Care of Patients with Diabetes Mellitus Insulin Administration

Care of Patients with Diabetes Mellitus: Insulin Administration Skills Lab Mrs. April Page, ARNP MSN FNPC NUR 1213 C INTERMEDIATE ADULT CARE GULF COAST STATE COLLEGE ASSOCIATE DEGREE NURISNG PROGRAM

Lesson Objectives • Demonstrate the technique for blood glucose monitoring and the proper technique for mixing insulins in an insulin syringe • Apply clinical skills to show proper technique for administering insulin injections including pens • Differentiate various types of insulins including onset, peak, and duration of action and what patient outcomes to expect

Demonstrate the technique for blood glucose monitoring and the proper technique for mixing insulins in an insulin syringe Lesson Objective One

Measuring Blood Glucose • Blood Glucose measurements are usually done several times a day: AC and HS; PC and PRN • They are physician ordered. • A Postprandial blood sugar is collected 2 hours after a meal; the blood sugar should be normal • Diabetes medication may be adjusted based on the postprandial blood sugar reading. 4

Infection Prevention Use standard precautions when performing blood glucose testing 5

CDC Requirements for Safe Glucometer Use Fingerstick devices should never be used for more than one person. If shared, blood glucose meters should be cleaned and disinfected after each use. www. cdc. gov/injectionsafety/blood-glucose-monitoring. html 6

Blood Glucose Monitors Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Glucometers • There are multiple kinds of glucometers. • The test strip and reagent used for blood sugar testing must be compatible with the meter. • Always Check the expiration date on the test strips. • Facilities calibrate their meters every day and record them on a log (or in the hospital it goes electronically to the lab). • In the hospital you will see q 12 hours or qday http: //commons. wikimedia. org/wiki/File: Blausen_0299_Diabetes_Blood. Glucose. Meter. png 8
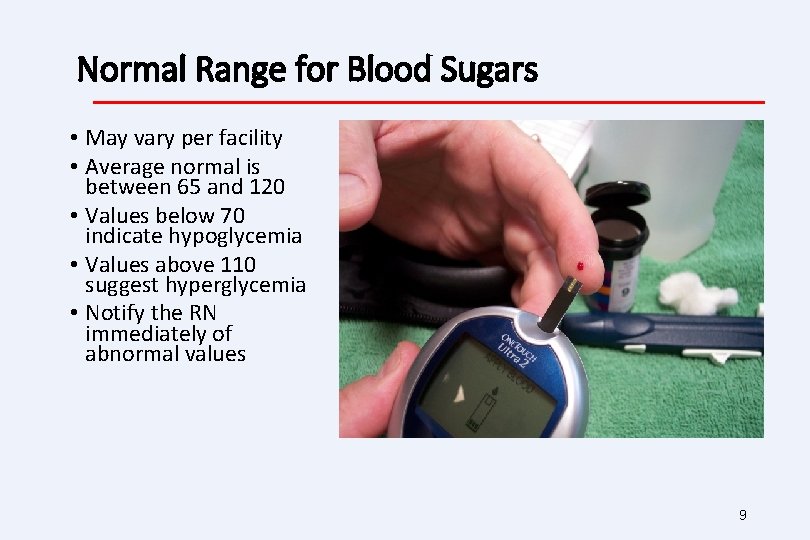
Normal Range for Blood Sugars • May vary per facility • Average normal is between 65 and 120 • Values below 70 indicate hypoglycemia • Values above 110 suggest hyperglycemia • Notify the RN immediately of abnormal values 9

Range of Glucometers • Some blood glucose meters do not have a large range • They may display “low” or “high” • If this happens the patient has the potential for serious complications. Notify the RN STAT 10

