Case Presentation Presented by Keya Bala90 Sutapa Das93


Case Presentation Presented by Keya Bala(90) Sutapa Das(93) Azma Parhin(91)

Particulars Of The Patients

Name: Mrs. Nurnahar Husband’s name: Mr. Mahbub Ali Age: 60 years Sex: Female Religion: Islam Marital status: Married Occupation: Housewife Address: Anowara, Chittagong Contact no: 01643125434 Date of admission: 02. 11. 13 at 3. 00 pm Date of examination: 05. 11. 13 at 7. 00 pm Ward no: 24 , Bed no: 46 Surgical unit: 24

Presenting Complaints 1. Pain in left breast for last 1 month 2. Progressive swelling in the left breast for last 1 year.

History of Present Illness

According to the patient’s statement she was relatively well 1 year back. Then she developed a swelling on her left breast which was gradually progressive in size. The skin overlying the lump was reddish in colour. She also complained of mild pain in the swelling for last 1 month. Pain was not associated with fever, chills and rigor. She also complained that her body weight decreased 1/5 th of previous weight since last month. Then she went to doctor and diagnosed as a case of invasive duct cell carcinoma of left breast. She has no history of chest pain, haemoptysis, haematemesis, melaena, jaundice, bone pain. Her bowel and bladder habits are normal. With this complaints she got admitted in CMCH for better management

History of past illness She has no history of same type of problem before. She has no history of hypertention, diabetes, asthma.

Personal history She is non smoker, non alcoholic, she gave history of taking betel leaf and betel nuts.

Family History She has four children, all children are breast fed. None of her first degree relatives is suffering from this disease.

Drug history She took no medication for lump.

Blood transfusion history She has no history of previous blood transfusion. Immunization history She can not give history of specific immunization.

History of contraception : She gave no history of taking contraceptive pill during her reproductive age. Menstrual history : She is a post menopausal woman for 10. years. Her menarche started at 13 years. Her menstrual cycle was regular.

Systemic Enquiry : Cardiorespiratory : Chest pain – Absent Intermittent claudication – Absent Palpitation – Absent Ankle swelling – Absent Orthopnoea – Absent Nocturnal dyspnoea – Absent Shortness of breath – Absent Cough with or without sputum –Absent Haemoptysis - Absent

Gastrointestinal : Abdominal pain – Absent Dyspepsia – Absent Dysphagia – Absent Nausea and/or vomiting – Absent Changes in appetite – Absent Weight loss – Absent Change in bowel pattern – Absent Rectal bleeding – Absent Jaundice – Absent
Genito-urinary : Haematuria – Absent Nocturia – Absent Frequency – Absent Dysuria – Absent Neurological : Seizure – Absent Dizziness and loss of balance – Absent Paraesthesia – Absent Muscle weakness – Absent Muscle wasting – Absent Spasm and involuntary movement – Absent Pain in limb and back - Absent

General Examination : Appearance : Anxious Build : Below average Co-operation : Co-operative Decubitus : On choice Anaemia : Mildly anaemic Jaundice : Absent Cyanosis : Absent Edema : Absent Asicitis : Absent Dehydration : Absent Nutrition : Average Blood pressure : 110/70 mm. Hg Pulse : 72 beats/minute Respiratory rate : 17 breaths per minute Neck vein : Not engorged Neck gland : Not palpable Hernial orifices : Intact Peripheral Lymph nodes: All accessible peripheral lymph node are not palpable including axillary lymph node.

Systemic Examination : A. Abdominal Examination : 1. Inspection : Shape – Normal Umbilicus –Centrally placed, inverted No visible peristalsis No engorged vein and scar mark 2. Palpation : a. Superficial – Temperature – Not raised Tenderness – Absent Hyperasthesia – Absent Muscle guard – Absent b. Deep – Liver, spleen and kidneys are not palpable. 3. Percussion : Percussion note - Tympanic 4. Auscultation : Bowel sound - Present : :
B. Cardio-respiratory Examination 1. Inspection : - Chest : Shape – Normal Movement with respiration – In both side normal Scar mark – Absent There is a lump in upper and inner quadrant of : : left breast Left nipple is retracted Visible engorged vein over the lump 2. Palpation : - Position of trachea – Central Apex beat – in left fifth intercostals space, 10 cm from the lateral border of sternum

Vocal fremitus – Normal Chest expansion – Normal Rib tenderness – Absent Apex beat – Palpable in left fifth intercostals space, 9. 5 cm from left lateral border of sternum 3. Percussion : Percussion note – Resonant Area of liver dullness – In fifth intercostals space 4. Auscultation : Breath sound – Vesicular Vocal resonance – Normal First and second heart sound - Normal : :

