Care of the newborn infant Partners in Global

Care of the newborn infant Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control Variations exist from place to place in the care of the newborn infant. However, although often neglected, their basic needs are the same. Infants who are unwell or have congenital abnormalities fall short of the mother’s expectation of a beautiful bundle of joy. All mothers require urgent and sensitive counselling. 10. Rooming in 11. Feeding 12. Immunizatio n For more information about the authors and reviewers of this module, click here

How should I study this module? Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control 10. Rooming in 11. Feeding 12. Immunizatio n • This self-directed learning (SDL) module has been designed primarily for medical students but may also be of use to healthcare providers especially at the primary care level. • We suggest that you first read the learning outcomes and try to keep these in mind as you go through the module slide by slide and at your own pace. • Answer the MCQ at the end to assess your learning. • You should research any issues that you are unsure about. Look in your textbooks, access the on-line resources indicated at the end of the module and discuss with your peers and teachers. • Finally, enjoy your learning! We hope that this module will be easy to study and complement your learning about newborn care from other sources.

Learning outcomes Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control 10. Rooming in 11. Feeding 12. Immunizatio n After studying this module, you should be able to • Describe the routine clinical assessment of newborn infants • Describe some common congenital abnormalities • Describe the essential elements of the routine management of newborn infants including hygiene, cord care, feeding and rooming-in • Describe what routine immunisations are required during infancy • Discuss what information is required by mothers prior to discharge

Clinical assessment Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control After delivery of the baby and in the absence of any immediate problems, essential newborn care begins with a thorough general clinical assessment. This should be done on all infants soon after birth to detect signs of illness and congenital abnormalities. The following slides describe the assessment that should be performed routinely in all infants. This initial assessment should indicate where more detailed clinical assessment is required. A resident doctor washing her hands up to the elbows prior to examination 10. Rooming in 11. Feeding 12. Immunizatio n Hand washing with soap and water before and after a baby is handled goes a long way in reducing the risk of infection
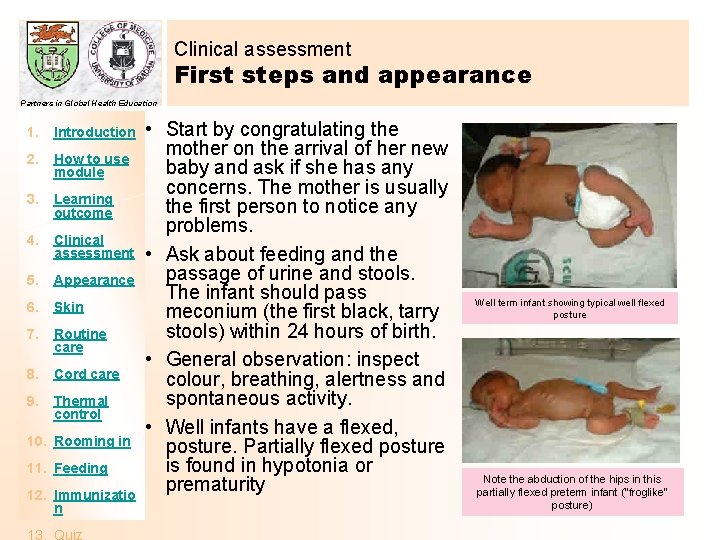
Clinical assessment First steps and appearance Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control 10. Rooming in 11. Feeding 12. Immunizatio n • Start by congratulating the mother on the arrival of her new baby and ask if she has any concerns. The mother is usually the first person to notice any problems. • Ask about feeding and the passage of urine and stools. The infant should pass meconium (the first black, tarry stools) within 24 hours of birth. • General observation: inspect colour, breathing, alertness and spontaneous activity. • Well infants have a flexed, posture. Partially flexed posture is found in hypotonia or prematurity Well term infant showing typical well flexed posture Note the abduction of the hips in this partially flexed preterm infant (“froglike” posture)
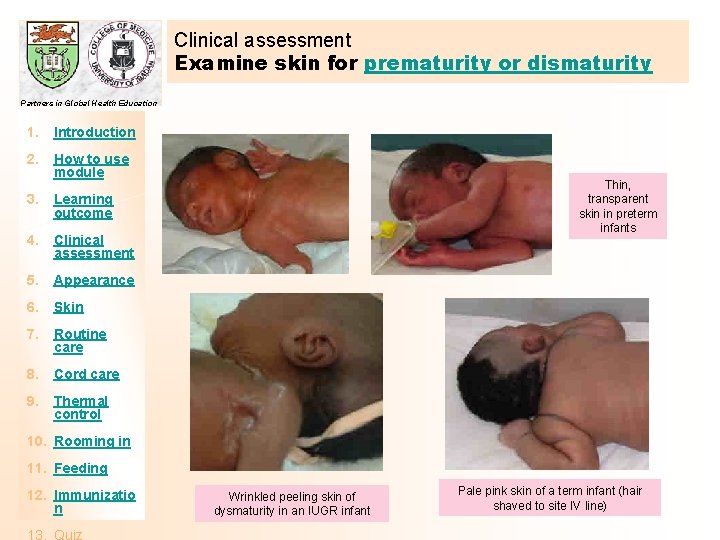
Clinical assessment Examine skin for prematurity or dismaturity Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control Thin, transparent skin in preterm infants 10. Rooming in 11. Feeding 12. Immunizatio n Wrinkled peeling skin of dysmaturity in an IUGR infant Pale pink skin of a term infant (hair shaved to site IV line)

