CBC Wbc 10900 N 45 Eosinophil 12 Hgb




• CBC Wbc: 10900 N: 45% Eosinophil: 12% Hgb: 12. 6 PT: 12. 7 INR: 1. 1 PTT: 39 FDP: >5(positive) Fibrinogen: NL D-dimer: >500(positive) plt: 63000

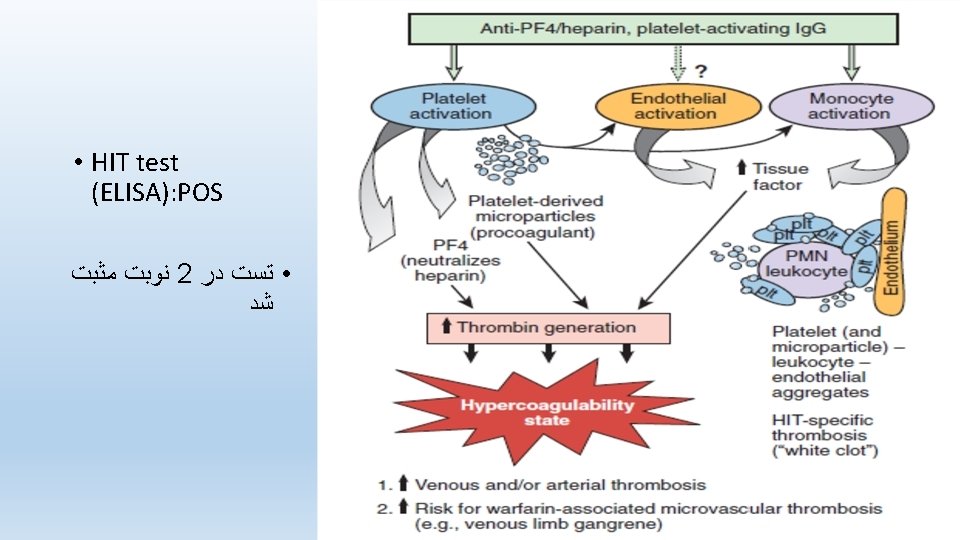

Thrombocytopenia and Thrombosis in association with heparin treatment PTP: causes bleeding but not thrombosis; however, PTP may resemble HIT in that both disorders usually occur about a week after major surgery requiring blood transfusion and postoperative heparin treatment

Vasculitis+thrombocytopenia+thrombosis • Buerger’s disease • Hypersensitivity (‘allergic’) vasculitis • Microscopic polyarteritis (MPA) • Polyarteritis nodosa (PAN) • Moya moya • Behc¸et’s disease

• ANA: neg • ds DNA: neg • ANCA: neg • HLA B 5: Neg • HLA B 51: Neg

. ﻫﺎی ﺳﺮیﺎﻝ ﺍﺋﻮﺯیﻨﻮﻓیﻠی ﻣﺪﺍﻭﻡ ﺩﺍﺷﺖ CBC • ﺩﺭ ﺑﺮﺭﺳی ﻫﺎ ﺑیﻤﺎﺭ ﻣﺎ ﺩﺭ . ﺑیﻤﺎﺭ ﻧیﺰ ﺑﺎﻻﺗﺮ ﺍﺯ ﺣﺪ ﻧﺮﻣﺎﻝ ﺑﻮﺩ Ig. E ﻭ ﺳﻄﺢ hyperimmunoglobulin E syndrome (HIES)=? ? Hyperimmunoglobulin E syndrome (HIES) is a rare primary immunodeficiency characterized by recurrent staphylococcal infections of skin and lungs and elevated levels of immunoglobulin E (Ig. E).


HIT Heparin-induced thrombocytopenia (HIT) is a prothrombotic, immunemediated complication of unfractionated and low molecular weight heparin (LMWH) therapy.

moderate thrombocytopenia 5 -10 days after initial heparin exposure, detection of platelet-activating anti-platelet factor 4 (PF 4)/heparin antibodies, and an increased risk of venous and arterial thrombosis.

• In adult patients receiving heparin, the prevalence of HIT is reported to be 0. 5 -5%. • published case series/reviews of HIT in children suggest that the prevalence of HIT may be lower than in adults (1. 5%-3. 7%) and as low as 0. 33% in non-neonates receiving cardiopulmonary bypass.