Performing Blood Glucose Testing • Preparing and Administring Insulin Video • Watch In Your Clinical Skills: Essentials Collection In Evolve
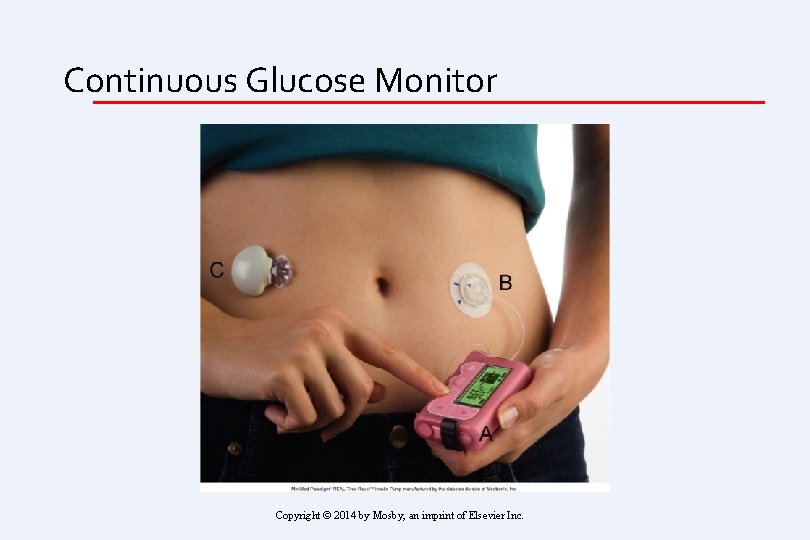
Continuous Glucose Monitor Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Differentiate various types of insulins including onset, peak, and duration of action and what patient outcomes to expect Lesson Objective Three
Insulin & Diabetes

Insulin therapy • Control of blood glucose is a balance between insulin therapy, diet and activities • The goal is to keep glucose as near normal as possible • The type of insulin regimen used depends on many factors, e. g. patient age, compliance, patient schedule, etc.
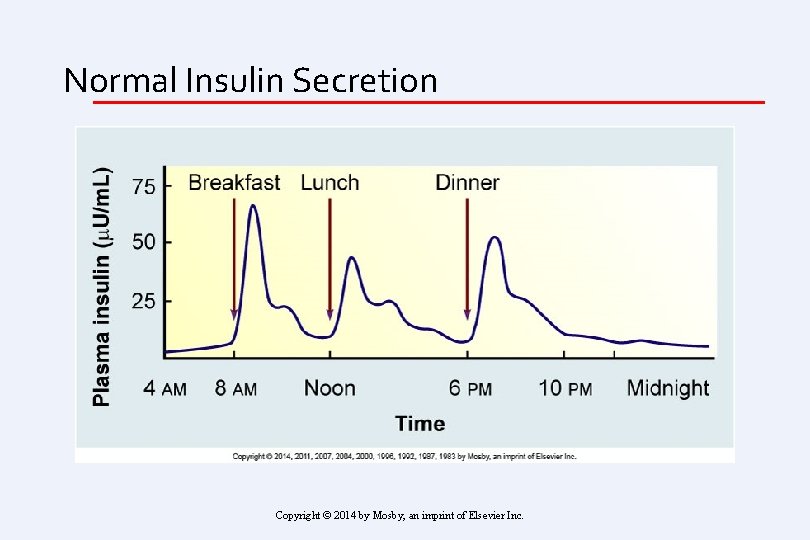
Normal Insulin Secretion Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
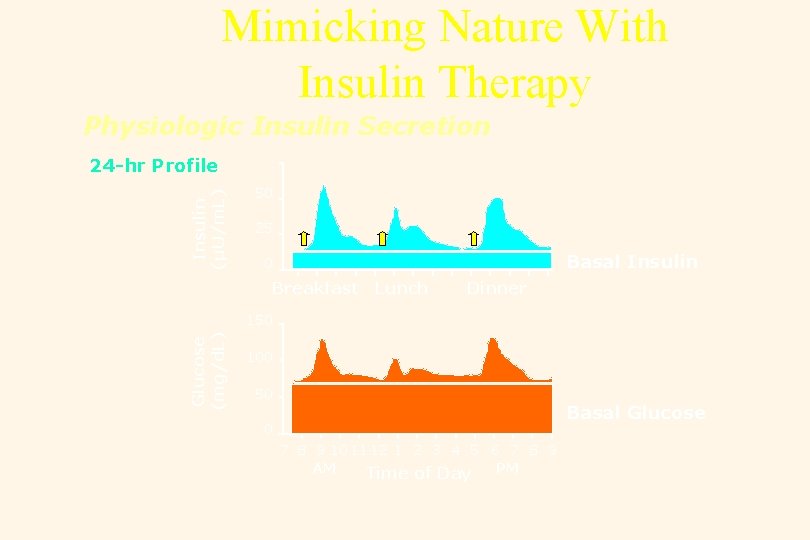
Mimicking Nature With Insulin Therapy Physiologic Insulin Secretion Insulin (µU/m. L) 24 -hr Profile 50 25 Basal Insulin 0 Breakfast Lunch Dinner Glucose (mg/d. L) 150 100 50 Basal Glucose 0 7 8 9 10 11 12 1 2 3 4 5 6 7 8 9 AM Time of Day PM

