CARE FOR THE DETERIORATING OB PATIENT DURING A

CARE FOR THE DETERIORATING OB PATIENT DURING A RAPID RESPONSE EVENT Dionne Walker MSN, RNC-OB Clinical Specialist, Women’s Services Tara Barrick MSN, RNC-OB High Risk OB Clinical Specialist

OBJECTIVES Discuss the overview and background in emergency obstetrics Review of Global Maternal Mortality data Describe the different roles and responsibilities of each team member during a rapid response event Recognize the importance of communication, collaboration and teamwork during an Rapid Response event Review of Women’s Services RRT data


Vicki Mc. Guire https: //www. usatoday. com/deadly-deliveries/videos/#vicki-mcguire

42

BACKGROUND The health of the population is rapidly changing, in part related to: Obesity related complications such as hypertension and diabetes The likelihood of developing a comorbidity increases with maternal age Snapshot of today’s OB patient Advanced Maternal Age Today’s average of first time mother is 3. 6 years older than in 1970 Overweight In 2009, 24. 4% of women in childbearing age were considered obese (BMI >30) More likely to undergo cesarean birth National rate for C-section delivery is 31. 8%
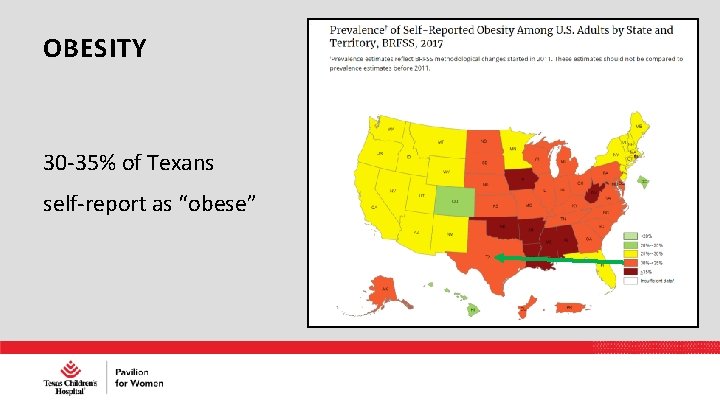
OBESITY 30 -35% of Texans self-report as “obese”

Globally speaking… Every minute a woman dies from complications related to pregnancy or childbirth Approximately 529, 000 women per year
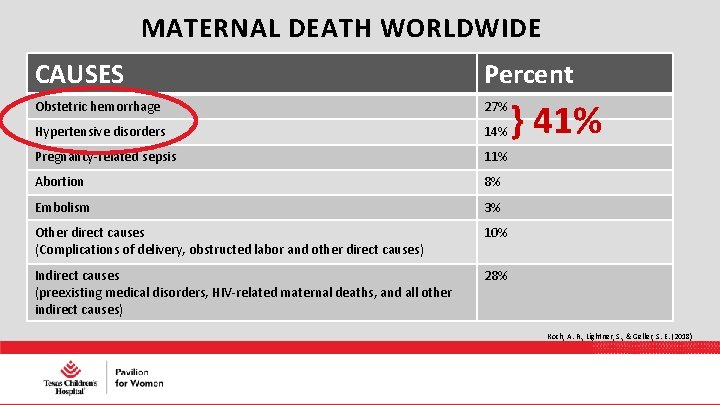


