CBT Instructors Workshop Todays Topics 1 State of

CBT Instructors Workshop

Today’s Topics 1 State of King County EMS 2 CPR: Then and Now 3 New CPR Guidelines 4 ROC Study

1 State of King County EMS 2006 Mickey Eisenberg, MD, Ph. D Medical Program Director
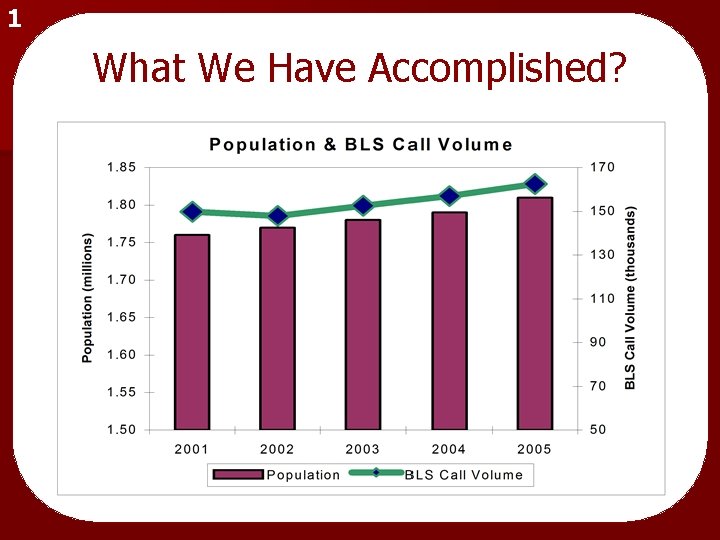
1 What We Have Accomplished?
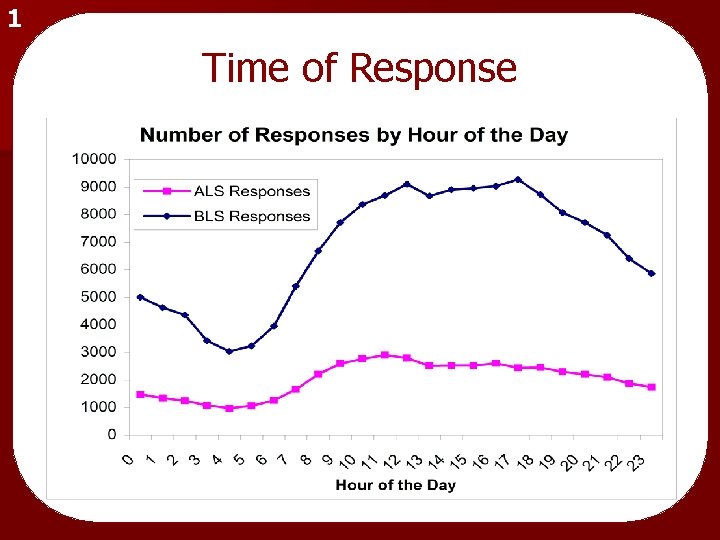
1 Time of Response
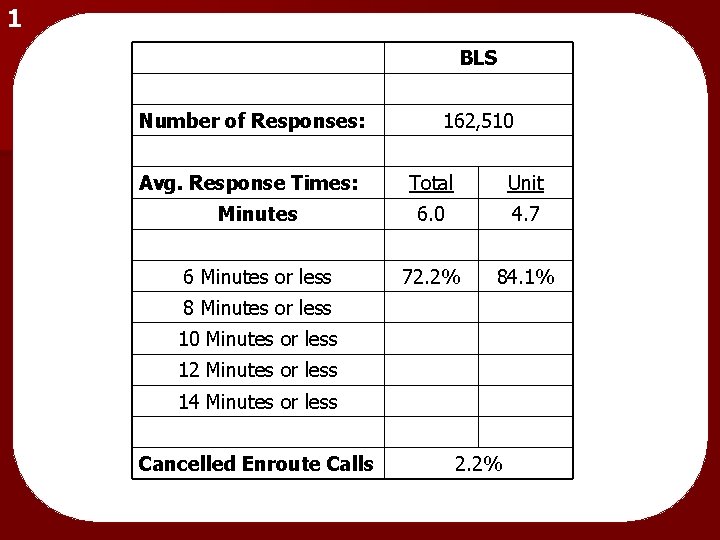
1 BLS Number of Responses: 162, 510 Avg. Response Times: Minutes Total Unit 6. 0 4. 7 6 Minutes or less 72. 2% 84. 1% 8 Minutes or less 10 Minutes or less 12 Minutes or less 14 Minutes or less Cancelled Enroute Calls 2. 2%
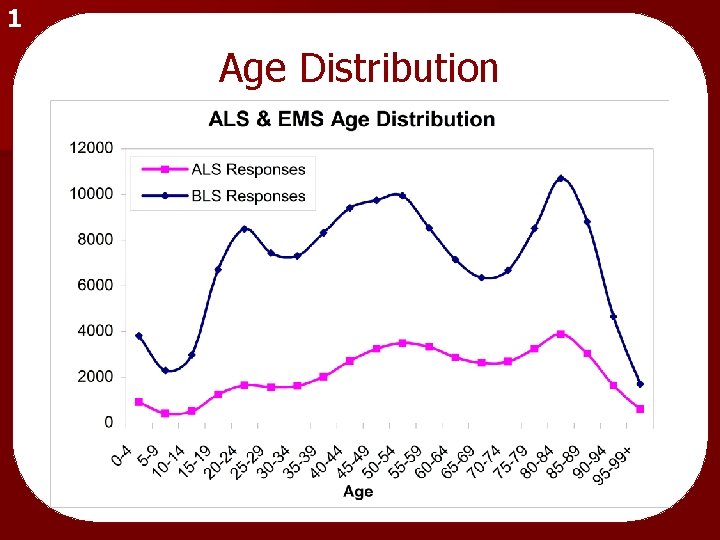
1 Age Distribution
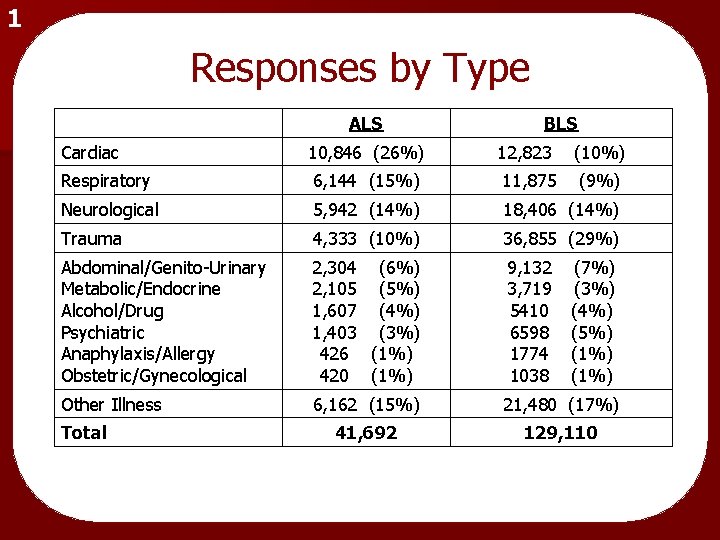
1 Responses by Type ALS BLS Cardiac 10, 846 (26%) 12, 823 (10%) Respiratory 6, 144 (15%) 11, 875 (9%) Neurological 5, 942 (14%) 18, 406 (14%) Trauma 4, 333 (10%) 36, 855 (29%) Abdominal/Genito-Urinary Metabolic/Endocrine Alcohol/Drug Psychiatric Anaphylaxis/Allergy Obstetric/Gynecological 2, 304 (6%) 2, 105 (5%) 1, 607 (4%) 1, 403 (3%) 426 (1%) 420 (1%) 9, 132 (7%) 3, 719 (3%) 5410 (4%) 6598 (5%) 1774 (1%) 1038 (1%) Other Illness 6, 162 (15%) 21, 480 (17%) 41, 692 129, 110 Total
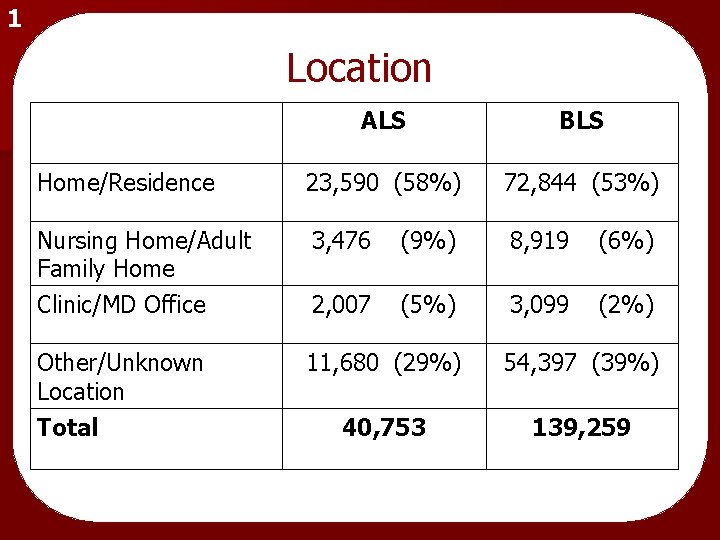
1 Location ALS BLS Home/Residence 23, 590 (58%) 72, 844 (53%) Nursing Home/Adult Family Home 3, 476 (9%) 8, 919 (6%) Clinic/MD Office 2, 007 (5%) 3, 099 (2%) Other/Unknown Location Total 11, 680 (29%) 54, 397 (39%) 40, 753 139, 259