Insulin • Exogenous insulin • Insulin from an outside source • Required for type 1 diabetes • Prescribed for patients with type 2 diabetes who cannot control blood glucose by other means

Insulin • Human insulin • Genetically engineered in laboratories • Categorized according to onset, peak action, and duration • • Rapid-acting Short-acting Intermediate-acting Long-acting
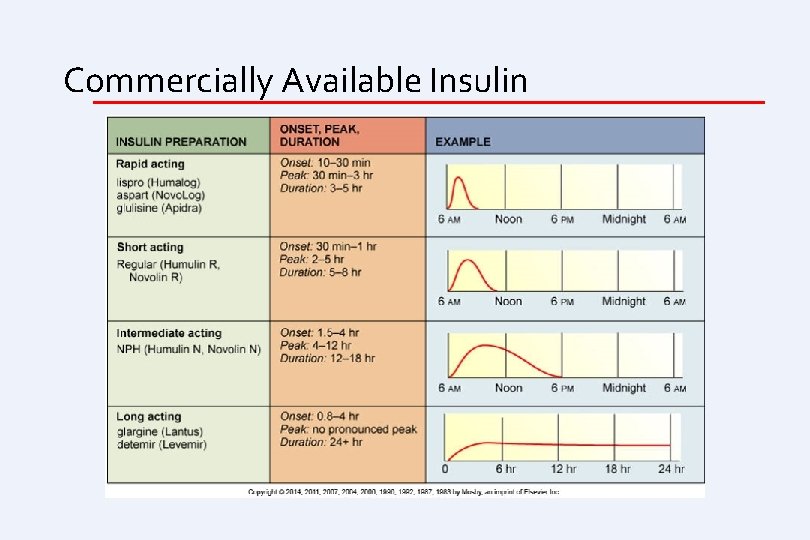
Commercially Available Insulin

The Basal/Bolus Insulin Concept • Basal Insulin – Suppresses glucose production between meals and overnight – 50% of daily needs • Bolus Insulin (Mealtime or Prandial) – Limits hyperglycemia after meals – Immediate rise and sharp peak at 1 hour – 10% to 20% of total daily insulin requirement at each meal

Insulin Regimens • Basal-bolus regimen • Most closely mimics endogenous insulin production • Rapid- or short-acting (bolus) insulin before meals • Intermediate- or long-acting (basal) background insulin once or twice a day • Less intense regimens can also be used

Mealtime Insulin (Bolus) • Insulin preparations • Rapid-acting (bolus) • Lispro, aspart, glulisine • Onset of action 15 minutes • Injected within 15 minutes of mealtime • Short-acting (bolus) • Regular with onset of action 30 to 60 minutes • Injected 30 to 45 minutes before meal • Onset of action 30 to 60 minutes Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Comparison of bolus insulins • Regular insulin • Requires administration 20 to 40 minutes prior to meal • Mismatch with postprandial hyperglycemic peak • Potential for late postprandial and nocturnal hypoglycemia • Rapid-acting (lispro, aspart, glulisine) • Convenient administration at/after meal • Matches postprandial glycemic peak • Reduced late postprandial hypoglycemia • Frequent late postprandial hyperglycemia • Risk for early hyopglycemia

(Basal) Background Insulin • Used to control glucose levels in between meals and overnight • Long-acting (basal) • • Insulin glargine (Lantus) and detemir (Levemir) Released steadily and continuously with no peak action Administered once or twice a day Do not mix with any other insulin or solution Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

(Basal) Background Insulin • Intermediate-acting insulin • • • NPH Duration 12 to 18 hours Peak 4 to 12 hours Can mix with short- and rapid-acting insulins Cloudy; must agitate to mix Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Comparison of basal insulins • NPH/lente • Pronounced peaks • Less than 24 -hour duration of action-requires BID dosing • Increased risk of hypoglycemia if meal delayed • Increased nocturnal hypoglycemia • Glargine • Usually once-a-day dosing • Flat peakless profile causes less hypoglycemia, esp. nocturnal • Risk of hypoglycemia when used as the only insulin