MATERNAL DEATH WORLDWIDE CAUSES Percent Obstetric hemorrhage 27% Hypertensive disorders 14% Pregnancy-related sepsis 11% Abortion 8% Embolism 3% Other direct causes (Complications of delivery, obstructed labor and other direct causes) 10% Indirect causes (preexisting medical disorders, HIV-related maternal deaths, and all other indirect causes) 28% } 41% Koch, A. R. , Lightner, S. , & Geller, S. E. (2018)
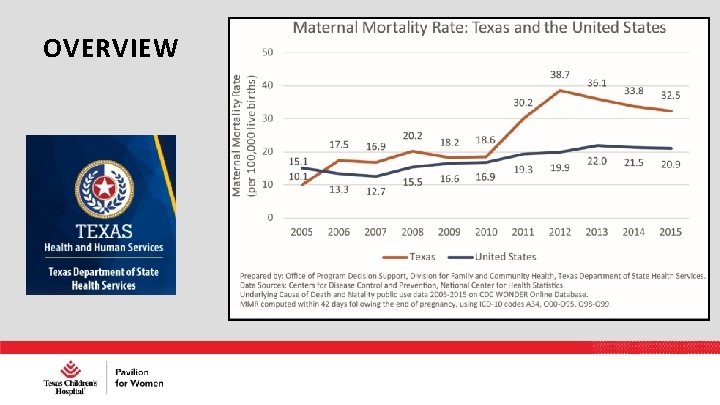
OVERVIEW
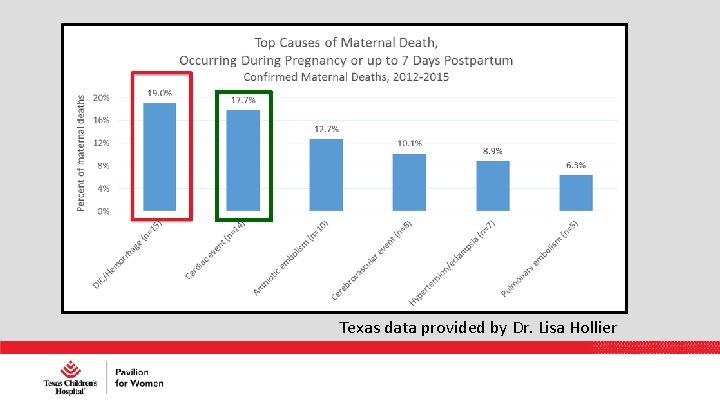
Texas data provided by Dr. Lisa Hollier

Since 2009, obstetric emergencies have 75% associated with delivery complications 114% associated with Postpartum hemorrhage The perinatal team must anticipate and be prepared to respond to obstetric emergencies Committee Opinion #590, 2018

Maternal Mortality: Three Contributing Factors Delay in the decision to seek care Delay in arrival to an appropriate medical care facility Delay in receiving adequate care once a woman arrives to medical facility Women’s Services


Recommendations 1. Mechanism for activating a RR based on clinical criteria Developed a rapid response (RR) for Perinatal Safety with a focus on physiological deterioration and urgent conditions of maternal and fetal patient population 2. Multidisciplinary clinical team that responds to, assesses and manages deteriorating patients 3. System for feedback to help mitigate and/or improve future RR events 4. Administrative structure responsible for implementing, training and monitoring all RR events

Recommendations 1. Planning 2. Resource Provision 3. Implementation of an Early Warning System Preparing for Clinical Emergencies in Obstetrics and Gynecology Committee Opinion #590 Hospital-Based Triage of Obstetric Patients 4. Implementation of a Rapid Response Team 5. Training ***Emergency Drills and Simulation*** Committee Opinion #667 Committee on Patient Safety & Quality Improvement 6. Implementation of the Maternal Fetal Triage Index


