Case Presentation Vestibular Schwannoma VP shunt NCLIN 411

Case Presentation: Vestibular Schwannoma & VP shunt NCLIN 411 Summer 2020 Lilia Peng

Case History • 41 -year old Caucasian cis female (she/her) • Readmitted for VP shunt placement after development of CSF leak & pseudomeningocele after surgery to excise vestibular schwannoma • Nov. 2019 – Jan. 2020: dizziness, HA, decreased hearing on L side (muffled sound), tinnitus, numbness/heat sensation across L side of face, few days of tingling across L arm with some L shoulder weakness, intermittent trouble with balance • May 29 th: L suboccipital craniotomy to excise L vestibular schwannoma. Some brainstem compression & slight deviation of 4 th ventricle by tumor noted, but no hydrocephalus. • June 13 -14 th: Bulging & leakage noted CSF leak & pseudomeningocele • June 23 rd: Surgery to place VP shunt • Med hx: N/A, healthy • Social hx: PA, triathlete, no tobacco / marijuana use, social ETOH use • Meds/supplements prior to hospitalization: Wellbutrin, fish oil, Ambien
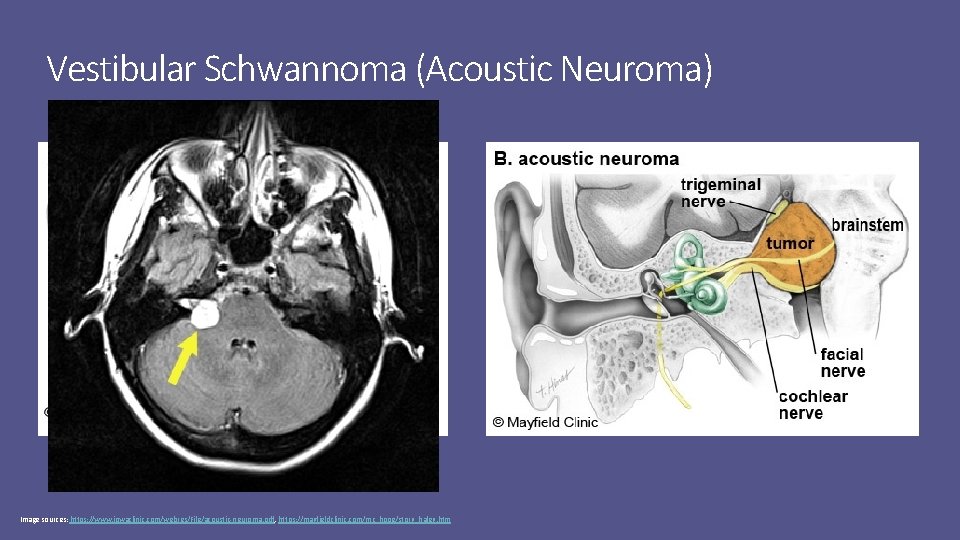
Vestibular Schwannoma (Acoustic Neuroma) Image sources: https: //www. iowaclinic. com/webres/File/acoustic-neuroma. pdf, https: //mayfieldclinic. com/mc_hope/story_haley. htm

Vestibular Schwannoma: Epidemiology & Risk Factors Epidemiology (Up. To. Date 2020) • Incidence in U. S. : 1 / 100, 000 • Taiwan: 2. 66 / 100, 000 and Asian Pacific Islanders: 1. 37 / 100, 000 • Hispanics: 0. 69 / 100, 000 and African Americans: 0. 36 / 100, 000 • Overall incidence increasing with incidental dx of asymptomatic tumors from MRI and CT • Median age at dx: 50 • Unilateral in >90% of cases (L & R affected equally) Risk factors (Up. To. Date 2020) • Neurofibromatosis type 2 (NF 2) – bilateral • Childhood exposure to low-dose radiation to head & neck • Cell phone use (controversial) • Noise exposure (conflicting data)
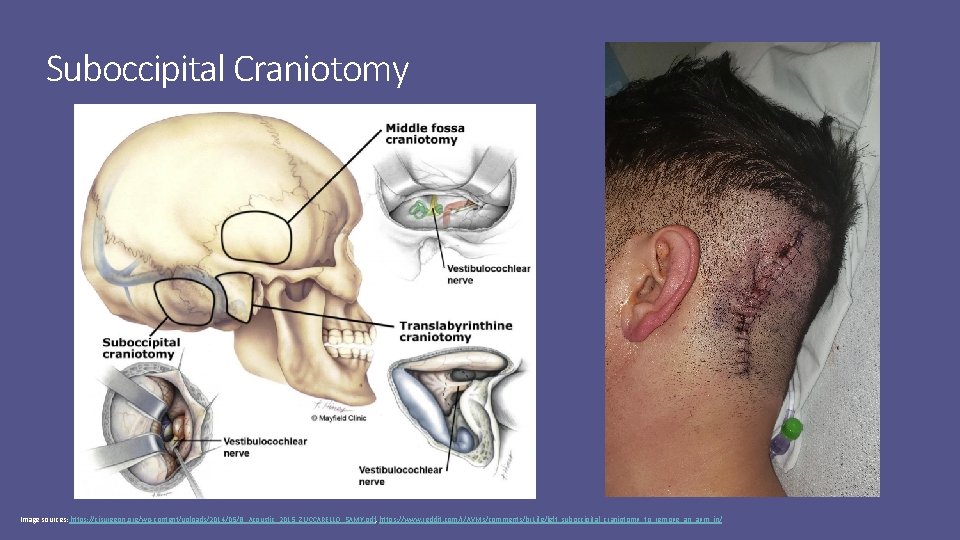
Suboccipital Craniotomy Image sources: https: //cisurgeon. org/wp-content/uploads/2014/05/B_Acoustic_2015_ZUCCARELLO_SAMY. pdf, https: //www. reddit. com/r/AVMs/comments/br 1 ife/left_suboccipital_craniotomy_to_remove_an_avm_in/

