Case of Inflammatory Bowel Disease Colic and intraabdominal

Case of Inflammatory Bowel Disease, Colic, and intra-abdominal abscess Naomi Chiero DVM - Intern Mentors: Margaret Mac. Harg, MS, DVM; John Vacek DVM Kendall Road Equine Hospital (KREH) Elgin, Illinois

Patient Signalment: • 12 year old Thoroughbred Gelding history: Treated by r. DVM previous night for colic (7 -2 -11) Initial colic signs treated by trainer with IV Banamine (500 mg) PE: mild tachycardia (44 bpm), passing normal manure Rectal: Tight band traveling craniodorsally on left side Abd US: unable to visualize left kidney Treated with additional dose of IV Banamine (250 mg) In morning continued to show colic signs and referred to KREH Previous history: Treated at University of Georgia (UGA) one year prior: Diagnosed with Inflammatory Bowel Disease and Gastric Ulcers History of chronic weight loss and intermittent colic Previous treatments include tapering dose of Dexamethasone, daily omeprazole, and dietary changes.

Inflammatory bowel disease: • Chronic idiopathic disease due to abnormal immune response – – – – Inciting cause is an unknown bacteria, virus, parasite, or dietary antigen Abnormal immune response causes massive cellular infiltration Generally the small intestine (SI) is predominantly affected Chronic cellular infiltrate creates a malabsorption and maldigestion • IBD is further classified based on the type cellular infiltrate – Eosinophilic enteritis – eosinophils and lymphocytes • MEED: multisystemic eosinophilic epitheliotrophic disease – more severe form of disease with multiple organ involvement – Granulomatous Enteritis – lymphocytes and macrophages • Similar to Crohn’s diease in humans and Johnne’s disease in cattle – Lymphocytic Enteritis – lymphocytes and plasma cells • May be an early form of intestinal lymphosarcoma

Inflammatory bowel disease: Historical findings in IBD horses Weight loss or failure to gain weight despite adequate nutrition Occasional history of chronic diarrhea (when large intestine is affected) Mild recurrent colic or acute/severe colic requiring surgery IBD is an uncommon disease of young to middle aged horses More common causes of weight loss and diarrhea include: Chronic Parasitism Dental Disease Malnutrition Use of NSAIDS Salmonellosis Gastrointestinal ulceration Sand Ingestion Other less common causes of weight loss and diarrhea include: Neoplasia Chronic Renal Failure Intra-abdominal abscess Infectious anemia Liver Failure Bacterial infection (pneumonia, plueropneumonia, peritonitis)

Inflammatory bowel disease: Diagnostics for history of Weight loss +/- chronic diarrhea Thorough history/examination of diet, physical exam, oral exam CBC and Biochemistry: IBD cases may have normal CBC or have mild neutrophila, hyperfibrogenemia, and anemia. Biochemistry often shows hypoproteinemia and hypoalbuminemia. Rectal Exam: Occasionally thickened loops of SI can be palpated in horses with IBD. Abdominal and Thoracic Ultrasound: Ultrasound is helpful to document small intestinal wall thickening. As well as examination of liver, kidneys, colon, and lungs, to rule out other differentials Abdominocentesis: Horses with IBD typically have normal peritoneal fluid Gastroscopy and Duodenal Biopsy: Confirm or rule out gastric ulcers and collect duodenal biopsy to rule in IBD Rectal Biopsy: Can detect evidence of inflammatory disease.

Presentation to KREH: 7 -3 -11 Physical Exam: Depressed attitude Tachycardia (60 bpm) Hypermotile borborygmi Repeatedly stretching out Mild pyrexia (102. 0°F) BCS: 2/9 PCV: 36% TS: 5. 4 g/d. L NG Tube: no net reflux Rectal: tight band traveling craniodorsally on left side in area of nephrosplenic space initial diagnosis: Nephrosplenic Entrapment of large colon

