Cardiovascular system By Dr Zkia Mohamed Cardiovascular physiology

Cardiovascular system By: Dr. Zkia Mohamed
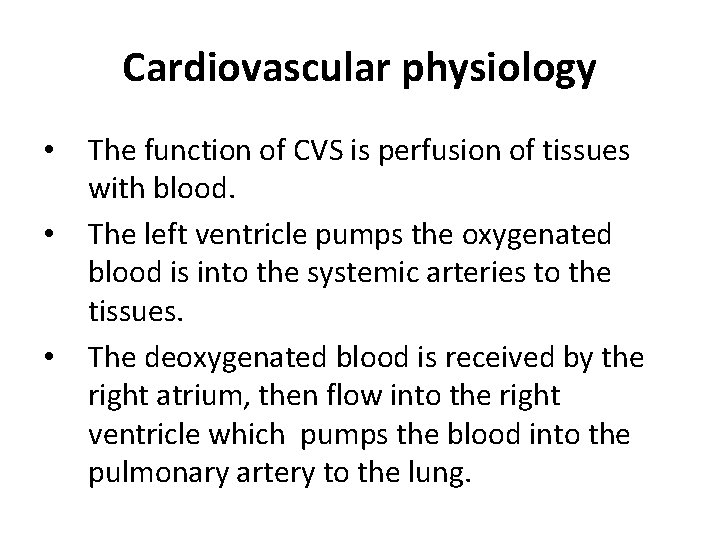
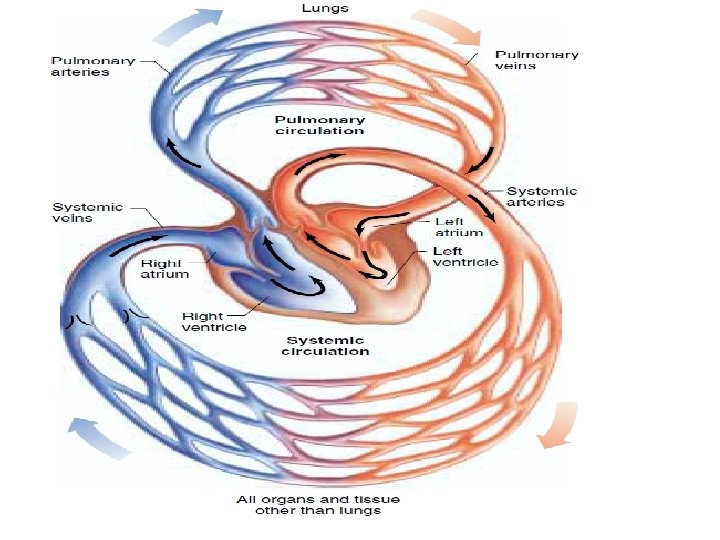
Cardiovascular physiology • • • The function of CVS is perfusion of tissues with blood. The left ventricle pumps the oxygenated blood is into the systemic arteries to the tissues. The deoxygenated blood is received by the right atrium, then flow into the right ventricle which pumps the blood into the pulmonary artery to the lung.

The venous return • The blood that returns from the tissues via the veins to the heart atria. • Increases by: ØIncrease in blood volume (H 2 O & electrolytes). ØVenoconstrictors eg. Noradrenaline. ØContraction of skeletal muscles (Exercise) pushes the blood by pressing the veins.

Ø Contraction of inspiratory muscles at start of inspiration decrease intrathoracic pressure Blood Suction to the heart. • The gravity decreases the venous return from the body parts below the heart level during standing. & vice versa. .

Cardiac cycle The events from one heart beat to another = 0. 8 second. • Each cycle is made of: 1. Diastole: Period of relaxation of cardiac muscles of 0. 5 second (2/3 cycle). Important for rest of the heart, filing of the heart chambers with blood & perfusion of the cardiac muscles. 2. Systole: Period of contraction of cardiac muscle = 0. 3 second (1/3 cycle).

Cardiac output COP The amount of blood pumped by each ventricle per unit of time = 5 L/Minute. COP = Heart rate x Stroke volume. COP = 72 BPM x 70 m. L= 5 L/min. COP ↑ by the factors that increase the heart rate & force of contraction (SV) : • ↑ Venous return to the heart. • ↑ Body or environmental temperature. • Catecholamines (Adrenaline & Nor adrenaline) via ᵝ 1 receptors. & Dopamine.
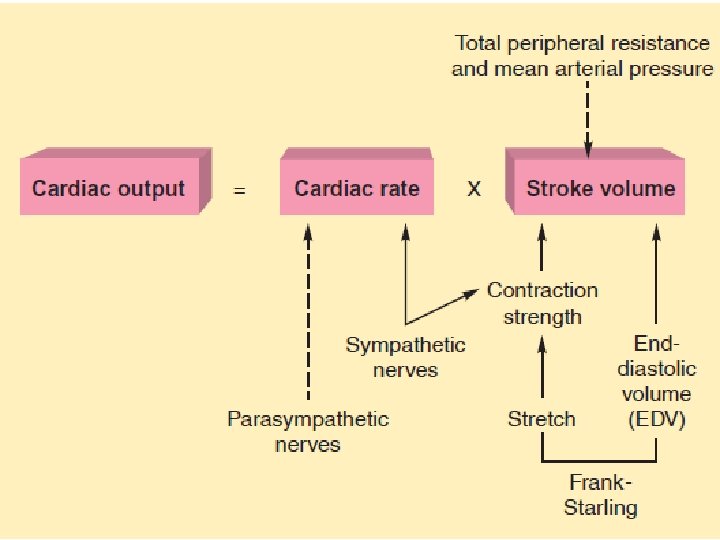