Pseudomeningocele & CSF Leak Image sources: https: //faculty. washington. edu/jeff 8 rob/trauma-radiology-reference-resource/1 -cns/extra-axial-fluid-collections/, https: //www. pinterest. com/pin/381961612118042096/, https: //www. pinterest. com/pin/54395107984579604/
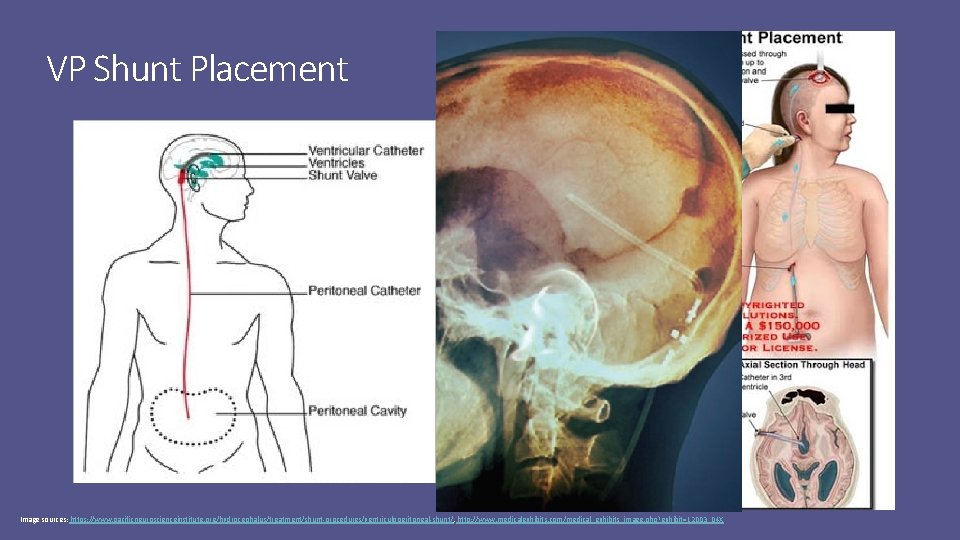
VP Shunt Placement Image sources: https: //www. pacificneuroscienceinstitute. org/hydrocephalus/treatment/shunt-procedures/ventriculoperitoneal-shunt/, http: //www. medicalexhibits. com/medical_exhibits_image. php? exhibit=12003_04 X

Assessment Neuro: • PERRLA: L pupil larger (4 mm) and sluggish response to light vs. R (3 mm, brisk) • CN: L facial droop/partial paralysis (CN VII-facial), complete loss of hearing on L (CN VIIIvestibulocochlear), slight R deviation of tongue (CN XII-hypoglossal) • Muscle strength – 4/5 in upper & lower extremities • Vision: Pt. noted blurry vision on L but was not tested. • Normal: EOM, speech, swallowing, sensation PT: • “Good functional strength. Limited by gait quality, pain, dizziness, vision. Good stability but ambulates with short steps and tentative gait. ” Pain: • 4 -6/10

Medications Scheduled: • Wellbutrin XL 300 mg po q. AM • Dexamethasone 4 mg po qd • Famotidine 20 mg po qd • Ketoralac 30 mg IV q 6 H • Lidocaine 5% patch, 2 patches qd, apply 12 hrs. then remove 12 hrs. • Polyethylene glycol 17 g qd PRN: • Tylenol 650 mg po q 4 H • Ibuprofen 800 mg po q 8 H • Methocarbamol 750 mg po q 8 H • Morphine 2. 8 mg IV q 2 H prn • Oxycodone 5 -20 mg po q 3 H • Lorazepam 0. 5 mg po q 6 H • Ondansetron 4 mg IV q 6 H • Biscodyl suppository 10 mg rectal gel • Senna 8. 6 mg po BID • Lactulose liquid 30 m. L po

