CCRNPCCN Review Neurology Cynthia Bautista Ph D CNRN

CCRN/PCCN Review Neurology Cynthia Bautista, Ph. D, CNRN, SCRN, CCNS, ACNS-BC, FNCS Associate Professor - Egan School of Nursing Fairfield University cabbrain@aol. com Mary Mc. Kenna Guanci MSN. RN. CNRN. SCRN. Clinical Nurse Specialist, Massachusetts General Hospital, Boston Ma. mguanci@partners. org

Questions on Exam • 12% CCRN Neurology – 18 questions • 5% PCCN Neurology – 5 -6 questions – Cerebrovascular Malformation – Encephalopathy – Intracranial Hemorrhage – Seizures – Stroke Copyright Nursing Brains, LLC
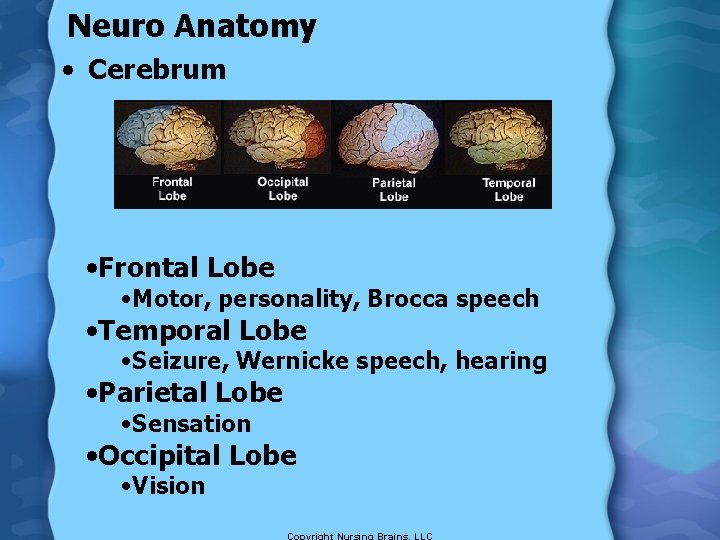
Neuro Anatomy • Cerebrum • Frontal Lobe • Motor, personality, Brocca speech • Temporal Lobe • Seizure, Wernicke speech, hearing • Parietal Lobe • Sensation • Occipital Lobe • Vision
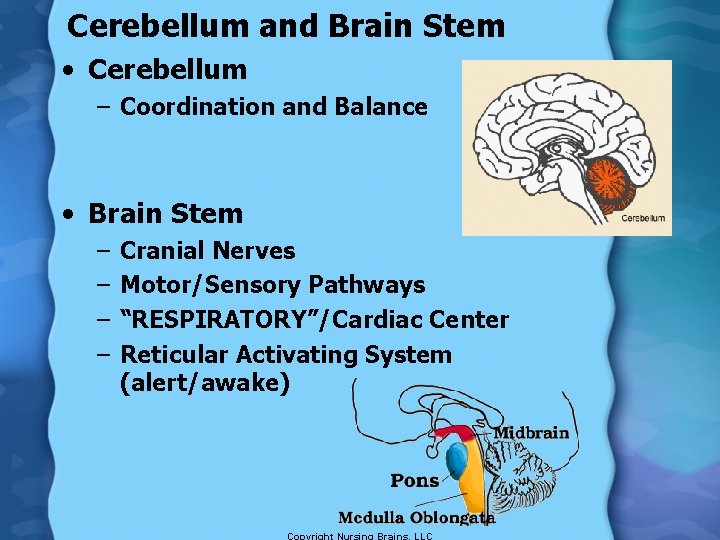
Cerebellum and Brain Stem • Cerebellum – Coordination and Balance • Brain Stem – – Cranial Nerves Motor/Sensory Pathways “RESPIRATORY”/Cardiac Center Reticular Activating System (alert/awake)
Neurological Assessment

Level of Consciousness Glasgow Coma Scale • Eye Opening – 4 - Spontaneous – 3 - To Speech – 2 - To Pain – 1 – None • Motor Response – 6 - Obeys Commands – 5 - Localizes – 4 - Withdraws – 3 - Abnormal Flexion – 2 - Abnormal Extension – 1 -None • Verbal Response – 5 - Oriented – 4 - Confused – 3 - Inappropriate Words – 2 - Inappropriate Sounds – 1 - None “BEST INDICATOR FOR CHANGE IN NEUROLOGICAL FUNCTION”
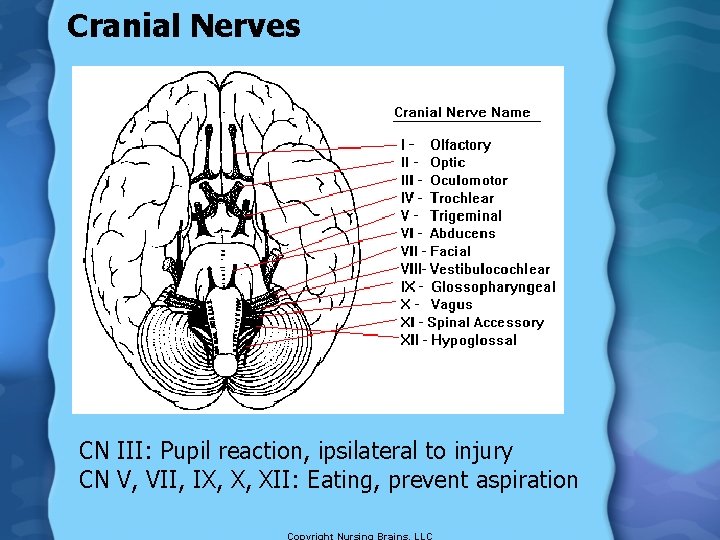
Cranial Nerves CN III: Pupil reaction, ipsilateral to injury CN V, VII, IX, X, XII: Eating, prevent aspiration

