Case Study Adenocarcinoma Catalina Esqueda BS Dietetic Intern

Case Study Adenocarcinoma Catalina Esqueda, BS Dietetic Intern Ball State University

Main Points ▪ ▪ ▪ 2 Introduce the Problem History of the Patient Nutrition Assessment Nutrition Diagnosis Nutrition Interventions Monitoring and Evaluation

Introduction to the Problem 3

Introduction to the Problem ▪ 2016: 1, 685, 210 new cancer diagnoses. 1 ▪ Abnormal cells with uncontrolled growth. ▪ Malignant cancers invade other areas of the body. 4

Cancer Classification ▪ Primary site ▪ Histology ▫ ▫ ▫ 5 Carcinoma Sarcoma Myeloma Leukemia Lymphoma.
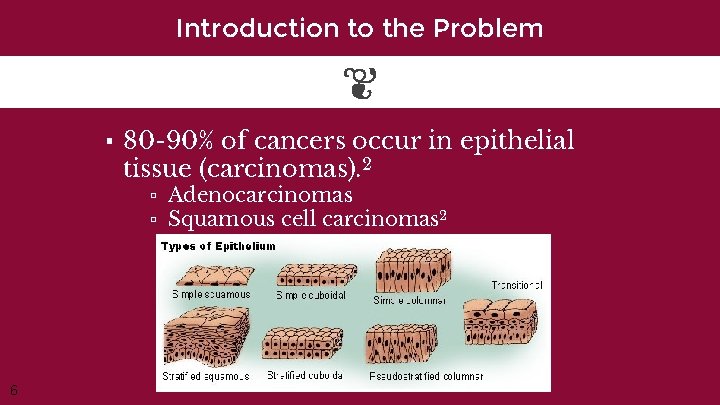
Introduction to the Problem ▪ 80 -90% of cancers occur in epithelial tissue (carcinomas). 2 ▫ Adenocarcinomas ▫ Squamous cell carcinomas 2 6

Introduction to the Problem ▪ Good nutritional status is critical. ▫ Helps patients complete treatment regimens with fewer interruptions. ▪ According to EAL, poor nutrition status associated with: ▫ Higher rates of readmission. ▫ Increased LOS. ▫ Greater mortality in oncology patients. 4 7 ▪ Increased risk: anorexia, weight loss, malnutrition.

Introduction to the Problem ▪ Nutrition support is not uncommon in cancer patients. ▪ Enteral nutrition is usually preferred, in part due to its ability to maintain the integrity of the GI tract, but contraindicated: ▫ Distal mechanical bowel obstruction. ▫ Short bowel syndrome. ▫ High output fistulas. 2 8

Introduction to the Problem ▪ Adenocarcinomas can occur together with neuroendocrine cells. 5 ▪ Some adenocarcinomas with neuroendocrine differentiation have been linked with a poor prognosis. 7, 8 9

Introduction of the Subject 10

Introduction to the Subject ▪ 70 year-old female ▪ Initially admitted for a bowel obstruction. ▪ C/O GI issues at admission, but otherwise normal state of health. 11

Introduction to the Subject ▪ 3 days before admission: ▫ Abdominal cramps/pain ▫ No bowel movements ▫ No gas ▪ Reported weight loss of 30 -35 pounds over six months. ▪ Admission: ▫ Palpable stool in colon. ▫ No bowel sounds. 12

Introduction to the Subject ▪ Patient had a low appetite throughout admission d/t pain. ▪ Did not like any supplements (Ensure, Magic Cup); said she might try Ensure Clear). ▪ Did not want a feeding tube. 13
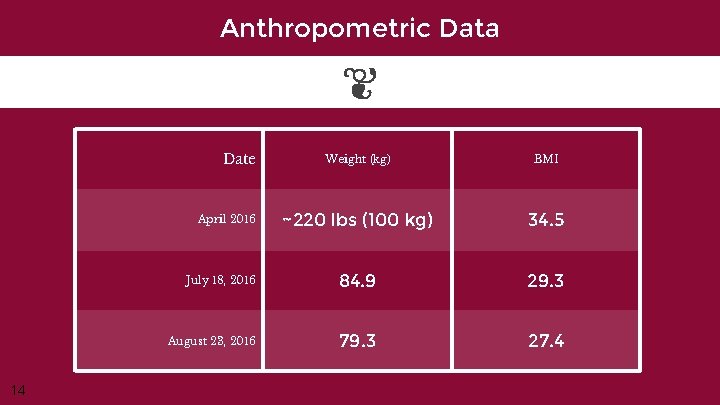
Anthropometric Data Date Weight (kg) BMI ~220 lbs (100 kg) 34. 5 July 18, 2016 84. 9 29. 3 August 23, 2016 79. 3 27. 4 April 2016 14

