Case Presentation Presented by Dr Safaa fadhl Supervised

Case Presentation Presented by: Dr. Safaa fadhl Supervised by: Dr. Kamal Marghani

29 yrs male presented to ED at 1: 40 pm complaining of cough , SOB, and fever. At triage : RR Pulse rate temp Bp 22 166 40. 2 - Oxygen saturati on 86

Pt was admitted to room A at 2: 00 pm 29 yrs old male whose known to be DM for 7 yrs on mixtard insuline presented with cough , SOB, and fever for 7 days prior to the presentation for which he received amoxicillin clavunate tabs without any significant improvement. OE: pt looks ill tachypnic vitals signs : - Pulse 144 - Bp 16080 - SPO 2 65% on room air - RBS 257 - Chest : bronchial breathing , and decrease air entery on the RT side.

Plane : - Give oxygen via NRM rate 15 Lmin. Normal saline 1000 ml. Samixon 1 g BD Clarithromycin 500 BD insulin mixtard Take investigation, ABG, CXR
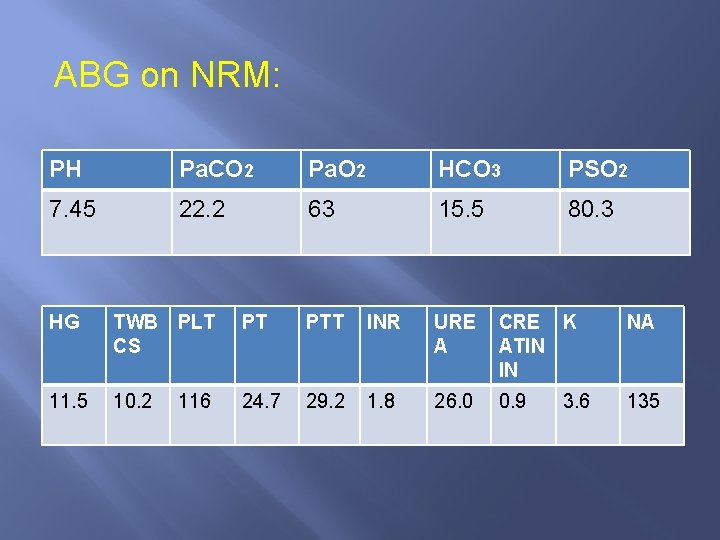
ABG on NRM: PH Pa. CO 2 Pa. O 2 HCO 3 PSO 2 7. 45 22. 2 63 15. 5 80. 3 HG TWB PLT CS PT PTT INR URE A CRE K ATIN IN NA 11. 5 10. 2 24. 7 29. 2 1. 8 26. 0 0. 9 135 116 3. 6
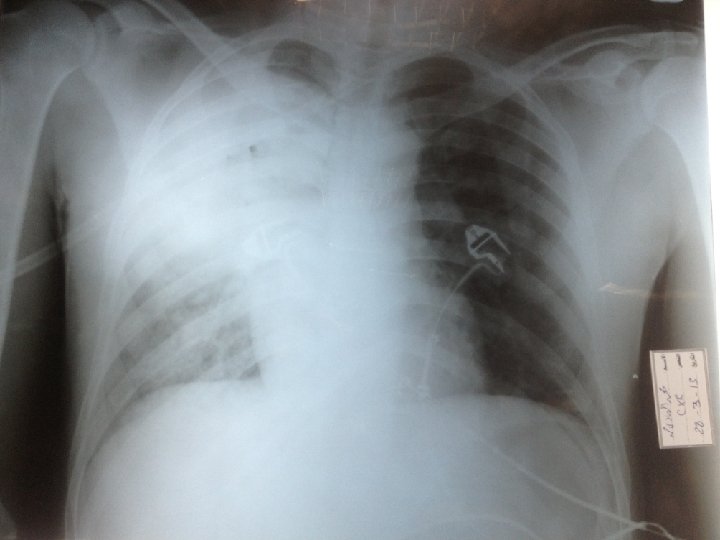