1 Cardiac Arrest Total number of cardiac arrests for all causes with resuscitation attempted: YEAR # 2001 1141 2002 1147 2003 1093 2004 1087 2005 1124
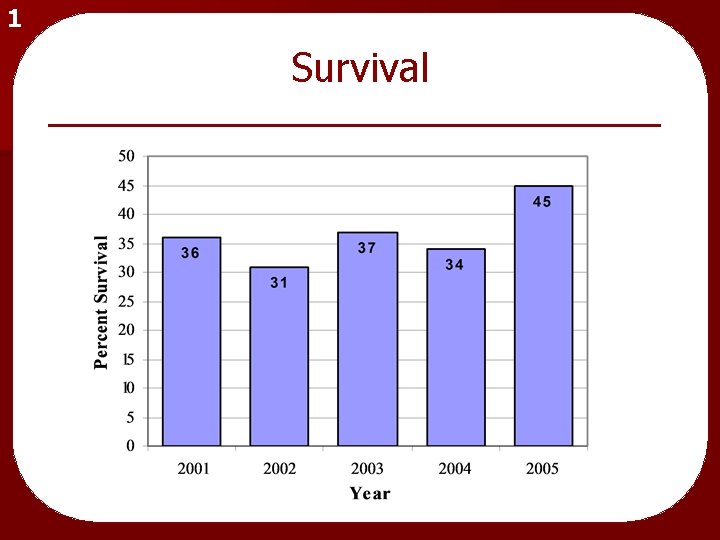
1 Survival

1 Past Year • • Infectious Disease Plan ROC infrastructure established CPR/Defibrillation protocol changed EMT naloxone

1 EMT Naloxone Study of potential benefit of EMT naloxone for narcotic overdose: • 164 patients received naloxone for OD in one year. • Respiratory rate < 10 in 48%. • Good response in 73%. • Uneven distribution among departments. • Agitation/combativeness in 15%, emesis in 6%.

