CELLS OF IMMUNE SYSTEM 1 Lymphocytes B cells


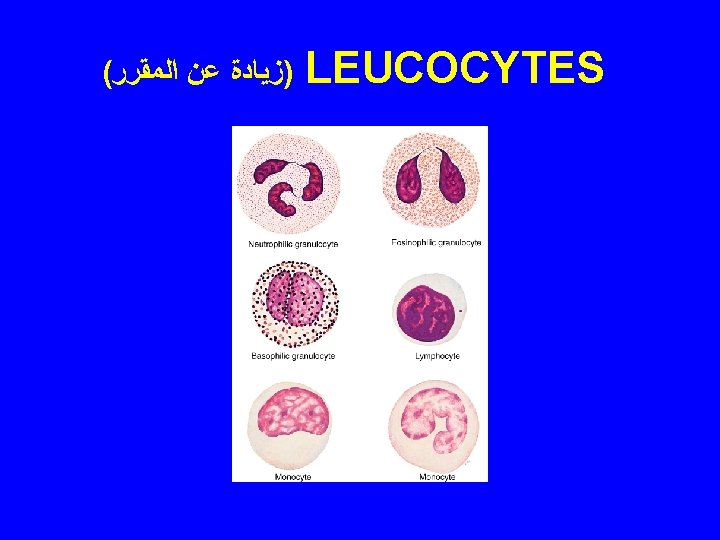
CELLS OF IMMUNE SYSTEM 1 - Lymphocytes: B cells T cells: memory, TH 1, TH 2, TC, TS Natural Killer Cells. 2 - Plasma cells 3 - Mast cells 4 - Neutrophils 5 - Eosinophils 6 - Antigen presenting cells

)ﺯﻳﺎﺩﺓ ﻋﻦ T-LYMPHOCYTES ( ﺍﻟﻤﻘﺮﺭ • Their plasmalemma has: 1 - T cell receptors (TCRs). 2 - CD molecules or markers ( cluster of differentiation proteins).

( )ﺯﻳﺎﺩﺓ ﻋﻦ ﺍﻟﻤﻘﺮﺭ T-LYMPHOCYTES • SUBTYPES: 1 - Memory cells. 2 - T helper cells: Are CD 4+ TH 1 & TH 2 cells 3 - T cytotoxic cells (Tc cells) (T killer cells) 4 - T suppressor cells ( Ts cells). N. B. Both Tc & Ts cells are CD 8+

( )ﺯﻳﺎﺩﺓ ﻋﻦ ﺍﻟﻤﻘﺮﺭ NULL CELLS 1 - Natural killer (NK) cells: are cytotoxic cells. antibody-dependent cell-mediated cytotoxicity. are non-B, non-T cells. are formed in red B. M. no need for maturation in thymus. Kill virally altered cells & tumor cells in nonspecific manner. 2 - Stem cells.

ANTIGEN PRESENTING CELLS ( )ﺍﻟﻤﻄﻠﻮﺏ ﻓﻘﻂ ﻣﺎ ﺗﺤﺘﻪ ﺧﻂ 1 - B lymphocytes. 2 - Macrophages. 3 - Dendritic cells: e. g. Follicular dendritic cells, Interdigitating dendritic cells Langerhans cells. 4 - Epithelial reticular cells of the thymus. N. B. APCs have class II MHC molecules (MHC II) but other cells have only MHC I

( )ﺯﻳﺎﺩﺓ ﻋﻦ ﺍﻟﻤﻘﺮﺭ LYMPHOKINES • Are released by: 1 - T helper lymphocytes. 2 - Antigen presenting cells.