Motor Response • Motor Strength Scale – Movement against Gravity and Resistance • 5 - Normal movement • 4 - Movement against moderate gravity and resistance • 3 - Movement against gravity only • 2 - Movement but not against gravity • 1 - Muscle contraction • 0 - No movement “CONTRALATERAL TO INJURY”
Vital Signs • Temperature – Hyperthermia, hypothermia • Pulse “CUSHINGS TRIAD – ICP LATE SIGN” – Bradycardia • Blood Pressure – Elevated systolic, widen pulse pressure • Respirations – Central Neurogenic Hyperventilation, Apneusis, Cluster breathing, Ataxic breathing, Chenyne Stokes
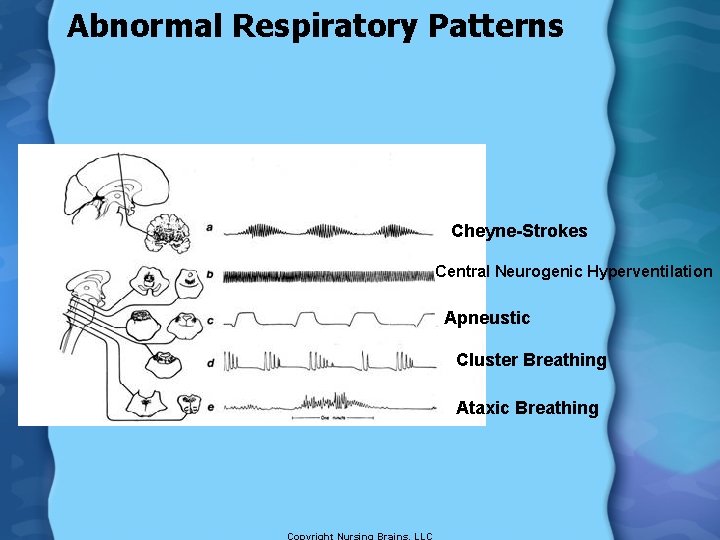
Abnormal Respiratory Patterns Cheyne-Strokes Central Neurogenic Hyperventilation Apneustic Cluster Breathing Ataxic Breathing
Head Trauma

Mild Head Injury • Concussion – Violent shaking of the brain – Postconcussion Syndrome • Confusion, forgets things, loses temper, impulsive, has a harder time learning, problems at work/school, personality change
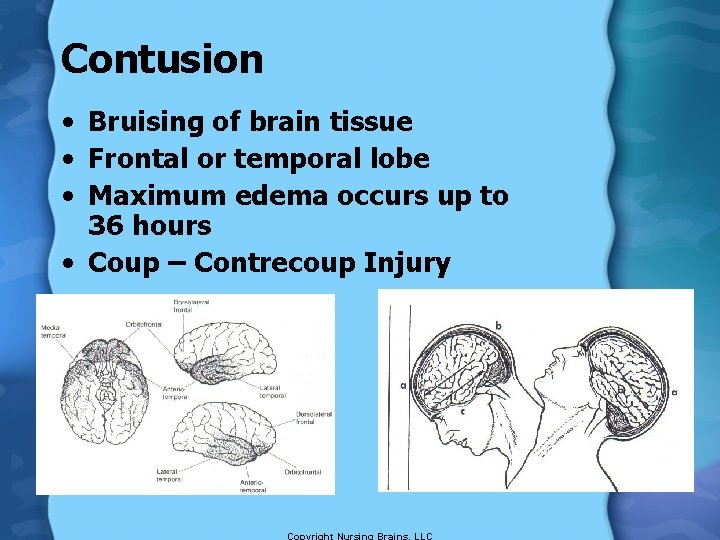
Contusion • Bruising of brain tissue • Frontal or temporal lobe • Maximum edema occurs up to 36 hours • Coup – Contrecoup Injury

Diffuse Axonal Injury (DAI) • Severe mechanical disruption of neuronal pathways (shearing injury) • Rapid acceleration and deceleration • Immediate/prolonged unconsciousness • MRI to diagnose • High morbidity rate • Vegetative care
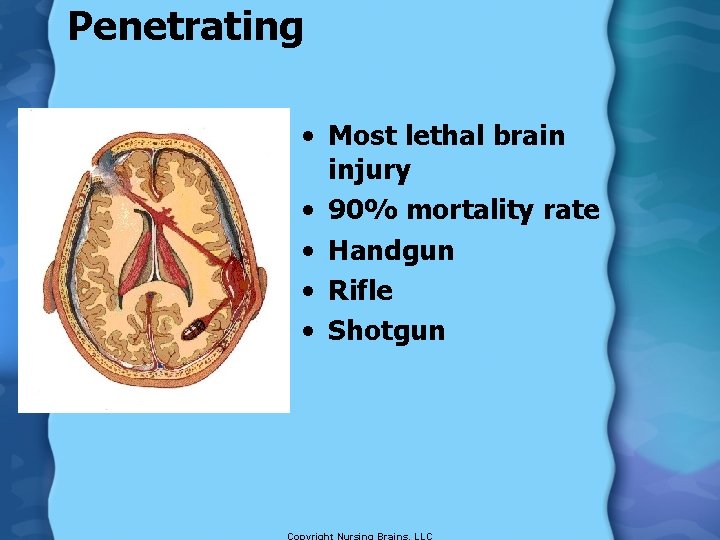
Penetrating • Most lethal brain injury • 90% mortality rate • Handgun • Rifle • Shotgun
Penetrating Head Injury Outcomes • Presenting Neuro Status – Awake = survive – Comatose = death • Path of Bullet – Single hemisphere = survive – Bilateral hemispheres = death • Caliber & Velocity of Bullet – Small & slow = survive – Large & fast = death

Penetrating Head Injury Outcomes (con’t) • Time to Treatment – Quick arrival to ED= survive – Delay in arrival to ED= death • Nature of Shooting – Assault = survive – Suicide = death
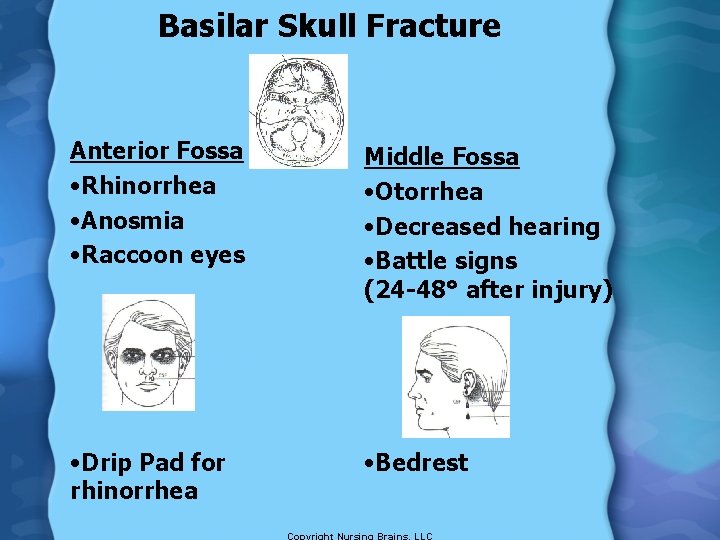
Basilar Skull Fracture Anterior Fossa • Rhinorrhea • Anosmia • Raccoon eyes Middle Fossa • Otorrhea • Decreased hearing • Battle signs (24 -48° after injury) • Drip Pad for rhinorrhea • Bedrest