1 Past Year • • • Infectious Disease Plan ROC infrastructure established CPR/Defibrillation protocol continuation EMT naloxone SPHERE pilot

1 JEMS: June 2006

1 SPHERE Pilot • South King Fire and Rescue, Kent, Port of Seattle, Auburn • Comparison of alert (given by EMTs) versus letter sent by medical director • Follow-up phone call

1 SPHERE Pilot

1 SPHERE Pilot Patient Characteristics Patients identified for the alert pilot had an average systolic blood pressure of 175, and an average diastolic blood pressure of 94.

1 SPHERE Pilot Patient Comments • One patient noted that she “absolutely loved” the firefighters. • Another patient appreciated being told about her blood pressure and said that it was “valuable information” for those who have elevated BP and don’t know it. • Another patient commented on the firefighters’ “excellent job. ”

1 SPHERE Pilot Preliminary Findings • 65% of patients interviewed said the firefighter influenced them to see a doctor. • 68% of patients interviewed said the firefighter influenced them to get their blood pressure rechecked. • 94% of patients interviewed were pleased that the firefighter told them their blood pressure was elevated. • Alert seemed to have more influence compared to letter.

1 New Projects for 2007 SPHERE (Supporting Public Health with Emergency Responders) • Expand to entire county. • Use of routinely collected information to give useful health information to patients • Duty to inform patients • Hypertension and diabetes

1 SPHERE: Standard of Care in King County for 2007 Alerts and after-care instructions: • High blood pressure alert • High blood sugar alert • Low blood sugar after-care instruction

1 High Blood Pressure Alert Eligible patients: • Systolic BP > 160 or • Diastolic BP > 100 Not eligible: • Paramedic transported patients • Nursing home patients Documentation is mandatory.

1 High Blood Sugar Alert Eligible patients: • Diabetic: BS > 300 • Non-diabetic: BS >175 Not eligible: • Paramedic transported patients • Nursing home patients Documentation is mandatory.

1 Low Blood Sugar After-Care Instructions Eligible patients: • Patients on insulin • Low blood sugar • Respond fully to therapy Documentation is mandatory.

1 2007 EMT Evaluations Underway • Study of glucagon for hypoglycemia • Study of left-at-scene patients following treatment for hypoglycemia

1 Possible Future EMT Evaluations? • EMS active screening for type II diabetes? • Consider aspirin for acute coronary syndrome? • SPHERE – How to achieve follow-up? ü Pilot in Renton, Bellevue, Shoreline • SPHERE – Pilot to compare alert versus alert followed by reminder letter.

My Thanks It is an honor to work with you all. Dr. Mickey Eisenberg Medical Director

And Finally • • • Questions Suggestions Comments Clarifications Opinions Orations

2 CPR: Then and Now Mike Helbock, M. I. C. P. , NREMT-P Manager – EMS Training and Education Seattle/King County

It’s all about history, learning and moving forward…
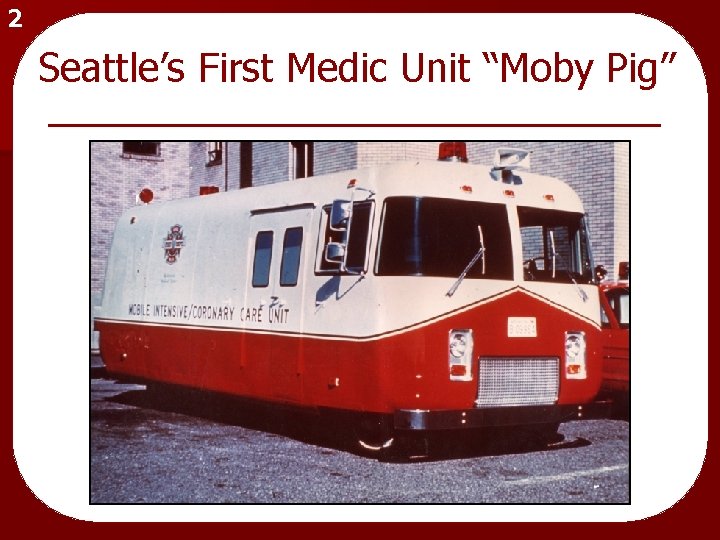
2 Seattle’s First Medic Unit “Moby Pig”

2 So…what’s on the ‘New to Do” list • • New thoughts…. CPR compression/numbers “Quality” of CPR (DVD-R) NEW airway obstruction techniques Resuscitation Outcome Consortium

