Celiac Sprue December 19 2005 Celiac Sprue Definitions
Celiac Sprue December 19, 2005

Celiac Sprue Definitions • celiac sprue is an immune disorder characterized by inflammation of the proximal small intestine induced by the ingestion of gluten • also known as celiac disease and glutensensitive enteropathy

Celiac Sprue History • recognized in the third century (Aretaeus of Cappadocia: chronic diarrhea and “atrophy of the body”) • 1600’s - Dutch term “sprouw” means aphthous disease • Dr. Samuel Gee (UK) in 1888 described the disease and made a link to the diet • Dicke (Dutch pediatrician) linked sprue with wheat during grain shortages in the Netherlands during WWII • 1940’s – water insoluble gluten moiety was causal • 1950’s – small bowel pathology was characterized • 1970’s – first immunoglobulin and autoantibody studies • 1980’s – anti-endomysial antibodies and HLA class II associations (DQ 2) • 1990’s – tissue transglutaminase (t. TG)
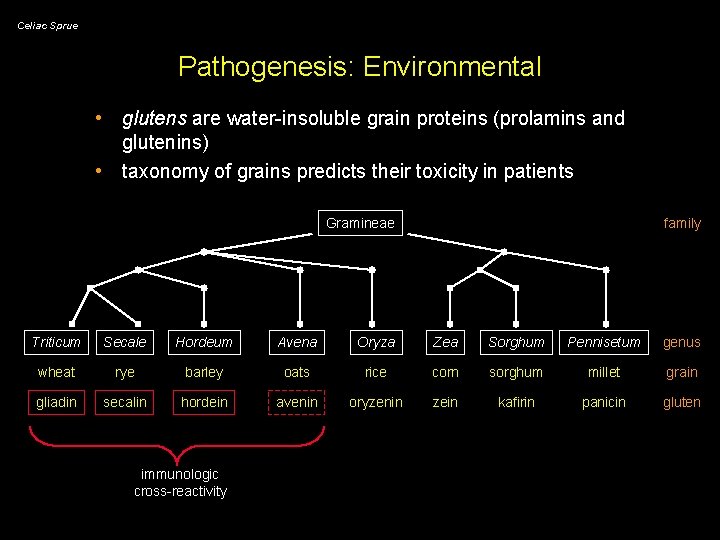
Celiac Sprue Pathogenesis: Environmental • glutens are water-insoluble grain proteins (prolamins and glutenins) • taxonomy of grains predicts their toxicity in patients Gramineae family Triticum Secale Hordeum Avena Oryza Zea Sorghum Pennisetum genus wheat rye barley oats rice corn sorghum millet grain gliadin secalin hordein avenin oryzenin zein kafirin panicin gluten immunologic cross-reactivity

Celiac Sprue Pathogenesis: Genetic • concordance - 8 -18% in first degree relatives - 70% in monozygotic twins • association with certain HLA DQ haplotypes - 95% of celiac patients are DQ 2 - most of the remaining are DQ 8 • sprue develops in a minority with DQ 2 - 25 -30% of Europeans are DQ 2 - non-HLA linked gene(s) likely determinant
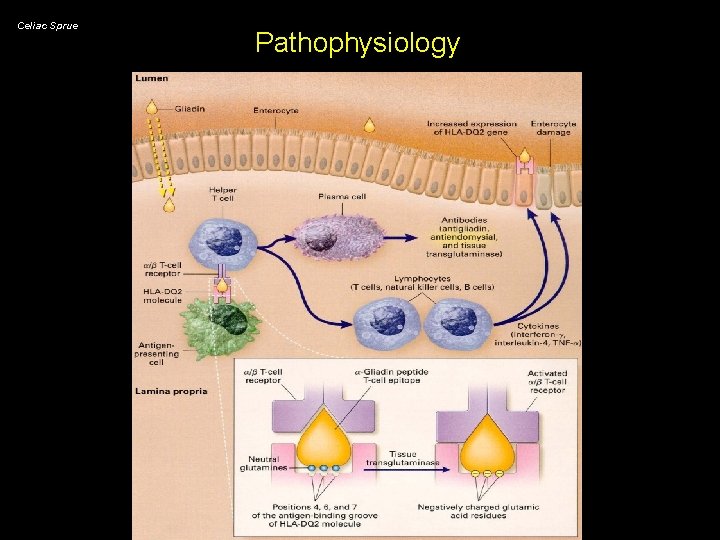
Celiac Sprue Pathophysiology
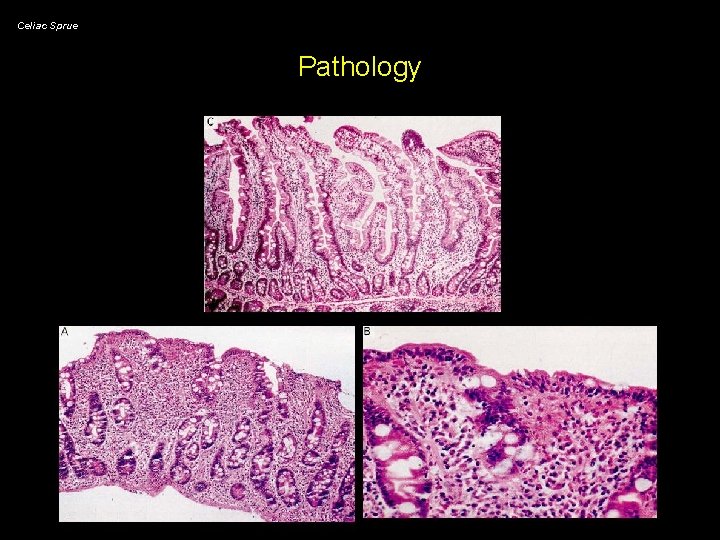
Celiac Sprue Pathology