Initial treatment: Administer Phenylephrine hydorchloride 20 mg Phenylephrine diluted in 60 mls of Lactated Ringers Solution and administered IV over period of 5 minutes Phenylephrine is a vasoconstrictor used in nephrosplenic entrapments to contract the spleen and allow release of entrapment Jogged patient for 15 min Maintenance IV Fluids (2 -3 mls/kg/hr) – Lactated Ringer’s Solution Monitoring: 2 hours post treatment Worsening colic signs (progressed from stretching to rolling) Persistent tachycardia (HR: 56 -60 bpm) Rectal exam: spleen responsive to phenylephrine, but large colon still entrapped with mild-moderate gas distension Recommendation: Exploratory Celiotomy to correct displacement due to persistent tachycardia, level of pain, and poor response to phenylephrine
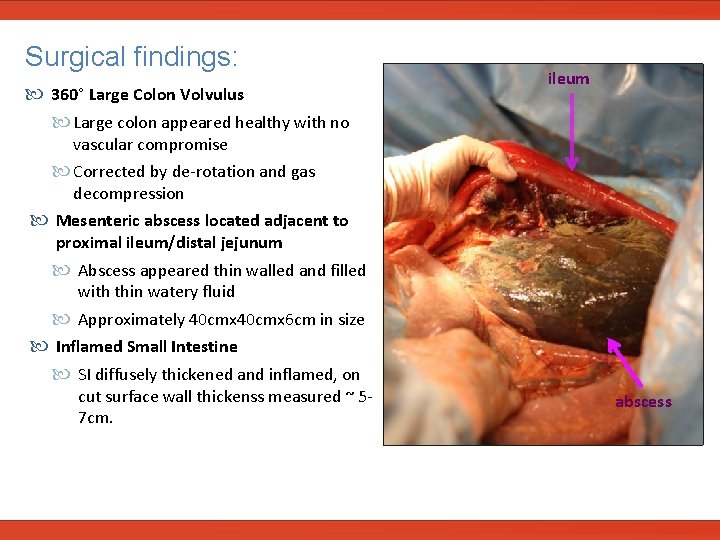
Surgical findings: 360° Large Colon Volvulus Large colon appeared healthy with no ileum vascular compromise Corrected by de-rotation and gas decompression Mesenteric abscess located adjacent to proximal ileum/distal jejunum Abscess appeared thin walled and filled with thin watery fluid Approximately 40 cmx 6 cm in size Inflamed Small Intestine SI diffusely thickened and inflamed, on cut surface wall thickenss measured ~ 57 cm. abscess
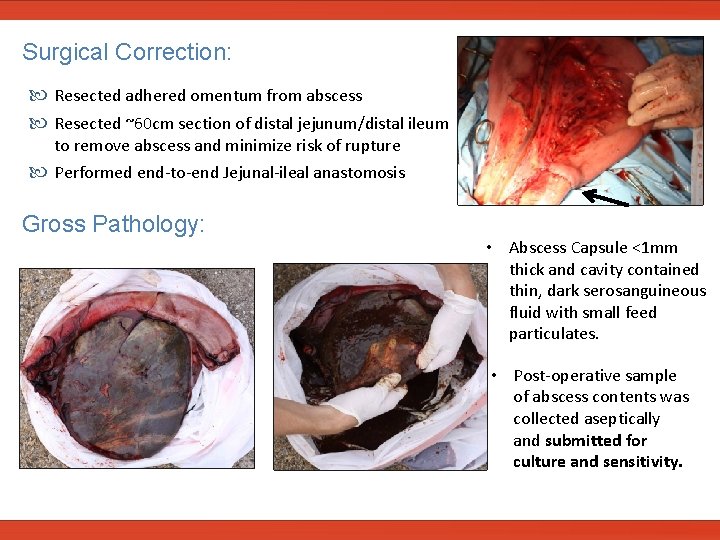
Surgical Correction: Resected adhered omentum from abscess Resected ~60 cm section of distal jejunum/distal ileum to remove abscess and minimize risk of rupture Performed end-to-end Jejunal-ileal anastomosis Gross Pathology: • Abscess Capsule <1 mm thick and cavity contained thin, dark serosanguineous fluid with small feed particulates. • Post-operative sample of abscess contents was collected aseptically and submitted for culture and sensitivity.