Combination Insulin Therapy • Can mix short- or rapid-acting insulin with intermediate-acting insulin in same syringe • Provides mealtime and basal coverage in one injection • Commercially premixed or self-mix Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Drawing Up Insulin • How to draw up more than one type of insulin • Watch In Your Clinical Skills: Essentials Collection In Evolve
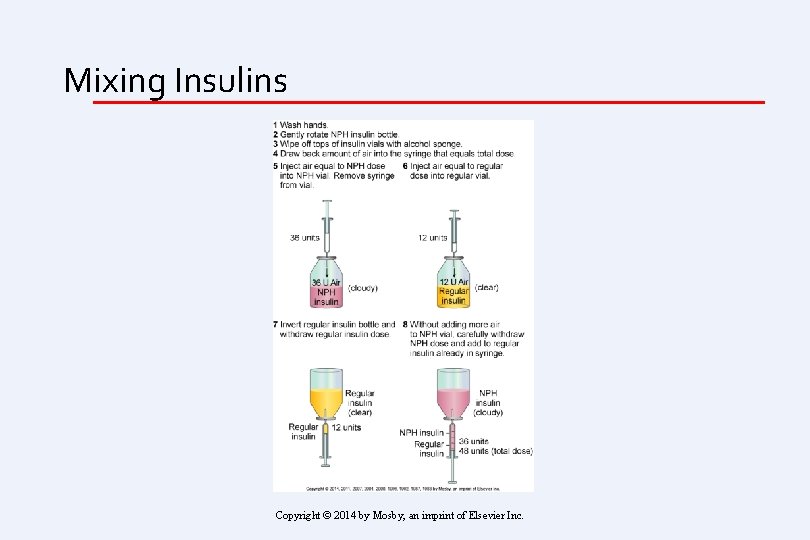
Mixing Insulins Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Insulin • Storage of insulin • • • Do not heat/freeze In-use vials may be left at room temperature up to 4 weeks Extra insulin should be refrigerated Avoid exposure to direct sunlight, extreme heat or cold Store prefilled syringes upright for 1 week if two insulin types; 30 days for one

Apply clinical skills to show proper technique for administering insulin injections including pens Lesson Objective Two

Insulin • Administration of insulin • Typically given by subcutaneous injection • Regular insulin may be given IV • Cannot be taken orally

Insulin • Administration of insulin • • Absorption is fastest from abdomen, followed by arm, thigh, and buttock Abdomen is preferred site Do not inject in site to be exercised Rotate injections within one particular site
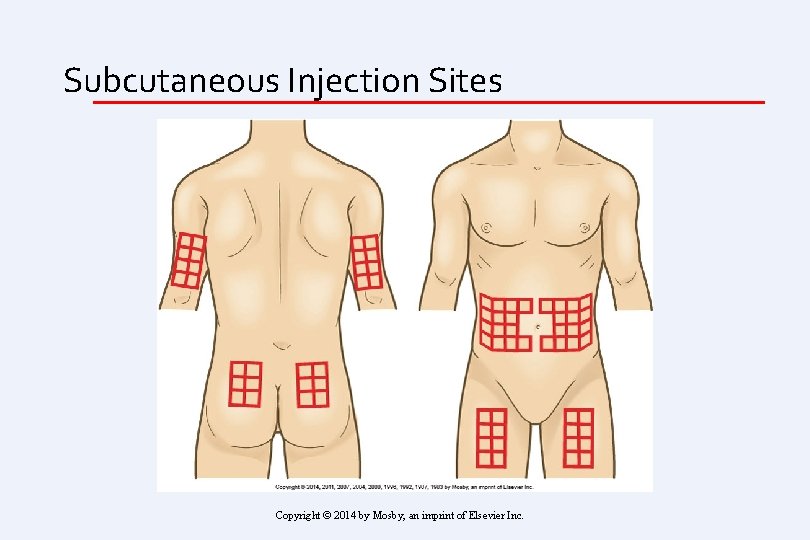
Subcutaneous Injection Sites Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Insulin • Administration of insulin • • • Usually available as U 100 insulin (1 m. L contains 100 U of insulin) Syringes marked for units: various sizes Only user recaps syringe No alcohol swab for self-injection; wash with soap and water Inject at 45 - to 90 -degree angle
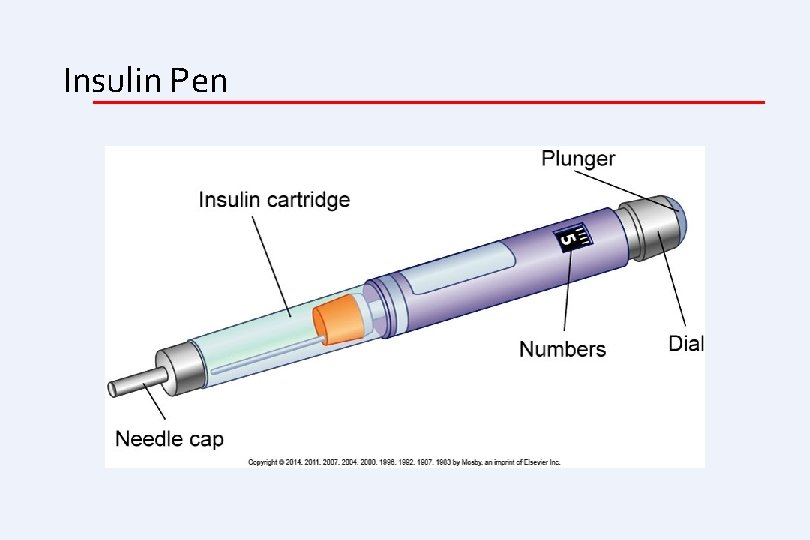
Insulin Pen