2 New thoughts on the numbers *One minute of CPR between shocks may not be enough…

2 CPR (and all of it’s friends) • Disappointment in the lack of increased survival rates since the 70’s. • Don’t be fooled…a round of CPR isn’t a minute! (closer to 40 seconds). • AEDs can take between 5 -28 seconds to detect a rhythm! • Delivering up to 3 shocks can range between 39 -90 seconds!
2 A Little Background Each of the links in the chain of survival are important for resuscitation. 9 -1 -1 Early CPR Early Defib Timely ALS

2 Background, continued Though the emphasis has been placed on early and frequent defibrillation. 9 -1 -1 Early CPR Early Defib Timely ALS
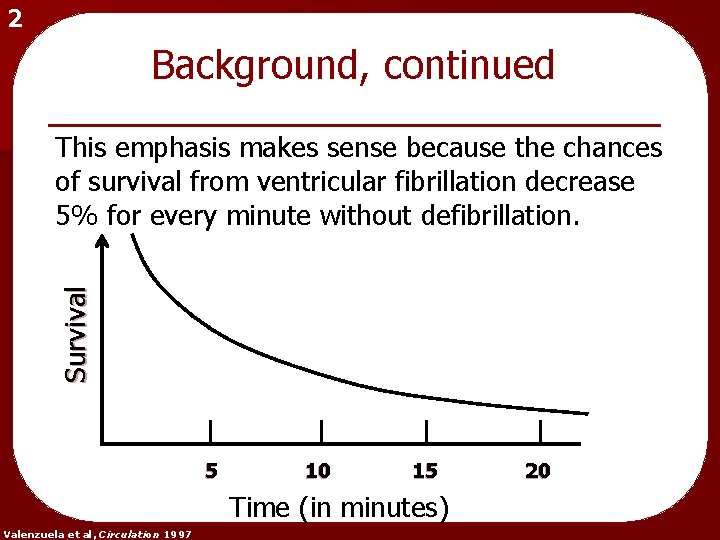
2 Background, continued Survival This emphasis makes sense because the chances of survival from ventricular fibrillation decrease 5% for every minute without defibrillation. 5 10 15 20 Time (in minutes) Valenzuela et al, Circulation 1997
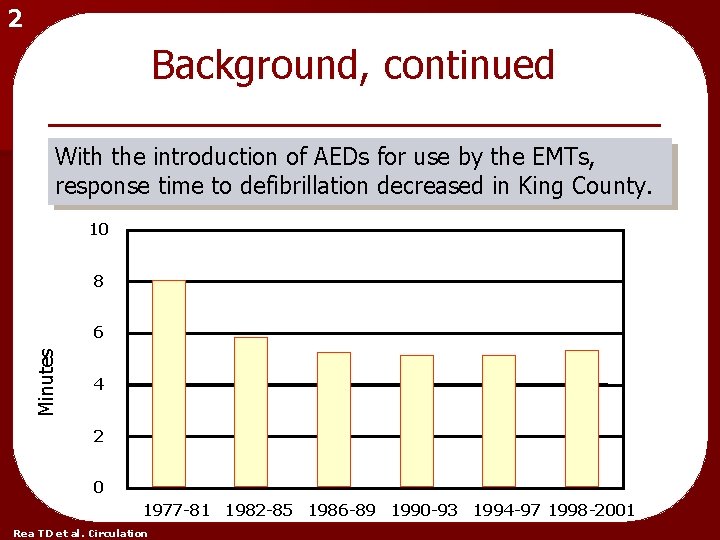
2 Background, continued With the introduction of AEDs for use by the EMTs, response time to defibrillation decreased in King County. 10 8 Minutes 6 4 2 0 1977 -81 1982 -85 1986 -89 1990 -93 1994 -97 1998 -2001 Rea TD et al. Circulation
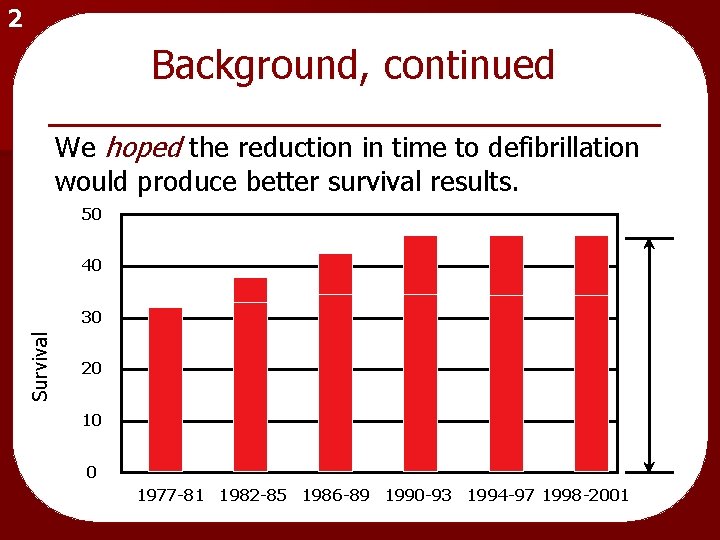
2 Background, continued We hoped the reduction in time to defibrillation would produce better survival results. 50 40 Survival 30 20 10 0 1977 -81 1982 -85 1986 -89 1990 -93 1994 -97 1998 -2001
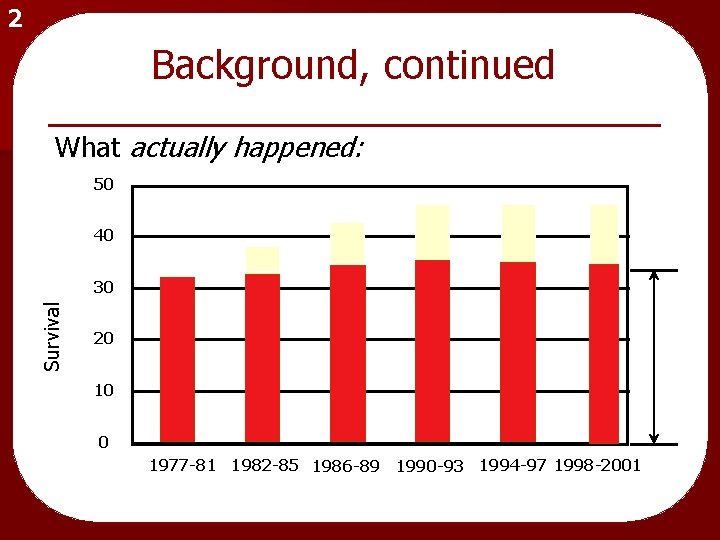
2 Background, continued What actually happened: 50 40 Survival 30 20 10 0 1977 -81 1982 -85 1986 -89 1990 -93 1994 -97 1998 -2001