Post-operative care: Analgesia Flunixin Meglumine: 0. 5 mg/kg IV BID x 2 days, then as needed Broad Spectrum Antibiotics Gentamicin sulfate: 6. 6 mg/kg IV SID x 4 days Aminoglycoside: gram negative spectrum Procaine Penicillin G: 22, 000 IU/kg IM BID x 4 days β-lactam: covers gram positive and gram negative cocci Metronidazole: 22 mg/kg PO TID x 4 days Anaerobic spectrum and anti-inflammatory/immune-modulatory affects Fluid Therapy Lactated Ringer’s Solution at maintenance dose (2 -3 mls/kg/hr) Monitoring q 4 hours Watch for colic signs, measure vitals, fecal output, and PCV/TP
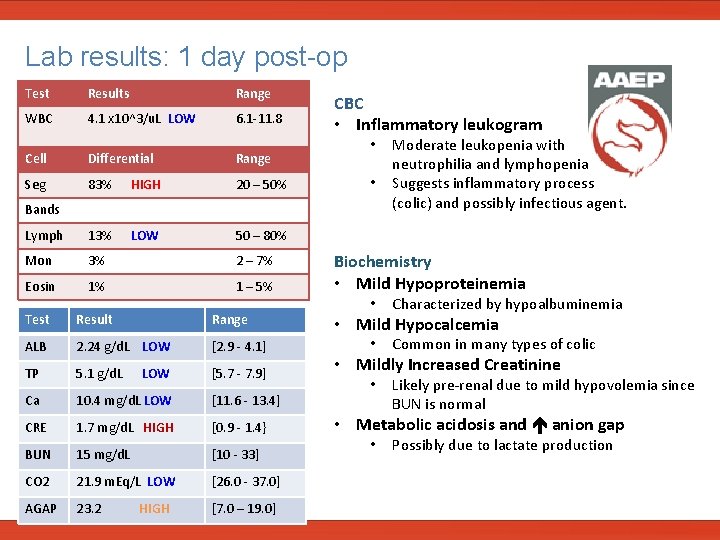
Lab results: 1 day post-op Test Results Range WBC 4. 1 x 10^3/u. L LOW 6. 1 -11. 8 Cell Differential Seg 83% HIGH 20 – 50% Lymph 13% LOW 50 – 80% Mon 3% 2 – 7% Eosin 1% 1 – 5% Test Result Range ALB 2. 24 g/d. L LOW [2. 9 - 4. 1] TP 5. 1 g/d. L LOW [5. 7 - 7. 9] Ca 10. 4 mg/d. L LOW [11. 6 - 13. 4] CRE 1. 7 mg/d. L HIGH [0. 9 - 1. 4} BUN 15 mg/d. L [10 - 33] CO 2 21. 9 m. Eq/L LOW [26. 0 - 37. 0] AGAP 23. 2 HIGH [7. 0 – 19. 0] Range CBC • Inflammatory leukogram • • Bands Moderate leukopenia with neutrophilia and lymphopenia Suggests inflammatory process (colic) and possibly infectious agent. Biochemistry • Mild Hypoproteinemia • Characterized by hypoalbuminemia • Mild Hypocalcemia • Common in many types of colic • Mildly Increased Creatinine • Likely pre-renal due to mild hypovolemia since BUN is normal • Metabolic acidosis and anion gap • Possibly due to lactate production

Further history & University Findings: Presented to University of Georgia (UGA) July 2010 History of drastic weight loss over 6 month period and development of foul smelling “cowpie” feces. Diagnostics and Findings PE: WNL, except BCS: 2/9 (1015 lbs) Rectal exam: mildly distended and thickened loops of small intestine. Abdominocentesis: peritoneal fluid WNL CBC/Chemistry: no significant abnormalities Gastroscopy/duodenal biopsy: Stomach: extensive hyperkeratosis, superficial gastric ulceration, and a few deeper bleeding ulcers along the margo plicatus and lesser curvature of the stomach. Grade 2 EGUS Duodenal histopathology: Eosinophilic infiltrates Grade 2 ulcers
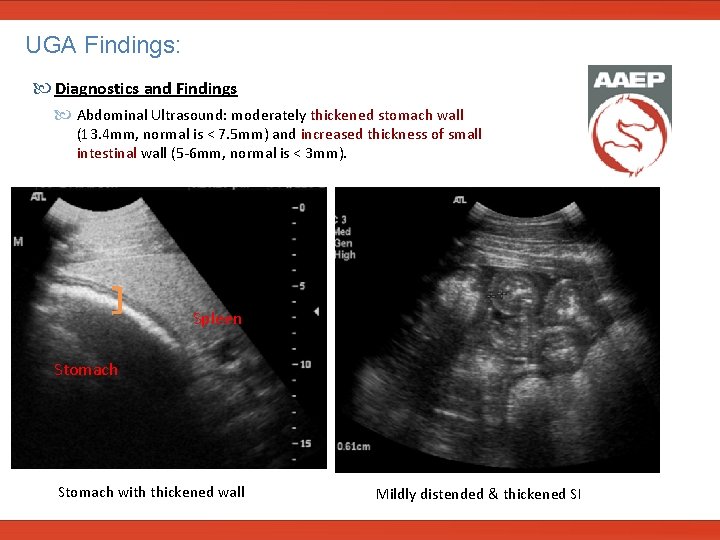
UGA Findings: Diagnostics and Findings Abdominal Ultrasound: moderately thickened stomach wall (13. 4 mm, normal is < 7. 5 mm) and increased thickness of small intestinal wall (5 -6 mm, normal is < 3 mm). Spleen Stomach with thickened wall Mildly distended & thickened SI