RAPID RESPONSE IN THE PERINATAL SETTING WOMEN’S SERVICES RRT DATA
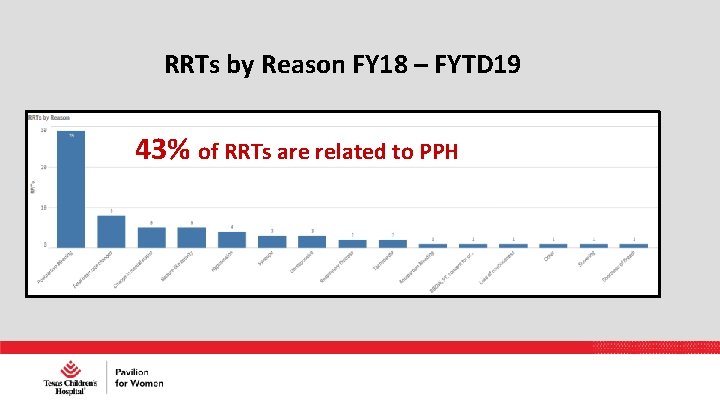
RRTs by Reason FY 18 – FYTD 19 43% of RRTs are related to PPH
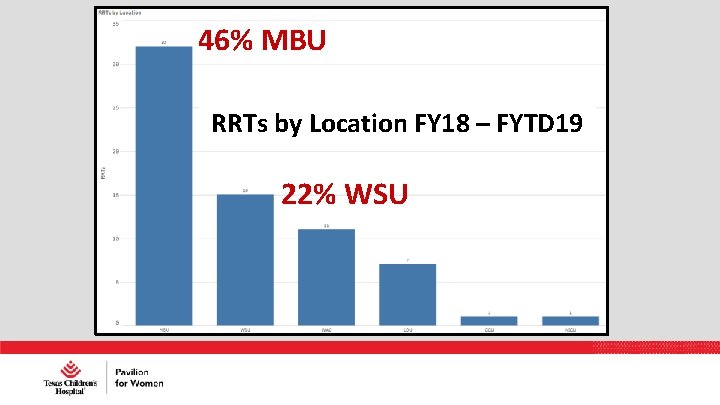
46% MBU RRTs by Location FY 18 – FYTD 19 22% WSU
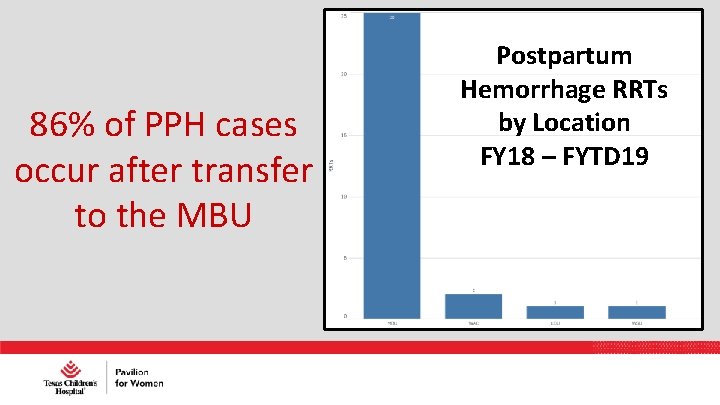
86% of PPH cases occur after transfer to the MBU Postpartum Hemorrhage RRTs by Location FY 18 – FYTD 19
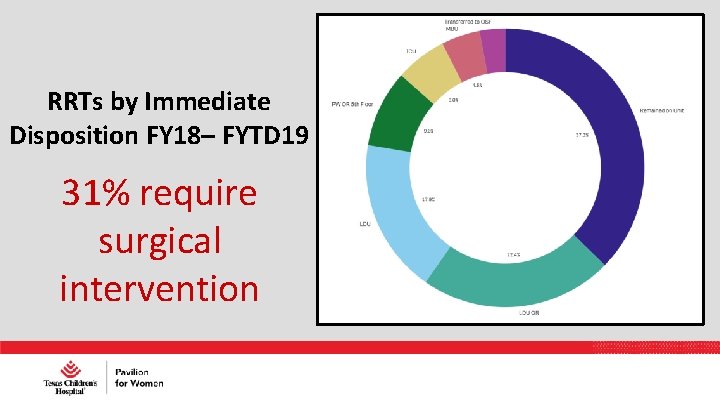
RRTs by Immediate Disposition FY 18– FYTD 19 31% require surgical intervention
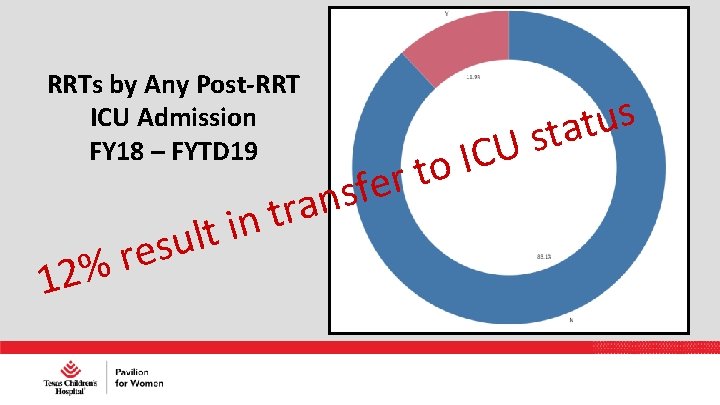
RRTs by Any Post-RRT ICU Admission FY 18 – FYTD 19 1 u s e r 2% r t lt in U C I o t r e f s an s u t sta