2 Background, continued So we reviewed the AHA protocol which was: 1. Determine VF. 2. Stacked shocks. 3. Pulse check after each shock. 4. 1 minute of CPR and re-analyze. AND………

2 Background, continued We looked more closely at the relationship between CPR and defibrillation from a physiological standpoint. 9 -1 -1 Early CPR Early Defib Timely ALS

2 What We Found The shock alone is not enough. The shock can reset the heart electrically but mechanically the heart still needs to pump blood. CPR before and after the shock can help the mechanical action of the heart.

2 So…Out With the Old The “old” AHA algorithm inadvertently increased the amount of time without the mechanical component of CPR. Yet these activities were very low yield because: • Only 10% needed a stacked shock, and • Only 2% had a pulse with the “after shock” pulse check.

2 In With the New So we implemented a single shock – start CPR algorithm in January 2005. Eliminated stacked shocks. Eliminated pulse check after shock. Extended period of CPR following shock from 1 to 2 minutes. The goal was to increase CPR especially during the period immediately following the shock.
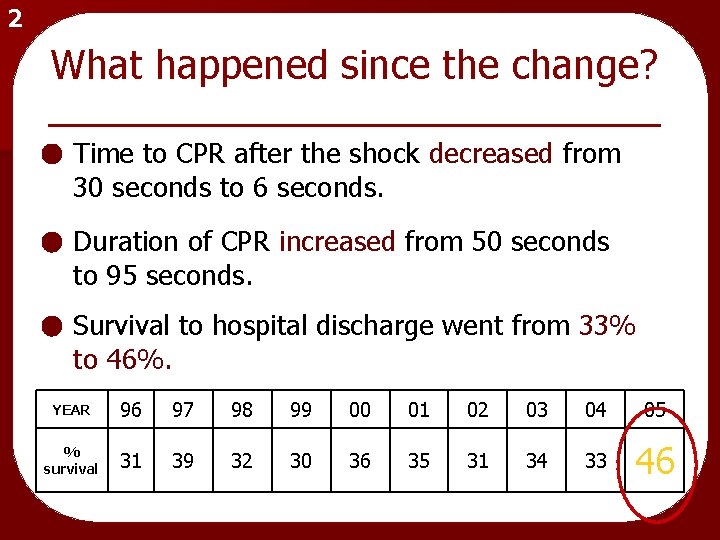
2 What happened since the change? Time to CPR after the shock decreased from 30 seconds to 6 seconds. Duration of CPR increased from 50 seconds to 95 seconds. Survival to hospital discharge went from 33% to 46%. YEAR 96 97 98 99 00 01 02 03 04 05 % survival 31 39 32 30 36 35 31 34 33 46

2 Summary *More “hands on” *Less shocks *More focus on “Quality CPR" *New methods of resuscitation - cooling - ITD - mechanical devices

Which brings us to the question: CAN WE DO EVEN BETTER?

3 New CPR Guidelines
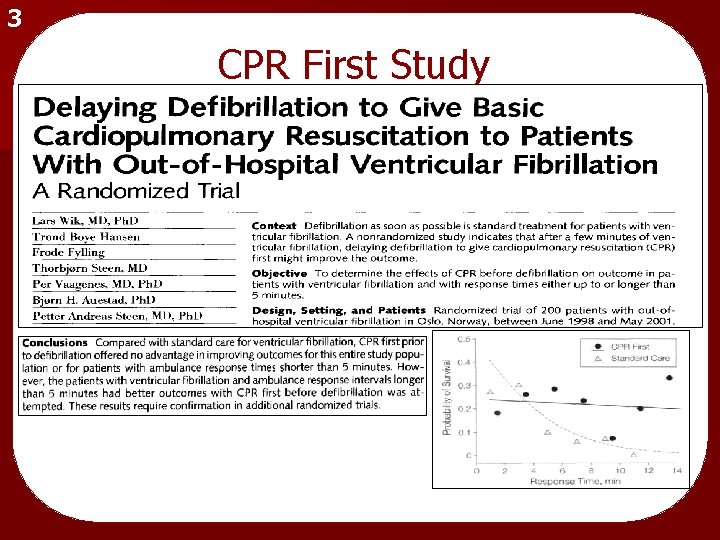
3 CPR First Study

3 CPR: Questions • Quantity of CPR…(how much? ) • Quality of CPR…(how good? ) • Interface between the AED and defibrillation

