Case Study 87 Systemic Lupus Erythematosus SLE By

Case Study #87: Systemic Lupus Erythematosus (SLE) By Albert Doyle

https: //www. youtube. com/watch? v=he. RWz 1 Qmu 4 Q Listen to his words and accent

Pathophysiology of Lupus Chronic, autoimmune disease that can affect literally any body system Rarely presents the same in any two lupus patients Disruption in apoptosis Immune system generates auto-antibodies › Antibodies clump together and can latch on to any body system. Attacking cells DNA surrounding the antibody.
No known cause No know treatment to cure the disease › Treatment is aimed at reducing symptoms and balancing the body’s immune system to a functional level › Genetic, epigenetic, hormonal, and other environmental factors associated with SLE
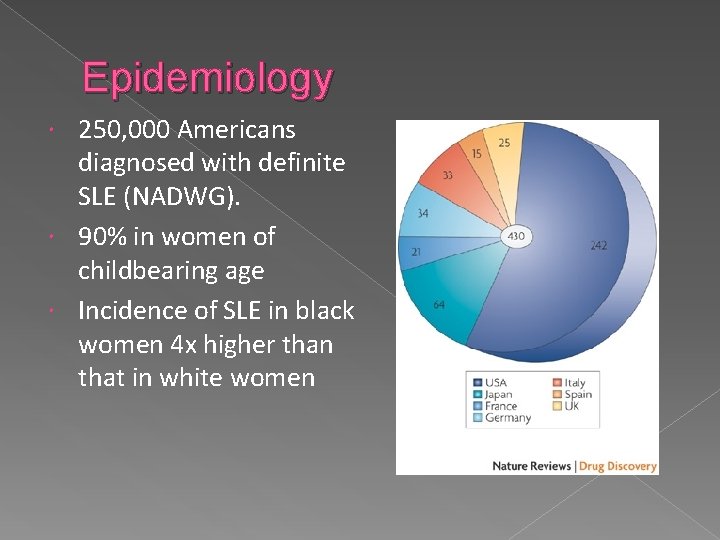
Epidemiology 250, 000 Americans diagnosed with definite SLE (NADWG). 90% in women of childbearing age Incidence of SLE in black women 4 x higher than that in white women
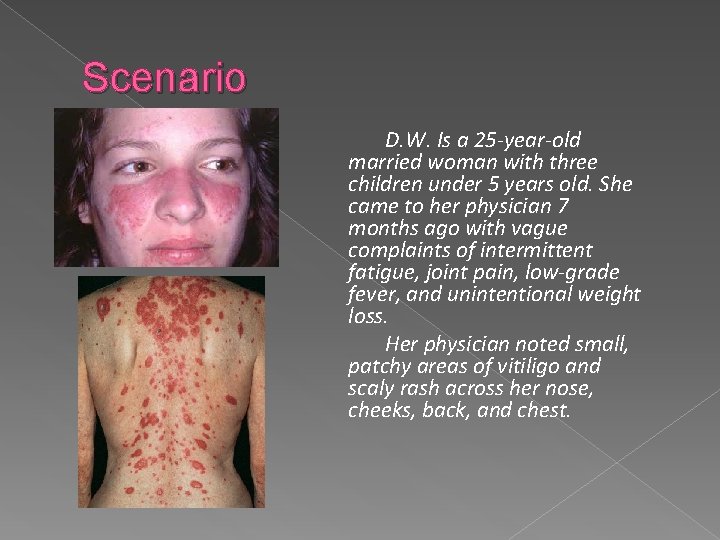
Scenario D. W. Is a 25 -year-old married woman with three children under 5 years old. She came to her physician 7 months ago with vague complaints of intermittent fatigue, joint pain, low-grade fever, and unintentional weight loss. Her physician noted small, patchy areas of vitiligo and scaly rash across her nose, cheeks, back, and chest.

D. W. ’s laboratory studies antinuclear antibody(ANA) revealed: Positive titer Positive ds. DNA(positive lupus erythematosus) Positive anti-Sm(anti-smooth muscle antibody) Elevated C-reactive protein(CRP) Elevated erythrocyte sedimentation rate (ESR) Decreased C 3 and C 4 serum complement

Joint x-ray films demonstrated joint swelling without joint erosion. D. W was subsequently diagnosed with systemic lupus erythematosus (SLE). She was initially treated with hydroxychloroquine (Plaquenil) 400 mg and Deltason (Prednisone) 20 mg PO qdaily, bed rest, and ice packs. › D. W responded well to treatment, the steroid was tapered and discontinued, and she was told she could report for follow-up every 6 months, unless her symptoms became acute. D. W. Resumed her job in environmental services at a large geriatric facility.