UGA Findings: – Diagnostics and Findings • Fecal egg count, fecal sand test, & Salmonella PCR: all negative • Glucose Absorption Test: Adequate • Serial PCV/TS: – Packed cell volume remained WNL – Total solids were persistently low (avg. 5. 5 g/d. L) – Final Diagnoses: • Inflammatory Bowel Disease (Eosinophilic enteritis) – Hallmarks of IBD that were found in this case include: » Chronic weight loss in spite of adequate nutrition » Chronic diarrhea » Thickened loops of small intestine detected through rectal examination and abdominal ultrasound » Duodenal biopsy revealing eosinophilic infiltrates » Persistent hypoproteinemia with low-normal albumin • Grade 2 Equine Gastric Ulcer Syndrome
UGA Treatment & Recommendations: – Gastric Ulcers • Sucralfate: 20 mg/kg PO QID x 2 weeks • Omeprazole: 4 mg/kg PO SID x 28 days – Inflammatory Bowel Disease • Fenbendazole: 10 mg/kg PO SID x 5 days • Ivermectin: 200 ug/kg PO once • Dexamethasone: – Week 1 - 46 mg (0. 1 mg/kg) IV for 7 days, – Week 2 - 46 mg (0. 1 mg/kg) PO for 7 days, » then ~25% tapered dose each week – Week 3 – 36 mg (0. 08 mg/kg) PO for 7 days – Week 4 – 26 mg (0. 06 mg/kg) PO for 7 days – Week 5 – 16 mg (0. 03 mg/kg) PO for 7 days – Week 6 – 8 mg (0. 02 mg/kg) PO for 7 days until recheck – Feeding Recommendations • • Free choice orchard grass and alfalfa hay 6 -12 hours daily pasture turn out Nutrena XTN 2 lbs 4 times a day Assure Guard (3/4 scp BID daily) & Assure Plus (1 scp SID daily x 2 weeks)

UGA Recheck: – Findings and Diagnostics – August 2010 • PE: WNL, BCS: 3/9 (1168 lbs – weight gain of 153 lbs in 4 weeks) • Ultrasound: Sm. Intestinal wall thickness: 4 mm (improved from 5 mm) • Gastroscopy: 2 superficial linear ulcers and mild hyperkeratosis present in the non-glandular portion of the stomach. Grade 1 ulcers. • Total Protein: 6. 1 g/d. L (previous avg. of 5. 5 g/d. L) • Albumin: 3. 3 g/d. L (previously 2. 2 g/d. L) – Treatment and Recommendations • Omeprazole: 4 mg/kg PO SID x 14 days, then 2 mg/kg SID x 7 days, followed by 1 mg/kg maintenance dose. – Recommend giving full 4 mg/kg dose 3 days prior to and for duration of any stressful event, diet change, or trailering. • Dexamethasone: 8 mg (0. 02 mg/kg) PO EOD x 2 weeks, then discontinue. May have to continue therapy if relapse occurs.
KREH 7 -4 -11 Patient Progress: Patient recovered well from surgery. All physical parameters WNL within 24 hrs of surgery. Maintained on IV fluids for first 48 hrs Fasted first 12 hours post-operatively Gradual re-introduction of feed starting with Equine Senior mashes, then grazing. Introduced incremental amounts of soaked hay 5 days post-op switched to oral antibiotics July 6 th Trimethoprim/sulfamethoxazole: 30 mg/kg PO BID x 6 days July 12 th • July 10 th – July 16 th • • • Patient had mild intermittent colic episodes approximately EOD. Initial colic episodes treated with Flunixin meglamine and feed removal, each episode milder and resolved with hand walking only. Visible weight gain