The term HIT has been used to describe 3 groups of patients: - those for whom laboratory testing for HIT was sent because of clinicalsuspicion(“suspected HIT”) -patients with expert clinician opinion HIT and positive laboratory testing (HIT) -HIT with thrombosis (HITT)

Definition of HIT/HITT Thrombocytopenia (platelet count fall >50% or platelet nadir >20000 cells/m. L) with Recent or concurrent heparin exposure and the absence of other causes for thrombocytopenia, were positive PF 4/heparin ELISA, and met expert consensus.

Differential diagnosis • • • • Hemodilution post-surgery Severe pulmonary embolism Sepsis DIC (multiple causes besides HIT) Cancer-associated DIC Antiphospholipid syndrome Thrombolytic therapy EDTA-induced pseudothrombocytopenia GP IIb/IIIa inhibitor-induced thrombocytopenia Drug-induced thrombocytopenia (other than heparin) Post-transfusion purpura Thrombotic thrombocytopenic purpura Non-immune heparin-associated thrombocytopenia

HEPARIN RESISTANCE • Definition: • Inadequate prolongation of the partial thromboplastin time (PTT) or activated clotting time despite administration of therapeutic dosages of unfractionated heparin (UFH; e. g. , >1500 U/hr for the treatment of venous thromboembolism [VTE]; 400 U/kg during cardiopulmonary bypass • Causes: • Supraphysiologic levels of factor VIII and/or fibrinogen (e. g. , acute phase response) • Antithrombin III (ATIII) deficiency: primary OR secondary (DIC , extensive thrombosis, CABG) • increased levels