Clinical assessment Skin: some common normal findings Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control 10. Rooming in 11. Feeding 12. Immunizatio n • Vernix caseosa: a cream/white cheesy material on the skin at birth which cleans off easily with oil. • Lanugo; fine downy hairs seen on the back and shoulders especially in preterm infants. • Milia: pinpoint whitish papules on nose and cheeks due to blocked sebaceous glands. • Mongolian blue spots: grey/bluish pigment patches seen in the lumbar area, buttocks and extremities in dark skinned babies. They usually disappear by one year. • Capillary heamangiomas (“stork bite” naevi): red flat patches which blanch with gentle pressure. Commonly occur on upper eyelids, forehead and nape of the neck. • Erythema toxicum: small white/yellow papules or pustules on a red base seen on face, trunk and limbs. Develop 1 – 3 days after birth and usually disappear by one week.
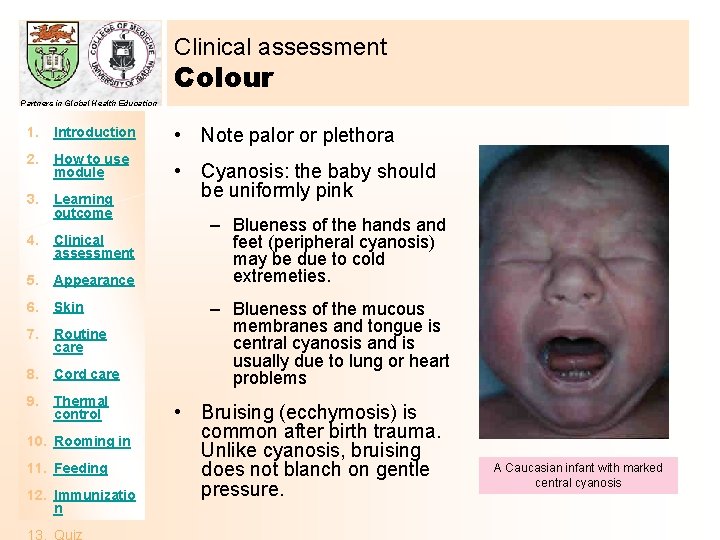
Clinical assessment Colour Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control 10. Rooming in 11. Feeding 12. Immunizatio n • Note palor or plethora • Cyanosis: the baby should be uniformly pink – Blueness of the hands and feet (peripheral cyanosis) may be due to cold extremeties. – Blueness of the mucous membranes and tongue is central cyanosis and is usually due to lung or heart problems • Bruising (ecchymosis) is common after birth trauma. Unlike cyanosis, bruising does not blanch on gentle pressure. A Caucasian infant with marked central cyanosis