Which disease came first? OR – Inflammatory Bowel Disease or Intra-abdominal abscess: • The mesenteric abscess was present for unknown amount of time, could have been present during previous work up at University and gone undetected. • Intra-abdominal abscesses can cause chronic weight loss and intermittent colic. • Abscess could be inciting cause of abnormal immune response creating inflammatory bowel disease. – Testing hypothesis: • To test the hypothesis it was decided to not restart steroid treatment. • If patient improved the abscess may have been inciting cause of IBD and the disease process may resolve with removal of inciting cause. • If patient does not improve then… – Abscess could be unrelated incidental finding – Abscess is inciting cause but IBD now chronic sequela requiring treatment – GI ulceration/perforation and abscess formation could have resulted from high steroid doses used to treat IBD.

Patient Progress: 7 -11 -11 CBC/Chem • Normal lymphocyte count – discontinue anitbiotics • Persistent hypoproteinemia (5. 5 g/d. L) and hypoalbuminemia(2/7 g/d. L) Abscess Culture & sensitivity • 1 Isolate: Escherichia coli • Sensitive to Gentamicin, Penicillin, and Tribrissin 7 -18 -11 July 6 th Discontinued all medications Diet consisting of: • 1 flake soaked grass hay 6 x/day • 2 lbs XTN 6 x/day (12 lbs total) • Turned out to graze 1 -2 hrs/day Significant visible weight gain, BSC 3/9 Discharged from hospital: Continue current diet, slowly decreasing frequency of feedings • Stall rest with 2 -3 hrs/daily turn out for 3 weeks, then return to normal turn-out Recheck in 60 -90 days • July 18 th

KREH 8 -16 -11 REcurrent Colic: • History after discharge • 1 st week: regular improvement with good appetite and weight gain. • 2 nd week: small decline in attitude and appetite • 3 rd & 4 th week: management changes led to return of appetite • Today: horse colicky, trying to lay down/roll no improvement with 1 dose (500 mg) of Flunixin meglamine. • Presentation • BAR, comfortable, passed normal manure in trailer • PE: WNL, except hypermotile borborgymi & BCS 2/9 *Recurrent weight loss despite adequate diet* • PCV: 32% TS: 4. 8 g/d. L *TS rechecked* • Nasogastric Tube – no net reflux • Rectal exam: gas distension of large colon and cecum, with large colon palpated medial to spleen, no tight bands palpated. • Initial Diagnosis: Nephrosplenic Entrapment
Recurrent Colic: • Initial Treatment: • Placed jugular catheter • Administered 20 mg Phenyleprhine (same as prev. described) • Patient jogged for 15 min – passed large amount of gas • Remained comfortable with no further colic signs • 6 hrs later re-introduced small amount of feed • Lab Results: • • • Mild leukopenia with near normal differential Persistent and worsening hypoproteinemia/ hypoalbuminemia Mild hypocalcemia Test Results Range WBC 5. 9 x 10^3/u. L low 6. 1 -11. 8 Cell Differential Range Seg 51% 20 – 50% 48% 50 – 80% Bands Lymph Mon Eosin 2 – 7% 1% 1 – 5% Test Result Range ALB 2. 8 g/d. L LOW [2. 9 - 4. 1] TP 5. 2 g/d. L LOW [5. 7 - 7. 9] Ca 11. 2 mg/d. L [11. 6 - 13. 4] Fibrinogen 155 mg/d. L [150 – 350]

