Care of the Client with Chest Tubes Matthew

Care of the Client with Chest Tubes Matthew D. Byrne, RN, MS, CPAN 9/9/2020

Outline l l Basics Indications Insertion Function 9/9/2020
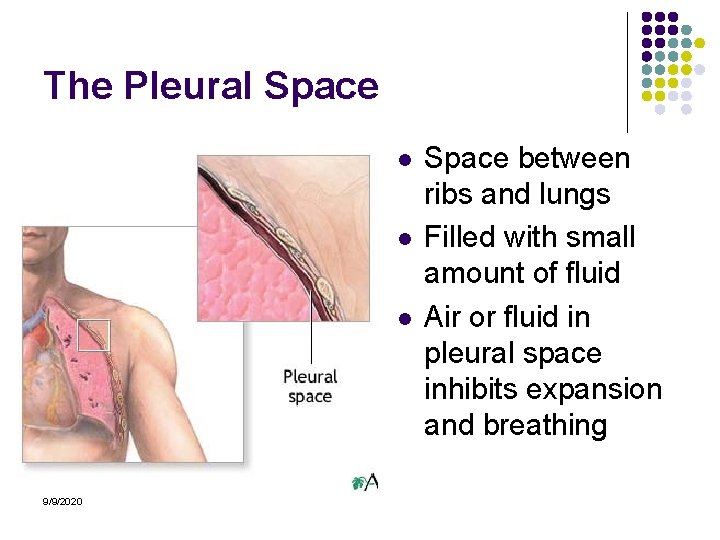
The Pleural Space l l l 9/9/2020 Space between ribs and lungs Filled with small amount of fluid Air or fluid in pleural space inhibits expansion and breathing

The Pleural Space l l l 9/9/2020 Physiologically, intrapleural pressure is 4 -5 cm H 2 O below atmospheric pressure during expiration Intrapleural pressure is 8 -10 cm H 2 O below atmospheric pressure during inspiration If the intrapleural pressure equals the atmospheric pressure, the lung will collapse, causing a pneumothorax
Chest Tubes: Basics l l l Used when integrity of the pleural space is lost Loss of normal intrapleural pressures Air or fluid may enter with loss of integrity 9/9/2020 Image from Trauma. org
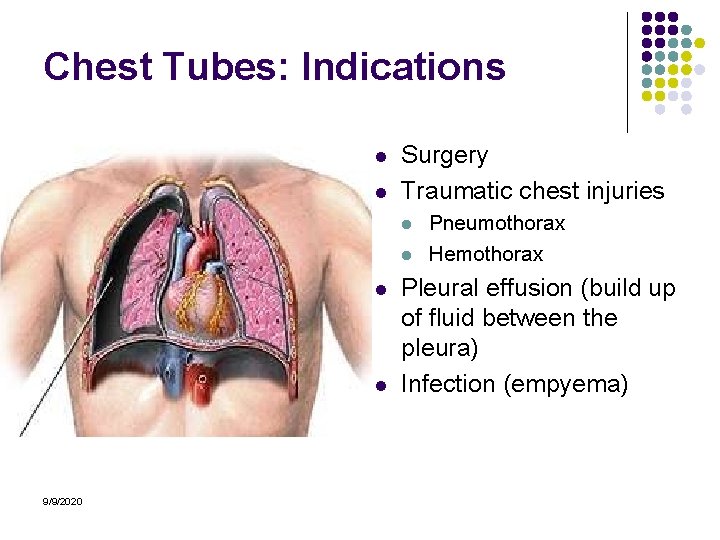
Chest Tubes: Indications l l Surgery Traumatic chest injuries l l 9/9/2020 Pneumothorax Hemothorax Pleural effusion (build up of fluid between the pleura) Infection (empyema)