of binding proteins; • Increased clearance (e. g. , during pregnancy). • Management: • If ATIII level is low (e. g. , <70% of normal): consider administering of FFP or an ATIII infusion to boost levels above 100%. • If ATIII level is normal : monitor heparin therapy with regular assay of anti–factor Xa levels.

Clinical events associated with HIT • Venous thrombosis (30 -70%) • • • Deep vein thrombosis (DVT) Pulmonary embolism (PE) Adrenal necrosis (adrenal vein thrombosis) Cerebral venous (sinus) thrombosis Venous limb gangrene (VKA associated) • Arterial thrombosis (“white clots”) (15 -30%) • Limb artery thrombosis • Stroke • Myocardial infarction • Skin lesions at heparin injection sites (10%) • Skin necrosis • Erythematous plaques • Acute reactions after i. v. heparin bolus (10%) • Disseminated intravascular coagulation (DIC) (10%)
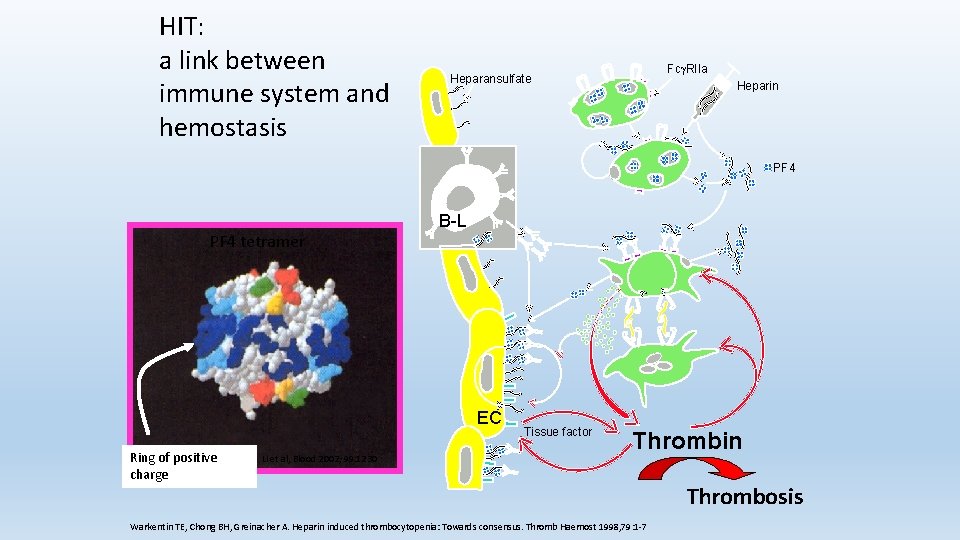
HIT: a link between immune system and hemostasis Fcg. RIIa Heparansulfate Heparin PF 4 tetramer B-L EC Ring of positive charge Li et al, Blood 2002; 99: 1230 Tissue factor Thrombin Warkentin TE, Chong BH, Greinacher A. Heparin induced thrombocytopenia: Towards consensus. Thromb Haemost 1998, 79: 1 -7 Thrombosis
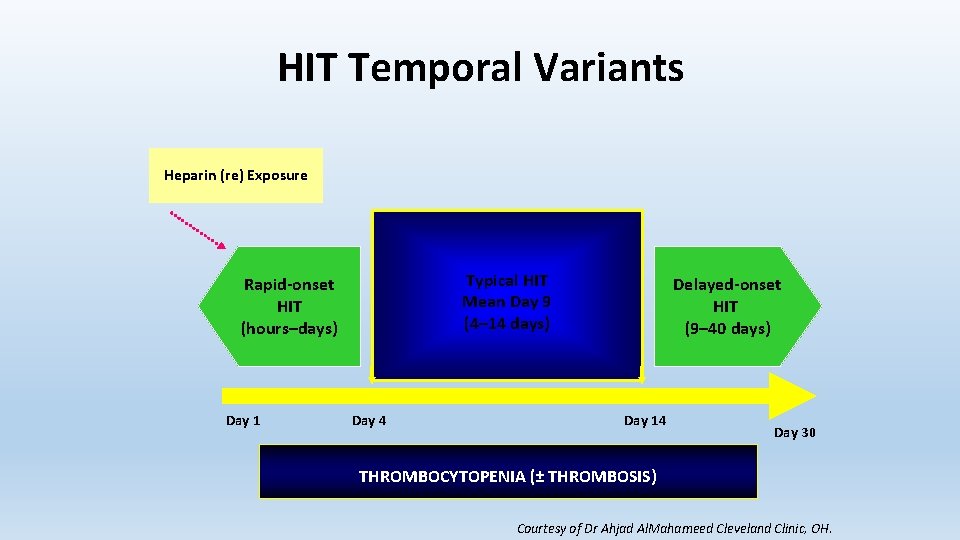
HIT Temporal Variants Heparin (re) Exposure Typical HIT Mean Day 9 (4– 14 days) Rapid-onset HIT (hours–days) Day 1 Day 4 Delayed-onset HIT (9– 40 days) Day 14 Day 30 THROMBOCYTOPENIA (± THROMBOSIS) Courtesy of Dr Ahjad Al. Mahameed Cleveland Clinic, OH.