RRT REBOOT Review of team members’ role & responsibilities Patient disposition process Post RRT patient assessment Procedural documentation

RRT MEMBERSHIP IN THE PFW Primary Bedside RN 1 st Emergency Responder LDU RN (ER 1) 2 nd Emergency Responder Unit Charge RN (ER 2) Pulmonary Critical Care Physician (PCCM) Hospitalist/OB Resident (PGY 3) Anesthesiologist/CRNA Pharmacy House Supervisor Respiratory Therapist (RT) Security

RRT ROLES & RESPONSIBILITIES Primary RN assumes a lead role during the RRT Activates RRT to summon help Remains with the patient prior to team arrival and throughout the RR event Delegates tasks to other team members as needed Helper to secure crash cart/PPH cart Recorder (records details of the RR event in the RRT Navigator) Runner (to obtain medications and supplies) Performs ongoing focused assessment/obtains vital signs Provides SBAR report to responding RRT Pertinent medical/obstetric history Other pertinent information (i. e. allergies, medications, lab results) Indication for activating RR Interventions performed prior to team arrival

RRT ROLES & RESPONSIBILITIES Activating Unit’s Charge RN assists the Primary RN/RR Team Assists with medication preparation or delegates this task Assists with procedures or delegates this task Audits EMR to ensure documentation is complete

RRT ROLES & RESPONSIBILITIES 1 st & 2 nd RN Responders (ER 1/ER 2) LDU RN/activating unit’s charge RN who assists the Primary RN/RR Team during the event ER 1 receives SBAR from Primary RN ER 1 reports clinical observations to the team as needed ER 1 & ER 2/activating unit’s Charge RN assist with clinical interventions as needed Performs a 1 hour re-assessment if the patient remains on the unit

RRT ROLES & RESPONSIBILITIES Pulmonary Critical Care Physician (PCCM) and/or Hospitalist/OB Resident (PGY 3) Performs comprehensive assessment Determines treatment/plan of care Enters orders as needed Determines whether patient remains on unit versus transfer to HLOC

RRT ROLES & RESPONSIBILITIES Pharmacist Provides emergency medications as needed

RRT ROLES & RESPONSIBILITIES House Supervisor Room traffic control Coordinates transfer to HLOC/room management

RRT ROLES & RESPONSIBILITIES Respiratory Therapist (RT) Performs respiratory assessment/treatments as needed Provides ventilation/oxygenation as needed Obtains blood gases if ordered

RRT ROLES & RESPONSIBILITIES Anesthesiologist/CRNA Obtain IV access Manages airway as needed Assume lead role if RR escalates to OH/MTP or necessity to transfer patient to the operating room

RRT ROLES & RESPONSIBILITIES Security Traffic control (hallways/elevators) Elevator securement Visitor management