Celiac Sprue Classification • classic (typical) celiac sprue - fully expressed form of celiac sprue - symptoms and signs of malabsorption (after breast milk weaning) • atypical celiac sprue - gluten-induced small bowel inflammation - atypical symptoms (anemia, short stature, etc. ) • silent celiac sprue - gluten-induced inflammation without symptoms or signs • latent celiac sprue - childhood sprue reverts to normal biopsy and does not recur when gluten is reintroduced (possibly re-develop celiac sprue later in life) - sprue presents later, after earlier documented absence on gluten • potential celiac sprue - abnormal serology but sub-diagnostic biopsy (normal or IELs) - genetic predisposition (DQ 2 and/or strong family history) - 50% probability of developing celiac sprue
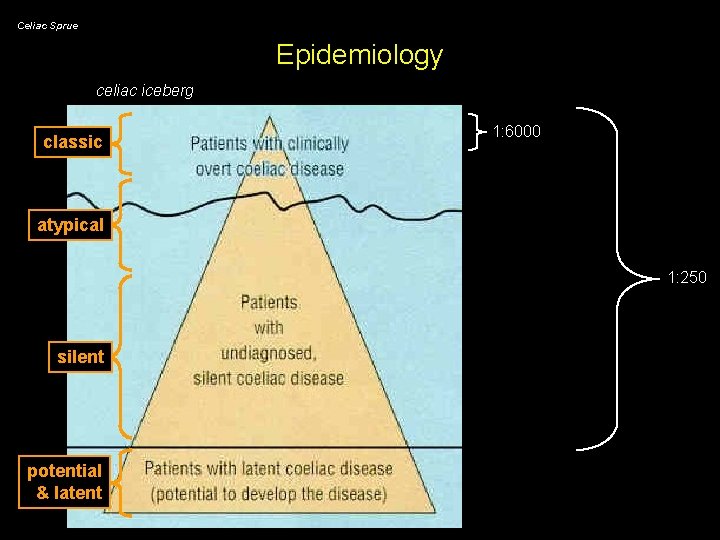
Celiac Sprue Epidemiology celiac iceberg classic 1: 6000 atypical 1: 250 silent potential & latent
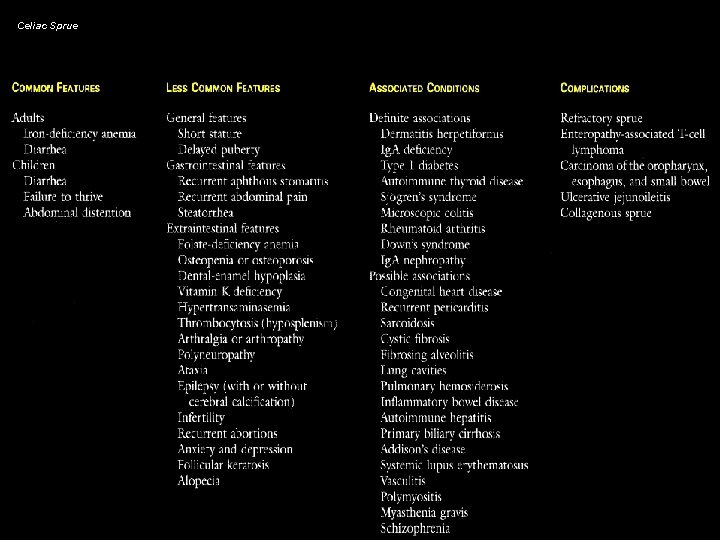
Celiac Sprue