)ﺯﻳﺎﺩﺓ DEVELOPMENT OF LYMPHOCYTES ( ﻋﻦ ﺍﻟﻤﻘﺮﺭ

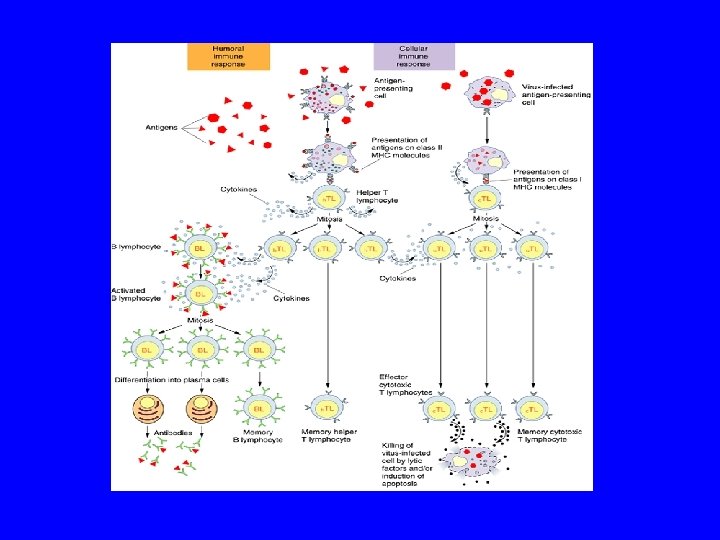
TYPES OF IMMUNE RESPONSE ( )ﺯﻳﺎﺩﺓ ﻋﻦ ﺍﻟﻤﻘﺮﺭ (1) Innate Response: (Fast, non-specific, no memory cells) By: Neutrophils, Macrophages, Mast cells, NK Cells. (2) Adaptive response: a- Humoral immune response b- Cell-mediated immune response
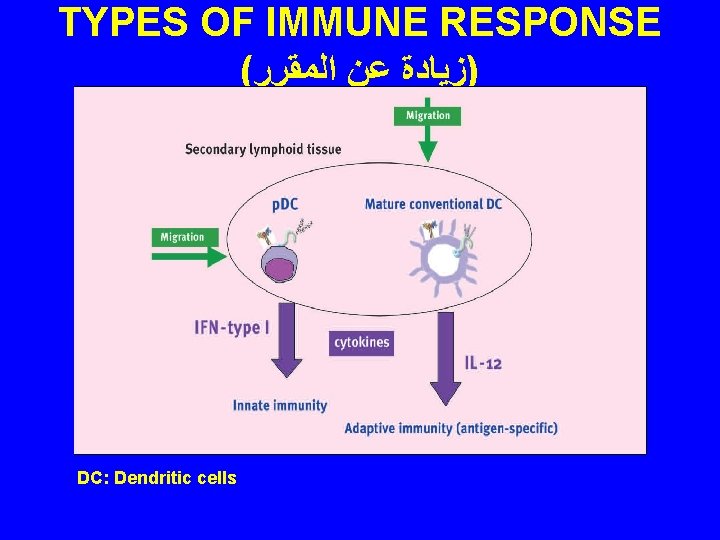
TYPES OF IMMUNE RESPONSE ( )ﺯﻳﺎﺩﺓ ﻋﻦ ﺍﻟﻤﻘﺮﺭ DC: Dendritic cells
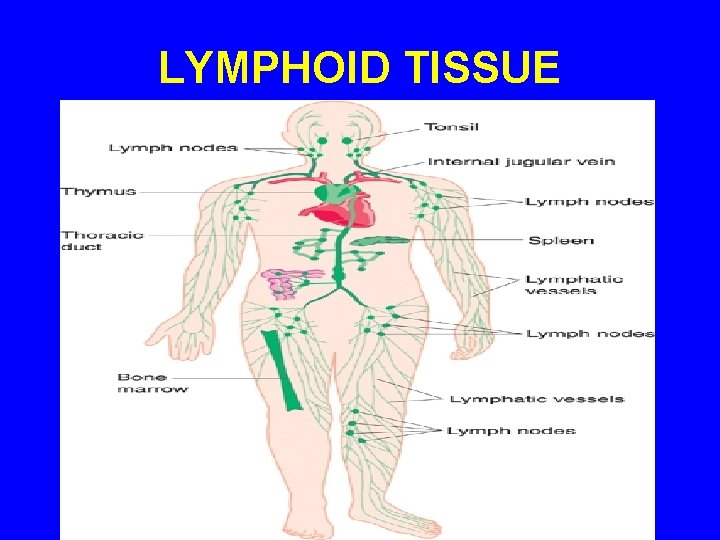
LYMPHOID TISSUE

LYMPHOID TISSUE A) Diffuse lymphoid tissue B) Encapsulated lymphoid organs: 1 - Lymph nodes. 2 - Spleen. 3 - Tonsils (are incompletely encapsulated) 4 - Thymus. N. B. Both red bone marrow & Thymus are considered 1 ry. Lymphoid organs.

DIFFUSE LYMPHOID TISSUE - MALT: lymphocyte infiltration, solitary lymphoid nodules & aggregated lymphoid nodules. - Under the wet epithelial membranes. - Loose C. T is infiltrated with lymphoid cells (lymphocytes, plasma cells, macrophages, reticular cells). - Lymphoid Nodules

LYMPHOID NODULE (LYMPHOID FOLLICLE) • 1 ry. : without germinal center • 2 ry. : with germinal center
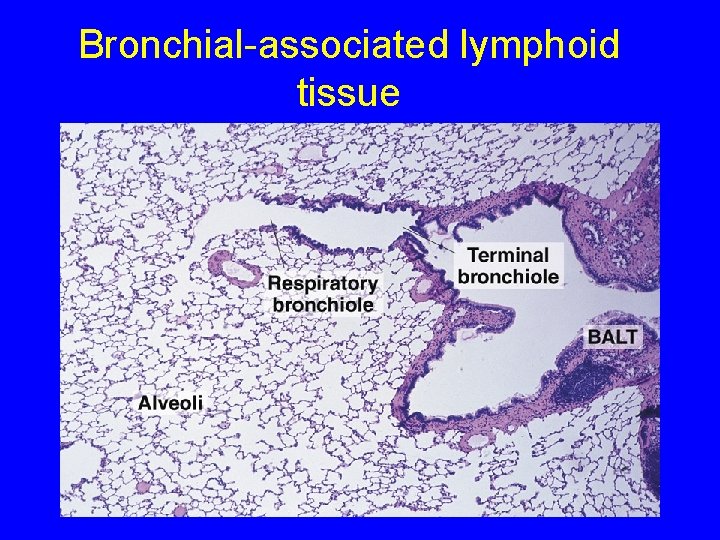
Bronchial-associated lymphoid tissue

