Cauda Equina Syndrome Toby Bateson Mark Jadav Royal

Cauda Equina Syndrome Toby Bateson Mark Jadav Royal Cornwall Hospital ED June 2019


Medico-legal �Research by MPS in 2016 found that failure or delay in diagnosis of cauda equina syndrome was one of the top five errors that led to the most expensive GP claims. �From 2013 to 2017 MPS received 105 claims involving cauda equina syndrome – most of these arising from primary care. �How do we prevent these from

Cauda Equina Syndrome �Patient story / Definition / Red Flags �Pathology / Anatomy �Pathways of care �Pitfalls

Patient Story – in ED �Middle-aged male, skilled tradesman � 5 week history of low back / left buttock pain since RTC � 3 days worse “cramping, dull” pain radiating down left leg & foot is now numb �Normal bowel & bladder function �O/Ex normal tone / coordn / reflexes �Left knee extension power 4/5 �Left L 2 reduced sensn, reduced JPS right great toe

Patient Story – next 24 h �Diagnosed with sciatica & advised about “red flag symptoms” �Home �Next day numbness from left buttock to foot & unable to walk due to pain. �Called GP – arranged ambulance to attend but paramedics spoke to someone in ED & thought no use in returning to hospital without GP referral : arranged for GP to call back. �Episode of urinary incontinence – called 999: taken to ED.

Patient Story – in ED again �In ED seen by FY 2 23: 40 – sensation altered in both buttocks and up to T 9(? ) level on left. Anaesthetic perineum & reduced anal tone. �Urinary incontinence without sensation �d/w Locum registrar – MRI in morning

Patient Story – next day �Constant urinary incontinence overnight �s/b consultant 9 am – left sensory loss L 1 to S 4, weak hip flexion & knee extension, absent ankle / foot movements. �MRI scan 10: 45 – results viewed 13: 20 – urgent transfer to spinal centre – arrived 5 pm �Operation 21: 20

Patient Story – outcome �Poor ◦ ◦ outcome: Urinary, bowel & sexual dysfunction Left foot drop Limited mobility, sunsequent fall & #NOF Unable to work

Definitions Cauda Equina Syndrome – a collection of symptoms and signs related to sacral nerve root innervation. � Must include ◦ bladder, bowel or sexual dysfunction � and/or ◦ sensory dysfunction in the perianal / “saddle” region. � May include ◦ back pain with or without sciatica, ◦ lower limb weakness or sensory deficit, ◦ diminished or absent lower limb reflexes. Cauda Equina Compression – proven compression of the nerves leading to Cauda Equina Syndrome.

Definitions CES-Incomplete � urinary difficulties of neurogenic origin including ◦ ◦ � altered urinary sensation, loss of desire to void, poor urinary stream and the need to strain in order to micturate [16]. Saddle and genital sensory deficit is often unilateral or partial and trigone sensation (need to micturate on catheter pull) should be present. CES-Retention (Complete) � painless urinary retention and � overflow incontinence � There is usually extensive or complete saddle and genital sensory deficit with deficient trigone sensation. CES-Incomplete is more likely reversible so try to treat as emergency at this stage

Red Flags (NICE) LEGS: Bilateral sciatica � Severe or progressive bilateral neurological deficit of the legs, such as major motor weakness with knee extension, ankle eversion, or foot dorsiflexion. � PERINEUM: � Perianal, perineal or genital sensory loss (saddle anaesthesia or paraesthesia). SPHINCTERS: Difficulty initiating micturition or impaired sensation of urinary flow, if untreated this may lead to irreversible… ◦ Urinary retention with overflow urinary incontinence � Loss of sensation of rectal fullness, if untreated this may lead to irreversible… ◦ Faecal incontinence � Laxity of the anal sphincter. �
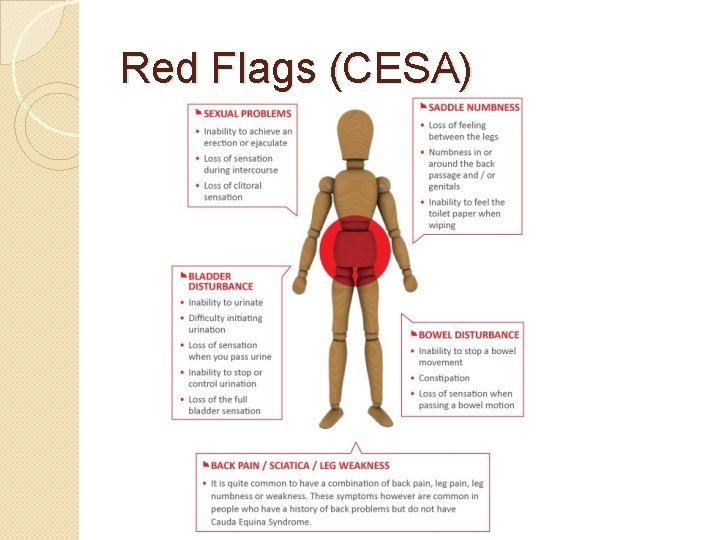
Red Flags (CESA)

