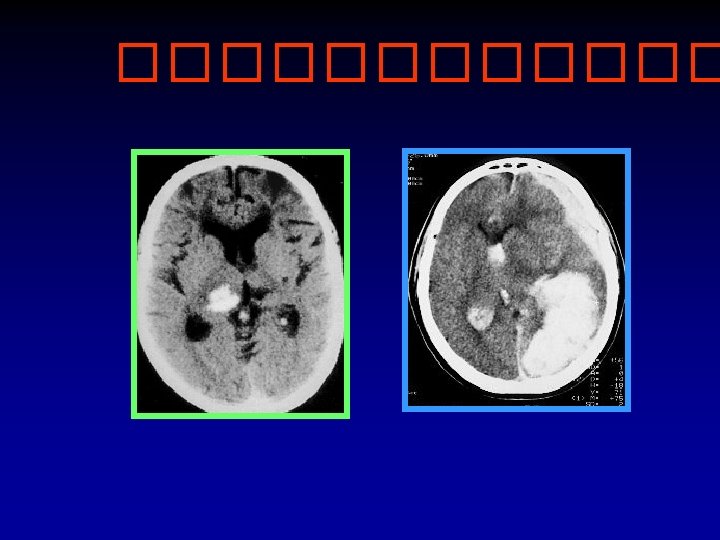
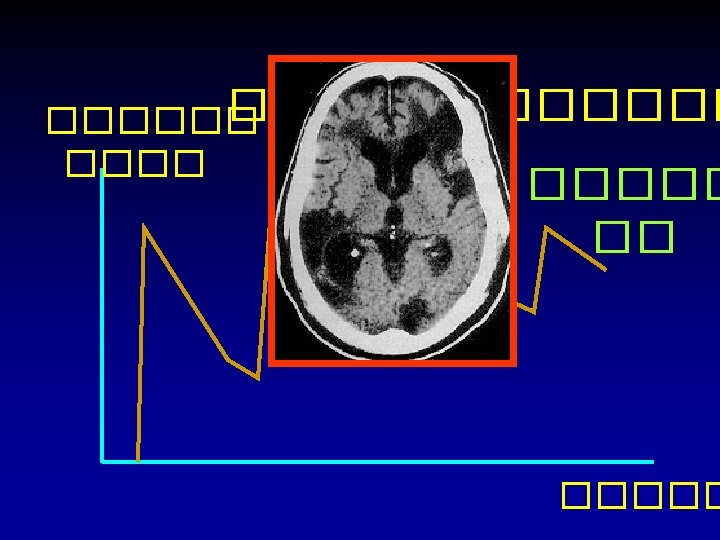
Brain CT scan in Stroke ! Abnormal Normal Hypodense Ischemic stroke Hyperdense Hemorrhagic stroke

Dosage 10% bolus in 1 min 90% infuse in 60 min

Nijasri C Suwanwela, et al Clin Neurol Neurosurg 2005 34 Thrombolysis (2. 1%) 164 within 3 hours (9. 8%) 1624 Acute ischemic stroke
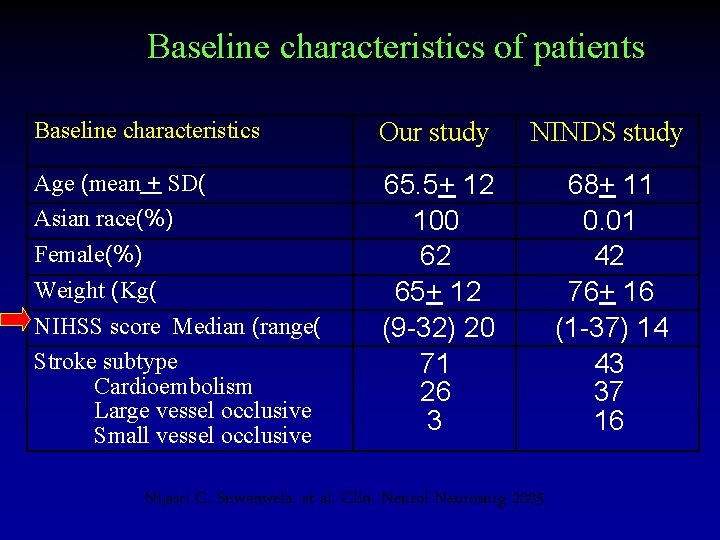
Baseline characteristics of patients Baseline characteristics Our study NINDS study Age (mean + SD( Asian race(%) Female(%) Weight (Kg( NIHSS score Median (range( Stroke subtype Cardioembolism Large vessel occlusive Small vessel occlusive 65. 