Local examination : 1. Inspection : Right breast : ØNormal in appearance Ø No scar mark Ø Nipple – Not retracted Left breast : Upwards in comparison to right breast Site - There is a visible lump in the central portion of the breast Size: 5 cm Shape - Irregular Overlying skin – Not ulcerated Nipple – Retracted : :

2. Palpation : Local temperature – Slightly increased Tenderness – Mildly tender Consistancy – Hard Size – 5 x 5 cm Surface - Irregular Border – ill-defined : : Fixation – Fixed with overlying skin and not fixed with underlying pectoralis major muscle Movement is possible in all direction. Axillary group of lymph node: Not palpable in both side. Supraclavicular lymph node : Not palpable in both sides.

Salient feature Mrs. Jakia Khatun, 70 years old, hypertensive, from Bohoddarhat, Chittagong presented to me with the complaint of: : Lump in left breast for one year According to her, she noticed a lump in her left breast one year ago, at first small in size, but gradually it is increasing in size, not associated with pain. She has no anorexia, weight loss, bone pain, jaundice, itching, melaena, haemoptysis.

On general examination, patient is pale, anxious. She is hypertensive, rest other vital signs are within normal limit. Systemic examination reveals no abnormality. On local examination, the lump is situated in upper and inner quadrant of left breast, non ulcerated, hard in consistency having irregular surface and ill defined border, with a size of 12 x 5 x 3 cm. There is local rise of temperature. It is not fixed with overlying skin, or underlying pectoralis major muscle, where movement in all : : direction is possible.

Provisional Diagnosis : ØCarcinoma of breast. Differential Diagnosis : : : Ø Fibroadenoma of breast ØLipoma

Investigation Profile

Cytopathology report Specimen: Left breast lump Aspiration note: Blood mixed material came out on aspiration M/E: Smear showed many irregular clusters and scattered malignant ductal epithelial cells with large hyper chromatic and pleomorphic nuclei in a blood mixed necrotic background. Impression: Left breast lump(FNA): Duct cell carcinoma

Report: Ultra sonogram of whole abdomen Liver: is normal in size, shows homogenous parenchymal echo texture. No focal or diffuse lesion is seen. IHBCs are not dilated. Gallbladder: is well distended with normal wall thickness. No calculus is seen. Common bile duct: is not dilated. Pancreas: visualized portion of pancreas appears normal. Spleen: is normal in size with homogenous echo texture. Kidneys: are normal in size, shape and position. Cortico-medullary differentiation is maintained. Pelvi-calyceal systems are not dilated. Urinary bladder: is well distended with normal wall thickness. No intravesical lesion is seen. Impression: Normal study.

Report: Chest X-ray P/A view Diaphragm: Normal in position. Heart: Normal in transverse diameter. Lungs: Both lung fields are clear. Bony thorax: Appears normal. Impression: Normal chest X-ray.
ECG Report
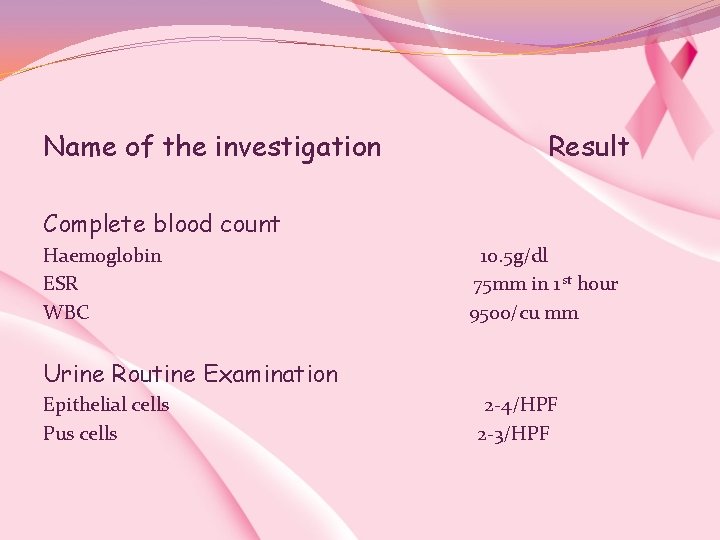
Name of the investigation Result Complete blood count Haemoglobin 10. 5 g/dl ESR 75 mm in 1 st hour WBC 9500/cu mm Urine Routine Examination Epithelial cells 2 -4/HPF Pus cells 2 -3/HPF