3 New CPR Guidelines ADULTS: 1 or 2 person CPR WITHOUT intubation 30: 2

3 New CPR Guidelines ADULTS: 1 or 2 person CPR WITHOUT intubation 30: 2 Medics arrive and intubate

3 New CPR Guidelines ADULTS: 1 or 2 person CPR WITHOUT intubation 30: 2 Medics arrive and intubate “Continuous compressions” with 8 -10 ventilations per minute. (1 breath/6 -8 sec. )

3 New CPR Guidelines INFANTS/ CHILDREN: 15: 2 2 person CPR WITHOUT intubation (HCP)

3 New CPR Guidelines INFANTS/ CHILDREN: 15: 2 2 person CPR WITHOUT intubation (HCP) Medics arrive and intubate
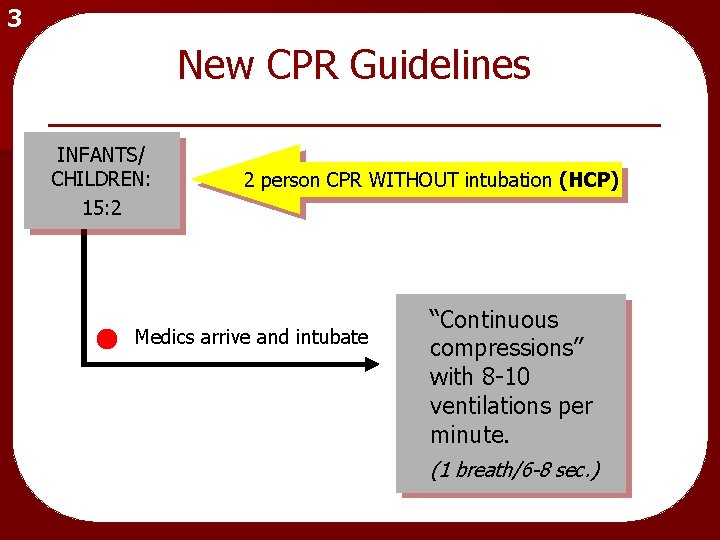
3 New CPR Guidelines INFANTS/ CHILDREN: 15: 2 2 person CPR WITHOUT intubation (HCP) Medics arrive and intubate “Continuous compressions” with 8 -10 ventilations per minute. (1 breath/6 -8 sec. )

3 CPR—Focus on Quality Depth of compressions • Depth of 1 1/2– 2 inches (or more in larger people). • Minimize interruptions in chest compressions. • Rotate compressors every 2– 3 minutes to minimize fatigue.

3 CPR—Focus on Quality Depth of compressions Ventilations • 30: 2 prior to intubation. • 8— 10 ventilations per minute when intubated. (1 breath/6 -8 sec). • Inspiration phase of no more than 1 second.

3 CPR—Focus on Quality Depth of compressions Ventilations Decompression • Complete chest recoil after each compression. REQUIRED!

3 CPR—Focus on Quality Depth of compressions Ventilations Decompression Rate of compression • Push Hard / Push Fast • (100/min)

Airway Obstruction

3 New Airway Guidelines ADULTS and CHILD Foreign-body airway obstruction
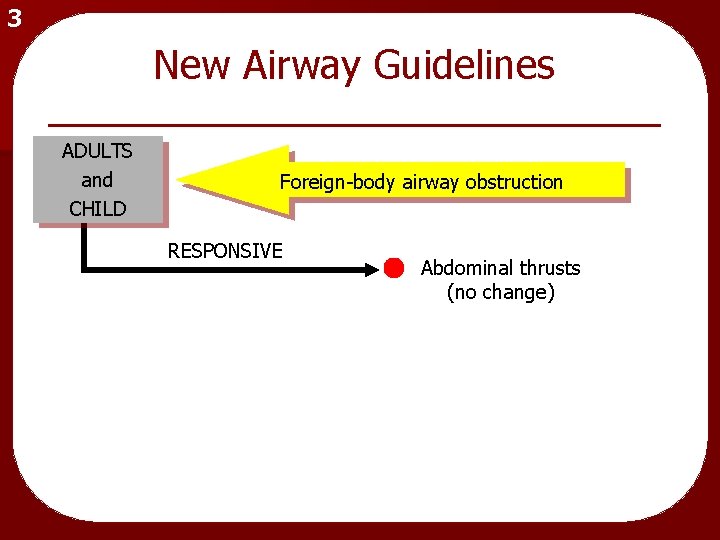
3 New Airway Guidelines ADULTS and CHILD Foreign-body airway obstruction RESPONSIVE Abdominal thrusts (no change)
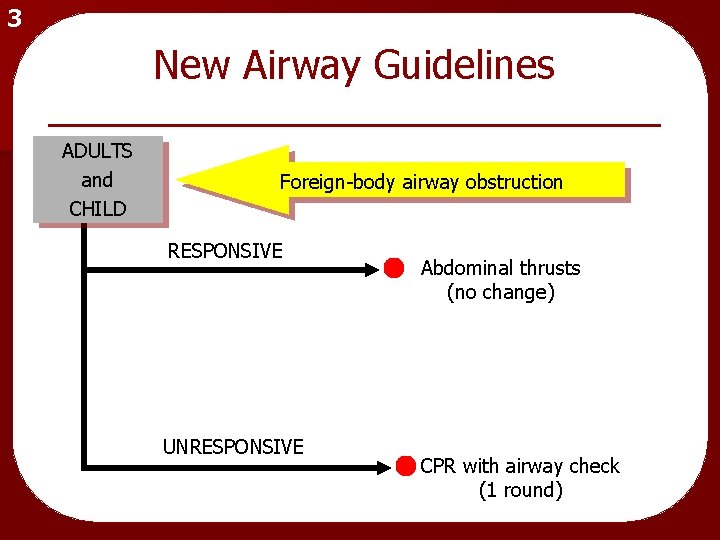
3 New Airway Guidelines ADULTS and CHILD Foreign-body airway obstruction RESPONSIVE UNRESPONSIVE Abdominal thrusts (no change) CPR with airway check (1 round)