SO , the pt was diagnose as pneumonia At 9: 30 pm pt was admitted to CCR. On admission he was looking ill , tachypnic on NRM. A : his airway was patent, on NRM B : RR 39, SPO 2 85, both sides of the chest moving equally, there was bronchial breathing and decrease breath sounds on Rt side. C : pulse 130, BP 11980 D : GCS 1515 , RBS 296 E : examination of all other systems were unremarkable.
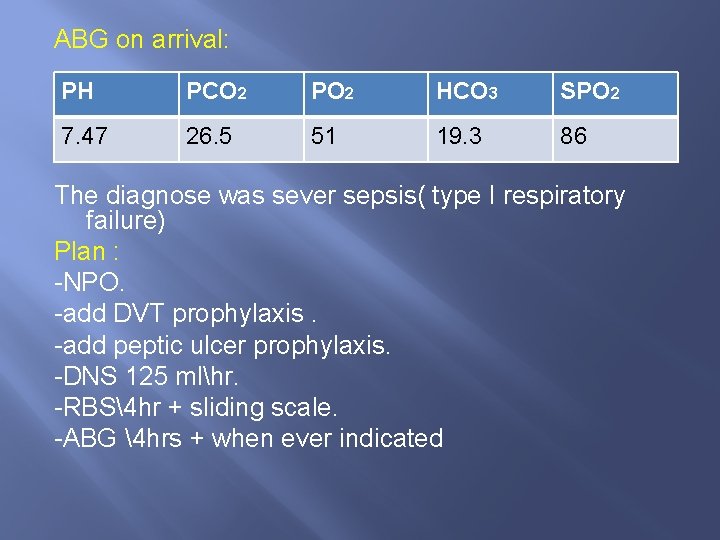
ABG on arrival: PH PCO 2 PO 2 HCO 3 SPO 2 7. 47 26. 5 51 19. 3 86 The diagnose was sever sepsis( type I respiratory failure) Plan : -NPO. -add DVT prophylaxis. -add peptic ulcer prophylaxis. -DNS 125 mlhr. -RBS4 hr + sliding scale. -ABG 4 hrs + when ever indicated
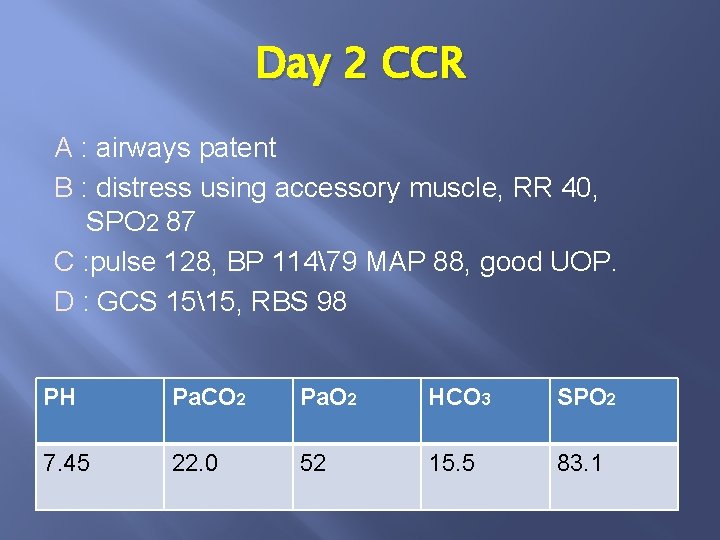
Day 2 CCR A : airways patent B : distress using accessory muscle, RR 40, SPO 2 87 C : pulse 128, BP 11479 MAP 88, good UOP. D : GCS 1515, RBS 98 PH Pa. CO 2 Pa. O 2 HCO 3 SPO 2 7. 45 22. 0 52 15. 5 83. 1
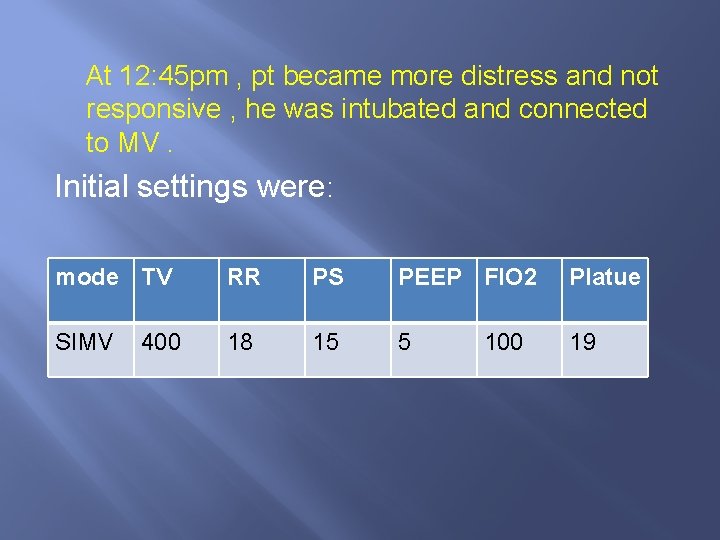