LYMPHOID NODULE

LYMPH NODES

LYMPH NODE (L. N. ) (A) 1 - Capsule 2 - Trabeculae (septa) 3 - Reticular C. T. (B) Parenchyma: (lymphoid tissue + lymph sinuses) 1 - Cortex 2 - Paracortex 3 - Medulla
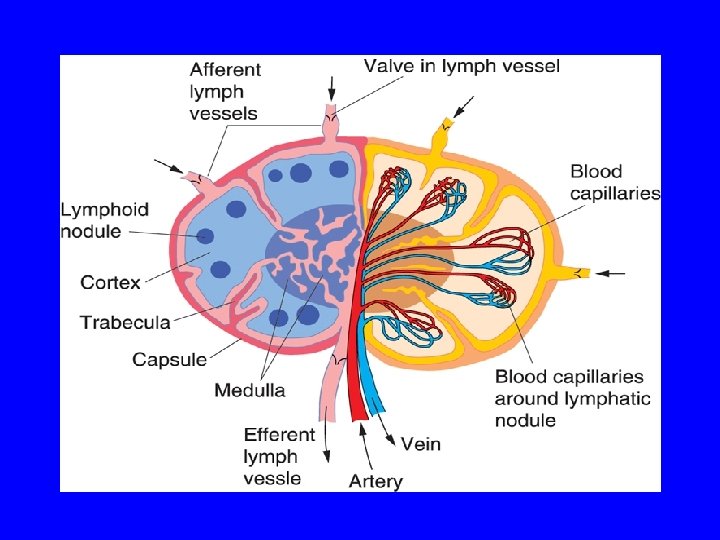
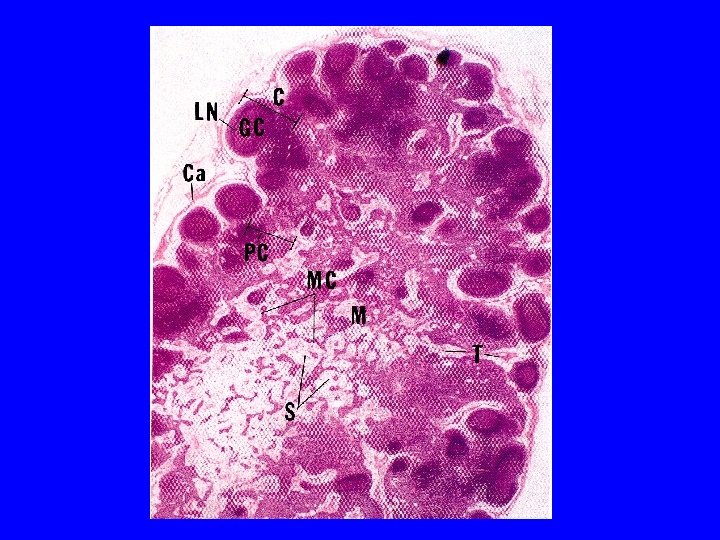
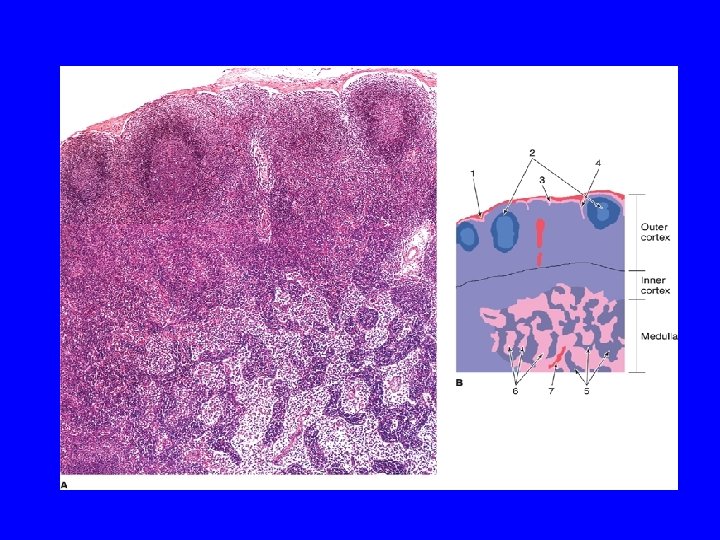
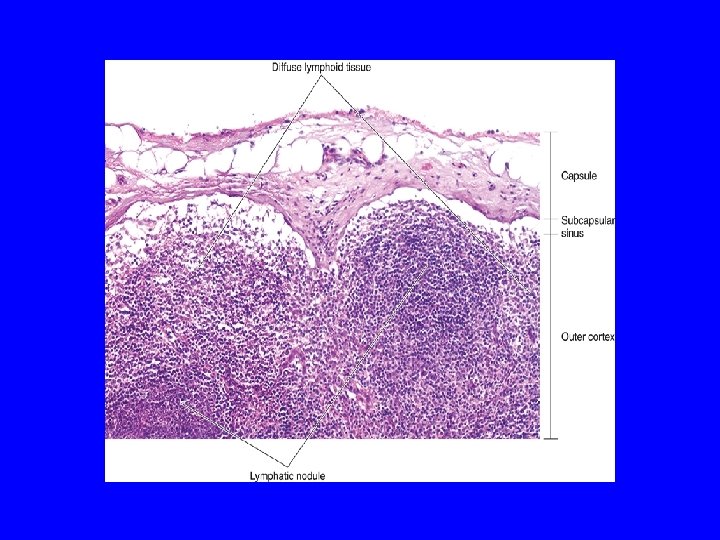

High endothelial venule (postcapillary venule)

CORTEX OF L. N. 1 - Lymphatic nodules (follicles): a- 1 ry: without germinal center b- 2 ry: is formed of: Corona (mantle): Dark, Mostly B-lymphocytes. Germinal center: Lighter, mostly activated B-lymphoblasts with macrophages & dendritic reticular cells. 2 - Subcapsular & Cortical (paratrabecular) lymph sinuses.