Interventions • Airway – Breathing – Oxygenate, ventilate (PCO 2 30 -35) – Suction only when necessary (2 passes) • Circulation – Maintain CPP > 60 mm. Hg – Normovolemia • Drain CSF • Control stimulation – Narcotic, sedatives, barbiturates • Regulating nursing activities • Thermoregulation – Normothermic (96. 8° – 98. 6°F, 36°-37°C)

Hydrocephalus
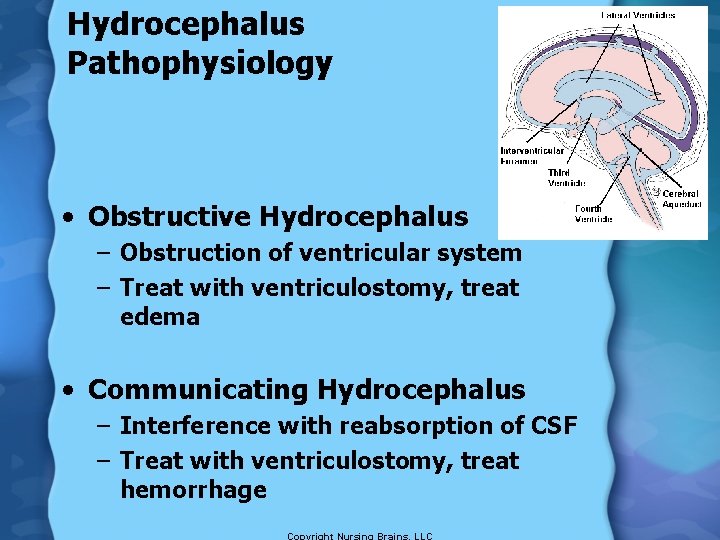
Hydrocephalus Pathophysiology • Obstructive Hydrocephalus – Obstruction of ventricular system – Treat with ventriculostomy, treat edema • Communicating Hydrocephalus – Interference with reabsorption of CSF – Treat with ventriculostomy, treat hemorrhage
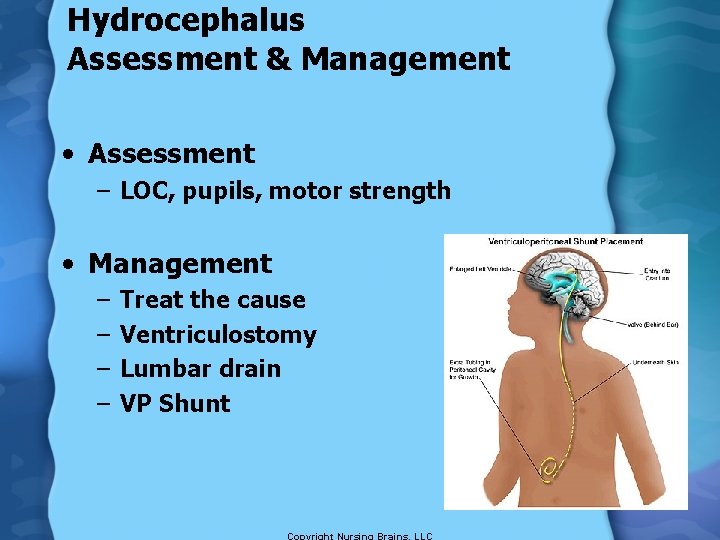
Hydrocephalus Assessment & Management • Assessment – LOC, pupils, motor strength • Management – – Treat the cause Ventriculostomy Lumbar drain VP Shunt
Intracranial Hemorrhage PCCN PAY ATTENTION!!!!
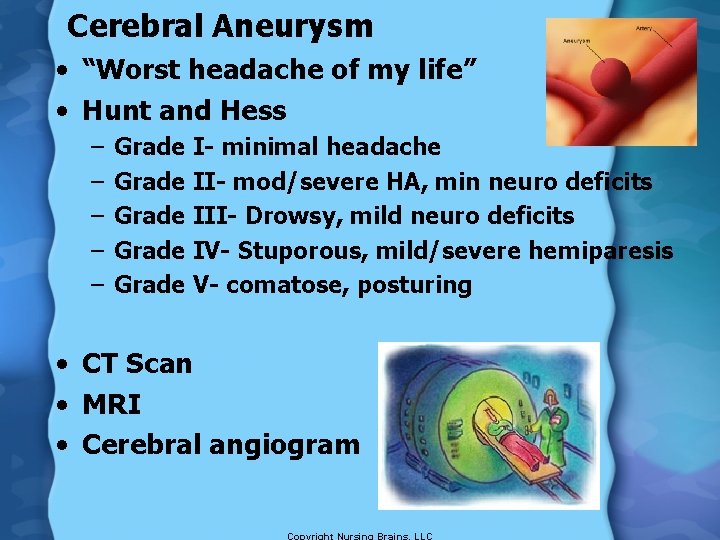
Cerebral Aneurysm • “Worst headache of my life” • Hunt and Hess – – – Grade I- minimal headache Grade II- mod/severe HA, min neuro deficits Grade III- Drowsy, mild neuro deficits Grade IV- Stuporous, mild/severe hemiparesis Grade V- comatose, posturing • CT Scan • MRI • Cerebral angiogram
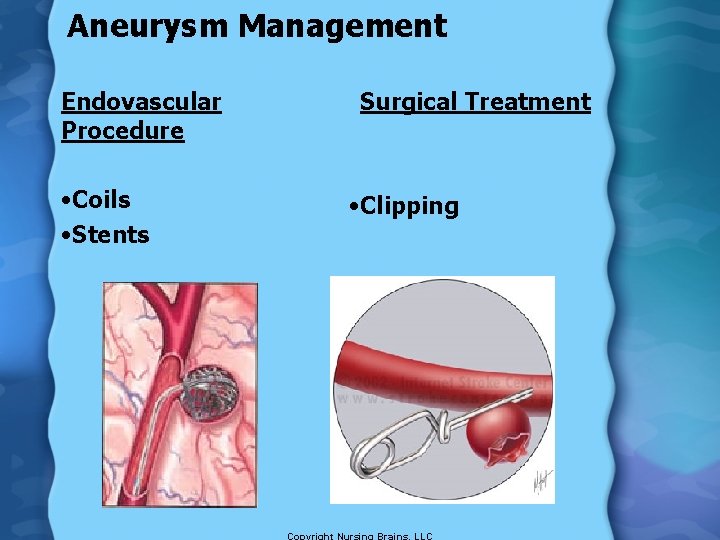
Aneurysm Management Endovascular Procedure • Coils • Stents Surgical Treatment • Clipping