At 12: 45 pm , pt became more distress and not responsive , he was intubated and connected to MV. Initial settings were: mode TV RR PS PEEP FIO 2 Platue SIMV 18 15 5 19 400 100
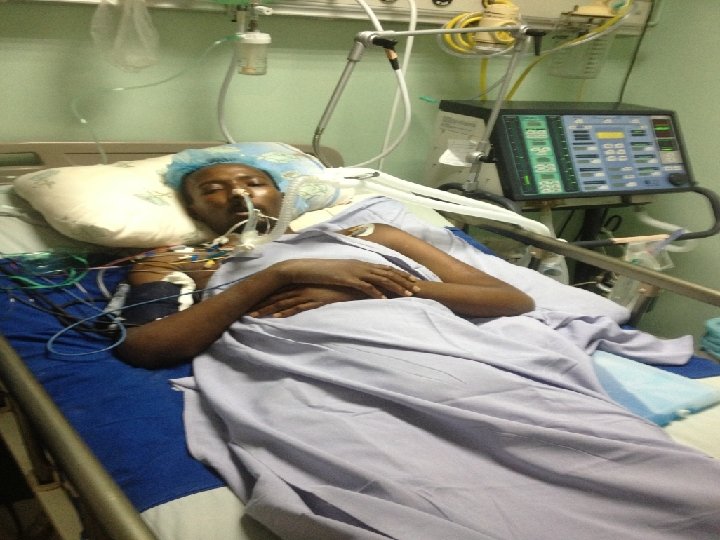
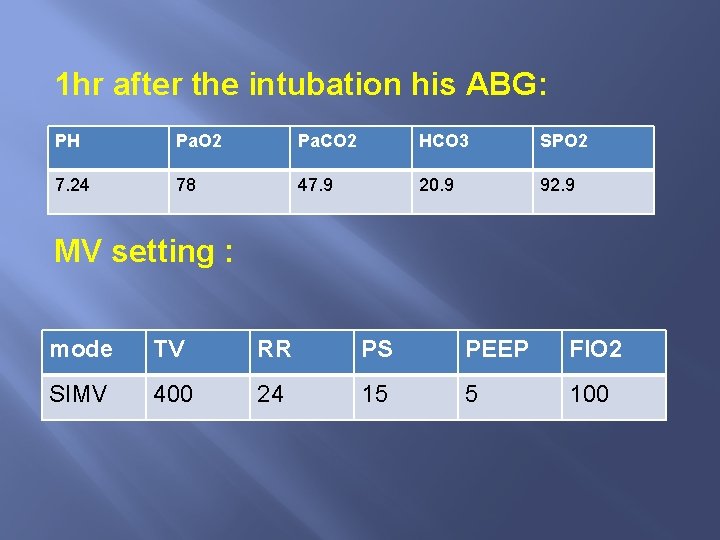
1 hr after the intubation his ABG: PH Pa. O 2 Pa. CO 2 HCO 3 SPO 2 7. 24 78 47. 9 20. 9 92. 9 MV setting : mode TV RR PS PEEP FIO 2 SIMV 400 24 15 5 100