Labs • CSF cell count with differential (from VP shunt): • CSF clarity: hazy • Xanthochromia: absent • CSF RBCs: 750 (H) • CSF nucleated cells (WBCs): 29 (H) • % Neutrophils: 40 • % Lymphocytes: 51 • % Macrophages: 9 • Protein, CSF: 18 • Glucose, CSF: 76 (H) • Creatinine: 0. 54 (L) • e. GFR: 118 • Hct: 43. 6% • POC Glucose: 106

Nursing Care Risk for falls related to dizziness, imbalance, recent surgery (weakness), and opioid medications • Fall precautions: bed low & locked, bed alarm on, 1 person assist with gait belt when up, non-skid socks • Patient education around fall precautions Acute pain related to recent surgery • Administration of pain medications as ordered with frequent reassessment of pain • Transition to oral pain medications and wean off IV meds important for discharge Nausea related to recent opioid medications • Administration of antiemetics as ordered • Emesis bag within reach • Essential oils pouch provided • Hold oral medications & food until no longer nauseated

Nursing Care Cont. Risk for constipation related to opioid medications • Administration of stool softeners and laxatives as ordered • Encourage ambulation with PT • Encourage oral intake as tolerated Risk for infection related to brain surgery and presence of shunt • Good hand hygiene and general hygiene practices (wiping down surfaces, keeping room clean) • Use of barrier precautions (masks, gloves during exam of incision sites) Anxiety related to pain and illness • Regularly checking in with patient about pain • Routine administration of pain meds as ordered • Administration of anxiolytic medications as needed per orders • Allowing time to talk to patient and allow exploration of feelings

Outcome • Patient was able to wean off IV pain medications with pain controlled on oral medications • PT cleared patient to be independent on POD 2 bed alarm off • Patient was able to start processing changes in her life while in the hospital expressed gratitude to nursing student for listening • Patient was discharged home on POD 2 with follow-up outpatient appointments already made

NCLEX Question 1 A patient with a suspected brain tumor is scheduled for computed tomography (CT). What should the nurse do when preparing the client for this test? A. Immobilize the neck before the client is moved onto a stretcher. B. Determine whether the client is allergic to iodine, contrast dyes, or shellfish. C. Place a cap on the client’s head. D. Administer a sedative as ordered.
NCLEX Question 2 The nurse is evaluating the status of a patient who had a craniotomy 3 days ago. Which of the following is NOT a potential sign that the patient has developed meningitis as a complication of surgery? A. B. C. D. Headache Fever Nuchal rigidity Glasgow Coma Scale score of 15

NCLEX Question 3 A patient is recovering from a VP shunt placement surgery. Which position would best optimize CSF drainage? A. Have the patient lie flat in bed. B. Have the patient lie with HOB at 30 degrees. C. Have the patient lie on the opposite side of their cranial incision. D. Have the patient lie with HOB at 45 degrees.

NCLEX Question 4 A patient who is recovering from a VP shunt placement surgery has developed abdominal pain. Which of the following actions should the nurse take? A. Reassure the patient that it is likely gas from the surgery. B. Provide the patient with a heating pack for pain relief. C. Administer pain medication as ordered. D. Assess for peritonitis as a complication of surgery.

References Acoustic neuroma (vestibular schwannoma). (2013). The Iowa Clinic. Retrieved June 30, 2020 from https: //www. iowaclinic. com/webres/File/acoustic-neuroma. pdf. Cerebral spinal fluid (CSF) collection. (2019). Medline Plus. Retrieved July 2, 2020 from https: //medlineplus. gov/ency/article/003428. htm#: ~: text=Increased%20 CSF%20 glucose%20 is%20 a, certain%20 other%20 types%20 of%2 0 meningitis. . CSF cell count. (2019). Medline Plus. Retrieved July 2, 2020 from https: //medlineplus. gov/ency/article/003625. htm. Park, J. K. , Vernick D. M. , and Ramakrishna N. (2020). Vestibular schwannoma (acoustic neuroma). Up. To. Date. Retrieved June 30, 2020 from https: //www-uptodate-com. offcampus. lib. washington. edu/contents/vestibular-schwannoma-acousticneuroma? search=vestibular%20 schwannoma&source=search_result&selected. Title=1~40&usage_type=default&display_rank=1#H 2. Vacca, V. M. (2018). Ventriculoperitoneal shunts: What nurses need to know. Nursing, 14(12), 20 -26. Retrieved July 2, 2020 from https: //nursing. ceconnection. com/ovidfiles/00152193 -201812000 -00008. pdf; jsessionid=F 47 D 6 E 1554 E 836 EBE 822 AB 76 FE 729 A 5 C. Zuccarello, M. and Samy, R. N. (2014). Contemporary Perspectives on Vestibular Schwannoma. University of Cincinnati Neuroscience Institute Brain Tumor Center. Retrieved June 30, 2020 from https: //cisurgeon. org/wpcontent/uploads/2014/05/B_Acoustic_2015_ZUCCARELLO_SAMY. pdf.
- Slides: 18