Chest Tubes: Insertion l l l l l 9/9/2020 Placed in the OR/ER/PACU or bedside Metal trocar used as guide Generally done with some sedation Ideally restores negative pressure and allows air to escape/fluid to drain Sutured to chest wall Occlusive dressing applied Serial chest X-Rays for progress/placement Free end attached to drainage system Connections are secured (taped/banded) Pre and post vital signs and pain assessment
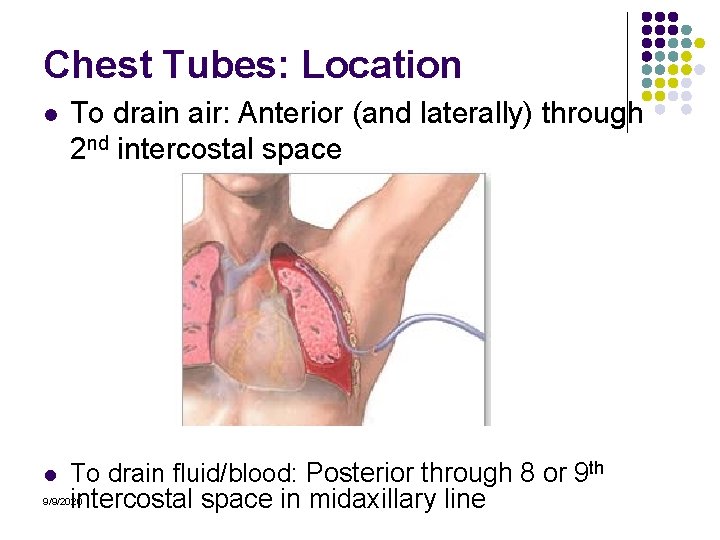
Chest Tubes: Location l To drain air: Anterior (and laterally) through 2 nd intercostal space l To drain fluid/blood: Posterior through 8 or 9 th intercostal space in midaxillary line 9/9/2020

Chest Tubes: How they function l Drainage systems: l l One chamber Two chamber Three chamber Two types of suction control chambers: l l 9/9/2020 1) dry (valve/regulator) 2) wet (water chamber) control

When you breathe… l l When you inhale, negative pressure is created in your chest that pulls air in through your mouth/nose What would happen if there was a hole in your chest? A chest tube system can act as a one-way valve that can remove air/fluid Can also be set up to create “pull” in the form of negative pressure 9/9/2020

Chest tube systems l What do we need to connect to this tube in the patient’s chest? l How can what we connect collect drainage, allow air to escape and create a slight pull? l We need a three part system to do this… 9/9/2020
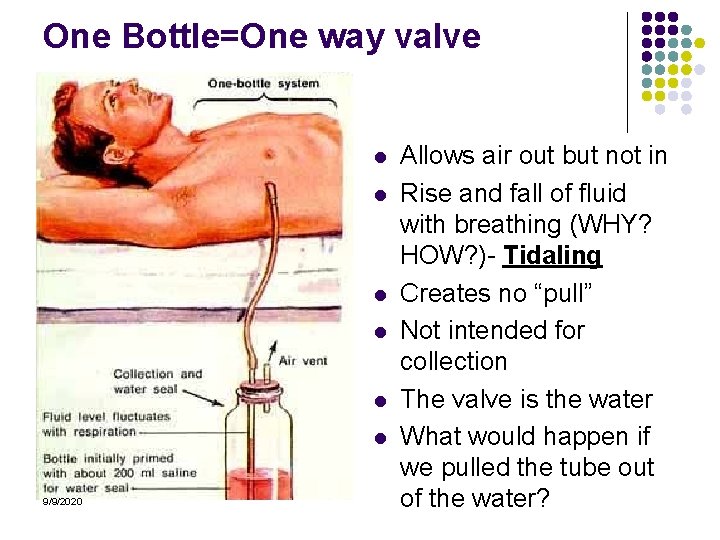
One Bottle=One way valve l l l 9/9/2020 Allows air out but not in Rise and fall of fluid with breathing (WHY? HOW? )- Tidaling Creates no “pull” Not intended for collection The valve is the water What would happen if we pulled the tube out of the water?
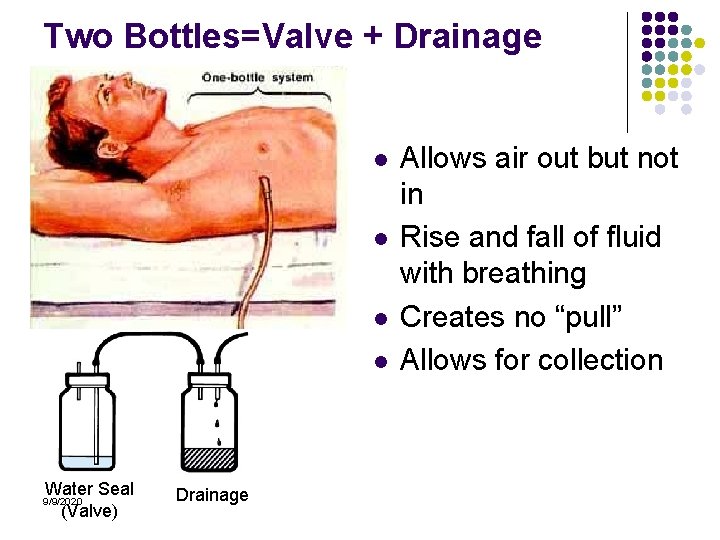
Two Bottles=Valve + Drainage l l Water Seal (Valve) 9/9/2020 Drainage Allows air out but not in Rise and fall of fluid with breathing Creates no “pull” Allows for collection
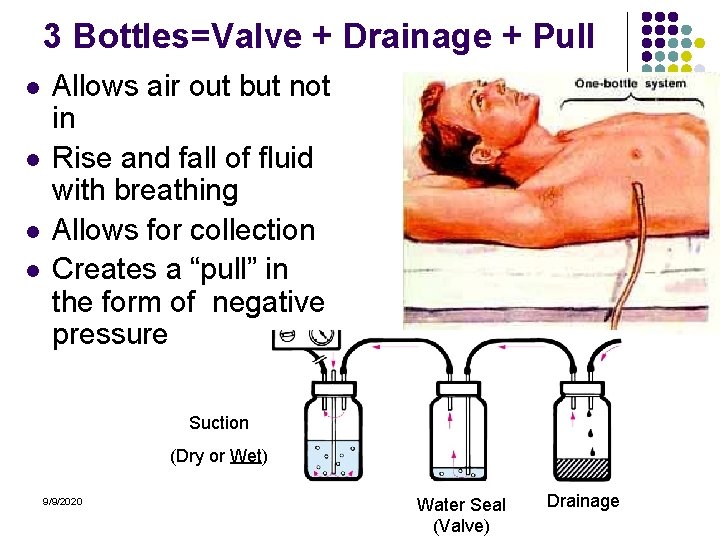
3 Bottles=Valve + Drainage + Pull l l Allows air out but not in Rise and fall of fluid with breathing Allows for collection Creates a “pull” in the form of negative pressure Suction (Dry or Wet) 9/9/2020 Water Seal (Valve) Drainage