5+ 12 100 62 65+ 12 (9 -32) 20 71 26 3 68+ 11 0. 01 42 76+ 16 (1 -37) 14 43 37 16 Nijasri C. Suwanwela, et al. Clin. Neurol Neurosurg 2005
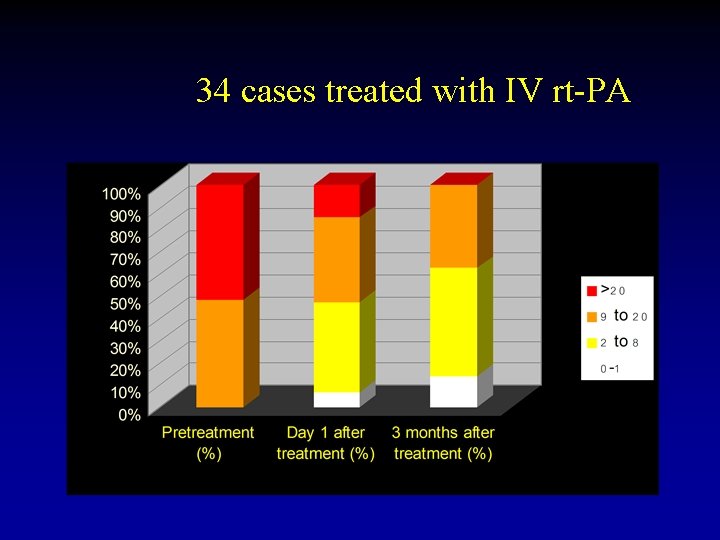
34 cases treated with IV rt-PA NIHSS
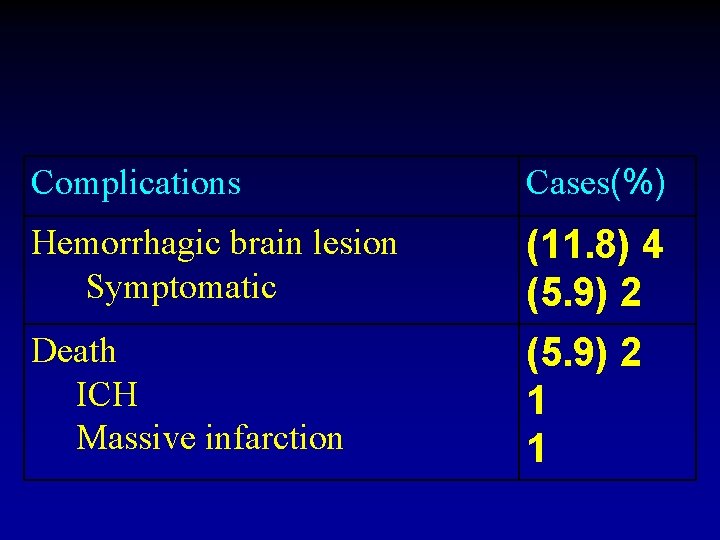
Complications Cases(%) Hemorrhagic brain lesion Symptomatic (11. 8) 4 (5. 9) 2 Death ICH Massive infarction (5. 9) 2 1 1
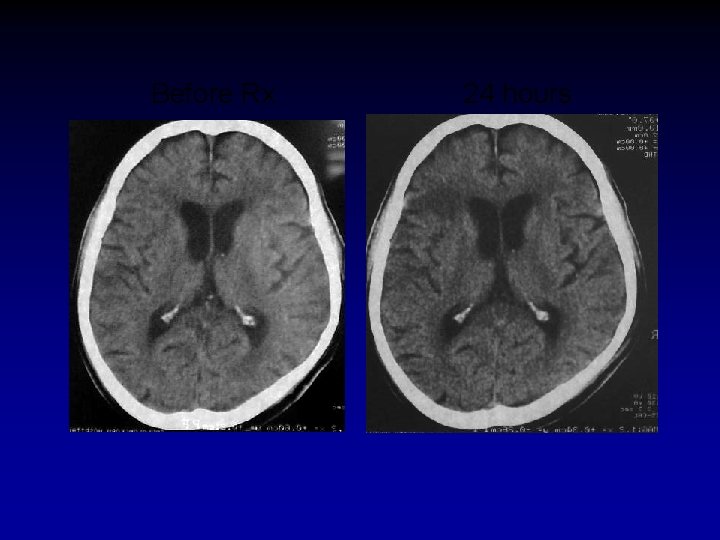
Before Rx 24 hours

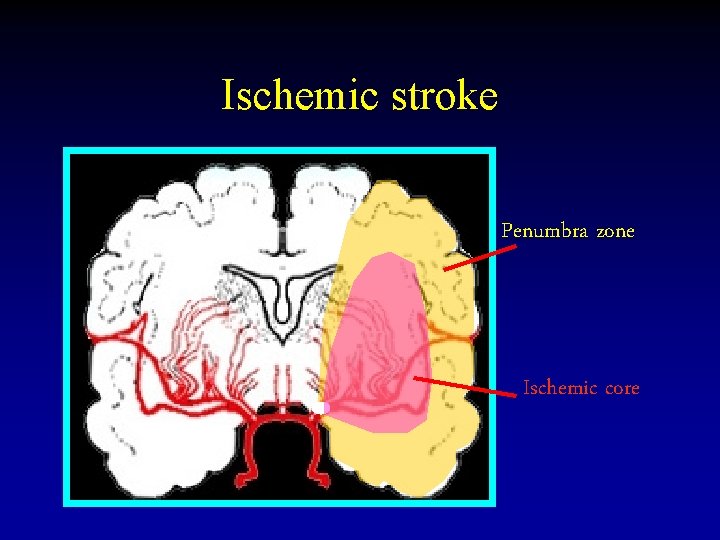
Ischemic stroke Penumbra zone Ischemic core
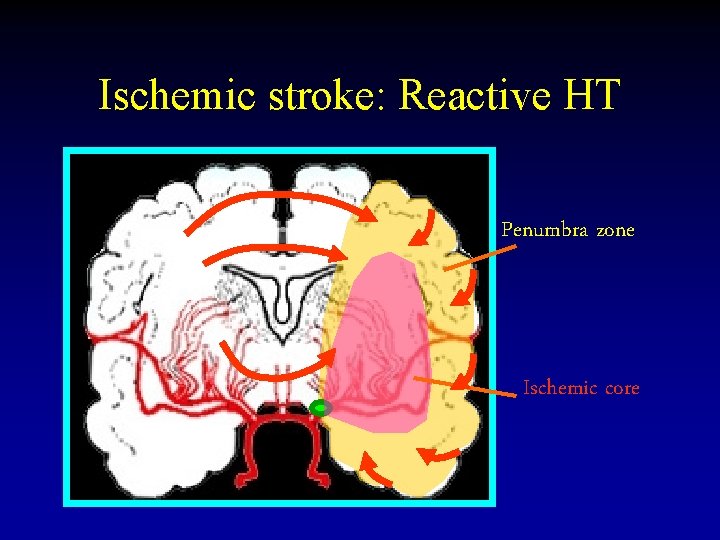
Ischemic stroke: Reactive HT Penumbra zone Ischemic core
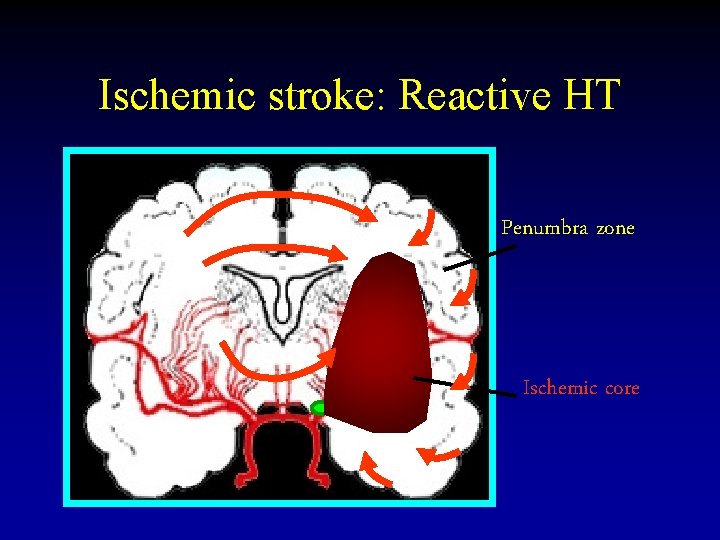