PARACORTEX Of L. N. • It is the thymus-dependent zone of L. N. • It is composed mostly of T-lymphocytes. • It contains high endothelial vessels (postcapillary venules): - PCV are lined with cuboidal endothelium. - PCV are the site of entry of lymphocytes to L. N.

Medulla of lymph node
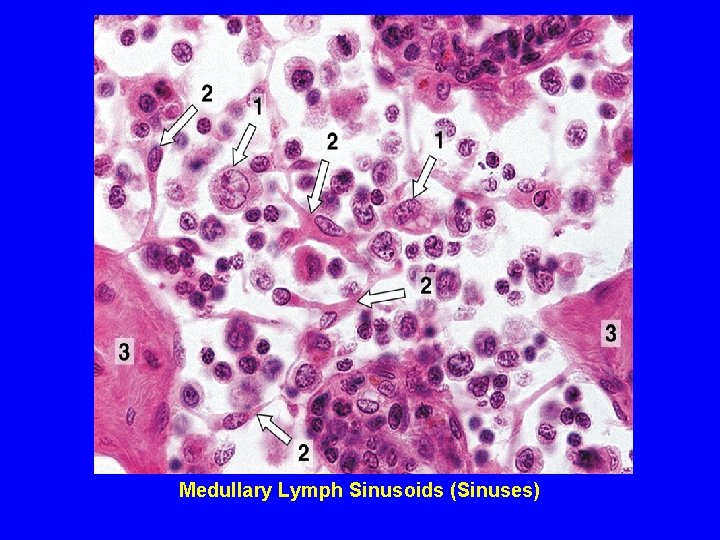
Medullary Lymph Sinusoids (Sinuses)

MEDULLA OF L. N. (1) Medullary cords: are formed mainly of lymphoid cells ( B & T lymphocytes, plasma cells, macrophages). (2) Medullary sinusoids ( or medullary sinuses). N. B. Efferent lymphatic vessels drain lymph with B & T lymphocytes.

MAIN CELLS OF L. N. 1 - B & T lymphocytes. 2 - Plasma cells. 3 - Macrophages 4 - Dendritic reticular cells

FUNCTIONS OF L. N. • 1 - Production of immunocompetent cells. • 2 - Filtration of lymph.

SPLEEN

STROMA OF SPLEEN 1 - Capsule: is covered by visceral layer of peritoneum; mesothelium. occasionally contains SMCs 2 - Trabeculae. 3 - Reticular C. T.