CLINICAL SCORING SYSTEMS • HIT Expert Probability Score by Cuker et al. • a post-CPB scoring system by Lillo-Le Louët et al. • 4 T’s scoring system by Warkentin et al.

OVERDIAGNOSIS OF HEPARIN-INDUCED THROMBOCYTOPENIA • At most, only 50% of patients with positive immunoassay results truly have HIT. • Even lower in patients in the ICU and patients who are tested for anti. PF 4/heparin antibodies because they have DVT

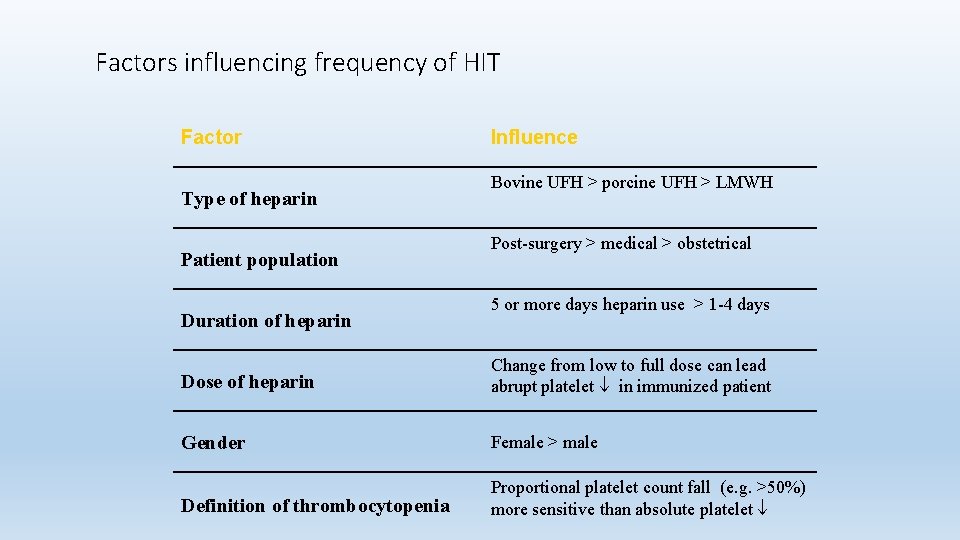
Factors influencing frequency of HIT Factor Type of heparin Patient population Duration of heparin Influence Bovine UFH > porcine UFH > LMWH Post-surgery > medical > obstetrical 5 or more days heparin use > 1 -4 days Dose of heparin Change from low to full dose can lead abrupt platelet in immunized patient Gender Female > male Definition of thrombocytopenia Proportional platelet count fall (e. g. >50%) more sensitive than absolute platelet
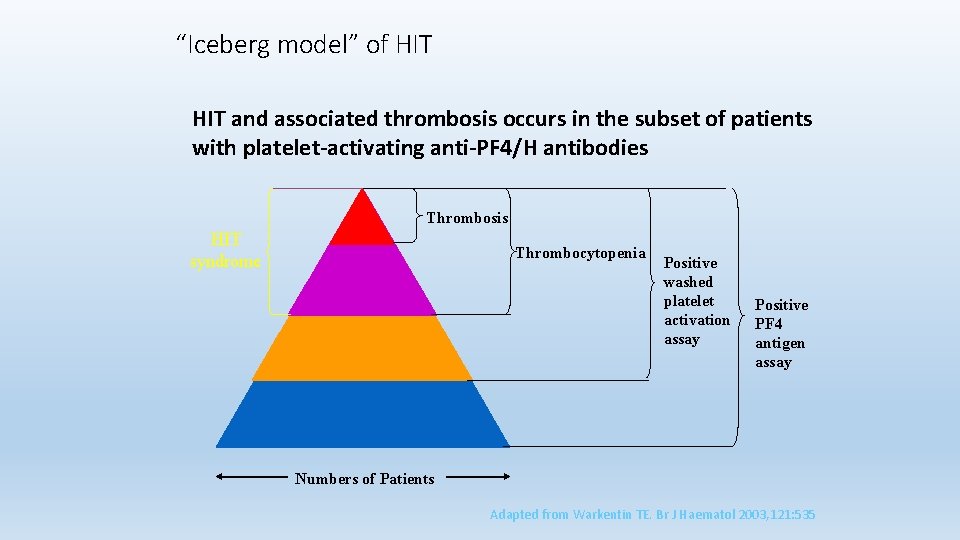
“Iceberg model” of HIT and associated thrombosis occurs in the subset of patients with platelet-activating anti-PF 4/H antibodies Thrombosis HIT syndrome Thrombocytopenia Positive washed platelet activation assay Positive PF 4 antigen assay Numbers of Patients Adapted from Warkentin TE. Br J Haematol 2003, 121: 535

LABORATORY STUDIES • Currently, the 2 classes of tests used to assist in the diagnosis of HIT are: immunologic (antigenic) and Functional (platelet activation) assays. the antigen assay detects the initial immune response, whereas the functional assay detects the activation of platelets, leading to thrombosis.

Detection of HIT antibodies • Platelet activation assays • Serotonin release assay (SRA; uses “washed” platelets) • Heparin-induced platelet activation (HIPA) assay (uses “washed” platelets) • Platelet aggregation test (PAT; uses citrateanticoagulated platelet-rich plasma) • Platelet microparticles (flow cytometry) • Antigen assays • • PF 4/heparin-enzyme immunoassay (ELISA) PF 4/polyvinyl sulfonate EIA Fluid-phase EIA Particle gel immunoassay

enzyme-linked immunosorbent assay (ELISA), have a high degree of sensitivity (99%) and thus have high negative predictive value, making them excellent tests to rule out a diagnosis of HIT. repeating the ELISA using 2 -point increases the specificity of HIT testing but can decrease the negative predictive value and sensitivity.

functional (platelet activation) assay These tests measure platelet activation from the heparin-PF 4 -antibody complex by mixing donor platelet-rich plasma with patient plasma and heparin. The 2 most common functional assays are : the heparin-induced platelet activation assay and the serotonin release assay.

Heparin-induced Platelet Aggregation Assay (HIPAA) The heparin-induced platelet activation assay will exhibit platelet aggregation and an increase in turbidity at therapeutic concentrations of heparin, but not at supratherapeutic concentrations.