3 New Airway Guidelines INFANT Foreign-body airway obstruction
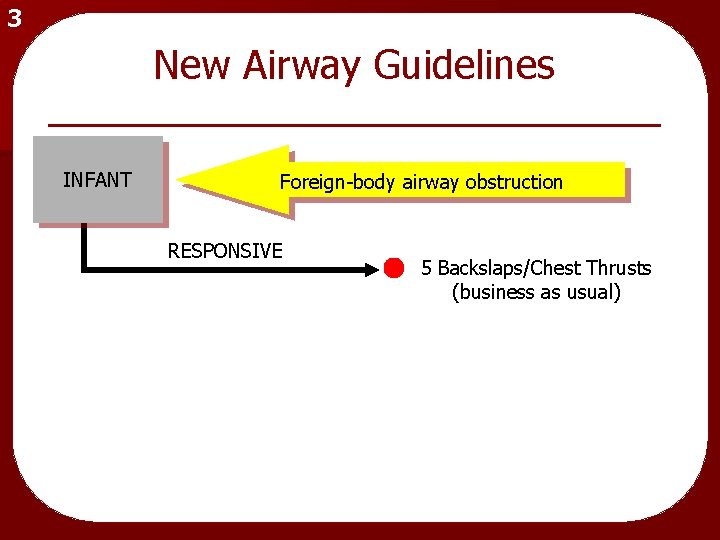
3 New Airway Guidelines INFANT Foreign-body airway obstruction RESPONSIVE 5 Backslaps/Chest Thrusts (business as usual)
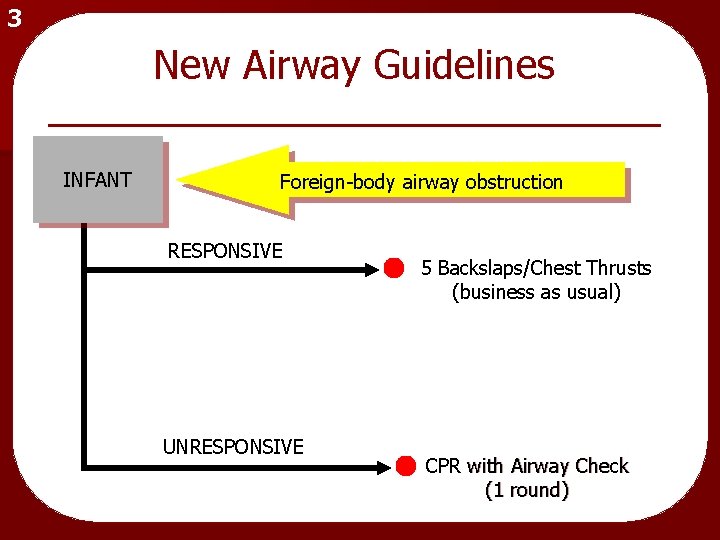
3 New Airway Guidelines INFANT Foreign-body airway obstruction RESPONSIVE UNRESPONSIVE 5 Backslaps/Chest Thrusts (business as usual) CPR with Airway Check (1 round)

Rescue Breathing

3 New Airway Guidelines ADULTS Rescue breathing
3 New Airway Guidelines ADULTS Rescue breathing 10 to 12 breaths/minute (1 breath every 5 -6 seconds)
3 New Airway Guidelines ADULTS Rescue breathing 10 to 12 breaths/minute (1 breath every 5 -6 seconds) Must obtain “chest rise”

3 New Airway Guidelines CHILD / INFANT Rescue breathing
3 New Airway Guidelines CHILD / INFANT Rescue breathing 12 to 20 breaths/minute (1 breath every 3 -5 seconds)
3 New Airway Guidelines CHILD / INFANT Rescue breathing 12 to 20 breaths/minute (1 breath every 3 -5 seconds) Must obtain “chest rise”

3 So…what are we doing about it? • • • Research, Research…. . Shock early…shock often…shock a lot… is out! Cases of VF on decline. Conversion with 1 st shock 95%. New studies are needed to help us understand what may be right!