Celiac Sprue Clinical Presentation Childhood Presentation • typical - • failure to thrive diarrhea/steatorrhea anorexia vomiting abdominal distension abdominal pain atypical - aphthous ulcers short stature anemia rickets Adult Presentation • typical - • diarrhea/steatorrhea (75 -80%) weight loss abdominal bloating/flatulence mild abdominal pain atypical - anemia (85%) osteoporosis (15 -30%) coagulopathy (10%) aphthous ulcers infertility/menstrual abnormalities neurologic symptoms short stature weakness/myopathy

Celiac Sprue Associated Conditions • dermatitis herpetiformis - rare in childhood; seen in 10% of adult celiac patients - very pruritic - >80% have at least silent or latent sprue, but only 10% of patients have intestinal symptoms - still have 10 -40 x risk of lymphoma if untreated • type I diabetes mellitus - 3 -6% of IDDM patients develop sprue (20 x risk) - 5% of sprue patients develop IDDM • Ig. A deficiency - seen in 10% of sprue patients (complicates diagnosis) - Ig. A deficient persons have 10 x prevalence of sprue • • thyroid disease (5% of sprue patients) autoimmune diseases (Sjögren’s, SLE, PBC) hyposplenism (~50% of sprue patients) microscopic colitis
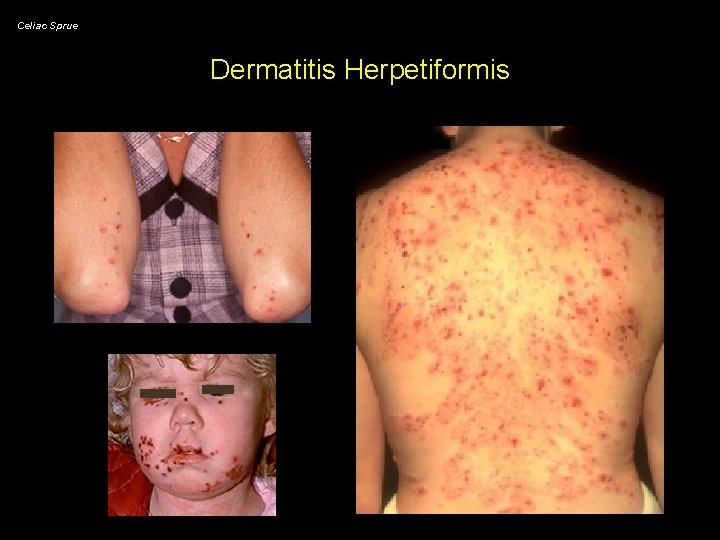
Celiac Sprue Dermatitis Herpetiformis
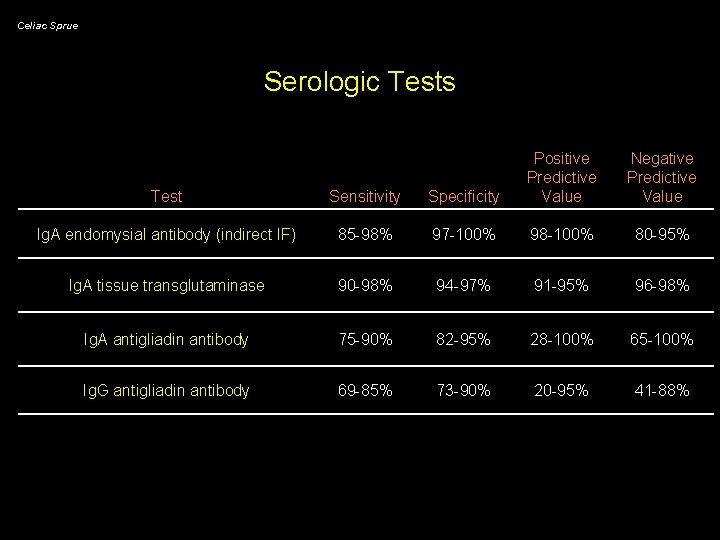
Celiac Sprue Serologic Tests Test Sensitivity Specificity Positive Predictive Value Negative Predictive Value Ig. A endomysial antibody (indirect IF) 85 -98% 97 -100% 98 -100% 80 -95% Ig. A tissue transglutaminase 90 -98% 94 -97% 91 -95% 96 -98% Ig. A antigliadin antibody 75 -90% 82 -95% 28 -100% 65 -100% Ig. G antigliadin antibody 69 -85% 73 -90% 20 -95% 41 -88%
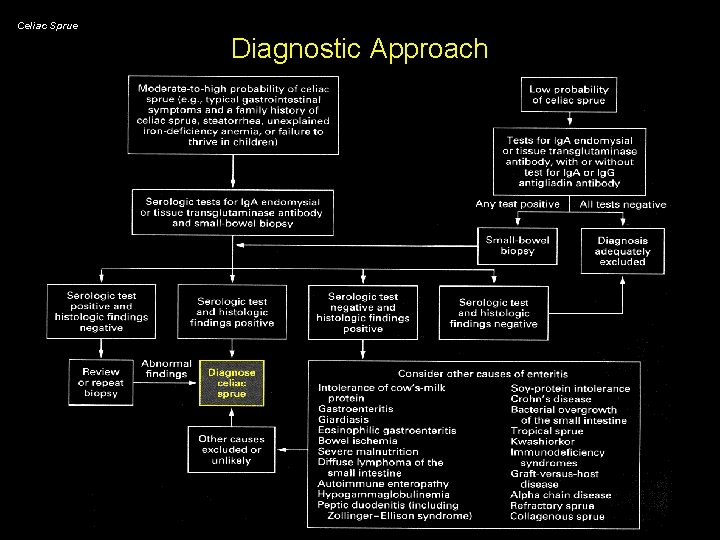
Celiac Sprue Diagnostic Approach

Celiac Sprue Dietary Guidelines • avoid all foods containing wheat, rye and barley gluten - • • • in Europe, look for gluten-free labels brand name foods differ from country to country avoid dairy products (until remission, ~3 -6 months) avoid oats until initial remission, then less than 50 -60 grams/day use only rice, corn, buckwheat, potato, soybean, sorghum or tapioca flour or starches read all labels and ingredients in processed foods & condiments watch for gluten in medications, thickeners, emulsifiers and additives avoid all beers (lagers, ales stouts…) wine, liqueurs, whiskey, brandy and most ciders are usually OK consider vitamin, calcium, iron and folate supplementation remember that medications can be malabsorbed as well remember that these restrictions are expensive and inconvenient

Celiac Sprue Response to Diet Restrictions • • 70% of patients have symptomatic improvement within 2 weeks histologic improvement lags unpredictably - • • may not be evident for 2 -3 months associated with fall in antibody levels in ~3 months is commonly complete in children 50% of adults have only partial histologic resolution failure to respond is most often due to incomplete removal of dietary gluten with strict adherence… - 5 year survival rate equal to general population infant and child growth and development normalizes lower risk of SB lymphoma (back to normal in 5 years)

Celiac Sprue Complications • refractory sprue - unresponsive sprue (other causes excluded) - may require immunosuppressive therapy or TPN - up to 75% may have cryptic T-cell lymphoma • collagenous sprue - subset of refractory sprue with a poor response and prognosis • ulcerative jejunoileitis (UJI) - ulcers, strictures and severe symptoms (pain, bleeding, obstruction) - high mortality (up to 33%) - higher risk of lymphoma (abnormal clones of T-cells) • malignancy - 3% incidence over 5 year study - SB lymphoma (EATCL) • T-cell origin and often multifocal • accounts for half of malignancies in sprue patients (40 x risk) • occurs ~20 -40 years after presentation - oropharyngeal and upper GI cancers

Celiac Sprue Future Directions • bio-engineering gluten-free grains • developing a vaccine or directed therapy against t. TG
- Slides: 19