Investigation Profile ØFBS (Fasting blood sugar) 85 mg/dl Ø 2 hrs ABF 126 mg/dl ØSerum creatinine 0. 8 mg/dl ØSerum albumin 4. 3 g/dl ØBlood group “ A ” positive ØCytopathology report: ØLeft breast lump (FNA). ØDuct cell carcinoma. ØUSG of whole abdomen: Normal ØChest X-ray P/A view: Normal
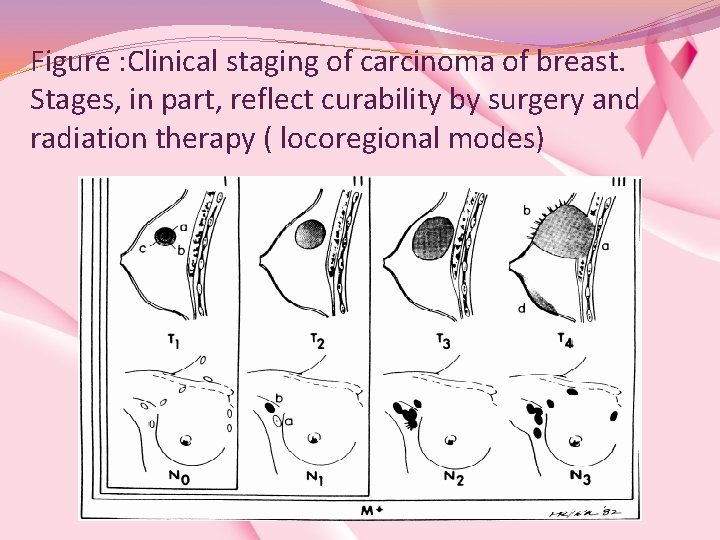
Figure : Clinical staging of carcinoma of breast. Stages, in part, reflect curability by surgery and radiation therapy ( locoregional modes)

Staging by IUAC : TNM Staging T (Tumour size) Ø T 0 =No evidence of primary tumour Ø Tis = Carcinoma in situ Ø T 1 = Tumour < 2 cm Ø T 2 = Tumour 2 -5 cm Ø T 3 = Tumour > 5 cm Ø T 4 = Any size involving skin or chest wall

N (Nodal involvement) Ø N 0 = No nodal metastasis Ø N 1 = Mobile palpable axillary lymph node Ø N 2 = Fixed axillary lymph node Ø N 3 = Ipsilateral palpable supraclavicular lymph node Ipsilateral palpable infraclavicular lymph node M (metastasis) Ø M 0 = No metastasis Ø M 1 = Distant metastasis

Manchester staging Ø Stage I= Tumour < 2 cm in diameter Ø Stage II = Tumour 2 - 5 cm in diameter with or without palpable mobile lymph node in ipsilateral axilla Ø Stage IIIa = Tumour > 5 cm in diameter with or without fixed palpable axillary lymph node. Ø Stage IIIb = Skin involvement. Skin involvement wide than tumour Peaud’ orange Fixation to underlying muscle Palpable supraclavicular lymph node Oedema of arm Ø Stage IV = Distant metastasis

Combination of Manchester and TNM staging Ø Tis : No palpable lump detected in mamography. No palpable lymph node. Ø Stage I : T 1 : Size < 2 cm in diameter No : No palpable lymph node M 0 : No metastasis Ø Stage II : T 2 : 2 -5 cm in diameter N 1 : Mobile axillary lymph node Mo : No metastasis Ø Stage IIIa : T 3 : > 5 cm in diameter N 2 : Fixed axillary lymph node M 0 : No metastasis Ø Stage IIIb : T 4 : Irrespective of size if there is any cutaneous ulceration or fixity with underlying structure N 3 : Other than axillary lymph node involvement with ipsilateral supraclavicular lymph node involvement Mo : No metastasis Ø Stage IV : M 1 : Metastasis is present No consideration about T and M

Confirmatory Diagnosis �According to the staging of combination Manchester and TNM the confirmatory diagnosis is Carcinoma of breast stage IIIa. Treatment Left sided simple mastectomy with axillary clearance.

Pre –requisite for surgery �Proper councelling �Informed written consent

Pre-operative Order Ø Keep the patient nothing by mouth from 11 pm today. Ø Take informed written consent from the patient or patient’s attendant for operation under G/A. Ø Clean and shave the operative field with right axilla. Ø Send the patient to the OT at 8 am on 10 -10 -2012. Ø Inf. Hartsol (1000 cc) I/V at 30 drops/min from 7 am on 10 -10 -2012.