1)What is the significance of each of D. W. ’s laboratory findings? Positive antinuclear antibody (ANA) titer: › Auto-antibodies are in the immune system Positive ds. DNA (positive lupus erythematosus): › Auto-antibodies that target DNA › Highly specific Positive anti-SM (smooth muscle antibody): › Presence of antibodies against smooth muscle

Elevated C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) › Measure of inflammation in the body Decreased C 3 and C 4 serum complement › Shows impending or current “flare” of lupus symptoms
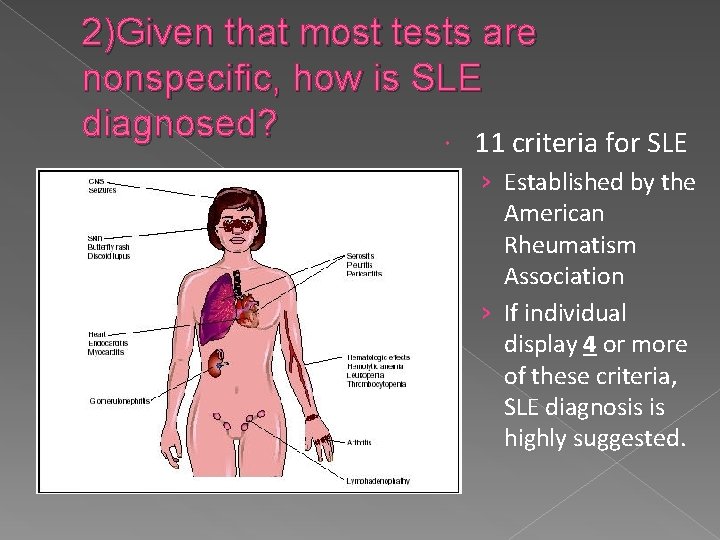
2)Given that most tests are nonspecific, how is SLE diagnosed? 11 criteria for SLE › Established by the American Rheumatism Association › If individual display 4 or more of these criteria, SLE diagnosis is highly suggested.

Malar- purplish/mildly scaly rash over the cheeks and nose Known as a “butterfly” rash › D. W. displays scaly rash over cheeks, nose, back and chest.
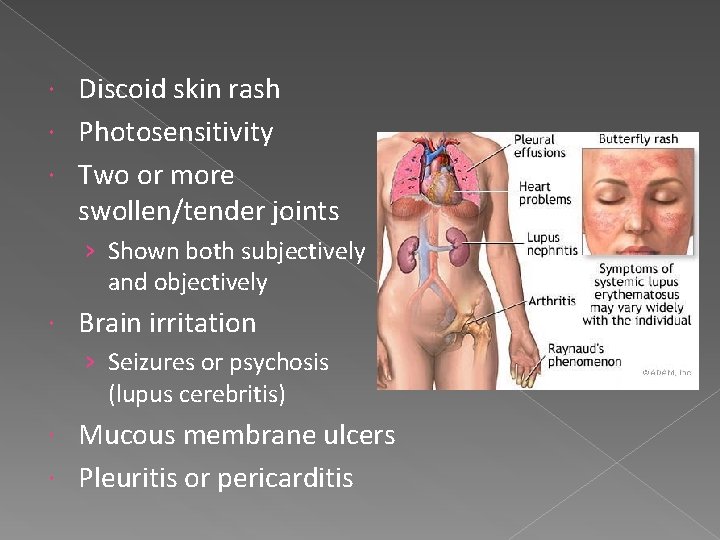
Discoid skin rash Photosensitivity Two or more swollen/tender joints › Shown both subjectively and objectively Brain irritation › Seizures or psychosis (lupus cerebritis) Mucous membrane ulcers Pleuritis or pericarditis
Low blood counts Kidney abnormalities › Proteinuria Tests: › ds. DNA, anti-Sm, ANA › ESR and CRP