PARENCHYMA OF SPLEEN • (A) White pulp. • (B) RED PULP. • (C) Marginal zone. • N. B. No cortex, no medulla. No afferent lymphatic vessel.
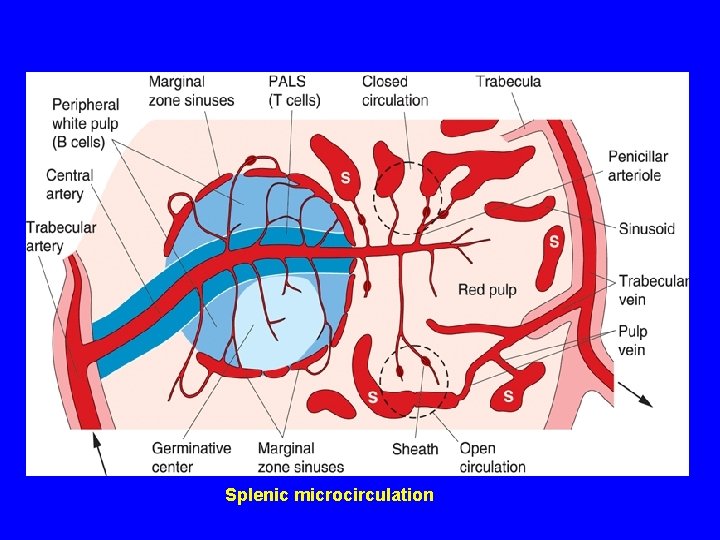
Splenic microcirculation
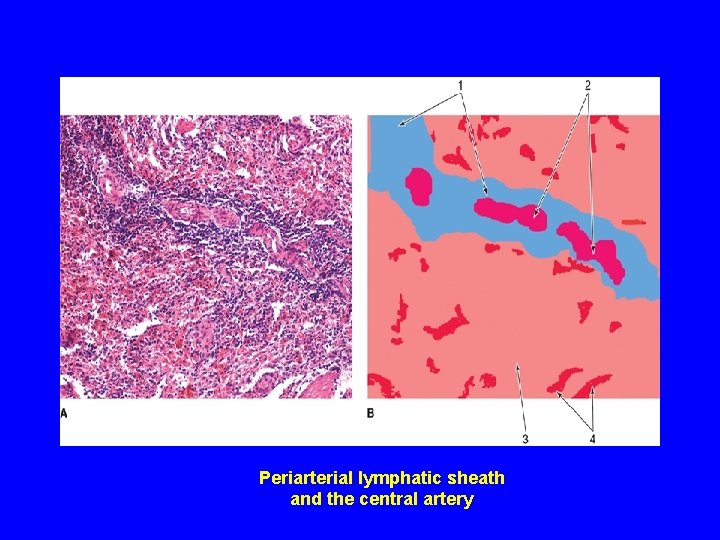
Periarterial lymphatic sheath and the central artery
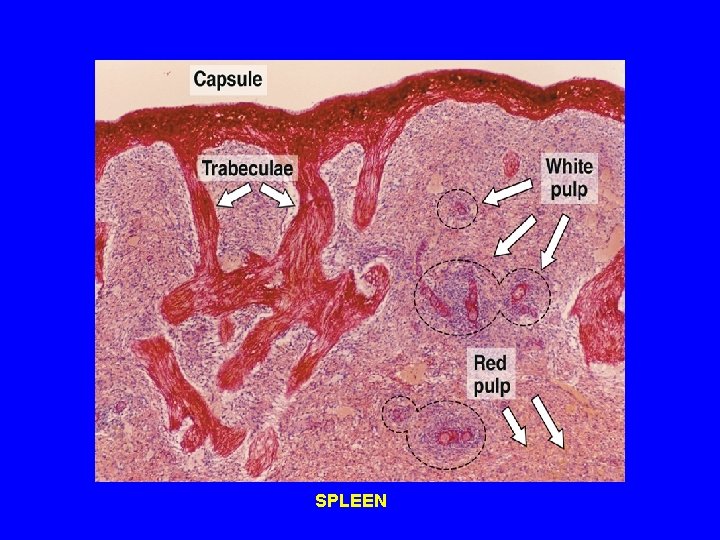
SPLEEN
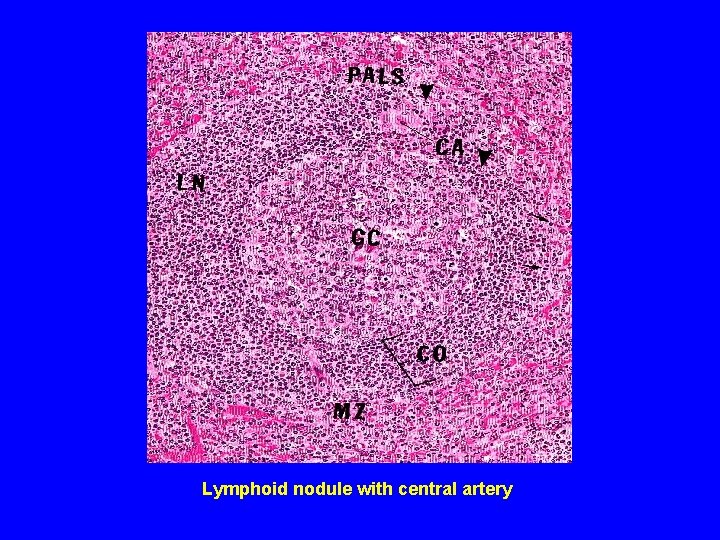
Lymphoid nodule with central artery
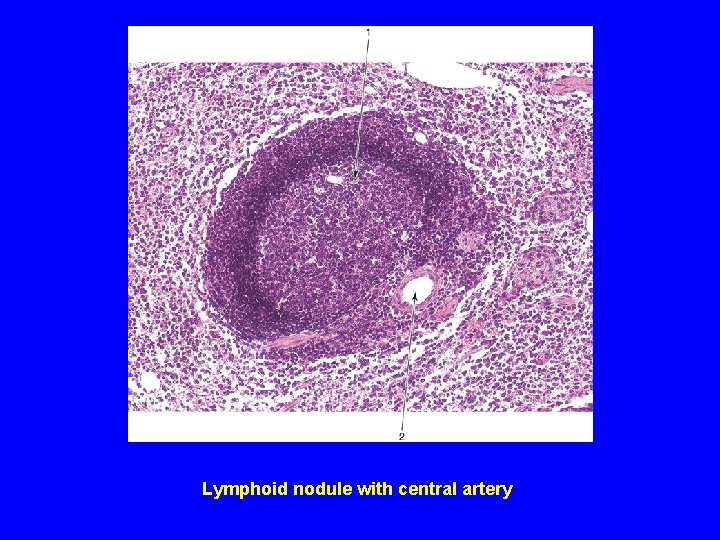
Lymphoid nodule with central artery