Surgery �With all aseptic condition left part chest wall is opened by doing left eliptical incision. �The excised mass is composed of The whole left breast All the fat and fascia and lymph node of ipsilateral axilla

Post operative order �Nothing by mouth – till further order �Inf. 5% DNS (2000 cc) �Inf. N/S (1000 cc) I/V at 30 drops/min �Inf. Furocef (750 mg) -1 vial I/V stat 8 hourly �Inf. Flubex (500 mg) - 1 vial I/V stat 6 hourly �Inj. Pethedine (100 mg) -3/4 th ampule (75 mg)I/M �Inj. Phenerex (50 mg) -1/2 ampule I/M with Inj. Pethedine I/M 8 hourly for 24 hours �Inj. Pantonix (40 mg) -1 vial I/V stat 12 hourly �Inj. Rolac (30 mg) - 1 ampule I/V stat �Drainage tube in situ is given (collection is 1000 cc/24 hours) �Dressing condition is examined properly (dressing is dry) �Specimen sent for cytopathology examination reveals duct cell carcinoma.

Follow Up �According to cytopathology report there is duct cell carcinoma in situ ( non invasive). �Post operative radiotherapy �Regular checkup 6 month interval for 3 years � 12 months interval for rest of life �If any complaints�Clinical examination : local and sysytemic �Investigation : Mamography