RRT ROLES & RESPONSIBILITIES FINDINGS #1 The primary RN should remain with the patient throughout the RR event Provides SBAR report to responders Delegates tasks to other team members (i. e. recorder, runner, etc. ) Assist with medication prep/procedures/transfers #2 The RR Team members should offer coaching & mentoring to the primary RN and the activating unit’s nursing team #3 The RN responder roles/responsibilities should be shared between the LDU RNs and the activating RNs charge RN #4 Charge RN on activating unit ensures that RRT documentation is complete

DRILLS/SIMULATION • Conducted periodic drills on the two units with highest incidence of rapid response events • Focused on PPH drills and the hypertensive/eclamptic patient.
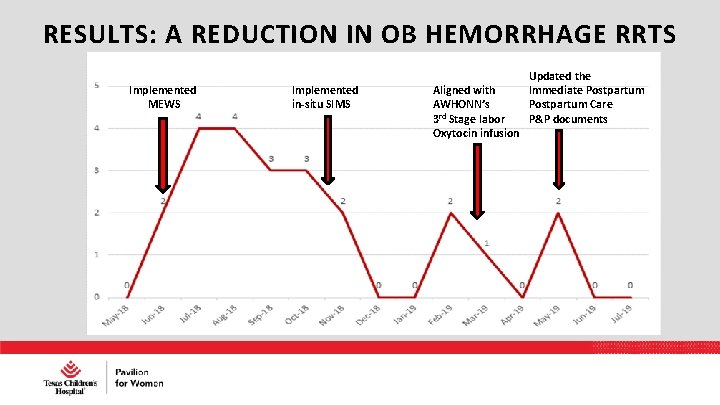
RESULTS: A REDUCTION IN OB HEMORRHAGE RRTS Implemented MEWS Implemented in-situ SIMS Aligned with AWHONN’s 3 rd Stage labor Oxytocin infusion Updated the Immediate Postpartum Care P&P documents

OTHER INITIATIVES Obstetric Hemorrhage Algorithm Adult Massive Transfusion Protocol Maternal Fetal Triage Index (MFTI) Maternal Early Warning System (MEWS) The Alliance for Innovation of Maternal Health (Texas AIM)

Obstetric Hemorrhage Algorithm (*related to uterine atony)

Adult Massive Transfusion Protocol (MTP)
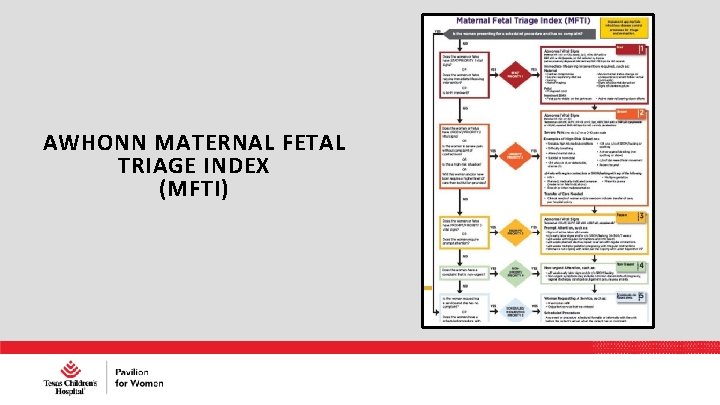
AWHONN MATERNAL FETAL TRIAGE INDEX (MFTI)

MATERNAL EARLY WARNING SYSTEM (MEWS)
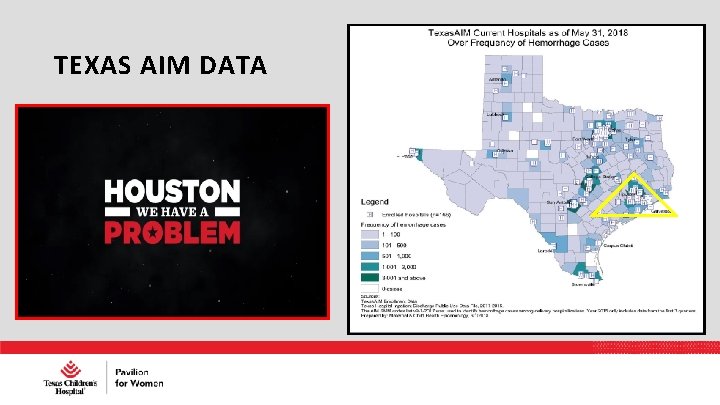
TEXAS AIM DATA

