Case Study 9 Celiac Disease By Kaili Acosta

Case Study #9: Celiac Disease By: Kaili Acosta Joyce Moore Elizabeth Olivares Rosalinda Ruiz

Overview � Celiac Disease and Pathophysiology � Nutrition Therapy � Nutrition Assessment � Intake Domain � Clinical Domain � Nutrition Diagnosis � Nutrition Intervention � Monitoring and Evaluation
Panel Rules � Directions 2 teams - panel style � First group to raise hand will be given 30 seconds to deliberate the answer and choose a spokesperson for each question (rotating spokesperson) (both groups will deliberate answer and spokesperson in case of incorrect answer made by other team) � If first team answers incorrectly question will fall to other panel and answer immediately � One point per question � No minus points � Panel with highest points wins!!!

Patient Information � Patient � DOB: name: � Age: � Sex: � Ethnicity: � Height: � Weight: � Referring � Chief MD: Melissa Gaines 3/14 36 female Caucasian 5’ 3” 92# Roger Smith, M. D. , gastroenterologist complaints: Weight loss, diarrhea, lack of energy

Patient History � Delivered a healthy baby boy (5 lb. 2 oz. ) � Gained weight during pregnancy (11 lbs. ) �Greatest pre-pregnancy weight: 112# �Current weight: 92# � Diarrhea on and off for most of her adult life ◦ Mother and grandmother also had diarrhea

What is Celiac Disease? Abnormal immune response to the consumption of gluten Etiology and Immune response: Gliadin component of gluten triggers inflammatory response Presence of antibodies – autoimmune response Ig. A - anti-tissue transglutaminase AGA – antiendomysial antibodies EMA – antigliadin antibodies

Test Results � Endoscopy and Biopsy ◦ Flat mucosa with villus atrophy and hyperplastic crypts –inflammatory infiltrate in lamina propria ◦ Antibodies: Positive AGA, EMA � 72 -Hour � Results: Fecal Test ◦ Steatorrhea and malabsorption ◦ 11. 5 g fat/24 hours

Nutrition Assessment � BMI=16. 3 kg/m 2 � UBW= 112 # � %UBW=82 % � IBW=115# �% IBW= 80 % �% weight change = 18 % weight change in 2 months � Nutritional risks

Clinical Domain � Anthropometric ◦ TSK=7. 5 mm. measurements �She is under the 5 th percentile of TSF below average. ◦ MAC= 180 mm � AMA = [(18 cm/12. 56) x (3. 14 x 0. 75 cm)]2 � (1. 43 x 2. 35)2 = 3. 362 = 11. 4 cm 2 ◦ Interpretation �AFA: 14. 4 cm 2. ◦ She is between the 5 th and 10 th percentile which classifies her as below average fat.

Nutrition Assessment � Nutrient requirements: � Calculation: Mifflin-St. Jeor equation: � Activity Factor: (1. 2) � Injury Factor: (1. 2) � EEN = (10 x 52. 3 kg) + (6. 25 x 160. 0 cm) - (5 x 36) – 161 = 1182 x (1. 2) = 1418 (1. 2)=1843 = 1800 kcal /day � EPR: (IBW 1. 2 g/kg) � 52. 3 kg x 1. 2 g/kg = 62. 76 = 63 g/d

Intake Domain 24 -Hour Recall Evaluation
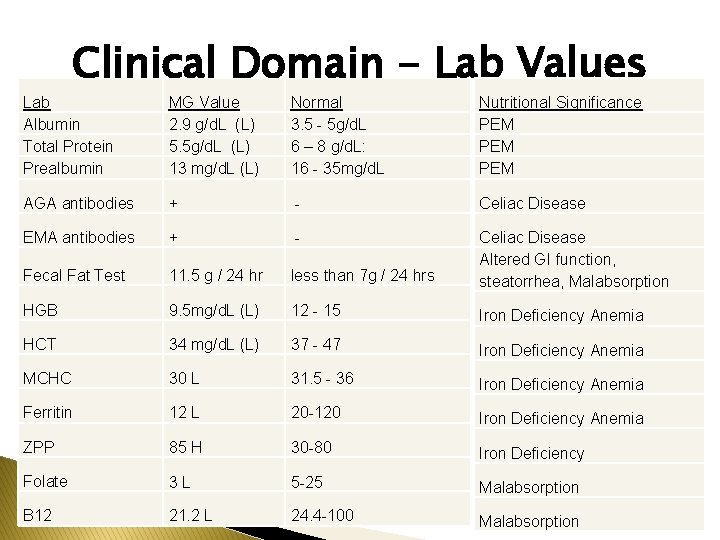
Clinical Domain - Lab Values Lab Albumin Total Protein Prealbumin MG Value 2. 9 g/d. L (L) 5. 5 g/d. L (L) 13 mg/d. L (L) Normal 3. 5 - 5 g/d. L 6 – 8 g/d. L: 16 - 35 mg/d. L Nutritional Significance PEM PEM AGA antibodies + - Celiac Disease EMA antibodies + - Fecal Fat Test 11. 5 g / 24 hr less than 7 g / 24 hrs Celiac Disease Altered GI function, steatorrhea, Malabsorption HGB 9. 5 mg/d. L (L) 12 - 15 Iron Deficiency Anemia HCT 34 mg/d. L (L) 37 - 47 Iron Deficiency Anemia MCHC 30 L 31. 5 - 36 Iron Deficiency Anemia Ferritin 12 L 20 -120 Iron Deficiency Anemia ZPP 85 H 30 -80 Iron Deficiency Folate 3 L 5 -25 Malabsorption B 12 21. 2 L 24. 4 -100 Malabsorption

Which lab values are related to consequences of Celiac disease?