Aneurysm Management • Prevent Rebleeding – – Decrease environmental stimuli Avoid valsalva SBP < 150 mm. Hg (pretreatment) Administer antihypertensives (Labetalol) • Prevent Vasospasm – SBP 160 – 180 mm. Hg (posttreatment) – Calcium channel blocker (Nimodipine) – Triple H therapy • Hypertension, Hypervolemia, Hemodilution
SAH Complications • Vasospasm – Abnormal narrowing of artery – Occurs day 3 to 2 -3 weeks after rupture – Peaks 7 -14 days • Rebleeding – Lysis of clot or hypertension – Occurs 24 hours or 7 -10 days after rupture • Hydrocephalus – Due to SAH, obstructing arachnoid villi – Place ventriculostomy, VP Shunt
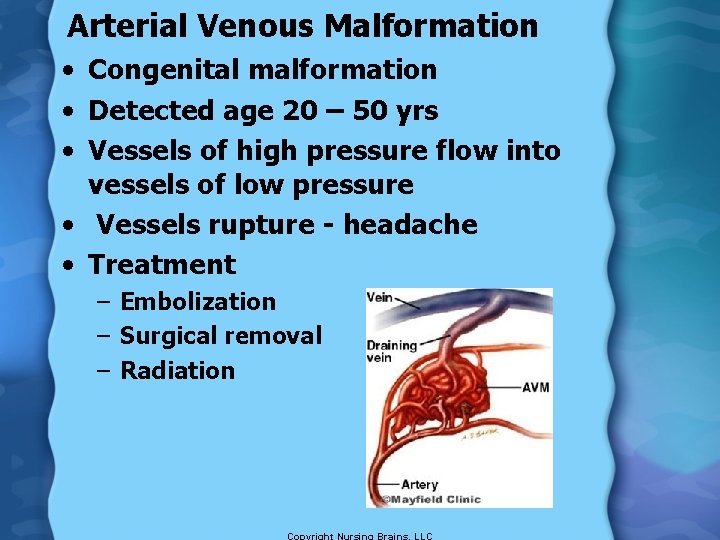
Arterial Venous Malformation • Congenital malformation • Detected age 20 – 50 yrs • Vessels of high pressure flow into vessels of low pressure • Vessels rupture - headache • Treatment – Embolization – Surgical removal – Radiation
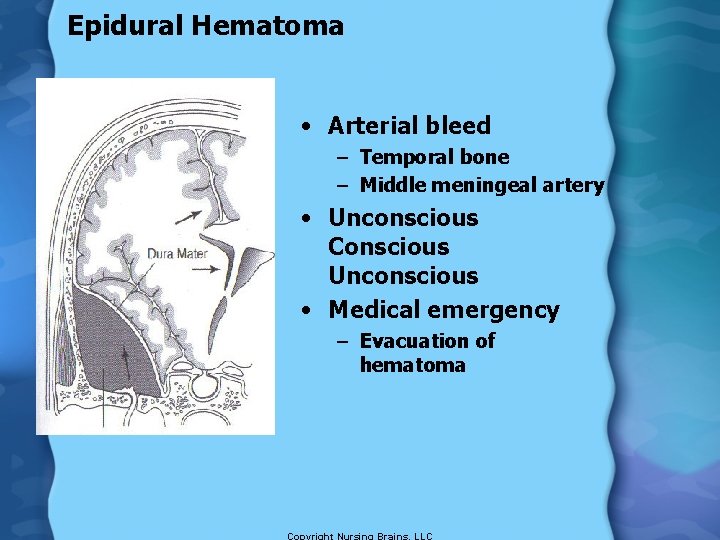
Epidural Hematoma • Arterial bleed – Temporal bone – Middle meningeal artery • Unconscious Conscious Unconscious • Medical emergency – Evacuation of hematoma
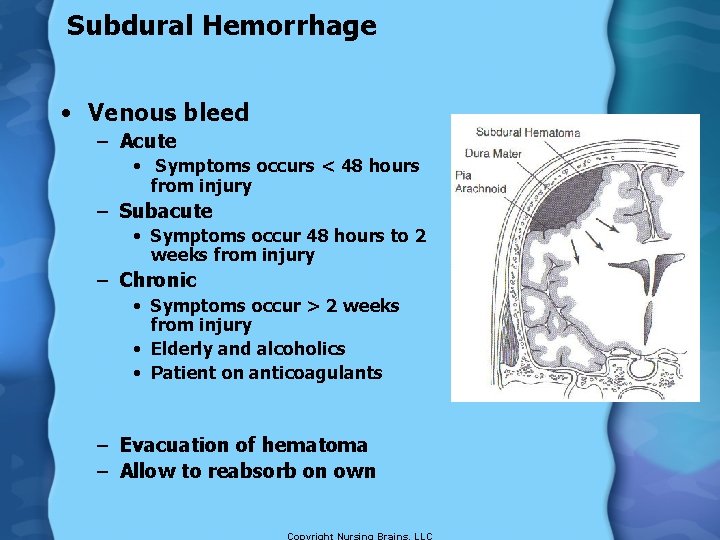
Subdural Hemorrhage • Venous bleed – Acute • Symptoms occurs < 48 hours from injury – Subacute • Symptoms occur 48 hours to 2 weeks from injury – Chronic • Symptoms occur > 2 weeks from injury • Elderly and alcoholics • Patient on anticoagulants – Evacuation of hematoma – Allow to reabsorb on own
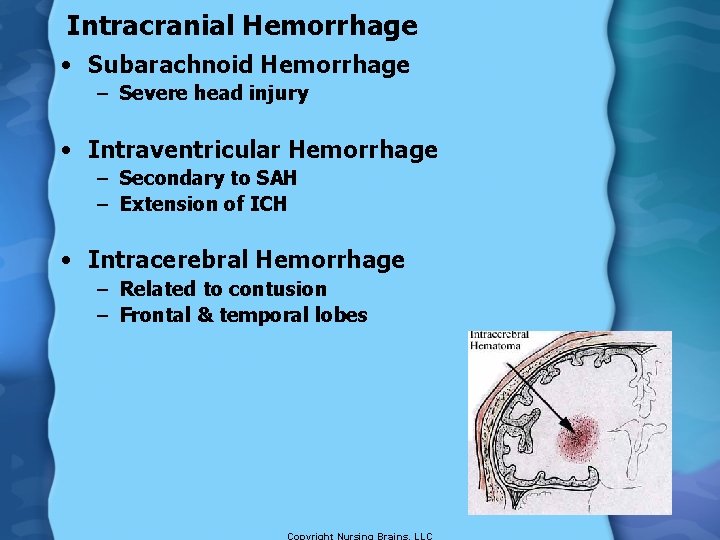
Intracranial Hemorrhage • Subarachnoid Hemorrhage – Severe head injury • Intraventricular Hemorrhage – Secondary to SAH – Extension of ICH • Intracerebral Hemorrhage – Related to contusion – Frontal & temporal lobes