COP decreases by factors that decrease the heart rate & force of contraction eg: Ø Parasympathetic N. system. Ø ↑ Potassium ions in the blood (Hyperkalaemia). Ø Cooling of the heart.
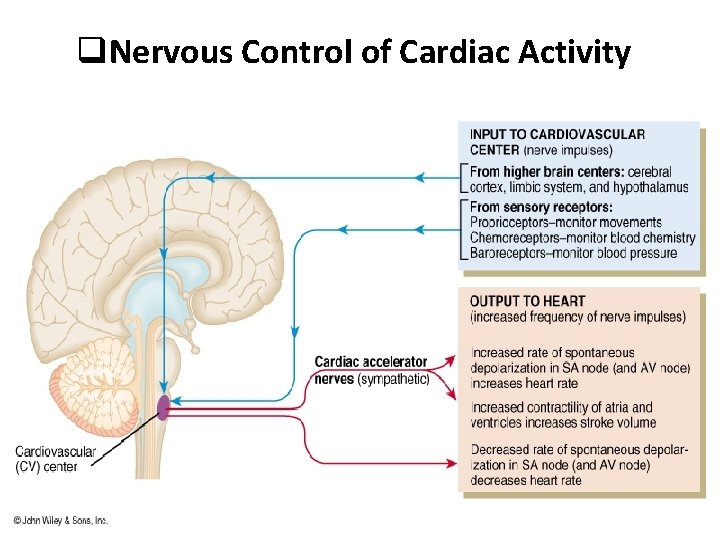
q. Nervous Control of Cardiac Activity

Arterial blood pressure ABPr: § Is the force that causes the blood flow in the vessels. § = Cardiac output x peripheral resistance. § peripheral resistance in arterioles: Ø ↑ by blood viscosity & vasoconstrictors Ø & ↓ by vasodilators. § Is measured, from the brachial artery by sphygmomanometer & stethoscope.
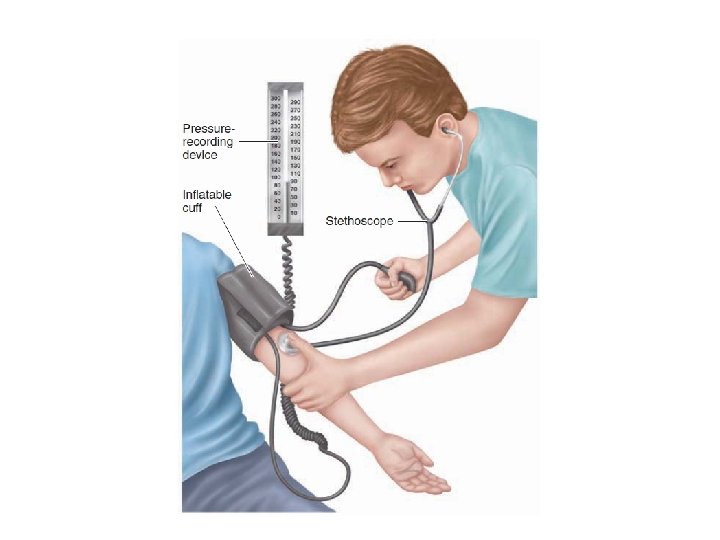

§ It is normally equal 120/70 mm. Hg (Systolic ABPr/Diastolic ABPr). • Systolic ABPr: The highest pressure in the arteries during contraction of the heart • Diastolic ABPr: The lowest pressure in the arteries during relaxation of the heart