Clinical assessment Jaundice Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control Jaundice is common in the first week of life and may be missed in dark skinned babies • Blanch the tip of the nose or hold baby up and gently tip forward and backward to get the eyes to open. • Teach mother to do the same at home in the first week and report to hospital if significant jaundice is observed. Blanching the tip of the nose 10. Rooming in 11. Feeding 12. Immunizatio n Two infants with jaundice; note yellow sclerae
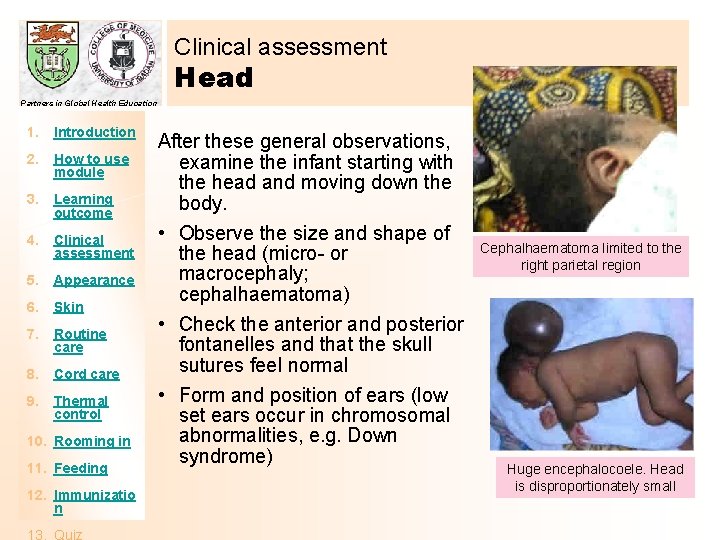
Clinical assessment Head Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control 10. Rooming in 11. Feeding 12. Immunizatio n After these general observations, examine the infant starting with the head and moving down the body. • Observe the size and shape of the head (micro- or macrocephaly; cephalhaematoma) • Check the anterior and posterior fontanelles and that the skull sutures feel normal • Form and position of ears (low set ears occur in chromosomal abnormalities, e. g. Down syndrome) Cephalhaematoma limited to the right parietal region Huge encephalocoele. Head is disproportionately small
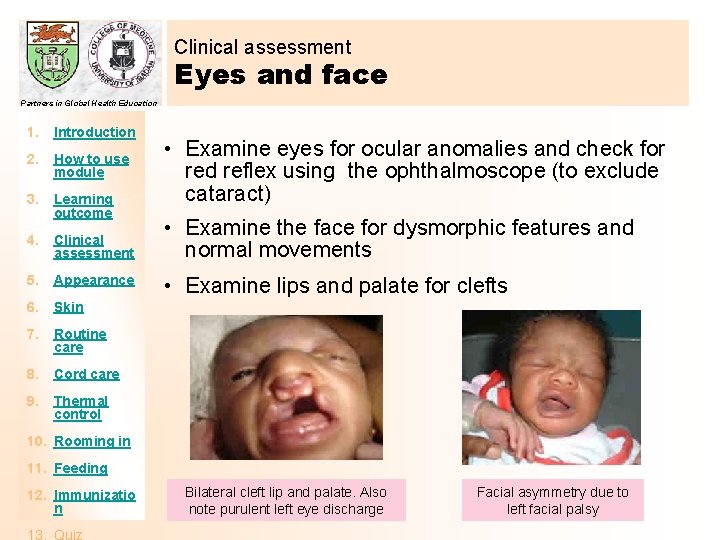
Clinical assessment Eyes and face Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control • Examine eyes for ocular anomalies and check for red reflex using the ophthalmoscope (to exclude cataract) • Examine the face for dysmorphic features and normal movements • Examine lips and palate for clefts 10. Rooming in 11. Feeding 12. Immunizatio n Bilateral cleft lip and palate. Also note purulent left eye discharge Facial asymmetry due to left facial palsy