The Heparin-induced Platelet Aggregation Assay (HIPAA) The HIPAA, like the SRA, employs washed platelets from normal donors platelet aggregation in the presence of heparin rather than serotonin release is used as an indicator of the presence of HIT antibodies. The assay is rapid, does not use a radioactive isotope and is less technically demanding than SRA.

14 C-serotonin-release assay (SRA) The serotonin release assay, generally considered the gold standard because of its high sensitivity (>95%)and specificity (>95%) , measures the sample’s radioactivity and the percentage release of serotonin from platelets.

14 C-serotonin-release assay (SRA) The basis of the SRA is that antibodies from patients with HIT will cause platelet activation and release of 14 C-serotonin from platelet-dense granules when HIT serum is incubated with normal donor platelets at therapeutic concentrations of heparin Disadvantages of this test are the use of radioactive substances and it is technically demanding.
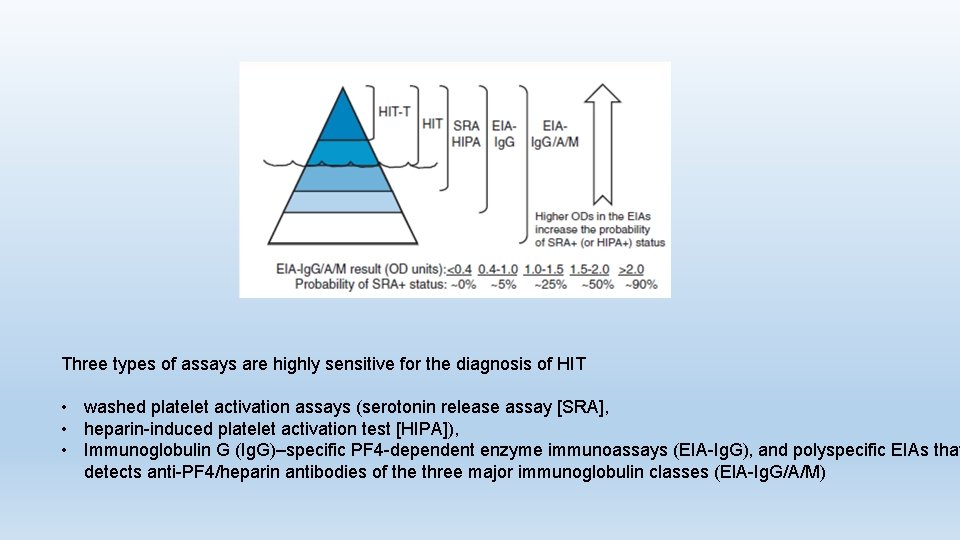
Three types of assays are highly sensitive for the diagnosis of HIT • washed platelet activation assays (serotonin release assay [SRA], • heparin-induced platelet activation test [HIPA]), • Immunoglobulin G (Ig. G)–specific PF 4 -dependent enzyme immunoassays (EIA-Ig. G), and polyspecific EIAs that detects anti-PF 4/heparin antibodies of the three major immunoglobulin classes (EIA-Ig. G/A/M)

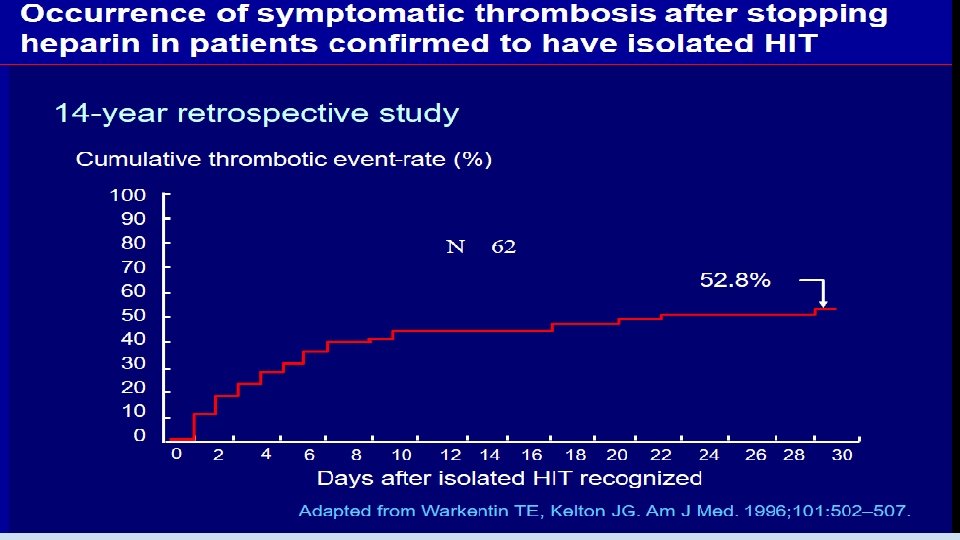
MANAGEMENT AND TREATMENT Cessation alone is not enough to prevent thrombotic events. The 30 -day risk for subsequent thrombosis following the cessation of heparin therapy is estimated to be at least 19% and possibly as high as 52%.