Stroke PCCN PAY ATTENTION!!!!
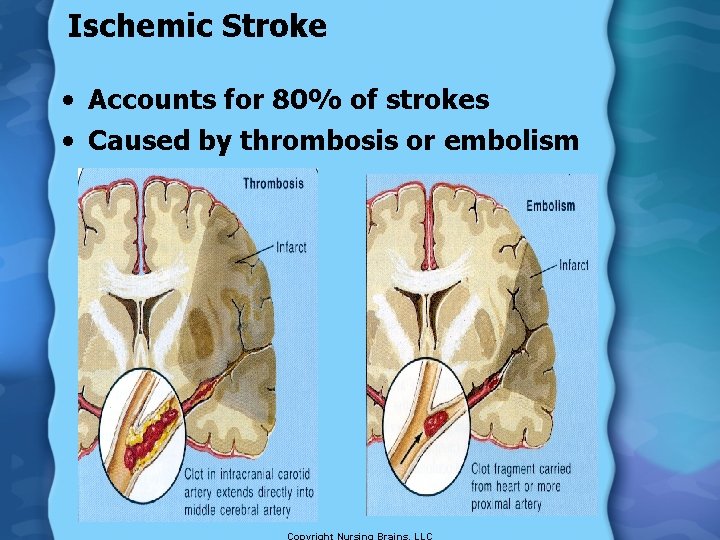
Ischemic Stroke • Accounts for 80% of strokes • Caused by thrombosis or embolism

Signs/Symptoms F-A-S-T – F = FACE numbness or weakness especially one side of body – A = ARM numbness or weakness one side of body – S = SPEECH slurred or difficulty speaking or understanding – T = TIME to immediately call 9 -1 -1 and note time symptoms started or last time person was seen normal

Ischemic Stroke Management • Oxygenation (pulse ox >92%) • BP Control ( 185/110) – Antihypertensives (labetalol) • Glucose control • Thrombolytics (t-PA) – Time of symptom onset (3 hours), CT Scan, weight, 0. 9 mg/kg, bolus 10% of total dose over 1”, remaining dose over 60” – Monitor BP and Neuro exam • Antiplatelets (ASA, Plavix, Aggrenox) • Anticoagulants (Coumadin)
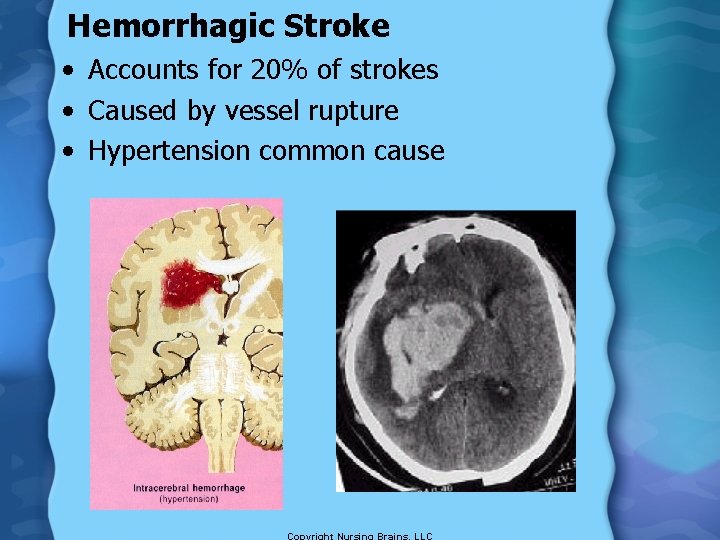
Hemorrhagic Stroke • Accounts for 20% of strokes • Caused by vessel rupture • Hypertension common cause

Hemorrhagic Stroke Signs and Symptoms • Severe headache • Loss of consciousness • Contralateral hemiparesis/hemiplegia • Nausea, vomiting

Hemorrhagic Stroke Management • Maintain airway • BP Management – Labetalol, Nicardipine • Control ICP – HOB 30 degrees, Hyperventilate, Mannitol
Encephalpathy PCCN PAY ATTENTION!!!!

Pathophysiology • Neurologic degeneration – Direct or indirect effect on brain • • • Build up of toxic metabolic products Structural changes Changes in blood flow to brain Changes in electrical activity Change in supply of neurotransmitter substance • Not a disease, results from other disease

Hypoxia/Anoxia • Airway obstruction • Arterial obstruction • Cardiac arrest

Hypoxic-Ischemic • Embolic • Thrombotic • Fat embolism • DIC

Metabolic • Hepatic • Renal • Electrolyte imbalance • Progressive symptom onset • Coma precedes motor abnormalities • Pupil reaction preserved
Infectious • Menigitis • Encephalitis • Vasculitis

Nursing Assessment/Management • Assessment – Level of consciousness - decreased – Chronic alcohol abuse • Management – Monitor level of consciousness – Treat underlying condition – Supportive care
Brain Death • Irreversible cessation of entire brain, including brain stem • Known cause of coma • Absence of the following reflexes – – – – Nonreactive pupils (CN III) Doll’s eyes (oculocephalic) Cold calorics (oculovestibular) Corneal (CN V) Cough Gag (CN IX and X) Spontaneous respirations (Apnea Test)

Seizures PCCN PAY ATTENTION!!!!!

Partial Seizures • 80% of people who have seizures • Starts in only one part of the cerebral cortex - it can spread OR • Stars focally and spreads slowly

• Simple Partial Seizure – Hand may shake – Mouth may twitch uncontrollably – Dizzy, unusual feeling, smell, sound, or sight – Doesn’t affect consciousness – Lasts less than a minute

• Complex Partial Seizure – – – – Staring straight ahead Looking around Fidgeting with clothes Lip smacking Aimless wandering Automatic hand movement LOC is impaired Last 1 -2 minutes

Generalized Seizures • • 20% of people who have seizures Involvement of both hemispheres Consciousness may be impaired Bilateral motor manifestations