Other vital differential diagnoses �Spinal Fracture �Cancer �Infection �Haematoma (from epidural / trauma)
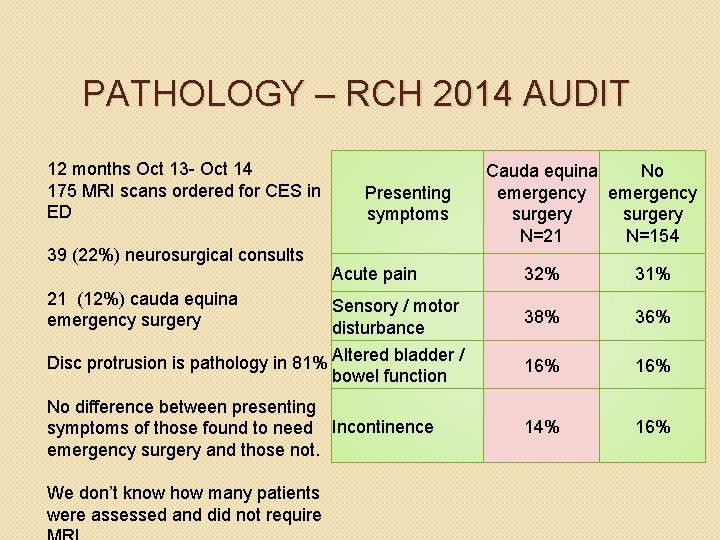

PATHOLOGY – RCH 2014 AUDIT 12 months Oct 13 - Oct 14 175 MRI scans ordered for CES in ED 39 (22%) neurosurgical consults Presenting symptoms Acute pain 21 (12%) cauda equina emergency surgery Sensory / motor disturbance Disc protrusion is pathology in 81% Altered bladder / bowel function No difference between presenting symptoms of those found to need Incontinence emergency surgery and those not. We don’t know how many patients were assessed and did not require Cauda equina No emergency surgery N=21 N=154 32% 31% 38% 36% 16% 14% 16%