PARENCHYMA OF SPLEEN (A) White pulp: 1 - Periarterial lymphatic sheaths: housing T lymphocytes. 2 - Lymphoid nodules ( with germinal centers): housing B lymphocytes. N. B. Both 1&2 have the acentrically located central artery
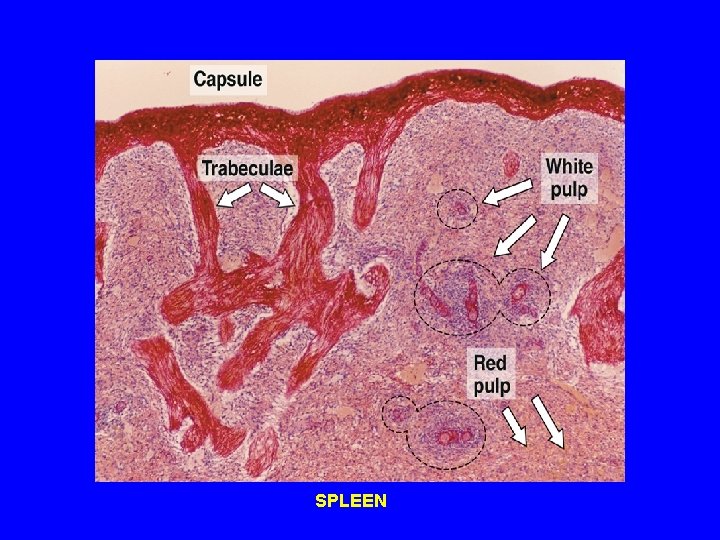
SPLEEN
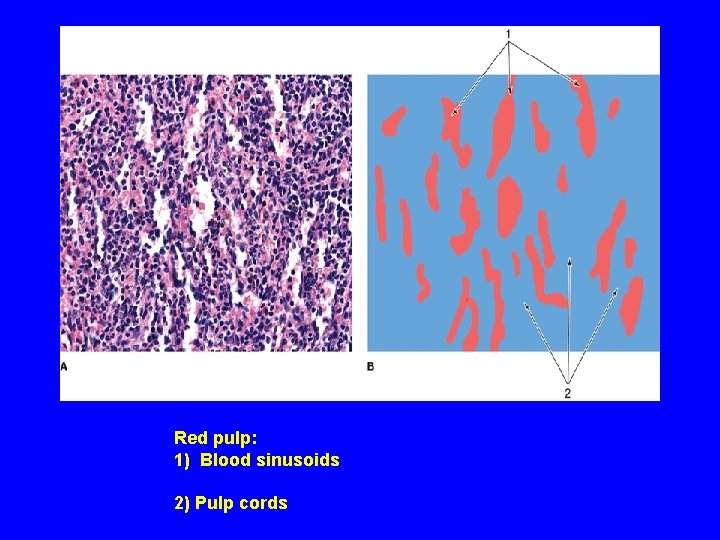
Red pulp: 1) Blood sinusoids 2) Pulp cords
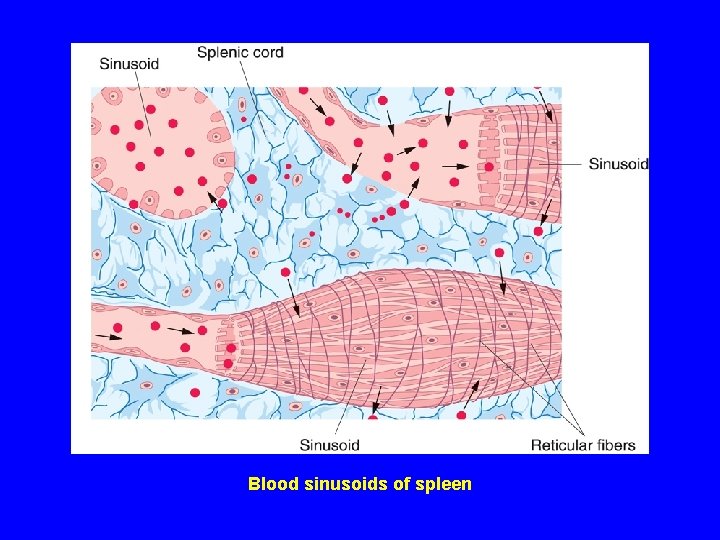
Blood sinusoids of spleen

(B) Red pulp: 1 - Pulp (splenic) cords (of Billroth): Extravasated blood cells, plasma cells, Macrophages & reticular cells and fibers. 2 - Blood sinusoids: Are lined with elongated fusiform endothelial cells with large intercellular spaces & supported by discontinuous, hoop-like basement membrane.

(C) Marginal zone: - Between white and red pulps. - Rich in vascular channels (marginal sinuses), especially surrounding the lymphoid nodules - Rich in avidly phagocytic macrophages. - Contains plasma cells, T & B cells, macrophages, interdigitating dendritic cells. - It houses B cells that are specialized to recognize thymic-independent antigens. - Site of first entry of B & T lymphocytes from blood stream to parenchyma of spleen.

FUNCTIONS OF SPLEEN 1 - Filtration of blood. 2 - Phagocytosis of old RBCs & old blood platelets & invading microorganisms. 3 - Production & proliferation of immunocompetent B & T lymphocytes. 4 - Production of antibodies.

SPLENIC MICROCIRCULATION 1 - Splenic artery 2 - Trabecular artery 3 - Enter the parenchyma as CENTRAL ARTERY ( in the white pulp) 4 - Enter the red pulp as several straight branches named PENICILLAR ARTERIES (pulp arterioles→ Sheathed arterioles→ Terminal arterial capillary) 5 - Blood sinusoids 6 - Pulp veins 7 - Trabecular veins 8 - Splenic vein.