Commercial chest tubes Wet Suction = actual column of water used 9/9/2020 (usually 20 cm) Dry Suction = pressure and vacuum internally regulated

In Clinical… l l l The units are connected to wall suction unless the order is for water seal only Wall suction creates a vacuum, while the column of water creates the actual “pull” Turning up the wall suction, WILL NOT increase the pull A column of water creates pressure, much like when you are diving underwater Therefore, increasing the column of water WILL increase the pull 9/9/2020

Nursing Responsibilities l Standard 1 Assessment l l l l 9/9/2020 Patency/functioning of system (kinks, clamps, atrium, suction, etc) Dressings Quantity and quality of drainage Dependency of collection system Coiled tubing, not hanging tubing Pain control Respiratory status and Vital signs (CDB/IS, lung sounds, respiratory quality/number)

Nursing Responsibilities l Standard 5 Implementation l Note specific orders regarding: l l l 9/9/2020 Suction versus water seal Amount of acceptable drainage I&O X-rays Administer pain medications regularly Patient should change positions frequently (promotes drainage, prevents complications)

BSN Essentials l l l Critical thinking and technical skills = Having the knowledge and skill to handle problems! Always have at the ready: l l l 9/9/2020 Extra atrium/set-up Oxygen Suction Occlusive dressings Chest tube clamps Bottle of sterile normal saline

Patient Ed: Standard 5 B Reducing anxiety… l l l l l Teach basics of drainage system, frequent checks, ask for analgesics PRN Assure that CT is sutured in place Remind not to kink/compress tubing Drainage system to be kept below level of chest Fluctuations in water seal are normal Prepare for expected amount & type of drainage May hear bubbling if it is a “wet” suction system Discuss ambulating and repositioning Plan of care 9/9/2020

Chest Tubes: Removal l l l When “tidaling” ceases and chest Xray/assessments confirm re-expansion of lung Pre-medicate for pain Breath in & hum out (have pt practice) CT is quickly removed Occlusive dressing applied over insertion site Pleura seals itself off Chest wound heals within a week 9/9/2020
- Slides: 21