Insulin • Insulin pump • Continuous subcutaneous infusion • Battery-operated device • Connected to a catheter inserted into subcutaneous tissue in abdominal wall • Program basal and bolus doses that can vary throughout the day • Potential for tight glucose control • Typically use aspart or lispro insulin in pumps, which makes the pumps very responsive • Considered the “gold standard” of treatment of type 1 diabetes
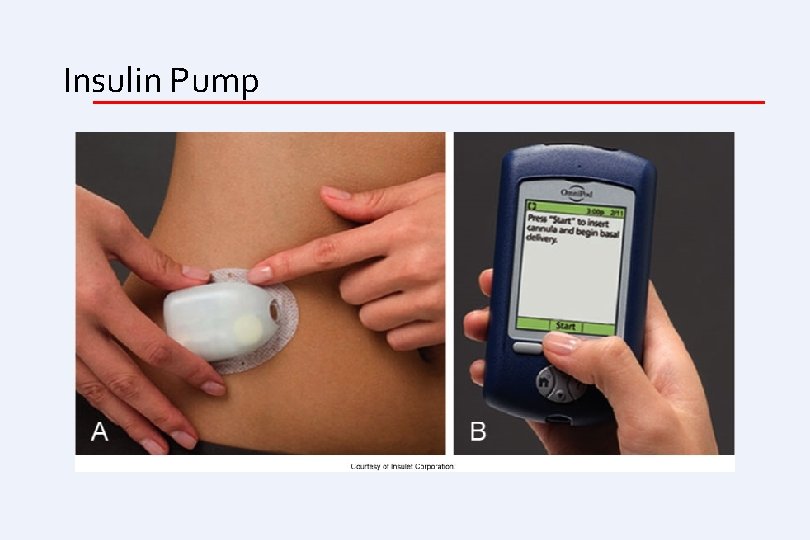
Insulin Pump

Insulin pumps-benefits • The most physiological way to deliver insulin • The most flexible way to deliver insulin • Timing of meals • Exercise • Sick-days • Can attain excellent glucose control with less hypoglycemia

Insulin • Problems with insulin therapy • Hypoglycemia • Allergic reaction • Lipodystrophy

Somogyi Effect • Somogyi effect • Rebound effect in which an overdose of insulin causes hypoglycemia • Release of counterregulatory hormones causes rebound hyperglycemia

Dawn Phenomenon • Dawn phenomenon • Morning hyperglycemia present on awakening • Due to release of counterregulatory hormones in predawn hours

Insulin pumps-basal rate • Pumps now allow for up to 48 basal rates per day • Up to 3 basal “patterns” • Can program to match individual patient needs, e. g. strong dawn phenomenon • Have temporary basal rates- e. g. use for exercise

Insulin pumps-disadvantages • Cost ($7500 with $2 -3000/yr. for supplies) • Skin problems • allergies/reactions to tape • infection at infusion site • Occasional pump malfunction • Lack of depot insulin- can rapidly develop DKA if infusion is disrupted
- Slides: 45