• Tonic - Clonic Seizure – – – Grand Mal Entire cerebral cortex is involved Aura Tonic Phase Clonic Phase Doesn’t feel, see, or remember anything during seizure
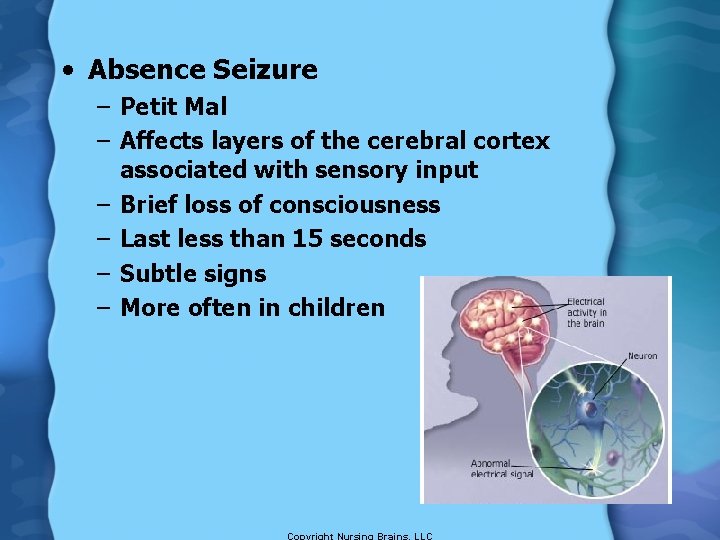
• Absence Seizure – Petit Mal – Affects layers of the cerebral cortex associated with sensory input – Brief loss of consciousness – Last less than 15 seconds – Subtle signs – More often in children

• Myoclonic Seizure – – Generalized jerking of an extremity May cause patient to fall Less than 5 seconds Brief, easy to miss period of unconsciousness – Occur in clusters

• Atonic Seizure – Sudden loss of muscle tone (fall) – Loss of consciousness

Diagnostic Evaluation • • • History EEG CT/MRI Continuous AV/EEG Monitoring SPECT

Management • Protect patient from injury – Move objects, stay with patient, padded bed rails, low bed • Observe and record seizure activity – Note time of onset, body parts involved, incontinence, • Assess airway and breathing – Head-tilt, chin lift – Oxygen, suction – Turn patient on side (aspiration risk) • Medication administration – Benzodiazepine – Antiepileptic drug – Drug levels

Neuromuscular Disorders PCCN you can leave now…. .

Muscular Dystrophy • Myopathy – Progressive muscular weakness • Most common hereditary myopathy • Four common types of MD – – Duchennes (DMD) Becker (BMD) Limb-Girdle Muscular Dystrophy (LGMD) Facioscapulohumeral (FSHD)

Duchenne’s Muscular Dystrophy (DMD) • Most common form of MD • X-linked and primarily affects males • Symptoms begin by age 5 • Death by 3 rd decade
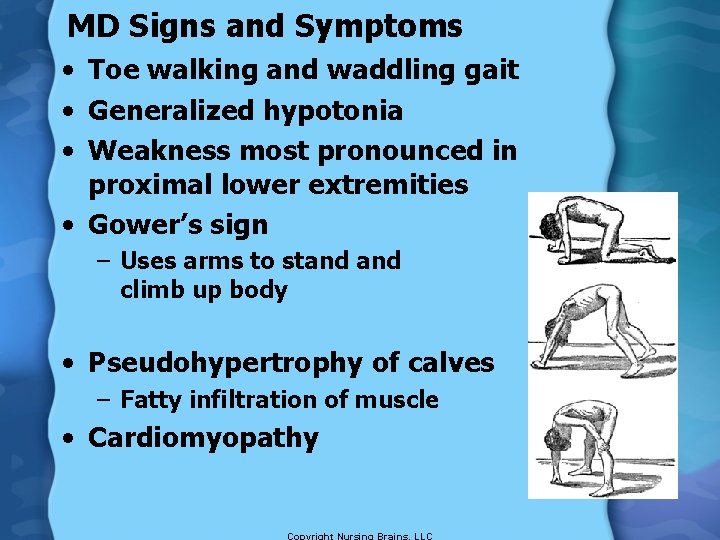
MD Signs and Symptoms • Toe walking and waddling gait • Generalized hypotonia • Weakness most pronounced in proximal lower extremities • Gower’s sign – Uses arms to stand climb up body • Pseudohypertrophy of calves – Fatty infiltration of muscle • Cardiomyopathy

MD Diagnostics and Treatment • Diagnostics – – – Serum CK Genetic testing NCV, EMG MRI with contrast Muscle biopsy EKG, echo • Treatment – – No definitive treatment Prednisone PT, OT Surgical contracture release and fusion

Guillain-Barré Syndrome • Description – Inflammatory process of the nervous system – Demyelination of peripheral nerves – Preceded by suspected viral infection – Accompanied by fever Guillain Barre Strohl

Guillain-Barré Syndrome (con’t) • Signs/Symptoms – Progressive, symmetrical, ASCENDING paralysis – Difficulty in speech, swallowing, mastication (50% of cases) – Impairment of muscles of respiration – ASCENDING bilateral flaccid paralysis with pain – Autonomic dysfunction (hypotension, hypertension, ileus, arrhythmias) – No decrease in LOC – CSF has high protein count – EMG slowing conduction

Guillain-Barré Syndrome (con’t) • Management – Supportive care (immobility & pain issues) – Plasma exchange QOD for 10 -15 days – IVIG over 3 -5 days – Airway management – Adequate hydration and nutrition

Myasthenia Gravis • Chronic, progressive autoimmune-mediated disorder • Causes sporadic weakness of the skeletal muscles – Primarily in the face, lips, tongue, neck and throat – Eyelid drooping and double vision • Muscle weakness with exercise and improved muscle strength with rest • No cure – death (40 -70%) due to respiratory arrest

MG Etiology • T cells and various antibodies attack and impair or destroy acetylcholine receptors at the motor end-plate of neuromuscular junction – Decreased number of acetylcholine receptors at neuromuscular junction • 75% abnormal thymus • 85% hyperplasia of thymus • 15% thymoma

MG Signs and Symptoms Voluntary muscle weakness Exacerbated by continuous use, warmer climates, and stress Increased fatigue in the AM Diplopia, weak EOMs, and ptosis Dysphagia Difficulty/weakness chewing Difficulty swallowing / choking

MG Diagnostic Test • Three tests required for diagnosis Acetylcholine receptor antibody blood test • 85% MG patients have antibody • 50% Occular MG Anti-Mu. SK antibody blood test • Test negative for above then 70% MG patients have antibody Tensilon (edrophonium) challenge test • Give IV 2 -5 mg (max 10 mg) (duration 5 minutes) • Increases level of acetylcholine at junction by blocking acetylcholinesterase • Test + if muscle strength improves • False negative reported with ocular MG Electromyography (EMG): nerve stimulation test showing speed between stimulation and muscle contraction; slowed with MG

MG Medications • Acetylcholinesterase inhibitors Allows ACTH to remain in neuromuscular junction longer Pyridostigmine (Mestinon) • 60 mg every 4 hours • Time released every 12 hours Neostigmine (Prostigmin) • 2 hour duration – Take prior to activity, assess motor strength and secretions – Give medications on time, within 30” of food, and with snack (GI upset) – Atropine to tx diarrhea/salivation from acetylcholinesterase inhibitors – Decrease dose for fasiculations due to nicotinic effects