The plan was to keep the pt MASS zero. 1 hr later the pt became hypotensive , he received 2 L of nomal saline without improvement , so noreadrenaline was added, then the BP was maintain on max dose of inotropse. .
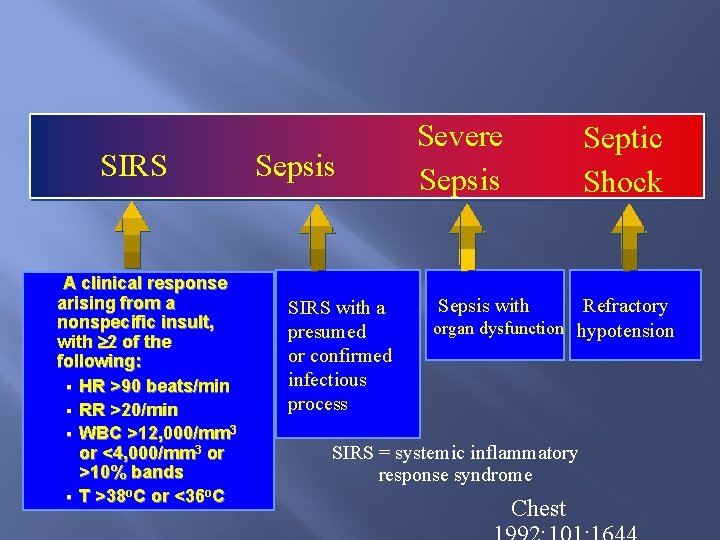
SIRS A clinical response arising from a nonspecific insult, with 2 of the following: § HR >90 beats/min § RR >20/min § WBC >12, 000/mm 3 or <4, 000/mm 3 or >10% bands § T >38 o. C or <36 o. C Sepsis SIRS with a presumed or confirmed infectious process Severe Sepsis Septic Shock Refractory organ dysfunction hypotension Sepsis with SIRS = systemic inflammatory response syndrome Chest
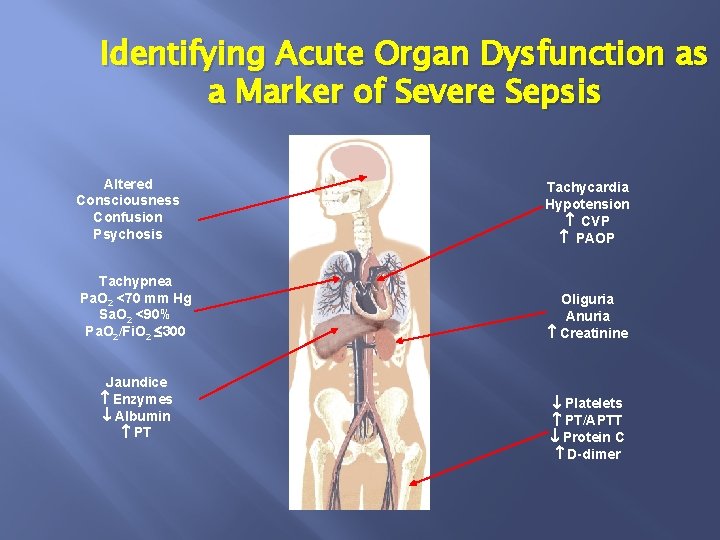
Identifying Acute Organ Dysfunction as a Marker of Severe Sepsis Altered Consciousness Confusion Psychosis Tachycardia Hypotension CVP PAOP Tachypnea Pa. O 2 <70 mm Hg Sa. O 2 <90% Pa. O 2/Fi. O 2 300 Oliguria Anuria Creatinine Jaundice Enzymes Albumin PT Platelets PT/APTT Protein C D-dimer

Early Goal-directed Therapy in the Treatment of Severe Sepsis and Septic Shock To Examine whether Early Goal Directed Therapy (EGDT) before admission to the ICU is superior to standard hemodynamic therapy in patients with sever sepsis and septic shock


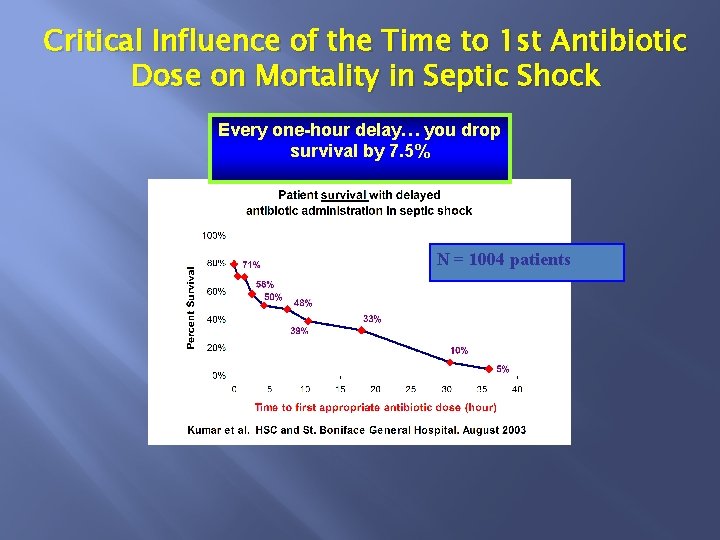
Critical Influence of the Time to 1 st Antibiotic Dose on Mortality in Septic Shock Every one-hour delay… you drop survival by 7. 5% N = 1004 patients

Initial Resuscitation, Diagnosis, and Antibiotic Therapy Recommend early goal-directed therapy Give early appropriate antibiotics Give early appropriate fluids Give appropriate inotropic support Take early cultures Take early lactate level Take early central venous oxygen saturation(SVO 2)