Which disease came first? – Inflammatory Bowel Disease or Intra-abdominal abscess: • Previous Hypothesis: Abscess is inciting cause of an abnormal immune response creating inflammatory bowel disease and disease will resolve if remove inciting cause. – Results: • Poor Clinical Response… Recurrent Weight Loss Recurrent Colic Persistent Hypoproteinemia Persistent Hypoalbuminemia • “If patient does not improve then…” – Abscess may be secondary incidental finding – Abscess is inciting cause but IBD now chronic sequela requiring treatment – GI ulceration/perforation and abscess formation could have resulted from high steroid doses used to treat IBD. • Don’t know which scenario is true. However, solution is the same no matter the cause, need immunosuppressive treatment for IBD.
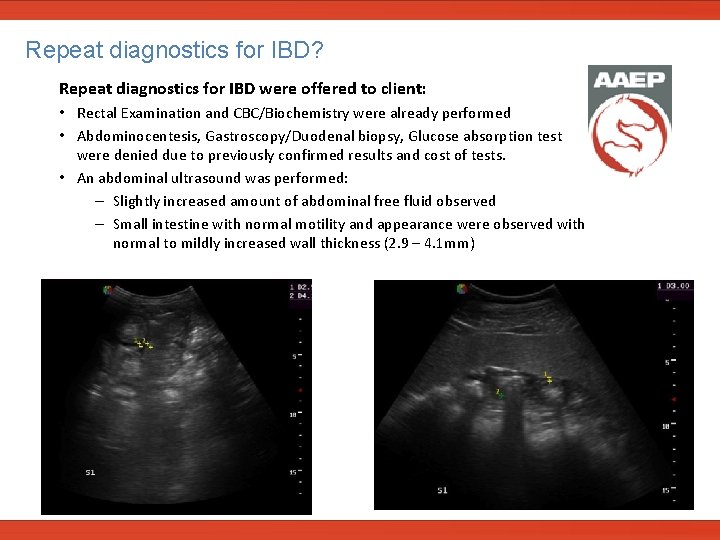
Repeat diagnostics for IBD? Repeat diagnostics for IBD were offered to client: • Rectal Examination and CBC/Biochemistry were already performed • Abdominocentesis, Gastroscopy/Duodenal biopsy, Glucose absorption test were denied due to previously confirmed results and cost of tests. • An abdominal ultrasound was performed: – Slightly increased amount of abdominal free fluid observed – Small intestine with normal motility and appearance were observed with normal to mildly increased wall thickness (2. 9 – 4. 1 mm)

Initiate Treatment for IBD – Immunosuppressive Steroid Treatment: Moderate steroid dose was chosen since cause of abdominal abscess remains unknown and risk of GI ulceration. – Dexamethasone: » 12 mg (0. 025 mg/kg) IM SID x 2 days » 10 mg (0. 02 mg/kg) IM SID x 4 days » 10 mg IM EOD x 7 days » 10 mg PO TIW x 30 days – Immunomodulatory Supplement: – 4 Life Transfer Factor Livestock Stress Formula: » 1 Scoop PO SID » Transfer Factor is a vitamin, mineral, electrolyte, and probiotic supplement that also contains transfer factors. Transfer Factors are immune-modulatory molecules extracted from cow colostrum and egg yolks that are said to promote immune function » Anecdotal improvement in animals with immune related diseases such as melanomas and hypersensitivities.

Patient Progress: • Feeding during hospitalization • • • Free choice grass hay fed 6 x/day 2 lbs XTN and 1 lb Equine Senior 6 x/day 2 -3 hours daily turn-out/grazing • Weight Tape 8/17: 1, 003 lbs. 8/29: 1, 049 lbs • Documented weight gain over two week period • Feeding Recommendations • • Free choice grass hay Minimum 3 -4 hours daily pasture turn-out Grain: Transition to Buckeye EQ 8 Gut Health • 3. 5 lbs fed 3 x/day (10 -11 lb total/day) • High fat, low carbohydrate feed with highly digestible fiber and live probiotic Fat Supplement: Buckeye Ultimate Finish 40 • 2 oz/day for 7 days, then increase to 4 oz/day • Highly palatable fat supplement with omega 6 and omega 3 fatty acids • Discharged 8/31, recommend recheck in 30 days August 29 th

Recheck Exam: 10 -14 -11 • Current Medications: • Dexamethasone 10 mg (0. 02 mg/kg) PO TIW • 1 Scoop Transfer Factor PO SID • BCS: 4. 5/9 Weight Tape: 1126 lbs. • Abdominal Ultrasound: • Normal loops of small intestine visible with normal motility. Wall thickness: 3 -4 mm, diameter: 2 -3 cm • PCV/TS: 32% / 6. 0 g. d. L • Recommendations: • Decrease Dexamethasone to 6 mg (0. 01 mg/kg) PO TIW • Continue Transfer Factor 1 Scoop PO SID • Continue previous feeding instructions • Recheck in 3 months