MG Medications • Immunosuppressants Prednisone • 20 -60 mg/day • Give potassium chloride, calcium carbonate, vitamin D 2 to side effects Azathioprine (Imuran) • 2 -3 mg/kg/day, divided doses (usually 50 mg TID) • Takes up to 6 months for effect Cyclophosphamide (Cytoxan) – rarely used due to toxicity • Reboot immune system • 1. 5 - 5 mg/kg/day • Usually 100 -200 mg a day

MG Treatment • Plasmaphoresis and plasma exchange – Removes antibodies – Short term treatment– must be done regularly – Especially useful for crisis treatment • Intravenous immunoglobulin (IVIG) – – – Pooled human gamma globulin Short term treatment of serious relapse Begin 1 – 2 weeks of onset 2 g/kg dose over 2 -5 days Improvement in 4 -5 days, lasts about 1 month

MG Crisis • Respiratory support is essential in both crisis • Myasthenic is due to infection • Cholinergic is due to over medication
Neurologic Infectious Diseases

Meningitis • Description – Inflammation of meninges • Infective agent – Bacterial: streptococcus pneumonia, neisseria meningitidis, H. influenzae, direct, hematogenous, CSF leak entry – Viral: enteroviruses, arboviruses, herpes viruses, fecal-oral contamination, respiratory droplets – Fungal: cryptococcus neoformans, open wound, mucous membrane

Meningitis • Signs/Symptoms – Headache, fever, nausea, vomiting – Nuchal rigidity, Kernig’s, Brudinski's, photophobia – Altered LOC, seizures – CSF • Bacterial: Cloudy, protein, glucose • Viral: Clear, protein, normal glucose • Management – – – Control symptoms Antibiotics, antiviral, antifungal Assess LOC Assess for ICP Monitor temperature

West Nile Virus • Arbovirus—mosquito-borne viruses that are transmitted by bloodfeeding arthropods • Transmission – – – Blood transfusion Organ transplantation Breast milk Intrauterine Laboratory acquisition • Incubation period of 3– 14 days

West Nile Virus • Clinical presentation of mild Infection • 20% of people develop mild infection • Flu-like symptoms: Fever, headache, nausea and vomiting, backache, malaise, myalgia, maculopapular rash • Symptoms may last 3– 6 days

West Nile Virus • Personal protective – Avoid being outdoors at dawn and dusk – Wear light-colored, long clothing – Use DEET insect repellent – Drain standing water

Lyme Disease • Ticks transmit Lyme borreliosis during a blood meal • Occurs May–Sept. • Tick must be attached for 24– 72 hrs • Serology studies – ELISA a positive Ig. M response – Western blot used as confirmatory test if ELISA is positive
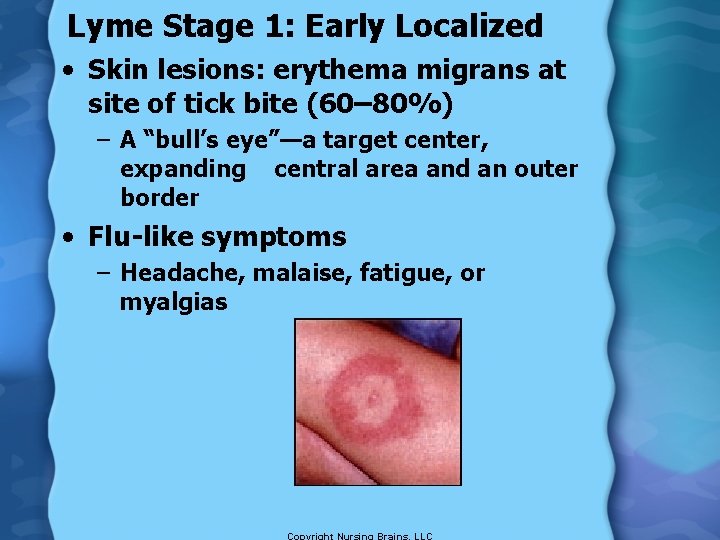
Lyme Stage 1: Early Localized • Skin lesions: erythema migrans at site of tick bite (60– 80%) – A “bull’s eye”—a target center, expanding central area and an outer border • Flu-like symptoms – Headache, malaise, fatigue, or myalgias
Lyme Stage 2: Early Disseminated • Acute neuroborreliosis appears weeks, months • Malaise, fatigue, lymphadenopathy • Nervous System: – Meningeal signs, headache, neck stiffness, difficult concentrating, cranial nerve dysfunction, Bell’s palsy, radiculopathies, and ataxia • Cardiac System: – Atrioventricular block, myopericarditis, pancarditis • Lyme arthritis

Lyme Stage 3: Late Chronic • Nervous system and joints continuous inflammation for >1 year • Cognitive changes and fatigue • Lyme encephalopathy, polyneuropathy, and leukoencephalitis • Chronic arthritis • Lymphocytoma; acrodermatitis, chronica atrophicans

Lyme Disease - Management • Early infection – 10– 21 days antibiotics • Doxycycline for adults and children >8 years • Amoxicillin for children < 8 years • Late infection – Ceftriaxone given IV for 2– 4 weeks – Cefotaxime or penicillin G (alternative)

Lyme Prevention • Check for ticks after being outdoors • Wear light clothing, long sleeves, and pants • Apply tick/insect repellent to clothing • Remove tick properly: grasp tick with tweezers or a piece of tissue, then pull straight out • Human vaccine: available – Booster injections needed every 1– 3 years • Vaccinate pets annually and check for ticks

Bell’s Palsy • Herpes virus causes inflammation/compression of CN VII (Facial Nerve) • Unilateral facial weakness • Steroids and antiviral agents – Prednisone and acyclovir
Brain Tumor