Clinical Domain � Breastfeeding difficulty (NC-1. 3) � Altered GI function (NC-1. 4) � Impaired nutrient utilization (NC-2. 2) � Altered nutrition related lab values (NC-2. 2) � Underweight (NC-3. 1) � Involuntary weight loss (NC-3. 2)

Protein Energy Malnutrition (PEM) Patient meets criteria: Moderate Protein Energy Malnutrition (PEM) �Albumin 2. 9 g/d. L � 82 % of UBW

Intake Domain � Inadequate energy expenditure (NI-1. 4) � Inadequate oral food/beverage intake (NI-2. 1) � Inadequate fluid intake (NI-3. 1) � Inadequate mineral intake (sulfate, iron, Ca)(NI 5. 10. 1) � Inadequate vitamin intake (Folate)(NI-5. 9. 2) � Malnutrition (NI-5. 2) � Inadequate protein energy intake (NI-5. 3) � Inadequate fat intake (NI-5. 6. 1) � Inadequate protein intake (NI-5. 7. 1) � Inadequate carbohydrate intake (NI-5. 8. 1) � Inadequate fiber intake (NI-5. 8. 5)

PES Statements Inadequate oral and beverage intake (NI-2. 1) RT altered GI function and food- and nutrition-related knowledge deficit secondary to CD AEB 24 -hour recall reveals 440 kcals, consuming 24% EEN, BMI 16. 3 kg/m 2, 80 % IBW, 82 % UBW, 30# weight loss and 18% weight change past 2 months revealing severe weight loss. Altered GI function (NC-1. 4) RT intolerance to foods containing gluten AEB diarrhea, weight loss (30#) altered lab values: ferritin: 12 mg/ml. L (L), HGB: 9. 5 g/d. L (L), HCT: 34% (L), Alb: 2. 9 g/d. L (L), Total PRO: 5. 5 g/d. L (L), PAB: 13 mg/d. L (L), ZPP : 85 umol/mol(H), Folate: 3 ug/d. L(L), B 12: 21. 2 ng/d. L (L) and positive AGA and EMA.

Nutrition Therapy �Gluten-free �What diet is gluten? �Where can it be found? �Consumption of oats?

Nutrition Therapy � Other ◦ ◦ sources than food Food additives Coloring agents Modified food starch Medications � Lactose intolerance Damage to villi affects ability to absorb lactose

Nutrition Intervention � Diet to start out on: � High-protein � Glutamine � Length supplement recommended: supplementation: of stay on diet

Mrs. Gains at home

Monitoring and Evaluation � Follow-up � How can we modify Mrs. Gaines’ diet?

� � � � References Nelms, MN, Sucher, K, Long, S. Nutrition Therapy and Pathophysiology, 2 nd ed. Belmont, CA: Wadsworth/Thomas Learning; 2011. National Institutes of Health. What People With Celiac Disease Need to Know About Osteoporosis. NIH Osteoporosis and Related Bone Diseases ~ National Resource Center Web site. Available at: http: //www. niams. nih. gov/Health_Info/Bone/Osteoporosis/Conditions_Behaviors/celiac. asp. Published January 2012. Accessed February 28, 2013. Celiac-disease. Gluten Free Diet – Do You Eat Oats? Celiac-disease Web site. Available at: http: //celiacdisease. com/gluten-free-diet-do-you-eat-oats/. Accessed March 2, 2013. Serra S, Jani PA. An approach to duodenal biopsies. Journal of Clinical Pathology. 2006(11); 1133 -1150. Medline. Plus. National Institutes of Health. Available at: http: //www. nlm. nih. gov/medlineplus/ency/article/003588. htm. Accessed March 2, 2013. Fecal Fat. Lab Tests Online. Available at: http: //labtestsonline. org/understanding/analytes/fecal-fat/tab/test. Accessed on March 2, 2013. Mayo Clinic. Gluten-free diet: What's allowed, what's not. Mayo Clinic Website. Available at: http: //www. mayoclinic. com/health/gluten-free-diet/MY 01140. Accessed March 2, 2013. Thompson T. The celiac disease & lactose intolerant connection. Gluten Free Dietitian Website. Available at: http: //www. glutenfreedietitian. com/newsletter/dietcom-blog-the-celiac-disease-lactose-intolerant-connection/. Accessed March 2, 2013. Evidence Analysis Library. Academy of Nutrition and Dietetics. Eatright. org. Available at: http: //andevidencelibrary. com/topic. cfm? cat=3253. Accessed March 2, 2013. My. Plate. Super. Tracker. Myplate Website. Available at: https: //www. supertracker. usda. gov/Nutrients. Report. aspx. Accessed March 2, 2013. Improving patient outcomes with nutrition therapy. 2013 Abbott Nutrition Product Reference. International Dietetics & Nutrition Terminology (IDNT) Reference Manual, 4 th ed. eat right. Academy of Nutrition and Dietetics. Herzig L. Identifying Celiac Disease. Valley Health Magazine. 9: 12. Hlywiak K. . Hidden Sources of Gluten. Celiac Disease: a comprehensive review and update. Series #2. Available at: http: //www. practicalgastro. com/pdf/September 08/Hlywiak. Article. pdf. Accessed March 3, 2013. Escott-Stump S. Nutrition and Diagnosis Related Care. 7 th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2012.
- Slides: 23