PATHOLOGY – RCH 2014 AUDIT 12 months Oct 13 - Oct 14 175 MRI scans ordered for CES in ED 39 (22%) neurosurgical consults 21 (12%) cauda equina emergency surgery Disc protrusion is pathology in 81% No difference between presenting symptoms of those found to need emergency surgery and those not. We don’t know how many patients were assessed and did not require
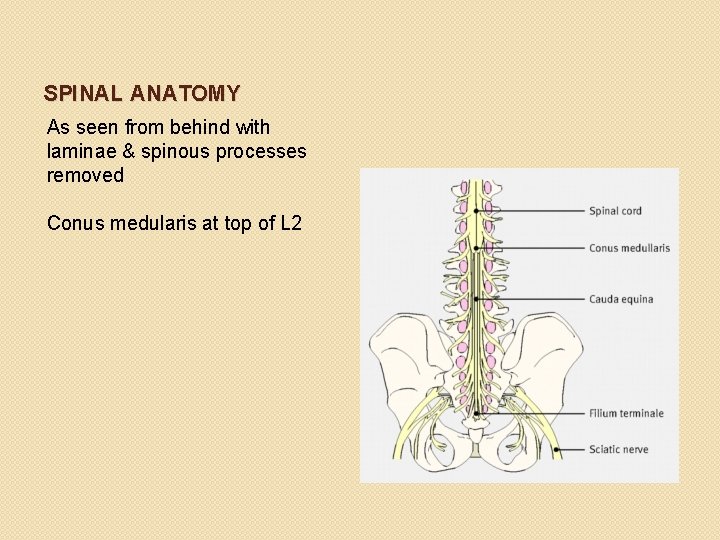
SPINAL ANATOMY As seen from behind with laminae & spinous processes removed Conus medularis at top of L 2
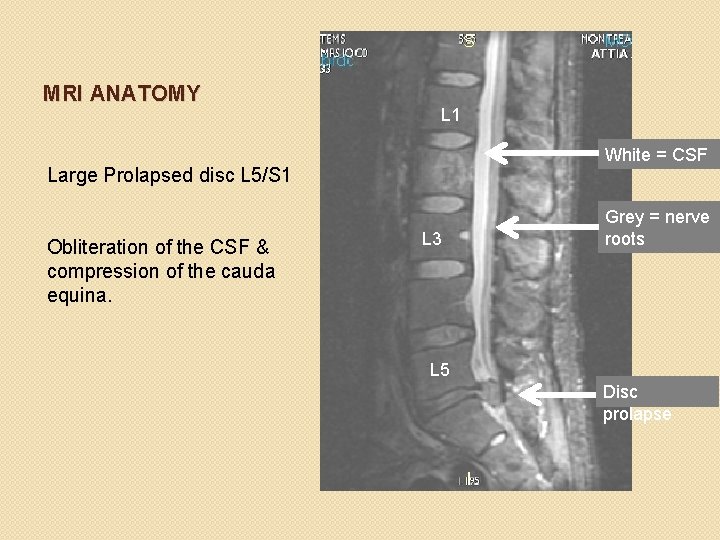
MRI ANATOMY L 1 White = CSF Large Prolapsed disc L 5/S 1 Obliteration of the CSF & compression of the cauda equina. L 3 Grey = nerve roots L 5 Disc prolapse
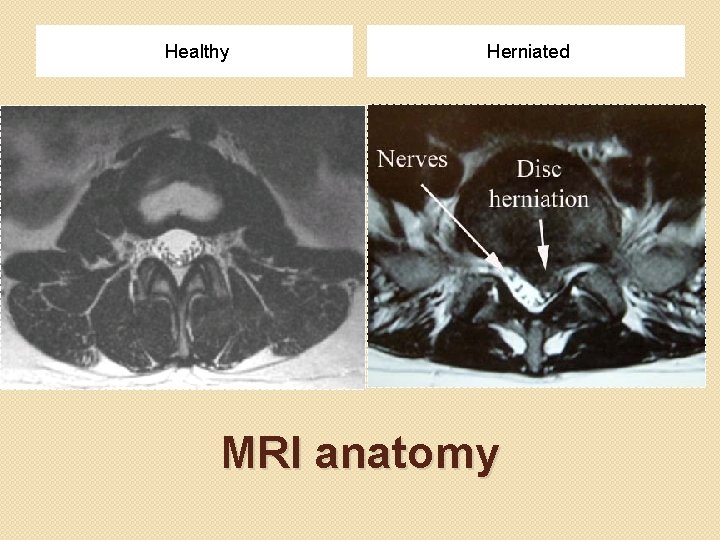
Healthy Herniated MRI anatomy
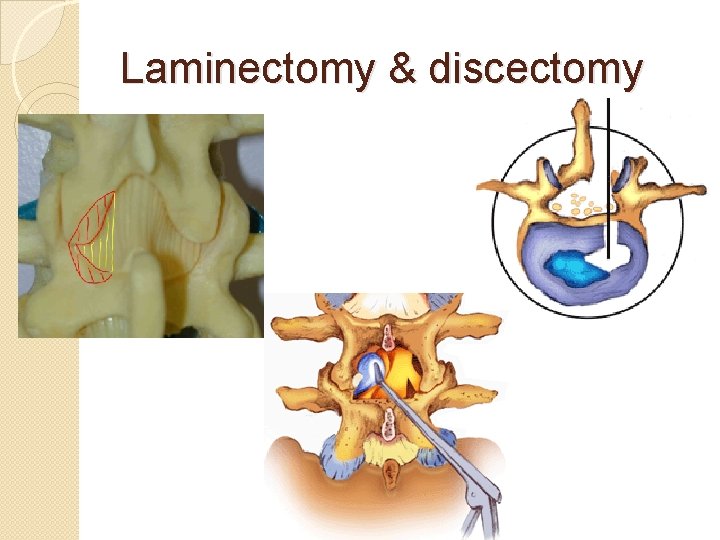
Laminectomy & discectomy
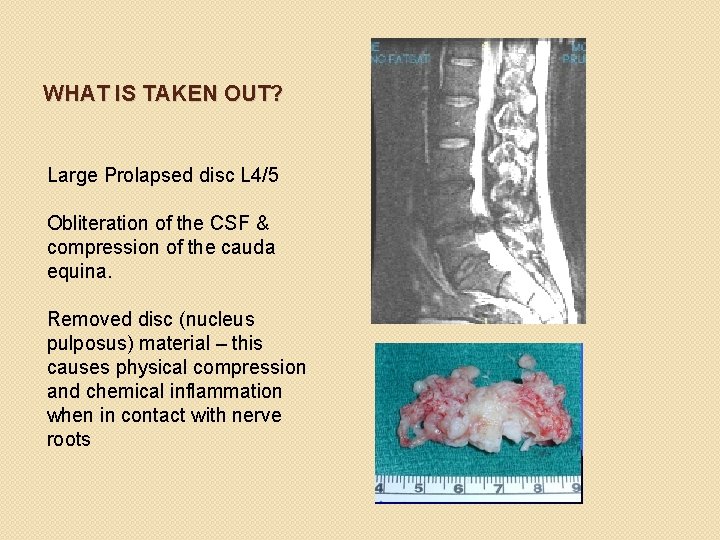
WHAT IS TAKEN OUT? Large Prolapsed disc L 4/5 Obliteration of the CSF & compression of the cauda equina. Removed disc (nucleus pulposus) material – this causes physical compression and chemical inflammation when in contact with nerve roots