3) What priority problems were addressed in D. W. ’s care plan at that time of diagnosis? Coping and understanding of dx Monitor pain and temp Medication administration and understanding Ways to live a normal and safe life dx. w/ SLE
Progress: Eighteen months after diagnosis, D. W. Seeks out her physician because of puffy hands and feet and increased fatigue. D. W. Reports that she has been working longer hours because of the absence of two of her fellow workers.
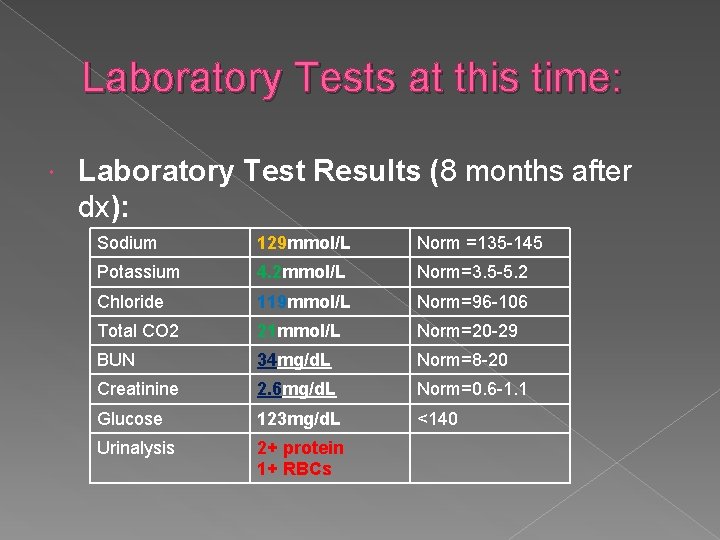
Laboratory Tests at this time: Laboratory Test Results (8 months after dx): Sodium 129 mmol/L Norm =135 -145 Potassium 4. 2 mmol/L Norm=3. 5 -5. 2 Chloride 119 mmol/L Norm=96 -106 Total CO 2 21 mmol/L Norm=20 -29 BUN 34 mg/d. L Norm=8 -20 Creatinine 2. 6 mg/d. L Norm=0. 6 -1. 1 Glucose 123 mg/d. L <140 Urinalysis 2+ protein 1+ RBCs

4) Which laboratory findings concern you, and why? Elevated BUN and Creatinine Proteinuria and hematuria Slightly elevated sodium and chloride

5) How will D. W. 's treatment and care plan likely change? Stabilize labs Decrease swelling and fatigue Medication adjustment Promote kidney function Decrease risk of infection

6) The physician orders cyclophosphamide (Cytoxan) 100 mg/m 2/day orally in two divided doses. D. W. Weighs 140 lbs and is 5 ft, 4 in tall. How much will she receive with each dose?

So what was that med? cyclophosphamide (Cytoxan) › Aklylating agent used for immunosuppressant therapy › Used for D. W. ’s worsening symptoms of SLE

Progress: D. W. Is seen in the immunology clinic twice monthly during the next 3 months. Although her condition does not worsen, her BUN and creatinine remain elevated. While at work one afternoon, D. W. Beings to feel dizzy and develops a severe headache. She reports to her supervisor, who has her lie down. When D. W. Starts to become disoriented, her supervisor calls 911, and D. W. Is taken to the hospital. D. W. Is admitted for probable lupus cerebritis related to acute exacerbation of her disease.

7) What other findings indicative of central nervous system (CNS) involvement from SLE should D. W. Be assessed for? Seizures Decreased LOC Slurred speech PERRLA A&O Muscle tone Symmetry

8) What preventive measures need to be instituted to protect D. W. At this time? Seizure precautions Infection control › Standard precautions › IV antibiotics Close monitoring Neurological assessments

9) While caring for D. W. , which of these care activities can be safely delegated to the NAP? (select all that apply): a: Measuring D. W. 's BP every 2 hrs b: Assisting D. W. With personal hygiene measures c: Counseling D. W. On seizure safety precautions d: Assessing D. W. 's neurological status every 2 hrs e: Emptying the urine collection device and measuring the output f: Monitoring D. W. 's BUN and creatinine levels A, b, e
Progress: The physician orders pulse therapy with methylprednisolone (Solu. Medrol) 125 mg IV every 6 hours and plasmapheresis once daily.
10) What major complications associated with immunosuppression therapy will D. W. Have to be monitored for? Increased risk of infection Change in VS N/V, bone marrow suppression, hair loss, lethargy
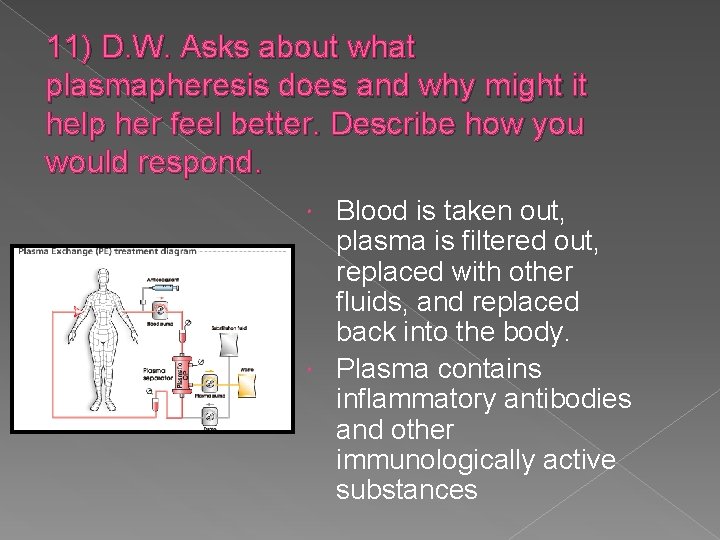
11) D. W. Asks about what plasmapheresis does and why might it help her feel better. Describe how you would respond. Blood is taken out, plasma is filtered out, replaced with other fluids, and replaced back into the body. Plasma contains inflammatory antibodies and other immunologically active substances