Ischemic stroke: Reactive HT Penumbra zone Ischemic core
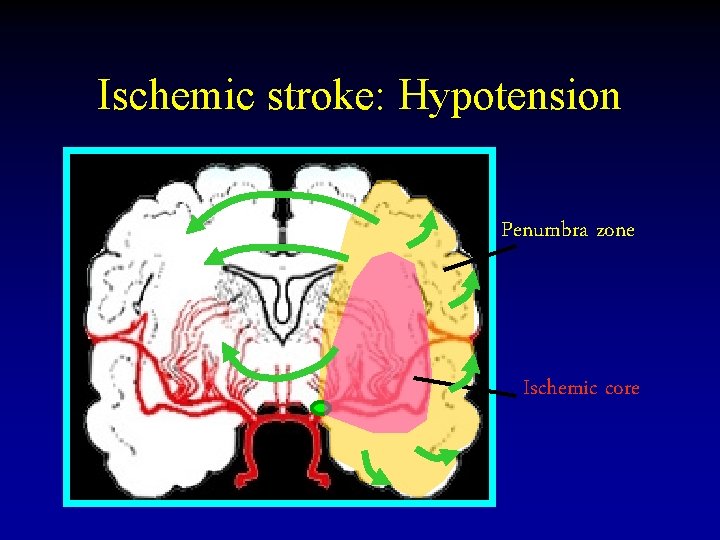
Ischemic stroke: Hypotension Penumbra zone Ischemic core
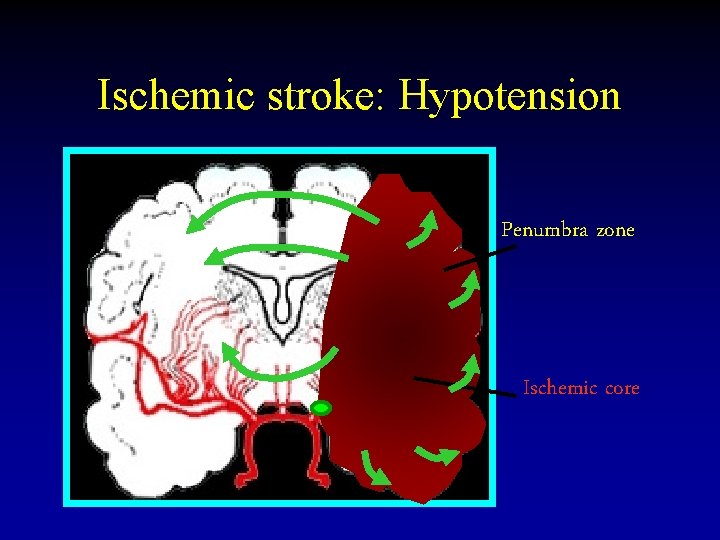
Ischemic stroke: Hypotension Penumbra zone Ischemic core

Stroke Unit Definition 1. Key physician (Neurologist, Internist, GP, NS) with stroke interest 2. Nursing staff and multidisplinary team 3. Geographically located 4. Availability of 24 hr CT 5. Basic labs : PG, Electrolytes, PTT, lipid 6. EKG, CXR, Echocardiogram 7. Rehabilitation facility 8. Stroke treatment guideline and care map Further investigations Carotid duplex และ Transcranial Ultrasound MRI และ MRA Diffusion และ Perfusion MRI CT Angiography Transesophageal echocardiography Cerebral angiography การตรวจทางหองปฏบตการอนๆ ไดแก การตรวจหาภาวะ Vasculitis, antiphospholipid antibody, hypercoagulable state ฯลฯ

STROKE PROTOCOL Care map short stay and ten days, Follow up sheet, Stroke Discharge summary, Home health care/ Home care forms
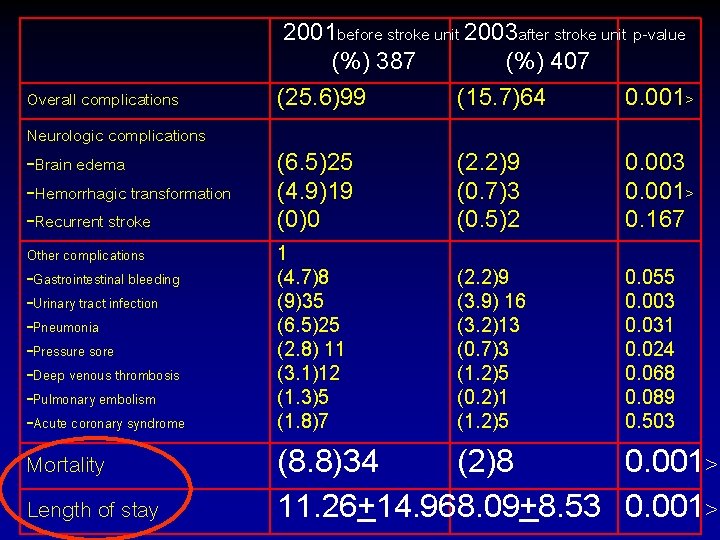
Overall complications Neurologic complications -Brain edema -Hemorrhagic transformation -Recurrent stroke 2001 before stroke unit 2003 after stroke unit p-value (%) 387 (%) 407 (25. 6)99 (15. 7)64 0. 001> (6. 5)25 (4. 9)19 (0)0 (2. 2)9 (0. 7)3 (0. 5)2 0. 003 0. 001> 0. 