Clinical assessment Cardiovascular and respiratory Partners in Global Health Education 1. Introduction 2. How to use module • Feel femoral and radial pulses for volume, rate and rhythm. • In aortic coarctation, femoral pulse is reduced, absent or not synchronous with radial pulse. 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care – faster in preterms. 9. Thermal control – > 60 / minute abnormal 10. Rooming in 11. Feeding 12. Immunizatio n • If child is sick, measure blood pressure. • Locate the apex beat and listen to the heart sounds for murmurs. • Count the respiratory rate – normal 30 – 40 breaths/min in term infants • Observe for respiratory distress: nasal flaring, intercostal and subcostal recession.
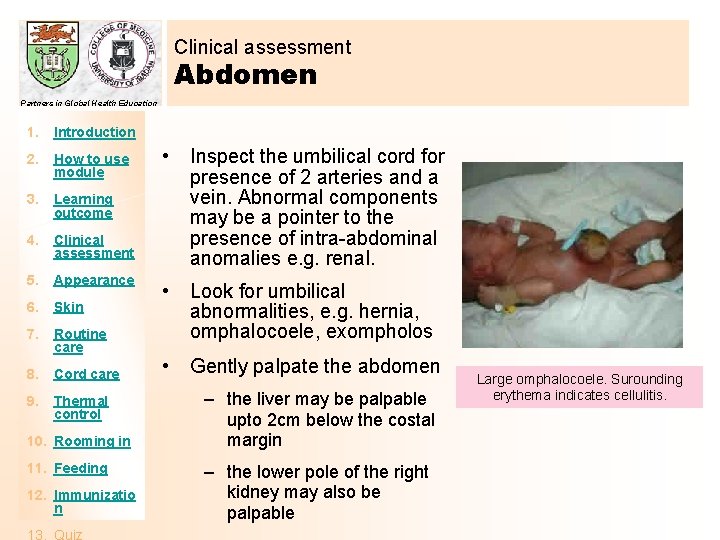
Clinical assessment Abdomen Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control 10. Rooming in 11. Feeding 12. Immunizatio n • Inspect the umbilical cord for presence of 2 arteries and a vein. Abnormal components may be a pointer to the presence of intra-abdominal anomalies e. g. renal. • Look for umbilical abnormalities, e. g. hernia, omphalocoele, exompholos • Gently palpate the abdomen – the liver may be palpable upto 2 cm below the costal margin – the lower pole of the right kidney may also be palpable Large omphalocoele. Surounding erythema indicates cellulitis.
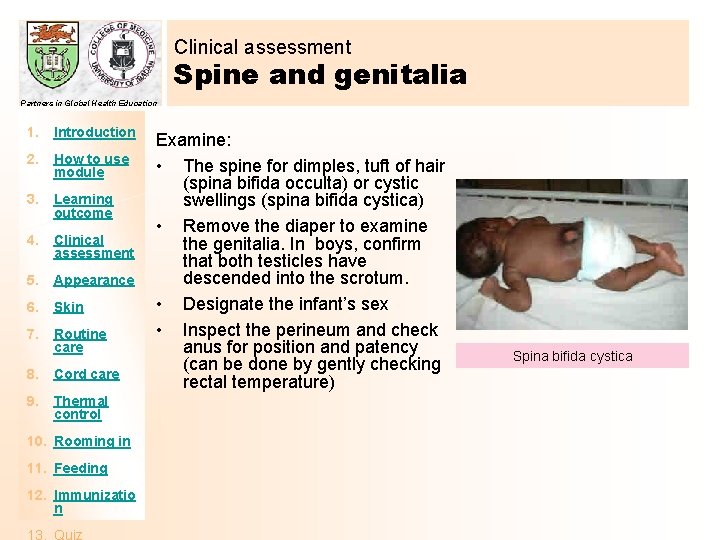
Clinical assessment Spine and genitalia Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control 10. Rooming in 11. Feeding 12. Immunizatio n Examine: • The spine for dimples, tuft of hair (spina bifida occulta) or cystic swellings (spina bifida cystica) • Remove the diaper to examine the genitalia. In boys, confirm that both testicles have descended into the scrotum. • Designate the infant’s sex • Inspect the perineum and check anus for position and patency (can be done by gently checking rectal temperature) Spina bifida cystica