Recheck Exam: 3/23/12 • Current Medications: • Dexamethasone 6 mg (0. 01 mg/kg) PO TIW • 1 Scoop Transfer Factor PO SID • BCS: 7/9 Weight Tape: 1238 lbs. • Abdominal Ultrasound: WNL, SI wall thickness: 2 -3 mm • PCV/TS: 35% / 5. 8 g. d. L • Recommendations: • Transfer Factor 1 scp PO SID • Decrease feed or increase work • Continue tapering Dexamethasone dose • 6 mg PO Mon/Fri and 4 mg Wed x 30 days • 6 mg PO Wed and 4 mg Mon/Fri x 30 days • 4 mg PO Mon/Wed/Fri x 60 days • 4 mg PO Mon/Fri for maintenance • Recheck in 4 -5 months or if clinical signs return
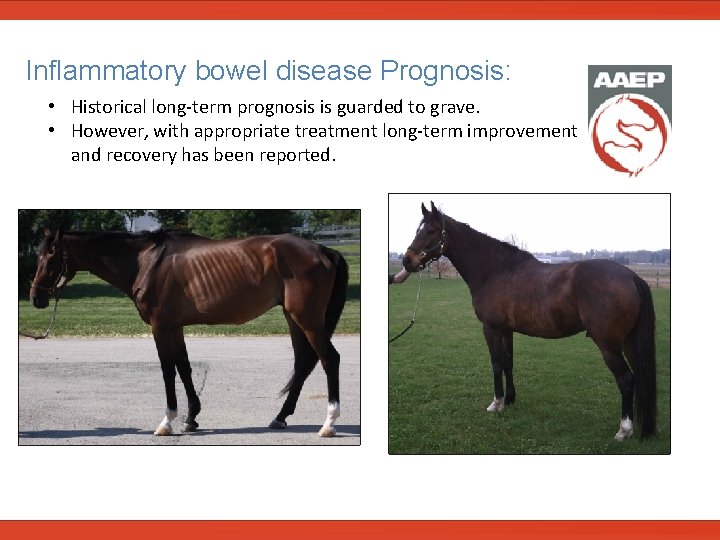
Inflammatory bowel disease Prognosis: • Historical long-term prognosis is guarded to grave. • However, with appropriate treatment long-term improvement and recovery has been reported.

References & further reading: 1. Abutarbush, S. M. , & Naylor, J. M. (2005). Comparison of surgical versus medical of nephrosplenic entrapment of the large colon in horses: 19 cases (1992 -2002). JAVMA, 227(4), 603 -605. 2. Baker, W. T. , Frederick, J. , Giguere, S. , Lynch, T. M. , Lehmkuhl, H. D. , & Slone, D. E. (2011). Reevaluation of the effect of phenylephrine on resolution of nephrosplenic entrapment by the rolling procedure in 87 horses. Veterinary Surgery, 40(7), 825 -829. 1. Buchanan, B. R. , & Andrews, F. M. (2003). Treatment and prevention of equine gastric ulcer syndrome. Veterinary Clinics of North America: Equine Practice, 2003(3), 575 -597. 2. Kalck, K. A. (2009). Inflammatory bowel disease in horses. Veterinary Clinics of North America: Equine Practice, 25(2), 303 -315. 1. Mair, T. S. , & Sherlock, C. E. (2011). Surgical drainage and post operative lavage of large abdominal abscess in six mature horses. Equine Veterinary Journal, 43(Suppl. 39), 123 -127. 2. Schumacher, J. , Edwards, J. F. , & Cohen, N. D. (2000). Chronic iodiopathic inflammatory bowel diseases of the horse. Journal of Veterinary Internal Medicine, 14, 258 -265.

Acknowledgments: Thank you to: Dr. Mac. Harg for surgical correction of case, mentorship of Margaret medical management, and case report assistance. Dr. John Vacek for assisting in initial case work up and continued mentorship. Dr. Elizabeth Pollak for case anesthesia and assistance with patient care. Dr. Megan Coveyou for case referral and continued patient care. Drs. Erin L Mc. Conachie, Michelle Barton, and Kelsey Hart for consultation and initial diagnosis at the University of Georgie College Veterinary Medicine.
- Slides: 30