167 Other complications -Gastrointestinal bleeding -Urinary tract infection -Pneumonia -Pressure sore -Deep venous thrombosis -Pulmonary embolism -Acute coronary syndrome 1 (4. 7)8 (9)35 (6. 5)25 (2. 8) 11 (3. 1)12 (1. 3)5 (1. 8)7 (2. 2)9 (3. 9) 16 (3. 2)13 (0. 7)3 (1. 2)5 (0. 2)1 (1. 2)5 0. 055 0. 003 0. 031 0. 024 0. 068 0. 089 0. 503 Mortality Length of stay (8. 8)34 (2)8 0. 001> 11. 26+14. 968. 09+8. 53 0. 001>
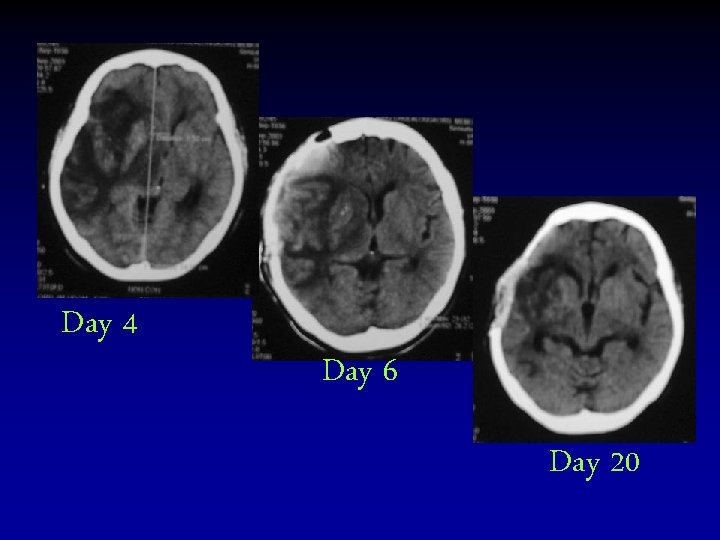
Day 4 Day 6 Day 20



������� 1. Antiplatelets • • • Aspirin 50 -325 mg Ticlopidine Clopidogrel ASA+ Dipyridamole Cilostazol • ACEI/ARB • Statins 2. Antihypertensives 3. Lipid lowering agents

- Slides: 81