The “ROC”

4 Welcome to the ROC

4 R. O. C. • Resuscitation Outcome Consortia • Federally Funded Data Collection Study • Study Specific EMS Interventions
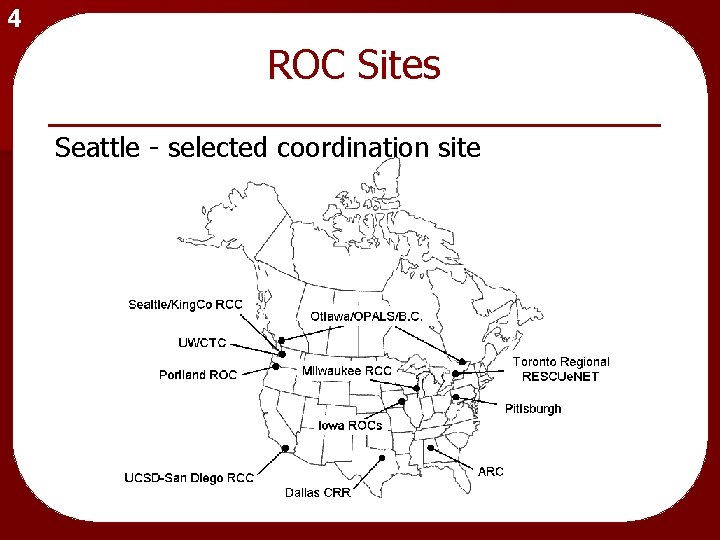
4 ROC Sites Seattle - selected coordination site

4 ROC Sponsors • National Institutes of Health • Canadian Institutes of Health Research • Defense Research & Development Canada • American Heart Association • Heart & Stroke - Canada

4 What is the ROC? • Consortium of EMS providers and researchers focused on outcomes from cardiac arrest and trauma. • Goal is to evaluate new approaches and treatments. • EMS providers will be primarily responsible for conducting studies.

The Cardiac Arm…

4 Purpose of the Study To determine outcomes in cardiac arrest when comparing… 1 Difference between CPR with the ITD and CPR with a sham valve. 2 Difference between analyze early and analyze late protocols.

4 Analyze Early/Analyze Late • The heart may need to be "primed" before it can be defibrillated. • CPR – especially chest compressions primes the heart by filling it with oxygenated blood. • How much priming does the heart need before the shock?

4 Analyze Early/Analyze Late Analyze Early: – 1 round (30 compressions) of priming before AED analysis – Business as usual in Seattle/King County Analyze Late: – Longer period of priming before AED analysis – 3 minutes of CPR before first analysis
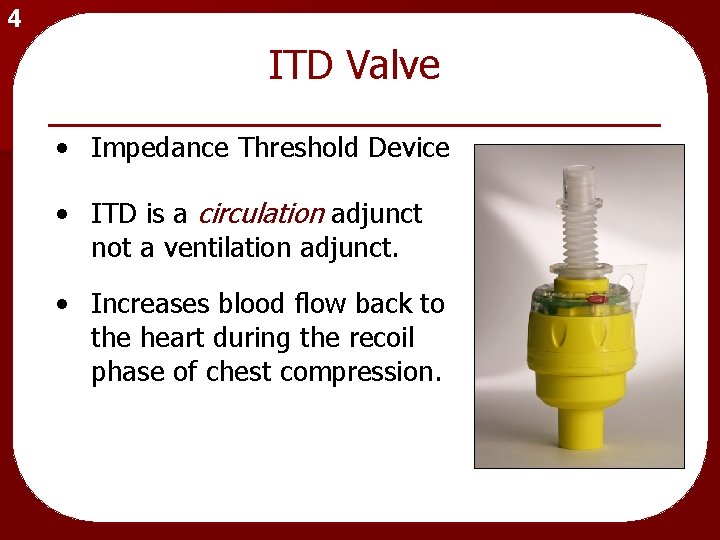
4 ITD Valve • Impedance Threshold Device • ITD is a circulation adjunct not a ventilation adjunct. • Increases blood flow back to the heart during the recoil phase of chest compression.

4 Purpose of an ITD Valve • Prevents air flow into chest during recoil. • Maximizes the vacuum effect, pulling more blood back to the heart. • Which enables more forward blood flow with the next compression.
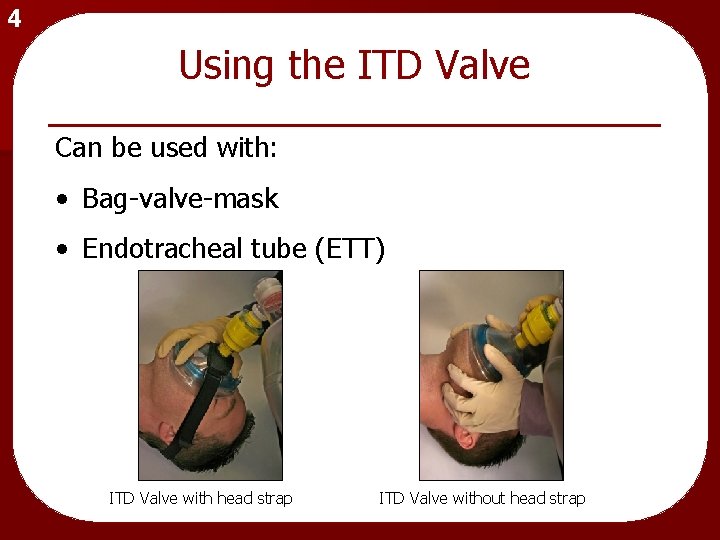
4 Using the ITD Valve Can be used with: • Bag-valve-mask • Endotracheal tube (ETT) ITD Valve with head strap ITD Valve without head strap

and the quest continues…

Acknowledgments • • • Mickey Eisenberg, MD Tom Rea, MD Leonared Cobb, MD Michael Copass, MD Michele Olsufka, RN David Carlbom, MD • • • Will Longstreth, MD Steve Deem, MD Peter Kudenchuk, MD Charles Maynard, Ph. D Billy Reuben Medic One Foundation

Mike Helbock 206 -423 -4674 mike. helbock@metrokc. gov
- Slides: 93