Outline �Female Breast Anatomy �Breast Cancer �Mammography �Computer-Aided Diagnosis of Breast Cancer 46
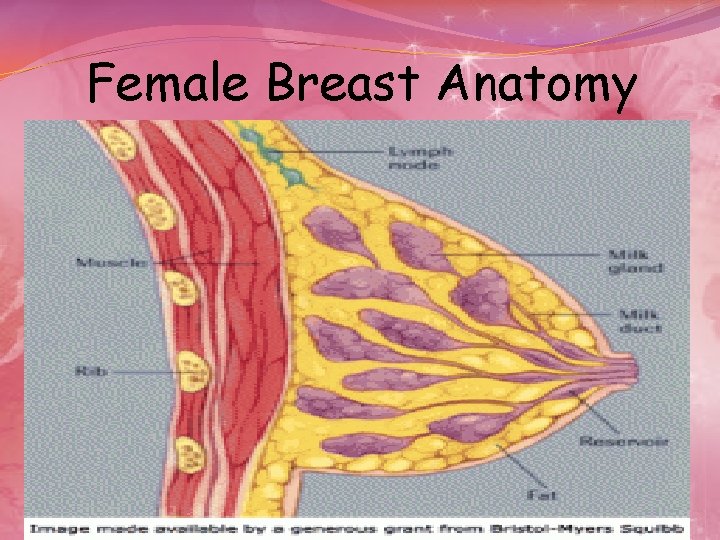
Female Breast Anatomy 47
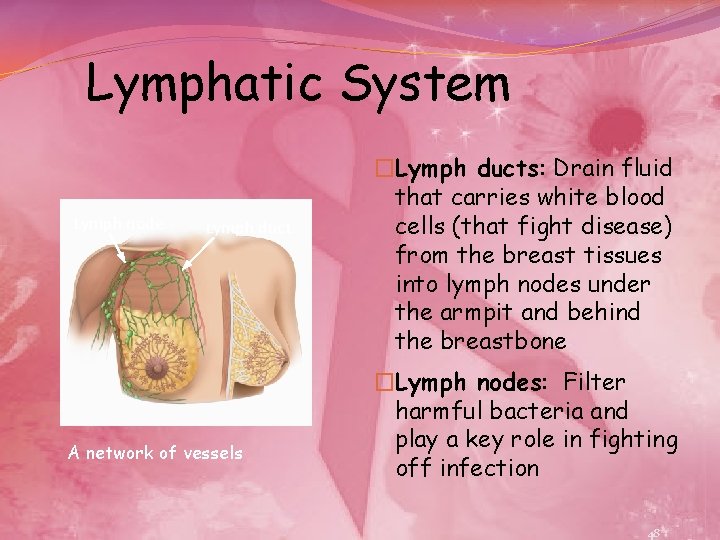
Lymphatic System Lymph node Lymph duct A network of vessels �Lymph ducts: Drain fluid that carries white blood cells (that fight disease) from the breast tissues into lymph nodes under the armpit and behind the breastbone �Lymph nodes: Filter harmful bacteria and play a key role in fighting off infection 48
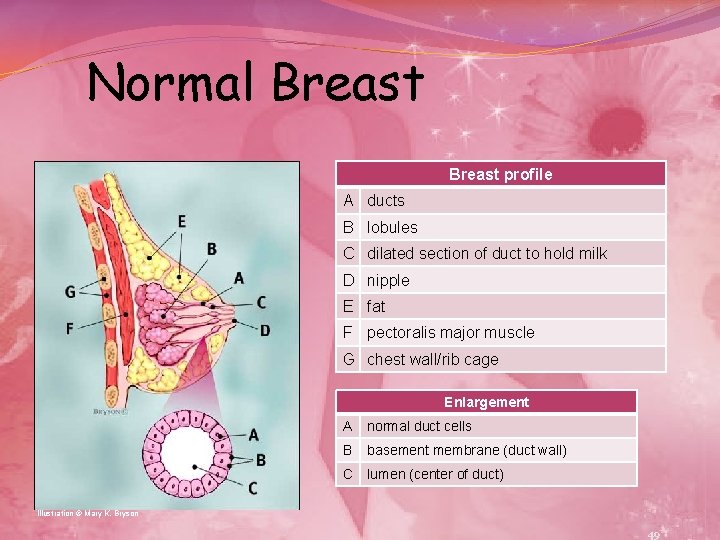
Normal Breast profile A ducts B lobules C dilated section of duct to hold milk D nipple E fat F pectoralis major muscle G chest wall/rib cage Enlargement A normal duct cells B basement membrane (duct wall) C lumen (center of duct) Illustration © Mary K. Bryson 49
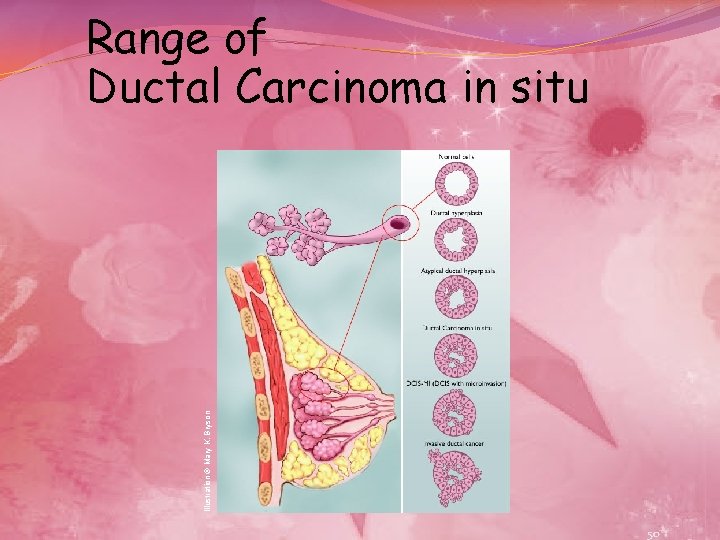
Illustration © Mary K. Bryson Range of Ductal Carcinoma in situ 50
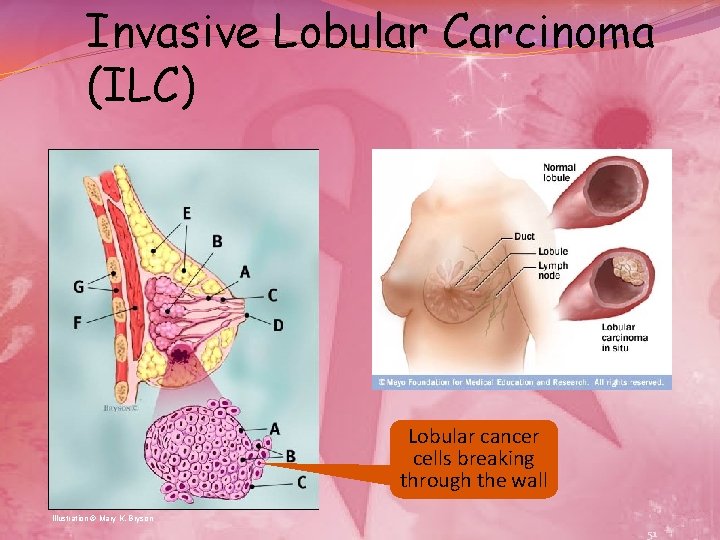
Invasive Lobular Carcinoma (ILC) Lobular cancer cells breaking through the wall Illustration © Mary K. Bryson 51