Inotropes in septic shock � � Noradrenaline Adrenaline Vasopressin Dopamine( selected cases) NO RENAL DOSE DOPAMINE









Intensive insulin therapy � Target glucose 140 -200 mg � Improved survival � Decreased infections � Decreased organ failure


At this stage the pt went from sever sepsis to septic shock. Plane : - NPO N. S 125 mlhr Meropenum 1 g TDS (given within 1 hr of diagnosis) Noreadrenaline infusion titrated to keep map more than 65 mmhg For septic screening. VBG RBS4 hrs + give insulin according to sliding scale( Target 140 -200)
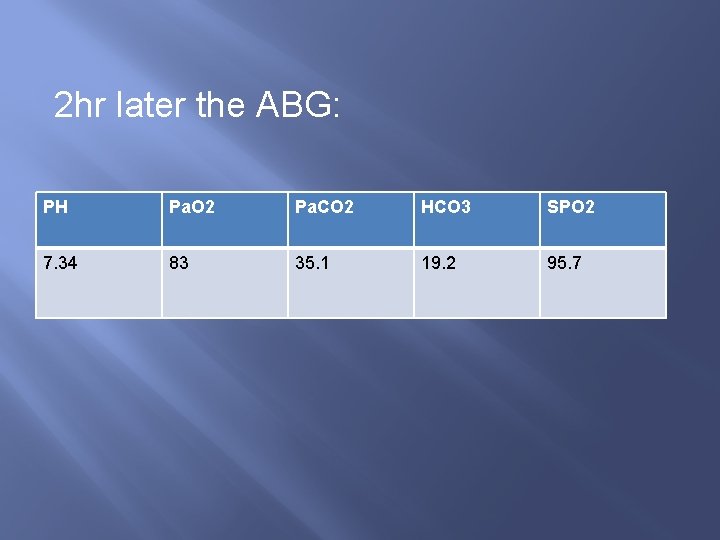
2 hr later the ABG: PH Pa. O 2 Pa. CO 2 HCO 3 SPO 2 7. 34 83 35. 1 19. 2 95. 7

Day 3 PH Pa. O 2 Pa. CO 2 HCO SPO 2 7. 52 51 35. 4 28. 9 89. 5 - As the pt had a refractory hypoxymia , he was kept MASS zero for another 48 hrs. -Noreadrenaline : weaned to off But the pt still febrile so vancomycine was added

Day 4 Off Noreadrenaline. Sedation vacation done, GCS 1115
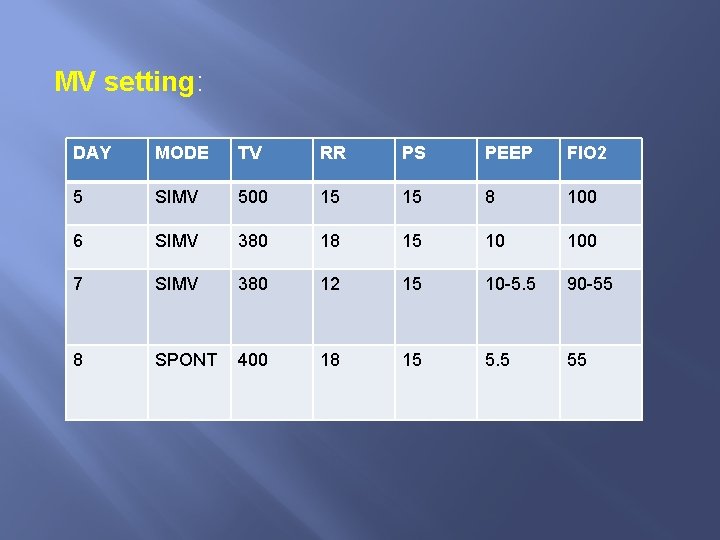
MV setting: DAY MODE TV RR PS PEEP FIO 2 5 SIMV 500 15 15 8 100 6 SIMV 380 18 15 10 100 7 SIMV 380 12 15 10 -5. 5 90 -55 8 SPONT 400 18 15 5. 5 55

Day 9 CCR: -Pt on spont for more than 24 hrs on minimal ps - fully conscious communicating in tube. -Good cough reflex. - NPO. EXTUBATED AT 11: 00 am and put on simple mask

THE Message Time is life Timing

Thank you for your attention
- Slides: 41