Brain Tumor Etiology • Primary—unknown • Metastatic – 35% lung – 20% breast – 10% kidney – 10% gastrointestinal tract
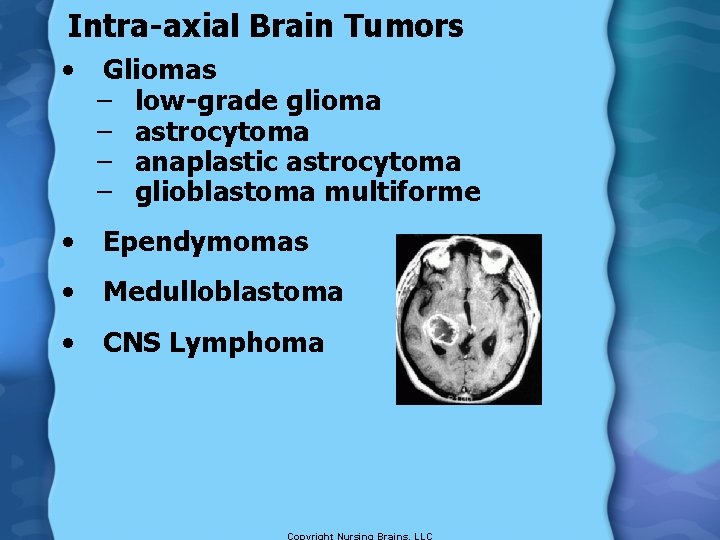
Intra-axial Brain Tumors • Gliomas – low-grade glioma – astrocytoma – anaplastic astrocytoma – glioblastoma multiforme • Ependymomas • Medulloblastoma • CNS Lymphoma
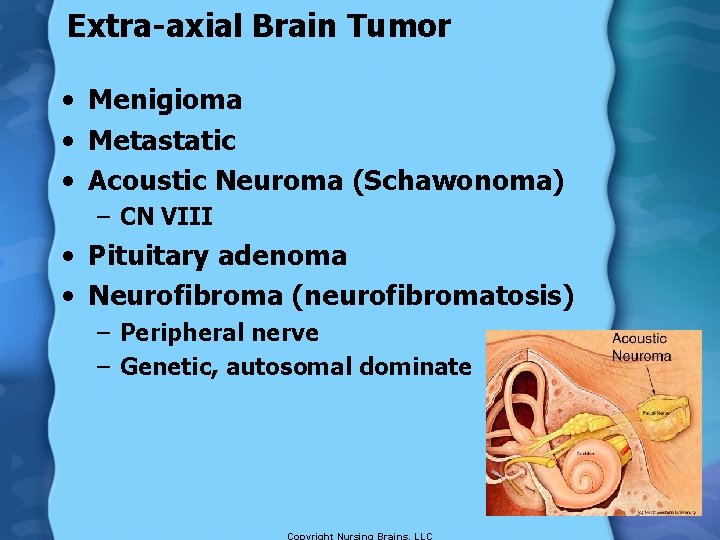
Extra-axial Brain Tumor • Menigioma • Metastatic • Acoustic Neuroma (Schawonoma) – CN VIII • Pituitary adenoma • Neurofibroma (neurofibromatosis) – Peripheral nerve – Genetic, autosomal dominate

Brain Tumor Surgical Treatment • Biopsy • Craniotomy • Stereotaxis Surgery • Transsphenoidal/Endoscopic

Brain Tumor Radiation Therapy • Damages DNA of rapidly dividing cells • 4000– 6000 c. Gy total dose • Duration of 4– 8 weeks • Side Effects – Skin burns, hair loss, fatigue, local swelling • Patient teaching includes “do not erase” markings • Radiation necrosis

Brain Tumor Chemotherapy • Slows cell growth • Cytotoxic Drugs – CCNU, BCNU, PCV, Cisplatin, Etoposide, Vincristine, Temozolomide (Temodar) • Side effects – Oral mucositis, bone marrow suppression, fatigue, hair loss, nausea and vomiting, anxiety, peripheral neuropathy
Neurosurgery
Postop Neurological Deficits • Diminished level of consciousness • Communication deficits – Expressive/receptive aphasia (cerebral edema) • Motor and sensory deficits • Headache – First few days – Check head dressing – Codeine, Tylenol #3

Postop Neurological Deficits • Elevated temperature – Hypothalamus, infection – Antipyretics, hypothermia blanket • Periocular edema – Discoloration, ecchymosis – Peak 48 – 72 hours (edema last 5 days, ecchymosis last 12 days) – Cold compress • Diminished gag/swallow (CN IX & X) – Posterior fossa surgery
Postop Neurological Deficits • Visual disturbances – Diplopia (eye patch) – Field cuts (scan the room) • Loss of corneal reflex – Eye shield, tape lid shut, artificial tears • Personality changes – Edema, drugs, stress, surgery
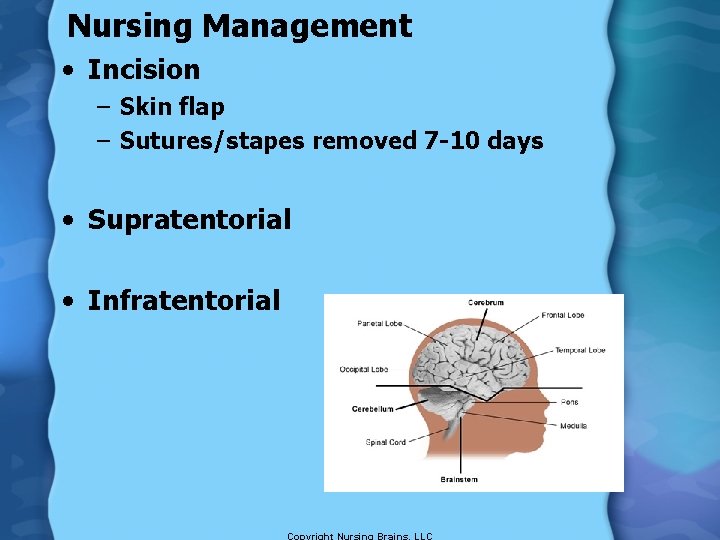
Nursing Management • Incision – Skin flap – Sutures/stapes removed 7 -10 days • Supratentorial • Infratentorial

Nursing Management • Head Dressing – – Turban style dressing MD to remove after 24 hours Monitor for blood or CSF Once removed observe incision for redness, drainage, or signs of wound infection

Nursing Management • Positioning Head of Bed – Elevate HOB 30 degrees – Maintain neck in neutral position • Turning and Positioning – No restriction • Ambulation – Allowed OOB as soon as tolerated – Infratentorial caution with dizziness

Nursing Management • Fluid and Electrolyte Balance – Maintain euvolemia – Record I & O – Monitor electrolyte and osmolarity • DVT Prophylaxis – Sequential compression device – Heparin, Lovenox • Administer analgesics as ordered
Postoperative Complications • Cerebral hemorrhage • Increased intracranial pressure – Peak 72 hours • Tension pneumocephalus – Entry of air, posterior fossa craniotomy – Within 24 hours to 1 week • Hydrocephalus – Edema or subarachnoid bleeding
Postoperative Complications • Seizures – Within first 7 days, focal seizure – Prophylactic anticonvulsants • CSF Leakage • Meningitis – Prophylactic antibiotics • Wound infection – Staphylococcal – Redness, drainage, foul odor, elevated WBC

GOOD LUCK!!!!
- Slides: 104