Mammography �Use a low-dose x-ray system to examine breasts �Digital mammography replaces x-ray film by solid-state detectors that convert x-rays into electrical signals. These signals are used to produce images that can be displayed on a computer screen (similar to digital cameras) �Mammography can show changes in the breast up to two years before a physician can feel them 52

Computer-Aided Diagnosis �Mammography allows for efficient diagnosis of breast cancers at an earlier stage �Radiologists misdiagnose 10 -30% of the malignant cases �Of the cases sent for surgical biopsy, only 10 -20% are actually malignant CAD systems can assist radiologists to Reduce these problems National Cancer Institute 53

Risk factors �Breast Cancer (BC) �Etiology: �The variation of incidence among �different populations: � Environmental factors: e. g. high �consumption of dietary fat, sugar. � Genetic factors especially in younger �women.

�Other risk factors: �Gross cystic disease, atypical hyperplasia �and multiple papillomatosis, �- Most forms of benign breast disease �do not predispose BC �Lobular carcinoma in situ carries a 30 �percent risk of invasive cancer.

Factors known to decrease risk: Asian ancestry. Term pregnancy before age 18 years. Early menopause , Surgical castration before the age of 37 years. Factors having no effect on risk (previously thought to be risk factors): Multiparty. Lactation. Breast feeding
Clinical breast exam Ø Mammogram - to check breast tissue Ø Computer-aided detection (CAD) Ø Digital mammography Ø Magnetic resonance imaging (MRI) Ø Breast ultraasound (ultrasonography) Other tests Experimental procedures Ø Ductal lavage Ø Molecular breast imaging (MBI)

Diagnostic procedures Ø Ultrasound Ø Biopsy – Fine-needle aspiration biopsy, core needle biopsy, sterotactic biopsy, wire localization biopsy, surgical biopsy Ø Estrogen and progesterone receptor tests Ø Staging tests – Stage 0 to IV Ø Genetic stage
Treatment �Advanced metastatic disease: �(any T, any N, M 1) �Palliative intent. �Factors affecting treatment decision: �– Menstrual states. �– Site of metastases (vital organs). �– Extent of the disease. �– Performance status and age. �Treatment: �– Systemic therapy, RT, Surgery, trials of new therapy �and supportive treatment.

Role of RT in Breast Cancer Preoperative RT. Post-mastectomy RT. Conservative surgery + RT. Palliative RT. PORT ( Post opertive radiotherapy) Indications: Patients with T 3 and T 4 tumors. > 4 Positive axillary lymph nodes. Residual disease
TREATMENT OPTION Ø In addition to coping with a potentially life-threatening illness – must make complex decisions about treatment. Ø Treatments exist for every type and stage of breast cancer. Ø Most women will have surgery and an additional (adjuvant) therapy such as radiation, chemotherapy or hormone therapy. Ø Experimental treatments are also available at cancer treatment centers.
SURGERY Ø Ø Lumpectomy Partial or segmental mastectomy Simple mastectomy Modified radical mastectomy Ø Ø Sentinel lymph node biopsy Axillary lymph node dissection Radiation therapy Chemotherapy
Reconstructive surgery Ø Reconstruction with implants Ø Reconstruction with a tissue flap Ø Deep inferior epigastric perforator reconstruction Ø Reconstruction of the nipple and areola (DIEP)

Hormonal therapy Ø Selective estrogen receptor modulators (SERMs) Ø Aromatase inhibitors Biological therapy Ø Trastuzumab (Herceptin) Ø Bevacizumab (Avastin) Ø Lapatinib (Tykerb)

COPING SKILLS Ø Telling others Ø Maintaining a strong support system Ø Dealing with intimacy Ø Self-care taking

Epidemiology Ø Breast cancer, the second-leading cause of cancer deaths in women, is the disease women fear most. Ø Breast cancer can also occur in men, but it's far less common. Ø Yet there's more reason for optimism than ever before. Ø In the last 30 years, doctors have made great strides in early diagnosis and treatment of the disease and in reducing breast cancer deaths.

Ø 80% of breast cancers occur in women older than age 50. In 30 s, have a one in 233 chance of developing breast cancer. By age 85, chance is one in eight. Ø In 1975, a diagnosis of breast cancer usually meant radical mastectomy – removal of the entire breast along with underarm lymph nodes and muscles underneath the breast. Ø Today, radical mastectomy is rarely performed. Instead, there are more and better treatment options, and many women are candidates for breast-sparing operations.

Thank you

Thank you
- Slides: 69