Splenic microcirculation
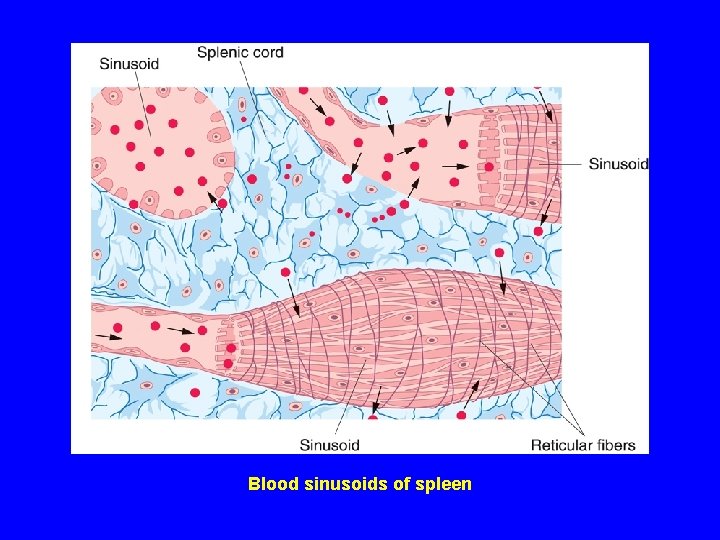
Blood sinusoids of spleen

Tonsils (1) Palatine Tonsils. (2) Pharyngeal Tonsil. (3) Lingual Tonsils.

PALATINE TONSILS 1 - Epithelium 2 - Tonsillar crypts: 10 -12 3 - Lymphatic nodules 4 - Capsule
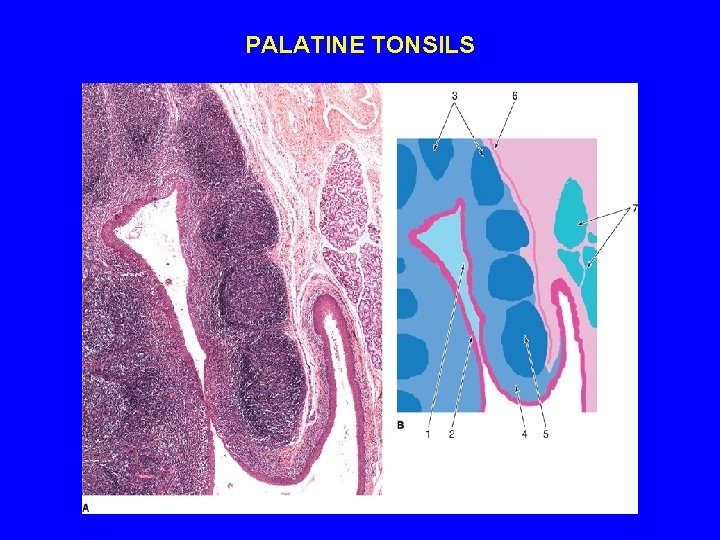
PALATINE TONSILS


PHARYNGEAL TONSIL 1 - Epithelium 2 - Pleats: Longitudinal infoldings (instead of tonsillar crypts). 3 - Lymphatic nodules & diffuse lymphoid tissue. 4 - Capsule. 5 - Ducts of seromucous glands.

PHARYNGEAL TONSIL

LINGUAL TONSILS 1 - Epithelium. 2 - Crypt: a single crypt for each lingual tonsil. 3 - Lymphatic nodules. 4 - Capsule. 5 - Glands: ducts of mucous minor salivary glands open into the base of a single crypt of each lingual tonsil.

FUNCTION OF TONSILS Production of antibodies.

THYMUS

THYMUS A) Stroma: 1 -Capsule 2 -Interlobular trabeculae: incomplete B) Thymic lobules: 1 -Cortex 2 -Medulla
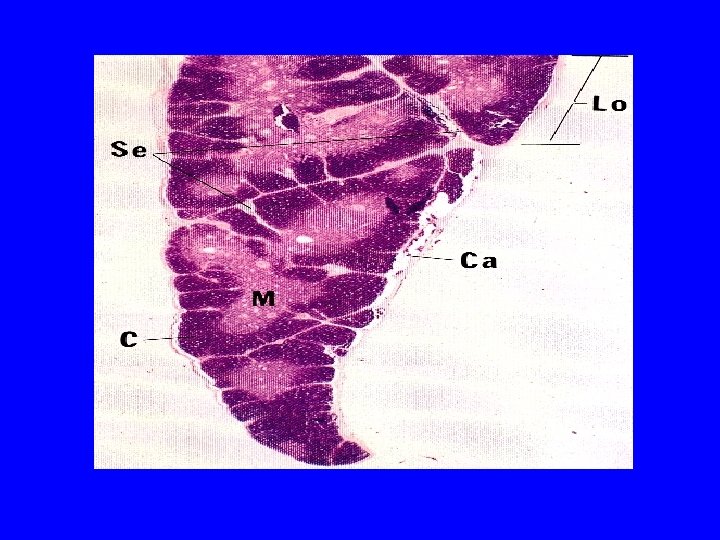
l