If warfarin therapy has been started when HIT is diagnosed, reversal with vitamin K should occur because of its depletion of proteins C and S and the increased risk for venous limb gangrene.

PLATELET TRANSFUSION====? the 2012 American College of Chest Physicians (ACCP) guidelines do not recommend routine platelet transfusion in patients with HIT. However, they do support transfusions to severely thrombocytopenic patients with HIT who are bleeding or necessitate transfusion during the performance of an invasive procedure with a high risk for bleeding.

ALTERNATIVE ANTICOAGULATION. Two groups of alternative nonheparin anticoagulant are currently available: a) Direct Thrombin Inhibitors which reduce thrombin activity b) Antifactor Xa which reduce thrombin generation.
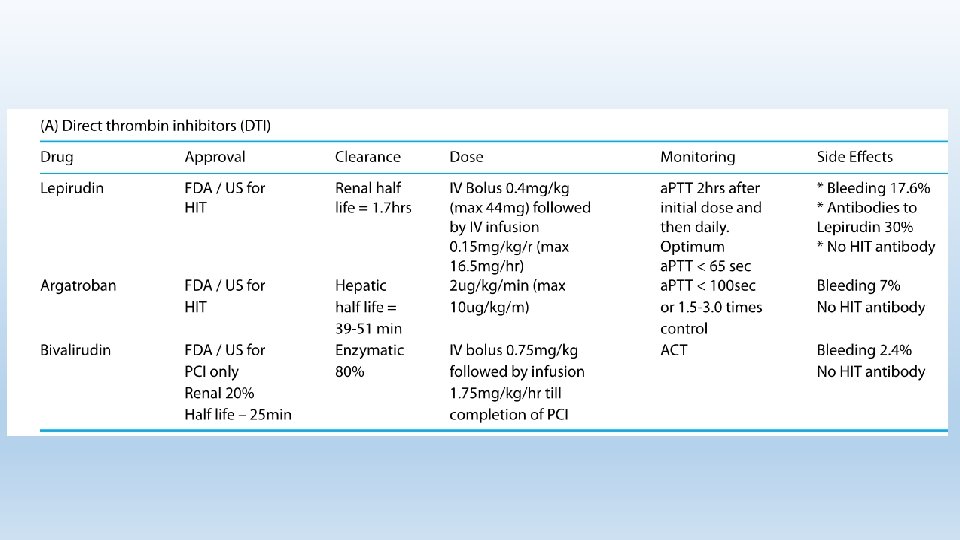