Clinical assessment Dysmorphic features Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance • Inspect the feet. Note effects of foetal posture should be noted. 6. Skin • Check hips for dislocation 7. Routine care 8. Cord care 9. Thermal control • Limitation of limb movements occurs in fractures and nerve injury • Examine hands. Note single palmar crease in chromosome abnormalities. Short stuby fingers and single palmar crease of Down syndrome 10. Rooming in 11. Feeding 12. Immunizatio n Talipes affecting the left leg
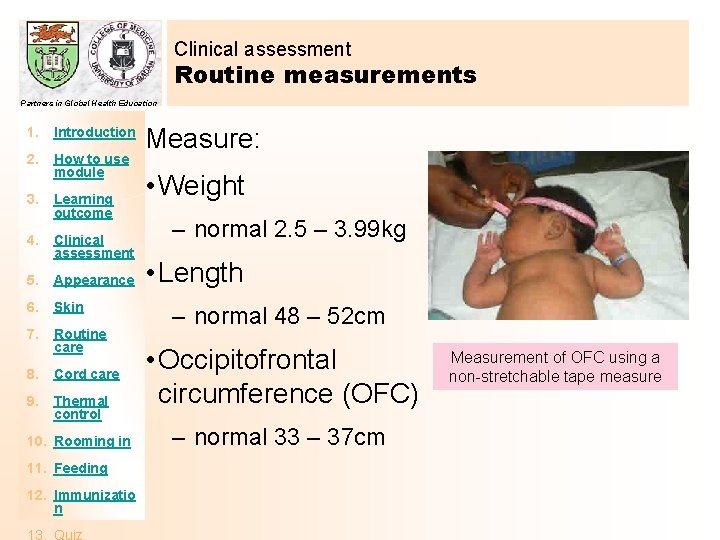
Clinical assessment Routine measurements Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control 10. Rooming in 11. Feeding 12. Immunizatio n Measure: • Weight – normal 2. 5 – 3. 99 kg • Length – normal 48 – 52 cm • Occipitofrontal circumference (OFC) – normal 33 – 37 cm Measurement of OFC using a non-stretchable tape measure

Routine care of the well newborn Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome Any problems identified during the initial assessment will need specific management. However, newborn infants are a highly susceptible group and high-quality routine care prevents a multitude of problems. The major elements of routine care include: 4. Clinical assessment • Cord care 5. Appearance • Thermal control 6. Skin • 24 hour rooming in 7. Routine care • Feeding 8. Cord care • Immunization 9. Thermal control 10. Rooming in 11. Feeding 12. Immunizatio n Click on the links for more information on these important elements of routine care • Maternal education on hygiene and every other aspect of routine care Hand washing with soap and water every time a baby is handled goes a long way in reducing the risk of infection!

Quiz: Concerning care of the newborn Write “T” or “F” on the answer sheet. When you have completed all 5 questions, click on each box and mark your answers. Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control 10. Rooming in 11. Feeding 12. Immunizatio n a. Nursing a newborn with the mother rather than in the nursery predisposes the child to infections b. Hand washing with soap and water before handling a newborn significantly reduces the risk of infection in the baby c. Fortified infant formula is superior to mother’s breast milk in a sick term newborn d. Newborn babies cannot be kept warm without the use of incubators e. Jaundice cannot be detected early in dark skinned babies Click to reveal correct answers a b c d e

Sources of information Partners in Global Health Education 1. Introduction 2. How to use module 3. Learning outcome 4. Clinical assessment 5. Appearance 6. Skin 7. Routine care 8. Cord care 9. Thermal control 10. Rooming in 11. Feeding 12. Immunizatio n • Pocket book of Hospital care for children; guidelines for the management of common illnesses with limited resources. WHO http: //www. who. int/child-adolescenthealth/publications/CHILD_HEALTH/PB. htm • Essential newborn care http: //www. who. int/reproductive health/publications/ • Nelson Textbook of Pediatrics: 16 th Edition. Richard E. Behrman Robert Kliegman, Hal B. Jenson (Editors),
- Slides: 19