Pathways �Assessment �Investigation �Neurosurgical Referral

Pathways - Assessment should be : �Full – ◦ history covering all red flags ◦ Examination all dermatomes / myotomes �Focussed ◦ History must ask the right questions ◦ Examination should be standardised, quick and reproducible

Pathways - Assessment �History ◦ Try to get accurate timelines ◦ Always ask about changes in urinary, bowel & sexual function ◦ If the patient uses “sciatica” ask them to explain �Examination ◦ Sensation - dermatomes (is it normal, is it the same? ) ◦ Power – myotomes (one movement each) ◦ Reflexes & voluntary anal contraction ◦ ASIA chart – standardised, quick & reproducible

ASIA Chart

Pathways -Investigation If meets the criteria for CES then needs emergency investigation & transfer if compression proven �MRI at RCH runs 8 am-8 pm: try to get the patient here before they close �Telephone ahead to ED consultant �Book the MRI & ask the radiologist to ring ED with the result

Pathways -Investigation Out of hours: �Discuss with neurosurgical registrar at Derriford: do they agree that this is an emergency presentation? Document the discussion carefully. �If needs emergency scan then will need to be sent to Derriford ED. Explain to the patient that they will be sent back if not requiring surgery.

Pathways - referral �All referrals now need to be made online www. referapatient. org �Emergency referrals should be followed up with a telephone call �Transport for emergencies is “Time. Critical Transfer” i. e. “blue light”

Pitfalls �If discharging with back pain / sciatica give written advice about cauda equina syndrome �“CES-Incomplete” has the better prognosis so this is the true emergency situation �Most patients we see have vague symptoms, unclear onset times, slow progression, no hard neurology: we often investigate them within 24 h rather than immediately BUT run the risk of missing CES-

Pitfalls �Urinary incontinence can be caused by pain and/ or constipation. �Documentation of “no red flags” is not enough – need to list them.

�So what diagnosis should in hindsight be given to our case study at each stage? �Choose from: ◦ Back pain / Sciatica without Red Flags ◦ CES-Incomplete ◦ CES-Retention

Acute low back pain with unilateral Patient Story – in ED sciatica and minor weakness �Middle-aged male, skilled tradesman � 5 week history of low back / left buttock pain since RTC � 3 days worse “cramping, dull” pain radiating down left leg & foot is now numb �Normal bowel & bladder function �O/Ex normal tone / coordn / reflexes �Left knee extension power 4/5 �Left L 2 reduced sensn, reduced JPS right great toe

Once incontinent: CES-Incomplete Patient Story – next 24 h (at least) �Diagnosed with sciatica & advised about “red flag symptoms” �Home �Next day numbness from left buttock to foot & unable to walk due to pain. �Called GP – arranged ambulance to attend but paramedics spoke to someone in ED & thought no use in returning to hospital without GP referral : arranged for GP to call back. �Episode of urinary incontinence – called 999: taken to ED.

Patient Story –CES-Retention? in ED again CES-Incomplete? �In ED seen by FY 2 23: 40 – sensation altered in both buttocks and up to T 9 level on left. Anaesthetic perineum & reduced anal tone. �Urinary incontinence without sensation �d/w Locum registrar – MRI in morning

Patient Story – in ED again Definite CES-Retention �Constant urinary incontinence overnight �s/b consultant 9 am – left sensory loss L 1 to S 4, weak hip flexion & knee extension, absent ankle / foot movements. �MRI scan 10: 45 – results viewed 13: 20 – urgent transfer to spinal centre – arrived 5 pm �Operation 21: 20

Questions ?

Summary � Definitions & Red Flags – understand them & have a ready reference � History & Examination ◦ correct wording ◦ ASIA charts ◦ documentation � MRI urgency – lots of chances to incur delay � Referral & Transfer
- Slides: 37