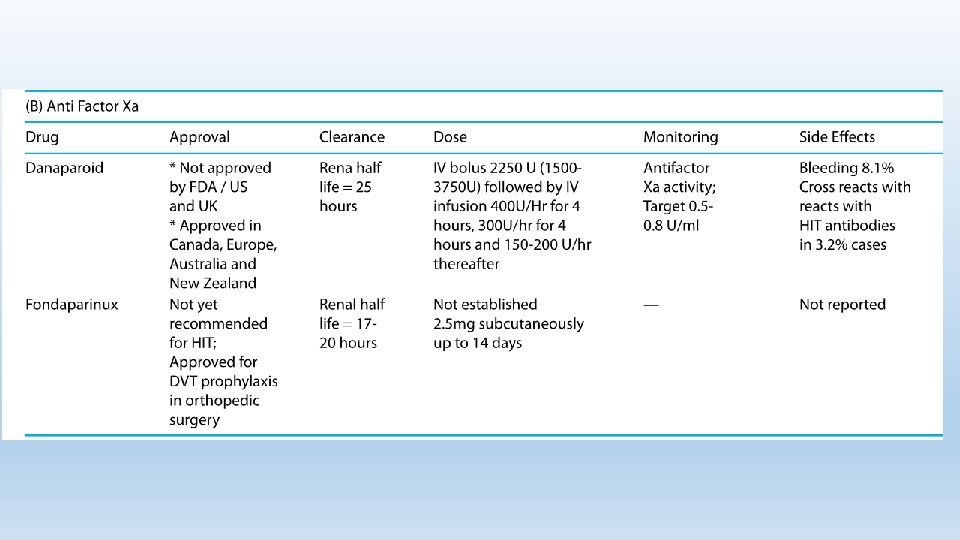

Several novel oral anticoagulants exist (eg, rivaroxaban, dabigatran, apixaban), and preliminary evidence suggests that they may be beneficial for HIT, particularly in cases refractory to standard therapies.

Rivaroxaban, sold under the brand name Xarelto It is the first available active direct factor Xa inhibitor which is taken by mouth. The maximum inhibition of factor Xa occurs four hours after a dose. The effects last approximately 8– 12 hours, but factor Xa activity does not return to normal within 24 hours, so once-daily dosing is possible. Rivaroxaban inhibits both free Factor Xa and Factor Xa bound in the prothrombinase complex.
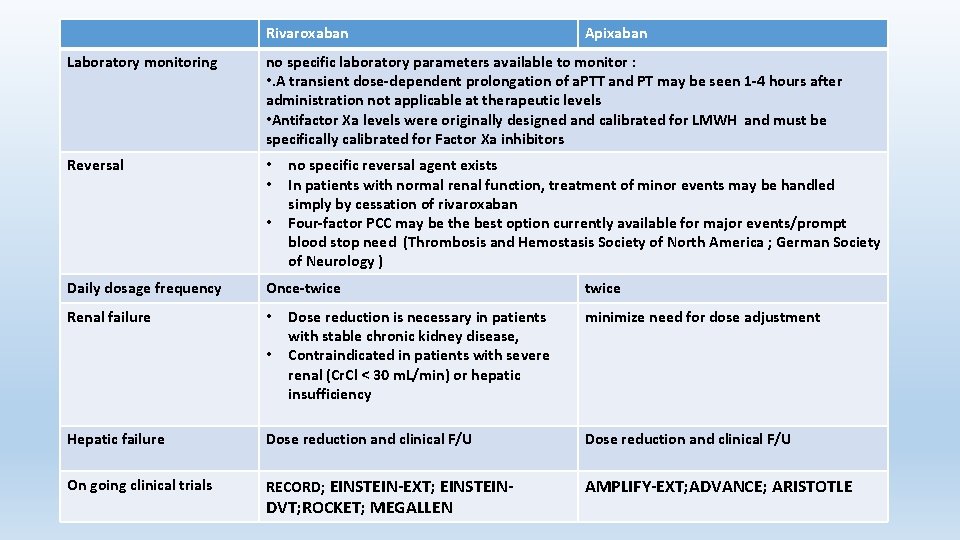
Rivaroxaban Apixaban Laboratory monitoring no specific laboratory parameters available to monitor : • . A transient dose-dependent prolongation of a. PTT and PT may be seen 1 -4 hours after administration not applicable at therapeutic levels • Antifactor Xa levels were originally designed and calibrated for LMWH and must be specifically calibrated for Factor Xa inhibitors Reversal • • • no specific reversal agent exists In patients with normal renal function, treatment of minor events may be handled simply by cessation of rivaroxaban Four-factor PCC may be the best option currently available for major events/prompt blood stop need (Thrombosis and Hemostasis Society of North America ; German Society of Neurology ) Daily dosage frequency Once-twice Renal failure • • Dose reduction is necessary in patients with stable chronic kidney disease, Contraindicated in patients with severe renal (Cr. Cl < 30 m. L/min) or hepatic insufficiency twice minimize need for dose adjustment Hepatic failure Dose reduction and clinical F/U On going clinical trials RECORD; EINSTEIN-EXT; EINSTEIN- AMPLIFY-EXT; ADVANCE; ARISTOTLE DVT; ROCKET; MEGALLEN

PLASMAPHERESIS in a randomized controlled study performed in 1999, Robinson et al. showed decreased mortality in HIT patients when treated within 4 days of the onset of thrombocytopenia.



• CBC WBC: 9200 N: 72% EOS: 1% PT: 14 INR: 1. 2 PTT: 33 FDP: pos D dimer : pos Fibrinogene: decreased HGB: 13. 3 PLT: 194000


- Slides: 52