Introduction to the Subjects ▪ Nutrition needs: ▫ 1, 512 -1, 814 kcal/day (REE x SF 1. 2 postop) ▫ 96 -144 g/day of protein (1 -1. 5 g/kg postop) ▫ 2, 877 ml/day of fluids. 15

Patient History 16

Patient History ▪ ▪ ▪ Neuropathy Chronic edema of lower extremities Hypothyroidism Arthritis GERD Family History ▫ Mother had at least six operations d/t cancerous lesions. 17
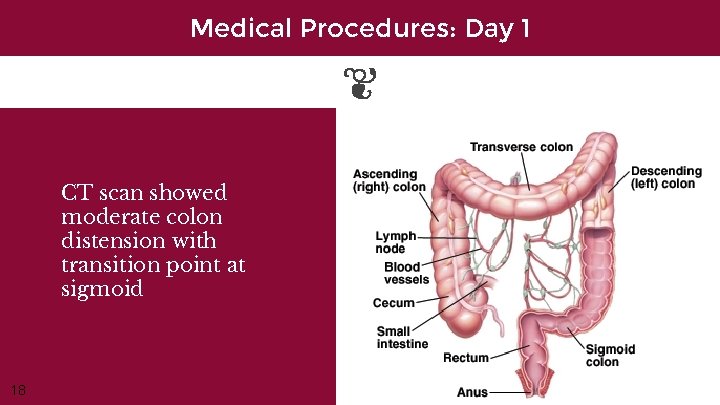
Medical Procedures: Day 1 CT scan showed moderate colon distension with transition point at sigmoid 18

Medical Procedures: Day 1 ▪ ▪ 19 Colonic diverticulosis Hiatal hernia Gallstones Barium enema unable to go past sigmoid.
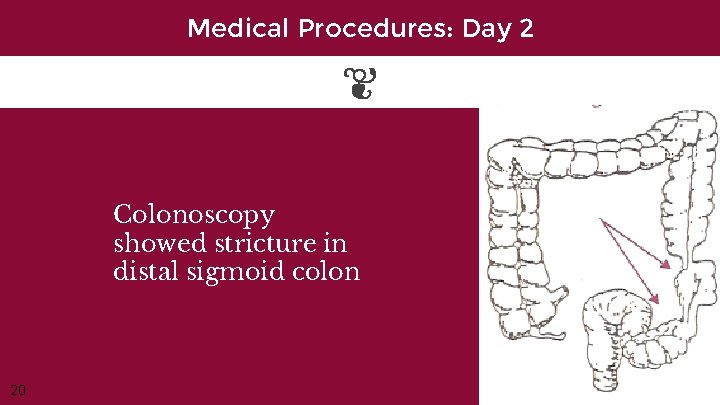
Medical Procedures: Day 2 Colonoscopy showed stricture in distal sigmoid colon 20

Medical Procedures: Day 2 ▪ Exploratory laparotomy ▫ Colonic mass ▫ Hard fibrotic uterine mass ▫ Right hydroureter ▪ Colonic mass = poorly differentiated adenocarcinoma with unclear primary location. 21
Medical Procedures: Day 2 ▪ Surgery ▫ Total abdominal hysterectomy with bilateral salpingo-oophorectomy ▫ Bilateral iliac node dissection ▫ Sigmoid colectomy ▫ Colostomy ▫ Peritoneal biopsy 22

Medical Procedures: Day 8 ▪ Infection of the abdominal wall below the ostomy. ▪ Ostomy retracted ▫ Stool leaked into soft tissue. ▫ Surgery for ostomy revision. ▫ NPO 23