12) D. W. Returns to the floor following plasmapheresis. The NAP reports to you D. W. 's vital signs. BP=86/43, HR=108, RR=18, Temp=97. 2(36. 2) You go in to assess D. W. And find that she is complaining of a headache and some dizziness.

What do you immediately suspect is occurring? BP=86/43, HR=108, RR=18, Temp=97. 2(36. 2) › Hypotensive- from plasmapheresis › Dehydrated

13) What do you anticipate your care of D. W. Will include over the next 2 -3 hrs? Stabilizing BP Hydrating Decrease dizziness and headache Stabilize temp Assessing neurological signs and VS › Keeping doctor aware of any complications

14) What outcome criteria would support that D. W. 's condition is stabilizing? Stable VS A&O x 4 Decreased report of pain and swelling extremities Decrease in fatigue Decrease in inflammation Fight off infection

15) Identify at least five topics that D. W. must be taught before she is discharged that might help her lead as normal a life as possible. 1) 2) 3) 4) 5) Medication regimen Coping Proper hygiene Self-care with SLE and kidney complications When to notify health care provider

16) You note that D. W. 's husband is visiting her this afternoon. You enter the room to as whether they have any questions. D. W. 's husband states, “I have tried to tell her that she cannot go back to work. Sure, we need the money, but the kids and I need her more. I’m afraid that this lupus has weakened her whole body and it will kill her if she goes back to work. Is that right? ” How should you respond to his concerns?

Further Research: Main cause of SLE Treatments aimed at curing the disease rather than managing it › grasp further understanding for health care workers to take the best care possible for SLE patients

Citations: Ramachandran, R. R. , Sakhuja, V. V. , Jha, V. V. , Kohli, H. S. , & Rathi, M. M. (2012). Plasmapheresis in systemic lupus erythematosus with thrombotic microangiopathy. Internal Medicine Journal, 42(6), 734. doi: 10. 1111/j. 1445 -5994. 2012. 02810. x Robinson, M. , Sheets Cook, , . , & Currie, L. M. (2011). Systemic lupus erythematosus: A genetic review for advanced practice nurses. Journal Of The American Academy Of Nurse Practitioners, 23(12), 629 -637. doi: 10. 1111/j. 1745 -7599. 2011. 00675. x Ferenkeh-Koroma, A. (2012). Systemic lupus erythematosus: nurse and patient education. Nursing Standard, 26(39), 49 -57. Poole, J. L. , Hare, K. , Turner-Montez, S. , Mendelson, C. , & Skipper, B. (2014). Mothers With Chronic Disease: A Comparison of Parenting in Mothers With Systemic Sclerosis and Systemic Lupus Erythematosus. OTJR: Occupation, Participation & Health, 34(1), 1219. doi: 10. 3928/15394492 -20131029 -06 Christian Pagnoux, C. P. (2007). Plasma exchange for systemic lupus erythematosus. Transfusion and Apheresis Science , 187 -192. Retrieved from http: //vincentbourquin. files. wordpress. com/2009/12/pe-for-sle. pdf Kang, I. , & Park, S. H. (2003). Infectious complications in SLE after immunosuppressive t herapies. Current opinion in rheumatology, 5, 528– 534. Hari, P. , & Srivastava, R. N. Pulse corticosteroid therapy with methylprednisolone or dexamethasone. Indian journal of pediatrics, 4, 557– 560.
- Slides: 36