PATIENT SAFETY BUNDLE: OBSTETRIC HEMORRHAGE q. Readiness q. Recognition & Prevention q. Response q. Reporting/Learning

Our goal as a perinatal team: Healthy Mom, Healthy Newborn, Happy Family! #oneamazingteam

REFERENCES (n. d. ). Clinical Update: Improving response to signs of patient deterioration. Retrieved from https: //www. nursingtimes. net/roles/practice-nurses/clinical-update-improving-response-to-signs-of-patientdeterioration/296278. article#. (2016). Committee Opinion No. 667. Obstetrics & Gynecology, 128(1). doi: 10. 1097/aog. 0000001524. (2014). Committee Opinion No. 590. Obstetrics & Gynecology, 123(3), 722– 725. doi: 10. 1097/01. aog. 0000444442. 04111. c 6. (2011). Guidelines for Professional Registered Nurse Staffing for Perinatal Units Executive Summary. Journal of Obstetric, Gynecologic & Neonatal Nursing, 40(1), 131– 134. doi: 10. 1111/j. 1552 -6909. 2010. 01214. x. AWHONN. Guidelines for Oxytocin Administration after Birth: AWHONN Practice Brief Number 2. (2015). Nursing for Womens Health, 19(1), 99 -101. doi: 10. 1111/1751 -486 x. 12199. Aebeersold, M. , & Tschannen, D. (2013). Simulation in nursing practice: The impact on patient care. The Online Journal of Issues in Nursing, 18(2), manuscript 6. doi: 10. 3912/OJIN. Vol 18 No. O 2 Man 06. Brown, H. L. , Simpson, L. L. , & Eckler, K. (2019, May 22). Overview of maternal mortality and morbidity. Retrieved from https: //www. uptodate. com/contents/overview-of-maternal-mortality-and-morbidity. Women’s Services

REFERENCES, CONTINUED Green, M. , Rider, C. , Ratcliff, D. , & Woodring, B. C. (2015). Developing a Systematic Approach to Obstetric Emergencies. Journal of Obstetric, Gynecologic & Neonatal Nursing, 44(5), 677– 682. doi: 10. 1111/1552 -6909. 12729. Koch, A. R. , Lightner, S. , & Geller, S. E. (2018). Identifying Maternal Deaths in Texas Using an Enhanced Method, 2012. Obstetrics & Gynecology, 132(2), 520– 521. doi: 10. 1097/aog. 0000002771. Massey, D. , Chalboyer, W. , & Anderson, V. (2016). What factors influence ward nurses' recognition of and response to patient deterioration? An integrative review of the literature. Nursing Open, 1 -18. doi: 10. 1002/nop 2. 53. (n. d. ). Maternal and Child Health Epidemiology Program | Reproductive Health | CDC. Retrieved from https: //www. cdc. gov/reproductivehealth/mchepi/index. htm. Petersen EE, Davis NL, Goodman D, et al. Vital Signs: Pregnancy-Related Deaths, United States, 2011– 2015, and Strategies for Prevention, 13 States, 2013– 2017. MMWR Morb Mortal Wkly Rep 2019; 68: 423– 429. DOI: http: //dx. doi. org/10. 15585/mmwr. mm 6818 e 1 external icon. Vincent, J. , Einav, S. , Pearse, R. , Jaber, S. , Kranke, P. , Overdyk, F. J. , . . . Hoeft, A. (2018). Improving detection of patient deterioration in the general hospital ward environment. European Journal of Anaesthesiology, 1. doi: 10. 1097/eja. 0000000798. Women’s Services
COMMENTS/QUESTIONS?
- Slides: 50