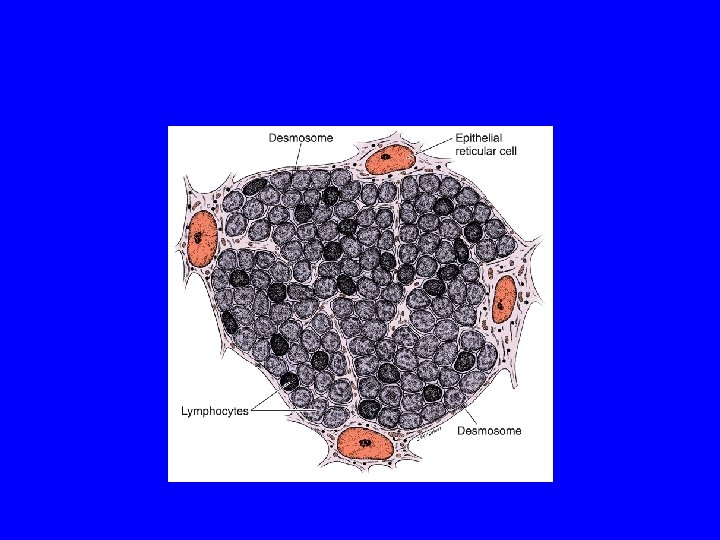

CORTEX OF THYMIC LOBULE A) It contains developing (immature) thymocytes. 98% of thymocytes die? 1 -Whose TCRs recognize self-proteins OR CD 4 or CD 8 molecules can not recognize MHC I or MHC II molecules. B) Epithelial reticular cells C) Macrophages

CORTEX OF THYMIC LOBULE (cont. ) No lymphatic nodules No plasma cells N. B. Tingible body macrophages (resident macrophages with apoptotic bodies)
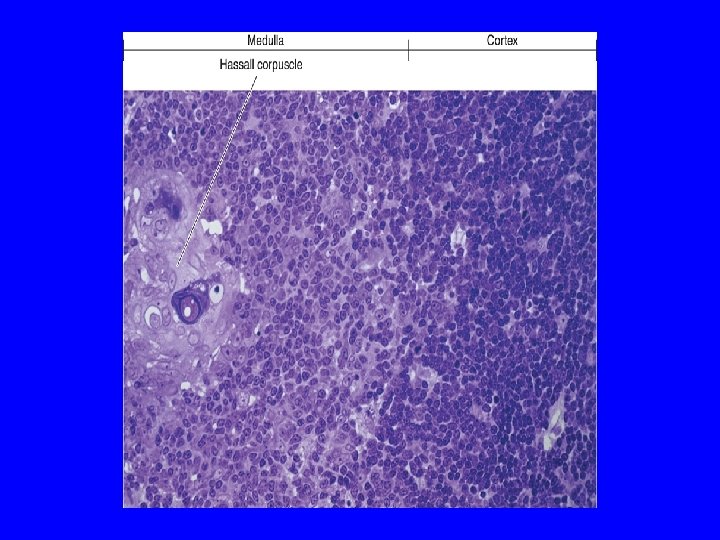

MEDULLA OF THYMIC LOBULE 1 -Hassall’s (thymic) corpuscles: -Concentrically arranged epithelial reticular cells in the medulla. - Whose number increases with aging. 2 -Virgin (naive) mature small T lymphocytes 3 - Macrophages 4 -Epithelial reticular cells N. B. Medulla of adjacent thymic lobules are interconnected- Why? Incomplete trabeculae

BLOOD-THYMUS BARRIER Site: It is found in the cortex Components: 1) Continuous blood capillaries ( The only blood vessel in the cortex) 2) Thick basal lamina 3) Sheath of the epithelial reticular cells

FUNCTION OF THYMUS Formation, Maturation & Destruction of T lymphocytes. Maturation: Immunoincompetent T cells →→→ Immunocompetent T cells.

General notes about thymus • No lymphoid nodules • No reticular fibers • No sinuses or sinusoids

Development and Involution of the thymus • It attains its greatest development shortly after birth • It involutes after puberty and becomes infiltrated by adipose tissue • Remnants of thymus remain in adult to form T lymphocytes
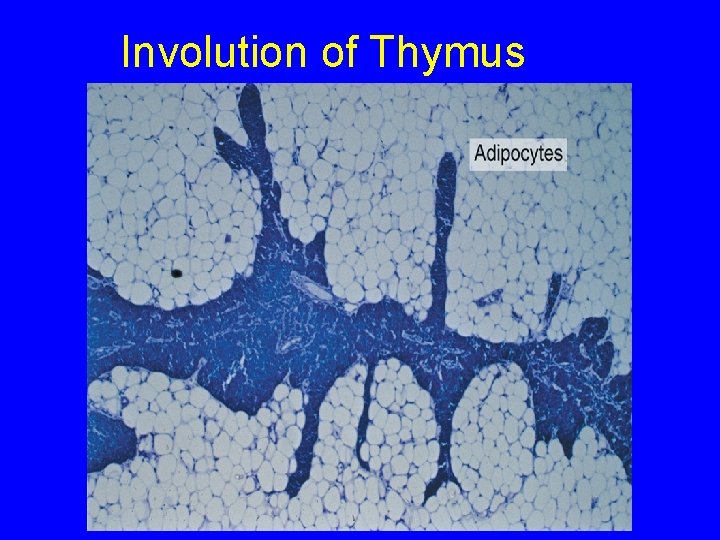
Involution of Thymus

BEST WISHES



- Slides: 77