Medical Procedures: Day 12 ▪ Transferred to oncology ▫ Adenocarcinoma was involved sigmoid colon, bilateral ovaries, uterus, cervix, and peritoneum. ▫ Gross disease resected, but likely still had residual microscopic disease in abdomen and pelvis. Origin unknown, but aggressive stage. Recommended chemotherapy. 24
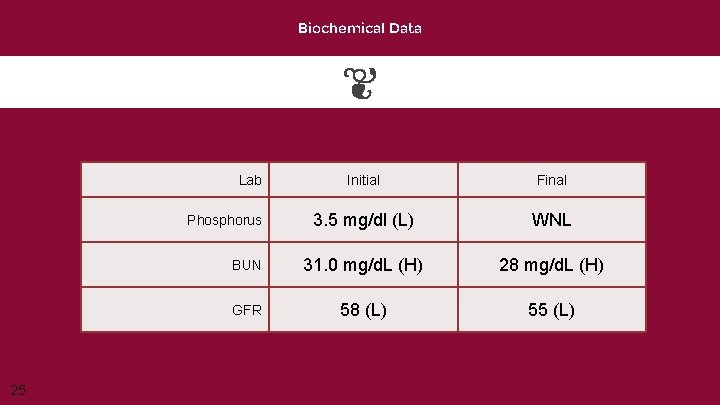
Biochemical Data Lab Initial Final 3. 5 mg/dl (L) WNL BUN 31. 0 mg/d. L (H) 28 mg/d. L (H) GFR 58 (L) 55 (L) Phosphorus 25
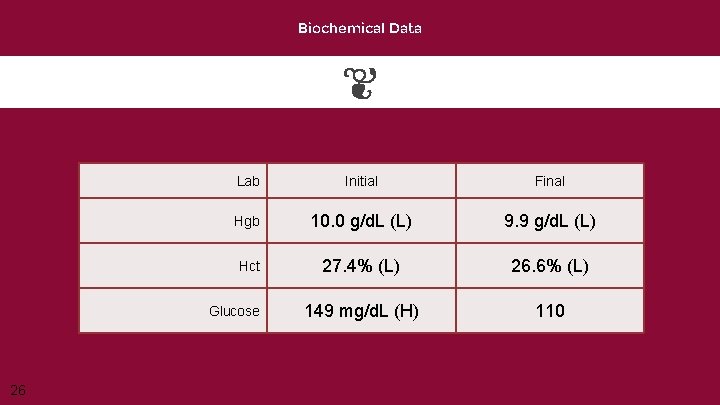
Biochemical Data Lab Initial Final Hgb 10. 0 g/d. L (L) 9. 9 g/d. L (L) Hct 27. 4% (L) 26. 6% (L) 149 mg/d. L (H) 110 Glucose 26

Nutrition Diagnosis and PES Statement 27

Nutrition Diagnosis and PES Statement ▪ Inadequate energy intake r/t decreased ability to consume sufficient energy as evidenced by NPO/CL diet >5 days this admission. ▪ Day 19: Inadequate energy intake r/t decreased appetite d/t pain as evidenced by >7 days poor PO intake <50% nutrition needs. 28

Nutrition Diagnosis and PES Statement ▪ Day 24: Malnutrition r/t chronic illness as evidenced by PO intake providing <75% of estimated needs for >1 month, 9% weight loss in previous 3 months & moderate muscle and subcutaneous fat loss. Meets criteria for moderate protein calorie malnutrition. 29

Interventions 30

Interventions ▪ Started on a clear liquid diet. ▪ Goal: Advance to full liquid diet. ▪ Medical Food Supplement: Ensure Clear BID. ▪ Vitamins & Minerals: Daily MVI. ▪ Enteral Nutrition: Vital AF 1. 2 Cal, goal rate 60 ml/hr. TPN if enteral nutrition contraindicated. 31

Interventions: Day 7 ▪ Put on a full liquid diet, with Ensure TID. ▪ Meals and Snacks: Advance to regular house diet as able. Encourage intake x 3 meals/day and snacks. ▪ Medical Food Supplement: Continue Ensure Clear TID. ▪ Day 8: NPO for ostomy revision. 32

Interventions: Day 13 ▪ Regular diet ▪ Appetite improved ▫ Patient was eating ~75% of meals 3 x/day 33

Interventions: Day 16 ▪ Regular diet with Ensure Clear TID ▫ Just bites of food and refusing meals for the past ~2 days. 34

Interventions: Day 19 ▪ Regular diet with Ensure Plus TID. ▫ 0 -50% of food and 25 -50% of supplements. ▪ Recommended also adding Magic Cup. 35

Interventions: Day 21 ▪ Medical Food Supplements: ▫ ▫ 36 Two smoothies with Unjury Two Magic Cups Ensure Plus Patient eating most of the supplements