Regulation of ABPr: 1. Neural regulation: • Center in the medulla oblongata. Made of vasomotor area which activates the sympathetic system & cardioinhibitory area which activates the parasympathetic system. • Main receptors are baroreceptors in arterial walls mainly aortic arch & carotid sinus,
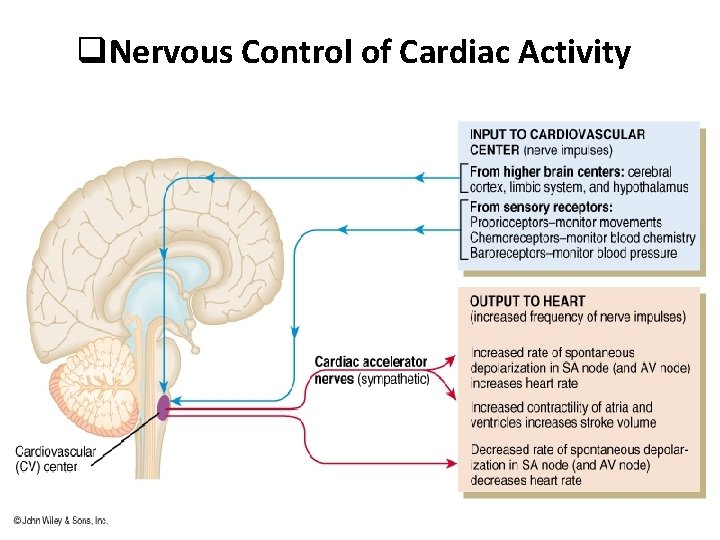
q. Nervous Control of Cardiac Activity
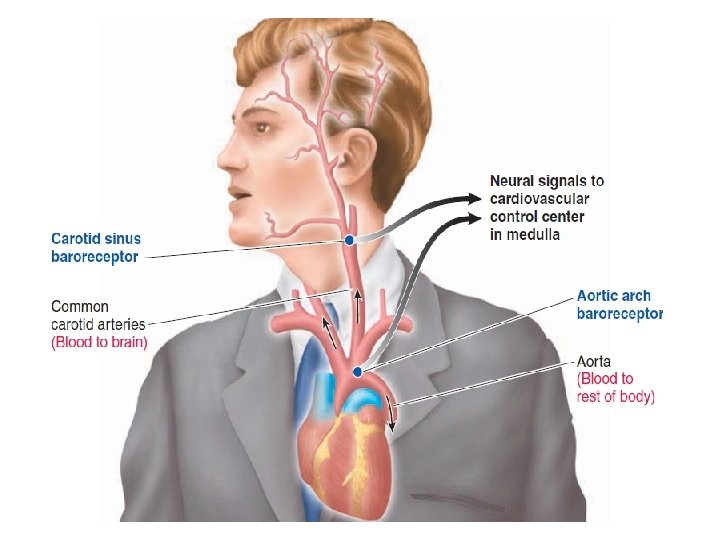

• Baroreceptors are stimulated by increase in blood pressure • The response to Baroreceptors stimulation is activation of parasympathetic system & inhibition of sympathetic system to decrease the pressure to normal.

2. Hormonal regulation of ABPr: Role of Renin–Angiotensin system in control of ABPr: • Renin is a polypeptide hormone secreted by the kidneys in response to: Ø Fall in systemic blood pressure ↓due to hypovolaemia & hyponatraemia. Ø Sympathetic stimulation. Ø Catecholamines.

• Angiotensinogen is a large protein synthesized by the liver • Renin acts on circulating angiotensinogen to produce Angiotensin 1, which is then converted to Angiotensin 11 by the action of angiotensin converting enzyme (ACE) secreted by the endothelial cells mainly In lungs.
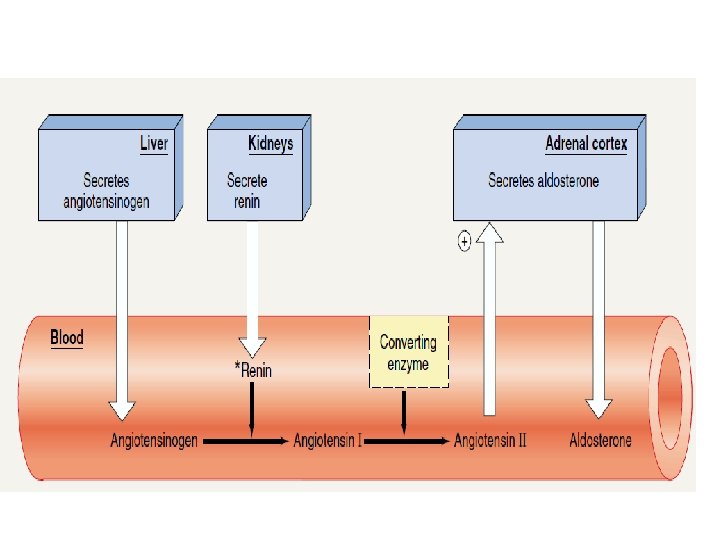

• Angiotensin. II maintains ABPr by: Ø Vasoconstriction. Ø Stimulates contraction of the heart, Ø Stimulation of thirst centre Ø Stimulates Aldosterone secretion from adrenal cortex.

Aldosterone Stimulates Sodium reabsorption from renal distal collecting tubules & collecting duct. Ø Stimulation of Vasopressin secretion from posterior pituitary gland.
- Slides: 22