Interventions: Day 24 ▪ ▪ NPO day 22 for surgical debridement Still NPO on day 24 Developed small bowel fistula TPN with 1680 ml Clinimix 5/15% sol’n + 250 ml 20% lipids, providing: ▫ 1693 calories (95 -115% estimated needs) ▫ 84 g protein (61 -91% estimated needs) 37

Interventions: Day 32 ▪ No ongoing fistula identified. ▪ Back on clear liquid diet, TPN decreased to 840 ml with 250 ml of 20% lipids. ▫ 1096 kcal, 42 g protein. ▪ Medical Food Supplement: Recommend three scoops of Unjury daily. ▪ Patient was eating 100% of meals and 50% of medical food supplement drinks. 38

Interventions: Day 36 ▪ Bowel fistula still present. ▪ Patient NPO again, expected to last ~3 weeks. ▪ Recommended increasing TPN ▫ Placed on 1, 440 ml. ▫ 1, 522 kcal, 72 g protein. ▪ Discharged on day 38 to long-term care. 39

Proposed Outcomes to Monitor/Evaluate 40

Proposed Outcomes to Monitor/Evaluate Food Intake: >75% intake 3 x/day. Energy/Protein Intake: >75% of needs met. Supplement Intake: Goal of 100% intake. Nutrition-Focused Physical Exam: Overall appearance ▪ Anthropometric Measurements: Weight changes. ▪ ▪ 41

Conclusion 42

Conclusion ▪ Patient was admitted with bowel obstruction. ▪ Discovery of adenocarcinoma and uterine mass. ▪ Multiple abdominal surgeries. ▪ Colostomy and colostomy revision. ▪ Post-op complication: fistula. 43

Conclusion ▪ Reports show improvements in mortality and fistula volume in patients receiving TPN. ▪ TPN should reach goal rate in 1 -2 days. ▪ Recommendation to transition to continuous postpyloric enteral nutrition over 4 -5 days. ▫ Caution with high-output fistulas. 12 44

Thanks! Any questions? 45

References 46

References 1. Cancer Facts & Figures 2016 | American Cancer Society. http: //www. cancer. org/research/cancerfactsstatistics/cancerfactsfigures 2016/. Accessed September 3, 2016. 2. Oncology General Guidance - Nutrition Care Manual. https: //www. nutritioncaremanual. org/topic. cfm? ncm_category_id=1&ncm_toc_id=255467. Accessed September 3, 2016. 3. Adenocarcinoma - Cancer Types & Treatment Options | CTCA. http: //www. cancercenter. com/terms/adenocarcinoma/. Accessed September 3, 2016. 4. EAL. http: //www. andeal. org/template. cfm? template=guide_summary&key=4155&reset=true. Accessed September 3, 2016. 5. La Rosa S, Marando A, Sessa F, Capella C. Mixed adenoneuroendocrine carcinomas (MANECs) of the gastrointestinal tract: an update. Cancers. 2012; 4(1): 11 -30. 6. Neuroendocrine Tumors - Nutrition Care Manual. https: //www. nutritioncaremanual. org/topic. cfm? ncm_category_id=1&ncm_toc_id=145188. Accessed September 3, 2016. 47

References 48 7. Shinji S, Naito Z, Ishiwata T, et al. Neuroendocrine cell differentiation of poorly differentiated colorectal adenocarcinoma correlates with liver metastasis. Int J Oncol. 2006; 29(2): 357 -364. 8. Liu Y, Xu J, Jiao Y, et al. Neuroendocrine Differentiation Is a Prognostic Factor for Stage II Poorly Differentiated Colorectal Cancer. Bio. Med Res Int. 2014; 2014: e 789575. doi: 10. 1155/2014/789575. 9. Inflammatory Bowel Disease (Intestinal Problems of IBD) Symptoms, Treatment, Causes What are symptoms of intestinal strictures, and how are they diagnosed and treated? Medicine. Net. http: //www. medicinenet. com/inflammatory_bowel_disease_intestinal_problems/article. htm. Accessed September 4, 2016. 10. Hydronephrosis and Hydroureter: Background, Pathophysiology, Epidemiology. July 2016. http: //emedicine. medscape. com/article/436259 -overview. Accessed September 4, 2016. 11. pmhdev. Total Abdominal Hysterectomy with Bilateral Salpingo-Oophorectomy - National Library of Medicine. Pub. Med Health. http: //www. ncbi. nlm. nih. gov/pubmedhealth/PMHT 0022840/. Accessed September 4, 2016. 12. http: //www. ncbi. nlm. nih. gov/pmc/articles/PMC 2967313/
- Slides: 48